Retrovirus mediated hematopoietic gene therapy: A European regulatory perspective with special focus on the situation in Germany
Christine Voelkel1,2, Anke Lührmann2, Christopher Baum1,3, and Heiko E. von der Leyen2
1Department of Experimental Hematology, Hannover Medical School, D-30625 Hannover, Germany;
2Hannover Clinical Trial Center GmbH, D-30625 Hannover, Germany;
3Division of Experimental Hematology, Cincinnati Children’s Research Foundation, Cincinnati, Ohio, USA
Correspondence
Prof. Dr. Heiko E. von der Leyen, Hannover Clinical Trial Center GmbH, Carl-Neuberg-Str. 1, D-30625 Hannover, Germany,
Tel.: +49 511 533 333 0, Fax: +49 511 533 333 99, E-mail: vdleyen@clinical-trial-center.de
Accepted 30 March 2009
Published 14 May 2009
Summary
Retrovirus mediated gene therapy has already proven to be more than just a theoretical option to treat patients with severe genetic defects. Clinical gene therapy trials of X-linked severe combined immunodeficiency or adenosine deaminase deficiency have demonstrated the success and potential benefit of the therapy. Nevertheless, the complexity of the therapeutic products and their biological origin, as well as virus-related safety concerns require the need of a strict regulatory framework in order to guarantee the quality of the individual products and safety of the patients. The aim of this review is to give an overview of the rapidly evolving regulatory framework of Advanced Therapy Medicinal Products in Europe. We will summarize the most important regulatory documents to be considered before entering the clinical development phase – not only from a German but also from a European perspective.
Keywords
Clinical trials, gene therapy, side effects, regulatory framework, retrovirus
Introduction
Clinical gene therapy is a very ambitious intent. The general principle sounds as easy as it is ingenious. Instead of treating the symptoms of severe genetic diseases such as immunodeficiencies or metabolic disorders, gene therapy intends to cure the underlying genetic defect by introducing a corrected copy of the mutated gene, or even by correcting the affected gene itself. In the context of disorders affecting the hematopoietic system, patient-derived cells can be treated ex vivo with engineered gene vectors designed to deliver the therapeutic gene. Except in those diseases associated with a strong selective advantage of the gene-modified cells, a preparatory “conditioning” by cytoreductive treatment may be required to promote engraftment.
Stable gene transfer, and therefore long-term genetic modification, is achieved by gene vectors, which integrate their genetic material and the therapeutic gene respectively into the chromatin of the target cells. Unlike classical pharmaceutical drug treatment, gene therapy is an approach highly specific to the patient and the disease. Parameters like cell source and origin, vector type, therapeutic dose, route of administration and, in particular, the transgene itself have to be adapted to each specific approach and medicinal purpose. For example, between 1989 and 2009 there were 1537 clinical gene therapy trials approved employing 35 different vector types (predominantly derived from Adenovirus, Retrovirus or naked DNA) in more than 8 different fields of medicine (predominantly cancer) (http://www.wiley.co.uk/genetherapy/clinical/). The consequence of the diversity of the products is a challenge for legal regulation, which should normally be universally valid while giving specific guidance to certain therapies in order to guarantee the safety and efficacy of the individual products.
While a gene therapy approach allows for the desired efficient long-term correction of a genetic defect on the one hand, it also brings up the concern of side effects on the other. The most noted example has been the clinical gene therapy trial for treatment of the rare genetic disorder X-linked severe combined immunodeficiency (X-SCID). While the majority of treated patients benefited from a life-saving and long-term immune reconstitution, the occurrence of lymphoproliferative disease due to insertional mutagenesis in 5 patients to date has gained notoriety [1, 2]. Integration site analysis revealed vector integrations close to cellular proto-oncogenes such as the LMO2 gene, known to be activated by chromosomal translocations in T-lymphoblastic leukemia [3, 4]. These severe adverse events made the theoretical concerns a reality. Additional concerns related to immunogenicity, spread of genetic sequences or toxic and infectious byproducts of vector preparations cause many gene therapy products to be classified as high-risk products that need to be strongly regulated by the authorities. This poses a tremendous challenge, since regulation can only be defined in general terms and an all-in-one document suitable for every purpose and individual need of a product cannot be established. To overcome this dilemma, case-by-case considerations are indicated.
Since researchers who invent the individual product initiate many clinical gene therapy trials, this review targets those investigators planning to enter the clinical development phase and initiating a clinical trial. It will clarify the complex situation and will give an overview of the current regulatory status as well as important points to consider before applying for a clinical trial authorization. This review involves preclinical and clinical issues as well as references to the necessary documents to be prepared.
Viral gene transfer and its associated risks
The regulatory framework should define uniform requirements in order to ensure compliance with quality standards and therefore guarantee the safety and well being of trial participants. In consideration of the major risks accompanied by viral gene transfer, it becomes clear that a thorough and complex regulatory framework is needed to control these biological products. As indicated above, the complexity of the individual product itself accounts for the necessity for evaluation of the risks and benefits of a certain gene therapy application on a case-by-case basis.
Integrating replication-defective vectors based on gamma-retroviruses have been frequently used in initial gene therapy protocols, and their risks will therefore be discussed as an example. Target cells are transduced in most cases ex vivo with the viral vector preparation. Shortly after entry of the retroviral particles, the viral RNA carrying the transgene of choice is reverse-transcribed into dsDNA, and a preintegration complex (PIC) is formed in which the DNA is associated with retroviral and cellular proteins (Figure 1). After translocation to the nucleus, the retroviral DNA including the transgene is stably integrated into the chromosomal DNA by the viral protein integrase.
Figure 1. The retroviral life cycle (reproduced with permission from the Journal Molecular Therapy (Nature Publishing Group); adapted from [5])
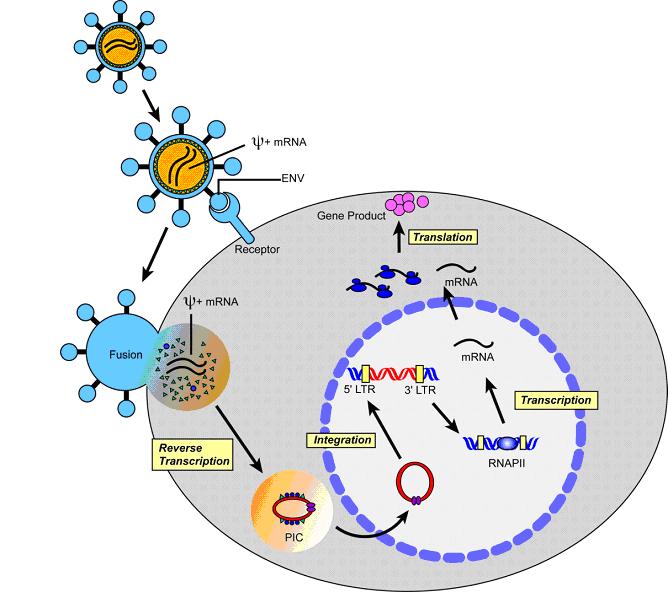
The integration of the transgene makes the desired correction of the genetic defect possible in the first place, not only in the transduced cell but also in its progeny. However, at the same time it forms the basis of one of the major safety concerns of integrating retroviral vectors: insertional mutagenesis. The process of integration is highly efficient but occurs in a semi-random manner with respect to the targeted genetic loci. Although gamma-retroviral integration tends to occur preferentially in open chromatin regions, which is associated with actively transcribed genes [6], it does not favor a specific target sequence. Therefore, insertion of the transgene in a non-predictable unspecific way may lead to activation, inactivation or truncation of cellular genes adjacent to the site of integration. Cellular proto-oncogenes might be placed under control of the viral enhancer/promoter elements resulting in a non-physiological expression of the respective gene with loss of cellular regulation. The tumorigenic risk associated with such an event appears to be highly context dependent. Available evidence suggests that additional mutations are required before cells transform to overt malignancy [7].
The concern of genotoxicity especially affects the first generation of retroviral-based gene transfer vectors in which the transgene is driven by the strong long terminal repeat (LTR) enhancer/promoter elements of the virus. New strategies in vector design with reduced potential for enhancer-mediated interaction with adjacent cellular genes may decrease the risk of genotoxicity, e.g., the use of self-inactivating (SIN) vectors [8], the incorporation of cellular promoters [9], the use of chromatin insulators [10], or the use of lentivirus-based vectors, which have a lower likelihood of integration in promoter-proximal or other regulatory gene regions [11]. In all circumstances, the genotoxic potential of a given vector designed for clinical use needs to be preclinically assessed and evaluated.
Another concern regarding the risk of oncogenesis is the formation of replication-competent retrovirus (RCR). Although retroviral vectors are replication-deficient due to the lack of the sequences encoding for the structural and enzymatic viral proteins, there is still the possibility of formation of RCR by recombination of the vector sequence with the so-called “helper” plasmids or with other, endogenous retroviral genetic information present in the producer or target cells [12]. As a consequence, unintended infection of target or even off-target cells might occur. This might introduce harmful viral pathogens into treated patients.
In order to assess the risk of RCR formation, investigators should evaluate the presence of homologous sequences suitable for recombination in the vector constructs, as well as the presence of endogenous viruses in the packaging cells. If possible, such sequences should be avoided or at least limited. Nevertheless, strict testing for the presence of RCR in retroviral vector batches intended for clinical application is required.
Another major concern of viral gene transfer is vertical germ line transmission. In general, gene therapy trials with the aim of direct germ line manipulation are prohibited [28]. Nevertheless, also in somatic gene therapy the concern of inadvertent germ line integration exists and gained new attention when semen of clinical trial participants for treatment of hemophilia tested positive for vector sequences [13, 14]. Although this does not necessarily imply that vector sequences were present in germ cells, this observation underlines the need for diligent biodistribution studies. The risk of germline transmission is in particular dependent on the biodistribution pattern of a given vector. In this regard, the route of administration, vector type and dose, and the innate and adapted immunity of the patient play pivotal roles. A replication deficient integrating vector used for ex vivo transduction of the target cell might have a much lower risk than the same vector applied systemically in an in vivo application. At the same time, a gamma-retroviral vector which can only transduce dividing cells might have a lower risk in transducing mature sperm cells than a lentiviral vector, which has the ability to also infect non-dividing cells. Still, spermatogonial stem cells that have a high proliferation activity might be accessible for gamma-retroviral vectors. Therefore, regulatory agencies have developed guidelines describing how to address the risk of inadvertent germ line transmission in preclinical studies (see below and Table 1).
Table 1. Applicable guidelines addressing GTMPs

Regulatory framework for Gene Therapy Medicinal Products
Currently, the regulatory situation for Gene Therapy Medicinal Products (GTMPs) is evolving rapidly on the European level. The new core regulation (EC) No 1394/2007 on Advanced Therapy Medicinal Products (ATMPs), which became effective in December 2008 (from here on referred to as ‘ATMP regulation’), lays the foundation for a harmonized regulatory situation applicable for all member states in the European Communion. According to Article 2 of this regulation, GTMPs together with Somatic Cell Therapy Medicinal Products and Tissue Engineered Products are classified as ATMPs (Figure 2). Until incorporation of this regulation, these products fell in a regulatory gap somewhere in between legislation 93/42/EEC on Medical Devices and Directive 2001/83/EC on Medicinal Products. The new ‘ATMP regulation’ fills this gap and "lays down specific rules concerning the authorization, supervision and pharmacovigilance of Advanced Therapy Medicinal Products” [50, Article 1].
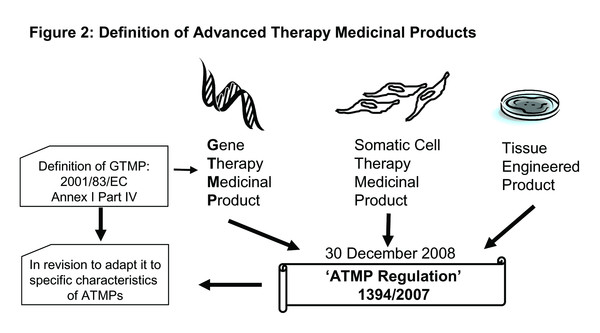
For the definition of a GTMP itself, the regulation refers to Annex I Part IV of Directive 2001/83/EC, as amended by Directive 2003/63/EC, which states: “For the purposes of this Annex, Gene Therapy Medicinal Product shall mean a product obtained through a set of manufacturing processes aimed at the transfer, to be performed either in vivo or ex vivo, of a prophylactic, diagnostic or therapeutic gene (i.e. a piece of nucleic acid), to human/animal cells and its subsequent expression in vivo.” Within the implementation of the ‘ATMP regulation’, this annex is currently under revision in order to adjust it to the specific characteristics of ATMPs (Figure 2). There is no draft version currently available, but the outcome of the public consultation paper as well as single contributions can be found on the webpage of the European Commission.
On the national German level, GTMPs are similarly defined as Medicinal Products in the Medicinal Products Act (“AMG”), Section 4 No. 9, [48]. Within the 15th amendment of the Medicinal Products Act, the new ATMP regulation will be implemented into national German law. Though a regulation, the translation into national law is necessary because the ‘ATMP regulation’ amends Directive 2001/83/EC.
GTMPs are often very complex products that may contain other components that are regulated by additional legislation. The GTMP may for instance contain human cells or tissues. Regarding the quality and safety for the donation, procurement and testing of these cells or tissues, Directive 2004/23/EC as implemented by Directive 2006/17/EC applies (Figure 3A). Directive 2004/23/EC is already transposed into national law by the German Tissue Act (“Gewebegesetz”). The processing, preservation, storage and distribution of these cells and tissues, however, fall under Section 14 of the ‘ATMP regulation’. When the GTMP also contains human blood or blood components, Directive 2002/98/EC as implemented by Directives 2004/33/EC, 2005/61/EC and 2005/62/EC applies (Figure 3B). On the German level, these aspects are addressed in the Medicinal Products Act and Transfusion Law.
In addition, the GTMP may be a combination product consistent of a Medicinal Product and Medical Device. This would, for instance, be the case if the gene-modified cells are applied to the patient via a specific biodelivery implant. Whether the regulatory rules and standards of Medicinal Products or of Medical Devices apply to combination products generally depends on their mode of action. Nevertheless, if ATMPs (and therefore GTMPs) are incorporated into a combination product, the ‘ATMP regulation’ applies regardless of the function of the Medical Device [50, Section 4]. However, the latter have to furthermore fulfill the quality and safety requirements of Directive 93/42/EEC (in case of a Medical Device) and accordingly Directive 90/385/EEC (in case of an active implantable Medical Device) as amended by Directive 2007/47/EC (Figure 3C). On the German level, both directives are implemented by the German Act on Medical Devices (“MPG”).
For clinical trials involving GTMPs, the overall requirements and ethical standards of the Clinical Trial Directive 2001/20/EC apply as well as for all other medicinal products (Figure 3D). In Germany, this directive is translated into national law by the GCP Ordinance (“GCP-Verordnung”). Furthermore, the German Medicinal Products Act applies, in particular concerning clinical trials in Chapter 6, together with the general considerations for clinical trials laid down in ICH E8 Step 5 [27]. Within the scope of the implementation of the ‘ATMP regulation’, the standards of good clinical practices shall be expanded to the specific needs of ATMPs [50, Article 4]. The adaption process is currently proceeding. A public consultation paper is already published on the European Commission webpage. The public consultation process has been closed so that a draft document on good clinical practice specific for ATMPs is expected to be published soon.
In Germany, the competent authority concerning clinical trial authorization related to GTMPs is the Paul-Ehrlich-Institute (PEI). General principles for requesting the authorization of a clinical trial in Germany are laid down in the third Notification of the joint announcement from PEI and the Federal Institute for Drugs and Medical Devices (BfArM) (third Notification).
In Germany there are some particularities for GTMPs compared to conventional medicinal products. While for example the ethics committee has to give an opinion within 60 days after a clinical trial application (multicentric trial) for conventional medicinal products, the time period extends up to 180 days if GTMPs are concerned [44, Section 8(4)]. Furthermore, the competent authority has to provide a written approval (explicit authorization) for clinical trials concerning GTMPs within 90 days after complete clinical trial application. This period may be extended to 180 days if the authority consults experts or professional opinions for decision-making [44, Section 9(4)].
The manufacture of GTMPs needs to be consistent with the requirements of Directive 2003/94/EC on Good Manufacturing Practice (“GMP“) (Figure 3E). Due to the complexity of ATMPs (and GTMPs) and the extensive manufacturing processes, the ‘ATMP regulation’ implicates an adaption of the guidelines for GMP to the specific situation of ATMPs [50, Article 5].
Figure 3. Regulatory framework for Gene Therapy Medicinal Products

Currently, a draft version of the adapted Eudralex Volume 4 Annex 2 on the manufacture of biological medicinal products is published. Furthermore, the European Pharmacopoeia serves as a legally binding framework for quality standards of medicinal products in Europe [43]. The General Chapter 5.14, which deals with GTMPs, gives instructions for the testing of batches of recombinant vectors and gene-modified cells. In Germany, good manufacturing practice is regulated in the ordinance for the manufacture of medicinal products and active pharmaceutical ingredients (AMWHV).
There are in addition various guidelines published addressing manufacturing and quality aspects during the development of ATMPs (Table 1). One is the multidisciplinary “Guideline on human Cell-Based Medicinal Products” of the European Medicines Agency (EMEA) [35], which gives advice for the “development, manufacturing and quality control as well as non-clinical and clinical development of Cell-Based Medicinal Products” which also include GTMPs. The guideline is aimed at products already in the phase of marketing authorization but the general considerations also apply for clinical trials. The EMEA “Note for guidance on the quality, preclinical and clinical aspects of Gene Transfer Medicinal Products” [25] gives recommendations for producing data aiming at an application for marketing authorization. Affiliated is the “Concept paper on the development of a guideline on the quality, preclinical and clinical aspects of medicinal products containing genetically modified cells” by EMEA [40]. If the GTMP was generated with the help of lentiviral vectors, the EMEA “Guideline on development and manufacture of lentiviral vectors” gives advice regarding quality and safety of the vectors [24].
Importantly, the specific safety aspects related to GTMPs have to be considered and analyzed before the products can be used in the clinic. The EMEA “Guideline on the non-clinical studies required before first clinical use of Gene Therapy Medicinal Products” [38] specifies which studies are essential prior to the first application to humans. This includes but is not limited to non-clinical proof of concept studies, biodistribution studies, as well as studies on dose finding, germ line transmission, immunotoxicity and studies addressing the environmental risks/shedding. Specific recommendations for the later are defined in the EMEA “Guideline on scientific requirements for the environmental risk assessment of Gene Therapy Medicinal Products” [39]. This guideline states: "Generally the purpose of clinical trials are to study the adsorption, distribution, metabolism and excretion of one or more Investigational Medicinal Products with the object of ascertaining its (their) safety and/or efficacy ([28]; definition of a clinical trial). As such the evaluation of vector shedding is a requirement for a phase I study.” Data of clinical trials regarding environmental risks need to be collected and integrated in a full environmental risk assessment (ERA) needed for a marketing authorization procedure. Other guidelines dealing with environmental risk assessments of genetically modified organisms are EMEA/BWP/473191/06-corr and EMEA/CHMP/BWP/135148/04.
Furthermore, in terms of studies addressing the risk and ethical concerns of inadvertent germline transmission, separate guidelines are available. The EMEA “Guideline on non-clinical testing for inadvertent germline transmission of gene transfer vectors” [34] recommends adjusted study designs depending on the type of vector used, as well as providing a decision tree regarding the necessary questions to be addressed by biodistribution and germ line transmission studies. Also a considerations paper of the International Conference On Harmonization Of Technical Requirements For Registration Of Pharmaceuticals For Human Use (ICH) is available on this topic and can be consulted in this regard (ICH considerations, general principles to address the risk of inadvertent germline integration of gene therapy vectors). The ICH S2B document “Note for guidance on genotoxicity” [26], however, gives recommendations for studies to address the risk of genotoxicity and can give advice in these questions.
If patients have been treated with a gene therapy approach in a clinical trial, clinical monitoring as well as intensive follow-up care should be performed in order to detect adverse events at an early stage to avoid clinical implications and to collect safety data. The “Guideline on follow-up of patients administered with Gene Therapy Medicinal Products” [41] gives recommendations in this regard.
Regulation (EC) No 726/2004 already regulates the marketing authorization procedure of biotechnology medicinal products on the European level. In this context, the products pass through a centralized authorization procedure at the EMEA in order to assess their quality, safety and efficacy. The technical requirements needed to prove the latter are defined in Annex I to Directive 2001/83/EC.
Nevertheless, the complexity and variety of ATMPs may result in a situation of very specific and individual questions to be addressed. Within the scope of the ‘ATMP regulation’, the Committee for Advanced Therapies (CAT) will be established within the EMEA in order to provide strong expertise in this field and exhibit draft opinions on ATMP applications presented to EMEA [50, Chapter 7]. Therefore, Regulation (EC) No 726/2004 needs to be amended. Currently, the CAT is in the process of establishment within the EMEA. Updated details can be found on the respective webpage of EMEA. Within the context of a marketing authorization, the standards for pharmacovigilance described in Regulation 726/2004 apply. Since clinical trials are typically powered for efficacy and furthermore the duration of the respective trials might not allow the detection of long term adverse events, the application has to provide a plan to ensure the follow-up of adverse reactions after marketing authorization. A specific EMEA guideline giving further recommendations on “Safety and Efficacy Follow-Up – Risk management of Advanced Therapy Medicinal Products” is already published [33]. Another measure of safety is the full traceability of the product (including the starting materials) and the treated patient. According to the ‘ATMP regulation’, the marketing authorization holder for an ATMP is responsible for setting up a traceability system [50, Article 15]. If human tissues or cells are involved, the traceability standards defined in Directive 2004/23/EC also apply, as do the requirements of Directive 2002/98/EC concerning human blood and blood components, respectively.
Finally, it should be noted that both the European agency EMEA and the German agency PEI (in charge of ATMPs) provide scientific advice. Investigators are welcome to consult the agencies in all phases of project development in order to obtain important project-specific advice, e.g., before applying for a clinical trial or marketing authorization. Details can be found on the webpages of EMEA or PEI, respectively.
Outlook
Application of new technologies of gene therapy to the treatment of diseases will yield the greatest benefits if approached on a sound scientific and medical basis. Regulatory guidelines are the basis of (i) current scientific knowledge, (ii) scientific expertise in a given research area, and (iii) the result of a continuous interaction between researchers and regulatory experts. Gene therapy has entered the stage of clinical evaluation. As always at the frontier of bench to bedside research, patient safety must be the first and foremost consideration in human gene therapy before one enters the stage of extensive clinical trials to assess efficacy.
References
Index of scientific references
1. Hacein-Bey-Abina S, Garrigue A, Wang GP, et al. Insertional oncogenesis in 4 patients after retrovirus-mediated gene therapy of SCID-X1. J Clin Invest. 2008;118(9):3132-3142.
2. Howe SJ, Mansour MR, Schwarzwaelder K, et al. Insertional mutagenesis combined with acquired somatic mutations causes leukemogenesis following gene therapy of SCID-X1 patients. J Clin Invest. 2008;118(9):3143-50.
3. Boehm T, Foroni L, Kaneko Y, et al. The rhombotin family of cysteine-rich LIM-domain oncogenes: Distinct members are involved in T-cell translocations to human chromosomes 11p15 and 11p13. Proc. Natl. Acad. Sci. 1991;88:4367–4371.
4. Royer-Pokora B, Loos U, and Ludwig WD. TTG-2, a new gene encoding a cysteine-rich protein with the LIM motif, is overexpressed in acute T-cell leukemia with the t(11;14)(p13;q11). Oncogene. 1991;6:1887–1893.
5. Baum C, Schambach A, Bohne J, and Galla M. Retrovirus Vectors: Toward the Plentivirus? Mol Ther. 2006;13:1050-1063.
6. Wu X, Li Y, Crise B, and Burgess SM. Transcription start regions in the human genome are favored targets for MLV integration. Science. 2003;300(5626):1749-1751.
7. Mullighan CG, Goorha S, Radtke I, et al. Genome-wide analysis of genetic alterations in acute lymphoblastic leukaemia. Nature. 2007;446:758-764.
8. Modlich U, Bohne J, Schmidt M, et al. Cell-culture assays reveal the importance of retroviral vector design for insertional genotoxicity. Blood. 2006;108:2545-2553.
9. Zychlinski D, Schambach A, Modlich U, et al. Physiological Promoters Reduce the Genotoxic Risk of Integrating Gene Vectors. Mol Ther. 2008;16(4):718-725.
10. Emery DW, Yannaki E, Tubb J, et al. Development of virus vectors for gene therapy of beta chain hemoglobinopathies: flanking with a chromatin insulator reduces gamma-globin gene silencing in vivo. Blood. 2002;100:2012-2019.
11. De Palma M, Montini E, Santoni de Sio FR, et al. Promoter trapping reveals significant differences in integration site selection between MLV and HIV vectors in primary hematopoietic cells. Blood.2005;105(6):2307-15.
12. Chong H, Starkey W, and Vile RG. A replication-competent retrovirus arising from a split-function packaging cell line was generated by recombination events between the vector, one of the packaging constructs, and endogenous retroviral sequences. J Virol.1998;72:2663–2670.
13. Marshall E. Gene therapy. Viral vectors still pack surprises. Science. 2001;294(5547):1640.
14. Manno CS, Pierce GF, Arruda VR, et al. Successful transduction of liver in hemophilia by AAV-Factor IX and limitations imposed by the host immune response. Nat Med. 2006;12(3):342-7.
Index of regulatory references
15. 3. Notification (“3. Bekanntmachung”) of the Federal Institute for Drugs and Medical Devices and the Paul Ehrlich Institute of 10 August 2006 on the clinical trial of medicinal products for human use.
16. Commission Directive 2003/63/EC of 25 June 2003 amending Directive 2001/83/EC of the European Parliament and of the Council on the Community code relating to medicinal products for human use. OJ L 159, 27.06.2006, p.46.
17. Commission Directive 2003/94/EC of 8 October 2003 laying down the principles and guidelines of good manufacturing practice in respect of medicinal products for human use and investigational medicinal products for human use.OJ L 262, 14.10.2003, p.22.
18. Commission Directive 2004/33/EC of 22 March 2004 implementing Directive 2002/98/EC of the European Parliament and of the Council as regards certain technical requirements for blood and blood components. OJ L 91, 30.03.2004, p.25.
19. Commission Directive 2005/61/EC of 30 September 2005 implementing Directive 2002/98/EC of the European Parliament and of the Council as regards traceability requirements and notification of serious adverse reactions and events. OJ L 256, 01.10.2005, p.32.
20. Commission Directive 2005/62/EC of 30 September 2005 implementing Directive 2002/98/EC of the European Parliament and of the Council as regards Community standards and specifications relating to a quality system for blood establishments. OJ L 256, 01.10.2005, p.41.
21. Commission Directive 2006/17/EC of 8 February 2006 implementing Directive 2004/23/EC of the European Parliament and of the Council as regards certain technical requirements for the donation, procurement and testing of human tissues and cells. OJ L 38, 09.02.2006, p.40.
22. Council Directive 90/385/EEC of 20 June 1990 on the approximation of the laws of the Member States relating to active implantable medical devices. OJ L 189, 20.07.1990, p.17
23. Council Directive 93/42/EEC of 14 June 1993 concerning medical devices. OJ L 169, 12.07.1993, p.1.
24. CHMP/BWP/2458/03 of the Committee for Medicinal Products for Human Use (CHMP) of 26 May 2005. Guideline on development and manufacture of lentiviral vectors.
25. CPMP/BWP/3088/99 of the Committee for Proprietary Medicinal Products (CPMP) of 24 April 2001. Note for Guidance on the quality, preclinical and clinical aspects of gene transfer medicinal products.
26. CPMP/ICH/174/95 ICH Topic S 2 B of March 1998. Genotoxicity: A standard battery for genotoxicity testing of pharmaceuticals, Step 5. Note for guidance on genotoxicity: A standard battery for genotoxicity testing of pharmaceuticals.
27. CPMP/ICH/291/95 ICH Topic E 8 of March 1998. General considerations for clinical trials, step 5. Note for guidance on general considerations for clinical trials.
28. Directive 2001/20/EC of the European Parliament and of the Council of 4 April 2001 on the approximation of the laws, regulations and administrative provisions of the member states relating to the implementation of good clinical practice in the conduct of clinical trials on medicinal products for human use. OJ L 121, 1.5.2001, p.34.
29. Directive 2001/83/EC of the European Parliament and of the Council of 6 November 2001 on the Community code relating to medicinal products for human use. OJ L 311, 28.11.2001, p.67.
30. Directive 2002/98/EC of the European Parliament and of the Council of 27 January 2003 setting standards of quality and safety for the collection, testing, processing, storage and distribution of human blood and blood componentsand amending Directive 2001/83/EC. OJ L 33, 08.02.2003, p.30.
31. Directive 2004/23/EC of the European Parliament and of the Council of 31 March 2004 on setting standards of quality and safety for the donation, procurement, testing, processing, preservation, storage and distribution of human tissues and cells. OJ L 102, 07.04.2004, p.48.
32. Directive 2007/47/EC of the European Parliament and of the Council of 5 September 2007 amending Council Directive 90/385/EEC on the approximation of the laws of the Member States relating to active implantable medical devices, Council Directive 93/42/EEC concerning medical devices and Directive 98/8/EC concerning the placing of biocidal products on the market.
33. EMEA/149995/08 of the Committee for Medicinal Products for Human Use (CHMP) of 20 November 2008. Guideline on safety and efficacy follow-up – risk management of advanced therapy medicinal products.
34. EMEA/273974/05 of the Committee for Medicinal Products for Human Use (CHMP) of 16 November 2006. Guideline on non-clinical testing for inadvertent germline transmission of gene transfer vectors.
35. EMEA/CHMP/410869/06 of the Committee for Medicinal Products for Human Use (CHMP) of 21 May 2008. Guideline on human cell-based medicinal products.
36. EMEA/CHMP/BWP/135148/04 of the Committee for Medicinal Products for Human Use (CHMP) of 20 January 2005. Environmental risk assessments for medicinal products containing, or consisting of, genetically modified organisms (GMOs) (Module 1.6.2).
37. EMEA/CHMP/BWP/473191/06 - Corr of the Committee for Medicinal Products for Human Use (CHMP) of 11 December 2006. Guideline on environmental risk assessments for medicinal products consisting of, or containing, genetically modified organisms (GMOs).
38. EMEA/CHMP/GTWP/125459/06 of the Committee for Medicinal Products for Human Use (CHMP) of 30 May 2008. Guideline on the non-clinical studies required before first clinical use of gene therapy medicinal products.
39. EMEA/CHMP/GTWP/125491/06 of the Committee for Medicinal Products for Human Use (CHMP) of 30 May 2008. Guideline on scientific requirements for the environmental risk assessment of gene therapy medicinal products.
40. EMEA/CHMP/GTWP/405681/06 of the Committee for Medicinal Products for Human Use (CHMP) of 24 May 2007. Concept paper on the development of a guideline on the quality, preclinical and clinical aspects of medicinal products containing genetically modified cells.
41. EMEA/CHMP/GTWP/60436/07 of the Committee for Medicinal Products for Human Use (CHMP) of 30 May 2008. Draft guideline on follow-up of patients administered with gene therapy medicinal products.
42. Eudralex Volume 4. Good manufacturing practice guidelines. Volume 4 of “The rules governing medicinal products in the European Union”. http://ec.europa.eu/enterprise/pharmaceuticals/eudralex/vol4_en.htm
43. European Pharacopoeia. http://www.pheur.org
44. GCP Ordinance (“GCP-Verordnung“). Of the German Federal Ministry for Health and Social Security of 09 August 2004 for good clinical practice in the conduct of clinical trials on medicinal products for human use. Federal Law Gazette I, 12.08.2004, p.2081.
45. German Act on Medical Devices (“Medizinproduktegesetz”) of the Federal Republic of Germany of 02.08.1994 in the version of the notification of the Law of 07.08. 2002. Federal Law Gazette I p.3146.
46. German Tissue Act (“Gewebegesetz“) of the German Federal Parliament of 20 July 2007 on the quality and safety of human tissues and cells. Federal Law Gazette I, 27.07.2007, p.1574.
47. ICH Considerations of the International Conference On Harmonisation Of Technical Requirements For Registration Of Pharmaceuticals For Human Use of 25 October 2006. General principles to address the risk of inadvertent germline integration of gene therapy vectors.
48. Medicinal Products Act (“Arzneimittelgesetz”) of the Federal Republic of Germany of 24.08.1976 in the version of the notification of the Law of 12th December 2005. Federal Law Gazette I p.3394.
49. Ordinance for the manufacture of medicinal products and active pharmaceutical ingredients (“AMWHV”) of the German Federal Ministries for Health and Food, Agriculture and Consumer Protection of 03 November 2006. Federal Law Gazette I, 09.11.2006, p.2523.
50. Regulation (EC) No 1394/2007 of the European Parliament and of the Council of 13 November 2007 on advanced therapy medicinal products and amending Directive 2001/83/EC and Regulation (EC) No 726/2004. OJ L 324, 10.12.2007, p.121.
51. Regulation (EC) No 726/2004 of the European Parliament and of the Council of 31 March 2004 laying down Community procedures for the authorisation and supervision of medicinal products for human and veterinary use and establishing a European Medicines Agency. OJ L 136, 30.04.2004, p.1.
52. Transfusion Law (“Transfusionsgesetz”) of the Federal Republic of Germany of 01.07.1998 in the version of the notification of the Law of 28.08.2007. Federal Law Gazette I p.2169.
Accepted 30 March 2009
Published 14 May 2009


