Introduction
Allogeneic hematopoietic stem cell transplantation (alloHSCT) is an effective treatment for a number of hematologic malignancies and non-malignant disorders, but it is associated with significant non-relapse mortality (NRM). Recently, a number of studies emphasized the role of endothelial dysfunction in such life-threatening complications of alloHSCT as graft-versus-host disease (GVHD) and veno-occlussive disease (VOD). The concept of endothelial injury in alloHSCT is not new, in 1996 Testa S et al., reported association between level of thrombomodulin, an endothelial damage marker, and GVHD, VOD and septicemia [30]. Since then the role of endothelium in acute alloHSCT complications were predicted to be more complex. On the one hand, neovascularization of bone marrow, skin and gastrointestinal tract is presiding event to acute GVHD, and it is associated with increased level of vascular endothelial growth factor (VEGF) [13,17,21]. On the other hand, endothelium is damaged by conditioning and calcineurin inhibitors, which leads to increased incidence of microvascular complications, infections and non-relapse mortality [8]. Also it was proposed that not the overwhelming T-cell alloreactive cytotoxicity, but severe endothelial dysfunction is responsible for steroid-refractory form of acute GVHD [14]. These multiple roles of endothelium in complications of alloHSCT make endothelial damage markers an attractive tool to predict prognosis.
Furthermore, neovasculogenesis and its key regulator VEGF were found to play an important role in pathogenesis of hematologic malignancies. VEGF A expression was associated with altered morphology and increased vascularization of the bone marrow in myeloproliferative disorders [2,10]. Also it was demonstrated that increased level of VEGF A is associated with worse outcome of chemotherapy in patients with acute myeloid leukemia [1], chronic myeloid leukemia [34], acute lymphoblastic leukemia [5], myelodysplastic syndrome [33] and different types of lymphoproliferation [6, 11, 25]. Apart from VEGF, level of circulating endothelial cells (CEC) was also found to predict prognosis in patients treated with chemotherapy for acute myeloid leukemia [35]. The significance of this negative prognostic factor was not established in recipients of alloHSCT.
A number of endothelial damage was studied in alloHSCT patients. The principal groups are adhesion molecules (ICAM, VCAM etc.), VEGF, CEC, von Willebrand factor, thrombomodulin and anti-coagulants, which are rapidly depleted in cases of extensive endothelial injury (protein C, antithrombin III etc) [8]. Among all these markers for the present study we selected VEGF A and CECs, because they are increased both in situation of endothelial injury and tumor-associated neovasculogenesis, and thus, may have a prognostic significance for both early complications after alloHSCT and relapse of the underlying hematologic malignancy.
Previously, we have reported a predictive value of VEGF A for early non-relapse mortality and relapses after alloHSCT [20] and a diagnostic significance of CEC level for VOD [19].
In the present study we evaluated predictive significance of VEGF and CECs for short- and long-term outcomes of alloHSCT and association between these two endothelial damage markers.
Patients and methods
Patients
The study was based on the blood samples and hospital records of 91 consecutive adult patients with hematologic malignancies undergoing HSCT in R.M. Gorbacheva Memorial Institute of Children Hematology and Transplantation. Samples for the study were collected prospectively between 2010 and 2012. The study was approved by the Ethical Committee of I.P. Pavlov State Medical University and informed consent was received from all patients for blood collection.
73% of patients had acute leukemia, 10% chronic myeloid leukemia, 8% myelodysplastic syndrome and 9% other hematologic malignancies. Median age was 38 years (range 18-60), median performance score and modified EBMT risk score [12, 29] 2 and 8 mg/kg busulfan or 140 mg/m2 melphalan in case of previous busulfan-based conditioning or anamnesis of neurological disorders. Acute GVHD prophylaxis consisted of calcineurin inhibitor (tacrolimus in 81% of patients) and short-course methotrexate. Antilymphocyte globulin (Atgam, Pfizer, NY, USA) 60 mg/kg was used for unrelated grafts. All but two patients received single allogeneic graft. Ten patients had previous autologous transplantation. Detailed patient characteristics are given in table 1. VOD prophylaxis with fixed-dose heparin was performed in all patients.
The staging and grading of acute GVHD were performed using the modified Glucksberg consensus criteria [24] and occurred at the time of initiation of treatment. VOD was diagnosed clinically according to the modified Seattle criteria extended until day +30 after HSCT, which required the presence of at least two of the following three clinical findings: jaundice with bilirubin>34 µmol/l, painful hepatomegaly and fluid retention >5% of the body weight. VOD was classified as severe in presence of multi-organ failure.
Laboratory methods
Venous blood was collected using EDTA anticoagulant from the central venous catheter before the start of conditioning, on the day of SCT (day 0) before graft transfusion, on the day of engraftment and additionally on the day of VOD diagnosis.
For VEGF A analysis, the blood samples were centrifuged for 15 minutes at 1000 g and the plasma aliquots were stored in polypropylene tubes at -80ºC until the day of the assay. Measurement of VEGF A concentrations in plasma samples was performed by enzyme-linked immunosorbent assays (ELISA) using commercially available kits (eBioscience, CA, USA) according to the instructions of the manufacturer. The detection limit was 7.9 to 1000 pg/ml. Concentrations were determined without knowledge of clinical data.
Measurement of CEC was performed within 2 hours from the blood collection. Peripheral blood samples were processed by lysing buffer (BD Pharm Lyse, BD Biosciences). Cell-surface triple staining was performed with fluorochrome-labeled monoclonal anti-human mouse antibodies incubated for 20 minutes at room temperature. The following antibody combination was used: CD31-FITC, CD146-PE, and CD45-PerCP (Becton Dickinson, San Jose, CA,USA). Data acquisition and analysis were performed by using BD FACSAria II flow cytometer and BD FACSDiva software (Becton Dickinson). For CECs measurement at least 1 million events was acquired. To exclude platelets, dead cells, and microparticles, the FSC/SSC plot was used. CECs were identified as CD45-negative CD31-bright positive CD146-bright positive (CD45-/CD31bright/ CD146bright) [16].
Statistical analysis
Experimental and clinical data were analyzed using SPSS Version 17.0. Chi-square and Wilcoxon criteria were used for univariate non-parametric analysis. Kruskal-Wallis test was used to determine the effect of pre-transplant therapy on the level of endothelial damage markers before conditioning. Kaplan–Meier survival analysis and Log Rank test were used for univariate survival, transplant-related mortality and cumulative incidence of relapse comparisons. Multivariate analysis was performed using Cox regression. Multivariate models were built with the use of stepwise forward selection, using a p-value ≤0.01 to include variables in the model. Proportional-hazards assumption was tested for each variable individually, all variables met this assumption. Separate models were created for assessment of CEC predictive value, since they were measured only in 55 consecutive patients. Cut-off levels of VEGF for survival analysis were determined based on ROC curves. Results of VEGF measurement at different time points were selected for Kaplan–Meier analysis and Cox regression if ROC area under the curve (AUC) for this time point was ≥0.5, and the time point with the highest value was selected.
Laboratory samples were collected within 30 days after transplantation and then patients were followed-up for survival and relapse. Median follow-up was 895 days (range 135-1364). NRM was defined as the cumulative incidence of death from the date of transplant not related to the relapse and its subsequent treatment. Even-free survival (EFS) was defined as the time from the date of transplantation to the documented event (relapse or death).
Results
Clinical outcomes
Engraftment was achieved in 90% of patients, 10% had either primary graft failure and/or progressive disease. Three-year overall survival (OS), EFS and NRM in the whole group were 44%, 35% and 34% respectively. Three -year cumulative incidence of relapse was 31%. VOD was diagnosed in 14% (n=13) of patients, severe VOD- in 10%. Median day of VOD diagnosis was 13 (range 6-21). Acute GVHD grade 1-4 was diagnosed in 54.4% of patients, grade 3-4 GVHD in 20.9%.
Selection of the optimal time points and cut-offs
The ROC curve analysis was performed to determine the time points of alloHSCT with highest predictive value for NRM and RR. The analysis separated early events (within 1 year after alloHSCT) and late events (after 1 year). The analysis for late relapses was not performed since there was only single such event in the study group. The results for VEGF A and CEC are presented in table 1.
|
Time point |
Before |
Day 0 |
Upon |
|
VEGF A |
|||
|
1-year relapse incidence |
0.62 |
0.53 |
0.50 |
|
1-year non-relapse mortality |
0.46 |
0.67 |
0.57 |
|
Relapse incidence after one year |
n.a |
n.a |
n.a |
|
Non-relapse mortality after one year |
0.40 |
0.36 |
0.46 |
|
Circulating endothelial cells |
|||
|
1-year relapse incidence |
0.55 |
0.62 |
0.62 |
|
1-year non-relapse mortality |
0.66 |
0.50 |
0.54 |
|
Relapse incidence after one year |
n.a |
n.a |
n.a |
|
Non-relapse mortality after one year |
0.54 |
0.35 |
0.00 |
n.a.= not applicable
Table 1. ROC areas under the curves for predictive value of VEGF A and CECs
VEGF A before conditioning was found to have the highest predictive value for 1-year relapse (AUC=0.62). The ROC determined cut-off for relapse was 37 pg/ml. An additional analysis was performed to exclude the effect of pre-transplant chemotherapy on the level of VEGF A before conditioning. Neither time from diagnosis to HSCT (p=0.83), number of previous chemotherapy courses (p=0.12), number of high-dose chemotherapy courses (p=0.82), previous HSCT (p=0.11) or time from the last chemotherapy course (p=0.28) significantly effected the level of VEGF A.
Early NRM was best predicted by VEGF A level after conditioning (AUC=0.67). The determined cut-off value was the limit of quantification (<7.8 pg/ml). On the contrary, late NRM was not predicted by VEGF A concentrations with AUC<0.5 at all time points.
For CECs, early relapse was best predicted by level after conditioning ( AUC=0.62) with a cut-off 87 cells/ml. Level of CECs before conditioning was both predictive for 1-year (AUC=0.66) and late NRM (AUC=0.54) with a cut-off value of 38 cells/ml. As with VEGF time from diagnosis to HSCT (p=0.34), number of previous chemotherapy courses (p=0.40), number of high-dose chemotherapy courses (p=0.58) or time from the last chemotherapy course (p=0.25) were not significantly effecting the pre-transplant level of CECs.
As based on these results, we selected pre-transplant VEGF A level and day 0 CEC level to be tested in Kaplan–Meier survival analysis of relapse incidence, and day 0 VEGF along with pre-transplant CEC levels for NRM analysis.
Predictive value of VEGF for
relapse and non-relapse mortality
Patients with pre-conditioning level of VEGF A >37 pg/ml had significantly higher 1-year relapse incidence (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40, figure 1). Also patients VEGF A after conditioning <7.8 pg/ml demonstrated a trend to lower non-relapse mortality (17% vs 35%, p=0.10, Fig. 1). In a multivariate analysis VEGF A >37 pg/ml was a significant factor associated with relapse (HR 3.15, 95%CI 1.34-7.40, p=0.009, table 2). Moreover, when corrected for confounding factors in multivariate regression VEGF A after conditioning <7.8 pg/ml was a significant predictor of NRM (HR 0.15, 95%CI 0.03-0.69, p=0.015, table 2). Surprisingly, 3-year overall survival (OS) was not different in patients with high and low VEGF concentrations (50% vs 42% respectively, p=0.60), as majority of patients in high VEGF group responded to salvage therapy after relapse.


Figure 1. 1-year relapse incidence and non-relapse mortality according to VEGF level
|
Factor |
Multivariate, p-value |
HR |
HR 95% CI |
|
1-year cumulative relapse rate |
|||
|
Unrelated vs related donor |
0.232 |
||
|
Active disease at the time of HSCT |
0.002 |
4.05 |
1.68-9.79 |
|
MAC vs RIC conditioning |
0.461 |
||
|
Acute GVHD, grade 1-4 |
0.002 |
0.26 |
0.11-0.61 |
|
Chronic GVHD |
0.003 |
0.19 |
0.06-0.55 |
|
VEGF A before conditioning > 37 pg/ml |
0.009 |
3.15 |
1.34-7.40 |
|
1-year non-relapse mortality |
|||
|
Active disease at the time of HSCT |
0.027 |
4.67 |
1.19-18.30 |
|
Age |
0.70 |
||
|
Unrelated vs related donor |
0.022 |
6.64 |
1.32-33.40 |
|
MAC vs RIC conditioning |
0.32 |
||
|
Acute GVHD, grade 3-4 |
0.024 |
4.87 |
1.24-19.14 |
|
VEGF A on day 0 < 7.8 pg/ml |
0.015 |
0.15 |
0.03-0.69 |
Table 2. Multivariate analysis of relapse incidence and non-relapse mortality (whole group)
Predictive value of CECs for
relapse and non-relapse mortality
Univariate analysis with previously determined cut-off value showed patients with CEC level after conditioning >87 cells/ml had higher relapse incidence (60% vs 21%, p<0.001), but in multivariate analysis it was not a significant factor (p=0.09, table 3). So CECs was not an independent predictive marker of relapse, but rather demonstration the increased endothelial damage in patients with high-risk disease. This was confirmed by the fact that level >87 cells/ml was significantly more often observed in patients with active disease at the time of the alloHSCT (80% vs 20%, p=0.032).
Univariate analysis of NRM confirmed that patients with pre-conditioning level of CECs >71 had increased risk of transplant-related death during the first year (69% vs 20%, p=0.001), while the incidence of late NRM was not significantly different (0% vs 5%, p=0.70). Nevertheless, in multivariate analysis the differences in 1-year NRM were also not significant (95%CI 0.84-5.76, p=0.102, table 3). Regarding results of multivariate analysis of CEC as the predictive marker, the statistical power of the models was relatively low due to small number of patients with CEC measured, so with a larger group of patients, the CECs as the covariate might reach the significant level.
|
Factor |
Multivariate, p-value |
HR |
HR 95% CI |
|
1-year cumulative relapse rate |
|||
|
Active disease at the time of HSCT |
0.82 |
||
|
MAC vs RIC conditioning |
0.148 |
||
|
Acute GVHD, grade 1-4 |
0.035 |
0.24 |
0.07-0.91 |
|
Chronic GVHD |
0.019 |
0.08 |
0.01-0.66 |
|
CEC after conditioning>87 cells/ml |
0.086 |
||
|
1-year non-relapse mortality |
|||
|
Active disease at the time of HSCT |
0.050 |
3.05 |
1.00-9.31 |
|
Acute GVHD, grade 3-4 |
0.040 |
2.98 |
1.05-8.45 |
|
CEC before conditioning>71 cells/ml |
0.102 |
||
Table 3. Multivariate analysis of relapse incidence and non-relapse mortality (only patients with measured level of CECs)
Association between level
of VEGF A and CECs
The interesting result of the analysis was that there was no correlation between pre-transplant level of CECs and VEGF (p=0.81), as well as for after conditioning (p=0.74) and engraftment levels (p=0.59). But when the cut-off levels of CEC (>71 cells/ml) and VEGF (<7.8 pg/ml) that predicted NRM were tested, in patients with high CEC level pre-conditioning VEGF was significantly more frequently elevated on day 0 (83% vs 51%, p=0.036).
Discussion
In this study we confirmed the prognostic significance of endothelial damage markers for non-relapse mortality. As expected, these markers allow to predict only early, but not late mortality. This is due to the fact that late NRM is mostly associated with chronic GVHD or infections related to impaired immune system [26]. The factors that influence development of chronic GVHD and immune reconstitution are mostly immunologic and are associated with patient-donor major or minor HLA-antigen disparity and trigger these events in the late post-transplant period [3, 24]. On the contrary, in an early post-transplant period endothelial dysfunction plays a role in a number of acute complications. In our study due to small number of patients it was impossible to establish relationship between endothelial damage and all of the complications, but as we previously reported elevation of VEGF and CEC levels was closely related to development of VOD [19, 20]. Likewise, a number of studies demonstrated association between endothelial damage and acute GVHD [14, 15, 18],
In this study we found out that VEGF is predictive for NRM after conditioning, while CEC – when measured before conditioning. So different endothelial damage markers may represent different aspects of endothelial damage and are elevated variable time after a damage occurs. This was confirmed in our study by absence of correlation between VEGF and CEC, and only more sophisticated methods revealed association between these two biomarkers. So VEGF A is secreted a large variety of cells, including endothelial and blood mononuclears. It is eliminated via cleavage with serum proteases and binding to either soluble or cellular VEGF receptors. But also a large proportion of VEGF is bound to extracellular matrix (ECM) heparin sulfate proteoglycans. In response to endothelial and tissue damage ECM-bound VEGF is cleaved from proteoglycan complex and released into circulation to facilitate reparation. What is important is that activity of serum proteases in terms of VEGF elimination is insufficient to decrease its level in situations of its extensive release from ECM. But its levels in plasma return to normal values very rapidly, within hours, if there are no continuous stimuli [9, 28, 32]. Hence, VEGF A level in plasma represent the acute phase of endothelial damage, that is why the time-point post-conditioning is of highest predictive value. CEC levels, on the other hand, represent chronic endothelial damage and are present in circulation for a longer period of time than VEGF. That is why it is a valuable tool to predict complications in diabetes and cardiovascular disorders [3, 7]. Marginally significant predictive value of CEC in multivariate analysis may not indicate that this is less valuable prognostic marker, but may be a result of a smaller number of patients in whom it as measured. In summary, different endothelial damage markers complement each other and in further clinical research should be used in combination.
Another aspect of our study was a dual role of VEGF. Besides its role as endothelial damage biomarker, it is also a disease risk factor in hematologic malignancies [1, 5, 6, 11, 33, 34]. We have demonstrated that it is also a factor of adverse disease prognosis in HSCT, but it is important that there were no differences in OS respective to pre-transplant VEGF level. Successful salvage post-transplant chemotherapy and donor lymphocyte infusions, at least in some patients from the high-VEGF A group, demonstrates a potential utility of graft-versus-leukemia effect to overcome this factor of resistance. Allogeneic HSCT is considered a treatment of choice for high-risk disease in patients with acute leukemias, myelodysplastic syndrome, chronic myeloid leukemia and lymphomas [23, 36]. As standard therapy outcome for these malignancies was reported to be negatively influenced by VEGF A overexpression, further studies are required to determine whether patients with high level of this factor should be candidates for HSCT. Due to very low incidence of late relapses in the study group we failed to demonstrate if there was any influence of VEGF expression on late disease recurrence, so larger studies are required to test this, but given very high incidence of early relapses in our study in the high VEGF group, early post-transplant therapy should be considered for these patients.
Recently, a number of clinical scoring systems were validated to predict risk of alloHSCT, like EBMT risk score [12, 29] or Seattle PAM score [27]. The results of this study show that the endothelial damage markers are of distinct predictive value, irrelevant of clinical parameters. Therefore, further studies are required to evaluate if they could be incorporated into the risk assessment models. In conclusion, peripheral CECs and plasma VEGF levels represent a useful prognostic tool to predict the risk of alloHSCT and disease relapse.
Conflict of interests
No conflict interest is reported.
References
- Aguayo A, Estey E, Kantarjian H et al. Cellular vascular endothelial growth factor is a predictor of outcome in patients with acute myeloid leukemia. Blood 1999; 94(11): 3717-21.
- Aguayo A, Kantarjian H, Manshouri T et al. Angiogenesis in acute and chronic leukemias and myelodysplastic syndromes. Blood 2000; 96(6): 2240-5.
- Allen JL, Fore MS, Wooten J et al. B cells from patients with chronic GVHD are activated and primed for survival via BAFF-mediated pathways. Blood 2012; 120(12): 2529-36.
- Asicioglu E, Gogas Yavuz D, Koc M, Ozben B, Yazici D, Deyneli O, Akalin S. Circulating endothelial cells are elevated in patients with type 1 diabetes mellitus. Eur J Endocrinol 2010; 162(4): 711-7.
- Avramis IA, Panosyan EH, Dorey F, Holcenberg JS, Avramis VI. Children’s Oncology Group. Correlation between high vascular endothelial growth factor-A serum levels and treatment outcome in patients with standard-risk acute lymphoblastic leukemia: a report from Children’s Oncology Group Study CCG-1962. Clin Cancer Res 2006; 12(23): 6978-84.
- Ben Arush MW, Ben Barak A, Maurice S, Livne E. Serum VEGF as a significant marker of treatment response in Hodgkin lymphoma. Pediatr Hematol Oncol 2007; 24(2): 111-5.
- Boos CJ, Balakrishnan B, Blann AD, Lip GY. The relationship of circulating endothelial cells to plasma indices of endothelial damage/dysfunction and apoptosis in acute coronary syndromes: implications for prognosis. J Thromb Haemost 2008; 6(11): 1841-50.
- Carreras E, Diaz-Ricart M. The role of the endothelium in the short-term complications of hematopoietic SCT. Bone Marrow Transplant 2011; 46(12): 1495-502.
- Chen TT, Luque A, Lee S, Anderson SM, Segura T, Iruela-Arispe ML. Anchorage of VEGF to the extracellular matrix conveys differential signaling responses to endothelial cells. J Cell Biol 2010; 188(4): 595-609.
- de Bont ES, Rosati S, Jacobs S, Kamps WA, Vellenga E. Increased bone marrow vascularization in patients with acute myeloid leukaemia: a possible role for vascular endothelial growth factor. Br J Haematol 2001; 113(2) :296-304.
- Hatjiharissi E, Terpos E, Papaioannou M et al. The combination of intermediate doses of thalidomide and dexamethasone reduces bone marrow micro-vessel density but not serum levels of angiogenic cytokines in patients with refractory/relapsed multiple myeloma. Hematol Oncol 2004; 22(4): 159-68.
- Hemmati PG, Terwey TH, le Coutre P et al. A modified EBMT risk score predicts the outcome of patients with acute myeloid leukemia receiving allogeneic stem cell transplants. Eur J Haematol. 2011; 86(4): 305-16.
- Leonhardt F, Grundmann S, Behe M et al. Inflammatory neovascularization during graft-versus-host disease is regulated by αv integrin and miR-100. Blood. 2013; 121(17): 3307-18.
- Luft T, Dietrich S, Falk C et al. Steroid-refractory GVHD: T-cell attack within a vulnerable endothelial system. Blood 2011; 118(6): 1685-92.
- Lunn RA, Sumar N, Bansal AS, Treleaven J. Cytokine profiles in stem cell transplantation: possible use as a predictor of graft-versus-host disease. Hematology 2005; 10(2): 107-14.
- Mancuso P, Antoniotti P, Quarna J et al. Validation of a standardized method for enumerating circulating endothelial cells and progenitors: flow cytometry and molecular and ultrastructural analyses. Clin Cancer Res 2009;15(1): 267-73.
- Medinger M, Tichelli A, Bucher C et al. GVHD after allogeneic haematopoietic SCT for AML: angiogenesis, vascular endothelial growth factor and VEGF receptor expression in the BM. Bone Marrow Transplant. 2013; 48(5): 715-21.
- Min CK, Kim SY, Lee MJ et al. Vascular endothelial growth factor (VEGF) is associated with reduced severity of acute graft-versus-host disease and nonrelapse mortality after allogeneic stem cell transplantation. Bone Marrow Transplant 2006; 38(2): 149-56.
- Moiseev IS, Babenko EV, Sipol AA et al. Measurement of circulating endothelial cells to support the diagnosis of veno-occlusive disease after hematopoietic stem cell transplantation. Int J Lab Hematol. 2014; 36(4): e27-9.
- Moiseev IS, Lapin SV, Surkova EA et al. Level of vascular endothelial growth factor predicts both relapse and nonrelapse mortality after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant. 2013; 19(12): 1677-82.
- Norton J, Sloane JP, al-Saffar N et al. Vessel associated adhesion molecules in normal skin and acute graft-versus-host disease. J Clin Pathol. 1991; 44(7): 586-91.
- Page AV, Liles WC. Biomarkers of endothelial activation/dysfunction in infectious diseases. Virulence 2013; 4(6): 507-16.
- Phillips GL. Allogeneic hematopoietic stem cell transplantation (HSCT) for high-risk acute myeloid leukemia (AML)/myelodysplastic syndrome (MDS): how can we improve outcomes in the near future? Leuk Res. 2012; 36(12): 1490-5.
- Przepiorka D, Weisdorf D, Martin P et al. Consensus conference on acute GVHD grading. Bone Marrow Transplant 1995; 15(6): 825-828.
- Riihijärvi S, Nurmi H, Holte H et al. High serum vascular endothelial growth factor level is an adverse prognostic factor for high-risk diffuse large B-cell lymphoma patients treated with dose-dense chemoimmunotherapy. Eur J Haematol 2012; 89(5): 395-402.
- Schechter T, Pole JD, Darmawikarta D et al. Late mortality after hematopoietic SCT for a childhood malignancy. Bone Marrow Transplant. 2013; 48(10): 1291-5.
- Sorror ML, Storer BE, Maloney DG et al. Outcomes after allogeneic hematopoietic cell transplantation with nonmyeloablative or myeloablative conditioning regimens for treatment of lymphoma and chronic lymphocytic leukemia. Blood. 2008; 111(1): 446-52.
- Stefanini MO, Wu FT, Mac Gabhann F, Popel AS. A compartment model of VEGF distribution in blood, healthy and diseased tissues. BMC Syst Biol 2008; 2: 77.
- Terwey TH, Hemmati PG, Martus P et al. A modified EBMT risk score and the hematopoietic cell transplantation-specific comorbidity index for pre-transplant risk assessment in adult acute lymphoblastic leukemia. Haematologica. 2010; 95(5): 810-8.
- Testa S, Manna A, Porcellini A et al. Increased plasma level of vascular endothelial glycoprotein thrombomodulin as an early indicator of endothelial damage in bone marrow transplantation. Bone Marrow Transplant. 1996; 18(2): 383-8.
- Vassiliou AG, Mastora Z, Orfanos SE et al. Elevated biomarkers of endothelial dysfunction/activation at ICU admission are associated with sepsis development. Cytokine. 2014; 69(2): 240-7.
- Vempati P, Mac Gabhann F, Popel AS. Quantifying the proteolytic release of extracellular matrix-sequestered VEGF with a computational model. PLoS One 2010; 5(7): e11860.
- Verstovsek S, Estey E, Manshouri T et al. Clinical relevance of vascular endothelial growth factor receptors 1 and 2 in acute myeloid leukaemia and myelodysplastic syndrome. Br J Haematol 2002; 118(1): 151-6.
- Verstovsek S, Kantarjian H, Manshouri T et al. Prognostic significance of cellular vascular endothelial growth factor expression in chronic phase chronic myeloid leukemia. Blood 2002; 99(6): 2265-7.
- Wierzbowska A, Robak T, Krawczynska A et al. Kinetics and apoptotic profile of circulating endothelial cells as prognostic factors for induction treatment failure in newly diagnosed acute myeloid leukemia patients. Ann Hematol. 2008; 87(2): 97-106.
- Zikos P, Van Lint MT, Lamparelli T et al. Allogeneic hemopoietic stem cell transplantation for patients with high risk acute lymphoblastic leukemia: favorable impact of chronic graft-versus-host disease on survival and relapse. Haematologica. 1998; 83(10): 896-903.
Introduction
Allogeneic hematopoietic stem cell transplantation (alloHSCT) is an effective treatment for a number of hematologic malignancies and non-malignant disorders, but it is associated with significant non-relapse mortality (NRM). Recently, a number of studies emphasized the role of endothelial dysfunction in such life-threatening complications of alloHSCT as graft-versus-host disease (GVHD) and veno-occlussive disease (VOD). The concept of endothelial injury in alloHSCT is not new, in 1996 Testa S et al., reported association between level of thrombomodulin, an endothelial damage marker, and GVHD, VOD and septicemia [30]. Since then the role of endothelium in acute alloHSCT complications were predicted to be more complex. On the one hand, neovascularization of bone marrow, skin and gastrointestinal tract is presiding event to acute GVHD, and it is associated with increased level of vascular endothelial growth factor (VEGF) [13,17,21]. On the other hand, endothelium is damaged by conditioning and calcineurin inhibitors, which leads to increased incidence of microvascular complications, infections and non-relapse mortality [8]. Also it was proposed that not the overwhelming T-cell alloreactive cytotoxicity, but severe endothelial dysfunction is responsible for steroid-refractory form of acute GVHD [14]. These multiple roles of endothelium in complications of alloHSCT make endothelial damage markers an attractive tool to predict prognosis.
Furthermore, neovasculogenesis and its key regulator VEGF were found to play an important role in pathogenesis of hematologic malignancies. VEGF A expression was associated with altered morphology and increased vascularization of the bone marrow in myeloproliferative disorders [2,10]. Also it was demonstrated that increased level of VEGF A is associated with worse outcome of chemotherapy in patients with acute myeloid leukemia [1], chronic myeloid leukemia [34], acute lymphoblastic leukemia [5], myelodysplastic syndrome [33] and different types of lymphoproliferation [6, 11, 25]. Apart from VEGF, level of circulating endothelial cells (CEC) was also found to predict prognosis in patients treated with chemotherapy for acute myeloid leukemia [35]. The significance of this negative prognostic factor was not established in recipients of alloHSCT.
A number of endothelial damage was studied in alloHSCT patients. The principal groups are adhesion molecules (ICAM, VCAM etc.), VEGF, CEC, von Willebrand factor, thrombomodulin and anti-coagulants, which are rapidly depleted in cases of extensive endothelial injury (protein C, antithrombin III etc) [8]. Among all these markers for the present study we selected VEGF A and CECs, because they are increased both in situation of endothelial injury and tumor-associated neovasculogenesis, and thus, may have a prognostic significance for both early complications after alloHSCT and relapse of the underlying hematologic malignancy.
Previously, we have reported a predictive value of VEGF A for early non-relapse mortality and relapses after alloHSCT [20] and a diagnostic significance of CEC level for VOD [19].
In the present study we evaluated predictive significance of VEGF and CECs for short- and long-term outcomes of alloHSCT and association between these two endothelial damage markers.
Patients and methods
Patients
The study was based on the blood samples and hospital records of 91 consecutive adult patients with hematologic malignancies undergoing HSCT in R.M. Gorbacheva Memorial Institute of Children Hematology and Transplantation. Samples for the study were collected prospectively between 2010 and 2012. The study was approved by the Ethical Committee of I.P. Pavlov State Medical University and informed consent was received from all patients for blood collection.
73% of patients had acute leukemia, 10% chronic myeloid leukemia, 8% myelodysplastic syndrome and 9% other hematologic malignancies. Median age was 38 years (range 18-60), median performance score and modified EBMT risk score [12, 29] 2 and 8 mg/kg busulfan or 140 mg/m2 melphalan in case of previous busulfan-based conditioning or anamnesis of neurological disorders. Acute GVHD prophylaxis consisted of calcineurin inhibitor (tacrolimus in 81% of patients) and short-course methotrexate. Antilymphocyte globulin (Atgam, Pfizer, NY, USA) 60 mg/kg was used for unrelated grafts. All but two patients received single allogeneic graft. Ten patients had previous autologous transplantation. Detailed patient characteristics are given in table 1. VOD prophylaxis with fixed-dose heparin was performed in all patients.
The staging and grading of acute GVHD were performed using the modified Glucksberg consensus criteria [24] and occurred at the time of initiation of treatment. VOD was diagnosed clinically according to the modified Seattle criteria extended until day +30 after HSCT, which required the presence of at least two of the following three clinical findings: jaundice with bilirubin>34 µmol/l, painful hepatomegaly and fluid retention >5% of the body weight. VOD was classified as severe in presence of multi-organ failure.
Laboratory methods
Venous blood was collected using EDTA anticoagulant from the central venous catheter before the start of conditioning, on the day of SCT (day 0) before graft transfusion, on the day of engraftment and additionally on the day of VOD diagnosis.
For VEGF A analysis, the blood samples were centrifuged for 15 minutes at 1000 g and the plasma aliquots were stored in polypropylene tubes at -80ºC until the day of the assay. Measurement of VEGF A concentrations in plasma samples was performed by enzyme-linked immunosorbent assays (ELISA) using commercially available kits (eBioscience, CA, USA) according to the instructions of the manufacturer. The detection limit was 7.9 to 1000 pg/ml. Concentrations were determined without knowledge of clinical data.
Measurement of CEC was performed within 2 hours from the blood collection. Peripheral blood samples were processed by lysing buffer (BD Pharm Lyse, BD Biosciences). Cell-surface triple staining was performed with fluorochrome-labeled monoclonal anti-human mouse antibodies incubated for 20 minutes at room temperature. The following antibody combination was used: CD31-FITC, CD146-PE, and CD45-PerCP (Becton Dickinson, San Jose, CA,USA). Data acquisition and analysis were performed by using BD FACSAria II flow cytometer and BD FACSDiva software (Becton Dickinson). For CECs measurement at least 1 million events was acquired. To exclude platelets, dead cells, and microparticles, the FSC/SSC plot was used. CECs were identified as CD45-negative CD31-bright positive CD146-bright positive (CD45-/CD31bright/ CD146bright) [16].
Statistical analysis
Experimental and clinical data were analyzed using SPSS Version 17.0. Chi-square and Wilcoxon criteria were used for univariate non-parametric analysis. Kruskal-Wallis test was used to determine the effect of pre-transplant therapy on the level of endothelial damage markers before conditioning. Kaplan–Meier survival analysis and Log Rank test were used for univariate survival, transplant-related mortality and cumulative incidence of relapse comparisons. Multivariate analysis was performed using Cox regression. Multivariate models were built with the use of stepwise forward selection, using a p-value ≤0.01 to include variables in the model. Proportional-hazards assumption was tested for each variable individually, all variables met this assumption. Separate models were created for assessment of CEC predictive value, since they were measured only in 55 consecutive patients. Cut-off levels of VEGF for survival analysis were determined based on ROC curves. Results of VEGF measurement at different time points were selected for Kaplan–Meier analysis and Cox regression if ROC area under the curve (AUC) for this time point was ≥0.5, and the time point with the highest value was selected.
Laboratory samples were collected within 30 days after transplantation and then patients were followed-up for survival and relapse. Median follow-up was 895 days (range 135-1364). NRM was defined as the cumulative incidence of death from the date of transplant not related to the relapse and its subsequent treatment. Even-free survival (EFS) was defined as the time from the date of transplantation to the documented event (relapse or death).
Results
Clinical outcomes
Engraftment was achieved in 90% of patients, 10% had either primary graft failure and/or progressive disease. Three-year overall survival (OS), EFS and NRM in the whole group were 44%, 35% and 34% respectively. Three -year cumulative incidence of relapse was 31%. VOD was diagnosed in 14% (n=13) of patients, severe VOD- in 10%. Median day of VOD diagnosis was 13 (range 6-21). Acute GVHD grade 1-4 was diagnosed in 54.4% of patients, grade 3-4 GVHD in 20.9%.
Selection of the optimal time points and cut-offs
The ROC curve analysis was performed to determine the time points of alloHSCT with highest predictive value for NRM and RR. The analysis separated early events (within 1 year after alloHSCT) and late events (after 1 year). The analysis for late relapses was not performed since there was only single such event in the study group. The results for VEGF A and CEC are presented in table 1.
|
Time point |
Before |
Day 0 |
Upon |
|
VEGF A |
|||
|
1-year relapse incidence |
0.62 |
0.53 |
0.50 |
|
1-year non-relapse mortality |
0.46 |
0.67 |
0.57 |
|
Relapse incidence after one year |
n.a |
n.a |
n.a |
|
Non-relapse mortality after one year |
0.40 |
0.36 |
0.46 |
|
Circulating endothelial cells |
|||
|
1-year relapse incidence |
0.55 |
0.62 |
0.62 |
|
1-year non-relapse mortality |
0.66 |
0.50 |
0.54 |
|
Relapse incidence after one year |
n.a |
n.a |
n.a |
|
Non-relapse mortality after one year |
0.54 |
0.35 |
0.00 |
n.a.= not applicable
Table 1. ROC areas under the curves for predictive value of VEGF A and CECs
VEGF A before conditioning was found to have the highest predictive value for 1-year relapse (AUC=0.62). The ROC determined cut-off for relapse was 37 pg/ml. An additional analysis was performed to exclude the effect of pre-transplant chemotherapy on the level of VEGF A before conditioning. Neither time from diagnosis to HSCT (p=0.83), number of previous chemotherapy courses (p=0.12), number of high-dose chemotherapy courses (p=0.82), previous HSCT (p=0.11) or time from the last chemotherapy course (p=0.28) significantly effected the level of VEGF A.
Early NRM was best predicted by VEGF A level after conditioning (AUC=0.67). The determined cut-off value was the limit of quantification (<7.8 pg/ml). On the contrary, late NRM was not predicted by VEGF A concentrations with AUC<0.5 at all time points.
For CECs, early relapse was best predicted by level after conditioning ( AUC=0.62) with a cut-off 87 cells/ml. Level of CECs before conditioning was both predictive for 1-year (AUC=0.66) and late NRM (AUC=0.54) with a cut-off value of 38 cells/ml. As with VEGF time from diagnosis to HSCT (p=0.34), number of previous chemotherapy courses (p=0.40), number of high-dose chemotherapy courses (p=0.58) or time from the last chemotherapy course (p=0.25) were not significantly effecting the pre-transplant level of CECs.
As based on these results, we selected pre-transplant VEGF A level and day 0 CEC level to be tested in Kaplan–Meier survival analysis of relapse incidence, and day 0 VEGF along with pre-transplant CEC levels for NRM analysis.
Predictive value of VEGF for
relapse and non-relapse mortality
Patients with pre-conditioning level of VEGF A >37 pg/ml had significantly higher 1-year relapse incidence (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40, figure 1). Also patients VEGF A after conditioning <7.8 pg/ml demonstrated a trend to lower non-relapse mortality (17% vs 35%, p=0.10, Fig. 1). In a multivariate analysis VEGF A >37 pg/ml was a significant factor associated with relapse (HR 3.15, 95%CI 1.34-7.40, p=0.009, table 2). Moreover, when corrected for confounding factors in multivariate regression VEGF A after conditioning <7.8 pg/ml was a significant predictor of NRM (HR 0.15, 95%CI 0.03-0.69, p=0.015, table 2). Surprisingly, 3-year overall survival (OS) was not different in patients with high and low VEGF concentrations (50% vs 42% respectively, p=0.60), as majority of patients in high VEGF group responded to salvage therapy after relapse.


Figure 1. 1-year relapse incidence and non-relapse mortality according to VEGF level
|
Factor |
Multivariate, p-value |
HR |
HR 95% CI |
|
1-year cumulative relapse rate |
|||
|
Unrelated vs related donor |
0.232 |
||
|
Active disease at the time of HSCT |
0.002 |
4.05 |
1.68-9.79 |
|
MAC vs RIC conditioning |
0.461 |
||
|
Acute GVHD, grade 1-4 |
0.002 |
0.26 |
0.11-0.61 |
|
Chronic GVHD |
0.003 |
0.19 |
0.06-0.55 |
|
VEGF A before conditioning > 37 pg/ml |
0.009 |
3.15 |
1.34-7.40 |
|
1-year non-relapse mortality |
|||
|
Active disease at the time of HSCT |
0.027 |
4.67 |
1.19-18.30 |
|
Age |
0.70 |
||
|
Unrelated vs related donor |
0.022 |
6.64 |
1.32-33.40 |
|
MAC vs RIC conditioning |
0.32 |
||
|
Acute GVHD, grade 3-4 |
0.024 |
4.87 |
1.24-19.14 |
|
VEGF A on day 0 < 7.8 pg/ml |
0.015 |
0.15 |
0.03-0.69 |
Table 2. Multivariate analysis of relapse incidence and non-relapse mortality (whole group)
Predictive value of CECs for
relapse and non-relapse mortality
Univariate analysis with previously determined cut-off value showed patients with CEC level after conditioning >87 cells/ml had higher relapse incidence (60% vs 21%, p<0.001), but in multivariate analysis it was not a significant factor (p=0.09, table 3). So CECs was not an independent predictive marker of relapse, but rather demonstration the increased endothelial damage in patients with high-risk disease. This was confirmed by the fact that level >87 cells/ml was significantly more often observed in patients with active disease at the time of the alloHSCT (80% vs 20%, p=0.032).
Univariate analysis of NRM confirmed that patients with pre-conditioning level of CECs >71 had increased risk of transplant-related death during the first year (69% vs 20%, p=0.001), while the incidence of late NRM was not significantly different (0% vs 5%, p=0.70). Nevertheless, in multivariate analysis the differences in 1-year NRM were also not significant (95%CI 0.84-5.76, p=0.102, table 3). Regarding results of multivariate analysis of CEC as the predictive marker, the statistical power of the models was relatively low due to small number of patients with CEC measured, so with a larger group of patients, the CECs as the covariate might reach the significant level.
|
Factor |
Multivariate, p-value |
HR |
HR 95% CI |
|
1-year cumulative relapse rate |
|||
|
Active disease at the time of HSCT |
0.82 |
||
|
MAC vs RIC conditioning |
0.148 |
||
|
Acute GVHD, grade 1-4 |
0.035 |
0.24 |
0.07-0.91 |
|
Chronic GVHD |
0.019 |
0.08 |
0.01-0.66 |
|
CEC after conditioning>87 cells/ml |
0.086 |
||
|
1-year non-relapse mortality |
|||
|
Active disease at the time of HSCT |
0.050 |
3.05 |
1.00-9.31 |
|
Acute GVHD, grade 3-4 |
0.040 |
2.98 |
1.05-8.45 |
|
CEC before conditioning>71 cells/ml |
0.102 |
||
Table 3. Multivariate analysis of relapse incidence and non-relapse mortality (only patients with measured level of CECs)
Association between level
of VEGF A and CECs
The interesting result of the analysis was that there was no correlation between pre-transplant level of CECs and VEGF (p=0.81), as well as for after conditioning (p=0.74) and engraftment levels (p=0.59). But when the cut-off levels of CEC (>71 cells/ml) and VEGF (<7.8 pg/ml) that predicted NRM were tested, in patients with high CEC level pre-conditioning VEGF was significantly more frequently elevated on day 0 (83% vs 51%, p=0.036).
Discussion
In this study we confirmed the prognostic significance of endothelial damage markers for non-relapse mortality. As expected, these markers allow to predict only early, but not late mortality. This is due to the fact that late NRM is mostly associated with chronic GVHD or infections related to impaired immune system [26]. The factors that influence development of chronic GVHD and immune reconstitution are mostly immunologic and are associated with patient-donor major or minor HLA-antigen disparity and trigger these events in the late post-transplant period [3, 24]. On the contrary, in an early post-transplant period endothelial dysfunction plays a role in a number of acute complications. In our study due to small number of patients it was impossible to establish relationship between endothelial damage and all of the complications, but as we previously reported elevation of VEGF and CEC levels was closely related to development of VOD [19, 20]. Likewise, a number of studies demonstrated association between endothelial damage and acute GVHD [14, 15, 18],
In this study we found out that VEGF is predictive for NRM after conditioning, while CEC – when measured before conditioning. So different endothelial damage markers may represent different aspects of endothelial damage and are elevated variable time after a damage occurs. This was confirmed in our study by absence of correlation between VEGF and CEC, and only more sophisticated methods revealed association between these two biomarkers. So VEGF A is secreted a large variety of cells, including endothelial and blood mononuclears. It is eliminated via cleavage with serum proteases and binding to either soluble or cellular VEGF receptors. But also a large proportion of VEGF is bound to extracellular matrix (ECM) heparin sulfate proteoglycans. In response to endothelial and tissue damage ECM-bound VEGF is cleaved from proteoglycan complex and released into circulation to facilitate reparation. What is important is that activity of serum proteases in terms of VEGF elimination is insufficient to decrease its level in situations of its extensive release from ECM. But its levels in plasma return to normal values very rapidly, within hours, if there are no continuous stimuli [9, 28, 32]. Hence, VEGF A level in plasma represent the acute phase of endothelial damage, that is why the time-point post-conditioning is of highest predictive value. CEC levels, on the other hand, represent chronic endothelial damage and are present in circulation for a longer period of time than VEGF. That is why it is a valuable tool to predict complications in diabetes and cardiovascular disorders [3, 7]. Marginally significant predictive value of CEC in multivariate analysis may not indicate that this is less valuable prognostic marker, but may be a result of a smaller number of patients in whom it as measured. In summary, different endothelial damage markers complement each other and in further clinical research should be used in combination.
Another aspect of our study was a dual role of VEGF. Besides its role as endothelial damage biomarker, it is also a disease risk factor in hematologic malignancies [1, 5, 6, 11, 33, 34]. We have demonstrated that it is also a factor of adverse disease prognosis in HSCT, but it is important that there were no differences in OS respective to pre-transplant VEGF level. Successful salvage post-transplant chemotherapy and donor lymphocyte infusions, at least in some patients from the high-VEGF A group, demonstrates a potential utility of graft-versus-leukemia effect to overcome this factor of resistance. Allogeneic HSCT is considered a treatment of choice for high-risk disease in patients with acute leukemias, myelodysplastic syndrome, chronic myeloid leukemia and lymphomas [23, 36]. As standard therapy outcome for these malignancies was reported to be negatively influenced by VEGF A overexpression, further studies are required to determine whether patients with high level of this factor should be candidates for HSCT. Due to very low incidence of late relapses in the study group we failed to demonstrate if there was any influence of VEGF expression on late disease recurrence, so larger studies are required to test this, but given very high incidence of early relapses in our study in the high VEGF group, early post-transplant therapy should be considered for these patients.
Recently, a number of clinical scoring systems were validated to predict risk of alloHSCT, like EBMT risk score [12, 29] or Seattle PAM score [27]. The results of this study show that the endothelial damage markers are of distinct predictive value, irrelevant of clinical parameters. Therefore, further studies are required to evaluate if they could be incorporated into the risk assessment models. In conclusion, peripheral CECs and plasma VEGF levels represent a useful prognostic tool to predict the risk of alloHSCT and disease relapse.
Conflict of interests
No conflict interest is reported.
References
- Aguayo A, Estey E, Kantarjian H et al. Cellular vascular endothelial growth factor is a predictor of outcome in patients with acute myeloid leukemia. Blood 1999; 94(11): 3717-21.
- Aguayo A, Kantarjian H, Manshouri T et al. Angiogenesis in acute and chronic leukemias and myelodysplastic syndromes. Blood 2000; 96(6): 2240-5.
- Allen JL, Fore MS, Wooten J et al. B cells from patients with chronic GVHD are activated and primed for survival via BAFF-mediated pathways. Blood 2012; 120(12): 2529-36.
- Asicioglu E, Gogas Yavuz D, Koc M, Ozben B, Yazici D, Deyneli O, Akalin S. Circulating endothelial cells are elevated in patients with type 1 diabetes mellitus. Eur J Endocrinol 2010; 162(4): 711-7.
- Avramis IA, Panosyan EH, Dorey F, Holcenberg JS, Avramis VI. Children’s Oncology Group. Correlation between high vascular endothelial growth factor-A serum levels and treatment outcome in patients with standard-risk acute lymphoblastic leukemia: a report from Children’s Oncology Group Study CCG-1962. Clin Cancer Res 2006; 12(23): 6978-84.
- Ben Arush MW, Ben Barak A, Maurice S, Livne E. Serum VEGF as a significant marker of treatment response in Hodgkin lymphoma. Pediatr Hematol Oncol 2007; 24(2): 111-5.
- Boos CJ, Balakrishnan B, Blann AD, Lip GY. The relationship of circulating endothelial cells to plasma indices of endothelial damage/dysfunction and apoptosis in acute coronary syndromes: implications for prognosis. J Thromb Haemost 2008; 6(11): 1841-50.
- Carreras E, Diaz-Ricart M. The role of the endothelium in the short-term complications of hematopoietic SCT. Bone Marrow Transplant 2011; 46(12): 1495-502.
- Chen TT, Luque A, Lee S, Anderson SM, Segura T, Iruela-Arispe ML. Anchorage of VEGF to the extracellular matrix conveys differential signaling responses to endothelial cells. J Cell Biol 2010; 188(4): 595-609.
- de Bont ES, Rosati S, Jacobs S, Kamps WA, Vellenga E. Increased bone marrow vascularization in patients with acute myeloid leukaemia: a possible role for vascular endothelial growth factor. Br J Haematol 2001; 113(2) :296-304.
- Hatjiharissi E, Terpos E, Papaioannou M et al. The combination of intermediate doses of thalidomide and dexamethasone reduces bone marrow micro-vessel density but not serum levels of angiogenic cytokines in patients with refractory/relapsed multiple myeloma. Hematol Oncol 2004; 22(4): 159-68.
- Hemmati PG, Terwey TH, le Coutre P et al. A modified EBMT risk score predicts the outcome of patients with acute myeloid leukemia receiving allogeneic stem cell transplants. Eur J Haematol. 2011; 86(4): 305-16.
- Leonhardt F, Grundmann S, Behe M et al. Inflammatory neovascularization during graft-versus-host disease is regulated by αv integrin and miR-100. Blood. 2013; 121(17): 3307-18.
- Luft T, Dietrich S, Falk C et al. Steroid-refractory GVHD: T-cell attack within a vulnerable endothelial system. Blood 2011; 118(6): 1685-92.
- Lunn RA, Sumar N, Bansal AS, Treleaven J. Cytokine profiles in stem cell transplantation: possible use as a predictor of graft-versus-host disease. Hematology 2005; 10(2): 107-14.
- Mancuso P, Antoniotti P, Quarna J et al. Validation of a standardized method for enumerating circulating endothelial cells and progenitors: flow cytometry and molecular and ultrastructural analyses. Clin Cancer Res 2009;15(1): 267-73.
- Medinger M, Tichelli A, Bucher C et al. GVHD after allogeneic haematopoietic SCT for AML: angiogenesis, vascular endothelial growth factor and VEGF receptor expression in the BM. Bone Marrow Transplant. 2013; 48(5): 715-21.
- Min CK, Kim SY, Lee MJ et al. Vascular endothelial growth factor (VEGF) is associated with reduced severity of acute graft-versus-host disease and nonrelapse mortality after allogeneic stem cell transplantation. Bone Marrow Transplant 2006; 38(2): 149-56.
- Moiseev IS, Babenko EV, Sipol AA et al. Measurement of circulating endothelial cells to support the diagnosis of veno-occlusive disease after hematopoietic stem cell transplantation. Int J Lab Hematol. 2014; 36(4): e27-9.
- Moiseev IS, Lapin SV, Surkova EA et al. Level of vascular endothelial growth factor predicts both relapse and nonrelapse mortality after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant. 2013; 19(12): 1677-82.
- Norton J, Sloane JP, al-Saffar N et al. Vessel associated adhesion molecules in normal skin and acute graft-versus-host disease. J Clin Pathol. 1991; 44(7): 586-91.
- Page AV, Liles WC. Biomarkers of endothelial activation/dysfunction in infectious diseases. Virulence 2013; 4(6): 507-16.
- Phillips GL. Allogeneic hematopoietic stem cell transplantation (HSCT) for high-risk acute myeloid leukemia (AML)/myelodysplastic syndrome (MDS): how can we improve outcomes in the near future? Leuk Res. 2012; 36(12): 1490-5.
- Przepiorka D, Weisdorf D, Martin P et al. Consensus conference on acute GVHD grading. Bone Marrow Transplant 1995; 15(6): 825-828.
- Riihijärvi S, Nurmi H, Holte H et al. High serum vascular endothelial growth factor level is an adverse prognostic factor for high-risk diffuse large B-cell lymphoma patients treated with dose-dense chemoimmunotherapy. Eur J Haematol 2012; 89(5): 395-402.
- Schechter T, Pole JD, Darmawikarta D et al. Late mortality after hematopoietic SCT for a childhood malignancy. Bone Marrow Transplant. 2013; 48(10): 1291-5.
- Sorror ML, Storer BE, Maloney DG et al. Outcomes after allogeneic hematopoietic cell transplantation with nonmyeloablative or myeloablative conditioning regimens for treatment of lymphoma and chronic lymphocytic leukemia. Blood. 2008; 111(1): 446-52.
- Stefanini MO, Wu FT, Mac Gabhann F, Popel AS. A compartment model of VEGF distribution in blood, healthy and diseased tissues. BMC Syst Biol 2008; 2: 77.
- Terwey TH, Hemmati PG, Martus P et al. A modified EBMT risk score and the hematopoietic cell transplantation-specific comorbidity index for pre-transplant risk assessment in adult acute lymphoblastic leukemia. Haematologica. 2010; 95(5): 810-8.
- Testa S, Manna A, Porcellini A et al. Increased plasma level of vascular endothelial glycoprotein thrombomodulin as an early indicator of endothelial damage in bone marrow transplantation. Bone Marrow Transplant. 1996; 18(2): 383-8.
- Vassiliou AG, Mastora Z, Orfanos SE et al. Elevated biomarkers of endothelial dysfunction/activation at ICU admission are associated with sepsis development. Cytokine. 2014; 69(2): 240-7.
- Vempati P, Mac Gabhann F, Popel AS. Quantifying the proteolytic release of extracellular matrix-sequestered VEGF with a computational model. PLoS One 2010; 5(7): e11860.
- Verstovsek S, Estey E, Manshouri T et al. Clinical relevance of vascular endothelial growth factor receptors 1 and 2 in acute myeloid leukaemia and myelodysplastic syndrome. Br J Haematol 2002; 118(1): 151-6.
- Verstovsek S, Kantarjian H, Manshouri T et al. Prognostic significance of cellular vascular endothelial growth factor expression in chronic phase chronic myeloid leukemia. Blood 2002; 99(6): 2265-7.
- Wierzbowska A, Robak T, Krawczynska A et al. Kinetics and apoptotic profile of circulating endothelial cells as prognostic factors for induction treatment failure in newly diagnosed acute myeloid leukemia patients. Ann Hematol. 2008; 87(2): 97-106.
- Zikos P, Van Lint MT, Lamparelli T et al. Allogeneic hemopoietic stem cell transplantation for patients with high risk acute lymphoblastic leukemia: favorable impact of chronic graft-versus-host disease on survival and relapse. Haematologica. 1998; 83(10): 896-903.
Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,
Владимир Н. Вавилов, Борис В. Афанасьев
НИИ детской онкологии, гематологии и трансплантологии им. Р. М. Горбачевой, Первый Санкт-Петербургский государственный медицинский университет им. И. П. Павлова, Санкт-Петербург, Россия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "388" ["VALUE"]=> array(2) { ["TEXT"]=> string(4349) "<p class="Summery_Rus" lang="ru-RU">В ряде исследований проводилось изучение прогностического значения маркеров повреждения эндотелия для анализа риска различных исходов аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК). При этом, однако, редко сравнивали информативность различных лабораторных маркеров при длительных сроках наблюдения. В настоящей работе мы оценивали прогностическую значимость фактора роста сосудистого эндотелия (<span lang="en-US">VEGF</span>) в плазме крови и содержания циркулирующих эндотелиальных клеток (ЦЭК) как возможных факторов, ассоциированных с ранней и поздней смертностью, не связанной с рецидивами. Учитывая известный негативный прогностический эффект экспрессии <span lang="en-US">VEGF</span> при онкогематологических заболеваниях, леченных цитостатической терапией, другой целью работы была оценка ассоциаций между уровнями <span lang="en-US">VEGF</span> и частотой рецидивов после алло-ТГСК. Уровни <span lang="en-US">VEGF</span> анализировали у 91 пациента перед началом кондиционирующей терапии, в день трансплантации и в день приживления трансплантата. Содержание ЦЭК в крови определяли у 55 больных из той же группы и в те же сроки. Как уровни <span lang="en-US">VEGF</span>, так и содержание ЦЭК коррелировали с ранней, но не более поздней нерецидивной смертностью. Высокие уровни <span lang="en-US">VEGF</span> в день 0 при использовании мультивариантного анализа были ассоциированы с более высокой однолетней безрецидивной выживаемостью (55% против 22%; <span lang="en-US">HR</span> 3,15, 95%; <span lang="en-US">CI</span> 1,34-7,40, <span lang="en-US">p</span>=0,009), тогда как высокое содержание ЦЭК до кондиционирования было ассоциировано с повышенной безрецидивной выживаемостью при унивариантном (69% против 20%, <span lang="en-US">p</span>=0,001), но не многофакторном анализе (95%<span lang="en-US">CI</span> 0.84-5.76, <span lang="en-US">p</span>=0,102). Высокие уровни <span lang="en-US">VEGF</span> <span lang="en-US">A</span> перед кондиционированием были ассоциированы с повышенной частотой рецидивов в течение 1 года (55% против 22%, <span lang="en-US">p</span>=0,001, <span lang="en-US">HR</span> 3,15, 95%<span lang="en-US">CI</span> 1,34-7,40), но не были связаны с поздними рецидивами и общей 3-летней выживаемостью (50% против 42%, соответственно, <span lang="en-US">p</span>=0.60), поскольку многие пациенты были успешно пролечены после рецидива. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3921) "В ряде исследований проводилось изучение прогностического значения маркеров повреждения эндотелия для анализа риска различных исходов аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК). При этом, однако, редко сравнивали информативность различных лабораторных маркеров при длительных сроках наблюдения. В настоящей работе мы оценивали прогностическую значимость фактора роста сосудистого эндотелия (VEGF) в плазме крови и содержания циркулирующих эндотелиальных клеток (ЦЭК) как возможных факторов, ассоциированных с ранней и поздней смертностью, не связанной с рецидивами. Учитывая известный негативный прогностический эффект экспрессии VEGF при онкогематологических заболеваниях, леченных цитостатической терапией, другой целью работы была оценка ассоциаций между уровнями VEGF и частотой рецидивов после алло-ТГСК. Уровни VEGF анализировали у 91 пациента перед началом кондиционирующей терапии, в день трансплантации и в день приживления трансплантата. Содержание ЦЭК в крови определяли у 55 больных из той же группы и в те же сроки. Как уровни VEGF, так и содержание ЦЭК коррелировали с ранней, но не более поздней нерецидивной смертностью. Высокие уровни VEGF в день 0 при использовании мультивариантного анализа были ассоциированы с более высокой однолетней безрецидивной выживаемостью (55% против 22%; HR 3,15, 95%; CI 1,34-7,40, p=0,009), тогда как высокое содержание ЦЭК до кондиционирования было ассоциировано с повышенной безрецидивной выживаемостью при унивариантном (69% против 20%, p=0,001), но не многофакторном анализе (95%CI 0.84-5.76, p=0,102). Высокие уровни VEGF A перед кондиционированием были ассоциированы с повышенной частотой рецидивов в течение 1 года (55% против 22%, p=0,001, HR 3,15, 95%CI 1,34-7,40), но не были связаны с поздними рецидивами и общей 3-летней выживаемостью (50% против 42%, соответственно, p=0.60), поскольку многие пациенты были успешно пролечены после рецидива.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "389" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-38-46" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-38-46" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "390" ["VALUE"]=> array(2) { ["TEXT"]=> string(218) "<p class="Autor ParaOverride-3">Ivan S. Moiseev, Sergej V. Lapin, Elena A. Surkova, Margarita Y. Lerner, Elena V. Babenko, Alexandra A. Sipol, <br>Vladimir N. Vavilov, Boris V. Afanasyev</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(190) "Ivan S. Moiseev, Sergej V. Lapin, Elena A. Surkova, Margarita Y. Lerner, Elena V. Babenko, Alexandra A. Sipol,
Vladimir N. Vavilov, Boris V. Afanasyev
Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, The First St.Petersburg State I. Pavlov Medical University
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "392" ["VALUE"]=> array(2) { ["TEXT"]=> string(1973) "<h2>Summery</h2> <p class="Summery"> A number of studies evaluated predictive value of endothelial damage markers on outcomes of allogeneic hematopoietic stem cell transplantation (alloHSCT), but they were rarely measured in combination and with long follow up. In this study we evaluated predictive value of vascular endothelial growth factor (VEGF) and circulating endothelial cells (CEC) on early and late non-relapse mortality (NRM). Given the known negative prognostic impact of VEGF expression in hematologic malignancies undergoing chemotherapy, the second goal was to access impact of VEGF level on relapse incidence after alloHSCT. Level of VEGF was analyzed in 91 consecutive patients before the start of conditioning, on day 0 and on the day of engraftment. CEC were measured in 55 consecutive patients from the same study group at the same time points. Both VEGF and CEC were predicted early, but not late NRM. High level of VEGF on day 0 in multivariate analysis was associated with increased 1-year NRM (55% vs 22%, HR 3.15, 95%CI 1.34-7.40, p=0.009), while high level of CEC before conditioning was associated with increased 1-year NRM in univariate (69% vs 20%, p=0.001), but not multivariate analysis (95%CI 0.84-5.76, p=0.102). High VEGF A level before conditioning was associated with increased 1-year relapse rate (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40), but had no impact on late relapses and 3-year overall survival (50% vs 42% respectively, p=0.60), as a large proportion of patients were successfully salvaged after relapse. CEC were not a significant prognostic factor for relapse (p=0.09). No correlation was found between VEGF and CEC at any time point (p>0.05), indicating that they may represent different aspects of endothelial dysfunction. In conclusion, VEGF and CEC are valuable biomarkers to predict early NRM, and VEGF is also a predictive factor of early relapse after alloHSCT. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1935) "Summery
A number of studies evaluated predictive value of endothelial damage markers on outcomes of allogeneic hematopoietic stem cell transplantation (alloHSCT), but they were rarely measured in combination and with long follow up. In this study we evaluated predictive value of vascular endothelial growth factor (VEGF) and circulating endothelial cells (CEC) on early and late non-relapse mortality (NRM). Given the known negative prognostic impact of VEGF expression in hematologic malignancies undergoing chemotherapy, the second goal was to access impact of VEGF level on relapse incidence after alloHSCT. Level of VEGF was analyzed in 91 consecutive patients before the start of conditioning, on day 0 and on the day of engraftment. CEC were measured in 55 consecutive patients from the same study group at the same time points. Both VEGF and CEC were predicted early, but not late NRM. High level of VEGF on day 0 in multivariate analysis was associated with increased 1-year NRM (55% vs 22%, HR 3.15, 95%CI 1.34-7.40, p=0.009), while high level of CEC before conditioning was associated with increased 1-year NRM in univariate (69% vs 20%, p=0.001), but not multivariate analysis (95%CI 0.84-5.76, p=0.102). High VEGF A level before conditioning was associated with increased 1-year relapse rate (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40), but had no impact on late relapses and 3-year overall survival (50% vs 42% respectively, p=0.60), as a large proportion of patients were successfully salvaged after relapse. CEC were not a significant prognostic factor for relapse (p=0.09). No correlation was found between VEGF and CEC at any time point (p>0.05), indicating that they may represent different aspects of endothelial dysfunction. In conclusion, VEGF and CEC are valuable biomarkers to predict early NRM, and VEGF is also a predictive factor of early relapse after alloHSCT.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "393" ["VALUE"]=> string(177) "Prognostic significance of vascular endothelial growth factor and circulating endothelial cells for early and late outcomes of allogeneic hematopoietic stem cell transplantation" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(177) "Prognostic significance of vascular endothelial growth factor and circulating endothelial cells for early and late outcomes of allogeneic hematopoietic stem cell transplantation" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1225" ["VALUE"]=> string(2) "18" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "18" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1226" ["VALUE"]=> string(2) "19" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "19" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(14) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "390" ["VALUE"]=> array(2) { ["TEXT"]=> string(218) "<p class="Autor ParaOverride-3">Ivan S. Moiseev, Sergej V. Lapin, Elena A. Surkova, Margarita Y. Lerner, Elena V. Babenko, Alexandra A. Sipol, <br>Vladimir N. Vavilov, Boris V. Afanasyev</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(190) "Ivan S. Moiseev, Sergej V. Lapin, Elena A. Surkova, Margarita Y. Lerner, Elena V. Babenko, Alexandra A. Sipol,
Vladimir N. Vavilov, Boris V. Afanasyev
Ivan S. Moiseev, Sergej V. Lapin, Elena A. Surkova, Margarita Y. Lerner, Elena V. Babenko, Alexandra A. Sipol,
Vladimir N. Vavilov, Boris V. Afanasyev
Summery
A number of studies evaluated predictive value of endothelial damage markers on outcomes of allogeneic hematopoietic stem cell transplantation (alloHSCT), but they were rarely measured in combination and with long follow up. In this study we evaluated predictive value of vascular endothelial growth factor (VEGF) and circulating endothelial cells (CEC) on early and late non-relapse mortality (NRM). Given the known negative prognostic impact of VEGF expression in hematologic malignancies undergoing chemotherapy, the second goal was to access impact of VEGF level on relapse incidence after alloHSCT. Level of VEGF was analyzed in 91 consecutive patients before the start of conditioning, on day 0 and on the day of engraftment. CEC were measured in 55 consecutive patients from the same study group at the same time points. Both VEGF and CEC were predicted early, but not late NRM. High level of VEGF on day 0 in multivariate analysis was associated with increased 1-year NRM (55% vs 22%, HR 3.15, 95%CI 1.34-7.40, p=0.009), while high level of CEC before conditioning was associated with increased 1-year NRM in univariate (69% vs 20%, p=0.001), but not multivariate analysis (95%CI 0.84-5.76, p=0.102). High VEGF A level before conditioning was associated with increased 1-year relapse rate (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40), but had no impact on late relapses and 3-year overall survival (50% vs 42% respectively, p=0.60), as a large proportion of patients were successfully salvaged after relapse. CEC were not a significant prognostic factor for relapse (p=0.09). No correlation was found between VEGF and CEC at any time point (p>0.05), indicating that they may represent different aspects of endothelial dysfunction. In conclusion, VEGF and CEC are valuable biomarkers to predict early NRM, and VEGF is also a predictive factor of early relapse after alloHSCT.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1935) "Summery
A number of studies evaluated predictive value of endothelial damage markers on outcomes of allogeneic hematopoietic stem cell transplantation (alloHSCT), but they were rarely measured in combination and with long follow up. In this study we evaluated predictive value of vascular endothelial growth factor (VEGF) and circulating endothelial cells (CEC) on early and late non-relapse mortality (NRM). Given the known negative prognostic impact of VEGF expression in hematologic malignancies undergoing chemotherapy, the second goal was to access impact of VEGF level on relapse incidence after alloHSCT. Level of VEGF was analyzed in 91 consecutive patients before the start of conditioning, on day 0 and on the day of engraftment. CEC were measured in 55 consecutive patients from the same study group at the same time points. Both VEGF and CEC were predicted early, but not late NRM. High level of VEGF on day 0 in multivariate analysis was associated with increased 1-year NRM (55% vs 22%, HR 3.15, 95%CI 1.34-7.40, p=0.009), while high level of CEC before conditioning was associated with increased 1-year NRM in univariate (69% vs 20%, p=0.001), but not multivariate analysis (95%CI 0.84-5.76, p=0.102). High VEGF A level before conditioning was associated with increased 1-year relapse rate (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40), but had no impact on late relapses and 3-year overall survival (50% vs 42% respectively, p=0.60), as a large proportion of patients were successfully salvaged after relapse. CEC were not a significant prognostic factor for relapse (p=0.09). No correlation was found between VEGF and CEC at any time point (p>0.05), indicating that they may represent different aspects of endothelial dysfunction. In conclusion, VEGF and CEC are valuable biomarkers to predict early NRM, and VEGF is also a predictive factor of early relapse after alloHSCT.
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "389" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-38-46" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-38-46" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-38-46" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "393" ["VALUE"]=> string(177) "Prognostic significance of vascular endothelial growth factor and circulating endothelial cells for early and late outcomes of allogeneic hematopoietic stem cell transplantation" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(177) "Prognostic significance of vascular endothelial growth factor and circulating endothelial cells for early and late outcomes of allogeneic hematopoietic stem cell transplantation" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(177) "Prognostic significance of vascular endothelial growth factor and circulating endothelial cells for early and late outcomes of allogeneic hematopoietic stem cell transplantation" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "391" ["VALUE"]=> array(2) { ["TEXT"]=> string(203) "<p class="Autor_place_work">Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, The First St.Petersburg State I. Pavlov Medical University </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(181) "Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, The First St.Petersburg State I. Pavlov Medical University
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(181) "Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, The First St.Petersburg State I. Pavlov Medical University
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(8) { [0]=> string(3) "378" [1]=> string(3) "379" [2]=> string(3) "380" [3]=> string(3) "381" [4]=> string(3) "382" [5]=> string(3) "383" [6]=> string(3) "384" [7]=> string(3) "385" } ["VALUE"]=> array(8) { [0]=> string(2) "64" [1]=> string(2) "34" [2]=> string(2) "62" [3]=> string(2) "37" [4]=> string(2) "60" [5]=> string(2) "63" [6]=> string(2) "61" [7]=> string(2) "65" } ["DESCRIPTION"]=> array(8) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" [7]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(8) { [0]=> string(2) "64" [1]=> string(2) "34" [2]=> string(2) "62" [3]=> string(2) "37" [4]=> string(2) "60" [5]=> string(2) "63" [6]=> string(2) "61" [7]=> string(2) "65" } ["~DESCRIPTION"]=> array(8) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" [7]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(8) { [0]=> string(60) "Alexandra A. Sipol" [1]=> string(60) "Boris V. Afanasyev" [2]=> string(58) "Elena A. Surkova" [3]=> string(55) "Elena Babenko" [4]=> string(57) "Ivan S. Moiseev" [5]=> string(61) "Margarita Y. Lerner" [6]=> string(57) "Sergej V. Lapin" [7]=> string(61) "Vladimir N. Vavilov" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "386" ["VALUE"]=> array(2) { ["TEXT"]=> string(343) "<p class="Autor_Rus" lang="ru-RU">Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,<br>Владимир Н. Вавилов, Борис В. Афанасьев</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(305) "Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,
Владимир Н. Вавилов, Борис В. Афанасьев
Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,
Владимир Н. Вавилов, Борис В. Афанасьев
В ряде исследований проводилось изучение прогностического значения маркеров повреждения эндотелия для анализа риска различных исходов аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК). При этом, однако, редко сравнивали информативность различных лабораторных маркеров при длительных сроках наблюдения. В настоящей работе мы оценивали прогностическую значимость фактора роста сосудистого эндотелия (VEGF) в плазме крови и содержания циркулирующих эндотелиальных клеток (ЦЭК) как возможных факторов, ассоциированных с ранней и поздней смертностью, не связанной с рецидивами. Учитывая известный негативный прогностический эффект экспрессии VEGF при онкогематологических заболеваниях, леченных цитостатической терапией, другой целью работы была оценка ассоциаций между уровнями VEGF и частотой рецидивов после алло-ТГСК. Уровни VEGF анализировали у 91 пациента перед началом кондиционирующей терапии, в день трансплантации и в день приживления трансплантата. Содержание ЦЭК в крови определяли у 55 больных из той же группы и в те же сроки. Как уровни VEGF, так и содержание ЦЭК коррелировали с ранней, но не более поздней нерецидивной смертностью. Высокие уровни VEGF в день 0 при использовании мультивариантного анализа были ассоциированы с более высокой однолетней безрецидивной выживаемостью (55% против 22%; HR 3,15, 95%; CI 1,34-7,40, p=0,009), тогда как высокое содержание ЦЭК до кондиционирования было ассоциировано с повышенной безрецидивной выживаемостью при унивариантном (69% против 20%, p=0,001), но не многофакторном анализе (95%CI 0.84-5.76, p=0,102). Высокие уровни VEGF A перед кондиционированием были ассоциированы с повышенной частотой рецидивов в течение 1 года (55% против 22%, p=0,001, HR 3,15, 95%CI 1,34-7,40), но не были связаны с поздними рецидивами и общей 3-летней выживаемостью (50% против 42%, соответственно, p=0.60), поскольку многие пациенты были успешно пролечены после рецидива.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(3921) "В ряде исследований проводилось изучение прогностического значения маркеров повреждения эндотелия для анализа риска различных исходов аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК). При этом, однако, редко сравнивали информативность различных лабораторных маркеров при длительных сроках наблюдения. В настоящей работе мы оценивали прогностическую значимость фактора роста сосудистого эндотелия (VEGF) в плазме крови и содержания циркулирующих эндотелиальных клеток (ЦЭК) как возможных факторов, ассоциированных с ранней и поздней смертностью, не связанной с рецидивами. Учитывая известный негативный прогностический эффект экспрессии VEGF при онкогематологических заболеваниях, леченных цитостатической терапией, другой целью работы была оценка ассоциаций между уровнями VEGF и частотой рецидивов после алло-ТГСК. Уровни VEGF анализировали у 91 пациента перед началом кондиционирующей терапии, в день трансплантации и в день приживления трансплантата. Содержание ЦЭК в крови определяли у 55 больных из той же группы и в те же сроки. Как уровни VEGF, так и содержание ЦЭК коррелировали с ранней, но не более поздней нерецидивной смертностью. Высокие уровни VEGF в день 0 при использовании мультивариантного анализа были ассоциированы с более высокой однолетней безрецидивной выживаемостью (55% против 22%; HR 3,15, 95%; CI 1,34-7,40, p=0,009), тогда как высокое содержание ЦЭК до кондиционирования было ассоциировано с повышенной безрецидивной выживаемостью при унивариантном (69% против 20%, p=0,001), но не многофакторном анализе (95%CI 0.84-5.76, p=0,102). Высокие уровни VEGF A перед кондиционированием были ассоциированы с повышенной частотой рецидивов в течение 1 года (55% против 22%, p=0,001, HR 3,15, 95%CI 1,34-7,40), но не были связаны с поздними рецидивами и общей 3-летней выживаемостью (50% против 42%, соответственно, p=0.60), поскольку многие пациенты были успешно пролечены после рецидива.
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "387" ["VALUE"]=> array(2) { ["TEXT"]=> string(393) "<p class="Autor_place_work">НИИ детской онкологии, гематологии и трансплантологии им. Р. М. Горбачевой, Первый Санкт-Петербургский государственный медицинский университет им. И. П. Павлова, Санкт-Петербург, Россия </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(371) "НИИ детской онкологии, гематологии и трансплантологии им. Р. М. Горбачевой, Первый Санкт-Петербургский государственный медицинский университет им. И. П. Павлова, Санкт-Петербург, Россия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(371) "НИИ детской онкологии, гематологии и трансплантологии им. Р. М. Горбачевой, Первый Санкт-Петербургский государственный медицинский университет им. И. П. Павлова, Санкт-Петербург, Россия
" } } } [1]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "2" ["~IBLOCK_SECTION_ID"]=> string(1) "2" ["ID"]=> string(2) "86" ["~ID"]=> string(2) "86" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["~NAME"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:44:55" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:44:55" ["DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-47-57/" ["~DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-47-57/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(53728) "
Introduction
Myocardial infarction (MI) is a common reason of death and disability worldwide. Over the last decade, different cell therapy options have been tested to improve efficiency of MI treatment, including the s.c. cardiomyoplastics. Various cells are proposed to be used for this purpose. Autologous bone marrow is a widely used source of therapeutic cell preparations, thus providing freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchimal stromal cells (MMSC). Meanwhile, existing works concerning clinical effects of MF and MMSC transplantation in acute MI yield controversial results [6, 11, 16, 24, 26, 29, 31], thus necessitating further studies and getting experience in this area.
The aim of the study
The aim of our experimental study was to compare the effects of intramyocardial MF and MMSC transplantation upon clinical course and outcome of MI, using a rabbit model during prolonged observation terms by using complex of modern functional and morphological study.
Materials and methods
The experiments were performed with male Chinchilla rabbits of 2.8+ 0.2 kg weight, aged 3 - 4 months. All experimental procedures have been carried out in accordance with guidelines of local Ethical Committee at the First St.Petersburg I.Pavlov State Medical University.
Isolation, characterization, and morphological description of bone marrow cells
Bone marrow aspirate (10+ 1mL) was obtained from a rabbit by iliac puncture, following premedication with Droperidol (0.5 mg/kg, Xylasine, 14 mg/kg body mass), and local anesthesia with 0.5 per cent Novocaine, and placed into a tube containing CPDS (citrate phosphate dextrose solution, Terumo, Japan). Mononuclear cell fraction was obtained by means of centrifugation (1600 g, 20 min) Percoll density gradient (63%). Interphase cell fraction containing nucleated cells was washed in Са2+ and Mg2+-free Hanks’ solution (Gibco, USA), and span down by centrifuging. MMSC cell culture was obtained by MF cell passaging in а-МЕМ medium (ICN, USA) with 10 per cent fetal calf serum (Hyclone, New Zealand) supplied with gentamycin sulfate (50 mcg/mL; Invitrogen, Great Britain) in a СО2 incubator, at 5 per cent CO2 and 100% humidity for three weeks. The medium was changed twice a week. Ascorbic acid (ICN, USA) was added at a final concentration of 50 mcg/mL after first medium change. After reaching a semi-confluent state, the cells were reinoculated by means of 0.25% trypsin solution (Gibco, USA), and EDTA (0.02%, Gibco, USA). Before being transplanted, the cultured cells did not display any signs of spontaneous osteogenic differentiation, as evidenced by negative staining for alkaline phosphatase with a standard BCIP-NBT reagent (5-bromine-4-chloride-3-indolyl phosphate/ nitroblue tetrazolium, Sigma, USA), or any features of adipocytic transformation detectable with Sudan III/IV mixture (BDH Chemicals Ltd, Great Britain). Meanwhile, special studies with specific induction of differentiation to osteogenic and adipocytic lineage have shown their multipotency, i.e., the cultivated cells had typical MMSC characteristics.
In some animals, MNC or MMSC were stained prior to transplant with Hoechst nuclear fluorescent dye (Sigma, USA, final concentration of 1 mcg/mL), by shaking for 60 min in a СО2 incubator.
Nucleated marrow cells were counted in Buerker chamber, and their viability was assessed with Trypan Blue solution (Labtech, Russia). The cells labelled with Hoechst dye were detected by their blue nuclear fluorescence upon microscopy, using an «Axioscope» (Zeiss, Germany).
Experimental modelling and treatment of myocardial infarction
The rabbits were subjected to a left-sided thoracotomy under mechanical ventilation of lungs, followed by ligation of anterior descendent left coronary artery at a distance of 1 cm from the heart apex (Fig. 1, A, B). Ten minutes after the coronary occlusion, intramyocardial injections of ME or MMSC suspensions were performed into 6 points of the presumed infarction area, using insulin syringes, at a mean cell number of 2±0.2 x106 in 0.4 mL of а-МЕМ growth medium (modified Eagle medium), or with equivalent volumes of culture medium (placebo treatment), as shown in Fig. 1 C, D. Control animals were not subjected to myocardial injections. Surgical wounds were closed in layers, pneumothorax being eliminated by means of active air aspiration from the pleural cavity. The surviving animals were classified in four groups, each consisting of 13 animals, i.e., Group 1, (controls), Group 2 (placebo-treated), Group 3 (MMSC injections), and Group 4 (MF injections). Subgroups of ten animals were observed for 1 year after the surgery.




Figure 1. Modelling and treatment of myocardial infarction in rabbits: А – ligation of left anterior descendent coronary artery, B – a view of surgical area, C – topography of intramyocardial injections of marrow cells into the infarcted area; D – a view of surgical area
Detection of labelled cells in the myocardium
Twenty days after the surgical intervention, the subgroups of three rabbits from Groups 3 and 4 (subjected to myocardial injections) were sacrificed (this term was limited by the life-span of detectable fluorochrome in the cells). The hearts were teased in two parts (basal and apical), in order to get sections at the level of arterial ligature perpendicular to long axis of the heart. Apical part of the heart was pulped and treated with trypsin-collagenase enzyme mixture (Sigma, USA). The dissociated cells were collected by centrifugation, placed onto the microscopic slide, and the proportion of labeled cells have been counted.
Electrocardiography (ECG)
ECG was carried out in all animals before surgery, at the days +3, +7, +30, and one year after surgery.The results were evaluated by the 2nd standard lead on an ECG.
Heart ultrasonography
EchoCG was performed with a Sequoia 512 echocardiograph (Acuson, USA), using a linear 13 MGz transducer, according to a standard detection technique. EchoCG was performed in all cases before the surgery, at day +14, and 1 year after the surgery. The procedure was carried out in parallel with ECG recording. The end-diastolic size of left ventricle was registered in M-scanning regimen (EDSLV, mm). Left ventricular systolic function was registered by means of 2D scanning, from the apical access, in four-chamber and two-chamber positions. EF percentage calculations were made by means of a modified Simpson disc method, using the built-in software of the sonographic device .Aortal blood flow velocity was evaluated at the level of aortal valve (VAo, m/sec), using impulse-wave Doppler sonography. Dynamic features of the left ventricular wall were also studied in intervention/ infarction area, e.g., dyskinesia, hypokinesia, akinesia, calcification, or ossification in the areas of transplantation.
Myocardial perfusion evaluation
Perfusion rates were assessed with SPECT technique, using radiopharmaceutical tracer (RP) Myoview (Nycomed, Great Britain) labelled with Tc-99m. RP was injected, at a single dose of 30-50 MBq, into marginal ear vein via a peripheral catheter. 10 to 15 min after injection, a SPECT evaluation was performed by double-detector gamma chamber E.Cam. var (Siemens, Germany). To get quantitative values for myocardial perfusion rates, a ratio of mean RP accumulation in damaged versus reference areas was calculated in every case, as arbitrary units (Fig. 2). Uniformity of perfusion was determined as a minimum-to-maximum ratios (in pixels) for damaged and reference areas. The study was performed before surgical intervention, at day +10, and at 1,5, 6, and 12 months after surgery in all groups of animals.

Figure 2. SPECT visualization of left heart ventricle of rabbit. А, transverse heart projection at the level of ligated left anterior descendent coronary artery; B, a sketch of left ventricle with designation of its walls and localization of damaged and reference areas; C, perfusion SPECT tomography of the left ventricle of rabbit, with indication of reference zone (non-damaged myocardium area) and pathological zone (infarction localization area)
Sizing of infarcted area, LV dilatation measurements, histological studies
Dimensions of an experimental IM were determined by means of 2,3,5-triphenyltetrazolium chloride (TTC) staining of the heart sections, thus allowing to discern irreversibly damaged myocardial tissue from viable myocardium. Moreover, a routine histological evaluation was performed. All the animals surviving for 12 months post-surgery were subjected to euthanasia, followed by immediate heart extraction. The organ was rinsed in physiological saline and sectioned transversally with a special device below the ligature level into three segments of equal thickness, i.e., apical (1), middle (2), and basal sections (3), as shown in Fig. 3А.

Figure 3. A scheme of residual myocardial damage
assessment at 12 months post-treatment. А, sectioning of damaged myocardial area into three segments (apical, middle and basal); В, evaluation of post-infarction myocardial scarring by means of 1,3,5-TTC staining. Abbreviations: LV, left ventricle; RV, right heart ventricle.
In a half of all animals, the heart segments were then placed to 1% solution of TTC (ICN, USA) for 15 min. at 37ºC, pH 7.4. After development of bright-red color in viable myocardium, the stained heart segments were photographed by digital camera (Olimpus 2020, Japan), and the images were stored and processed by Adobe Photoshop CS2 software (Fig. 3В). For the second half of animals, the heart sections were fixed in 10% formaldehyde solution for 4 days followed by mounting in paraffin and preparing 7-mcm slices, using a routine technique. The histological samples were stained by HE (hematoxylin and eosin) and Mallory dye, thus allowing of discerning various types of connective tissues. Histological examinations were performed with a “BioLam” microscope (Russia). A grade of left ventricular dilatation (LV dilatation index) was determined as a ratio of LV lumen in TTC-positive heart segments to myocardial tissue area in both ventricles. This arbitrary index was calculated for each of three segments, and a mean value was then derived.
Quantitative evaluation of vascularization in damaged myocardial area
We have examined the borderline areas adjacent to the myocardial scars. Each tissue specimen was routinely stained by Mallory, and five consequent microscopic fields were evaluated at a 400x magnification. We performed separate counts of regulated-type vessels, i.e., arterioles, capillaries, venules, as well as non-regulated type-sinusoids, followed by calculating a mean blood vessel number per microscopic field.
Safety evaluation of approaches for angiogenesis stimulation in ischemic myocardium
To assess safety of cell transplantation in the studied groups of animals, we compared some general parameters, e.g., intra- and post-surgical mortality, incidence of arrhythmia and septic/inflammatory complications early after surgery. Condition of heart and internal organs was macroscopically evaluated by pathoanathomical obduction data, looking for occurrence of neoplastic processes, and microscopically evaluated for presence of local pathological changes in the areas of cell injections, in particular, atypically differentiated cells, focal sclerosis, or osteogenesis.
Statistical processing
We used SPSS software for statistical data processing. With small number of observations, the significance of differences was determined by a non-parametric Wilcoxon-Mann-Whitney criterion. All the data were presented as means + SD. The differences by P values of <0.05 were regarded as significant.
Results
Detection of labeled cells in damaged myocardium
Twenty days after treatment, both MFs and MMSCs were detectable as fluorescent cells, at, resp., 13+2% and 11+3% of initial numbers (Fig. 4).

Figure 4. ECG dynamics in studied groups
ECG dynamics in different experimetal groups
All the animals subjected to experimental coronary occlusion, developed typical ECG features of acute MI with distinct typical dynamics. However, all animals from control (placebo-treated), or MF-transplanted groups exhibited ECG signs of transmural MI, whereas MMSCs-transplant animals displayed only subendocardial myocardial damage (Fig. 5). Heart rate disturbances (atrial extrasystoles) in early postoperative period were developing with similar frequency (65%) in all the groups under study, except for MMSC-transplanted animals that showed them 3 times less often (20%). Twelve months after surgery, ECG patterns in MMSC-treated animals returned to the initial state, as compared with scar changes in ECG observed in MF-treated animals (Fig. 5)

Descriptions: MI-associated perfusion defects are shown by arrows; colour scale shows grade of myocardial perfusion from minimal to maximal values.
Figure 5. Typical changes on perfusion tomoscyntigraphy of myocardium in the groups under study, according to SPECT data before surgery, 1.5, and 12 months after surgery.
Initial EchoCG parameters did not differ between the groups under study. After the surgical intervention (coronary occlusion), a significant increase of EDSLV was observed, along with diminished EF, VAo. However, these disruptions were dissimilar for different groups, i.e., minimal for MMSC-treated animals and maximal for MNC-treated animals (Table 1, Fig. 6, 7). One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all cardiological parameters (p<0,05), absence of akinetic areas, that sufficiently differed from appropriate parameters in other groups. In controls and placebo group, the disturbances were long-standing, and a small akinetic area was formed in the apical segment. The most negative changes were detected among animals transplanted with MNC, which revealed drastic decrease in LV systolic function, increased LV size, development of extended akinetic areas, as compared with group 3, controls, and placebo group (p<0,05) (Table 1, Fig. 6, 7).
|
Groups |
Parameters and terms of the study |
||||||||
|
EF,% |
EDSLV, mm |
V Ao, m/sec |
|||||||
|
Initial values |
14 days after surgery |
12 months after surgery |
Initial values |
14 days after surgery |
12 months after surgery |
Initial values |
14 days after surgery |
12 months after |
|
|
№1 (controls) |
62.2±4.6 |
45.8±6.1 |
46.5±6.4 |
14.4±1.0 |
17.0±1.4 |
16.9±0.8 |
95±4 |
57±6 |
71±4 |
|
№2 (placebo) |
64.9±4.3 |
46.7±3.5 |
48.7±3.9 |
14.1±0.4 |
16.8±1.2 |
16.6±0.8 |
94±3 |
58±6 |
73±6 |
|
№3 (MMSC) |
61.7±4.0 |
53.1±4.8 |
58.2±3.1* |
14.7±0.9 |
15.2±0.7 |
14.9*±1.2 |
96±4 |
81±6 |
89±4* |
|
№4 (MNC) |
59.7±3.2 |
38.8±2.9 |
28.7*±4.1 |
14.9±1.2 |
17.9±0.8 |
19.8*±0.9 |
97±5 |
55±4 |
45±3* |
Abbreviations: LVEF, LV ejection fraction; EDSLV, end LV diastolic size; V Ao- blood flow velocity in ascending aorta; *, differences from control group are significant by p<0,05.
Table 1. Dynamics of LV systolic parameters from EchoCG data (M±m)

Figure 6. Transverse sections (1, apical; 2, median; 3, basal) from infarcted area of the heart wall in different experimental groups (Mallory staining) 12 months after MI modeling/ treatment
Dynamics of myocardial perfusion in the groups under study.
Cumulative findings concerning dynamics of myocardial perfusion in damaged areas are presented in Table 2. Before surgery, the perfusion parameters in all groups were within reference ranges. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, this decrease varied in different groups of animals, i.e., animals treated with MMSC or MNC showed less impaired perfusion rates than in control or placebo groups (p<0,05). At 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged area of myocardium in groups 3 and 4, reaching the pre-surgical rates by 3 months, in group 3 to a greater extent, without subsequent dynamics. In controls and placebo-treated group, the altered perfusion rates remained at similar levels at all the terms of observation.

Figure 7. Numbers of regulated vs. sinusoid-type microvessels per a space unit of MI area 12 months after modelling and treatment in compared groups of experimental animals.
Ordinate, number of microvessels per a IM space unit; abscissa, groups under study.
|
Groups |
TTC accumulation in damaged area (arb.un.), terms of study |
||||
|
Before surgery |
10 days after surgery |
1.5 months after surgery |
6 months after surgery |
12 months after surgery |
|
|
Controls |
1.01±0.01 |
0.57±0.02 |
0.59±0.04 |
0.61±0.02 |
0.61±0.04 |
|
Placebo |
1.01±0,02 |
0.59±0.02 |
0.62±0.02 |
0.64±0.04 |
0.61±0.03 |
|
MMSC |
0.98±0.03 |
0.81±0.01 * |
0.92±0.03 * |
0.98±0.02 * |
1.02±0.01* |
|
MF |
1,00±0.01 |
0.75±0.03 * |
0.89±0.03 * |
0.98±0.03 * |
0.99±0.01* |
Descriptions: arb.units = mean rates of TTC accumulation in damaged area/ mean values of TTC accumulation in reference area;
*- significance of differences as compared to control group (p<0.05)
Table 2. Dynamics of TTC accumulation in damaged myocardial area after treatment of acute MI in the groups under study by perfusion data (SPECT evaluation, M±m).
Morphometric heart studies
12 months after experimental MI modeling/ treatment, general macroscopic appearance of rabbit hearts was similar for control and placebo-treated groups, i.e., enlarged heart size, as compared to healthy hearts (intact animals), along with apical aneurism of LV. Distinct scarring of LV anterior wall was evident for the hearts from MMSC-treated animals, however, without evolving aneurysm, and without sufficient increase of the heart size. Heart dimensions among MF-treated animals did significantly exceed normal size, and appropriate heart parameters of healthy rabbits, and the animals from groups 1,2, and 3. The animals transplanted with MF had extendsive aneurysms at the apex and anterior wall of LV (Fig. 9,10,11). Scarring area and LV dilatation index for control group were, resp., 20.2±1.9%, and 0.19±0.02; 20,8±1.6% and 0.18±0.03 for placebo group; 35.8±1.6% and 0.34±0.03 for MF-transplanted group,. The animals treated with MMSCs exhibited the best characteristics, i.e., 6.0±2.6% and 0.11±0.02 (Fig. 12).
Histological pattern of myocardium
It was shown that intramyocardial MMSC vs. MF transplantation resulted, after 12 months, in the development of principally different heart morphology as compared to control or placebo groups of animals. After MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles.
Quantitative myocardial vascularization
12 months after MI modeling/treatment, a significant difference was revealed in vascularization patterns of damaged myocardium in the studied groups, i.e., the total microvessel numbers per 1 microscopic field were, resp., 15±3, 13+3, 7±1 and 6±2 for groups treated with MMSCs, MFs, controls and placebo-treated animals. After intramyocardial autotransplantation of bone marrow, the microvessel density in the area was not only increased over controls or placebo groups (p<0.05), but it exhibited a distinct type of microvessels showing a regulated type-wall, whereas control group recovered with development of sinusoid-type microvessels.
Safety evaluation of neoangiogenesis stimulation in ischemic myocardium
Intra- and post-operative mortality in all the studied groups did not significantly differ (a mean of 10±3% и 10±4%). Incidence of septic and inflammatory complications in the intervention area was, in general, significantly lower (p<0.05) among intramyocardially cell-treated animals (1) than in control or placebo group (3). No differences were here noted between MF and MMSC-treated groups. At macroscopic examination one year after surgical intervention, both groups of cell-treated animals did not show any signs of malignant neoplasia. Local examination of myocardium at the locations of cell injections did not reveal any cells with atypical differentiation (osteogenic or chondrogenic tissues).
Discussion
Rabbit model of myocardial infarction induced by ligation of anterior descendent left coronary artery proved to be a convenient and demonstrative technique for evaluation of therapeutic angiogenesis, testing the effects of vascular growth factors and cellular therapy [14]. The results obtained in present study have shown that intramyocardial transplantation of autologous bone marrow cells (MF versus MMSC) into the MI area in rabbits during acute period may considerably change the natural process of MI development and exerts different morpho-functional effects upon the damaged tissues.
MMSC transplantation, as compared to controls and placebo, was associated with definite reduction of the myocardial damage, and later (12 months after MI) this group of animals exhibited normalization of heart systolic function, ECG, myocardial perfusion. Meanwhile, upon morphological examination, the infracted area was represented by fine focal cardiosclerosis, without aneurism formation. The detected changes might have been caused by paracrine effect of transplanted cells and, probably, by their differentiation into various myocardial structures. At the first phase of MI characterized by death of the cardiomyocytes, the transplanted MMSC are able to inhibit apoptosis and produce a cytoprotective effect, thus allowing cardiomyocytes and transplanted cells to survive the ischemic state [6,16,30]. Moreover, the detected changes might be associated with changing degree of inflammatory response, due to effect of the transplant upon the cytokine profile. In the course of inflammation caused by ischemic damage of myocardium, there are two cytokine groups: pro-inflammatory factors (interleukin-1α, 1ß, 6, 8, tumor necrosis factor-α, ß and others) mostly secreted by macrophages and neutrophils, and anti-inflammatory molecules (interleukin-4, 10, transforming growth factor-β and others), mainly released by lymphocytes, monocytes and macrophages. It was shown in vitro that bone marrow MMSC, along with anti-inflammatory cytokines (interleukin-1α, 1ß, 6, 7, 8, tumor necrosis factor-α, ß) produce a broad spectrum of anti-inflammatory cytokines (interleukin-4, 10, transforming growth factor-β), as well as specific receptors for interleukin-1α, 1ß, 1, 3, 4, 6, 7, 8, tumor necrosis factor-α, ß [22]. Moreover, it has been shown that the bone marrow MMSC secrete different chemokines: MCP-1, RANTES, MIP-1alpha [23]. Most probably, such cytokine profile may induce significant populational changes, e.g., quantitative increase of macrophages, lymphocytes and monocytes that are able to secrete anti-inflammatory cytokines. This mechanism allows to reduce the degree of inflammatory response and the damaged area.
Progression of the small-focal myocardial infarction and normalization of systolic functions after BM MMSC transplantation, as shown in our study, can be also explained by potential ability of transplanted cells to differentiate into cardiomyocytes. However, an opportunity of BM MMSCs differentiation into cardiomyocites remains problematic. Most researchers note the ability of bone marrow MMSC to acquire cardiomyocyte-like phenotypes after transplantation into the damaged myocardium, as shown by synthesis of α-actinin, troponin-Т, tropomyosin. However, they have not revealed developing intercellular structures and/or contractile functions [20, 21, 27].
Thus, the changes in myocardial morphology and function after MMSC transplantation may be caused by their cytoprotective activity and ability to reduce the inflammatory response during acute infarction phase. By the contrary, intramyocardial MF transplantation, as compared to control and placebo groups, caused alterations of myocardial contractile function, expanding damage area, resulting into significant left ventricular fibroid aneurysms. Such effect is probably determined by MF ability to intensify inflammatory response, due to changing quantitative and qualitative cytokine profile in the damaged area, following direct massive injections of leukocytes. The bone marrow MFs constitute a heterogeneous population, containing mesenchymal stromal cells, hematopoietic stem cells, progenitor endothelial cells, as well as myeloid and lymphoid cells at different stages of maturation. There is an abundance of mature leukocytes among the bone marrow MF. Apparently, upon entering the ischemic myocardium, the MF start to release a variety of proteolytic enzymes and anti-inflammatory cytokines which attract blood cells to the altered areas, thus intensifying the inflammatory response [8]. The key point of myocardial repair is based on equilibrium between extracellular matrix degradation (needed for cell migration), and its resynthesis by the cells migrating to the damaged area. The proteolytic enzymes released by MF lyse intercellular collagen links and activate matrix metalloproteinases. Extracellular matrix degradation and expansion of infarcted area are caused by a cascade of proteolytic reactions. Moreover, the matrix metalloproteinases are also activated by some cytokines, e.g., as interleukin-1ß и tumor necrosis factor-α, ß [9, 19].
G. Ertl, S. Frantz have shown that dilatation of left ventricle and mortality were less expressed in the mice deficient for interleukin-1ß than in animals with normal cytokine levels [7]. In addition, proteolytic enzymes released by transplanted MF of bone marrow induce massive death of cardiomyocytes. Cardiac myosin released from necrotized myocardium is a proven potent autoantigen. The autoimmune reactions occur via activation of T lymphocytes followed by the secondary T-cell induced damage of cardiomyocytes and altered remodeling of extracellular matrix [2, 28].
Thus, morphological and functional changes revealed in myocardium after bone marrow MF injections may be caused by excessive intensification of inflammatory response during the hyperacute phase of MI.
The results of our study indicate that intramyocardial transplantation of MMSC and MF of bone marrow leads to increased vascularization of damage area. We assume that the angiogenic effect of these cells is accomplished by secretion of vascular growth factors and, probably, by differentiation of transplanted cells into cellular components of the vascular wall.
MMSCs are able to secrete angiogenic factors, such as VEGF (vascular endothelial growth factor), bFGF (basic fibroblast growth factor), HGF (hepatocyte growth factor), TGF-ß (transforming growth factor), angiopoietin-1 [13, 19]. Tang et al. (2005) demonstrated that the BM MMSC transplantation into the ischemic myocardium results into secretion of cytokine SDF-1 (stromal cell derived factor-1), which is a chemoattractant for endothelial cell progenitors and hematopoietic stem cells [22]. Progenitor endothelial cells migrating from peripheral blood into the damaged area are able to transform into mature endothelial cells and participate in angiogenesis [4, 12, 17]. Another mechanism of MMSCs involvement in post-transplant neoangiogenesis in myocardium is connected with their ability to differentiate into endothelial cells, smooth muscle cells, pericytes, fibroblasts that subsequently become components of the vascular wall, as shown in several studies [4,22].
Involvement of bone marrow MF in angiogenesis, according to the literature data, is regulated by several mechanisms. First of all, the MF populations, e.g., mesenchymal stromal cells, hematopoietic stem cells, progenitor endothelial cells, as well as immature cells of myeloid and lymphoid series, are secreting various angiogenic factors (VEGF, bFGF, TGF-ß, PDGF, angiopoietin-1, which stimulate proliferation of vascular endothelium and endothelial progenitors of damaged myocardium [13,25, 30, 31]. Secondly, the MF cells are able to secrete SDF-1 (stromal cell derived factor-1), which is a chemoattractant for progenitor endothelial cells and hematopoietic stem cells [20]. Thirdly, such mesenchymal stromal cells within the MF fraction are able to differentiate into endothelial cells and other vascular structures [22].
Our data differ from other studies that did not show such significant differences after MF and MMSC transplantation to the experimental MI area [6,13,16,21,25,27,31]. A probable explanation is that transplantation of bone marrow cells in these studies was performed either in later terms following MI, or the cells were administered by a different route, e.g., via coronary arteries, or intravenously [1,3,5,10,24,29]. A prolonged observation in our study did not register such complications as ossification or formation of angiomas in the cell transplantation area, as previously described [15], neither any neoplastic processes have been registered.
Conclusions
1. Local intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit, when performed in acute phase of experimental MI, was accompanied by changes in the MI development and resulted into different morphofunctional outcomes. I.e., transplantation of mesenchymal stem cells exerted a pronounced therapeutic effect, causing reduction of myocardial damage area and improvement of systolic functional indices. On the contrary, mononuclear cell transplantation produced negative effects, causing expansion of the damaged area and impairment of systolic indices.
2. Both MMSC and MF intramyocardial transplantation display stimulation of neoangiogenesis and improvement of perfusion in the infarcted area.
Conflict of interest
All the authors have no conflict of interest to declare.
References
- Chen Y, Teng X, Chen W et al. Timing of transplantation of autologous bone marrow derived mesenchymal stem cells for treating myocardial infarction. Sci China Life Sci 2014; 57(2): 195-200.
- Cheng X, Liao YH, Li B et al. Changes of rat lymphocyte proliferation and cytotoxic activity after acute myocardial infarction in vitro. Chin J Pathophysiol 2005; 21(9): 1848–50.
- Clifford DM, Fisher SA, Brunskill SJ et al. Long-term effects of autologous bone marrow stem cell treatment in acute myocardial infarction: factors that may influence outcomes. PLoS ONE 2012; 7(5): е37373.
- Davani S, Marandin A, Mersin N et al. Mesenchymal progenitor cells differentiate into an endothelial phenotype, enhance vascular density, and improve heart function in a rat cellular cardiomyoplasty model. Circulation 2003;108 (Suppl 1): 253-58.
- Delewi R, Andriessen A, Tijssen JG et al. Impact of intracoronary cell therapy on left ventricular function in the setting of acute myocardial infarction: a meta-analysis of randomised controlled clinical trials. Heart 2013; 99(4): 225-32.
- de Macedo Braga LM, Lacchini S, Schaan BD et al. In situ delivery of bone marrow cells and mesenchymal stem cells improves cardiovascular function in hypertensive rats submitted to myocardial infarction. J Biomed Sci 2008; 15(3): 365-74.
- Ertl G, Frantz S. Healing after myocardial infarction. Cardiovasc Res 2005; 66: 22-32.
- Frangogiannis NG, Entman ML. Chemokines in myocardial ischemia. Trends Cardiovasc Med 2005; 15(5): 163-9.
- Frantz S, Ducharme A, Sawyer D et al. Targeted deletion of caspase-1 reduces early mortality and left ventricular dilatation following myocardial infarction. J Mol Cell Cardiol 2003; 35(6): 685-94.
- Jeevanantham V, Butler M, Saad A et al. Adult bone marrow cell therapy improves survival and induces long-term improvement in cardiac parameters: a systematic review and meta-analysis. Circulation 2012; 126(5): 551-68.
- Jiang M, He B, Zhang Q et al. Randomized controlled tials on the therapeutic effects of adult progenitor cells for myocardial infarction: meta-analysis. Expert Opin Biol Ther 2010; 10(5): 667-80.
- Kahn J, Byk T, Jansson-Sjostrand L et al. Overexpression of CXCR4 on human CD34_ progenitors increases their proliferation, migration, and NOD/SCID repopulation. Blood 2004; 103: 2942-49.
- Kamihata H, Matsubara H, Nishiue T et al. Implantation of bone marrow mononuclear cells into ischemic myocardium enhances collateral perfusion and regional function via side supply of angioblasts, angiogenic ligands, and cytokines. Circulation 2001; 104: 1046-52.
- Landau C, Jacobs AK, Haudenschild CC. Intrapericardial basic fibroblast growth factor induces myocardial angiogenesis in a rabbit model of chronic heart ischemia Am Heart J 1995; 129(5): 924-31.
- Larionov PM, Sergeevichev DS, Chernyavskii AM et al. Angiomatosis and ectopic ossification in the dog myocardium after intramyocardial implantation of autologous bone marrow mononuclears in experimental coronary disease. Bull Exp Biol Med 2009; 147(5): 644-9.
- Li SR, Qi XY, Hu FL et al. Mechanisms of improvement of left ventricle remodeling by transplanting two kinds of autologous bone marrow stem cells in pigs. Chin Med J 2008; 121(23): 2403-9.
- Luttun A, Carmeliet G, Carmeliet P. Vascular progenitors: from biology to treatment.// Trends. Cardiovasc Med 2002; 12: 88-96.
- Matsumoto R, Omura T, Yoshiyama M et al. Vascular endothelial growth factor-expressing mesenchymal stem cell transplantation for the treatment of acute myocardial infarction. Arterioscl Thromb Vasc Biol 2005; 25(6): 1168-73.
- Pagani FD, Baker LS, Hsi C et al. Left ventricular systolic and diastolic dysfunction after infusion of tumor necrosis factor-alpha in conscious dogs. J Clin Invest 1992; 90: 389-98.
- Pittenger MF, Martin BJ, Finkel T, Bolli RE. Mesenchymal stem cells and their potential as cardiac therapeutics. Circ Res 2004; 95(1): 9-20.
- Shake JG, Gruber PJ, Baumgartner WA et al. Mesenchymal stem cell implantation in a swine myocardial infarct model: engraftment and functional effects. Ann Thorac Surg 2002; 73: 1919-26.
- Tang YL. Autologous mesenchymal stem cells for post-ischemic myocardial repair. Meth Mol Med 2005; 112: 183-92.
- Vandervelde S, Luyn MJ, Tio RA et al. Signaling factors in stem cell-mediated repair of infarcted myocardium. Mol Cell Cardiol 2005; 39(2): 363-76.
- van der Spoel TI, Jansen of Lorkeers SJ, Agostoni P et al. Human relevance of pre-clinical studies in stem cell therapy: systematic review and meta-analysis of large animal models of ischaemic heart disease Cardiovasc Res 2011; 91(4): 649-58.
- Waksman R, Fournadjiev J, Baffour R et al. Transepicardial autologous bone marrow-derived mononuclear cell therapy in a porcine infarcted myocardium. Cardiovasc Radiation Med 2004; 5: 125-31.
- Wen Y, Chen B, Wang C et al. Bone marrow-derived mononuclear cell therapy for patients with ischemic heart disease and ischemic heart failure Expert Opin Biol Ther 2012; 12(12): 1563-73.
- Yoon J, Min BG, Kim YH. Differentiation, engraftment and functional effects of pretreated mesenchymal stem cells in a rat myocardial infarct model. Acta Cardiol 2005; 60(3): 277-84.
- Zhang J, Chen J, Liao YH et al. Myocardial inflammation and remodeling driven by cardiac myosin specific-T lymphocytes. J Hong Kong Coll Cardiol 2005; 13(2): 130.
- Zhang H, van Olden C, Sweeney D, Martin-Rendon E. Blood vessel repair and regeneration in the ischaemic heart (review). Open Heart 2014; 1:doi:10.1136/openhrt-2013-000016
- Zhang S, Zhang P, Guo J et al. Enhanced cytoprotection and angiogenesis by bone marrow cell transplantation may contribute to improved ischemic myocardial function. Eur J Cardiothoracic Surg 2004; 25: 188-95.
- Zhang S, Ge J, Sun A et al. Comparison of various kinds of bone marrow stem cells for the repair of infracted myocardium: single clonally purifield non-hematopoietic mesenchymal stem cells serve as a superior source. J Cell Biochem 2006; 99(4): 1132-47.
" ["~DETAIL_TEXT"]=> string(53728) "
Introduction
Myocardial infarction (MI) is a common reason of death and disability worldwide. Over the last decade, different cell therapy options have been tested to improve efficiency of MI treatment, including the s.c. cardiomyoplastics. Various cells are proposed to be used for this purpose. Autologous bone marrow is a widely used source of therapeutic cell preparations, thus providing freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchimal stromal cells (MMSC). Meanwhile, existing works concerning clinical effects of MF and MMSC transplantation in acute MI yield controversial results [6, 11, 16, 24, 26, 29, 31], thus necessitating further studies and getting experience in this area.
The aim of the study
The aim of our experimental study was to compare the effects of intramyocardial MF and MMSC transplantation upon clinical course and outcome of MI, using a rabbit model during prolonged observation terms by using complex of modern functional and morphological study.
Materials and methods
The experiments were performed with male Chinchilla rabbits of 2.8+ 0.2 kg weight, aged 3 - 4 months. All experimental procedures have been carried out in accordance with guidelines of local Ethical Committee at the First St.Petersburg I.Pavlov State Medical University.
Isolation, characterization, and morphological description of bone marrow cells
Bone marrow aspirate (10+ 1mL) was obtained from a rabbit by iliac puncture, following premedication with Droperidol (0.5 mg/kg, Xylasine, 14 mg/kg body mass), and local anesthesia with 0.5 per cent Novocaine, and placed into a tube containing CPDS (citrate phosphate dextrose solution, Terumo, Japan). Mononuclear cell fraction was obtained by means of centrifugation (1600 g, 20 min) Percoll density gradient (63%). Interphase cell fraction containing nucleated cells was washed in Са2+ and Mg2+-free Hanks’ solution (Gibco, USA), and span down by centrifuging. MMSC cell culture was obtained by MF cell passaging in а-МЕМ medium (ICN, USA) with 10 per cent fetal calf serum (Hyclone, New Zealand) supplied with gentamycin sulfate (50 mcg/mL; Invitrogen, Great Britain) in a СО2 incubator, at 5 per cent CO2 and 100% humidity for three weeks. The medium was changed twice a week. Ascorbic acid (ICN, USA) was added at a final concentration of 50 mcg/mL after first medium change. After reaching a semi-confluent state, the cells were reinoculated by means of 0.25% trypsin solution (Gibco, USA), and EDTA (0.02%, Gibco, USA). Before being transplanted, the cultured cells did not display any signs of spontaneous osteogenic differentiation, as evidenced by negative staining for alkaline phosphatase with a standard BCIP-NBT reagent (5-bromine-4-chloride-3-indolyl phosphate/ nitroblue tetrazolium, Sigma, USA), or any features of adipocytic transformation detectable with Sudan III/IV mixture (BDH Chemicals Ltd, Great Britain). Meanwhile, special studies with specific induction of differentiation to osteogenic and adipocytic lineage have shown their multipotency, i.e., the cultivated cells had typical MMSC characteristics.
In some animals, MNC or MMSC were stained prior to transplant with Hoechst nuclear fluorescent dye (Sigma, USA, final concentration of 1 mcg/mL), by shaking for 60 min in a СО2 incubator.
Nucleated marrow cells were counted in Buerker chamber, and their viability was assessed with Trypan Blue solution (Labtech, Russia). The cells labelled with Hoechst dye were detected by their blue nuclear fluorescence upon microscopy, using an «Axioscope» (Zeiss, Germany).
Experimental modelling and treatment of myocardial infarction
The rabbits were subjected to a left-sided thoracotomy under mechanical ventilation of lungs, followed by ligation of anterior descendent left coronary artery at a distance of 1 cm from the heart apex (Fig. 1, A, B). Ten minutes after the coronary occlusion, intramyocardial injections of ME or MMSC suspensions were performed into 6 points of the presumed infarction area, using insulin syringes, at a mean cell number of 2±0.2 x106 in 0.4 mL of а-МЕМ growth medium (modified Eagle medium), or with equivalent volumes of culture medium (placebo treatment), as shown in Fig. 1 C, D. Control animals were not subjected to myocardial injections. Surgical wounds were closed in layers, pneumothorax being eliminated by means of active air aspiration from the pleural cavity. The surviving animals were classified in four groups, each consisting of 13 animals, i.e., Group 1, (controls), Group 2 (placebo-treated), Group 3 (MMSC injections), and Group 4 (MF injections). Subgroups of ten animals were observed for 1 year after the surgery.




Figure 1. Modelling and treatment of myocardial infarction in rabbits: А – ligation of left anterior descendent coronary artery, B – a view of surgical area, C – topography of intramyocardial injections of marrow cells into the infarcted area; D – a view of surgical area
Detection of labelled cells in the myocardium
Twenty days after the surgical intervention, the subgroups of three rabbits from Groups 3 and 4 (subjected to myocardial injections) were sacrificed (this term was limited by the life-span of detectable fluorochrome in the cells). The hearts were teased in two parts (basal and apical), in order to get sections at the level of arterial ligature perpendicular to long axis of the heart. Apical part of the heart was pulped and treated with trypsin-collagenase enzyme mixture (Sigma, USA). The dissociated cells were collected by centrifugation, placed onto the microscopic slide, and the proportion of labeled cells have been counted.
Electrocardiography (ECG)
ECG was carried out in all animals before surgery, at the days +3, +7, +30, and one year after surgery.The results were evaluated by the 2nd standard lead on an ECG.
Heart ultrasonography
EchoCG was performed with a Sequoia 512 echocardiograph (Acuson, USA), using a linear 13 MGz transducer, according to a standard detection technique. EchoCG was performed in all cases before the surgery, at day +14, and 1 year after the surgery. The procedure was carried out in parallel with ECG recording. The end-diastolic size of left ventricle was registered in M-scanning regimen (EDSLV, mm). Left ventricular systolic function was registered by means of 2D scanning, from the apical access, in four-chamber and two-chamber positions. EF percentage calculations were made by means of a modified Simpson disc method, using the built-in software of the sonographic device .Aortal blood flow velocity was evaluated at the level of aortal valve (VAo, m/sec), using impulse-wave Doppler sonography. Dynamic features of the left ventricular wall were also studied in intervention/ infarction area, e.g., dyskinesia, hypokinesia, akinesia, calcification, or ossification in the areas of transplantation.
Myocardial perfusion evaluation
Perfusion rates were assessed with SPECT technique, using radiopharmaceutical tracer (RP) Myoview (Nycomed, Great Britain) labelled with Tc-99m. RP was injected, at a single dose of 30-50 MBq, into marginal ear vein via a peripheral catheter. 10 to 15 min after injection, a SPECT evaluation was performed by double-detector gamma chamber E.Cam. var (Siemens, Germany). To get quantitative values for myocardial perfusion rates, a ratio of mean RP accumulation in damaged versus reference areas was calculated in every case, as arbitrary units (Fig. 2). Uniformity of perfusion was determined as a minimum-to-maximum ratios (in pixels) for damaged and reference areas. The study was performed before surgical intervention, at day +10, and at 1,5, 6, and 12 months after surgery in all groups of animals.

Figure 2. SPECT visualization of left heart ventricle of rabbit. А, transverse heart projection at the level of ligated left anterior descendent coronary artery; B, a sketch of left ventricle with designation of its walls and localization of damaged and reference areas; C, perfusion SPECT tomography of the left ventricle of rabbit, with indication of reference zone (non-damaged myocardium area) and pathological zone (infarction localization area)
Sizing of infarcted area, LV dilatation measurements, histological studies
Dimensions of an experimental IM were determined by means of 2,3,5-triphenyltetrazolium chloride (TTC) staining of the heart sections, thus allowing to discern irreversibly damaged myocardial tissue from viable myocardium. Moreover, a routine histological evaluation was performed. All the animals surviving for 12 months post-surgery were subjected to euthanasia, followed by immediate heart extraction. The organ was rinsed in physiological saline and sectioned transversally with a special device below the ligature level into three segments of equal thickness, i.e., apical (1), middle (2), and basal sections (3), as shown in Fig. 3А.

Figure 3. A scheme of residual myocardial damage
assessment at 12 months post-treatment. А, sectioning of damaged myocardial area into three segments (apical, middle and basal); В, evaluation of post-infarction myocardial scarring by means of 1,3,5-TTC staining. Abbreviations: LV, left ventricle; RV, right heart ventricle.
In a half of all animals, the heart segments were then placed to 1% solution of TTC (ICN, USA) for 15 min. at 37ºC, pH 7.4. After development of bright-red color in viable myocardium, the stained heart segments were photographed by digital camera (Olimpus 2020, Japan), and the images were stored and processed by Adobe Photoshop CS2 software (Fig. 3В). For the second half of animals, the heart sections were fixed in 10% formaldehyde solution for 4 days followed by mounting in paraffin and preparing 7-mcm slices, using a routine technique. The histological samples were stained by HE (hematoxylin and eosin) and Mallory dye, thus allowing of discerning various types of connective tissues. Histological examinations were performed with a “BioLam” microscope (Russia). A grade of left ventricular dilatation (LV dilatation index) was determined as a ratio of LV lumen in TTC-positive heart segments to myocardial tissue area in both ventricles. This arbitrary index was calculated for each of three segments, and a mean value was then derived.
Quantitative evaluation of vascularization in damaged myocardial area
We have examined the borderline areas adjacent to the myocardial scars. Each tissue specimen was routinely stained by Mallory, and five consequent microscopic fields were evaluated at a 400x magnification. We performed separate counts of regulated-type vessels, i.e., arterioles, capillaries, venules, as well as non-regulated type-sinusoids, followed by calculating a mean blood vessel number per microscopic field.
Safety evaluation of approaches for angiogenesis stimulation in ischemic myocardium
To assess safety of cell transplantation in the studied groups of animals, we compared some general parameters, e.g., intra- and post-surgical mortality, incidence of arrhythmia and septic/inflammatory complications early after surgery. Condition of heart and internal organs was macroscopically evaluated by pathoanathomical obduction data, looking for occurrence of neoplastic processes, and microscopically evaluated for presence of local pathological changes in the areas of cell injections, in particular, atypically differentiated cells, focal sclerosis, or osteogenesis.
Statistical processing
We used SPSS software for statistical data processing. With small number of observations, the significance of differences was determined by a non-parametric Wilcoxon-Mann-Whitney criterion. All the data were presented as means + SD. The differences by P values of <0.05 were regarded as significant.
Results
Detection of labeled cells in damaged myocardium
Twenty days after treatment, both MFs and MMSCs were detectable as fluorescent cells, at, resp., 13+2% and 11+3% of initial numbers (Fig. 4).

Figure 4. ECG dynamics in studied groups
ECG dynamics in different experimetal groups
All the animals subjected to experimental coronary occlusion, developed typical ECG features of acute MI with distinct typical dynamics. However, all animals from control (placebo-treated), or MF-transplanted groups exhibited ECG signs of transmural MI, whereas MMSCs-transplant animals displayed only subendocardial myocardial damage (Fig. 5). Heart rate disturbances (atrial extrasystoles) in early postoperative period were developing with similar frequency (65%) in all the groups under study, except for MMSC-transplanted animals that showed them 3 times less often (20%). Twelve months after surgery, ECG patterns in MMSC-treated animals returned to the initial state, as compared with scar changes in ECG observed in MF-treated animals (Fig. 5)

Descriptions: MI-associated perfusion defects are shown by arrows; colour scale shows grade of myocardial perfusion from minimal to maximal values.
Figure 5. Typical changes on perfusion tomoscyntigraphy of myocardium in the groups under study, according to SPECT data before surgery, 1.5, and 12 months after surgery.
Initial EchoCG parameters did not differ between the groups under study. After the surgical intervention (coronary occlusion), a significant increase of EDSLV was observed, along with diminished EF, VAo. However, these disruptions were dissimilar for different groups, i.e., minimal for MMSC-treated animals and maximal for MNC-treated animals (Table 1, Fig. 6, 7). One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all cardiological parameters (p<0,05), absence of akinetic areas, that sufficiently differed from appropriate parameters in other groups. In controls and placebo group, the disturbances were long-standing, and a small akinetic area was formed in the apical segment. The most negative changes were detected among animals transplanted with MNC, which revealed drastic decrease in LV systolic function, increased LV size, development of extended akinetic areas, as compared with group 3, controls, and placebo group (p<0,05) (Table 1, Fig. 6, 7).
|
Groups |
Parameters and terms of the study |
||||||||
|
EF,% |
EDSLV, mm |
V Ao, m/sec |
|||||||
|
Initial values |
14 days after surgery |
12 months after surgery |
Initial values |
14 days after surgery |
12 months after surgery |
Initial values |
14 days after surgery |
12 months after |
|
|
№1 (controls) |
62.2±4.6 |
45.8±6.1 |
46.5±6.4 |
14.4±1.0 |
17.0±1.4 |
16.9±0.8 |
95±4 |
57±6 |
71±4 |
|
№2 (placebo) |
64.9±4.3 |
46.7±3.5 |
48.7±3.9 |
14.1±0.4 |
16.8±1.2 |
16.6±0.8 |
94±3 |
58±6 |
73±6 |
|
№3 (MMSC) |
61.7±4.0 |
53.1±4.8 |
58.2±3.1* |
14.7±0.9 |
15.2±0.7 |
14.9*±1.2 |
96±4 |
81±6 |
89±4* |
|
№4 (MNC) |
59.7±3.2 |
38.8±2.9 |
28.7*±4.1 |
14.9±1.2 |
17.9±0.8 |
19.8*±0.9 |
97±5 |
55±4 |
45±3* |
Abbreviations: LVEF, LV ejection fraction; EDSLV, end LV diastolic size; V Ao- blood flow velocity in ascending aorta; *, differences from control group are significant by p<0,05.
Table 1. Dynamics of LV systolic parameters from EchoCG data (M±m)

Figure 6. Transverse sections (1, apical; 2, median; 3, basal) from infarcted area of the heart wall in different experimental groups (Mallory staining) 12 months after MI modeling/ treatment
Dynamics of myocardial perfusion in the groups under study.
Cumulative findings concerning dynamics of myocardial perfusion in damaged areas are presented in Table 2. Before surgery, the perfusion parameters in all groups were within reference ranges. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, this decrease varied in different groups of animals, i.e., animals treated with MMSC or MNC showed less impaired perfusion rates than in control or placebo groups (p<0,05). At 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged area of myocardium in groups 3 and 4, reaching the pre-surgical rates by 3 months, in group 3 to a greater extent, without subsequent dynamics. In controls and placebo-treated group, the altered perfusion rates remained at similar levels at all the terms of observation.

Figure 7. Numbers of regulated vs. sinusoid-type microvessels per a space unit of MI area 12 months after modelling and treatment in compared groups of experimental animals.
Ordinate, number of microvessels per a IM space unit; abscissa, groups under study.
|
Groups |
TTC accumulation in damaged area (arb.un.), terms of study |
||||
|
Before surgery |
10 days after surgery |
1.5 months after surgery |
6 months after surgery |
12 months after surgery |
|
|
Controls |
1.01±0.01 |
0.57±0.02 |
0.59±0.04 |
0.61±0.02 |
0.61±0.04 |
|
Placebo |
1.01±0,02 |
0.59±0.02 |
0.62±0.02 |
0.64±0.04 |
0.61±0.03 |
|
MMSC |
0.98±0.03 |
0.81±0.01 * |
0.92±0.03 * |
0.98±0.02 * |
1.02±0.01* |
|
MF |
1,00±0.01 |
0.75±0.03 * |
0.89±0.03 * |
0.98±0.03 * |
0.99±0.01* |
Descriptions: arb.units = mean rates of TTC accumulation in damaged area/ mean values of TTC accumulation in reference area;
*- significance of differences as compared to control group (p<0.05)
Table 2. Dynamics of TTC accumulation in damaged myocardial area after treatment of acute MI in the groups under study by perfusion data (SPECT evaluation, M±m).
Morphometric heart studies
12 months after experimental MI modeling/ treatment, general macroscopic appearance of rabbit hearts was similar for control and placebo-treated groups, i.e., enlarged heart size, as compared to healthy hearts (intact animals), along with apical aneurism of LV. Distinct scarring of LV anterior wall was evident for the hearts from MMSC-treated animals, however, without evolving aneurysm, and without sufficient increase of the heart size. Heart dimensions among MF-treated animals did significantly exceed normal size, and appropriate heart parameters of healthy rabbits, and the animals from groups 1,2, and 3. The animals transplanted with MF had extendsive aneurysms at the apex and anterior wall of LV (Fig. 9,10,11). Scarring area and LV dilatation index for control group were, resp., 20.2±1.9%, and 0.19±0.02; 20,8±1.6% and 0.18±0.03 for placebo group; 35.8±1.6% and 0.34±0.03 for MF-transplanted group,. The animals treated with MMSCs exhibited the best characteristics, i.e., 6.0±2.6% and 0.11±0.02 (Fig. 12).
Histological pattern of myocardium
It was shown that intramyocardial MMSC vs. MF transplantation resulted, after 12 months, in the development of principally different heart morphology as compared to control or placebo groups of animals. After MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles.
Quantitative myocardial vascularization
12 months after MI modeling/treatment, a significant difference was revealed in vascularization patterns of damaged myocardium in the studied groups, i.e., the total microvessel numbers per 1 microscopic field were, resp., 15±3, 13+3, 7±1 and 6±2 for groups treated with MMSCs, MFs, controls and placebo-treated animals. After intramyocardial autotransplantation of bone marrow, the microvessel density in the area was not only increased over controls or placebo groups (p<0.05), but it exhibited a distinct type of microvessels showing a regulated type-wall, whereas control group recovered with development of sinusoid-type microvessels.
Safety evaluation of neoangiogenesis stimulation in ischemic myocardium
Intra- and post-operative mortality in all the studied groups did not significantly differ (a mean of 10±3% и 10±4%). Incidence of septic and inflammatory complications in the intervention area was, in general, significantly lower (p<0.05) among intramyocardially cell-treated animals (1) than in control or placebo group (3). No differences were here noted between MF and MMSC-treated groups. At macroscopic examination one year after surgical intervention, both groups of cell-treated animals did not show any signs of malignant neoplasia. Local examination of myocardium at the locations of cell injections did not reveal any cells with atypical differentiation (osteogenic or chondrogenic tissues).
Discussion
Rabbit model of myocardial infarction induced by ligation of anterior descendent left coronary artery proved to be a convenient and demonstrative technique for evaluation of therapeutic angiogenesis, testing the effects of vascular growth factors and cellular therapy [14]. The results obtained in present study have shown that intramyocardial transplantation of autologous bone marrow cells (MF versus MMSC) into the MI area in rabbits during acute period may considerably change the natural process of MI development and exerts different morpho-functional effects upon the damaged tissues.
MMSC transplantation, as compared to controls and placebo, was associated with definite reduction of the myocardial damage, and later (12 months after MI) this group of animals exhibited normalization of heart systolic function, ECG, myocardial perfusion. Meanwhile, upon morphological examination, the infracted area was represented by fine focal cardiosclerosis, without aneurism formation. The detected changes might have been caused by paracrine effect of transplanted cells and, probably, by their differentiation into various myocardial structures. At the first phase of MI characterized by death of the cardiomyocytes, the transplanted MMSC are able to inhibit apoptosis and produce a cytoprotective effect, thus allowing cardiomyocytes and transplanted cells to survive the ischemic state [6,16,30]. Moreover, the detected changes might be associated with changing degree of inflammatory response, due to effect of the transplant upon the cytokine profile. In the course of inflammation caused by ischemic damage of myocardium, there are two cytokine groups: pro-inflammatory factors (interleukin-1α, 1ß, 6, 8, tumor necrosis factor-α, ß and others) mostly secreted by macrophages and neutrophils, and anti-inflammatory molecules (interleukin-4, 10, transforming growth factor-β and others), mainly released by lymphocytes, monocytes and macrophages. It was shown in vitro that bone marrow MMSC, along with anti-inflammatory cytokines (interleukin-1α, 1ß, 6, 7, 8, tumor necrosis factor-α, ß) produce a broad spectrum of anti-inflammatory cytokines (interleukin-4, 10, transforming growth factor-β), as well as specific receptors for interleukin-1α, 1ß, 1, 3, 4, 6, 7, 8, tumor necrosis factor-α, ß [22]. Moreover, it has been shown that the bone marrow MMSC secrete different chemokines: MCP-1, RANTES, MIP-1alpha [23]. Most probably, such cytokine profile may induce significant populational changes, e.g., quantitative increase of macrophages, lymphocytes and monocytes that are able to secrete anti-inflammatory cytokines. This mechanism allows to reduce the degree of inflammatory response and the damaged area.
Progression of the small-focal myocardial infarction and normalization of systolic functions after BM MMSC transplantation, as shown in our study, can be also explained by potential ability of transplanted cells to differentiate into cardiomyocytes. However, an opportunity of BM MMSCs differentiation into cardiomyocites remains problematic. Most researchers note the ability of bone marrow MMSC to acquire cardiomyocyte-like phenotypes after transplantation into the damaged myocardium, as shown by synthesis of α-actinin, troponin-Т, tropomyosin. However, they have not revealed developing intercellular structures and/or contractile functions [20, 21, 27].
Thus, the changes in myocardial morphology and function after MMSC transplantation may be caused by their cytoprotective activity and ability to reduce the inflammatory response during acute infarction phase. By the contrary, intramyocardial MF transplantation, as compared to control and placebo groups, caused alterations of myocardial contractile function, expanding damage area, resulting into significant left ventricular fibroid aneurysms. Such effect is probably determined by MF ability to intensify inflammatory response, due to changing quantitative and qualitative cytokine profile in the damaged area, following direct massive injections of leukocytes. The bone marrow MFs constitute a heterogeneous population, containing mesenchymal stromal cells, hematopoietic stem cells, progenitor endothelial cells, as well as myeloid and lymphoid cells at different stages of maturation. There is an abundance of mature leukocytes among the bone marrow MF. Apparently, upon entering the ischemic myocardium, the MF start to release a variety of proteolytic enzymes and anti-inflammatory cytokines which attract blood cells to the altered areas, thus intensifying the inflammatory response [8]. The key point of myocardial repair is based on equilibrium between extracellular matrix degradation (needed for cell migration), and its resynthesis by the cells migrating to the damaged area. The proteolytic enzymes released by MF lyse intercellular collagen links and activate matrix metalloproteinases. Extracellular matrix degradation and expansion of infarcted area are caused by a cascade of proteolytic reactions. Moreover, the matrix metalloproteinases are also activated by some cytokines, e.g., as interleukin-1ß и tumor necrosis factor-α, ß [9, 19].
G. Ertl, S. Frantz have shown that dilatation of left ventricle and mortality were less expressed in the mice deficient for interleukin-1ß than in animals with normal cytokine levels [7]. In addition, proteolytic enzymes released by transplanted MF of bone marrow induce massive death of cardiomyocytes. Cardiac myosin released from necrotized myocardium is a proven potent autoantigen. The autoimmune reactions occur via activation of T lymphocytes followed by the secondary T-cell induced damage of cardiomyocytes and altered remodeling of extracellular matrix [2, 28].
Thus, morphological and functional changes revealed in myocardium after bone marrow MF injections may be caused by excessive intensification of inflammatory response during the hyperacute phase of MI.
The results of our study indicate that intramyocardial transplantation of MMSC and MF of bone marrow leads to increased vascularization of damage area. We assume that the angiogenic effect of these cells is accomplished by secretion of vascular growth factors and, probably, by differentiation of transplanted cells into cellular components of the vascular wall.
MMSCs are able to secrete angiogenic factors, such as VEGF (vascular endothelial growth factor), bFGF (basic fibroblast growth factor), HGF (hepatocyte growth factor), TGF-ß (transforming growth factor), angiopoietin-1 [13, 19]. Tang et al. (2005) demonstrated that the BM MMSC transplantation into the ischemic myocardium results into secretion of cytokine SDF-1 (stromal cell derived factor-1), which is a chemoattractant for endothelial cell progenitors and hematopoietic stem cells [22]. Progenitor endothelial cells migrating from peripheral blood into the damaged area are able to transform into mature endothelial cells and participate in angiogenesis [4, 12, 17]. Another mechanism of MMSCs involvement in post-transplant neoangiogenesis in myocardium is connected with their ability to differentiate into endothelial cells, smooth muscle cells, pericytes, fibroblasts that subsequently become components of the vascular wall, as shown in several studies [4,22].
Involvement of bone marrow MF in angiogenesis, according to the literature data, is regulated by several mechanisms. First of all, the MF populations, e.g., mesenchymal stromal cells, hematopoietic stem cells, progenitor endothelial cells, as well as immature cells of myeloid and lymphoid series, are secreting various angiogenic factors (VEGF, bFGF, TGF-ß, PDGF, angiopoietin-1, which stimulate proliferation of vascular endothelium and endothelial progenitors of damaged myocardium [13,25, 30, 31]. Secondly, the MF cells are able to secrete SDF-1 (stromal cell derived factor-1), which is a chemoattractant for progenitor endothelial cells and hematopoietic stem cells [20]. Thirdly, such mesenchymal stromal cells within the MF fraction are able to differentiate into endothelial cells and other vascular structures [22].
Our data differ from other studies that did not show such significant differences after MF and MMSC transplantation to the experimental MI area [6,13,16,21,25,27,31]. A probable explanation is that transplantation of bone marrow cells in these studies was performed either in later terms following MI, or the cells were administered by a different route, e.g., via coronary arteries, or intravenously [1,3,5,10,24,29]. A prolonged observation in our study did not register such complications as ossification or formation of angiomas in the cell transplantation area, as previously described [15], neither any neoplastic processes have been registered.
Conclusions
1. Local intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit, when performed in acute phase of experimental MI, was accompanied by changes in the MI development and resulted into different morphofunctional outcomes. I.e., transplantation of mesenchymal stem cells exerted a pronounced therapeutic effect, causing reduction of myocardial damage area and improvement of systolic functional indices. On the contrary, mononuclear cell transplantation produced negative effects, causing expansion of the damaged area and impairment of systolic indices.
2. Both MMSC and MF intramyocardial transplantation display stimulation of neoangiogenesis and improvement of perfusion in the infarcted area.
Conflict of interest
All the authors have no conflict of interest to declare.
References
- Chen Y, Teng X, Chen W et al. Timing of transplantation of autologous bone marrow derived mesenchymal stem cells for treating myocardial infarction. Sci China Life Sci 2014; 57(2): 195-200.
- Cheng X, Liao YH, Li B et al. Changes of rat lymphocyte proliferation and cytotoxic activity after acute myocardial infarction in vitro. Chin J Pathophysiol 2005; 21(9): 1848–50.
- Clifford DM, Fisher SA, Brunskill SJ et al. Long-term effects of autologous bone marrow stem cell treatment in acute myocardial infarction: factors that may influence outcomes. PLoS ONE 2012; 7(5): е37373.
- Davani S, Marandin A, Mersin N et al. Mesenchymal progenitor cells differentiate into an endothelial phenotype, enhance vascular density, and improve heart function in a rat cellular cardiomyoplasty model. Circulation 2003;108 (Suppl 1): 253-58.
- Delewi R, Andriessen A, Tijssen JG et al. Impact of intracoronary cell therapy on left ventricular function in the setting of acute myocardial infarction: a meta-analysis of randomised controlled clinical trials. Heart 2013; 99(4): 225-32.
- de Macedo Braga LM, Lacchini S, Schaan BD et al. In situ delivery of bone marrow cells and mesenchymal stem cells improves cardiovascular function in hypertensive rats submitted to myocardial infarction. J Biomed Sci 2008; 15(3): 365-74.
- Ertl G, Frantz S. Healing after myocardial infarction. Cardiovasc Res 2005; 66: 22-32.
- Frangogiannis NG, Entman ML. Chemokines in myocardial ischemia. Trends Cardiovasc Med 2005; 15(5): 163-9.
- Frantz S, Ducharme A, Sawyer D et al. Targeted deletion of caspase-1 reduces early mortality and left ventricular dilatation following myocardial infarction. J Mol Cell Cardiol 2003; 35(6): 685-94.
- Jeevanantham V, Butler M, Saad A et al. Adult bone marrow cell therapy improves survival and induces long-term improvement in cardiac parameters: a systematic review and meta-analysis. Circulation 2012; 126(5): 551-68.
- Jiang M, He B, Zhang Q et al. Randomized controlled tials on the therapeutic effects of adult progenitor cells for myocardial infarction: meta-analysis. Expert Opin Biol Ther 2010; 10(5): 667-80.
- Kahn J, Byk T, Jansson-Sjostrand L et al. Overexpression of CXCR4 on human CD34_ progenitors increases their proliferation, migration, and NOD/SCID repopulation. Blood 2004; 103: 2942-49.
- Kamihata H, Matsubara H, Nishiue T et al. Implantation of bone marrow mononuclear cells into ischemic myocardium enhances collateral perfusion and regional function via side supply of angioblasts, angiogenic ligands, and cytokines. Circulation 2001; 104: 1046-52.
- Landau C, Jacobs AK, Haudenschild CC. Intrapericardial basic fibroblast growth factor induces myocardial angiogenesis in a rabbit model of chronic heart ischemia Am Heart J 1995; 129(5): 924-31.
- Larionov PM, Sergeevichev DS, Chernyavskii AM et al. Angiomatosis and ectopic ossification in the dog myocardium after intramyocardial implantation of autologous bone marrow mononuclears in experimental coronary disease. Bull Exp Biol Med 2009; 147(5): 644-9.
- Li SR, Qi XY, Hu FL et al. Mechanisms of improvement of left ventricle remodeling by transplanting two kinds of autologous bone marrow stem cells in pigs. Chin Med J 2008; 121(23): 2403-9.
- Luttun A, Carmeliet G, Carmeliet P. Vascular progenitors: from biology to treatment.// Trends. Cardiovasc Med 2002; 12: 88-96.
- Matsumoto R, Omura T, Yoshiyama M et al. Vascular endothelial growth factor-expressing mesenchymal stem cell transplantation for the treatment of acute myocardial infarction. Arterioscl Thromb Vasc Biol 2005; 25(6): 1168-73.
- Pagani FD, Baker LS, Hsi C et al. Left ventricular systolic and diastolic dysfunction after infusion of tumor necrosis factor-alpha in conscious dogs. J Clin Invest 1992; 90: 389-98.
- Pittenger MF, Martin BJ, Finkel T, Bolli RE. Mesenchymal stem cells and their potential as cardiac therapeutics. Circ Res 2004; 95(1): 9-20.
- Shake JG, Gruber PJ, Baumgartner WA et al. Mesenchymal stem cell implantation in a swine myocardial infarct model: engraftment and functional effects. Ann Thorac Surg 2002; 73: 1919-26.
- Tang YL. Autologous mesenchymal stem cells for post-ischemic myocardial repair. Meth Mol Med 2005; 112: 183-92.
- Vandervelde S, Luyn MJ, Tio RA et al. Signaling factors in stem cell-mediated repair of infarcted myocardium. Mol Cell Cardiol 2005; 39(2): 363-76.
- van der Spoel TI, Jansen of Lorkeers SJ, Agostoni P et al. Human relevance of pre-clinical studies in stem cell therapy: systematic review and meta-analysis of large animal models of ischaemic heart disease Cardiovasc Res 2011; 91(4): 649-58.
- Waksman R, Fournadjiev J, Baffour R et al. Transepicardial autologous bone marrow-derived mononuclear cell therapy in a porcine infarcted myocardium. Cardiovasc Radiation Med 2004; 5: 125-31.
- Wen Y, Chen B, Wang C et al. Bone marrow-derived mononuclear cell therapy for patients with ischemic heart disease and ischemic heart failure Expert Opin Biol Ther 2012; 12(12): 1563-73.
- Yoon J, Min BG, Kim YH. Differentiation, engraftment and functional effects of pretreated mesenchymal stem cells in a rat myocardial infarct model. Acta Cardiol 2005; 60(3): 277-84.
- Zhang J, Chen J, Liao YH et al. Myocardial inflammation and remodeling driven by cardiac myosin specific-T lymphocytes. J Hong Kong Coll Cardiol 2005; 13(2): 130.
- Zhang H, van Olden C, Sweeney D, Martin-Rendon E. Blood vessel repair and regeneration in the ischaemic heart (review). Open Heart 2014; 1:doi:10.1136/openhrt-2013-000016
- Zhang S, Zhang P, Guo J et al. Enhanced cytoprotection and angiogenesis by bone marrow cell transplantation may contribute to improved ischemic myocardial function. Eur J Cardiothoracic Surg 2004; 25: 188-95.
- Zhang S, Ge J, Sun A et al. Comparison of various kinds of bone marrow stem cells for the repair of infracted myocardium: single clonally purifield non-hematopoietic mesenchymal stem cells serve as a superior source. J Cell Biochem 2006; 99(4): 1132-47.
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "700" ["~SORT"]=> string(3) "700" ["CODE"]=> string(26) "1866-8836-2015-4-1-2-47-57" ["~CODE"]=> string(26) "1866-8836-2015-4-1-2-47-57" ["EXTERNAL_ID"]=> string(2) "86" ["~EXTERNAL_ID"]=> string(2) "86" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["ELEMENT_META_KEYWORDS"]=> string(290) "инфаркт миокарда, экспериментальный костный мозг мононуклеарные клетки мезенхимные стволовые клетки терапевтические инъекции функции миокарда, гистология" ["ELEMENT_META_DESCRIPTION"]=> string(451) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликовComparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(6788) "<h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8<span class="CharOverride-12">+</span>0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами. </p> <p class="Summery_H">Результаты</p> <p class="Summery_Rus" lang="ru-RU">Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков. </p> <p class="Summery_H">Заключение</p> <p class="Summery_Rus" lang="ru-RU">Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов. </p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_META_TITLE"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_META_KEYWORDS"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_META_DESCRIPTION"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_PICTURE_FILE_ALT"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_PICTURE_FILE_TITLE"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_PICTURE_FILE_NAME"]=> string(100) "sravnitelnye-effekty-vnutrimiokardialnoy-autotransplantatsii-razlichnykh-vidov-kletok-kostnogo-mozga" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(299) "Сравнительные эффекты внутримиокардиальной аутотрансплантации различных видов клеток костного мозга на исходы экспериментального инфаркта миокарда у кроликов" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(100) "sravnitelnye-effekty-vnutrimiokardialnoy-autotransplantatsii-razlichnykh-vidov-kletok-kostnogo-mozga" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(100) "sravnitelnye-effekty-vnutrimiokardialnoy-autotransplantatsii-razlichnykh-vidov-kletok-kostnogo-mozga" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(100) "sravnitelnye-effekty-vnutrimiokardialnoy-autotransplantatsii-razlichnykh-vidov-kletok-kostnogo-mozga" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(1) "2" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(6) { [0]=> string(4) "1227" [1]=> string(4) "1228" [2]=> string(4) "1229" [3]=> string(4) "1230" [4]=> string(4) "1231" [5]=> string(4) "1232" } ["VALUE"]=> array(6) { [0]=> string(2) "80" [1]=> string(2) "81" [2]=> string(2) "82" [3]=> string(2) "83" [4]=> string(2) "84" [5]=> string(2) "85" } ["DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(6) { [0]=> string(2) "80" [1]=> string(2) "81" [2]=> string(2) "82" [3]=> string(2) "83" [4]=> string(2) "84" [5]=> string(2) "85" } ["~DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "466" ["VALUE"]=> string(19) "06.04.2015 15:21:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "06.04.2015 15:21:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "467" ["VALUE"]=> string(19) "02.07.2015 15:21:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "02.07.2015 15:21:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "894" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "468" ["VALUE"]=> string(2) "73" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "73" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(7) { [0]=> string(3) "469" [1]=> string(3) "470" [2]=> string(3) "471" [3]=> string(3) "472" [4]=> string(3) "473" [5]=> string(3) "474" [6]=> string(3) "475" } ["VALUE"]=> array(7) { [0]=> string(2) "79" [1]=> string(2) "77" [2]=> string(2) "74" [3]=> string(2) "78" [4]=> string(2) "76" [5]=> string(2) "75" [6]=> string(2) "73" } ["DESCRIPTION"]=> array(7) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(7) { [0]=> string(2) "79" [1]=> string(2) "77" [2]=> string(2) "74" [3]=> string(2) "78" [4]=> string(2) "76" [5]=> string(2) "75" [6]=> string(2) "73" } ["~DESCRIPTION"]=> array(7) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "476" ["VALUE"]=> array(2) { ["TEXT"]=> string(452) "<p class="Autor">Владимир В. Давыденко<sup>1</sup>, Андрей А. Матюков<sup>1</sup>, Тимур Д. Власов<sup>1</sup>, Наталия В. Цупкина<sup>2</sup>, Анатолий Н. Ялфимов<sup>3</sup>, Георгий П. Пинаев<sup>2</sup>, Халида К. Аминева<sup>1</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(346) "
Владимир В. Давыденко1, Андрей А. Матюков1, Тимур Д. Власов1, Наталия В. Цупкина2, Анатолий Н. Ялфимов3, Георгий П. Пинаев2, Халида К. Аминева1
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "477" ["VALUE"]=> array(2) { ["TEXT"]=> string(651) "<p class="Autor_place_work-Rus"><sup>1</sup>Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова</p> <p class="Autor_place_work-Rus"><sup>2</sup>Институт цитологии Российской Академии наук, Санкт-Петербург</p> <p class="Autor_place_work-Rus"><sup>3</sup>Российский центр радиологии и хирургических технологий, Санкт-Петербург</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(549) "1Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова
2Институт цитологии Российской Академии наук, Санкт-Петербург
3Российский центр радиологии и хирургических технологий, Санкт-Петербург
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "478" ["VALUE"]=> array(2) { ["TEXT"]=> string(6788) "<h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8<span class="CharOverride-12">+</span>0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами. </p> <p class="Summery_H">Результаты</p> <p class="Summery_Rus" lang="ru-RU">Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков. </p> <p class="Summery_H">Заключение</p> <p class="Summery_Rus" lang="ru-RU">Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(6602) "Резюме
Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8+0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами.
Результаты
Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков.
Заключение
Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "479" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-47-57" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-47-57" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "480" ["VALUE"]=> array(2) { ["TEXT"]=> string(360) "<p class="Autor">Vladimir V. Davydenko<sup>1</sup>, Andrey A. Matyukov<sup>1</sup>, Timur D. Vlasov<sup>1</sup>, Natalya V. Tsupkina<sup>2</sup>, Anatoly N. Yalfimov<sup>3</sup>, <br>Georgy P. Pinaev<sup>2</sup>, Khalida K. Amineva<sup>1</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(248) "Vladimir V. Davydenko1, Andrey A. Matyukov1, Timur D. Vlasov1, Natalya V. Tsupkina2, Anatoly N. Yalfimov3,
Georgy P. Pinaev2, Khalida K. Amineva1
1FirstSt.Petersburg State I.Pavlov Medical University
2Institute of Cytology, Russian Academy of Sciences, St.Petersburg
3Russian Center of Radiology and Surgical Technologies, St.Petersburg
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "482" ["VALUE"]=> array(2) { ["TEXT"]=> string(3700) "<h2>Summary</h2><p class="Summery">Over the last decade, different cell therapy options have been tested to improve treatment of myocardial infarction (MI), including cardiomyoplastics. Autologous bone marrow is a widely used source of therapeutic cell preparations, i.e., freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchymal stromal cells (MMSC). The aim of our pilot study was to compare short- and long-term consequences of intramyocardial MF and MMSC transplantation upon clinical course and outcome of experimental MI. Materials and methods: The experiments were performed with male Chinchilla rabbits of 2.8<span class="CharOverride-12">+</span>0.2 kg weight. MI was modelled by ligation of anterior descendent left coronary artery. Mononuclear cell fraction was obtained from the bone marrow aspirate. MMSC cell culture was grown by MF cell passages in МЕМ medium with 10% fetal calf serum. Intramyocardial injections of MF or MMSC suspensions were performed into 6 points of the infarcted area. The surviving animals were divided in four groups, each consisting of 13 rabbits: group 1 (controls), group 2 (placebo-treated), group 3 (MMSC injections), and group 4 (MF injections). Electrocardiography (ECG) and echo-cardiography were carried out in all animals before surgery, during 1 mo and 1 year after surgery. Myocardial perfusion rates were assessed with SPECT technique. IM dimensions (perfusion areas) were determined by means of staining heart sections with 2,3,5-TTC. Routine histology of myocardial sections was also performed. Vascularization rates of different myocardial areas were assessed in similar way. </p> <p class="Summery_H">Results</p> <p class="Summery">Intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit experimental MI during the acute phase has changed natural process development and resulted in principally different morpho-functional outcomes. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, the animals, treated with MMSC or MF showed less impaired perfusion rates than in control or placebo groups (p<0.05). 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged myocardium in MMSC and MF-treated groups. These changes were confirmed by perfusion tomoscyntigraphy of myocardium at 1.5 and 12 months after surgery. Histological studies have shown that, after MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles. One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all functional parameters (LV ejection fraction; EDSLV, end LV diastolic size; blood flow rates in ascending aorta) at 12 months post-surgery (p<0.05), and absence of akinetic areas. </p> <p class="Summery_H">Conclusions </p> <p class="Summery">MMSC injections were associated with pronounced therapeutic effect, by reducing myocardium damage area. By the contrary, MF transplantation showed a negative effect, expanding myocardium damage area and impairing systolic function indices. Both MMSC and MF intramyocardial transplantation display neoangiogenesis stimulation and perfusion improvement in rabbit experimental infarction area. </p> " ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3544) "Summary
Over the last decade, different cell therapy options have been tested to improve treatment of myocardial infarction (MI), including cardiomyoplastics. Autologous bone marrow is a widely used source of therapeutic cell preparations, i.e., freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchymal stromal cells (MMSC). The aim of our pilot study was to compare short- and long-term consequences of intramyocardial MF and MMSC transplantation upon clinical course and outcome of experimental MI. Materials and methods: The experiments were performed with male Chinchilla rabbits of 2.8+0.2 kg weight. MI was modelled by ligation of anterior descendent left coronary artery. Mononuclear cell fraction was obtained from the bone marrow aspirate. MMSC cell culture was grown by MF cell passages in МЕМ medium with 10% fetal calf serum. Intramyocardial injections of MF or MMSC suspensions were performed into 6 points of the infarcted area. The surviving animals were divided in four groups, each consisting of 13 rabbits: group 1 (controls), group 2 (placebo-treated), group 3 (MMSC injections), and group 4 (MF injections). Electrocardiography (ECG) and echo-cardiography were carried out in all animals before surgery, during 1 mo and 1 year after surgery. Myocardial perfusion rates were assessed with SPECT technique. IM dimensions (perfusion areas) were determined by means of staining heart sections with 2,3,5-TTC. Routine histology of myocardial sections was also performed. Vascularization rates of different myocardial areas were assessed in similar way.
Results
Intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit experimental MI during the acute phase has changed natural process development and resulted in principally different morpho-functional outcomes. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, the animals, treated with MMSC or MF showed less impaired perfusion rates than in control or placebo groups (p<0.05). 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged myocardium in MMSC and MF-treated groups. These changes were confirmed by perfusion tomoscyntigraphy of myocardium at 1.5 and 12 months after surgery. Histological studies have shown that, after MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles. One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all functional parameters (LV ejection fraction; EDSLV, end LV diastolic size; blood flow rates in ascending aorta) at 12 months post-surgery (p<0.05), and absence of akinetic areas.
Conclusions
MMSC injections were associated with pronounced therapeutic effect, by reducing myocardium damage area. By the contrary, MF transplantation showed a negative effect, expanding myocardium damage area and impairing systolic function indices. Both MMSC and MF intramyocardial transplantation display neoangiogenesis stimulation and perfusion improvement in rabbit experimental infarction area.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "483" ["VALUE"]=> string(152) "Comparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(152) "Comparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1233" ["VALUE"]=> string(2) "20" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "20" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1234" ["VALUE"]=> string(2) "21" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "21" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(14) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "480" ["VALUE"]=> array(2) { ["TEXT"]=> string(360) "<p class="Autor">Vladimir V. Davydenko<sup>1</sup>, Andrey A. Matyukov<sup>1</sup>, Timur D. Vlasov<sup>1</sup>, Natalya V. Tsupkina<sup>2</sup>, Anatoly N. Yalfimov<sup>3</sup>, <br>Georgy P. Pinaev<sup>2</sup>, Khalida K. Amineva<sup>1</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(248) "Vladimir V. Davydenko1, Andrey A. Matyukov1, Timur D. Vlasov1, Natalya V. Tsupkina2, Anatoly N. Yalfimov3,
Georgy P. Pinaev2, Khalida K. Amineva1
Vladimir V. Davydenko1, Andrey A. Matyukov1, Timur D. Vlasov1, Natalya V. Tsupkina2, Anatoly N. Yalfimov3,
Georgy P. Pinaev2, Khalida K. Amineva1
Summary
Over the last decade, different cell therapy options have been tested to improve treatment of myocardial infarction (MI), including cardiomyoplastics. Autologous bone marrow is a widely used source of therapeutic cell preparations, i.e., freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchymal stromal cells (MMSC). The aim of our pilot study was to compare short- and long-term consequences of intramyocardial MF and MMSC transplantation upon clinical course and outcome of experimental MI. Materials and methods: The experiments were performed with male Chinchilla rabbits of 2.8+0.2 kg weight. MI was modelled by ligation of anterior descendent left coronary artery. Mononuclear cell fraction was obtained from the bone marrow aspirate. MMSC cell culture was grown by MF cell passages in МЕМ medium with 10% fetal calf serum. Intramyocardial injections of MF or MMSC suspensions were performed into 6 points of the infarcted area. The surviving animals were divided in four groups, each consisting of 13 rabbits: group 1 (controls), group 2 (placebo-treated), group 3 (MMSC injections), and group 4 (MF injections). Electrocardiography (ECG) and echo-cardiography were carried out in all animals before surgery, during 1 mo and 1 year after surgery. Myocardial perfusion rates were assessed with SPECT technique. IM dimensions (perfusion areas) were determined by means of staining heart sections with 2,3,5-TTC. Routine histology of myocardial sections was also performed. Vascularization rates of different myocardial areas were assessed in similar way.
Results
Intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit experimental MI during the acute phase has changed natural process development and resulted in principally different morpho-functional outcomes. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, the animals, treated with MMSC or MF showed less impaired perfusion rates than in control or placebo groups (p<0.05). 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged myocardium in MMSC and MF-treated groups. These changes were confirmed by perfusion tomoscyntigraphy of myocardium at 1.5 and 12 months after surgery. Histological studies have shown that, after MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles. One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all functional parameters (LV ejection fraction; EDSLV, end LV diastolic size; blood flow rates in ascending aorta) at 12 months post-surgery (p<0.05), and absence of akinetic areas.
Conclusions
MMSC injections were associated with pronounced therapeutic effect, by reducing myocardium damage area. By the contrary, MF transplantation showed a negative effect, expanding myocardium damage area and impairing systolic function indices. Both MMSC and MF intramyocardial transplantation display neoangiogenesis stimulation and perfusion improvement in rabbit experimental infarction area.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(3544) "Summary
Over the last decade, different cell therapy options have been tested to improve treatment of myocardial infarction (MI), including cardiomyoplastics. Autologous bone marrow is a widely used source of therapeutic cell preparations, i.e., freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchymal stromal cells (MMSC). The aim of our pilot study was to compare short- and long-term consequences of intramyocardial MF and MMSC transplantation upon clinical course and outcome of experimental MI. Materials and methods: The experiments were performed with male Chinchilla rabbits of 2.8+0.2 kg weight. MI was modelled by ligation of anterior descendent left coronary artery. Mononuclear cell fraction was obtained from the bone marrow aspirate. MMSC cell culture was grown by MF cell passages in МЕМ medium with 10% fetal calf serum. Intramyocardial injections of MF or MMSC suspensions were performed into 6 points of the infarcted area. The surviving animals were divided in four groups, each consisting of 13 rabbits: group 1 (controls), group 2 (placebo-treated), group 3 (MMSC injections), and group 4 (MF injections). Electrocardiography (ECG) and echo-cardiography were carried out in all animals before surgery, during 1 mo and 1 year after surgery. Myocardial perfusion rates were assessed with SPECT technique. IM dimensions (perfusion areas) were determined by means of staining heart sections with 2,3,5-TTC. Routine histology of myocardial sections was also performed. Vascularization rates of different myocardial areas were assessed in similar way.
Results
Intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit experimental MI during the acute phase has changed natural process development and resulted in principally different morpho-functional outcomes. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, the animals, treated with MMSC or MF showed less impaired perfusion rates than in control or placebo groups (p<0.05). 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged myocardium in MMSC and MF-treated groups. These changes were confirmed by perfusion tomoscyntigraphy of myocardium at 1.5 and 12 months after surgery. Histological studies have shown that, after MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles. One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all functional parameters (LV ejection fraction; EDSLV, end LV diastolic size; blood flow rates in ascending aorta) at 12 months post-surgery (p<0.05), and absence of akinetic areas.
Conclusions
MMSC injections were associated with pronounced therapeutic effect, by reducing myocardium damage area. By the contrary, MF transplantation showed a negative effect, expanding myocardium damage area and impairing systolic function indices. Both MMSC and MF intramyocardial transplantation display neoangiogenesis stimulation and perfusion improvement in rabbit experimental infarction area.
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "479" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-47-57" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-47-57" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-47-57" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "483" ["VALUE"]=> string(152) "Comparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(152) "Comparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(152) "Comparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "481" ["VALUE"]=> array(2) { ["TEXT"]=> string(748) "<p class="Autor_place_work"><span class="CharOverride-2" lang="en-US">1</span><span lang="en-US">FirstSt.Petersburg State I.Pavlov Medical University </span></p> <p class="Autor_place_work"><span class="CharOverride-2" lang="en-US">2</span><span lang="en-US">Institute of Cytology, Russian Academy of Sciences, St.Petersburg</span></p> <p class="Autor_place_work"><span class="CharOverride-2" lang="en-US">3</span><span lang="en-US">Russian Center of Radiology and Surgical Technologies, St.Petersburg</span></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(520) "1FirstSt.Petersburg State I.Pavlov Medical University
2Institute of Cytology, Russian Academy of Sciences, St.Petersburg
3Russian Center of Radiology and Surgical Technologies, St.Petersburg
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(520) "1FirstSt.Petersburg State I.Pavlov Medical University
2Institute of Cytology, Russian Academy of Sciences, St.Petersburg
3Russian Center of Radiology and Surgical Technologies, St.Petersburg
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(7) { [0]=> string(3) "469" [1]=> string(3) "470" [2]=> string(3) "471" [3]=> string(3) "472" [4]=> string(3) "473" [5]=> string(3) "474" [6]=> string(3) "475" } ["VALUE"]=> array(7) { [0]=> string(2) "79" [1]=> string(2) "77" [2]=> string(2) "74" [3]=> string(2) "78" [4]=> string(2) "76" [5]=> string(2) "75" [6]=> string(2) "73" } ["DESCRIPTION"]=> array(7) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(7) { [0]=> string(2) "79" [1]=> string(2) "77" [2]=> string(2) "74" [3]=> string(2) "78" [4]=> string(2) "76" [5]=> string(2) "75" [6]=> string(2) "73" } ["~DESCRIPTION"]=> array(7) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(7) { [0]=> string(60) "Khalida K. Amineva" [1]=> string(61) "Anatoly N. Yalfimov" [2]=> string(60) "Andrey A. Matyukov" [3]=> string(58) "Georgy P. Pinaev" [4]=> string(61) "Natalya V. Tsupkina" [5]=> string(57) "Timur D. Vlasov" [6]=> string(63) "Vladimir V. Davydenko" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "476" ["VALUE"]=> array(2) { ["TEXT"]=> string(452) "<p class="Autor">Владимир В. Давыденко<sup>1</sup>, Андрей А. Матюков<sup>1</sup>, Тимур Д. Власов<sup>1</sup>, Наталия В. Цупкина<sup>2</sup>, Анатолий Н. Ялфимов<sup>3</sup>, Георгий П. Пинаев<sup>2</sup>, Халида К. Аминева<sup>1</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(346) "Владимир В. Давыденко1, Андрей А. Матюков1, Тимур Д. Власов1, Наталия В. Цупкина2, Анатолий Н. Ялфимов3, Георгий П. Пинаев2, Халида К. Аминева1
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(346) "Владимир В. Давыденко1, Андрей А. Матюков1, Тимур Д. Власов1, Наталия В. Цупкина2, Анатолий Н. Ялфимов3, Георгий П. Пинаев2, Халида К. Аминева1
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "466" ["VALUE"]=> string(19) "06.04.2015 15:21:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "06.04.2015 15:21:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "06.04.2015 15:21:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "467" ["VALUE"]=> string(19) "02.07.2015 15:21:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "02.07.2015 15:21:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "02.07.2015 15:21:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "894" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(6) { [0]=> string(4) "1227" [1]=> string(4) "1228" [2]=> string(4) "1229" [3]=> string(4) "1230" [4]=> string(4) "1231" [5]=> string(4) "1232" } ["VALUE"]=> array(6) { [0]=> string(2) "80" [1]=> string(2) "81" [2]=> string(2) "82" [3]=> string(2) "83" [4]=> string(2) "84" [5]=> string(2) "85" } ["DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(6) { [0]=> string(2) "80" [1]=> string(2) "81" [2]=> string(2) "82" [3]=> string(2) "83" [4]=> string(2) "84" [5]=> string(2) "85" } ["~DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(6) { [0]=> string(110) "инфаркт миокарда, экспериментальный" [1]=> string(66) "костный мозг" [2]=> string(84) "мононуклеарные клетки" [3]=> string(97) "мезенхимные стволовые клетки" [4]=> string(90) "терапевтические инъекции" [5]=> string(96) "функции миокарда, гистология" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "468" ["VALUE"]=> string(2) "73" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "73" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(63) "Vladimir V. Davydenko" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "478" ["VALUE"]=> array(2) { ["TEXT"]=> string(6788) "<h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8<span class="CharOverride-12">+</span>0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами. </p> <p class="Summery_H">Результаты</p> <p class="Summery_Rus" lang="ru-RU">Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков. </p> <p class="Summery_H">Заключение</p> <p class="Summery_Rus" lang="ru-RU">Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(6602) "Резюме
Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8+0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами.
Результаты
Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков.
Заключение
Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(6602) "Резюме
Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8+0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами.
Результаты
Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков.
Заключение
Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов.
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "477" ["VALUE"]=> array(2) { ["TEXT"]=> string(651) "<p class="Autor_place_work-Rus"><sup>1</sup>Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова</p> <p class="Autor_place_work-Rus"><sup>2</sup>Институт цитологии Российской Академии наук, Санкт-Петербург</p> <p class="Autor_place_work-Rus"><sup>3</sup>Российский центр радиологии и хирургических технологий, Санкт-Петербург</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(549) "1Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова
2Институт цитологии Российской Академии наук, Санкт-Петербург
3Российский центр радиологии и хирургических технологий, Санкт-Петербург
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(549) "1Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова
2Институт цитологии Российской Академии наук, Санкт-Петербург
3Российский центр радиологии и хирургических технологий, Санкт-Петербург
" } } } [2]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "2" ["~IBLOCK_SECTION_ID"]=> string(1) "2" ["ID"]=> string(1) "9" ["~ID"]=> string(1) "9" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(149) "Химиотерапия у лиц старших возрастов: насколько интенсивным должно быть лечение?" ["~NAME"]=> string(149) "Химиотерапия у лиц старших возрастов: насколько интенсивным должно быть лечение?" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:37:59" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:37:59" ["DETAIL_PAGE_URL"]=> string(64) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-8-13/" ["~DETAIL_PAGE_URL"]=> string(64) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-8-13/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(32102) "Introduction
Little is known about cancer chemotherapy in the elderly. There are only a few studies which include patients with cancer who at the same time are older than seventy years of age. It is a common practice to treat elderly patients according to existing protocols for younger patients with reduced doses and off the record; the data are not collected and analyzed. Outcome of the chemotherapy in the elderly is influenced by age-related changes in body composition and normal organ function as well as age related deficiencies in cognitive processes. Reduced visual performance and reduced manual dexterity in the elderly lead frequently to dosing and compliance errors. Another complicating factor is the increasing use of complementary and alternative medicines by elderly patients. This article will review the age related changes of body function, organ toxicity after chemotherapy in the elderly and the potential impact of complementary and alternative medicines.
Defining old is a complex process. The age of 60 or 65, roughly equivalent to the age of retirement in most Western countries, is said to be the beginning of old age. The aging process is of course a biological reality with its own dynamic largely beyond individual control. In view of the increasing age of the population in industrialized countries, a differentiation by age (61-75 years: elderly persons; 76-90 years of age: old persons; above 90 years: very old persons) seems to be useful.
There are age-related changes in body composition such as increased body fat that amounts to circa 35% at age 75, reduction of total body water that amounts to about 17% at age 60, and decrease in extracellular liquid, to circa 40% at age 65. Aside from changes in body composition, there is a reduction of normal organ function every year: cardiac output, by about 1%; liver size, by 2%; liver blood flow, 1%; kidney blood flow, by 1%; tubular function, by 1%, and glomerular filtration rate (GFR), by 1ml/min/1,73m2.
Changes in biological functions in old age lead to consequences for pharmacotherapy. Reduced secretion of gastric acid and gastrointestinal tract motility might lead to a reduction of bioavailability of certain drugs. Increased body fat might change the distribution volume of lipophilic drugs. Reduction of albumin concentration might lead to an increase of non-albumin bound drugs. Reduction of GFR and tubular secretional function might lead to an accumulation of renally eliminated active substances.
Other age related deficiencies might complicate effective chemotherapy in old and very old patients. Reduced mobility and increased risk of osteoporosis increase the risk and the frequency of falls. Impairment of short-term memory leads to dosing errors and compliance problems and an increased belief in “tonics”, which might lead to drug interactions. Functional deficiencies, including emotional changes reduce the ability for directed and efficient actions and might lead to lethargy and non-adherence to treatment schedules. Reduced visual performance and reduced manual dexterity might lead to orientation problems, dosage errors and manual difficulties with splitting of tablets.
Polypharmacotherapy leads to particular problems in the elderly patient population. According to one study, the PRISCUS Project, every health insured older patient is prescribed 3.6 drugs on the average. Over-the-counter (OTC) products are added to this number. 25% of the prescribed drugs are potentially inadequate medications. [1]
The problem of non-compliance is already evident in twice daily (bid) vs. once daily (qd) dosing of medications. Published data on other twice daily medications (eg. metformine, glipizide, metoprolol) show that adequate adherence (defined as greater than 80% of pills taken) may be only 52-65% [11]. A Polish study comparing beta-blockers given once daily (betaxolol) or twice daily (metoprolol) to patients with stable angina pectoris showed 58.6% vs. 42.0% for doses taken in the correct time window and 77.4% vs. 53.1% for correct interdose intervals in favor of the drug taken once daily [8].
Hamaker et al. [6] state that currently ongoing trials in hematological malignancies are unlikely to significantly improve our knowledge of the optimal treatment of older patients, as those outcome measures, that are of primary importance to this patient population are still included in only a minority of studies. A broader database of chemotherapy data in elderly patients is needed to enable the oncologist to deliver evidence based and patient focused cancer care.
The experience with chemotherapeutic agents and their pharmacokinetics in patients with old age is limited. Hurria and Lichtman [7] analyze clinical pharmacology of cancer therapies in older patients in a mini review. In 18 studies older and younger patient groups were compared. When treated with Paclitaxel (3 studies), Docetaxel (4 studies), Oxaliplatin (1 study), Temozolomide (1 study), Vinorelbine (2 studies), 5- Fluorouracil (1 study), Capecitabine (1 study), Etoposide (3 studies), Doxorubicin (2 studies) only 5/18 studies could actually demonstrate age-related differences in clinical pharmacokinetics, but this remains controversial.
The International Society of Geriatric Oncology (SIOG) arrived at the following recommendations (Table 1) for the adjustment of dosing in elderly patients, according to the underlying renal function but also including clinical experience [10].
|
INN |
90-60 ml/min |
60-30 ml/min |
30-15 ml/min |
|
Melphalan |
100-200 mg/m2 |
75% |
50% |
|
Oxaliplatine |
85-100 mg/m2 |
100% |
100% |
|
Fludarabine |
25 mg/m2 |
20 mg/m2 |
15 mg/m2 |
|
Capecitabine |
1250 mg/m2 every 12 h |
950 mg/m2 every 12 h |
Contraindicated |
Table 1: Dosing adjustment in elderly cancer patients. Recommendations of the International Society of Geriatric Oncology (SIOG) according to the underlying renal function [10]
Kintzel and Dorr [9] recommended dose modification for another set of antineoplastic drugs for patients with renal dysfunction (Table 2). The dose modification is clearly related to the fraction of renally excreted active or toxic moiety of the drug. Etoposide with a fraction of 32% requires nearly no reduction in patients with a creatinine clearance of 30 ml/min., whereas methotrexate with a fraction of 77% of renally excreted or toxic moiety requires a reduction of 50% in patients with INN of 45 ml/min. and should not be given to patients with lower renal functions.
|
INN |
f |
60 ml/min |
45 ml/min |
30 ml/min |
|
Etoposide |
32% |
0.85 |
0.80 |
0.75 |
|
Hydroxyurea |
36% |
0.85 |
0.80 |
0.75 |
|
Dacarbazine |
41% |
0.80 |
0.75 |
0.70 |
|
Fludarabine |
44% |
0.80 |
0.75 |
0.65 |
|
Lomustine (CCNU) |
50% |
0.75 |
0.70 |
- |
|
Bleomycine |
62% |
0.70 |
0.60 |
- |
|
HD-AraC, MTX |
77% |
0.65 |
0.50 |
- |
Table 2. Dose modification for antineoplastic drugs in renal dysfunction [9]
Decreased organ functions, besides renal clearance that may lead to consequences for pharmacotherapy, are heart function, with a reduction of myocytes and reduction of dromotrophy, eventually: left ventricular ejection function (LVEF) that may lead to congestive heart failure and cardiac arrhythmias. Regarding the nervous system, co-morbidities, such as Diabetes Mellitus may lead to higher risk for sensory neuropathies. Reduced vital and diffusion capacity of the lung may lead to higher risk for lung toxic side-affects. The reduction of bone marrow reserve may lead to severe cytopenias. An increase in fibrinogen concentration may lead to a higher risk for venous thromboembolism.
An older study from von Hoff et al. [12] compares cumulative doses of Doxorubicin on incidence of cardiotoxicity in patients aged 40-59 vs. in patients older than 60 years of age. There was an increase in cardiotoxicity with all dose ranges in the older patient group. This difference was seen in the groups that received Doxorubicin every seven days as well as in the group that received the drug every three weeks.
|
Cumulative dose (mg/m2) |
q7d 40-59 y |
q7d > 60 y |
q3w 40-59 y |
q3w > 60 y |
|
300 |
0.6 |
0.9 |
2.2 |
3.4 |
|
400 |
0.7 |
1.2 |
2.3 |
4.6 |
|
500 |
1.5 |
2.3 |
5.8 |
8.9 |
|
600 |
3.9 |
6.1 |
14.9 |
22.4 |
|
700 |
8.7 |
13.2 |
30.5 |
43.5 |
Table 3: Doxorubicin-induced cardiotoxicity (%) related to cumulative dose. Modified from [12].
Newer orally available “targeted” anti-cancer agents are of special interest in the elderly patient group. E.c., target protein produced by bcr-abl fusion gene can be attacked by Imatinib (GLIVEC), Dasatinib (SPRYCEL), Nilotinib (TASIGNA), Bosutinib (BOSULIF), and Ponatinib (ICLUSIG). The epidermal growth factor receptor (EGFR) is target for several drugs like Erlotinib (TARCEVA), Imatinib (GLIVEC), Afatinib (GILOTRIF), and Lapatinib (TYVERB). Other drugs like Sorafenib (NEXAVAR) and Sunitinib (SUTENT) interfere with Vascular Endothelial Growth Factor (VEGF). Other drugs like Vemurafenib (ZELBORAF) and Dabrafenib (TAFINLAR) interfere with mutations of BRAF, the serine/threonine-protein kinase. Other targeted therapies include Crizotinib (XALKORI), Everolimus (AFINITOR), Vismodegib (ERIVEDGE), Trametinib (MEKINIST), and Ibrutinib (IMBRUVICA) as well as Thalidomide, Lenalidomide (REVLIMID), and Pomalidomide (IMNOVID) which in partly modulate the immune system.
Particular attention needs to be directed toward the toxicity of targeted anti-cancer therapy in the elderly [5]. The older human population compared to the younger population shows more toxicity in several areas. Imatinib shows more hematologic and non-hematologic toxicities in older patients. Bevacizumab shows more thromboembolism, more fatigue and more asthenia. Bortezomib shows more gastrointestinal problems, fatigue and neuropathies. Thalidomide shows more deeper vein thrombosis. Lenalidomide needed to be discontinued more frequently in the older population related to hematological and non-hematological toxicities. No age related differences in toxicity were seen in Trastuzumab.
A well-known example for influencing therapeutically needed drug levels are the Calcineurin inhibitors (CNI). Drugs which inhibit the Cytochrome P450 3A4 enzyme system that metabolizes CNIs lead to an increased risk for toxicity, drugs which induce enzymes catabolizing CNIs lead to a decreased drug concentrations and therefore an increased risk of treatment failure. Therefore, close attention needs to be given to the drug concentration, particularly if other drugs are given which induce or inhibit enzymes.
A particular problem of drug interference constitutes over-the-counter (OTC) and complementary and alternative medicine (CAM). There are many-fold explanations:
- OTCs require no prescription, “therefore they cannot be dangerous”.
- There is a need to address personal fears and worries
- Desire to do something for one’s health
- Therapy considered to be harmless (natural)
- Belief: “natural” things are good
- Can do no harm
- Strengthen the immune system
- Intriguing and useful information from friends, fellow sufferers and the Internet.
Complementary and alternative medicine are based on mysticism and magic:
Mysticism (nature is benign and curing negative damaging effects are ignored); Magic (delusions and wishful thinking attempt to influence processes outside one’s control).
There are only a few interactions between prescription drugs and CAM known and reported. One example is the interaction between Imatinib/St. John’s Wort (hypericum perforatum), a Cyp3A-inductor. Frye et al. [3] reported an increase of Imatinib-clearance by 43% through the effect of concomitantly given St. John’s Wort.
Another publication points to probable interaction of etoposide with Echinacea [2]. In this case, it was likely that Echinacea contributed to a patient’s profound life-threatening thrombocytopenia and therefore should be avoided in patients receiving etoposide and possible other chemotherapeutic drugs that are CYP 3A4 substrates.
Green Tea is widely used as a CAM. It has been reported in the treatment of patients with asymptomatic CLL, has been reported to induce cell death in AML, has been reported to prevent prostate cancer and pre-menopausal breast cancer. On the other hand, one of the active agents of green tea, the Epigallocatechin gallate (EGCG) decreases the bio-availability of Bortezomid, one of the most active agents in the treatment of multiple myeloma [4].
|
Phytopharmaca |
Active substance |
Possible pharmacokintetic interaction |
|
Cranberry fruit (Vaccinium macrocarpon) |
Anthocyane, Flavonoide |
Cyp (1A2, 2C9, 3A4)- and PgP-inhibition |
|
Garlic (Allium sativum) |
Allicin, |
Cyp3A- and PgP-induktion, Cyp2C9, 2C19, 2E1-inhibition |
|
Ginkgo (Ginkgo biloba) |
Ginkgolide, Flavonoide |
Cyp3A- induction, free radical scavenger properties; PD: TAH |
|
Ginseng (Panax ginseng) |
Ginsenoside |
Cyp3A-induction (& inhibition) |
|
Green tea (Camellia sinensis) |
Catechine (ECG, EGCG) |
Cyp3A, 2A6, 2C19, 2E1-Inhibition, increased Cyp1A2, 2B and NDAPH-Cyp450-reduktase-activity, PgP-inhibition, inhibits SULT1A1, SULT1A3 and OATP1A2, OAT1B1, OATP2B1-transport, stimulates OATP1B3-transport |
|
St John´s wort (Hypericum perforatum) |
Hyperforin, Hypericin et al. |
Broad spectrum of Cyp- and PgP-induction |
Table 4: Possible pharmacokinetic interaction of phytopharmaca with prescription drugs.
Conclusions
What needs to be generally considered regarding tumor therapy in older patients?
Many PK-studies in geriatric patients are contradictory, the problem being: small patient numbers, co-factors, analytical methods (standardization),
Especially, the kidney function is age-related and requires adherence to the treatment guides (e.g. SIOG),
Age-related co-morbidities and toxicity profiles of the involved active substances need to be correlated,
Polypharmacy (OTC) can create complex interactions in older patients. The medical history of an oncology patient should include his prescription drugs as well as the complimentary and alternative medicines.
More attention needs to be directed toward investigating these interactions. Education of patients, relatives and supportive staff is critical to achieve this.
There is a definite need for drug studies in elderly patients. It would be a first step if a means could be found to collect data from patients above the age cut-off of oncology studies when they are treated according to the protocol with or without “age adjustment” of drug doses. A second step may be the inclusion of elderly patients by increasing the age limit of the studies, and by designing specific chemotherapy studies for old patients in need of treatment.
Conflict of interest
All authors have no conflict of interest to declare.
References
- Amann U, Schmidt N, Garbe E. Prescribing of potentially inappropriate medications for the elderly: an analysis based on the PRISCUS list. Dtsch Arztebl Int 2012; 109(5): 69-75.
- Bossaer JB, Odle BL. Probable etoposide interaction with Echinacea. J Diet Suppl 2012;9(2): 90-5.
- Frye RF, Fitzgerald SM, Lagattuta TF, Hruska MW, Egorin MJ. Effect of St John’s wort on imatinib mesylate pharmacokinetics. Clin Pharmacol Ther 2004; 76(4): 323-9.
- Golden EB, Lam PY, Kardosh A, Gaffney KJ, Cadenas E, Louie SG, Petasis NA, Chen TC, Schönthal AH. Green tea polyphenols block the anticancer effects of bortezomib and other boronic acid-based proteasome inhibitors. Blood 2009; 113(23): 5927-37.
- Gonsalves W, Ganti AK. Targeted anti-cancer therapy in the elderly. Crit Rev Oncol Hematol 2011; 78(3): 227-42.
- Hamaker ME, Stauder R, van Munster BC. Ongoing clinical trials for elderly patients with a hematological malignancy: are we addressing the right end points? Ann Oncol 2014; 25(3): 675-81.
- Hurria A, Lichtman SM. Clinical pharmacology of cancer therapies in older adults. Br J Cancer 2008; 98(3): 517-22.
- Kardas P. Compliance, clinical outcome, and quality of life of patients with stable angina pectoris receiving once-daily betaxolol versus twice daily metoprolol: a randomized controlled trial. Vasc Health Risk Manag 2007; 3(2): 235-42.
- Kintzel PE, Dorr RT. Anticancer drug renal toxicity and elimination: dosing guidelines for altered renal function. Cancer Treatm Rev 1995; 21(1): 33-64.
- Lichtman SM, Wildiers H, Launay-Vacher V, Steer C, Chatelut E, Aapro M. International Society of Geriatric Oncology (SIOG) recommendations for the adjustment of dosing in elderly cancer patients with renal insufficiency. Eur J Cancer 2007; 43(1): 14-34.
- Tu W, Morris AB, Li J et al. Association between adherence measurements of metoprolol and health care utilization in older patients with heart failure. Clin Pharmacol Ther 2005; 77(3): 189-201.
- Von Hoff DD, Layard MW, Basa P, Davis HL, Jr, Von Hoff AL, Rozencweig M, Muggia FM. Risk factors for doxorubicin-induced congestive heart failure. Ann Intern Med 1979; 91(5): 710-7.
Introduction
Little is known about cancer chemotherapy in the elderly. There are only a few studies which include patients with cancer who at the same time are older than seventy years of age. It is a common practice to treat elderly patients according to existing protocols for younger patients with reduced doses and off the record; the data are not collected and analyzed. Outcome of the chemotherapy in the elderly is influenced by age-related changes in body composition and normal organ function as well as age related deficiencies in cognitive processes. Reduced visual performance and reduced manual dexterity in the elderly lead frequently to dosing and compliance errors. Another complicating factor is the increasing use of complementary and alternative medicines by elderly patients. This article will review the age related changes of body function, organ toxicity after chemotherapy in the elderly and the potential impact of complementary and alternative medicines.
Defining old is a complex process. The age of 60 or 65, roughly equivalent to the age of retirement in most Western countries, is said to be the beginning of old age. The aging process is of course a biological reality with its own dynamic largely beyond individual control. In view of the increasing age of the population in industrialized countries, a differentiation by age (61-75 years: elderly persons; 76-90 years of age: old persons; above 90 years: very old persons) seems to be useful.
There are age-related changes in body composition such as increased body fat that amounts to circa 35% at age 75, reduction of total body water that amounts to about 17% at age 60, and decrease in extracellular liquid, to circa 40% at age 65. Aside from changes in body composition, there is a reduction of normal organ function every year: cardiac output, by about 1%; liver size, by 2%; liver blood flow, 1%; kidney blood flow, by 1%; tubular function, by 1%, and glomerular filtration rate (GFR), by 1ml/min/1,73m2.
Changes in biological functions in old age lead to consequences for pharmacotherapy. Reduced secretion of gastric acid and gastrointestinal tract motility might lead to a reduction of bioavailability of certain drugs. Increased body fat might change the distribution volume of lipophilic drugs. Reduction of albumin concentration might lead to an increase of non-albumin bound drugs. Reduction of GFR and tubular secretional function might lead to an accumulation of renally eliminated active substances.
Other age related deficiencies might complicate effective chemotherapy in old and very old patients. Reduced mobility and increased risk of osteoporosis increase the risk and the frequency of falls. Impairment of short-term memory leads to dosing errors and compliance problems and an increased belief in “tonics”, which might lead to drug interactions. Functional deficiencies, including emotional changes reduce the ability for directed and efficient actions and might lead to lethargy and non-adherence to treatment schedules. Reduced visual performance and reduced manual dexterity might lead to orientation problems, dosage errors and manual difficulties with splitting of tablets.
Polypharmacotherapy leads to particular problems in the elderly patient population. According to one study, the PRISCUS Project, every health insured older patient is prescribed 3.6 drugs on the average. Over-the-counter (OTC) products are added to this number. 25% of the prescribed drugs are potentially inadequate medications. [1]
The problem of non-compliance is already evident in twice daily (bid) vs. once daily (qd) dosing of medications. Published data on other twice daily medications (eg. metformine, glipizide, metoprolol) show that adequate adherence (defined as greater than 80% of pills taken) may be only 52-65% [11]. A Polish study comparing beta-blockers given once daily (betaxolol) or twice daily (metoprolol) to patients with stable angina pectoris showed 58.6% vs. 42.0% for doses taken in the correct time window and 77.4% vs. 53.1% for correct interdose intervals in favor of the drug taken once daily [8].
Hamaker et al. [6] state that currently ongoing trials in hematological malignancies are unlikely to significantly improve our knowledge of the optimal treatment of older patients, as those outcome measures, that are of primary importance to this patient population are still included in only a minority of studies. A broader database of chemotherapy data in elderly patients is needed to enable the oncologist to deliver evidence based and patient focused cancer care.
The experience with chemotherapeutic agents and their pharmacokinetics in patients with old age is limited. Hurria and Lichtman [7] analyze clinical pharmacology of cancer therapies in older patients in a mini review. In 18 studies older and younger patient groups were compared. When treated with Paclitaxel (3 studies), Docetaxel (4 studies), Oxaliplatin (1 study), Temozolomide (1 study), Vinorelbine (2 studies), 5- Fluorouracil (1 study), Capecitabine (1 study), Etoposide (3 studies), Doxorubicin (2 studies) only 5/18 studies could actually demonstrate age-related differences in clinical pharmacokinetics, but this remains controversial.
The International Society of Geriatric Oncology (SIOG) arrived at the following recommendations (Table 1) for the adjustment of dosing in elderly patients, according to the underlying renal function but also including clinical experience [10].
|
INN |
90-60 ml/min |
60-30 ml/min |
30-15 ml/min |
|
Melphalan |
100-200 mg/m2 |
75% |
50% |
|
Oxaliplatine |
85-100 mg/m2 |
100% |
100% |
|
Fludarabine |
25 mg/m2 |
20 mg/m2 |
15 mg/m2 |
|
Capecitabine |
1250 mg/m2 every 12 h |
950 mg/m2 every 12 h |
Contraindicated |
Table 1: Dosing adjustment in elderly cancer patients. Recommendations of the International Society of Geriatric Oncology (SIOG) according to the underlying renal function [10]
Kintzel and Dorr [9] recommended dose modification for another set of antineoplastic drugs for patients with renal dysfunction (Table 2). The dose modification is clearly related to the fraction of renally excreted active or toxic moiety of the drug. Etoposide with a fraction of 32% requires nearly no reduction in patients with a creatinine clearance of 30 ml/min., whereas methotrexate with a fraction of 77% of renally excreted or toxic moiety requires a reduction of 50% in patients with INN of 45 ml/min. and should not be given to patients with lower renal functions.
|
INN |
f |
60 ml/min |
45 ml/min |
30 ml/min |
|
Etoposide |
32% |
0.85 |
0.80 |
0.75 |
|
Hydroxyurea |
36% |
0.85 |
0.80 |
0.75 |
|
Dacarbazine |
41% |
0.80 |
0.75 |
0.70 |
|
Fludarabine |
44% |
0.80 |
0.75 |
0.65 |
|
Lomustine (CCNU) |
50% |
0.75 |
0.70 |
- |
|
Bleomycine |
62% |
0.70 |
0.60 |
- |
|
HD-AraC, MTX |
77% |
0.65 |
0.50 |
- |
Table 2. Dose modification for antineoplastic drugs in renal dysfunction [9]
Decreased organ functions, besides renal clearance that may lead to consequences for pharmacotherapy, are heart function, with a reduction of myocytes and reduction of dromotrophy, eventually: left ventricular ejection function (LVEF) that may lead to congestive heart failure and cardiac arrhythmias. Regarding the nervous system, co-morbidities, such as Diabetes Mellitus may lead to higher risk for sensory neuropathies. Reduced vital and diffusion capacity of the lung may lead to higher risk for lung toxic side-affects. The reduction of bone marrow reserve may lead to severe cytopenias. An increase in fibrinogen concentration may lead to a higher risk for venous thromboembolism.
An older study from von Hoff et al. [12] compares cumulative doses of Doxorubicin on incidence of cardiotoxicity in patients aged 40-59 vs. in patients older than 60 years of age. There was an increase in cardiotoxicity with all dose ranges in the older patient group. This difference was seen in the groups that received Doxorubicin every seven days as well as in the group that received the drug every three weeks.
|
Cumulative dose (mg/m2) |
q7d 40-59 y |
q7d > 60 y |
q3w 40-59 y |
q3w > 60 y |
|
300 |
0.6 |
0.9 |
2.2 |
3.4 |
|
400 |
0.7 |
1.2 |
2.3 |
4.6 |
|
500 |
1.5 |
2.3 |
5.8 |
8.9 |
|
600 |
3.9 |
6.1 |
14.9 |
22.4 |
|
700 |
8.7 |
13.2 |
30.5 |
43.5 |
Table 3: Doxorubicin-induced cardiotoxicity (%) related to cumulative dose. Modified from [12].
Newer orally available “targeted” anti-cancer agents are of special interest in the elderly patient group. E.c., target protein produced by bcr-abl fusion gene can be attacked by Imatinib (GLIVEC), Dasatinib (SPRYCEL), Nilotinib (TASIGNA), Bosutinib (BOSULIF), and Ponatinib (ICLUSIG). The epidermal growth factor receptor (EGFR) is target for several drugs like Erlotinib (TARCEVA), Imatinib (GLIVEC), Afatinib (GILOTRIF), and Lapatinib (TYVERB). Other drugs like Sorafenib (NEXAVAR) and Sunitinib (SUTENT) interfere with Vascular Endothelial Growth Factor (VEGF). Other drugs like Vemurafenib (ZELBORAF) and Dabrafenib (TAFINLAR) interfere with mutations of BRAF, the serine/threonine-protein kinase. Other targeted therapies include Crizotinib (XALKORI), Everolimus (AFINITOR), Vismodegib (ERIVEDGE), Trametinib (MEKINIST), and Ibrutinib (IMBRUVICA) as well as Thalidomide, Lenalidomide (REVLIMID), and Pomalidomide (IMNOVID) which in partly modulate the immune system.
Particular attention needs to be directed toward the toxicity of targeted anti-cancer therapy in the elderly [5]. The older human population compared to the younger population shows more toxicity in several areas. Imatinib shows more hematologic and non-hematologic toxicities in older patients. Bevacizumab shows more thromboembolism, more fatigue and more asthenia. Bortezomib shows more gastrointestinal problems, fatigue and neuropathies. Thalidomide shows more deeper vein thrombosis. Lenalidomide needed to be discontinued more frequently in the older population related to hematological and non-hematological toxicities. No age related differences in toxicity were seen in Trastuzumab.
A well-known example for influencing therapeutically needed drug levels are the Calcineurin inhibitors (CNI). Drugs which inhibit the Cytochrome P450 3A4 enzyme system that metabolizes CNIs lead to an increased risk for toxicity, drugs which induce enzymes catabolizing CNIs lead to a decreased drug concentrations and therefore an increased risk of treatment failure. Therefore, close attention needs to be given to the drug concentration, particularly if other drugs are given which induce or inhibit enzymes.
A particular problem of drug interference constitutes over-the-counter (OTC) and complementary and alternative medicine (CAM). There are many-fold explanations:
- OTCs require no prescription, “therefore they cannot be dangerous”.
- There is a need to address personal fears and worries
- Desire to do something for one’s health
- Therapy considered to be harmless (natural)
- Belief: “natural” things are good
- Can do no harm
- Strengthen the immune system
- Intriguing and useful information from friends, fellow sufferers and the Internet.
Complementary and alternative medicine are based on mysticism and magic:
Mysticism (nature is benign and curing negative damaging effects are ignored); Magic (delusions and wishful thinking attempt to influence processes outside one’s control).
There are only a few interactions between prescription drugs and CAM known and reported. One example is the interaction between Imatinib/St. John’s Wort (hypericum perforatum), a Cyp3A-inductor. Frye et al. [3] reported an increase of Imatinib-clearance by 43% through the effect of concomitantly given St. John’s Wort.
Another publication points to probable interaction of etoposide with Echinacea [2]. In this case, it was likely that Echinacea contributed to a patient’s profound life-threatening thrombocytopenia and therefore should be avoided in patients receiving etoposide and possible other chemotherapeutic drugs that are CYP 3A4 substrates.
Green Tea is widely used as a CAM. It has been reported in the treatment of patients with asymptomatic CLL, has been reported to induce cell death in AML, has been reported to prevent prostate cancer and pre-menopausal breast cancer. On the other hand, one of the active agents of green tea, the Epigallocatechin gallate (EGCG) decreases the bio-availability of Bortezomid, one of the most active agents in the treatment of multiple myeloma [4].
|
Phytopharmaca |
Active substance |
Possible pharmacokintetic interaction |
|
Cranberry fruit (Vaccinium macrocarpon) |
Anthocyane, Flavonoide |
Cyp (1A2, 2C9, 3A4)- and PgP-inhibition |
|
Garlic (Allium sativum) |
Allicin, |
Cyp3A- and PgP-induktion, Cyp2C9, 2C19, 2E1-inhibition |
|
Ginkgo (Ginkgo biloba) |
Ginkgolide, Flavonoide |
Cyp3A- induction, free radical scavenger properties; PD: TAH |
|
Ginseng (Panax ginseng) |
Ginsenoside |
Cyp3A-induction (& inhibition) |
|
Green tea (Camellia sinensis) |
Catechine (ECG, EGCG) |
Cyp3A, 2A6, 2C19, 2E1-Inhibition, increased Cyp1A2, 2B and NDAPH-Cyp450-reduktase-activity, PgP-inhibition, inhibits SULT1A1, SULT1A3 and OATP1A2, OAT1B1, OATP2B1-transport, stimulates OATP1B3-transport |
|
St John´s wort (Hypericum perforatum) |
Hyperforin, Hypericin et al. |
Broad spectrum of Cyp- and PgP-induction |
Table 4: Possible pharmacokinetic interaction of phytopharmaca with prescription drugs.
Conclusions
What needs to be generally considered regarding tumor therapy in older patients?
Many PK-studies in geriatric patients are contradictory, the problem being: small patient numbers, co-factors, analytical methods (standardization),
Especially, the kidney function is age-related and requires adherence to the treatment guides (e.g. SIOG),
Age-related co-morbidities and toxicity profiles of the involved active substances need to be correlated,
Polypharmacy (OTC) can create complex interactions in older patients. The medical history of an oncology patient should include his prescription drugs as well as the complimentary and alternative medicines.
More attention needs to be directed toward investigating these interactions. Education of patients, relatives and supportive staff is critical to achieve this.
There is a definite need for drug studies in elderly patients. It would be a first step if a means could be found to collect data from patients above the age cut-off of oncology studies when they are treated according to the protocol with or without “age adjustment” of drug doses. A second step may be the inclusion of elderly patients by increasing the age limit of the studies, and by designing specific chemotherapy studies for old patients in need of treatment.
Conflict of interest
All authors have no conflict of interest to declare.
References
- Amann U, Schmidt N, Garbe E. Prescribing of potentially inappropriate medications for the elderly: an analysis based on the PRISCUS list. Dtsch Arztebl Int 2012; 109(5): 69-75.
- Bossaer JB, Odle BL. Probable etoposide interaction with Echinacea. J Diet Suppl 2012;9(2): 90-5.
- Frye RF, Fitzgerald SM, Lagattuta TF, Hruska MW, Egorin MJ. Effect of St John’s wort on imatinib mesylate pharmacokinetics. Clin Pharmacol Ther 2004; 76(4): 323-9.
- Golden EB, Lam PY, Kardosh A, Gaffney KJ, Cadenas E, Louie SG, Petasis NA, Chen TC, Schönthal AH. Green tea polyphenols block the anticancer effects of bortezomib and other boronic acid-based proteasome inhibitors. Blood 2009; 113(23): 5927-37.
- Gonsalves W, Ganti AK. Targeted anti-cancer therapy in the elderly. Crit Rev Oncol Hematol 2011; 78(3): 227-42.
- Hamaker ME, Stauder R, van Munster BC. Ongoing clinical trials for elderly patients with a hematological malignancy: are we addressing the right end points? Ann Oncol 2014; 25(3): 675-81.
- Hurria A, Lichtman SM. Clinical pharmacology of cancer therapies in older adults. Br J Cancer 2008; 98(3): 517-22.
- Kardas P. Compliance, clinical outcome, and quality of life of patients with stable angina pectoris receiving once-daily betaxolol versus twice daily metoprolol: a randomized controlled trial. Vasc Health Risk Manag 2007; 3(2): 235-42.
- Kintzel PE, Dorr RT. Anticancer drug renal toxicity and elimination: dosing guidelines for altered renal function. Cancer Treatm Rev 1995; 21(1): 33-64.
- Lichtman SM, Wildiers H, Launay-Vacher V, Steer C, Chatelut E, Aapro M. International Society of Geriatric Oncology (SIOG) recommendations for the adjustment of dosing in elderly cancer patients with renal insufficiency. Eur J Cancer 2007; 43(1): 14-34.
- Tu W, Morris AB, Li J et al. Association between adherence measurements of metoprolol and health care utilization in older patients with heart failure. Clin Pharmacol Ther 2005; 77(3): 189-201.
- Von Hoff DD, Layard MW, Basa P, Davis HL, Jr, Von Hoff AL, Rozencweig M, Muggia FM. Risk factors for doxorubicin-induced congestive heart failure. Ann Intern Med 1979; 91(5): 710-7.
Аксель Р. Цандер1, Рене Дж. Хорнунг2, Ханс П. Липп3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "98" ["VALUE"]=> array(2) { ["TEXT"]=> string(756) "<p class="Autor_place_work-Rus"><sup>1</sup>Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия </p> <p class="Autor_place_work-Rus"><sup>2</sup>Университетский медицинский центр Гамбург-Эппендорф, Германия</p> <p class="Autor_place_work-Rus"><sup>3</sup><span class="affiliation">Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия</span></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(632) "1Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия
2Университетский медицинский центр Гамбург-Эппендорф, Германия
3Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "99" ["VALUE"]=> array(2) { ["TEXT"]=> string(5589) "<h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.</p> <p class="Summery_Rus" lang="ru-RU">Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (<span class="CharOverride-4">Hypericum perforatum</span>), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.</p> <p class="Summery_Rus" lang="ru-RU">Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(5459) "Резюме
Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.
Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (Hypericum perforatum), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.
Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "22" ["VALUE"]=> string(34) "10.18620/1866-8836-2015-4-1-2-8-13" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(34) "10.18620/1866-8836-2015-4-1-2-8-13" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "100" ["VALUE"]=> array(2) { ["TEXT"]=> string(164) "<p class="Autor">Axel R. Zander<sup>1</sup>, René J. Hornung<sup>2</sup>, Hans-Peter Lipp<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(106) "Axel R. Zander1, René J. Hornung2, Hans-Peter Lipp3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "101" ["VALUE"]=> array(2) { ["TEXT"]=> string(512) "<p class="Autor_place_work">Research Department Cell and Gene Therapy, Clinic for Stem Cell Transplantation, University Medical Centre Hamburg-Eppendorf, Hamburg, Germany<sup>1</sup></p><p class="Autor_place_work">University Medical Centre Hamburg-Eppendorf, Hamburg, Germany<sup>2</sup></p> <p class="Autor_place_work">Department of Hospital Pharmacy, University Tübingen, Tübingen, Germany<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(410) "Research Department Cell and Gene Therapy, Clinic for Stem Cell Transplantation, University Medical Centre Hamburg-Eppendorf, Hamburg, Germany1
University Medical Centre Hamburg-Eppendorf, Hamburg, Germany2
Department of Hospital Pharmacy, University Tübingen, Tübingen, Germany3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "102" ["VALUE"]=> array(2) { ["TEXT"]=> string(1517) "<h2 class="Summery"> Summary</h2> <p class="Summery"> Physiological changes and deficiencies in cognitive processes in the elderly have an influence on therapy and drug dosage compliance. The consequences of differences for the outcome of especially chemotherapies are neither well nor systematically studied. Existing studies though could actually demonstrate age-related differences in clinical pharmacokinetics. Another problem is the increased number of prescribed drugs that are often necessary when getting older (polypharmacy) and their interference with over-the-counter drugs (OTC) and complementary and alternative medicine (CAM). While they are often seen as harmless since they require no prescription or are of “natural origin”, they can contain pharmaceutical active agents. For example green tea is reported to prevent prostate cancer and pre-menopausal breast cancer and is therefore often recommended to cancer patients, but also contains Epigallocatechin gallate (EGCg) an active substance which decreases the bio-availability of the anti-cancer drugs Bortezomid or Sunitinib. Conclusion: a further and more systematic study of age-related differences in the outcome of chemotherapies in the elderly is necessary. Here especially the kidney function requires adaption of treatment regimen. Furthermore the interactions with other drugs, in particular over-the-counter and alternative medicine, need to be better understood and communicated. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1473) "Summary
Physiological changes and deficiencies in cognitive processes in the elderly have an influence on therapy and drug dosage compliance. The consequences of differences for the outcome of especially chemotherapies are neither well nor systematically studied. Existing studies though could actually demonstrate age-related differences in clinical pharmacokinetics. Another problem is the increased number of prescribed drugs that are often necessary when getting older (polypharmacy) and their interference with over-the-counter drugs (OTC) and complementary and alternative medicine (CAM). While they are often seen as harmless since they require no prescription or are of “natural origin”, they can contain pharmaceutical active agents. For example green tea is reported to prevent prostate cancer and pre-menopausal breast cancer and is therefore often recommended to cancer patients, but also contains Epigallocatechin gallate (EGCg) an active substance which decreases the bio-availability of the anti-cancer drugs Bortezomid or Sunitinib. Conclusion: a further and more systematic study of age-related differences in the outcome of chemotherapies in the elderly is necessary. Here especially the kidney function requires adaption of treatment regimen. Furthermore the interactions with other drugs, in particular over-the-counter and alternative medicine, need to be better understood and communicated.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "23" ["VALUE"]=> string(64) "Chemotherapy in the elderly – How intense should treatment be?" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(64) "Chemotherapy in the elderly – How intense should treatment be?" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1186" ["VALUE"]=> string(1) "8" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(1) "8" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1187" ["VALUE"]=> string(1) "9" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(1) "9" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(14) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "100" ["VALUE"]=> array(2) { ["TEXT"]=> string(164) "<p class="Autor">Axel R. Zander<sup>1</sup>, René J. Hornung<sup>2</sup>, Hans-Peter Lipp<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(106) "Axel R. Zander1, René J. Hornung2, Hans-Peter Lipp3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(106) "Axel R. Zander1, René J. Hornung2, Hans-Peter Lipp3
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "102" ["VALUE"]=> array(2) { ["TEXT"]=> string(1517) "<h2 class="Summery"> Summary</h2> <p class="Summery"> Physiological changes and deficiencies in cognitive processes in the elderly have an influence on therapy and drug dosage compliance. The consequences of differences for the outcome of especially chemotherapies are neither well nor systematically studied. Existing studies though could actually demonstrate age-related differences in clinical pharmacokinetics. Another problem is the increased number of prescribed drugs that are often necessary when getting older (polypharmacy) and their interference with over-the-counter drugs (OTC) and complementary and alternative medicine (CAM). While they are often seen as harmless since they require no prescription or are of “natural origin”, they can contain pharmaceutical active agents. For example green tea is reported to prevent prostate cancer and pre-menopausal breast cancer and is therefore often recommended to cancer patients, but also contains Epigallocatechin gallate (EGCg) an active substance which decreases the bio-availability of the anti-cancer drugs Bortezomid or Sunitinib. Conclusion: a further and more systematic study of age-related differences in the outcome of chemotherapies in the elderly is necessary. Here especially the kidney function requires adaption of treatment regimen. Furthermore the interactions with other drugs, in particular over-the-counter and alternative medicine, need to be better understood and communicated. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1473) "Summary
Physiological changes and deficiencies in cognitive processes in the elderly have an influence on therapy and drug dosage compliance. The consequences of differences for the outcome of especially chemotherapies are neither well nor systematically studied. Existing studies though could actually demonstrate age-related differences in clinical pharmacokinetics. Another problem is the increased number of prescribed drugs that are often necessary when getting older (polypharmacy) and their interference with over-the-counter drugs (OTC) and complementary and alternative medicine (CAM). While they are often seen as harmless since they require no prescription or are of “natural origin”, they can contain pharmaceutical active agents. For example green tea is reported to prevent prostate cancer and pre-menopausal breast cancer and is therefore often recommended to cancer patients, but also contains Epigallocatechin gallate (EGCg) an active substance which decreases the bio-availability of the anti-cancer drugs Bortezomid or Sunitinib. Conclusion: a further and more systematic study of age-related differences in the outcome of chemotherapies in the elderly is necessary. Here especially the kidney function requires adaption of treatment regimen. Furthermore the interactions with other drugs, in particular over-the-counter and alternative medicine, need to be better understood and communicated.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1473) "Summary
Physiological changes and deficiencies in cognitive processes in the elderly have an influence on therapy and drug dosage compliance. The consequences of differences for the outcome of especially chemotherapies are neither well nor systematically studied. Existing studies though could actually demonstrate age-related differences in clinical pharmacokinetics. Another problem is the increased number of prescribed drugs that are often necessary when getting older (polypharmacy) and their interference with over-the-counter drugs (OTC) and complementary and alternative medicine (CAM). While they are often seen as harmless since they require no prescription or are of “natural origin”, they can contain pharmaceutical active agents. For example green tea is reported to prevent prostate cancer and pre-menopausal breast cancer and is therefore often recommended to cancer patients, but also contains Epigallocatechin gallate (EGCg) an active substance which decreases the bio-availability of the anti-cancer drugs Bortezomid or Sunitinib. Conclusion: a further and more systematic study of age-related differences in the outcome of chemotherapies in the elderly is necessary. Here especially the kidney function requires adaption of treatment regimen. Furthermore the interactions with other drugs, in particular over-the-counter and alternative medicine, need to be better understood and communicated.
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "22" ["VALUE"]=> string(34) "10.18620/1866-8836-2015-4-1-2-8-13" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(34) "10.18620/1866-8836-2015-4-1-2-8-13" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(34) "10.18620/1866-8836-2015-4-1-2-8-13" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "23" ["VALUE"]=> string(64) "Chemotherapy in the elderly – How intense should treatment be?" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(64) "Chemotherapy in the elderly – How intense should treatment be?" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(64) "Chemotherapy in the elderly – How intense should treatment be?" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "101" ["VALUE"]=> array(2) { ["TEXT"]=> string(512) "<p class="Autor_place_work">Research Department Cell and Gene Therapy, Clinic for Stem Cell Transplantation, University Medical Centre Hamburg-Eppendorf, Hamburg, Germany<sup>1</sup></p><p class="Autor_place_work">University Medical Centre Hamburg-Eppendorf, Hamburg, Germany<sup>2</sup></p> <p class="Autor_place_work">Department of Hospital Pharmacy, University Tübingen, Tübingen, Germany<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(410) "Research Department Cell and Gene Therapy, Clinic for Stem Cell Transplantation, University Medical Centre Hamburg-Eppendorf, Hamburg, Germany1
University Medical Centre Hamburg-Eppendorf, Hamburg, Germany2
Department of Hospital Pharmacy, University Tübingen, Tübingen, Germany3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(410) "Research Department Cell and Gene Therapy, Clinic for Stem Cell Transplantation, University Medical Centre Hamburg-Eppendorf, Hamburg, Germany1
University Medical Centre Hamburg-Eppendorf, Hamburg, Germany2
Department of Hospital Pharmacy, University Tübingen, Tübingen, Germany3
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(3) { [0]=> string(2) "24" [1]=> string(2) "25" [2]=> string(2) "84" } ["VALUE"]=> array(3) { [0]=> string(2) "11" [1]=> string(2) "12" [2]=> string(2) "14" } ["DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(3) { [0]=> string(2) "11" [1]=> string(2) "12" [2]=> string(2) "14" } ["~DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(3) { [0]=> string(56) "Axel R. Zander" [1]=> string(58) "René J. Hornung" [2]=> string(57) "Hans-Peter Lipp" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "97" ["VALUE"]=> array(2) { ["TEXT"]=> string(225) "<p class="Autor_Rus" lang="ru-RU">Аксель Р. Цандер<sup>1</sup>, Рене Дж. Хорнунг<sup>2</sup>, Ханс П. Липп<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(157) "Аксель Р. Цандер1, Рене Дж. Хорнунг2, Ханс П. Липп3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(157) "Аксель Р. Цандер1, Рене Дж. Хорнунг2, Ханс П. Липп3
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "923" ["VALUE"]=> string(19) "25.01.2015 17:40:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "25.01.2015 17:40:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "25.01.2015 17:40:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "924" ["VALUE"]=> string(19) "23.06.2015 17:40:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "23.06.2015 17:40:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "23.06.2015 17:40:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "925" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(6) { [0]=> string(4) "1180" [1]=> string(4) "1181" [2]=> string(4) "1182" [3]=> string(4) "1183" [4]=> string(4) "1184" [5]=> string(4) "1185" } ["VALUE"]=> array(6) { [0]=> string(2) "15" [1]=> string(2) "16" [2]=> string(2) "17" [3]=> string(2) "18" [4]=> string(2) "19" [5]=> string(2) "20" } ["DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(6) { [0]=> string(2) "15" [1]=> string(2) "16" [2]=> string(2) "17" [3]=> string(2) "18" [4]=> string(2) "19" [5]=> string(2) "20" } ["~DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(6) { [0]=> string(134) "трансплантация гемопоэтических стволовых клеток" [1]=> string(67) "химиотерапия" [2]=> string(92) "взаимодействие препаратов" [3]=> string(78) "клинические исходы" [4]=> string(86) "возрастная зависимость" [5]=> string(88) "альтернативная медицина" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "21" ["VALUE"]=> string(2) "11" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "11" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Axel R. Zander" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "99" ["VALUE"]=> array(2) { ["TEXT"]=> string(5589) "<h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.</p> <p class="Summery_Rus" lang="ru-RU">Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (<span class="CharOverride-4">Hypericum perforatum</span>), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.</p> <p class="Summery_Rus" lang="ru-RU">Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(5459) "Резюме
Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.
Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (Hypericum perforatum), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.
Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(5459) "Резюме
Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.
Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (Hypericum perforatum), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.
Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов.
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "98" ["VALUE"]=> array(2) { ["TEXT"]=> string(756) "<p class="Autor_place_work-Rus"><sup>1</sup>Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия </p> <p class="Autor_place_work-Rus"><sup>2</sup>Университетский медицинский центр Гамбург-Эппендорф, Германия</p> <p class="Autor_place_work-Rus"><sup>3</sup><span class="affiliation">Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия</span></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(632) "1Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия
2Университетский медицинский центр Гамбург-Эппендорф, Германия
3Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(632) "1Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия
2Университетский медицинский центр Гамбург-Эппендорф, Германия
3Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия
" } } } [3]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "2" ["~IBLOCK_SECTION_ID"]=> string(1) "2" ["ID"]=> string(2) "59" ["~ID"]=> string(2) "59" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["~NAME"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:43:27" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:43:27" ["DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-31-37/" ["~DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-31-37/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(29544) "
Introduction
Nijmegen breakage syndrome (NBS) is a rare autosomal recessive chromosome instability disorder which occurs worldwide with prevalence among Eastern and Central European population and caused by mutation in NBN gene at 8q21, the most often mutation 657-661delACAAA in 6 exon, named Slavic mutation [1-4]. Except of progressing microcephaly, low birth weight, growth retardation and characteristic bird-like facial features, it is characterized by combined immunodeficiency, radiosensitivity and high predisposition to malignancy development in childhood, mostly of lymphoid origin [5-6]. NBN gene encoding the nibrin protein plays a key role in DNA double-strand break repair and the maintenance of genomic stability. Insufficient function of defective nibrin decreases cellular response to DNA damage and results in genomic instability and finally can lead to cancer, which remains the most common cause of death in patients with NBS [7-8]. Other known causes of death are fatal infections and bone marrow aplasia [8]. Currently, no specific therapy is available for NBS. Substitution therapy with immunoglobulins is indicated in patients with agammaglobulinemia. Antibiotic prophylaxis is considered in patients with recurrent respiratory tract and urinary tract infections. Cancer treatment is accompanied by severe toxic complications and should be adapted to individual risk factors and tolerance [9-13]. The NBS patients are usually not subject to hematopoietic stem cells transplantation (HSCT), owing to concerns about increased toxicity. European experience of HSCT performed with reduced-intensity conditioning regimens in order to correct severe immunodeficiency or to treat refractory or recurring malignancy is limited but quite successful [14-15]. But there is still no consensus on optimal management of NBS patient, and no recommended options about benefits of HSCT and appropriate protocols for individual patients.
The aim of our review article was to share our experience in NBS management and to discuss indications for allo-HSCT performance. We presented here general clinical characteristics, laboratory data, treatment details and clinical outcomes of 19 Belarusian NBS patients.
Patients and Methods
According to data, provided by the Belarusian National Children Registry of primary immune deficiency (PID) diseases, a total of 238 children were diagnosed with PID until December 2014, including 18 cases of NBS. A single adult patient (21 years old) was diagnosed in our center as having NBS. The diagnosis of PID was based on the diagnostic PID criteria, as described in the last classification issued by the International Union of Immunological Societies Expert Committee for Primary Immunodeficiencies, 2013 [16].
To reveal and classify the PID condition, we used immunological criteria as well as genetic studies. Serum concentrations of immunoglobulins IgG, IgA and IgM were measured by immunonephelometry. Analysis of peripheral blood lymphocyte subpopulations was performed by flow cytometry. The blood cells were incubated with specific monoclonal antibodies (MoAbs) against CD45, CD3, CD4, CD8, CD16/CD56, CD19, CD31, CD45RA (obtained from Beckman Coulter and Beckton Dickinson). Recent thymic emigrants (RTE) were determined as CD4+CD45RA+CD31+ T cells.
Quantification of TRECs and KRECs was determined by RT-qPCR. Healthy age-matched donors of peripheral blood lymphocytes (n = 4) were taken as a control. RT-qPCR data were normalized with albumin control gene and calculated by 2-∆Ct [17]. Average values of TREC/KREC expression in healthy control group were taken as 100%, the patients’ results were presented as a percentage of control values. Statistical analysis was performed by Mann-Whitney U test and Spearman rank test.
Mutational analysis of exon 6 of the NBN gene was performed in all patients. Chromosomal instability assays reflecting increased chromosomal breakage in peripheral lymphocytes was evaluated in 5 patients. Chromosomal somatic mutations (translocations and/or inversions involving chromosomes 7 and 14) were revealed in 6 cases by conventional G-banding.
Nine NBS patients were diagnosed as having acute leukemia or non-Hodgkin lymphoma (NHL). Histological classification of haematopoietic neoplasms was performed and revised, according to World Health Organization classification, 2008 [18]. Immunophenotyping was carried out in eight cases by immunohistochemical analysis or by flow cytometry. The NHL staging was based on St.Jude criteria [19]. Chemotherapy was performed according to ALL-BFM 90/2000, ALL-MB 2008 (Moscow-Berlin), AML-MM 2003 (Moscow-Minsk) and NHL-BFM 90/95 regimens with some modifications [20-26]. One patient with peripheral T-cell lymphoma received individual chemotherapy (see below). Clinical data and outcomes are presented as by January l, 2015.
Parents of the patients provided written informed consent for leukemia/lymphoma treatment, as well as for blood sampling and processing for PID diagnostics, in accordance with protocols approved by the local Ethical Committee.
Results
NBS accounted for 8.0% of all the registered PID cases. A specific 657del5 mutation in the NBN gene was found in all 19 patients. Patient characteristics and immunological data are presented in Table 1. NBS occurrence was nearly equal in boys and girls (M:F ratio of 1.1:1). Median age at the NBS diagnosis was 7.1 years. NBS has been revealed only in 4 patients (21%) under 1 year old. In most cases, examination for PID and NBS was performed after recurrent infections or development of autoimmune disease, or in connection with lymphoma or leukemia diagnosis. In four cases the diagnosis of NBS was confirmed only post mortem.
Immunological investigations revealed highly variable immunological features of the NBS patients, without evident correlations between immune markers and degree of clinical immunodeficiency, or malignancy development. Abnormalities in immunoglobulin concentrations were found in 62.5% of examined patients. Just one child with hypogammaglobulinemia who received regular substitution therapy with intravenous immunoglobulin had no severe infections in anamnesis. All other patients had frequent or chronic respiratory infections. All NBS patients with autoimmune pathology, and half of the children with lymphoid malignancies had decreased serum immunoglobulin level. Moreover, two patients from our cohort developed lymphoid neoplasia at the age of 16 and 21 years, despite normal immunoglobulin serum levels and absence of frequent infections in anamnesis. Two other patients (without evidence of malignancy at the age of 3.7 and 5.7 years) had low numbers of CD3+ T cells (<300 cells/µL), thus indicative for pronounced abnormalities of T-cell immunity, similar to severe combined immunodeficiency. Expression of TREC and KREC mRNAs was detected at very low levels in all examined patients, including 5 children without malignancies. Immunophenotyping was performed to 13 NBS patients. A reduction of T- and/or B-cell immunity was revealed in all cases but the majority of patients had normal percentage and absolute number of CD3+ T-lymphocytes. Seven patients with low RTE level were analyzed for TRECs quantity. We found statistically significant decrease of the number of TRECs in NBS patients compared with healthy donors (p = 0.01). And a high correlation between RTE (%) and TRECs’ level was revealed (R = 0.89, p < 0.05).
Lymphoproliferative disorders occurred in 47.4% of all registered NBS patients and in 60.0% patients older than 4 years. The median age at the time of malignancy diagnosis was 10.7 years (ranged from 4 to 21). In 7 of 9 cases, NBS was diagnosed simultaneously or after the lymphoid neoplasm was confirmed. T cell malignancies prevailed in our series (7 out of 8 cases with identified immunophenotype, including one case with mixed phenotype, i.e., early T/myeloid leukemia), being T-mature in half of the cases. Some details of treatment and outcomes are presented in Table 2.
Despite full chemotherapy dosage, a complete remission (CR) was achieved only in 66.7% cases (6 out of 9 cases). Two patients died of infectious complications before CR was achieved, and one patient was lost with sepsis in the 1s CR, while on maintenance therapy. A patient with peripheral T cell lymphoma developed rapid tumor growth after short-term partial clinical response to chemotherapy and died of progression. One girl developed a secondary lymphoma 4.5 years after the treatment of diffuse large B-cell lymphoma. Three patients (two cases of T-mature lymphoblastic lymphoma, and one patient with ETP-ALL) did not respond to standard induction chemotherapy; their blast cells also had poor in vitro sensitivity to most cytostatics, as measured by MTT-test. In these patients, CR was achieved only after intensive chemotherapy (HR-blocks). The patient with ETP-ALL developed early relapse prior HSCT, and two others underwent unrelated HSCT and are alive with no evidence of disease at, resp., 6 and 13 months after transplantation. Overall, only two NBS patients (22.2%) with malignancy are alive in CR1 with a follow-up of 12 and 20 months.
All NBS patients exhibited grade 3 to 4 complications after chemotherapy. Of those, most common were neutropenic infections and hemostatic disorders. Three fatal outcomes were related to first-line treatment, two from sepsis and one patient with invasive aspergillosis and massive pulmonary bleeding. Unrecognized NBS was the main reason for non-reduced dose regimens during induction therapy.
Three patients from this cohort underwent allo-HSCT (HLA-matched sibling donor in one case, and matched unrelated donors in two cases). A graft from sibling donor was transplanted 9.8 years ago to a boy without malignancy, but with infectious and autoimmune disorders (Table 1, patient #4). His sister with NBS died from leukemia ten years earlier. Two other patients developed T-mature ALL/NHL without response to induction chemotherapy, as mentioned above (Table 2, patients #15, 16). They all received reduced-intensity conditioning regimens (Bu 8 mg/kg, FLU 150 mg/m2, ATG 90 mg/kg; MEL 140 mg/m2, FLU 125 mg/m2, ATG 60 mg/kg; MEL 140 mg/m2, FLU 150 mg/m2, ATG 60 mg/kg) that were well tolerated. Every patient experienced acute graft-versus host disease (GvHD) grade II-III. Extensive chronic GvHD developed in 2 patients. Cytomegalovirus infection occurred in 2 patients and adenovirus infection was found in one case.
Currently there are 9 NBS patients under our observation, ranging from 1.1 to 20.7 years of age, who did not undergo HSCT and have no signs of malignant disorders. Unfortunately, there are no data of any living older patients with NBS in Belarus.
Discussion
NBS is a rare disease, but the number of patients identified worldwide is rapidly increasing, probably because physicians are becoming more aware of the disorder. The frequency of NBN gene mutation carriers is rather high in the population of Slavic origin, being estimated as 1 case in 177 newborns [2]. The majority of Belarusian NBS patients are residents of the southwestern part of the country, likely as a result of a founder effect. Etiopathogenesis and clinical manifestations of NBS are well studied, but no specific therapy is available. Early diagnosis of NBS is crucial, in order to avoid even diagnostic irradiation, and to prevent severe and recurrent infections by appropriate management. Increasing number of newly diagnosed NBS cases and high risk of potential complications makes it necessary to develop optimal therapeutic strategies.
Only 21% of Belarusian patients were diagnosed as having NBS at the age less than 1 year. Moreover, 78% of NBS patients who developed lymphoma or leukemia were not recognized as immunodeficient before the malignancy became evident. Their immune status was, therefore, not tested, preventive measures were not complied, and they did not receive timely treatment with intravenous immunoglobulin. As a result, their initial infectious status supposed to be worse and made their management more challenging. Therefore, the most important thing to do is to diagnose NBS as early as possible.
Combined cellular and humoral immunodeficiency is an essential feature of the disease, unless the patients with NBS mutation had variable initial immune status with inevitably increasing immune insufficiency over time [27-28]. Unlike some other combined immunodeficiency syndromes, HSCT is not a recommended therapeutic approach for immune system restoration in NBS patients, due to the high risk of toxic complications. Meanwhile, life-long monitoring of the immune system allows for preventive measures and maintains the patients in good clinical condition for a long time. There are patients with very mild manifestations who do not suffer from frequent infections and do not need immunoglobulin supplementation. In most patients, however, a number of complications increase over time. Chronic infections leading to development of respiratory or renal failure, severe autoimmune pathology, or malignancy cause death of NBS patients in childhood or in younger adults [4, 28-31].
In the presented cohort, combined immunodeficiency was confirmed in all patients, whereas the degree of cellular and/or humoral immunodeficiency varied from very mild to severe with very low CD3+ cells counts or serum immunoglobulin levels, similar to manifestations of severe combined immunodeficiency. Severity of the complications also differed individually. Our adult NBS patient had no particular history of infections before ALL diagnosed at the age of 21 years, and his clinical condition was sufficiently satisfactory to perform full dose chemotherapy treatment and allo-HSCT (Table 2, patient #15). We have also treated another NBS patient who received adequate immunoglobulin supplementation, but multiple infectious and autoimmune complications urged us to limit the intensity of chemotherapy in the first lymphoma episode and made it impossible to perform treatment of the second lymphoma (Table 2, patient #3). This diversity in immune and clinical status implies a personalized therapeutic approach. Obviously, the patients with decreased immunoglobulin concentration need a substitution treatment. But we suppose that HSCT should be taken into consideration both for NBS patients with severe cellular or humoral immunodeficiency prior to the development of malignancies or other serious complications.
Patients with NBS have very high risk of cancer in childhood, mostly lymphoid malignancies, but medulloblastoma, rhabdomyosarcoma and some other tumors have been described as well [11, 32-34]. As reported by the International NBS Study Group and by the Polish NBS Registry, 40 to 60% of NBS patients develop NHL by the age of 20 years [11, 35-36]. We have obtained similar data, with 47% of NBS patients who developed lymphoproliferative disorders. The survival of children with PID-associated NHL is much lower in comparison with immunocompetent patients and ranges from 35 to 58% [9-13]. There are no specific treatment protocols designed for patients with NBS and NHL. Due to the higher risk of treatment-related toxicity, there is a common tendency to modify treatment by reducing dosage of some chemotherapy agents. Complication rate during cancer treatment was high in our cohort of children, thus being consistent with other reports [9, 11-12]. Tolerability of chemotherapy was limited mostly by infectious status rather than toxic side effects. In future, modified chemotherapy schemes combined with monoclonal antibodies should be designed for the treatment of patients with NBS and NHL.
Relapses or refractory cases of NHL occur more often in NBS than in immunocompetent patients and represent a major cause of treatment failure [9, 11-12]. Moreover, the surviving NBS patients are at increased risk for developing a second malignancy, more often, lymphoma [11, 37]. As a result, only few patients survived the whole-scale cancer treatment. There are some data on successful treatment of refractory or relapsed lymphoma with allo-HSCT in NBS patients [15]. Five out of 6 patients have restored T cell immunity and are alive, with a median follow up of 2.2 years. It has been suggested that HSCT should be considered for NBS patients with recurrent or second lymphoma.
In the present group, 87.5% patients (7 out of 8) were suffering from T cell lymphoid malignancies with T-mature immunophenotype in a half of cases, which is different from normal spectrum of ALL/NHL in immunocompetent children, since both T and B cell lymphoid neoplasms have been described, with some prevalence of B-cell lineage and a high recurrent disease rate in T cell malignancies [11-12, 37]. The outcome of our patients was poor with only 2 survivors (22.2%) after allo-HSCT with less than 2 years follow-up term. The reasons for this poor outcome were either infectious complications or treatment failure. More than half of the patients (5 out of 9) with NBS and malignancy did not respond to standard full dose chemotherapy or developed early relapse. Taking into account a case of secondary lymphoma development as a late event in the present cohort, the prognosis for patients with NBS and malignancies seems to be poor initially. However, despite limited tolerability of chemotherapy and a high rate of infectious complications, we demonstrated the possibility of safe allo-HSCT performance using reduced-intensity conditioning regimens.
In spite of small group under observation, we may assume that NBS patients are prone to develop T-ALL/NHL subtypes with limited curative potential. These patients may benefit from allo-HSCT as a consolidation therapy, in order to prevent relapse and to partially restore immune system, seeking to reduce the risk of secondary malignancies.
Conclusion
Our data show that NBS needs to be diagnosed at the early age. Taking into account a progressive immunodeficiency with deteriorating clinical state and extremely high risk of lymphoid malignancy with uncertain curative potential, allogeneic HSCT with reduced-intensity conditioning may be a rational therapeutic option for NBS patients with severe defects of immune function and for any NBS patients with lymphoid malignancy in first remission.
Conflict of interest
All authors have no conflict of interest to declare.
Acknowledgements
Authors gratefully acknowledges Mikhail V. Belevtsev, Chief, Belarusian National Children Registry of PID Diseases who provided information of PID cases; Dr.Svetlana N. Aleshkevich, (patient examination and collection of immunological data), Maria Stsegantseva, (PCR analysis of mutations), and to the physicians from our Center.
References
- Kleier S, Herrmann M, Wittwer B et al. Clinical presentation and mutation identification in the NBS1 gene in a boy with Nijmegen breakage syndrome. Clin Genet 2000, 57: 384-387.
- Varon R, Seemanova E, Chrzanowska K et al. Clinical ascertainment of Nijmegen breakage syndrome (NBS) and prevalence of the major mutation, 657del5, in three Slav populations. Eur J Hum Genet 2000, 8: 900-902.
- Mauer MH, Hoffmann K, Sperling K et al. High prevalence of the NBN gene mutation c.657-661del5 in Southeast Germany. J Appl Genet 2010, 51: 211-214.
- Seemanova E, Passarge E, Beneskova D et al. Familial microcephaly with normal intelligance, immunodeficiency, and risk for lymphoreticular malignancies: a new autosomal recessive disorder. Am J Med Genet 1985, 20: 639-648.
- De Miranda NF, Björkman A, Pan-Hammarström Q. DNA repair: the link between primary immunodeficiency and cancer. Ann NY Academy of Sciences 2011, 1246: 50–63.
- Tran H, Nourse J, Hall S et al. Immunodeficiency-associated lymphomas. Blood Reviews, 2008, 22: 261-281.
- Oertel S, Reiss H. Immunosurveillance, immunodeficiency and lymphoproliferations, Heidelberg: Springer, 2002.
- Chinen J, Anmuth D, Franklin AR et al. Long-term follow-up of patients with primary immunodeficiencies.
J Allergy and Clinical Immunology 2007, 120: 795-797. - Seidemann K, Tiemann M, Henze G et al. Therapy for Non-Hodgkin lymphoma in children with primary immunodeficiency: analysis of 19 patients from the BFM Trials. Med Pediatr Oncology 1999, 33: 536-544.
- Sandoval C, Swift M. Treatment of lymphoid malignancies in patients with ataxia teleangiectasia. Med Pediatr Oncology 1998, 31: 491-497.
- Dembowska-Baginska B, Perek D, Brozyna A et al. Non-Hodgkin lymphoma (NHL) in children with Nijmegen Breakage syndrome (NBS). Pediatr Blood Cancer 2009, 52: 186-190.
- Bienemann K, Burkhardt B, Modlich S et al. Promising therapy results for lymphoid malignancies in children with chromosomal breakage syndromes (Ataxia teleangiectasia or Nijmegen-breakage syndrome): a retrospective survey. Br J Haematology 2011, 155: 468-476.
- Sandlung JT, Hudson MM, Kennedy W et al. Pilot study of modified LMB-based therapy for children with ataxia-teleangiectasia and advanced stage high grade mature B-cell malignancies, Pediatr Blood Cancer 2014, 61: 360-362.
- New HV, Cale CM, Tischkowitz M et al. Nijmegen breakage syndrome diagnosed as Fanconi anaemia, Pediatr Blood Cancer 2005, 44: 494-499.
- Albert MH, Gennery AR, Greil J et al. Successful SCT for Nijmegen breakage syndrome. Bone Marrow Transplant 2010, 45: 622–626.
- Al-Herz W, Bousfiha A, Casanova JL et al. Primary immunodeficiency diseases: an update on the classification from the International Union of Immunological Societies Expert Committee for Primary Immunodeficiency. Front. Immunol. 2014, 5: art.162.
- Pfaff MW. Quantification strategies in real-time PCR. A – Z of quantitative PCR. 2004. Chapter 3: 87-112.
- Swerdlow SH, Campo E, Harris NL et al. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. IARC Pres, Lyon, France, 4th edition, 2008: 312-316.
- Murphy SB. Classification, staging and end results of treatment in childhood non-Hodgkin’s lymphoma: dissimilarities from lymphomas in adults. Semin in Oncology 1980, 7: 332-339.
- Schrappe M, Reiter A, Ludwig WD et al. Improved outcome in childhood acute lymphoblastic leukemia despite reduced use of anthracyclines and cranial radiotherapy: results of trial ALL-BFM 90. German-Austrian-Swiss ALL-BFM Study Group. Blood 2000, 95: 3310-22.
- Seidemann K, Tiemann M, Schrappe M et al. Short-pulse B-non-Hodgkin lymphoma-type chemotherapy is efficacious treatment for pediatric anaplastic large cell lymphoma: a report of the Berlin-Frankfurt-Munster Group Trial NHL-BFM 90. Blood 2001, 97: 3699-3706.
- Reiter A, Schrappe M, Tiemann M et al. Improved treatment results in childhood B-cell neoplasms with tailored intensification of therapy: a report of the Berlin-Frankfurt-Munster Group Trial NHL-BFM-90. Blood 1999, 94: 3294-3306.
- Burkhardt B, Woessmann W, Zimmermann M et al. Impact of cranial radiotherapy on central nervous system prophylaxix in children and adolescents with central nervous system-negative stage III or IV lymphoblastic lymphoma. J Clin Oncol 2006, 24: 491-499.
- Barovskaya Yu А, Aleinikova ОV. Results of pediatric AML treatment according to the AML-MM 2006 in Belarus. Meditsinsky Journal, 2014, №4: 56-59. (In Russian)
- Popov AM, Tsaur GA, Solodivnikov AG et al. Significance of different prognostic factors for occurrence of minimal residual disease in children with acute myeloblastic leukemia after induction therapy by the ALL-MB-2008 protocol. Voprosy Gematologii/Onkologii i Immunopatologii v Pediatrii, 2012; v.11: 20-27. (In Russian)
- Conter V, Bartram CR, Valsecchi MC et al. Molecular response to treatment redefines all prognostic factors in children and adolescents with B-cell precursor acute lymphoblastic leukemia: results in 3184 patients of the AIEOP-BFM ALL 2000 study. Blood 2010, 115: 3206-14.
- Gregorek H, Chrzanowska KH, Michalkiewicz J et al. Heterogeneity of humoral immune abnormalities in children with Nijmegen breakage syndrome: a 8-year follow-up study in a single centre. Clin Exp Immunol 2002, 130: 319-324.
- Gregorek H, Chrzanowska KH, Dzierzanowska-Fangrat K et al. Nijmegen breakage syndrome: long-term monitoring of viral and immunological biomarkers in peripheral blood before development of malignancy. Clin Immunol 2010, 135: 440-447.
- Resnick I, Kondratenko I, Togoev O et al. Nijmegen breakage syndrome: clinical characteristics and mutation analysis in eight unrelated Russian families. J Pediatr 2002, 140: 355-361.
- Kondratenko I, Paschenko O, Plyakov A et al. Nijmegen breakage syndrome. Adv Exp Med Biol 2007, 601: 61-67.
- Kostyuchenko L, Makuch H, Kitsera N et al. Nijmegen breakage syndrome in Ukraine: diagnostics and follow-up. Centr Eur J Immunol 2009, 34: 46-52.
- Distel L, Neubauer S, Varon R et al. Fatal toxicity following radio- and chemotherapy of medulloblastoma in a child with unrecognized Nijmegen breakage syndrome. Med Pediatr Oncol 2003, 41: 44-48.
- Bakhshi S, Cerosaletti KM, Concannon P et al. Medulloblastoma with adverse reaction to radiation therapy in Nijmegen breakage syndrome. J Pediatr Hematol Oncol 2003, 25: 248-251.
- Meyer S, Kingston H, Taylor A et al. Rhabdomyosarcoma in Nijmegen breakage syndrome: strong association with perianal primary site. Cancer Genet Cytogenet. 2004; 154: 169-174.
- Chrzanowska KH, Digweed M, Sperling K et al. DNA-repair deficiency and cancer: Lessons from lymphoma. Hereditary tumors. From genes to clinical consequences. Edited by: Allgayer H., Rehder H., Fulda S. Weinheim: WILEY-VH; 2009: 377-391.
- International Nijmegen breakage syndrome study group. Nijmegen breakage syndrome. Arch Dis Child 82: 400-406, 2000.
- Gładkowska-Dura M, Dzierzanowska-Fangrat K, Dura WT et al. Unique morphological spectrum of lymphomas in Nijmegen breakage syndrome (NBS) patients with high frequency of consecutive lymphoma formation.
J Pathol. 2008, 216: 337-44.
" ["~DETAIL_TEXT"]=> string(29544) "
Introduction
Nijmegen breakage syndrome (NBS) is a rare autosomal recessive chromosome instability disorder which occurs worldwide with prevalence among Eastern and Central European population and caused by mutation in NBN gene at 8q21, the most often mutation 657-661delACAAA in 6 exon, named Slavic mutation [1-4]. Except of progressing microcephaly, low birth weight, growth retardation and characteristic bird-like facial features, it is characterized by combined immunodeficiency, radiosensitivity and high predisposition to malignancy development in childhood, mostly of lymphoid origin [5-6]. NBN gene encoding the nibrin protein plays a key role in DNA double-strand break repair and the maintenance of genomic stability. Insufficient function of defective nibrin decreases cellular response to DNA damage and results in genomic instability and finally can lead to cancer, which remains the most common cause of death in patients with NBS [7-8]. Other known causes of death are fatal infections and bone marrow aplasia [8]. Currently, no specific therapy is available for NBS. Substitution therapy with immunoglobulins is indicated in patients with agammaglobulinemia. Antibiotic prophylaxis is considered in patients with recurrent respiratory tract and urinary tract infections. Cancer treatment is accompanied by severe toxic complications and should be adapted to individual risk factors and tolerance [9-13]. The NBS patients are usually not subject to hematopoietic stem cells transplantation (HSCT), owing to concerns about increased toxicity. European experience of HSCT performed with reduced-intensity conditioning regimens in order to correct severe immunodeficiency or to treat refractory or recurring malignancy is limited but quite successful [14-15]. But there is still no consensus on optimal management of NBS patient, and no recommended options about benefits of HSCT and appropriate protocols for individual patients.
The aim of our review article was to share our experience in NBS management and to discuss indications for allo-HSCT performance. We presented here general clinical characteristics, laboratory data, treatment details and clinical outcomes of 19 Belarusian NBS patients.
Patients and Methods
According to data, provided by the Belarusian National Children Registry of primary immune deficiency (PID) diseases, a total of 238 children were diagnosed with PID until December 2014, including 18 cases of NBS. A single adult patient (21 years old) was diagnosed in our center as having NBS. The diagnosis of PID was based on the diagnostic PID criteria, as described in the last classification issued by the International Union of Immunological Societies Expert Committee for Primary Immunodeficiencies, 2013 [16].
To reveal and classify the PID condition, we used immunological criteria as well as genetic studies. Serum concentrations of immunoglobulins IgG, IgA and IgM were measured by immunonephelometry. Analysis of peripheral blood lymphocyte subpopulations was performed by flow cytometry. The blood cells were incubated with specific monoclonal antibodies (MoAbs) against CD45, CD3, CD4, CD8, CD16/CD56, CD19, CD31, CD45RA (obtained from Beckman Coulter and Beckton Dickinson). Recent thymic emigrants (RTE) were determined as CD4+CD45RA+CD31+ T cells.
Quantification of TRECs and KRECs was determined by RT-qPCR. Healthy age-matched donors of peripheral blood lymphocytes (n = 4) were taken as a control. RT-qPCR data were normalized with albumin control gene and calculated by 2-∆Ct [17]. Average values of TREC/KREC expression in healthy control group were taken as 100%, the patients’ results were presented as a percentage of control values. Statistical analysis was performed by Mann-Whitney U test and Spearman rank test.
Mutational analysis of exon 6 of the NBN gene was performed in all patients. Chromosomal instability assays reflecting increased chromosomal breakage in peripheral lymphocytes was evaluated in 5 patients. Chromosomal somatic mutations (translocations and/or inversions involving chromosomes 7 and 14) were revealed in 6 cases by conventional G-banding.
Nine NBS patients were diagnosed as having acute leukemia or non-Hodgkin lymphoma (NHL). Histological classification of haematopoietic neoplasms was performed and revised, according to World Health Organization classification, 2008 [18]. Immunophenotyping was carried out in eight cases by immunohistochemical analysis or by flow cytometry. The NHL staging was based on St.Jude criteria [19]. Chemotherapy was performed according to ALL-BFM 90/2000, ALL-MB 2008 (Moscow-Berlin), AML-MM 2003 (Moscow-Minsk) and NHL-BFM 90/95 regimens with some modifications [20-26]. One patient with peripheral T-cell lymphoma received individual chemotherapy (see below). Clinical data and outcomes are presented as by January l, 2015.
Parents of the patients provided written informed consent for leukemia/lymphoma treatment, as well as for blood sampling and processing for PID diagnostics, in accordance with protocols approved by the local Ethical Committee.
Results
NBS accounted for 8.0% of all the registered PID cases. A specific 657del5 mutation in the NBN gene was found in all 19 patients. Patient characteristics and immunological data are presented in Table 1. NBS occurrence was nearly equal in boys and girls (M:F ratio of 1.1:1). Median age at the NBS diagnosis was 7.1 years. NBS has been revealed only in 4 patients (21%) under 1 year old. In most cases, examination for PID and NBS was performed after recurrent infections or development of autoimmune disease, or in connection with lymphoma or leukemia diagnosis. In four cases the diagnosis of NBS was confirmed only post mortem.
Immunological investigations revealed highly variable immunological features of the NBS patients, without evident correlations between immune markers and degree of clinical immunodeficiency, or malignancy development. Abnormalities in immunoglobulin concentrations were found in 62.5% of examined patients. Just one child with hypogammaglobulinemia who received regular substitution therapy with intravenous immunoglobulin had no severe infections in anamnesis. All other patients had frequent or chronic respiratory infections. All NBS patients with autoimmune pathology, and half of the children with lymphoid malignancies had decreased serum immunoglobulin level. Moreover, two patients from our cohort developed lymphoid neoplasia at the age of 16 and 21 years, despite normal immunoglobulin serum levels and absence of frequent infections in anamnesis. Two other patients (without evidence of malignancy at the age of 3.7 and 5.7 years) had low numbers of CD3+ T cells (<300 cells/µL), thus indicative for pronounced abnormalities of T-cell immunity, similar to severe combined immunodeficiency. Expression of TREC and KREC mRNAs was detected at very low levels in all examined patients, including 5 children without malignancies. Immunophenotyping was performed to 13 NBS patients. A reduction of T- and/or B-cell immunity was revealed in all cases but the majority of patients had normal percentage and absolute number of CD3+ T-lymphocytes. Seven patients with low RTE level were analyzed for TRECs quantity. We found statistically significant decrease of the number of TRECs in NBS patients compared with healthy donors (p = 0.01). And a high correlation between RTE (%) and TRECs’ level was revealed (R = 0.89, p < 0.05).
Lymphoproliferative disorders occurred in 47.4% of all registered NBS patients and in 60.0% patients older than 4 years. The median age at the time of malignancy diagnosis was 10.7 years (ranged from 4 to 21). In 7 of 9 cases, NBS was diagnosed simultaneously or after the lymphoid neoplasm was confirmed. T cell malignancies prevailed in our series (7 out of 8 cases with identified immunophenotype, including one case with mixed phenotype, i.e., early T/myeloid leukemia), being T-mature in half of the cases. Some details of treatment and outcomes are presented in Table 2.
Despite full chemotherapy dosage, a complete remission (CR) was achieved only in 66.7% cases (6 out of 9 cases). Two patients died of infectious complications before CR was achieved, and one patient was lost with sepsis in the 1s CR, while on maintenance therapy. A patient with peripheral T cell lymphoma developed rapid tumor growth after short-term partial clinical response to chemotherapy and died of progression. One girl developed a secondary lymphoma 4.5 years after the treatment of diffuse large B-cell lymphoma. Three patients (two cases of T-mature lymphoblastic lymphoma, and one patient with ETP-ALL) did not respond to standard induction chemotherapy; their blast cells also had poor in vitro sensitivity to most cytostatics, as measured by MTT-test. In these patients, CR was achieved only after intensive chemotherapy (HR-blocks). The patient with ETP-ALL developed early relapse prior HSCT, and two others underwent unrelated HSCT and are alive with no evidence of disease at, resp., 6 and 13 months after transplantation. Overall, only two NBS patients (22.2%) with malignancy are alive in CR1 with a follow-up of 12 and 20 months.
All NBS patients exhibited grade 3 to 4 complications after chemotherapy. Of those, most common were neutropenic infections and hemostatic disorders. Three fatal outcomes were related to first-line treatment, two from sepsis and one patient with invasive aspergillosis and massive pulmonary bleeding. Unrecognized NBS was the main reason for non-reduced dose regimens during induction therapy.
Three patients from this cohort underwent allo-HSCT (HLA-matched sibling donor in one case, and matched unrelated donors in two cases). A graft from sibling donor was transplanted 9.8 years ago to a boy without malignancy, but with infectious and autoimmune disorders (Table 1, patient #4). His sister with NBS died from leukemia ten years earlier. Two other patients developed T-mature ALL/NHL without response to induction chemotherapy, as mentioned above (Table 2, patients #15, 16). They all received reduced-intensity conditioning regimens (Bu 8 mg/kg, FLU 150 mg/m2, ATG 90 mg/kg; MEL 140 mg/m2, FLU 125 mg/m2, ATG 60 mg/kg; MEL 140 mg/m2, FLU 150 mg/m2, ATG 60 mg/kg) that were well tolerated. Every patient experienced acute graft-versus host disease (GvHD) grade II-III. Extensive chronic GvHD developed in 2 patients. Cytomegalovirus infection occurred in 2 patients and adenovirus infection was found in one case.
Currently there are 9 NBS patients under our observation, ranging from 1.1 to 20.7 years of age, who did not undergo HSCT and have no signs of malignant disorders. Unfortunately, there are no data of any living older patients with NBS in Belarus.
Discussion
NBS is a rare disease, but the number of patients identified worldwide is rapidly increasing, probably because physicians are becoming more aware of the disorder. The frequency of NBN gene mutation carriers is rather high in the population of Slavic origin, being estimated as 1 case in 177 newborns [2]. The majority of Belarusian NBS patients are residents of the southwestern part of the country, likely as a result of a founder effect. Etiopathogenesis and clinical manifestations of NBS are well studied, but no specific therapy is available. Early diagnosis of NBS is crucial, in order to avoid even diagnostic irradiation, and to prevent severe and recurrent infections by appropriate management. Increasing number of newly diagnosed NBS cases and high risk of potential complications makes it necessary to develop optimal therapeutic strategies.
Only 21% of Belarusian patients were diagnosed as having NBS at the age less than 1 year. Moreover, 78% of NBS patients who developed lymphoma or leukemia were not recognized as immunodeficient before the malignancy became evident. Their immune status was, therefore, not tested, preventive measures were not complied, and they did not receive timely treatment with intravenous immunoglobulin. As a result, their initial infectious status supposed to be worse and made their management more challenging. Therefore, the most important thing to do is to diagnose NBS as early as possible.
Combined cellular and humoral immunodeficiency is an essential feature of the disease, unless the patients with NBS mutation had variable initial immune status with inevitably increasing immune insufficiency over time [27-28]. Unlike some other combined immunodeficiency syndromes, HSCT is not a recommended therapeutic approach for immune system restoration in NBS patients, due to the high risk of toxic complications. Meanwhile, life-long monitoring of the immune system allows for preventive measures and maintains the patients in good clinical condition for a long time. There are patients with very mild manifestations who do not suffer from frequent infections and do not need immunoglobulin supplementation. In most patients, however, a number of complications increase over time. Chronic infections leading to development of respiratory or renal failure, severe autoimmune pathology, or malignancy cause death of NBS patients in childhood or in younger adults [4, 28-31].
In the presented cohort, combined immunodeficiency was confirmed in all patients, whereas the degree of cellular and/or humoral immunodeficiency varied from very mild to severe with very low CD3+ cells counts or serum immunoglobulin levels, similar to manifestations of severe combined immunodeficiency. Severity of the complications also differed individually. Our adult NBS patient had no particular history of infections before ALL diagnosed at the age of 21 years, and his clinical condition was sufficiently satisfactory to perform full dose chemotherapy treatment and allo-HSCT (Table 2, patient #15). We have also treated another NBS patient who received adequate immunoglobulin supplementation, but multiple infectious and autoimmune complications urged us to limit the intensity of chemotherapy in the first lymphoma episode and made it impossible to perform treatment of the second lymphoma (Table 2, patient #3). This diversity in immune and clinical status implies a personalized therapeutic approach. Obviously, the patients with decreased immunoglobulin concentration need a substitution treatment. But we suppose that HSCT should be taken into consideration both for NBS patients with severe cellular or humoral immunodeficiency prior to the development of malignancies or other serious complications.
Patients with NBS have very high risk of cancer in childhood, mostly lymphoid malignancies, but medulloblastoma, rhabdomyosarcoma and some other tumors have been described as well [11, 32-34]. As reported by the International NBS Study Group and by the Polish NBS Registry, 40 to 60% of NBS patients develop NHL by the age of 20 years [11, 35-36]. We have obtained similar data, with 47% of NBS patients who developed lymphoproliferative disorders. The survival of children with PID-associated NHL is much lower in comparison with immunocompetent patients and ranges from 35 to 58% [9-13]. There are no specific treatment protocols designed for patients with NBS and NHL. Due to the higher risk of treatment-related toxicity, there is a common tendency to modify treatment by reducing dosage of some chemotherapy agents. Complication rate during cancer treatment was high in our cohort of children, thus being consistent with other reports [9, 11-12]. Tolerability of chemotherapy was limited mostly by infectious status rather than toxic side effects. In future, modified chemotherapy schemes combined with monoclonal antibodies should be designed for the treatment of patients with NBS and NHL.
Relapses or refractory cases of NHL occur more often in NBS than in immunocompetent patients and represent a major cause of treatment failure [9, 11-12]. Moreover, the surviving NBS patients are at increased risk for developing a second malignancy, more often, lymphoma [11, 37]. As a result, only few patients survived the whole-scale cancer treatment. There are some data on successful treatment of refractory or relapsed lymphoma with allo-HSCT in NBS patients [15]. Five out of 6 patients have restored T cell immunity and are alive, with a median follow up of 2.2 years. It has been suggested that HSCT should be considered for NBS patients with recurrent or second lymphoma.
In the present group, 87.5% patients (7 out of 8) were suffering from T cell lymphoid malignancies with T-mature immunophenotype in a half of cases, which is different from normal spectrum of ALL/NHL in immunocompetent children, since both T and B cell lymphoid neoplasms have been described, with some prevalence of B-cell lineage and a high recurrent disease rate in T cell malignancies [11-12, 37]. The outcome of our patients was poor with only 2 survivors (22.2%) after allo-HSCT with less than 2 years follow-up term. The reasons for this poor outcome were either infectious complications or treatment failure. More than half of the patients (5 out of 9) with NBS and malignancy did not respond to standard full dose chemotherapy or developed early relapse. Taking into account a case of secondary lymphoma development as a late event in the present cohort, the prognosis for patients with NBS and malignancies seems to be poor initially. However, despite limited tolerability of chemotherapy and a high rate of infectious complications, we demonstrated the possibility of safe allo-HSCT performance using reduced-intensity conditioning regimens.
In spite of small group under observation, we may assume that NBS patients are prone to develop T-ALL/NHL subtypes with limited curative potential. These patients may benefit from allo-HSCT as a consolidation therapy, in order to prevent relapse and to partially restore immune system, seeking to reduce the risk of secondary malignancies.
Conclusion
Our data show that NBS needs to be diagnosed at the early age. Taking into account a progressive immunodeficiency with deteriorating clinical state and extremely high risk of lymphoid malignancy with uncertain curative potential, allogeneic HSCT with reduced-intensity conditioning may be a rational therapeutic option for NBS patients with severe defects of immune function and for any NBS patients with lymphoid malignancy in first remission.
Conflict of interest
All authors have no conflict of interest to declare.
Acknowledgements
Authors gratefully acknowledges Mikhail V. Belevtsev, Chief, Belarusian National Children Registry of PID Diseases who provided information of PID cases; Dr.Svetlana N. Aleshkevich, (patient examination and collection of immunological data), Maria Stsegantseva, (PCR analysis of mutations), and to the physicians from our Center.
References
- Kleier S, Herrmann M, Wittwer B et al. Clinical presentation and mutation identification in the NBS1 gene in a boy with Nijmegen breakage syndrome. Clin Genet 2000, 57: 384-387.
- Varon R, Seemanova E, Chrzanowska K et al. Clinical ascertainment of Nijmegen breakage syndrome (NBS) and prevalence of the major mutation, 657del5, in three Slav populations. Eur J Hum Genet 2000, 8: 900-902.
- Mauer MH, Hoffmann K, Sperling K et al. High prevalence of the NBN gene mutation c.657-661del5 in Southeast Germany. J Appl Genet 2010, 51: 211-214.
- Seemanova E, Passarge E, Beneskova D et al. Familial microcephaly with normal intelligance, immunodeficiency, and risk for lymphoreticular malignancies: a new autosomal recessive disorder. Am J Med Genet 1985, 20: 639-648.
- De Miranda NF, Björkman A, Pan-Hammarström Q. DNA repair: the link between primary immunodeficiency and cancer. Ann NY Academy of Sciences 2011, 1246: 50–63.
- Tran H, Nourse J, Hall S et al. Immunodeficiency-associated lymphomas. Blood Reviews, 2008, 22: 261-281.
- Oertel S, Reiss H. Immunosurveillance, immunodeficiency and lymphoproliferations, Heidelberg: Springer, 2002.
- Chinen J, Anmuth D, Franklin AR et al. Long-term follow-up of patients with primary immunodeficiencies.
J Allergy and Clinical Immunology 2007, 120: 795-797. - Seidemann K, Tiemann M, Henze G et al. Therapy for Non-Hodgkin lymphoma in children with primary immunodeficiency: analysis of 19 patients from the BFM Trials. Med Pediatr Oncology 1999, 33: 536-544.
- Sandoval C, Swift M. Treatment of lymphoid malignancies in patients with ataxia teleangiectasia. Med Pediatr Oncology 1998, 31: 491-497.
- Dembowska-Baginska B, Perek D, Brozyna A et al. Non-Hodgkin lymphoma (NHL) in children with Nijmegen Breakage syndrome (NBS). Pediatr Blood Cancer 2009, 52: 186-190.
- Bienemann K, Burkhardt B, Modlich S et al. Promising therapy results for lymphoid malignancies in children with chromosomal breakage syndromes (Ataxia teleangiectasia or Nijmegen-breakage syndrome): a retrospective survey. Br J Haematology 2011, 155: 468-476.
- Sandlung JT, Hudson MM, Kennedy W et al. Pilot study of modified LMB-based therapy for children with ataxia-teleangiectasia and advanced stage high grade mature B-cell malignancies, Pediatr Blood Cancer 2014, 61: 360-362.
- New HV, Cale CM, Tischkowitz M et al. Nijmegen breakage syndrome diagnosed as Fanconi anaemia, Pediatr Blood Cancer 2005, 44: 494-499.
- Albert MH, Gennery AR, Greil J et al. Successful SCT for Nijmegen breakage syndrome. Bone Marrow Transplant 2010, 45: 622–626.
- Al-Herz W, Bousfiha A, Casanova JL et al. Primary immunodeficiency diseases: an update on the classification from the International Union of Immunological Societies Expert Committee for Primary Immunodeficiency. Front. Immunol. 2014, 5: art.162.
- Pfaff MW. Quantification strategies in real-time PCR. A – Z of quantitative PCR. 2004. Chapter 3: 87-112.
- Swerdlow SH, Campo E, Harris NL et al. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. IARC Pres, Lyon, France, 4th edition, 2008: 312-316.
- Murphy SB. Classification, staging and end results of treatment in childhood non-Hodgkin’s lymphoma: dissimilarities from lymphomas in adults. Semin in Oncology 1980, 7: 332-339.
- Schrappe M, Reiter A, Ludwig WD et al. Improved outcome in childhood acute lymphoblastic leukemia despite reduced use of anthracyclines and cranial radiotherapy: results of trial ALL-BFM 90. German-Austrian-Swiss ALL-BFM Study Group. Blood 2000, 95: 3310-22.
- Seidemann K, Tiemann M, Schrappe M et al. Short-pulse B-non-Hodgkin lymphoma-type chemotherapy is efficacious treatment for pediatric anaplastic large cell lymphoma: a report of the Berlin-Frankfurt-Munster Group Trial NHL-BFM 90. Blood 2001, 97: 3699-3706.
- Reiter A, Schrappe M, Tiemann M et al. Improved treatment results in childhood B-cell neoplasms with tailored intensification of therapy: a report of the Berlin-Frankfurt-Munster Group Trial NHL-BFM-90. Blood 1999, 94: 3294-3306.
- Burkhardt B, Woessmann W, Zimmermann M et al. Impact of cranial radiotherapy on central nervous system prophylaxix in children and adolescents with central nervous system-negative stage III or IV lymphoblastic lymphoma. J Clin Oncol 2006, 24: 491-499.
- Barovskaya Yu А, Aleinikova ОV. Results of pediatric AML treatment according to the AML-MM 2006 in Belarus. Meditsinsky Journal, 2014, №4: 56-59. (In Russian)
- Popov AM, Tsaur GA, Solodivnikov AG et al. Significance of different prognostic factors for occurrence of minimal residual disease in children with acute myeloblastic leukemia after induction therapy by the ALL-MB-2008 protocol. Voprosy Gematologii/Onkologii i Immunopatologii v Pediatrii, 2012; v.11: 20-27. (In Russian)
- Conter V, Bartram CR, Valsecchi MC et al. Molecular response to treatment redefines all prognostic factors in children and adolescents with B-cell precursor acute lymphoblastic leukemia: results in 3184 patients of the AIEOP-BFM ALL 2000 study. Blood 2010, 115: 3206-14.
- Gregorek H, Chrzanowska KH, Michalkiewicz J et al. Heterogeneity of humoral immune abnormalities in children with Nijmegen breakage syndrome: a 8-year follow-up study in a single centre. Clin Exp Immunol 2002, 130: 319-324.
- Gregorek H, Chrzanowska KH, Dzierzanowska-Fangrat K et al. Nijmegen breakage syndrome: long-term monitoring of viral and immunological biomarkers in peripheral blood before development of malignancy. Clin Immunol 2010, 135: 440-447.
- Resnick I, Kondratenko I, Togoev O et al. Nijmegen breakage syndrome: clinical characteristics and mutation analysis in eight unrelated Russian families. J Pediatr 2002, 140: 355-361.
- Kondratenko I, Paschenko O, Plyakov A et al. Nijmegen breakage syndrome. Adv Exp Med Biol 2007, 601: 61-67.
- Kostyuchenko L, Makuch H, Kitsera N et al. Nijmegen breakage syndrome in Ukraine: diagnostics and follow-up. Centr Eur J Immunol 2009, 34: 46-52.
- Distel L, Neubauer S, Varon R et al. Fatal toxicity following radio- and chemotherapy of medulloblastoma in a child with unrecognized Nijmegen breakage syndrome. Med Pediatr Oncol 2003, 41: 44-48.
- Bakhshi S, Cerosaletti KM, Concannon P et al. Medulloblastoma with adverse reaction to radiation therapy in Nijmegen breakage syndrome. J Pediatr Hematol Oncol 2003, 25: 248-251.
- Meyer S, Kingston H, Taylor A et al. Rhabdomyosarcoma in Nijmegen breakage syndrome: strong association with perianal primary site. Cancer Genet Cytogenet. 2004; 154: 169-174.
- Chrzanowska KH, Digweed M, Sperling K et al. DNA-repair deficiency and cancer: Lessons from lymphoma. Hereditary tumors. From genes to clinical consequences. Edited by: Allgayer H., Rehder H., Fulda S. Weinheim: WILEY-VH; 2009: 377-391.
- International Nijmegen breakage syndrome study group. Nijmegen breakage syndrome. Arch Dis Child 82: 400-406, 2000.
- Gładkowska-Dura M, Dzierzanowska-Fangrat K, Dura WT et al. Unique morphological spectrum of lymphomas in Nijmegen breakage syndrome (NBS) patients with high frequency of consecutive lymphoma formation.
J Pathol. 2008, 216: 337-44.
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "500" ["~SORT"]=> string(3) "500" ["CODE"]=> string(26) "1866-8836-2015-4-1-2-31-37" ["~CODE"]=> string(26) "1866-8836-2015-4-1-2-31-37" ["EXTERNAL_ID"]=> string(2) "59" ["~EXTERNAL_ID"]=> string(2) "59" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["ELEMENT_META_KEYWORDS"]=> string(134) "Синдром Ниймеген иммунодефицит лимфома трансплантация стволовых клеток" ["ELEMENT_META_DESCRIPTION"]=> string(371) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт БеларусиShould Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(4903) "<p class="Summery">Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.</p> <p class="Summery">Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии. </p> <p class="Summery">Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена <span lang="en-US">NBN</span>. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.</p> <p class="Summery">Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661<span lang="en-US">delACAAA</span> в гене <span lang="en-US">NBN</span> и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (<span lang="en-US">III</span> стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.</p> <p class="Summery">Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.</p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_META_TITLE"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_META_KEYWORDS"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_META_DESCRIPTION"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_PICTURE_FILE_ALT"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_PICTURE_FILE_TITLE"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_PICTURE_FILE_NAME"]=> string(100) "rol-allogennoy-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-v-lechenii-patsientov-s-sindromom" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(224) "Роль аллогенной трансплантации гемопоэтических стволовых клеток в лечении пациентов с синдромом Ниймеген. Опыт Беларуси" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(100) "rol-allogennoy-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-v-lechenii-patsientov-s-sindromom" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(100) "rol-allogennoy-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-v-lechenii-patsientov-s-sindromom" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(100) "rol-allogennoy-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-v-lechenii-patsientov-s-sindromom" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(1) "2" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(4) { [0]=> string(4) "1212" [1]=> string(4) "1213" [2]=> string(4) "1214" [3]=> string(4) "1215" } ["VALUE"]=> array(4) { [0]=> string(2) "54" [1]=> string(2) "56" [2]=> string(2) "57" [3]=> string(2) "58" } ["DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(4) { [0]=> string(2) "54" [1]=> string(2) "56" [2]=> string(2) "57" [3]=> string(2) "58" } ["~DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "290" ["VALUE"]=> string(19) "27.02.2015 14:23:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "27.02.2015 14:23:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "291" ["VALUE"]=> string(19) "12.06.2015 14:23:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "12.06.2015 14:23:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "872" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "292" ["VALUE"]=> string(2) "51" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "51" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(3) { [0]=> string(3) "293" [1]=> string(3) "294" [2]=> string(3) "295" } ["VALUE"]=> array(3) { [0]=> string(2) "52" [1]=> string(2) "51" [2]=> string(2) "53" } ["DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(3) { [0]=> string(2) "52" [1]=> string(2) "51" [2]=> string(2) "53" } ["~DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "296" ["VALUE"]=> array(2) { ["TEXT"]=> string(151) "<p class="Autor">Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(129) "
Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "297" ["VALUE"]=> array(2) { ["TEXT"]=> string(262) "<p class="Autor_place_work">Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(240) "Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "298" ["VALUE"]=> array(2) { ["TEXT"]=> string(4903) "<p class="Summery">Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.</p> <p class="Summery">Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии. </p> <p class="Summery">Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена <span lang="en-US">NBN</span>. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.</p> <p class="Summery">Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661<span lang="en-US">delACAAA</span> в гене <span lang="en-US">NBN</span> и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (<span lang="en-US">III</span> стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.</p> <p class="Summery">Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(4705) "Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.
Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии.
Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена NBN. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.
Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661delACAAA в гене NBN и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (III стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.
Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "299" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-31-37" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-31-37" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "300" ["VALUE"]=> array(2) { ["TEXT"]=> string(103) "<p class="Autor">Olga V. Aleinikova, Alina S. Fedorova, Svetlana O. Sharapova</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(81) "Olga V. Aleinikova, Alina S. Fedorova, Svetlana O. Sharapova
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "301" ["VALUE"]=> array(2) { ["TEXT"]=> string(153) "<p class="Autor_place_work">Belarusian Research Center for Pediatric Oncology, Hematology and Immunology, Minsk Region, Belarus</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(131) "Belarusian Research Center for Pediatric Oncology, Hematology and Immunology, Minsk Region, Belarus
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "302" ["VALUE"]=> array(2) { ["TEXT"]=> string(2827) "<h2>Summery </h2> <p class="Summery"> Introduction: Nijmegen breakage syndrome (NBS) is characterized by chromosome instability, combined immunodeficiency, radiosensitivity and high predisposition to lymphoid malignancy. A specific therapy is not available, however, hematopoietic stem cell transplantation (HSCT) is considered for NBS patients with refractory or recurrent leukemia or lymphoma. </p> <p class="Summery"> Purpose: We aimed to present Belarusian data in NBS diagnosis and management and to discuss indications for allo-HSCT treatment. </p> <p class="Summery"> Patients and Methods: A total of 238 patients were registered with primary immune deficiency (PID), including 19 cases of NBS. DNA was analyzed for mutation in NBN gene by direct sequencing of exon 6. Histological classification of lymphoid neoplasms was performed according to World Health Organization classification (2008). The patients were treated according to modified pediatric regimens or individually. </p> <p class="Summery"> Results: NBS accounted for 8.0% of all PID cases and was diagnosed at the age from 0.3 to 21.6 years (median 7.1). Mutation 657-661delACAAA in NBN gene and combined immunodeficiency of various degrees was confirmed in all patients. Lymphoid malignancy developed in 9 (47.4%) NBS patients ageing from 4.3 to 21.6 years (median 10.7). Acute leukemia was diagnosed in 4 patients, and stage III non-Hodgkin’s lymphoma in 5. Lymphoma/leukemia were in 7 out of 9 cases of T-cell origin. Complete remission (CR) was achieved in 66.7% of the patients.. Events were: death from infections in induction or in CR1 in 3 patients, progression/relapse in 3, second lymphoma in 1. Totally 7 NBS patients died, all after the development of malignancies. Two patients with T-mature lymphoma/leukemia did not respond to induction chemotherapy, were treated with unrelated HSCT in the 1CT and alive disease free within 6 and 13 months after transplantation. HSCT from a sibling donor was performed 9.8 years ago in a boy without malignancy but with infectious and autoimmune complications. They all received reduced-intensity conditioning regimens, which were well tolerated. </p> <p class="Summery"> Conclusions:<span class="CharOverride-10"> </span>NBS needs to be diagnosed early. With respect to progressive immunodeficiency and high risk of lymphoid malignancies with uncertain curative prospective, an allo-HSCT approach with reduced-intensity conditioning could be proposed as a treatment option for NBS patients with severe defects of immune function, and for all NBS patients with lymphoid malignancy in 1<sup>st</sup> complete remission. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2671) "Summery
Introduction: Nijmegen breakage syndrome (NBS) is characterized by chromosome instability, combined immunodeficiency, radiosensitivity and high predisposition to lymphoid malignancy. A specific therapy is not available, however, hematopoietic stem cell transplantation (HSCT) is considered for NBS patients with refractory or recurrent leukemia or lymphoma.
Purpose: We aimed to present Belarusian data in NBS diagnosis and management and to discuss indications for allo-HSCT treatment.
Patients and Methods: A total of 238 patients were registered with primary immune deficiency (PID), including 19 cases of NBS. DNA was analyzed for mutation in NBN gene by direct sequencing of exon 6. Histological classification of lymphoid neoplasms was performed according to World Health Organization classification (2008). The patients were treated according to modified pediatric regimens or individually.
Results: NBS accounted for 8.0% of all PID cases and was diagnosed at the age from 0.3 to 21.6 years (median 7.1). Mutation 657-661delACAAA in NBN gene and combined immunodeficiency of various degrees was confirmed in all patients. Lymphoid malignancy developed in 9 (47.4%) NBS patients ageing from 4.3 to 21.6 years (median 10.7). Acute leukemia was diagnosed in 4 patients, and stage III non-Hodgkin’s lymphoma in 5. Lymphoma/leukemia were in 7 out of 9 cases of T-cell origin. Complete remission (CR) was achieved in 66.7% of the patients.. Events were: death from infections in induction or in CR1 in 3 patients, progression/relapse in 3, second lymphoma in 1. Totally 7 NBS patients died, all after the development of malignancies. Two patients with T-mature lymphoma/leukemia did not respond to induction chemotherapy, were treated with unrelated HSCT in the 1CT and alive disease free within 6 and 13 months after transplantation. HSCT from a sibling donor was performed 9.8 years ago in a boy without malignancy but with infectious and autoimmune complications. They all received reduced-intensity conditioning regimens, which were well tolerated.
Conclusions: NBS needs to be diagnosed early. With respect to progressive immunodeficiency and high risk of lymphoid malignancies with uncertain curative prospective, an allo-HSCT approach with reduced-intensity conditioning could be proposed as a treatment option for NBS patients with severe defects of immune function, and for all NBS patients with lymphoid malignancy in 1st complete remission.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "303" ["VALUE"]=> string(147) "Should Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(147) "Should Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1216" ["VALUE"]=> string(2) "16" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "16" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1217" ["VALUE"]=> string(2) "17" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "17" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(14) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "300" ["VALUE"]=> array(2) { ["TEXT"]=> string(103) "<p class="Autor">Olga V. Aleinikova, Alina S. Fedorova, Svetlana O. Sharapova</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(81) "Olga V. Aleinikova, Alina S. Fedorova, Svetlana O. Sharapova
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(81) "Olga V. Aleinikova, Alina S. Fedorova, Svetlana O. Sharapova
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "302" ["VALUE"]=> array(2) { ["TEXT"]=> string(2827) "<h2>Summery </h2> <p class="Summery"> Introduction: Nijmegen breakage syndrome (NBS) is characterized by chromosome instability, combined immunodeficiency, radiosensitivity and high predisposition to lymphoid malignancy. A specific therapy is not available, however, hematopoietic stem cell transplantation (HSCT) is considered for NBS patients with refractory or recurrent leukemia or lymphoma. </p> <p class="Summery"> Purpose: We aimed to present Belarusian data in NBS diagnosis and management and to discuss indications for allo-HSCT treatment. </p> <p class="Summery"> Patients and Methods: A total of 238 patients were registered with primary immune deficiency (PID), including 19 cases of NBS. DNA was analyzed for mutation in NBN gene by direct sequencing of exon 6. Histological classification of lymphoid neoplasms was performed according to World Health Organization classification (2008). The patients were treated according to modified pediatric regimens or individually. </p> <p class="Summery"> Results: NBS accounted for 8.0% of all PID cases and was diagnosed at the age from 0.3 to 21.6 years (median 7.1). Mutation 657-661delACAAA in NBN gene and combined immunodeficiency of various degrees was confirmed in all patients. Lymphoid malignancy developed in 9 (47.4%) NBS patients ageing from 4.3 to 21.6 years (median 10.7). Acute leukemia was diagnosed in 4 patients, and stage III non-Hodgkin’s lymphoma in 5. Lymphoma/leukemia were in 7 out of 9 cases of T-cell origin. Complete remission (CR) was achieved in 66.7% of the patients.. Events were: death from infections in induction or in CR1 in 3 patients, progression/relapse in 3, second lymphoma in 1. Totally 7 NBS patients died, all after the development of malignancies. Two patients with T-mature lymphoma/leukemia did not respond to induction chemotherapy, were treated with unrelated HSCT in the 1CT and alive disease free within 6 and 13 months after transplantation. HSCT from a sibling donor was performed 9.8 years ago in a boy without malignancy but with infectious and autoimmune complications. They all received reduced-intensity conditioning regimens, which were well tolerated. </p> <p class="Summery"> Conclusions:<span class="CharOverride-10"> </span>NBS needs to be diagnosed early. With respect to progressive immunodeficiency and high risk of lymphoid malignancies with uncertain curative prospective, an allo-HSCT approach with reduced-intensity conditioning could be proposed as a treatment option for NBS patients with severe defects of immune function, and for all NBS patients with lymphoid malignancy in 1<sup>st</sup> complete remission. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2671) "Summery
Introduction: Nijmegen breakage syndrome (NBS) is characterized by chromosome instability, combined immunodeficiency, radiosensitivity and high predisposition to lymphoid malignancy. A specific therapy is not available, however, hematopoietic stem cell transplantation (HSCT) is considered for NBS patients with refractory or recurrent leukemia or lymphoma.
Purpose: We aimed to present Belarusian data in NBS diagnosis and management and to discuss indications for allo-HSCT treatment.
Patients and Methods: A total of 238 patients were registered with primary immune deficiency (PID), including 19 cases of NBS. DNA was analyzed for mutation in NBN gene by direct sequencing of exon 6. Histological classification of lymphoid neoplasms was performed according to World Health Organization classification (2008). The patients were treated according to modified pediatric regimens or individually.
Results: NBS accounted for 8.0% of all PID cases and was diagnosed at the age from 0.3 to 21.6 years (median 7.1). Mutation 657-661delACAAA in NBN gene and combined immunodeficiency of various degrees was confirmed in all patients. Lymphoid malignancy developed in 9 (47.4%) NBS patients ageing from 4.3 to 21.6 years (median 10.7). Acute leukemia was diagnosed in 4 patients, and stage III non-Hodgkin’s lymphoma in 5. Lymphoma/leukemia were in 7 out of 9 cases of T-cell origin. Complete remission (CR) was achieved in 66.7% of the patients.. Events were: death from infections in induction or in CR1 in 3 patients, progression/relapse in 3, second lymphoma in 1. Totally 7 NBS patients died, all after the development of malignancies. Two patients with T-mature lymphoma/leukemia did not respond to induction chemotherapy, were treated with unrelated HSCT in the 1CT and alive disease free within 6 and 13 months after transplantation. HSCT from a sibling donor was performed 9.8 years ago in a boy without malignancy but with infectious and autoimmune complications. They all received reduced-intensity conditioning regimens, which were well tolerated.
Conclusions: NBS needs to be diagnosed early. With respect to progressive immunodeficiency and high risk of lymphoid malignancies with uncertain curative prospective, an allo-HSCT approach with reduced-intensity conditioning could be proposed as a treatment option for NBS patients with severe defects of immune function, and for all NBS patients with lymphoid malignancy in 1st complete remission.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(2671) "Summery
Introduction: Nijmegen breakage syndrome (NBS) is characterized by chromosome instability, combined immunodeficiency, radiosensitivity and high predisposition to lymphoid malignancy. A specific therapy is not available, however, hematopoietic stem cell transplantation (HSCT) is considered for NBS patients with refractory or recurrent leukemia or lymphoma.
Purpose: We aimed to present Belarusian data in NBS diagnosis and management and to discuss indications for allo-HSCT treatment.
Patients and Methods: A total of 238 patients were registered with primary immune deficiency (PID), including 19 cases of NBS. DNA was analyzed for mutation in NBN gene by direct sequencing of exon 6. Histological classification of lymphoid neoplasms was performed according to World Health Organization classification (2008). The patients were treated according to modified pediatric regimens or individually.
Results: NBS accounted for 8.0% of all PID cases and was diagnosed at the age from 0.3 to 21.6 years (median 7.1). Mutation 657-661delACAAA in NBN gene and combined immunodeficiency of various degrees was confirmed in all patients. Lymphoid malignancy developed in 9 (47.4%) NBS patients ageing from 4.3 to 21.6 years (median 10.7). Acute leukemia was diagnosed in 4 patients, and stage III non-Hodgkin’s lymphoma in 5. Lymphoma/leukemia were in 7 out of 9 cases of T-cell origin. Complete remission (CR) was achieved in 66.7% of the patients.. Events were: death from infections in induction or in CR1 in 3 patients, progression/relapse in 3, second lymphoma in 1. Totally 7 NBS patients died, all after the development of malignancies. Two patients with T-mature lymphoma/leukemia did not respond to induction chemotherapy, were treated with unrelated HSCT in the 1CT and alive disease free within 6 and 13 months after transplantation. HSCT from a sibling donor was performed 9.8 years ago in a boy without malignancy but with infectious and autoimmune complications. They all received reduced-intensity conditioning regimens, which were well tolerated.
Conclusions: NBS needs to be diagnosed early. With respect to progressive immunodeficiency and high risk of lymphoid malignancies with uncertain curative prospective, an allo-HSCT approach with reduced-intensity conditioning could be proposed as a treatment option for NBS patients with severe defects of immune function, and for all NBS patients with lymphoid malignancy in 1st complete remission.
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "299" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-31-37" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-31-37" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-31-37" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "303" ["VALUE"]=> string(147) "Should Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(147) "Should Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(147) "Should Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "301" ["VALUE"]=> array(2) { ["TEXT"]=> string(153) "<p class="Autor_place_work">Belarusian Research Center for Pediatric Oncology, Hematology and Immunology, Minsk Region, Belarus</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(131) "Belarusian Research Center for Pediatric Oncology, Hematology and Immunology, Minsk Region, Belarus
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(131) "Belarusian Research Center for Pediatric Oncology, Hematology and Immunology, Minsk Region, Belarus
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(3) { [0]=> string(3) "293" [1]=> string(3) "294" [2]=> string(3) "295" } ["VALUE"]=> array(3) { [0]=> string(2) "52" [1]=> string(2) "51" [2]=> string(2) "53" } ["DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(3) { [0]=> string(2) "52" [1]=> string(2) "51" [2]=> string(2) "53" } ["~DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(3) { [0]=> string(59) "Alina S. Fedorova" [1]=> string(60) "Olga V. Aleinikova" [2]=> string(63) "Svetlana O. Sharapova" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "296" ["VALUE"]=> array(2) { ["TEXT"]=> string(151) "<p class="Autor">Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(129) "Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(129) "Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "290" ["VALUE"]=> string(19) "27.02.2015 14:23:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "27.02.2015 14:23:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "27.02.2015 14:23:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "291" ["VALUE"]=> string(19) "12.06.2015 14:23:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "12.06.2015 14:23:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "12.06.2015 14:23:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "872" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(4) { [0]=> string(4) "1212" [1]=> string(4) "1213" [2]=> string(4) "1214" [3]=> string(4) "1215" } ["VALUE"]=> array(4) { [0]=> string(2) "54" [1]=> string(2) "56" [2]=> string(2) "57" [3]=> string(2) "58" } ["DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(4) { [0]=> string(2) "54" [1]=> string(2) "56" [2]=> string(2) "57" [3]=> string(2) "58" } ["~DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(4) { [0]=> string(74) "Синдром Ниймеген" [1]=> string(69) "иммунодефицит" [2]=> string(57) "лимфома" [3]=> string(103) "трансплантация стволовых клеток" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "292" ["VALUE"]=> string(2) "51" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "51" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(60) "Olga V. Aleinikova" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "298" ["VALUE"]=> array(2) { ["TEXT"]=> string(4903) "<p class="Summery">Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.</p> <p class="Summery">Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии. </p> <p class="Summery">Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена <span lang="en-US">NBN</span>. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.</p> <p class="Summery">Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661<span lang="en-US">delACAAA</span> в гене <span lang="en-US">NBN</span> и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (<span lang="en-US">III</span> стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.</p> <p class="Summery">Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(4705) "Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.
Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии.
Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена NBN. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.
Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661delACAAA в гене NBN и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (III стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.
Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(4705) "Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.
Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии.
Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена NBN. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.
Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661delACAAA в гене NBN и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (III стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.
Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "297" ["VALUE"]=> array(2) { ["TEXT"]=> string(262) "<p class="Autor_place_work">Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(240) "Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(240) "Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь
" } } } [4]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "2" ["~IBLOCK_SECTION_ID"]=> string(1) "2" ["ID"]=> string(2) "50" ["~ID"]=> string(2) "50" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(238) "Аллогенная трансплантация гемопоэтических стволовых клеток у пациентов с острым лейкозом и ВИЧ-инфекцией, опыт Санкт-Петербурга" ["~NAME"]=> string(238) "Аллогенная трансплантация гемопоэтических стволовых клеток у пациентов с острым лейкозом и ВИЧ-инфекцией, опыт Санкт-Петербурга" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:42:53" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:42:53" ["DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-24-30/" ["~DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-24-30/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(42786) "HIV and cancer risk
Human immunodeficiency virus (HIV) infection represents a growing socio-economic and healthcare problem. Global situation and trends based on World Health Organization data (WHO): since the beginning of the epidemic 35.0 million (33.1–37.2 million) people around the world were living with HIV at the end of 2013 [46]. Patients living with HIV are at high risk of cancer. The introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HAART is affecting the incidence of several hematological malignancies: the incidence of primary central nervous system lymphoma (PCNSL) has dropped since the introduction of HAART in 1996 and non-Hodgkin lymphoma (NHL) appears to be declining in incidence as well, but to a lesser degree than PCNLS. Between 1990-1995 and 1996-2002, risk declined for non-Hodgkin lymphoma [(NHL) n = 3412; SIR, 53.2 and 22.6, respectively; p < 0.0001]. In contrast, the risk of Hodgkin lymphoma increased substantially over the 1990-2002 period (n = 149; SIR, 8.1 and 13.6, respectively; p = 0.003) [10, 26].
Acute leukemias (AL) are not HIV-indicating diseases. The epidemiology and clinical outcome of acute leukemias in HIV-infected individuals is poorly documented. Rare cases of acute myeloid leukaemia (AML) have been reported during HIV infection and no clear relationship with the characteristic immune deficiency has been established [2, 11, 22, 24, 38, 41]. Like with many other malignancies, the incidence of AML appears to be increased in HIV-infected patients. The estimated risk of AML in 1990 to 1996 among HIV-infected adults was twice that of the general population (standardized incidence ratio 2.05; 95% confidence interval, 1.17±3.34) [41]. Acute lymphoblastic leukemia (ALL) is most common in childhood with a peak incidence at 2–5 years of age and rare in adults. An association with HIV infection is not typical and limited to case reports [12, 14, 33, 43]. About 55 cases of AL in HIV-infected patients have been published. Their outcome is very poor, with the median survival of 7 weeks to 7 months [1, 12].
Despite introduction of HAART, the HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy [31, 32]. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection [9, 25]. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown, due to limited number of case reports and small clinical series. In most of these patients, hematological malignancies are potentially curable by allo-HSCT [13, 19, 20]. Wide application of this method is limited by the high risk of fatal infectious complications. Over recent years, some improvements in supportive care, HAART and transplantation technology, allowed to use this therapeutic approach for highly immunocompromised patients.
Donor CCR5
mutation and potential HIV cure
Interest in finding a potential ‘cure’ for HIV in anticancer therapy has actually started since the report of an individual who underwent allo-HSCT from a donor with homozygote gene CCR5 delta 32 mutation for acute myeloid leukemia treatment. A potential role of cancer chemotherapy and HSCT treatment is discussed in the context of their role in potential HIV elimination from infected host [20, 29]. Allo-HSCT from a donor with homozygotic CCR5 del 32 mutation may cure from the both diseases: HIV and cancer. This opportunity that has been shown in case of the ‘Berlin patient’ [3, 17, 20, 47]. Most experts ascribe the successful allo-HSCT in ‘Berlin patient’ to a genetic mutation in donor’s hematopoietic cells (HSC). The unrelated donor had a del32 mutation of the CCR5 co-receptor, thus causing inability of HIV-1 to infect immune cells [20]. A homozygous state for this mutation, which was found in the population at a frequency of <1:1000, dramatically reduces the risk of HIV-1 entry inside the human lymphocytes. However, prevalence of this mutation is low, and this approach seems unacceptable for the most HIV-positive patients with high-risk hematologic malignancies [18, 34].
Allo-HSCT from donors with a wild-type CCR5, along with ongoing HAART, has looked more promising, but it has failed in clinical cases reported as ‘Boston patients’ [16, 15]. But other aspects, including HSC source, donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and novel anti-HIV and anti-cancer agents still maintain interest for allo-HSCT, as a potential cure procedure.
Choice of cord blood (CB) as a source of HSCs can increase the chances of finding an HLA-matched homozygous CCR5 del32 mutation donor for allo-HSCT, and co-transplantation with haplo-HSCs may overcome problems associated with CB HSCT, because the CB transplantation does not require as stringent HLA match between donor and recipient, as bone marrow or peripheral blood HCTs [34]. There is still unclear, which factor in ‘Berlin patient’ played a crucial role in HIV clearance (donor homozygosity for CCR5 mutation, cytotoxic chemotherapy, graft-associated immunoadoptive effect, or a combined action). There are still no reports on allo-HSCT outcome with donors heterozygous for CCR5 del32 mutation.
Several cytotoxic agents which are routinely used in pre-transplant conditioning regimen, including alkylating agents, such as cyclophosphamide, busulfan, and antimetabolites, have been shown to be effective in depleting HIV-infected cells in vivo or in vitro, and in murine models [6, 27, 29, 40]. Introduction of reduced-intensity conditioning regimens (RIC) allows to continue HAART through the transplant procedure. ‘Boston patients’ demonstrated that allo-HSCT from donor without CCR5 del 32 mutation with ongoing HAART is not sufficient for HIV clearance [15]. But some novel antiretroviral medications could have an additional curative effect post-HSCT. E.g., Maraviroc is a new antiretroviral agent of entry inhibitor class. Therefore, application of Maraviroc after allo-HSCT could functionally mimic the CCR5 del32 mutation of the HIV target cells. Moreover, it can be used not only for HIV control, but also as a component of GvHD prophylaxis [7, 30, 36].
Immune therapy
It has been shown that chemotherapy alone cannot eradicate the body reservoirs of HIV. In addition to the cytostatic impact, there is an immunoadoptive effect which can devoid the organism of HIV following allo-HSCT procedure. Moreover, some other anti-cancer post-transplant strategies can be useful in HIV cure. Reduced-intensity conditioning regimens before allo-HSCT represent a promising platform for cancer immunotherapy. This post-transplant strategy includes immunoadoptive therapy with donor lymphocyte infusions (DLI), and new anti-cancer agents that are able for selective killing of tumor cells, as based on their surface expression of tumor-associated antigens targeted by the therapeutic antibodies per se, or linked to cytotoxic compounds (Gentuzimab Ozogamicin, a humanized anti-CD33 monoclonal antibody, Brentuximab Vedotin, a doxorubicin-conjugated anti-envelope antibody). These therapeutic strategies suggest a curative potential for the both diseases, i.e., leukemia and HIV infection [5, 21, 40].
Latently HIV-infected cells comprise the major problem because they are “invisible” to the targeted killing agents. This issue can be resolved by means of activating the infected cells by anti-cancer agents applicable in post-transplant period for targeted chemotherapy, like as GvHD prophylaxis and treatment. E.g., epigenetic manipulation of malignant or virally infected cells with appropriate drugs, such as histone deacetylase inhibitors and proteasome inhibitors, yields results in new cancer therapies (vorinostat for lymphoma, romidepsin for peripheral T-cell lymphoma, and bortezomib for multiple myeloma and mantle cell lymphoma). They could be used to another aim, as HIV-activating drugs in latently infected cells, thus making them more susceptible to apoptosis, or more amenable to direct cytotoxic targeting by other agents [4, 29, 35, 37]. Moreover, bortezomib may also have additional anti-HIV effects [28, 29].
Allo-HSCT in patients with hematological malignances and HIV may present a model for the investigations in the field of adoptive therapy with engineered T cells, or stem cell-based treatment against both diseases, i.e., cancer and HIV. Recent progress in stem cell manipulation and in gene engineering of autologous HSCs with vectors carrying the CCR5 mutation has allowed rapid developments in gene therapy for HIV treatment. A number of relevant in vitro and in vivo studies have been published, but the results still are far from definite success [8, 23, 39, 42, 44, 45, 48,]. This strategy looks very promising in the near future.
Clinical cases
This report includes three cases of the allo-HSCT in patients with an HIV that were performed in Saint-Petersburg, Russia. Baseline values of the patients and transplant characteristics are shown in Table 1.
Patient 1, female, 50 years old was diagnosed with an acute myeloid leukemia in September 2008. First complete remission (CR) was achieved after the fist course of chemotherapy (CT). HIV was diagnosed in March 2009. HIV was transmitted through blood products transfusion (platelets). HAART was not initiated at that time. First early relapse of AML was confirmed in November 2009. No CR after FLAG was registered. Patient had a matched related donor. On March 26th 2010 the allogeneic stem cell transplantation with reduced intensity conditioning regimen (RIC) and standard GVHD prophylaxis (Cyclosporine A + Methotrexate) was performed. Donor: MRD, female (sister), ABO compatibility, CCR5 unknown. Peripheral blood stem cells were used for transplantation (CD34+ cells, 5.8 x 106). No early complications were observed after allo-HSCT. Engraftment was registered on Day +18. On Day +30 no CR: 80% donor chimerism and no cytogenetic remission 46,XX,der(8)t(8;?)(q10;?)[4]/46,XX[16]. Cyclosporine A was discontinued. DLI with 1x105 CD3+/kg was performed on Day +46. On Day +70 full donor chimerism and complete remission AML 46,XX were registered. Immunoadoptive therapy was continued: DLI was performed 7 times. HAART was started at the time of immunoadoptive therapy. No GVHD was registered. Viral loads and CD4+ counts for the patient 1 upon treatment are presented in Figure 1.
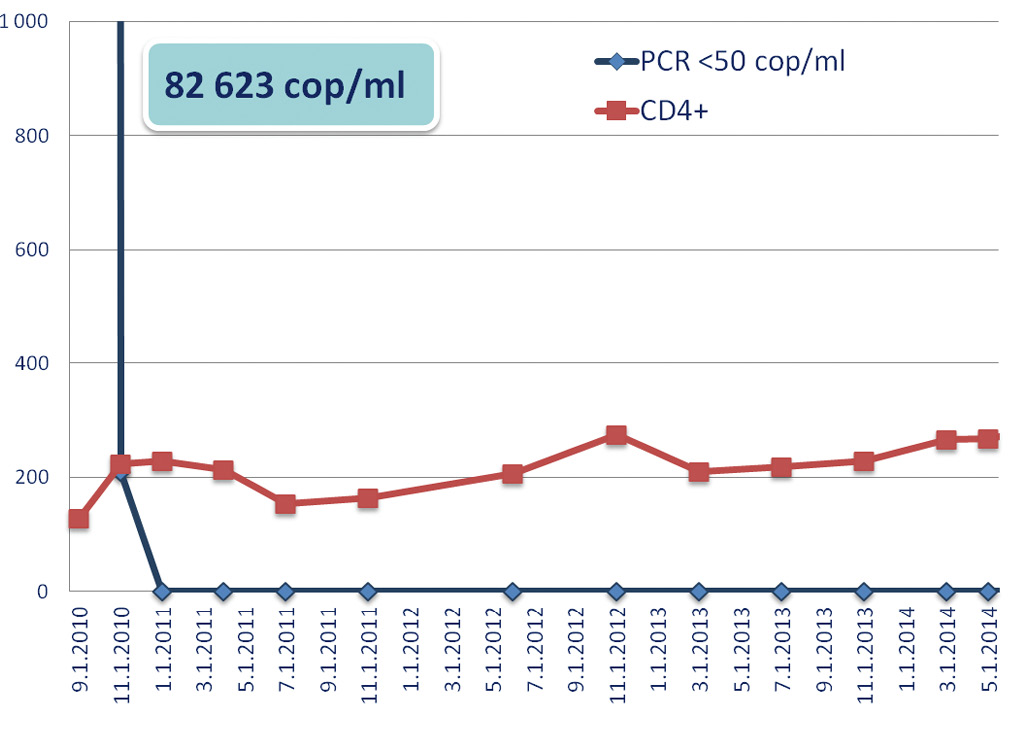
Figure 1. Patient 1: Dynamics of HIV amounts (PCR) and CD4+ counts
At 57 months after allo-HSCT, the patient is in good health and has active lifestyle, in CR AML (full chimerism, 46,XX). There are no signs of HIV-reactivation (PCR <50 copies, CD4+ 295 cells; deep virology status performed in Hamburg: Plasma VL RNA copies/ml: 1107, DNA/1 Mio. PBMC: 2265, Integrated HIV DNA/PCR: 17.670, HIVAb/p24Ag 4th generation: pos./neg.). She is still on HAART: Prezista 800 + Ritonavir 100 + Lamivudine 300.
Patient 2, female, 29 years old was diagnosed with an acute lymphoblastic leukemia in 1993 (at the age of 10). First CR was achieved after the first course of chemotherapy. A HIV/hepatitis C co-infection was diagnosed in 2005. HIV was transmitted from the patient’s husband. HAART was started in 2009. First late relapse of ALL was confirmed in October 2011. Second CR MRD (+) was achieved after second course Hyper-CVAD / MxA treatment in December 2011. Full chemotherapy program (8 cycles) of Hyper-CVAD / MxA was completed in May 2012. Patient had no related matched donors. A search for the unrelated donor was initiated in February 2012. By the time of HSCT, the patient has achieved a second remission of ALL, MRD (+), HIV status was satisfactory: PCR <50 copies, CD4+ 108 cells on HAART. On 19 July 2012, an allogeneic stem cell transplantation was performed, with reduced intensity conditioning (RIC) regimen and standard GVHD prophylaxis, including ATG + tacrolimus and MMF. Donor: MUD, female, ABO-compatible, CCR5, wt/wt. Source of HSC: PBSC (CD34+ 9.1 x 106). No severe infectious complications were registered in pre-engraftment phase. Due to severe tacrolimus toxicity, the GVHD prophylaxis was modified, by switching from tacrolimus to corticosteroids. Engraftment was registered on Day +12. On Day +23, CMV reactivation with severe CMV disease of gut was diagnosed, as shown by biopsy. The patient died on Day +41 from generalized gancyclovir-resistant CMV disease affecting gut, liver, and kidneys.
Patient 3, female, 26 years old was diagnosed with HIV, and HAART was immediately administered in April 2012. HIV was transmitted from the patient’s husband. Acute leukemia of mixed phenotype was diagnosed in May 2012. First CR with MRD (+) was achieved only after at the 3rd course of chemotherapy. The patient had no matched related donors. A search for unrelated donor was initiated in December 2012. At the moment of HSCT, the ALL disease was in its first remission, MRD (+); HIV status was satisfactory: PCR <50 copies, CD4+ 117 cells on HAART. On the April 1, 2013, allogeneic stem cell transplantation with a RIC regimen and standard GVHD prophylaxis (ATG+cyclosporine A+MMF), including Maraviroc, was performed.
Maraviroc is an antiretroviral agent belonging to the CCR5 receptor antagonists, as well as entry inhibitors, it is used for treatment of HIV infection. It also appears to reduce graft-versus-host disease in patients treated with allogeneic bone marrow transplantation for leukemia, in a phase 1/2 study [36].
We have tested the recipient and donor for a CCR5 gene mutation. The recipient (patient 3) had no CCR5 delta32 mutation (wild type/wild type). The donor harbored a single CCR5 delta32 allele (a heterozygotic state). A male, HLA-matched, ABO-incompatible, unrelated donor was used for HST. Peripheral blood stem cells were used as a source of HSCs (CD34+ cells, 6,5 x 106). No relevant complications in pre-engraftment phase were registered. Engraftment and acute GVHD of the skin grade 2-3 were registered since Day +12. GVHD was treated by a high dose of CsA (control serum level) + prolonged MMF and Maraviroc + topic steroids. On the Day +60, no signs of GVHD were reported. Immunosupressive therapy was discontinued on the Day +100 due to the MRD positivity registered by flow cytometry. Local light skin chronic GVHD was observed for two months, and CR with MRD (-) was achieved. Viral loads and CD4+ counts in the patient 3 during treatment are presented in Fig. 2.
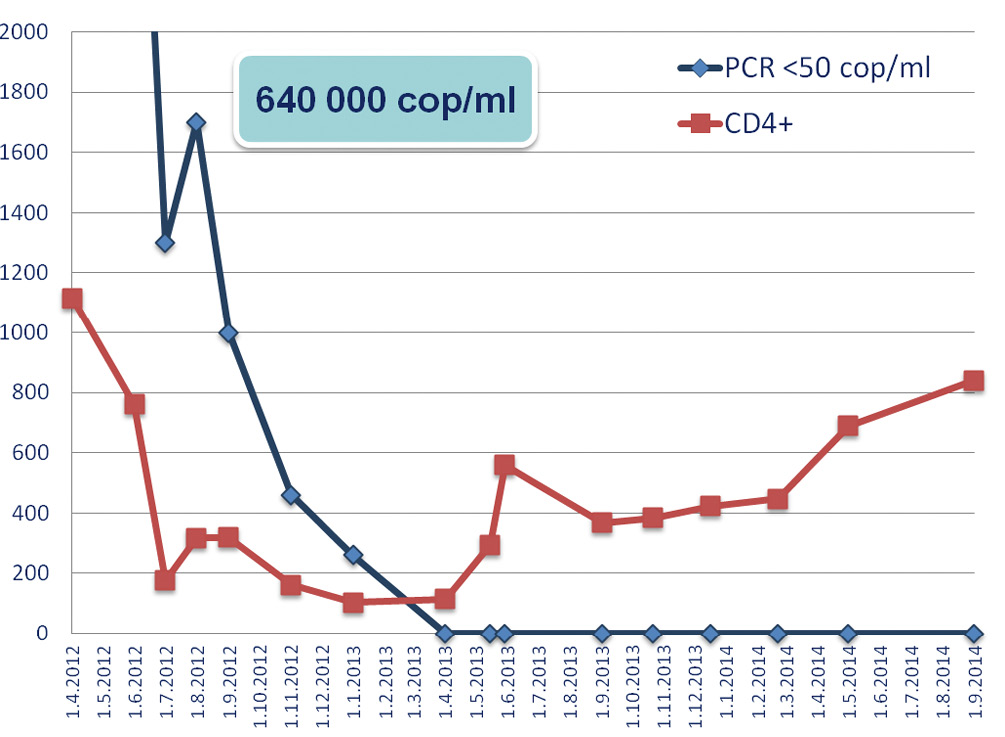
Figure 2. Patient 3: Dynamics of HIV amounts (PCR) and CD4+ counts
Currently, at 22 months after allo-HSCT, the patient is in a good health and has an active lifestyle, CR of acute leukemia (full chimerism, MRD(-)), with no signs of HIV-reactivation (PCR <50 copies, CD4+ 828 cells; deep virology status in Hamburg: Plasma VL RNA copies/ml: 43, DNA/1 Mio. PBMC: 71, Integrated HIV DNA/PCR: 517, HIVAb/p24Ag 4th generation: pos./neg.). She is still on HAART: Abacavir 600 + Lamivudine 300 + Raltegravir 800. An important fact is that the patient’s sample contained the CCR5-wildtype-allele and the CCR5 del 32 mutation = donor’s heterozygote type and was converted to heterozygote CCR5 del 32 mutation.
In conclusion, allo-HSCT with RIC is an effective and feasible therapeutic modality for high-grade hematological malignancies in patients with HIV. There were no severe toxicity and drug-drug interactions between HAART, conditioning regimen, and immunosuppressive drugs. HAART and immunosuppressive agents can be safely administered after allo-HSCT. Engraftment and full donor chimaerism were achieved at term as in the general population allo-HSCT recipients. Relapse of acute leukemia could be successful and safety treated with immunoadoptive therapy (DLI) after allo-HSCT. There were no specific infections or other particular complication in HIV positive pts after allo-HSCT. We suggest that patient 3 may be “near to functional cure”. Allo-HSCT ongoing with HAART is the same effective and safety strategy for the treatment high-risk hematologic malignancies in HIV population.
Acknowledgements
Staff of CIC 725, Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, First Pavlov State Medical University of Saint-Petersburg, Russia and International Registry Stefan Morsch Stiftung, Birkenfeld, Germany.
No conflict of interest is reported.
|
Characteristics |
Case 1 |
Case 2 |
Case3 |
|
Demographic Age |
50 |
29 |
26 |
|
Diagnosis |
AML |
ALL |
AL, mixed phenotype |
|
Status |
CR2 |
CR2 |
CR1 |
|
HIV status at Tx CD4+ |
500 cells/ml |
380 cells/ml |
114 cells/ml |
|
HIV-VL |
700 copies/ml |
<50 copies/ml |
<50 copies/ml |
|
cART |
No |
Yes |
Yes |
|
Transplant Donor type CCR5 del32 |
Sibling matched NA |
MUD (12/12) wt/wt |
MUD (12/12) del 32/wt; heterozygote |
|
Conditioning |
RIC (Flu150+Bu8) |
RIC (Flu150+Mel140) |
RIC (Flu150+Bu8) |
|
GvHD proph |
CsA |
ATG, MMF, steroids |
ATG, CsA, MMF, maraviroc |
|
Engraftment Neutrophil |
+ 18 d |
+ 12 d |
+ 18 d |
|
Platelet |
+ 19 d |
+ 14 d |
+ 18 d |
|
Full donor chimaerism |
+ 25 d |
+ 20 d |
+ 20 d |
|
GvHD Acute, grade |
No |
No |
II |
|
Chronic |
No |
No |
No |
|
LFU |
57 months |
41 days |
22 months |
|
Status at LFU |
Alive |
Dead |
Alive |
|
HIV status at LFU CD4+ |
800 cells/ml |
NA |
480 cells/ml |
|
HIV-VL |
<50 copies/ml |
NA |
<50 copies/ml |
|
cART |
Continues |
NA |
Continues |
Table 1. Baseline patients and transplants characteristics
References
- Aboulafia DM, Meneses M, Ginsberg S et al. Acute myeloid leukemia in patients infected with HIV-1. AIDS 2002; 16(6):865-76.
- Al-Bahar S, Pandita R, Dhabhar BN, Al-Bahar E. Human immunodeficiency virus (HIV) infection associated with acute myeloblastic leukaemia in a low HIV prevalence area. Acta Haematol 1994; 91: 52-53.
- Allers K, Hütter G, Hofmann J et al. Evidence for the cure of HIV infection by CCR5 delta 32 / delta32 stem cell transplantation. Blood 2011; 117(10): 2791-9.
- Archin NM, Libesty AL, Kashuba AD et al. Administration of vorinostat disrupts HIV-1 latency in patients on antiretroviral therapy. Nature 2012; 482: 482–5.
- Berger EA. Targeted cytotoxic therapy: adapting a rapidly progressing anti-cancer paradign for depleting HIV infected cell reservoirs. Curr Opin HIV/AIDS 2011; 6: 80-5.
- Borvak J, Chou CS, Van Dyke G et al. The use of cyclosporine, FK506, and SDZ NIM811 to prevent CD25-quiescent peripheral blood mononuclear cells from producing HIV. J Infect Dis 1996; 174: 850-3.
- Choi SW, Reddy P. Current and emerging strategies for the prevention of graft versus host disease. Nat Rev Clin Oncol 2014; 11(9): 536-47.
- Didigu CA, Wilen CB, Wang J et al. Simultaneous zinc-finger nuclease editing of the HIV coreceptors CCR5 and CXCR4 protects CD4+ T cells from HIV-1 infection. Blood 2014; 123(1): 61-9.
- Diez-Martin JL, Balsalobre P, Re A et al. Comparable survival between HIV+ and HIV–non-Hodgkin and Hodgkin lymphoma patients undergoing autologous peripheral blood stem cell transplantation. Blood 2009; 113(23): 6011-14.
- Engels EA, Pfeiffer RM, Goedert JJ et al. Trends in cancer risk among people with AIDS in the United States 1980-2002. AIDS 2006; 20(12): 1645-54.
- Farber CM, Ferehans W, Capel P et al. Chemotherapy of acute myeloblastic leukaemia in an HIV carrier. Eur J Haematol 1993; 51: 180.
- Geriniere L, Bastion Y, Dumontet C et al. Heterogeneneity of acute lymphoblastic leukaemia in HIV-seropositive patients. Ann Oncol 1994; 5(5): 437-40.
- Gupta V, Tomblyn M, Pedersen TL et al. Allogeneic hematopoietic cell transplantation in human immunodeficiency virus-positive patients with hematologic disorders: a report from the Center for International Blood and Marrow Transplant Research. Biol Blood Marrow Transplantion 2009; 15: 864-71.
- Hamilton J, McBride M, Kettle P. Acute B cell lymphoblastic leukaemia and human immunodeficiency virus infection (HIV). Ulster Med J 2002; 71(1): 72-5.
- Henrich T, Hanhauser E, Marty FM et al. Antiretroviral-free HIV-1 remission and viral rebound after allogeneic stem cell transplantation: report of 2 cases. Ann Intern Med 2014; 161(5): 319-27.
- Henrich T, Hu Z, Li JZ et al. Long-term reduction in peripheral blood HIV type 1 reservoirs following reduced-intensity conditioning allogeneic stem cell transplantation. J Infect Dis 2013; 207(11):1694-702.
- Hütter G, Ganepola S. Eradication of HIV by transplantation of CCR5-deficient hematopoietic stem cells. The Scientific World J 2011; 11: 1068-76.
- Hütter G, Thielb E. Allogeneic transplantation of CCR5-deficient progenitor cells in a patient with HIV infection: an update after 3 years and the search for patient no.2. AIDS 2011;25: 273-75.
- Hütter G, Zaia JA. Allogeneic haematopoietic stem cell transplantation in patients with human immunodeficiency virus: the experiences of more than 25 years. Clin Exp Immunol 2011; 163; 284-95.
- Hütter G, Nowak D, Mossner M et al. Long-term control of HIV by CCR5 delta32/ delta32 stem-cell transplantation. N Engl J Med 2009; 360: 692-8.
- Johansson S, Goldenberg DM, Griffiths GL et al. Elimination of HIV-1 infection by treatment with a doxorubicin-conjugated antienvelope antibody. AIDS 2006; 20: 1911-5.
- Kane D, Keating S, McCann S, Mulcahy F. The management of acute myeloid leukaemia (AML) in human immunodeficiency virus (HIV) infection: a case report and review. Int J STD and AIDS, 1997; 8: 272-4.
- Kiem HP, Jerome KR, Deeks SG et al. Hematopoietic-stem-cell-based gene therapy for HIV disease. Stem Cell 2012; 10: 137-47.
- King JAC, Nye DM, O’Connor MB et al. Acute myelogenous leukemia (FAB AMLM1) in the setting of HIV infection and G-CSF therapy: a case report and review of the literature. Ann Hematol 1998; 77: 69-73.
- Krishnan A, Palmer JM, Zaia JA et al. HIV status does not affect the outcome of autologous stem cell transplantation (ASCT) for non-Hodgkin lymphoma (NHL). Biol Blood Marrow Transplant 2010; 16(9): 1302-8.
- Launay O, Guillevin L. Epidemiology of HIV-associated malignancies. Bull Cancer 2003; 90(5); 387-92.
- Little RF, Pittaluga S, Grant N et al. Highly effective treatment of AIDS-related lymphoma with dose-adjusted EPOCH: impact of antiretroviral therapy suspension and tumor biology. Blood. 2003; 101: 4653-9.
- Liu B, Yu X, Luo K et al. Influence of primate lentiviral Vif and proteasome inhibitors on human immunodeficiency virus type 1 virion packaging of APOBEC3G. J Virol 2004; 78: 2072-81.
- Mitsuyasu R. Curing HIV: lessons from cancer therapy. Curr Opin HIV AIDS 2013; 8(3): 224-9.
- Nakamura R, Forman SJ. Reduced intensity conditioning for allogeneic hematopoietic cell transplantation: considerations for evidence-based GVHD prophylaxis
Expert Rev Hematol 2014; 7(3), :407-21. - Passweg J, Baldomero H, Bader P et al. Hematopoietic SCT in Europe: recent trends in the use of alternative donors showing more haploidentical donors but fewer cord blood transplants. Bone Marrow Transplantation 2015; Suppl 50: 476-82.
- Passweg J, Baldomero H, Peters C et al. Hematopoietic SCT in Europe: data and trends in 2012 with special consideration of pediatric transplantation. Bone Marrow Transplantation 2014 ; Suppl 49: 744-50.
- Pees HW, Radtke H, Schwamborn J et al. The BFM-protocol for HIV-negative Burkitt’ s lymphomas and L3 ALL in adult patients: a high chance for a cure. Ann Hematol 1992; 65(5): 201-5.
- Petz L. Cord Blood Transplantation for Cure of HIV Infections. Stem Cells Transl Med 2013; 2: 635-7.
- Piekarz RL, Frye R, Prince HM et al. Phase 2 trial of romidepsin in patients with peripheral T-cell lymphoma. Blood 2011; 117: 5827-34.
- Reshef R, Luger SM, Hexner EO et al. Blockade of lymphocyte chemotaxis in visceral graft-versus-host disease. N Engl J Med 2012; 367(2): 135-45.
- Reuse S, Calao M, Kabeya K et al. Synergistic activation of HIV-1 expression by deacetylase inhibitors and prostratin: implications for treatment of latent infection. PLoS One 2009;4:e6903.
- Rivers JK, Laubenstein LJ, Postel AH. Acute monocytic leukaemia in an HIV-seropositive man. Clin Exp Dermatol 1992; 17: 203-5.
- Shimizu S, Ringpis GE, Marsden MD et al. RNAi-mediated CCR5 knockdown provides HIV-1 resistance to memory T cells in humanized BLT mice. Mol Ther Nucl Acids 2015 Feb; 4(2): e227.
- Simard C, Jolicoueur P. The effect of antineoplastic drugs on murine acquired immunodeficiency syndrome. Science 1991; 252:305-8.
- Sutton L, GueAnel P, Tanguy ML et al. Acute myeloid leukaemia in human immunodeficiency virus infected adults: epidemiology, treatment feasibility and outcome. Brit J Haematol 2001; 112: 900-8.
- Tebas P, Stein D, Tang WW et al. Gene editing of CCR5 in autologous CD4 T cells of persons infected with HIV. N Engl J Med 2014; 370: 901-10.
- Turner ML, Watson HG, Russell L et al. An HIV positive haemophiliac with acute lymphoblastic leukaemia successfully treated with intensive chemotherapy and syngeneic bone marrow transplantation. Bone Marrow Transplant 1992; 9(5): 387-9.
- van Lunzen J, Fehse B, Hauber J. Gene Therapy Strategies: Can We Eradicate HIV? Curr HIV/AIDS 2011; Rep 8: 78-84.
- van Lunzen J, Glaunsinger T, Stahmer I et al. Transfer of autologous gene-modified T cells in HIV-infected patients with advanced immunodeficiency and drug-resistant virus Mol Ther 2007; 15: 1024-33.
- World Health Organization http://www.who.int/hiv/data
- Yukl SA, Boritz E, Busch M et al. Challenges in detecting HIV persistence during potentially curative interventions: A study of the Berlin patient. PLOS Pathogens 2013; 9 (5): e1003347. doi:10.1371/journal.ppat.1003347.
- Zhen A, Kitchen S. Stem-cell-based gene therapy for HIV infection. Viruses 2014; 6: 1-12; doi:10.3390/v6010001.
HIV and cancer risk
Human immunodeficiency virus (HIV) infection represents a growing socio-economic and healthcare problem. Global situation and trends based on World Health Organization data (WHO): since the beginning of the epidemic 35.0 million (33.1–37.2 million) people around the world were living with HIV at the end of 2013 [46]. Patients living with HIV are at high risk of cancer. The introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HAART is affecting the incidence of several hematological malignancies: the incidence of primary central nervous system lymphoma (PCNSL) has dropped since the introduction of HAART in 1996 and non-Hodgkin lymphoma (NHL) appears to be declining in incidence as well, but to a lesser degree than PCNLS. Between 1990-1995 and 1996-2002, risk declined for non-Hodgkin lymphoma [(NHL) n = 3412; SIR, 53.2 and 22.6, respectively; p < 0.0001]. In contrast, the risk of Hodgkin lymphoma increased substantially over the 1990-2002 period (n = 149; SIR, 8.1 and 13.6, respectively; p = 0.003) [10, 26].
Acute leukemias (AL) are not HIV-indicating diseases. The epidemiology and clinical outcome of acute leukemias in HIV-infected individuals is poorly documented. Rare cases of acute myeloid leukaemia (AML) have been reported during HIV infection and no clear relationship with the characteristic immune deficiency has been established [2, 11, 22, 24, 38, 41]. Like with many other malignancies, the incidence of AML appears to be increased in HIV-infected patients. The estimated risk of AML in 1990 to 1996 among HIV-infected adults was twice that of the general population (standardized incidence ratio 2.05; 95% confidence interval, 1.17±3.34) [41]. Acute lymphoblastic leukemia (ALL) is most common in childhood with a peak incidence at 2–5 years of age and rare in adults. An association with HIV infection is not typical and limited to case reports [12, 14, 33, 43]. About 55 cases of AL in HIV-infected patients have been published. Their outcome is very poor, with the median survival of 7 weeks to 7 months [1, 12].
Despite introduction of HAART, the HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy [31, 32]. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection [9, 25]. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown, due to limited number of case reports and small clinical series. In most of these patients, hematological malignancies are potentially curable by allo-HSCT [13, 19, 20]. Wide application of this method is limited by the high risk of fatal infectious complications. Over recent years, some improvements in supportive care, HAART and transplantation technology, allowed to use this therapeutic approach for highly immunocompromised patients.
Donor CCR5
mutation and potential HIV cure
Interest in finding a potential ‘cure’ for HIV in anticancer therapy has actually started since the report of an individual who underwent allo-HSCT from a donor with homozygote gene CCR5 delta 32 mutation for acute myeloid leukemia treatment. A potential role of cancer chemotherapy and HSCT treatment is discussed in the context of their role in potential HIV elimination from infected host [20, 29]. Allo-HSCT from a donor with homozygotic CCR5 del 32 mutation may cure from the both diseases: HIV and cancer. This opportunity that has been shown in case of the ‘Berlin patient’ [3, 17, 20, 47]. Most experts ascribe the successful allo-HSCT in ‘Berlin patient’ to a genetic mutation in donor’s hematopoietic cells (HSC). The unrelated donor had a del32 mutation of the CCR5 co-receptor, thus causing inability of HIV-1 to infect immune cells [20]. A homozygous state for this mutation, which was found in the population at a frequency of <1:1000, dramatically reduces the risk of HIV-1 entry inside the human lymphocytes. However, prevalence of this mutation is low, and this approach seems unacceptable for the most HIV-positive patients with high-risk hematologic malignancies [18, 34].
Allo-HSCT from donors with a wild-type CCR5, along with ongoing HAART, has looked more promising, but it has failed in clinical cases reported as ‘Boston patients’ [16, 15]. But other aspects, including HSC source, donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and novel anti-HIV and anti-cancer agents still maintain interest for allo-HSCT, as a potential cure procedure.
Choice of cord blood (CB) as a source of HSCs can increase the chances of finding an HLA-matched homozygous CCR5 del32 mutation donor for allo-HSCT, and co-transplantation with haplo-HSCs may overcome problems associated with CB HSCT, because the CB transplantation does not require as stringent HLA match between donor and recipient, as bone marrow or peripheral blood HCTs [34]. There is still unclear, which factor in ‘Berlin patient’ played a crucial role in HIV clearance (donor homozygosity for CCR5 mutation, cytotoxic chemotherapy, graft-associated immunoadoptive effect, or a combined action). There are still no reports on allo-HSCT outcome with donors heterozygous for CCR5 del32 mutation.
Several cytotoxic agents which are routinely used in pre-transplant conditioning regimen, including alkylating agents, such as cyclophosphamide, busulfan, and antimetabolites, have been shown to be effective in depleting HIV-infected cells in vivo or in vitro, and in murine models [6, 27, 29, 40]. Introduction of reduced-intensity conditioning regimens (RIC) allows to continue HAART through the transplant procedure. ‘Boston patients’ demonstrated that allo-HSCT from donor without CCR5 del 32 mutation with ongoing HAART is not sufficient for HIV clearance [15]. But some novel antiretroviral medications could have an additional curative effect post-HSCT. E.g., Maraviroc is a new antiretroviral agent of entry inhibitor class. Therefore, application of Maraviroc after allo-HSCT could functionally mimic the CCR5 del32 mutation of the HIV target cells. Moreover, it can be used not only for HIV control, but also as a component of GvHD prophylaxis [7, 30, 36].
Immune therapy
It has been shown that chemotherapy alone cannot eradicate the body reservoirs of HIV. In addition to the cytostatic impact, there is an immunoadoptive effect which can devoid the organism of HIV following allo-HSCT procedure. Moreover, some other anti-cancer post-transplant strategies can be useful in HIV cure. Reduced-intensity conditioning regimens before allo-HSCT represent a promising platform for cancer immunotherapy. This post-transplant strategy includes immunoadoptive therapy with donor lymphocyte infusions (DLI), and new anti-cancer agents that are able for selective killing of tumor cells, as based on their surface expression of tumor-associated antigens targeted by the therapeutic antibodies per se, or linked to cytotoxic compounds (Gentuzimab Ozogamicin, a humanized anti-CD33 monoclonal antibody, Brentuximab Vedotin, a doxorubicin-conjugated anti-envelope antibody). These therapeutic strategies suggest a curative potential for the both diseases, i.e., leukemia and HIV infection [5, 21, 40].
Latently HIV-infected cells comprise the major problem because they are “invisible” to the targeted killing agents. This issue can be resolved by means of activating the infected cells by anti-cancer agents applicable in post-transplant period for targeted chemotherapy, like as GvHD prophylaxis and treatment. E.g., epigenetic manipulation of malignant or virally infected cells with appropriate drugs, such as histone deacetylase inhibitors and proteasome inhibitors, yields results in new cancer therapies (vorinostat for lymphoma, romidepsin for peripheral T-cell lymphoma, and bortezomib for multiple myeloma and mantle cell lymphoma). They could be used to another aim, as HIV-activating drugs in latently infected cells, thus making them more susceptible to apoptosis, or more amenable to direct cytotoxic targeting by other agents [4, 29, 35, 37]. Moreover, bortezomib may also have additional anti-HIV effects [28, 29].
Allo-HSCT in patients with hematological malignances and HIV may present a model for the investigations in the field of adoptive therapy with engineered T cells, or stem cell-based treatment against both diseases, i.e., cancer and HIV. Recent progress in stem cell manipulation and in gene engineering of autologous HSCs with vectors carrying the CCR5 mutation has allowed rapid developments in gene therapy for HIV treatment. A number of relevant in vitro and in vivo studies have been published, but the results still are far from definite success [8, 23, 39, 42, 44, 45, 48,]. This strategy looks very promising in the near future.
Clinical cases
This report includes three cases of the allo-HSCT in patients with an HIV that were performed in Saint-Petersburg, Russia. Baseline values of the patients and transplant characteristics are shown in Table 1.
Patient 1, female, 50 years old was diagnosed with an acute myeloid leukemia in September 2008. First complete remission (CR) was achieved after the fist course of chemotherapy (CT). HIV was diagnosed in March 2009. HIV was transmitted through blood products transfusion (platelets). HAART was not initiated at that time. First early relapse of AML was confirmed in November 2009. No CR after FLAG was registered. Patient had a matched related donor. On March 26th 2010 the allogeneic stem cell transplantation with reduced intensity conditioning regimen (RIC) and standard GVHD prophylaxis (Cyclosporine A + Methotrexate) was performed. Donor: MRD, female (sister), ABO compatibility, CCR5 unknown. Peripheral blood stem cells were used for transplantation (CD34+ cells, 5.8 x 106). No early complications were observed after allo-HSCT. Engraftment was registered on Day +18. On Day +30 no CR: 80% donor chimerism and no cytogenetic remission 46,XX,der(8)t(8;?)(q10;?)[4]/46,XX[16]. Cyclosporine A was discontinued. DLI with 1x105 CD3+/kg was performed on Day +46. On Day +70 full donor chimerism and complete remission AML 46,XX were registered. Immunoadoptive therapy was continued: DLI was performed 7 times. HAART was started at the time of immunoadoptive therapy. No GVHD was registered. Viral loads and CD4+ counts for the patient 1 upon treatment are presented in Figure 1.

Figure 1. Patient 1: Dynamics of HIV amounts (PCR) and CD4+ counts
At 57 months after allo-HSCT, the patient is in good health and has active lifestyle, in CR AML (full chimerism, 46,XX). There are no signs of HIV-reactivation (PCR <50 copies, CD4+ 295 cells; deep virology status performed in Hamburg: Plasma VL RNA copies/ml: 1107, DNA/1 Mio. PBMC: 2265, Integrated HIV DNA/PCR: 17.670, HIVAb/p24Ag 4th generation: pos./neg.). She is still on HAART: Prezista 800 + Ritonavir 100 + Lamivudine 300.
Patient 2, female, 29 years old was diagnosed with an acute lymphoblastic leukemia in 1993 (at the age of 10). First CR was achieved after the first course of chemotherapy. A HIV/hepatitis C co-infection was diagnosed in 2005. HIV was transmitted from the patient’s husband. HAART was started in 2009. First late relapse of ALL was confirmed in October 2011. Second CR MRD (+) was achieved after second course Hyper-CVAD / MxA treatment in December 2011. Full chemotherapy program (8 cycles) of Hyper-CVAD / MxA was completed in May 2012. Patient had no related matched donors. A search for the unrelated donor was initiated in February 2012. By the time of HSCT, the patient has achieved a second remission of ALL, MRD (+), HIV status was satisfactory: PCR <50 copies, CD4+ 108 cells on HAART. On 19 July 2012, an allogeneic stem cell transplantation was performed, with reduced intensity conditioning (RIC) regimen and standard GVHD prophylaxis, including ATG + tacrolimus and MMF. Donor: MUD, female, ABO-compatible, CCR5, wt/wt. Source of HSC: PBSC (CD34+ 9.1 x 106). No severe infectious complications were registered in pre-engraftment phase. Due to severe tacrolimus toxicity, the GVHD prophylaxis was modified, by switching from tacrolimus to corticosteroids. Engraftment was registered on Day +12. On Day +23, CMV reactivation with severe CMV disease of gut was diagnosed, as shown by biopsy. The patient died on Day +41 from generalized gancyclovir-resistant CMV disease affecting gut, liver, and kidneys.
Patient 3, female, 26 years old was diagnosed with HIV, and HAART was immediately administered in April 2012. HIV was transmitted from the patient’s husband. Acute leukemia of mixed phenotype was diagnosed in May 2012. First CR with MRD (+) was achieved only after at the 3rd course of chemotherapy. The patient had no matched related donors. A search for unrelated donor was initiated in December 2012. At the moment of HSCT, the ALL disease was in its first remission, MRD (+); HIV status was satisfactory: PCR <50 copies, CD4+ 117 cells on HAART. On the April 1, 2013, allogeneic stem cell transplantation with a RIC regimen and standard GVHD prophylaxis (ATG+cyclosporine A+MMF), including Maraviroc, was performed.
Maraviroc is an antiretroviral agent belonging to the CCR5 receptor antagonists, as well as entry inhibitors, it is used for treatment of HIV infection. It also appears to reduce graft-versus-host disease in patients treated with allogeneic bone marrow transplantation for leukemia, in a phase 1/2 study [36].
We have tested the recipient and donor for a CCR5 gene mutation. The recipient (patient 3) had no CCR5 delta32 mutation (wild type/wild type). The donor harbored a single CCR5 delta32 allele (a heterozygotic state). A male, HLA-matched, ABO-incompatible, unrelated donor was used for HST. Peripheral blood stem cells were used as a source of HSCs (CD34+ cells, 6,5 x 106). No relevant complications in pre-engraftment phase were registered. Engraftment and acute GVHD of the skin grade 2-3 were registered since Day +12. GVHD was treated by a high dose of CsA (control serum level) + prolonged MMF and Maraviroc + topic steroids. On the Day +60, no signs of GVHD were reported. Immunosupressive therapy was discontinued on the Day +100 due to the MRD positivity registered by flow cytometry. Local light skin chronic GVHD was observed for two months, and CR with MRD (-) was achieved. Viral loads and CD4+ counts in the patient 3 during treatment are presented in Fig. 2.

Figure 2. Patient 3: Dynamics of HIV amounts (PCR) and CD4+ counts
Currently, at 22 months after allo-HSCT, the patient is in a good health and has an active lifestyle, CR of acute leukemia (full chimerism, MRD(-)), with no signs of HIV-reactivation (PCR <50 copies, CD4+ 828 cells; deep virology status in Hamburg: Plasma VL RNA copies/ml: 43, DNA/1 Mio. PBMC: 71, Integrated HIV DNA/PCR: 517, HIVAb/p24Ag 4th generation: pos./neg.). She is still on HAART: Abacavir 600 + Lamivudine 300 + Raltegravir 800. An important fact is that the patient’s sample contained the CCR5-wildtype-allele and the CCR5 del 32 mutation = donor’s heterozygote type and was converted to heterozygote CCR5 del 32 mutation.
In conclusion, allo-HSCT with RIC is an effective and feasible therapeutic modality for high-grade hematological malignancies in patients with HIV. There were no severe toxicity and drug-drug interactions between HAART, conditioning regimen, and immunosuppressive drugs. HAART and immunosuppressive agents can be safely administered after allo-HSCT. Engraftment and full donor chimaerism were achieved at term as in the general population allo-HSCT recipients. Relapse of acute leukemia could be successful and safety treated with immunoadoptive therapy (DLI) after allo-HSCT. There were no specific infections or other particular complication in HIV positive pts after allo-HSCT. We suggest that patient 3 may be “near to functional cure”. Allo-HSCT ongoing with HAART is the same effective and safety strategy for the treatment high-risk hematologic malignancies in HIV population.
Acknowledgements
Staff of CIC 725, Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, First Pavlov State Medical University of Saint-Petersburg, Russia and International Registry Stefan Morsch Stiftung, Birkenfeld, Germany.
No conflict of interest is reported.
|
Characteristics |
Case 1 |
Case 2 |
Case3 |
|
Demographic Age |
50 |
29 |
26 |
|
Diagnosis |
AML |
ALL |
AL, mixed phenotype |
|
Status |
CR2 |
CR2 |
CR1 |
|
HIV status at Tx CD4+ |
500 cells/ml |
380 cells/ml |
114 cells/ml |
|
HIV-VL |
700 copies/ml |
<50 copies/ml |
<50 copies/ml |
|
cART |
No |
Yes |
Yes |
|
Transplant Donor type CCR5 del32 |
Sibling matched NA |
MUD (12/12) wt/wt |
MUD (12/12) del 32/wt; heterozygote |
|
Conditioning |
RIC (Flu150+Bu8) |
RIC (Flu150+Mel140) |
RIC (Flu150+Bu8) |
|
GvHD proph |
CsA |
ATG, MMF, steroids |
ATG, CsA, MMF, maraviroc |
|
Engraftment Neutrophil |
+ 18 d |
+ 12 d |
+ 18 d |
|
Platelet |
+ 19 d |
+ 14 d |
+ 18 d |
|
Full donor chimaerism |
+ 25 d |
+ 20 d |
+ 20 d |
|
GvHD Acute, grade |
No |
No |
II |
|
Chronic |
No |
No |
No |
|
LFU |
57 months |
41 days |
22 months |
|
Status at LFU |
Alive |
Dead |
Alive |
|
HIV status at LFU CD4+ |
800 cells/ml |
NA |
480 cells/ml |
|
HIV-VL |
<50 copies/ml |
NA |
<50 copies/ml |
|
cART |
Continues |
NA |
Continues |
Table 1. Baseline patients and transplants characteristics
References
- Aboulafia DM, Meneses M, Ginsberg S et al. Acute myeloid leukemia in patients infected with HIV-1. AIDS 2002; 16(6):865-76.
- Al-Bahar S, Pandita R, Dhabhar BN, Al-Bahar E. Human immunodeficiency virus (HIV) infection associated with acute myeloblastic leukaemia in a low HIV prevalence area. Acta Haematol 1994; 91: 52-53.
- Allers K, Hütter G, Hofmann J et al. Evidence for the cure of HIV infection by CCR5 delta 32 / delta32 stem cell transplantation. Blood 2011; 117(10): 2791-9.
- Archin NM, Libesty AL, Kashuba AD et al. Administration of vorinostat disrupts HIV-1 latency in patients on antiretroviral therapy. Nature 2012; 482: 482–5.
- Berger EA. Targeted cytotoxic therapy: adapting a rapidly progressing anti-cancer paradign for depleting HIV infected cell reservoirs. Curr Opin HIV/AIDS 2011; 6: 80-5.
- Borvak J, Chou CS, Van Dyke G et al. The use of cyclosporine, FK506, and SDZ NIM811 to prevent CD25-quiescent peripheral blood mononuclear cells from producing HIV. J Infect Dis 1996; 174: 850-3.
- Choi SW, Reddy P. Current and emerging strategies for the prevention of graft versus host disease. Nat Rev Clin Oncol 2014; 11(9): 536-47.
- Didigu CA, Wilen CB, Wang J et al. Simultaneous zinc-finger nuclease editing of the HIV coreceptors CCR5 and CXCR4 protects CD4+ T cells from HIV-1 infection. Blood 2014; 123(1): 61-9.
- Diez-Martin JL, Balsalobre P, Re A et al. Comparable survival between HIV+ and HIV–non-Hodgkin and Hodgkin lymphoma patients undergoing autologous peripheral blood stem cell transplantation. Blood 2009; 113(23): 6011-14.
- Engels EA, Pfeiffer RM, Goedert JJ et al. Trends in cancer risk among people with AIDS in the United States 1980-2002. AIDS 2006; 20(12): 1645-54.
- Farber CM, Ferehans W, Capel P et al. Chemotherapy of acute myeloblastic leukaemia in an HIV carrier. Eur J Haematol 1993; 51: 180.
- Geriniere L, Bastion Y, Dumontet C et al. Heterogeneneity of acute lymphoblastic leukaemia in HIV-seropositive patients. Ann Oncol 1994; 5(5): 437-40.
- Gupta V, Tomblyn M, Pedersen TL et al. Allogeneic hematopoietic cell transplantation in human immunodeficiency virus-positive patients with hematologic disorders: a report from the Center for International Blood and Marrow Transplant Research. Biol Blood Marrow Transplantion 2009; 15: 864-71.
- Hamilton J, McBride M, Kettle P. Acute B cell lymphoblastic leukaemia and human immunodeficiency virus infection (HIV). Ulster Med J 2002; 71(1): 72-5.
- Henrich T, Hanhauser E, Marty FM et al. Antiretroviral-free HIV-1 remission and viral rebound after allogeneic stem cell transplantation: report of 2 cases. Ann Intern Med 2014; 161(5): 319-27.
- Henrich T, Hu Z, Li JZ et al. Long-term reduction in peripheral blood HIV type 1 reservoirs following reduced-intensity conditioning allogeneic stem cell transplantation. J Infect Dis 2013; 207(11):1694-702.
- Hütter G, Ganepola S. Eradication of HIV by transplantation of CCR5-deficient hematopoietic stem cells. The Scientific World J 2011; 11: 1068-76.
- Hütter G, Thielb E. Allogeneic transplantation of CCR5-deficient progenitor cells in a patient with HIV infection: an update after 3 years and the search for patient no.2. AIDS 2011;25: 273-75.
- Hütter G, Zaia JA. Allogeneic haematopoietic stem cell transplantation in patients with human immunodeficiency virus: the experiences of more than 25 years. Clin Exp Immunol 2011; 163; 284-95.
- Hütter G, Nowak D, Mossner M et al. Long-term control of HIV by CCR5 delta32/ delta32 stem-cell transplantation. N Engl J Med 2009; 360: 692-8.
- Johansson S, Goldenberg DM, Griffiths GL et al. Elimination of HIV-1 infection by treatment with a doxorubicin-conjugated antienvelope antibody. AIDS 2006; 20: 1911-5.
- Kane D, Keating S, McCann S, Mulcahy F. The management of acute myeloid leukaemia (AML) in human immunodeficiency virus (HIV) infection: a case report and review. Int J STD and AIDS, 1997; 8: 272-4.
- Kiem HP, Jerome KR, Deeks SG et al. Hematopoietic-stem-cell-based gene therapy for HIV disease. Stem Cell 2012; 10: 137-47.
- King JAC, Nye DM, O’Connor MB et al. Acute myelogenous leukemia (FAB AMLM1) in the setting of HIV infection and G-CSF therapy: a case report and review of the literature. Ann Hematol 1998; 77: 69-73.
- Krishnan A, Palmer JM, Zaia JA et al. HIV status does not affect the outcome of autologous stem cell transplantation (ASCT) for non-Hodgkin lymphoma (NHL). Biol Blood Marrow Transplant 2010; 16(9): 1302-8.
- Launay O, Guillevin L. Epidemiology of HIV-associated malignancies. Bull Cancer 2003; 90(5); 387-92.
- Little RF, Pittaluga S, Grant N et al. Highly effective treatment of AIDS-related lymphoma with dose-adjusted EPOCH: impact of antiretroviral therapy suspension and tumor biology. Blood. 2003; 101: 4653-9.
- Liu B, Yu X, Luo K et al. Influence of primate lentiviral Vif and proteasome inhibitors on human immunodeficiency virus type 1 virion packaging of APOBEC3G. J Virol 2004; 78: 2072-81.
- Mitsuyasu R. Curing HIV: lessons from cancer therapy. Curr Opin HIV AIDS 2013; 8(3): 224-9.
- Nakamura R, Forman SJ. Reduced intensity conditioning for allogeneic hematopoietic cell transplantation: considerations for evidence-based GVHD prophylaxis
Expert Rev Hematol 2014; 7(3), :407-21. - Passweg J, Baldomero H, Bader P et al. Hematopoietic SCT in Europe: recent trends in the use of alternative donors showing more haploidentical donors but fewer cord blood transplants. Bone Marrow Transplantation 2015; Suppl 50: 476-82.
- Passweg J, Baldomero H, Peters C et al. Hematopoietic SCT in Europe: data and trends in 2012 with special consideration of pediatric transplantation. Bone Marrow Transplantation 2014 ; Suppl 49: 744-50.
- Pees HW, Radtke H, Schwamborn J et al. The BFM-protocol for HIV-negative Burkitt’ s lymphomas and L3 ALL in adult patients: a high chance for a cure. Ann Hematol 1992; 65(5): 201-5.
- Petz L. Cord Blood Transplantation for Cure of HIV Infections. Stem Cells Transl Med 2013; 2: 635-7.
- Piekarz RL, Frye R, Prince HM et al. Phase 2 trial of romidepsin in patients with peripheral T-cell lymphoma. Blood 2011; 117: 5827-34.
- Reshef R, Luger SM, Hexner EO et al. Blockade of lymphocyte chemotaxis in visceral graft-versus-host disease. N Engl J Med 2012; 367(2): 135-45.
- Reuse S, Calao M, Kabeya K et al. Synergistic activation of HIV-1 expression by deacetylase inhibitors and prostratin: implications for treatment of latent infection. PLoS One 2009;4:e6903.
- Rivers JK, Laubenstein LJ, Postel AH. Acute monocytic leukaemia in an HIV-seropositive man. Clin Exp Dermatol 1992; 17: 203-5.
- Shimizu S, Ringpis GE, Marsden MD et al. RNAi-mediated CCR5 knockdown provides HIV-1 resistance to memory T cells in humanized BLT mice. Mol Ther Nucl Acids 2015 Feb; 4(2): e227.
- Simard C, Jolicoueur P. The effect of antineoplastic drugs on murine acquired immunodeficiency syndrome. Science 1991; 252:305-8.
- Sutton L, GueAnel P, Tanguy ML et al. Acute myeloid leukaemia in human immunodeficiency virus infected adults: epidemiology, treatment feasibility and outcome. Brit J Haematol 2001; 112: 900-8.
- Tebas P, Stein D, Tang WW et al. Gene editing of CCR5 in autologous CD4 T cells of persons infected with HIV. N Engl J Med 2014; 370: 901-10.
- Turner ML, Watson HG, Russell L et al. An HIV positive haemophiliac with acute lymphoblastic leukaemia successfully treated with intensive chemotherapy and syngeneic bone marrow transplantation. Bone Marrow Transplant 1992; 9(5): 387-9.
- van Lunzen J, Fehse B, Hauber J. Gene Therapy Strategies: Can We Eradicate HIV? Curr HIV/AIDS 2011; Rep 8: 78-84.
- van Lunzen J, Glaunsinger T, Stahmer I et al. Transfer of autologous gene-modified T cells in HIV-infected patients with advanced immunodeficiency and drug-resistant virus Mol Ther 2007; 15: 1024-33.
- World Health Organization http://www.who.int/hiv/data
- Yukl SA, Boritz E, Busch M et al. Challenges in detecting HIV persistence during potentially curative interventions: A study of the Berlin patient. PLOS Pathogens 2013; 9 (5): e1003347. doi:10.1371/journal.ppat.1003347.
- Zhen A, Kitchen S. Stem-cell-based gene therapy for HIV infection. Viruses 2014; 6: 1-12; doi:10.3390/v6010001.
Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "239" ["VALUE"]=> array(2) { ["TEXT"]=> string(4127) "<p class="Summery_Rus" lang="ru-RU">Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти <span lang="en-US">HLA</span>-совместимого донора с гомозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32. Алло-ТГСК от донора без мутации гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3853) "Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена CCR5 del 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена CCR5 del 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти HLA-совместимого донора с гомозиготной мутацией гена CCR5 del 32. Алло-ТГСК от донора без мутации гена CCR5 del 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена CCR5 del 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "240" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-24-30" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-24-30" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "241" ["VALUE"]=> array(2) { ["TEXT"]=> string(497) "<p class="Autor">Boris V. Afanasyev<sup>1</sup>, Marina Popova<sup>1</sup>, Sergey Bondarenko<sup>1</sup>, Ilya Zyuzgin<sup>2</sup>, Elena Babenko<sup>1</sup>, Aleksander Alyanskiy<sup>1</sup>, Susanne Morsch<sup>3</sup>, Jan van Lunzen<sup>4</sup>, Boris Fehse<sup>5</sup>, Axel R. Zander <sup>5</sup>, Ludmila S. Zubarovskaya<sup>1</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(343) "Boris V. Afanasyev1, Marina Popova1, Sergey Bondarenko1, Ilya Zyuzgin2, Elena Babenko1, Aleksander Alyanskiy1, Susanne Morsch3, Jan van Lunzen4, Boris Fehse5, Axel R. Zander 5, Ludmila S. Zubarovskaya1
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "242" ["VALUE"]=> array(2) { ["TEXT"]=> string(1269) "<p class="Autor_place_work"> <sup>1</sup>Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, </p> <p class="Autor_place_work"> First Pavlov State Medical University of Saint-Petersburg, Russia </p> <p class="Autor_place_work"> <sup>2</sup>Oncology, Hematology and BMT department, Petrov Research Institute of Oncology, Saint-Petersburg, Russia </p> <p class="Autor_place_work"> <sup>3</sup>Stefan Morsch Stiftung, Birkenfeld, Germany </p> <p class="Autor_place_work"> <sup>4</sup>Infectious Diseases Unit, University Medical Center Hamburg-Eppendorf, Hamburg, Germany </p> <p class="Autor_place_work"> <sup>5</sup>Clinic for Stem Cell Transplantation, University Medical Center Hamburg-Eppendorf, Hamburg, Germany </p> <p class="Autor_place_work"> Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation </p> <p class="Autor_place_work"> First Pavlov State Medical University of Saint-Petersburg, Russia </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1033) "1Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation,
First Pavlov State Medical University of Saint-Petersburg, Russia
2Oncology, Hematology and BMT department, Petrov Research Institute of Oncology, Saint-Petersburg, Russia
3Stefan Morsch Stiftung, Birkenfeld, Germany
4Infectious Diseases Unit, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
5Clinic for Stem Cell Transplantation, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation
First Pavlov State Medical University of Saint-Petersburg, Russia
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "243" ["VALUE"]=> array(2) { ["TEXT"]=> string(2113) "<h2 class="Summery"> <span style="font-family: Arial, sans-serif;">Summery</span><br> </h2> <p class="Summery"> Introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown with only limited case reports and small series. Most of these patients are potentially curable from hematological malignancies by allo-HSCT. Allo-HSCT from donor with homozygote CCR5 del 32 mutation can cure from the both diseases: HIV and cancer that was demonstrated by the Berlin patient. Prevalence of this mutation is low and this way seems unacceptable in most HIV-positive patients with high-risk hematologic malignancies. Allo-HSCT from donor without CCR5 mutation with ongoing HAART has looked more promising but has failed which was reported as Boston patients. But other aspects including donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and new agent therapy in HIV-patients maintain interest to allo-HSCT as a potential cure procedure. It was not reported an allo-HSCT from donor with heterozygote CCR5 del 32 mutation. An application of HAART in post-transplant period can be used not only for HIV control also as a component of GvHD prophylaxis. We report on three HIV-infected patients with high-risk acute leukemia which have undergone an allo-HSCT and donor lymphocyte infusions (DLI) to treat post-allo-HSCT relapse in Saint-Petersburg. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2041) " Summery
Introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown with only limited case reports and small series. Most of these patients are potentially curable from hematological malignancies by allo-HSCT. Allo-HSCT from donor with homozygote CCR5 del 32 mutation can cure from the both diseases: HIV and cancer that was demonstrated by the Berlin patient. Prevalence of this mutation is low and this way seems unacceptable in most HIV-positive patients with high-risk hematologic malignancies. Allo-HSCT from donor without CCR5 mutation with ongoing HAART has looked more promising but has failed which was reported as Boston patients. But other aspects including donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and new agent therapy in HIV-patients maintain interest to allo-HSCT as a potential cure procedure. It was not reported an allo-HSCT from donor with heterozygote CCR5 del 32 mutation. An application of HAART in post-transplant period can be used not only for HIV control also as a component of GvHD prophylaxis. We report on three HIV-infected patients with high-risk acute leukemia which have undergone an allo-HSCT and donor lymphocyte infusions (DLI) to treat post-allo-HSCT relapse in Saint-Petersburg.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "244" ["VALUE"]=> string(146) "Saint-Petersburg experience of allogeneic hematopoietic stem cell transplantation in patients with acute leukemia and human immunodeficiency virus" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(146) "Saint-Petersburg experience of allogeneic hematopoietic stem cell transplantation in patients with acute leukemia and human immunodeficiency virus" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1210" ["VALUE"]=> string(2) "14" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "14" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1211" ["VALUE"]=> string(2) "15" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "15" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(13) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "241" ["VALUE"]=> array(2) { ["TEXT"]=> string(497) "<p class="Autor">Boris V. Afanasyev<sup>1</sup>, Marina Popova<sup>1</sup>, Sergey Bondarenko<sup>1</sup>, Ilya Zyuzgin<sup>2</sup>, Elena Babenko<sup>1</sup>, Aleksander Alyanskiy<sup>1</sup>, Susanne Morsch<sup>3</sup>, Jan van Lunzen<sup>4</sup>, Boris Fehse<sup>5</sup>, Axel R. Zander <sup>5</sup>, Ludmila S. Zubarovskaya<sup>1</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(343) "Boris V. Afanasyev1, Marina Popova1, Sergey Bondarenko1, Ilya Zyuzgin2, Elena Babenko1, Aleksander Alyanskiy1, Susanne Morsch3, Jan van Lunzen4, Boris Fehse5, Axel R. Zander 5, Ludmila S. Zubarovskaya1
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(343) "Boris V. Afanasyev1, Marina Popova1, Sergey Bondarenko1, Ilya Zyuzgin2, Elena Babenko1, Aleksander Alyanskiy1, Susanne Morsch3, Jan van Lunzen4, Boris Fehse5, Axel R. Zander 5, Ludmila S. Zubarovskaya1
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "243" ["VALUE"]=> array(2) { ["TEXT"]=> string(2113) "<h2 class="Summery"> <span style="font-family: Arial, sans-serif;">Summery</span><br> </h2> <p class="Summery"> Introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown with only limited case reports and small series. Most of these patients are potentially curable from hematological malignancies by allo-HSCT. Allo-HSCT from donor with homozygote CCR5 del 32 mutation can cure from the both diseases: HIV and cancer that was demonstrated by the Berlin patient. Prevalence of this mutation is low and this way seems unacceptable in most HIV-positive patients with high-risk hematologic malignancies. Allo-HSCT from donor without CCR5 mutation with ongoing HAART has looked more promising but has failed which was reported as Boston patients. But other aspects including donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and new agent therapy in HIV-patients maintain interest to allo-HSCT as a potential cure procedure. It was not reported an allo-HSCT from donor with heterozygote CCR5 del 32 mutation. An application of HAART in post-transplant period can be used not only for HIV control also as a component of GvHD prophylaxis. We report on three HIV-infected patients with high-risk acute leukemia which have undergone an allo-HSCT and donor lymphocyte infusions (DLI) to treat post-allo-HSCT relapse in Saint-Petersburg. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2041) " Summery
Introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown with only limited case reports and small series. Most of these patients are potentially curable from hematological malignancies by allo-HSCT. Allo-HSCT from donor with homozygote CCR5 del 32 mutation can cure from the both diseases: HIV and cancer that was demonstrated by the Berlin patient. Prevalence of this mutation is low and this way seems unacceptable in most HIV-positive patients with high-risk hematologic malignancies. Allo-HSCT from donor without CCR5 mutation with ongoing HAART has looked more promising but has failed which was reported as Boston patients. But other aspects including donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and new agent therapy in HIV-patients maintain interest to allo-HSCT as a potential cure procedure. It was not reported an allo-HSCT from donor with heterozygote CCR5 del 32 mutation. An application of HAART in post-transplant period can be used not only for HIV control also as a component of GvHD prophylaxis. We report on three HIV-infected patients with high-risk acute leukemia which have undergone an allo-HSCT and donor lymphocyte infusions (DLI) to treat post-allo-HSCT relapse in Saint-Petersburg.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(2041) " Summery
Introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown with only limited case reports and small series. Most of these patients are potentially curable from hematological malignancies by allo-HSCT. Allo-HSCT from donor with homozygote CCR5 del 32 mutation can cure from the both diseases: HIV and cancer that was demonstrated by the Berlin patient. Prevalence of this mutation is low and this way seems unacceptable in most HIV-positive patients with high-risk hematologic malignancies. Allo-HSCT from donor without CCR5 mutation with ongoing HAART has looked more promising but has failed which was reported as Boston patients. But other aspects including donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and new agent therapy in HIV-patients maintain interest to allo-HSCT as a potential cure procedure. It was not reported an allo-HSCT from donor with heterozygote CCR5 del 32 mutation. An application of HAART in post-transplant period can be used not only for HIV control also as a component of GvHD prophylaxis. We report on three HIV-infected patients with high-risk acute leukemia which have undergone an allo-HSCT and donor lymphocyte infusions (DLI) to treat post-allo-HSCT relapse in Saint-Petersburg.
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "240" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-24-30" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-24-30" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-24-30" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "244" ["VALUE"]=> string(146) "Saint-Petersburg experience of allogeneic hematopoietic stem cell transplantation in patients with acute leukemia and human immunodeficiency virus" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(146) "Saint-Petersburg experience of allogeneic hematopoietic stem cell transplantation in patients with acute leukemia and human immunodeficiency virus" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(146) "Saint-Petersburg experience of allogeneic hematopoietic stem cell transplantation in patients with acute leukemia and human immunodeficiency virus" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "242" ["VALUE"]=> array(2) { ["TEXT"]=> string(1269) "<p class="Autor_place_work"> <sup>1</sup>Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, </p> <p class="Autor_place_work"> First Pavlov State Medical University of Saint-Petersburg, Russia </p> <p class="Autor_place_work"> <sup>2</sup>Oncology, Hematology and BMT department, Petrov Research Institute of Oncology, Saint-Petersburg, Russia </p> <p class="Autor_place_work"> <sup>3</sup>Stefan Morsch Stiftung, Birkenfeld, Germany </p> <p class="Autor_place_work"> <sup>4</sup>Infectious Diseases Unit, University Medical Center Hamburg-Eppendorf, Hamburg, Germany </p> <p class="Autor_place_work"> <sup>5</sup>Clinic for Stem Cell Transplantation, University Medical Center Hamburg-Eppendorf, Hamburg, Germany </p> <p class="Autor_place_work"> Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation </p> <p class="Autor_place_work"> First Pavlov State Medical University of Saint-Petersburg, Russia </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1033) "1Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation,
First Pavlov State Medical University of Saint-Petersburg, Russia
2Oncology, Hematology and BMT department, Petrov Research Institute of Oncology, Saint-Petersburg, Russia
3Stefan Morsch Stiftung, Birkenfeld, Germany
4Infectious Diseases Unit, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
5Clinic for Stem Cell Transplantation, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation
First Pavlov State Medical University of Saint-Petersburg, Russia
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1033) "1Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation,
First Pavlov State Medical University of Saint-Petersburg, Russia
2Oncology, Hematology and BMT department, Petrov Research Institute of Oncology, Saint-Petersburg, Russia
3Stefan Morsch Stiftung, Birkenfeld, Germany
4Infectious Diseases Unit, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
5Clinic for Stem Cell Transplantation, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation
First Pavlov State Medical University of Saint-Petersburg, Russia
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(11) { [0]=> string(3) "227" [1]=> string(3) "228" [2]=> string(3) "229" [3]=> string(3) "230" [4]=> string(3) "231" [5]=> string(3) "232" [6]=> string(3) "233" [7]=> string(3) "234" [8]=> string(3) "235" [9]=> string(3) "236" [10]=> string(3) "237" } ["VALUE"]=> array(11) { [0]=> string(2) "39" [1]=> string(2) "34" [2]=> string(2) "33" [3]=> string(2) "38" [4]=> string(2) "11" [5]=> string(2) "37" [6]=> string(2) "36" [7]=> string(2) "40" [8]=> string(2) "42" [9]=> string(2) "35" [10]=> string(2) "41" } ["DESCRIPTION"]=> array(11) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" [7]=> string(0) "" [8]=> string(0) "" [9]=> string(0) "" [10]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(11) { [0]=> string(2) "39" [1]=> string(2) "34" [2]=> string(2) "33" [3]=> string(2) "38" [4]=> string(2) "11" [5]=> string(2) "37" [6]=> string(2) "36" [7]=> string(2) "40" [8]=> string(2) "42" [9]=> string(2) "35" [10]=> string(2) "41" } ["~DESCRIPTION"]=> array(11) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" [7]=> string(0) "" [8]=> string(0) "" [9]=> string(0) "" [10]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(11) { [0]=> string(56) "Susanne Morsch" [1]=> string(60) "Boris V. Afanasyev" [2]=> string(55) "Marina Popova" [3]=> string(62) "Aleksander Alyanskiy" [4]=> string(56) "Axel R. Zander" [5]=> string(55) "Elena Babenko" [6]=> string(54) "Ilya Zyuzgin" [7]=> string(56) "Jan van Lunzen" [8]=> string(65) "Ludmila S. Zubarovskaya" [9]=> string(59) "Sergey Bondarenko" [10]=> string(53) "Boris Fehse" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "238" ["VALUE"]=> array(2) { ["TEXT"]=> string(395) "<p class="Autor">Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская<sup> </sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(361) "Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(361) "Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "224" ["VALUE"]=> string(19) "13.04.2015 13:38:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "13.04.2015 13:38:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "13.04.2015 13:38:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "225" ["VALUE"]=> string(19) "12.06.2015 13:39:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "12.06.2015 13:39:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "12.06.2015 13:39:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "902" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(7) { [0]=> string(4) "1203" [1]=> string(4) "1204" [2]=> string(4) "1205" [3]=> string(4) "1206" [4]=> string(4) "1207" [5]=> string(4) "1208" [6]=> string(4) "1209" } ["VALUE"]=> array(7) { [0]=> string(2) "43" [1]=> string(2) "44" [2]=> string(2) "45" [3]=> string(2) "46" [4]=> string(2) "47" [5]=> string(2) "48" [6]=> string(2) "49" } ["DESCRIPTION"]=> array(7) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(7) { [0]=> string(2) "43" [1]=> string(2) "44" [2]=> string(2) "45" [3]=> string(2) "46" [4]=> string(2) "47" [5]=> string(2) "48" [6]=> string(2) "49" } ["~DESCRIPTION"]=> array(7) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(7) { [0]=> string(60) "Алло-ТГСК" [1]=> string(49) "ВИЧ" [2]=> string(68) "острый лейкоз" [3]=> string(123) "кондиционирование сниженной интенсивности" [4]=> string(97) "инфузии донорских лимфоцитов" [5]=> string(69) "мутации CCR5 del 32" [6]=> string(61) "маравирок" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "226" ["VALUE"]=> string(2) "33" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "33" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(55) "Marina Popova" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "239" ["VALUE"]=> array(2) { ["TEXT"]=> string(4127) "<p class="Summery_Rus" lang="ru-RU">Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти <span lang="en-US">HLA</span>-совместимого донора с гомозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32. Алло-ТГСК от донора без мутации гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3853) "Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена CCR5 del 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена CCR5 del 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти HLA-совместимого донора с гомозиготной мутацией гена CCR5 del 32. Алло-ТГСК от донора без мутации гена CCR5 del 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена CCR5 del 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(3853) "Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена CCR5 del 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена CCR5 del 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти HLA-совместимого донора с гомозиготной мутацией гена CCR5 del 32. Алло-ТГСК от донора без мутации гена CCR5 del 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена CCR5 del 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.
" } } } [5]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "2" ["~IBLOCK_SECTION_ID"]=> string(1) "2" ["ID"]=> string(1) "6" ["~ID"]=> string(1) "6" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(180) "Аллогенная трансплантация гемопоэтических стволовых клеток и органов у одного и того же пациента" ["~NAME"]=> string(180) "Аллогенная трансплантация гемопоэтических стволовых клеток и органов у одного и того же пациента" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:41:31" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:41:31" ["DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-14-18/" ["~DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-14-18/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(21234) "Introduction
Solid organ transplantation (SOT) is widely used for the treatment of end-stage organ insufficiency. About 30000 SOTs were performed in the European Union in 2011, comprising approximately 19000 kidney, 7000 liver and 2000 heart and other (including combined) transplants [3]. Allogeneic hematopoietic stem cell transplantation (HSCT) is the only cure or the most effective treatment for a large number of malignant and non-malignant diseases of the lympho-hematopoietic system with an otherwise poor prognosis. At present, the number of allogeneic HSCTs in Europe is approximately 15000 per year [8]. With these large numbers of patients, the likelihood of coincidental occurrence of disorders potentially indicating SOT and HSCT in the same patient is increasing. Such transplantation combinations can be problematic for many reasons.
Allogeneic HSCT is an intensive treatment which causes frequently organ injury and failure, resulting in a potential indication for a SOT. The mechanisms of organ injury include cytotoxic drugs and radiotherapy in the pretransplant conditioning, organ-toxic agents in supportive care, and immunological mechanisms. The organs most often affected are kidney, liver, lung and heart. Factors that may complicate a SOT in this setting are the fragility of the patient as a consequence of the toxicity of HSCT, immunosuppressive treatment for the HSCT which may not be optimal for the SOT, potential immunological problems caused by tissue type differences between the recipient, the hematopoietic graft and the solid organ graft, and infections. In SOT recipients, the long-lasting immunosuppressive medication may affect the function of organs, and increase the risk of infections. SOT can be associated with development of hematological disorders comprising aplastic anemia, post-transplant lymphoproliferative disease, acute myeloid leukemia and myelodysplastic syndromes [1] which may be a potential indication for allogeneic HSCT.
As the clinical situation is often found to be complicated and the risk of treatment failure regarded as high, the numbers of SOTs to HSCT recipients and those of HSCTs to SOT recipients have been low as compared to the number of patients who would have a potential indication for such treatment. Until recent years the literature of such transplantations consisted mainly of case reports as reviewed by Basak et al. [1], Chiang and Lazarus [2], Koenecke et al. [7], with obvious risk of publication bias. As the results of such combined transplantations were not well known, the European Society for Blood and Marrow Transplantation (EBMT) carried out two surveys to collect the experience in Europe and to analyze the outcome. One survey evaluated the experience with SOT in HSCT recipients, the other HSCTs carried out in SOT recipients.
EBMT surveys
In the EBMT survey of SOTs carried out in HSCT recipients by Koenecke et al [7], 107 centers with the total of 67000 allogeneic HSCTs carried out between 1984 and 2007 participated. Among them, 28 centers reported having carried out a total of 45 SOTs in 40 patients for organ failure after HSCT. The transplantations comprised 15 renal, 15 liver, 13 lung grafts, 1 heart, and 1 skin transplantation. In approximately 2/3 of the HSCTs, they were performed for malignant hematological disease (n=28), the other patients had aplastic anemia, or an inherited disorder (n=6 for both). In most cases, the donor had been a sibling, and bone marrow has been transplanted. Almost all patients had received a standard full-intensity conditioning. Twenty-two patients had developed grade II or higher acute GVHD and 23 patients, extensive chronic GVHD before the SOT. This was the cause for SOT in six patients receiving liver transplants, and in 13 patients undergoing lung transplantation. In all other patients, clinically significant GVHD resolved before the SOT. Median age at the time of the renal transplantation was 35 (range 8-64) years, for liver transplantation, 20 (1-56) years, and for lung transplantation, 32 (11-55) years. The median time between HSCT and renal transplantation was 84 (range 8-188) months, that in liver transplantations 34 (range 1-137) months, and in lung transplantations, 69 (range 7-196) months. In renal transplantations following HSCT, the most common cause was drug- or radiation-induced kidney failure. Patients receiving liver transplantation could be divided in two groups, early and late transplantation after HSCT. Early liver transplantation (up to six months post-HSCT) was performed due to acute liver failure caused by veno-occlusive disease (VOD) or acute GVHD, late transplantation (usually, 2-5 years after HSCT) was mostly carried out because of chronic liver-GVHD or cirrhosis. The indication for lung transplantation was bronchiolitis obliterans (BOS)/ chronic GVHD in all these patients. The overall 5-year survival after SOT was 78%, in renal transplantations, 100%, in liver transplantations, 71% and in lung transplantations, 63%. None of the renal transplantation patients was on dialysis at the end of the follow-up. The overall 2-year incidence of SOT failure was 16% (20% in patients with GVHD preceding SOT versus 7% in GVHD-free cases). Graft rejection occurred in approximately 30% of the patients with each type of transplantation, but it could be usually treated. Two patients with renal transplantation, 2 with liver transplantation and 4 with lung transplantation experienced graft failure. The relapse incidence of the underlying malignant disease was 4% at 5 years after the SOT. Six patients received the SOT from the original HSCT donors (4 kidneys, 1 liver, 1 lung transplantation). All of them, except of the lung transplantation patient, were alive at the time of the analysis.
In the course of EBMT survey by Basak et al [1], with 101 centers participating, 18 centers reported a total of 31 HSCTs in 28 SOT recipients. Thirteen of the patients have received a liver transplantation, 12 patients received renal grafts, and three underwent heart transplantation. Malignant hematological disease was the reason for HSCT in 22 of the 28 patients, the most common indications being acute myeloblastic leukemia (AML) in 8 cases, acute lymphoblastic leukemia (ALL) and chronic myeloid leukemia (CML) in 4 cases each. The diagnosis leading to HSCT was known before the SOT in 8/28 patients (AML, ALL, CML, chronic granulomatous disease, primary immunodeficiency, severe aplastic anemia). The patients were young, with median age at the HSCT of 25 (1-62) years. The median time from SOT to HSCT was 37 (1-315) months. The sources of hematopoietic graft were as follows: peripheral blood stem cells in 21, bone marrow in 9, and the both in one patient. The donor was a HLA-identical sibling in 12, a matched unrelated donor in 14, and haploidentical, in 4 cases. Seventeen patients received myeloablative conditioning. In the rest of this group, intensity of the conditioning was reduced. Ex vivo T-cell depletion was carried out in five cases. Successful engraftment was registered in 25/26 evaluable patients. Eight patients developed grade II-IV acute GVHD. Chronic GVHD occurred in seven patients. Despite commonly advanced stage of the underlying disease at the time of HSCT, the relapse rate was low (22%). With a 5-year follow-up, solid organ graft failure occurred in 9 of 31 patients, i.e., in 5/13 (38%) of the renal transplantations, 3/15 (20%) of the liver transplantations, and in one of the three heart transplantations. Five of the nine failures were defined as graft rejection. The median time to graft failure was 1.8 months, with a range of 0 to 131 months. Transplant-related mortality at three months was 25%. Infection was the most common cause of death. The overall survival at five years after allogeneic HSCT was 40% for the entire group, 51% for liver transplant recipients and 42% for renal transplant recipients. There were no significant differences in the outcomes between different types of HSCT donors or grafts, or the conditioning intensity.
Other clinical experience
Numerous case reports have described successful liver, lung, kidney and heart transplantation after HSCT. Similarly, several case reports over the last 20 years have detailed encouraging results of allogeneic HSCT in solid organ transplant recipients. These experiences have been summarized by Chiang and Lazarus [2], Koenecke et al [7], and Basak et al [1].
Holm and coworkers [5, 6] presented a survey from the Nordic countries about lung transplantations carried out for BOS after allogeneic HSCT. Thirteen patients were reported. The indication for the HSCT had been a malignant hematological disease in all but two patients. All had clinical chronic GVHD. The median time from the HSCT to the lung transplantation was 8.2 (range 0.7-16) years. The median age at the lung transplantation was 34 (16-55) years. With a median follow-up time from the lung transplantation of 4.2 years, the survival of the patients was 90% at one year, and 75% at 5 years. Of the two deceased patients, one died with a relapse of underlying disease, and one of infection. These results were compared to the data obtained from the Scandiatransplant registry and did not differ from the general cohort of lung transplant patients. Four patients developed BOS in the transplanted lung; in one case a retransplantation was carried out.
Vogl et al. [9] reported a cohort of seven patients who received lung transplantation for BOS after allogeneic HSCT. In this cohort there was a case fatality rate of 57%, and median survival was 24 months after the lung transplantation. In this cohort the interval between HSCT and lung transplantation was much shorter than in the study of Holm et al. [5], with a median of 18 (6-120) months.
Discussion
Although a considerable number of reports describing SOT following HSCT have been published [2, 7], the number of such transplantations has been small in relation to the frequent problems of organ injury and failure seen in clinical practice. There are apparently many reasons to this, including the often complicated clinical situation, poor general condition of the patient, and possibly a certain resistance of clinicians to consider such treatment approach, but also insufficient information of such transplantations results. The described recent publications show that the outcomes can be quite good. In a survey by Koenecke et al. [7], the 5-year survival of patients receiving a renal transplantation was 100%, with no patient being on dialysis. The 5-year survival for liver transplantation was 71% and that for lung transplantation 63%. These figures are nor markedly different from the outcomes in general SOT populations. It is clear that the patient populations in dual transplantations have been selected, with young patient age, benign diseases somewhat overrepresented, and underlying malignant disease under good control, but the results show that SOT carried out for organ failure after HSCT is a feasible treatment option in carefully selected patients. There is no indication that prolonged immunosuppressive treatment due to the SOT would significantly increase the risk of disease relapse. However, it was noted by Koenecke et al. [7], that in a large proportion of the patients with SOTs following HSCT, they were carried out late, when the risk of relapse is already relatively low.
BOS is a serious and problematic complication of allogeneic HSCT, for which there is no effective treatment. Therefore, good results of lung transplantations for this disorder are encouraging. According to a report by Holm et al. [5], the 5-year OS was 75%, as compared with 63% in the study by Koenecke [7]. In contrast, the results presented by Vogl et al. [9] are showing that the median survival in a group of seven patients was only 24 months, and the case-fatality rate was 57%. As discussed by Holm et al. [6], the timing of lung transplantation comprised the major difference between clinical data in their study and those by Vogl et al., i.e., the median time from HSCT having been 8.2 years in the Holm study versus 18 months in the Vogl study. This difference may reflect, at least in part, the general importance of patient selection: the patients undergoing SOT early after HSCT being more likely to be at a higher risk of failure because of rapidly progressing complications and a poorer general condition due to the recently performed HSCT.
The number of dual transplantations including cardiac transplantation published is small. Chiang and Lazarus [2] have identified only one patient presented. In the survey [7], one such patient was identified from EBMT centers, and three, in the survey by Basak [1]. Therefore, no general conclusions can be drawn on heart transplantations combined with HSCT.
In a HSCT recipient treated with SOT, the immunological conditions may be complicated. The immunosuppressive strategy applied in the two types of transplantations is somewhat different. These factors might affect the risk of solid organ graft rejection. In the survey of Koenecke et al [7], graft rejection was seen in 4/13 cases of renal transplantationsn, leading to kidney failure in two patients. These were treated with a second renal transplantation. In 2/14 liver transplantations, the rejection led to graft failure. In 2/10 lung transplantations rejection resulted in respiratory failure; in one case this was treated with repeated transplantation. Among the patients treated with lung transplantation in the study of Holm et al [6], no rejection causing organ failure took place. Therefore, also given the small numbers of patients, the incidences of graft rejection were not markedly different from those that can be seen in non-HSCT SOT patients. The occurrence or absence of GVHD did not significantly affect the outcome.
The number of reports of HSCT in SOT recipients in the literature is quite limited (1,2). In such HSCTs the function and fate of the solid organ graft would be a concern. As shown in the survey by Basak et al [1], graft failure presents a distinct risk, as it was seen in 9/31 patients. There was a renal graft failure in 38%, liver graft failure in 20% and heart graft failure in 1/3 of the patients. In approximately half of the cases, this was considered a result of rejection. There were no major problems with hematopoietic engraftment: with one exception, engraftment took place in all evaluable patients.
There are many possible mechanisms of graft rejection in this transplant setting. An immune response can be directed against mismatched HLA molecules, because the hematopoietic graft is HLA-matched with the recipient rather than the solid organ. However, recent studies [4] have suggested that allogeneic HSCT can have a tolerogenic effect, allowing maintenance of a solid organ graft without immune suppression. Conditioning prior to allogeneic HSCT and infection may increase the immunogenicity of the organ graft by enhancing antigen presentation, increasing costimulatory signals, changing the properties of the vascular endothelium, and suppressing regulatory T-cell function. Whereas the majority of solid organ grafts are matched with the recipient based on their blood group, this is no require for HSCT donors. Thus, the majority of hematopoietic transplants are probably not matched with the solid organ graft, and this could affect the survival of the organ graft. Moreover, in most patients, the immunosuppressive regimen is changed after allogeneic HSCT from a regimen typical for SOT to an HSCT-specific regimen, which could be suboptimal in this situation.
In summary, SOT can represent a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic HSCT and experience long-term survival without loss of organ function.
Acknowledgements
The authors declare no conflicts of interest.
References
- Basak GW, Wiktor-Jedrzejczak W, Labopin M, Schoemans H, Ljungman P, Kobbe G, Beguin Y, Lang P, Koenecke C, Sykora KW, te Boome L, van Biezen A, van der Werf S, Mohty M, de Witte T, Marsh J, Dreger P, Kröger N, Duarte R, Ruutu T. Allogeneic hematopoietic stem cell transplantation in solid organ transplant recipients: a retrospective, multicenter study of the EBMT. Am J Transplant 2015; 15: 705-14.
- Chiang KY, Lazarus HM. Should we be performing more combined hematopoietic stem cell plus solid organ transplants? Bone Marrow Transplant 2003; 31: 633-42.
- European Transplant Coordinators Organization. International donation and transplantation activity 2012. Available from: http://www.europeantransplantcoordinators.org.
- Fandrich F. Cell therapy approaches aiming at minimization immunosuppression in solid organ transplantation. Curr Opin Organ Transplant 2010; 15: 703-8.
- Holm AM, Riise GC, Hansson L, Brinch L, Bjortuft O, Iversen M, Simonsen S, Floisand Y. Lung transplantation for bronchiolitis obliterans syndrome after allo-SCT. Bone Marrow Transplantation 2013a; 48: 703-7.
- Holm AM, Riise GC, Brinch L, Bjortuft O, Iversen M, Simonsen S, Floisand Y. Lung transplantation for bronchiolitis obliterans after allogeneic hematopoietic stem cell transplantation: unsolved questions. Transplantation 2013b; 96: e21-e22.
- Koenecke C, Hertenstein B, Schetelig J, van Biezen A, Dammann E, Gratwohl A, Ganser A, Schleuning M, Bornhäuser M, Jacobsen N., Kröger N, Niederwieser D, de Witte T, Ruutu T. Solid organ transplantation after allogeneic hematopoietic stem cell transplantation: a retrospective, multicenter study of the EBMT. Am J Transplant 2010; 10: 1897-906.
- Passweg JR, Baldomero H, Bader P, Bonini C, Cesaro S, Dreger P, Duarte RF, Dufour C, Falkenburg JHF, Farge-Bancel D, Gennery A, Kröger N, Lanza F, Nagler A, Sureda A, Mohty M for the European Society for Blood and Marrow Transplantation (EBMT). Hematopoietic SCT in Europe 2013: recent trends in the use of alternative donors showing more haploidentical donors but fewer cord blood transplants. Bone Marrow Transplant advance online publication, February 2, 2015; doi:10.1038/bmt.2014.312
- Vogl UM, Nagayama K, Bojic M, Hoda MAR, Klepetko W, Jaksch P, Dekan S, Siersch V, Mitterbauer M, Schellongowski P, Greinix HT, Petkov V, Schulenburg A, Kalhs P, Rabitsch W. Lung transplantation for bronchiolitis obliterans after allogeneic hematopoietic stem cell transplantation: a single-center experience. Transplantation 2013; 95: 623-28.
Introduction
Solid organ transplantation (SOT) is widely used for the treatment of end-stage organ insufficiency. About 30000 SOTs were performed in the European Union in 2011, comprising approximately 19000 kidney, 7000 liver and 2000 heart and other (including combined) transplants [3]. Allogeneic hematopoietic stem cell transplantation (HSCT) is the only cure or the most effective treatment for a large number of malignant and non-malignant diseases of the lympho-hematopoietic system with an otherwise poor prognosis. At present, the number of allogeneic HSCTs in Europe is approximately 15000 per year [8]. With these large numbers of patients, the likelihood of coincidental occurrence of disorders potentially indicating SOT and HSCT in the same patient is increasing. Such transplantation combinations can be problematic for many reasons.
Allogeneic HSCT is an intensive treatment which causes frequently organ injury and failure, resulting in a potential indication for a SOT. The mechanisms of organ injury include cytotoxic drugs and radiotherapy in the pretransplant conditioning, organ-toxic agents in supportive care, and immunological mechanisms. The organs most often affected are kidney, liver, lung and heart. Factors that may complicate a SOT in this setting are the fragility of the patient as a consequence of the toxicity of HSCT, immunosuppressive treatment for the HSCT which may not be optimal for the SOT, potential immunological problems caused by tissue type differences between the recipient, the hematopoietic graft and the solid organ graft, and infections. In SOT recipients, the long-lasting immunosuppressive medication may affect the function of organs, and increase the risk of infections. SOT can be associated with development of hematological disorders comprising aplastic anemia, post-transplant lymphoproliferative disease, acute myeloid leukemia and myelodysplastic syndromes [1] which may be a potential indication for allogeneic HSCT.
As the clinical situation is often found to be complicated and the risk of treatment failure regarded as high, the numbers of SOTs to HSCT recipients and those of HSCTs to SOT recipients have been low as compared to the number of patients who would have a potential indication for such treatment. Until recent years the literature of such transplantations consisted mainly of case reports as reviewed by Basak et al. [1], Chiang and Lazarus [2], Koenecke et al. [7], with obvious risk of publication bias. As the results of such combined transplantations were not well known, the European Society for Blood and Marrow Transplantation (EBMT) carried out two surveys to collect the experience in Europe and to analyze the outcome. One survey evaluated the experience with SOT in HSCT recipients, the other HSCTs carried out in SOT recipients.
EBMT surveys
In the EBMT survey of SOTs carried out in HSCT recipients by Koenecke et al [7], 107 centers with the total of 67000 allogeneic HSCTs carried out between 1984 and 2007 participated. Among them, 28 centers reported having carried out a total of 45 SOTs in 40 patients for organ failure after HSCT. The transplantations comprised 15 renal, 15 liver, 13 lung grafts, 1 heart, and 1 skin transplantation. In approximately 2/3 of the HSCTs, they were performed for malignant hematological disease (n=28), the other patients had aplastic anemia, or an inherited disorder (n=6 for both). In most cases, the donor had been a sibling, and bone marrow has been transplanted. Almost all patients had received a standard full-intensity conditioning. Twenty-two patients had developed grade II or higher acute GVHD and 23 patients, extensive chronic GVHD before the SOT. This was the cause for SOT in six patients receiving liver transplants, and in 13 patients undergoing lung transplantation. In all other patients, clinically significant GVHD resolved before the SOT. Median age at the time of the renal transplantation was 35 (range 8-64) years, for liver transplantation, 20 (1-56) years, and for lung transplantation, 32 (11-55) years. The median time between HSCT and renal transplantation was 84 (range 8-188) months, that in liver transplantations 34 (range 1-137) months, and in lung transplantations, 69 (range 7-196) months. In renal transplantations following HSCT, the most common cause was drug- or radiation-induced kidney failure. Patients receiving liver transplantation could be divided in two groups, early and late transplantation after HSCT. Early liver transplantation (up to six months post-HSCT) was performed due to acute liver failure caused by veno-occlusive disease (VOD) or acute GVHD, late transplantation (usually, 2-5 years after HSCT) was mostly carried out because of chronic liver-GVHD or cirrhosis. The indication for lung transplantation was bronchiolitis obliterans (BOS)/ chronic GVHD in all these patients. The overall 5-year survival after SOT was 78%, in renal transplantations, 100%, in liver transplantations, 71% and in lung transplantations, 63%. None of the renal transplantation patients was on dialysis at the end of the follow-up. The overall 2-year incidence of SOT failure was 16% (20% in patients with GVHD preceding SOT versus 7% in GVHD-free cases). Graft rejection occurred in approximately 30% of the patients with each type of transplantation, but it could be usually treated. Two patients with renal transplantation, 2 with liver transplantation and 4 with lung transplantation experienced graft failure. The relapse incidence of the underlying malignant disease was 4% at 5 years after the SOT. Six patients received the SOT from the original HSCT donors (4 kidneys, 1 liver, 1 lung transplantation). All of them, except of the lung transplantation patient, were alive at the time of the analysis.
In the course of EBMT survey by Basak et al [1], with 101 centers participating, 18 centers reported a total of 31 HSCTs in 28 SOT recipients. Thirteen of the patients have received a liver transplantation, 12 patients received renal grafts, and three underwent heart transplantation. Malignant hematological disease was the reason for HSCT in 22 of the 28 patients, the most common indications being acute myeloblastic leukemia (AML) in 8 cases, acute lymphoblastic leukemia (ALL) and chronic myeloid leukemia (CML) in 4 cases each. The diagnosis leading to HSCT was known before the SOT in 8/28 patients (AML, ALL, CML, chronic granulomatous disease, primary immunodeficiency, severe aplastic anemia). The patients were young, with median age at the HSCT of 25 (1-62) years. The median time from SOT to HSCT was 37 (1-315) months. The sources of hematopoietic graft were as follows: peripheral blood stem cells in 21, bone marrow in 9, and the both in one patient. The donor was a HLA-identical sibling in 12, a matched unrelated donor in 14, and haploidentical, in 4 cases. Seventeen patients received myeloablative conditioning. In the rest of this group, intensity of the conditioning was reduced. Ex vivo T-cell depletion was carried out in five cases. Successful engraftment was registered in 25/26 evaluable patients. Eight patients developed grade II-IV acute GVHD. Chronic GVHD occurred in seven patients. Despite commonly advanced stage of the underlying disease at the time of HSCT, the relapse rate was low (22%). With a 5-year follow-up, solid organ graft failure occurred in 9 of 31 patients, i.e., in 5/13 (38%) of the renal transplantations, 3/15 (20%) of the liver transplantations, and in one of the three heart transplantations. Five of the nine failures were defined as graft rejection. The median time to graft failure was 1.8 months, with a range of 0 to 131 months. Transplant-related mortality at three months was 25%. Infection was the most common cause of death. The overall survival at five years after allogeneic HSCT was 40% for the entire group, 51% for liver transplant recipients and 42% for renal transplant recipients. There were no significant differences in the outcomes between different types of HSCT donors or grafts, or the conditioning intensity.
Other clinical experience
Numerous case reports have described successful liver, lung, kidney and heart transplantation after HSCT. Similarly, several case reports over the last 20 years have detailed encouraging results of allogeneic HSCT in solid organ transplant recipients. These experiences have been summarized by Chiang and Lazarus [2], Koenecke et al [7], and Basak et al [1].
Holm and coworkers [5, 6] presented a survey from the Nordic countries about lung transplantations carried out for BOS after allogeneic HSCT. Thirteen patients were reported. The indication for the HSCT had been a malignant hematological disease in all but two patients. All had clinical chronic GVHD. The median time from the HSCT to the lung transplantation was 8.2 (range 0.7-16) years. The median age at the lung transplantation was 34 (16-55) years. With a median follow-up time from the lung transplantation of 4.2 years, the survival of the patients was 90% at one year, and 75% at 5 years. Of the two deceased patients, one died with a relapse of underlying disease, and one of infection. These results were compared to the data obtained from the Scandiatransplant registry and did not differ from the general cohort of lung transplant patients. Four patients developed BOS in the transplanted lung; in one case a retransplantation was carried out.
Vogl et al. [9] reported a cohort of seven patients who received lung transplantation for BOS after allogeneic HSCT. In this cohort there was a case fatality rate of 57%, and median survival was 24 months after the lung transplantation. In this cohort the interval between HSCT and lung transplantation was much shorter than in the study of Holm et al. [5], with a median of 18 (6-120) months.
Discussion
Although a considerable number of reports describing SOT following HSCT have been published [2, 7], the number of such transplantations has been small in relation to the frequent problems of organ injury and failure seen in clinical practice. There are apparently many reasons to this, including the often complicated clinical situation, poor general condition of the patient, and possibly a certain resistance of clinicians to consider such treatment approach, but also insufficient information of such transplantations results. The described recent publications show that the outcomes can be quite good. In a survey by Koenecke et al. [7], the 5-year survival of patients receiving a renal transplantation was 100%, with no patient being on dialysis. The 5-year survival for liver transplantation was 71% and that for lung transplantation 63%. These figures are nor markedly different from the outcomes in general SOT populations. It is clear that the patient populations in dual transplantations have been selected, with young patient age, benign diseases somewhat overrepresented, and underlying malignant disease under good control, but the results show that SOT carried out for organ failure after HSCT is a feasible treatment option in carefully selected patients. There is no indication that prolonged immunosuppressive treatment due to the SOT would significantly increase the risk of disease relapse. However, it was noted by Koenecke et al. [7], that in a large proportion of the patients with SOTs following HSCT, they were carried out late, when the risk of relapse is already relatively low.
BOS is a serious and problematic complication of allogeneic HSCT, for which there is no effective treatment. Therefore, good results of lung transplantations for this disorder are encouraging. According to a report by Holm et al. [5], the 5-year OS was 75%, as compared with 63% in the study by Koenecke [7]. In contrast, the results presented by Vogl et al. [9] are showing that the median survival in a group of seven patients was only 24 months, and the case-fatality rate was 57%. As discussed by Holm et al. [6], the timing of lung transplantation comprised the major difference between clinical data in their study and those by Vogl et al., i.e., the median time from HSCT having been 8.2 years in the Holm study versus 18 months in the Vogl study. This difference may reflect, at least in part, the general importance of patient selection: the patients undergoing SOT early after HSCT being more likely to be at a higher risk of failure because of rapidly progressing complications and a poorer general condition due to the recently performed HSCT.
The number of dual transplantations including cardiac transplantation published is small. Chiang and Lazarus [2] have identified only one patient presented. In the survey [7], one such patient was identified from EBMT centers, and three, in the survey by Basak [1]. Therefore, no general conclusions can be drawn on heart transplantations combined with HSCT.
In a HSCT recipient treated with SOT, the immunological conditions may be complicated. The immunosuppressive strategy applied in the two types of transplantations is somewhat different. These factors might affect the risk of solid organ graft rejection. In the survey of Koenecke et al [7], graft rejection was seen in 4/13 cases of renal transplantationsn, leading to kidney failure in two patients. These were treated with a second renal transplantation. In 2/14 liver transplantations, the rejection led to graft failure. In 2/10 lung transplantations rejection resulted in respiratory failure; in one case this was treated with repeated transplantation. Among the patients treated with lung transplantation in the study of Holm et al [6], no rejection causing organ failure took place. Therefore, also given the small numbers of patients, the incidences of graft rejection were not markedly different from those that can be seen in non-HSCT SOT patients. The occurrence or absence of GVHD did not significantly affect the outcome.
The number of reports of HSCT in SOT recipients in the literature is quite limited (1,2). In such HSCTs the function and fate of the solid organ graft would be a concern. As shown in the survey by Basak et al [1], graft failure presents a distinct risk, as it was seen in 9/31 patients. There was a renal graft failure in 38%, liver graft failure in 20% and heart graft failure in 1/3 of the patients. In approximately half of the cases, this was considered a result of rejection. There were no major problems with hematopoietic engraftment: with one exception, engraftment took place in all evaluable patients.
There are many possible mechanisms of graft rejection in this transplant setting. An immune response can be directed against mismatched HLA molecules, because the hematopoietic graft is HLA-matched with the recipient rather than the solid organ. However, recent studies [4] have suggested that allogeneic HSCT can have a tolerogenic effect, allowing maintenance of a solid organ graft without immune suppression. Conditioning prior to allogeneic HSCT and infection may increase the immunogenicity of the organ graft by enhancing antigen presentation, increasing costimulatory signals, changing the properties of the vascular endothelium, and suppressing regulatory T-cell function. Whereas the majority of solid organ grafts are matched with the recipient based on their blood group, this is no require for HSCT donors. Thus, the majority of hematopoietic transplants are probably not matched with the solid organ graft, and this could affect the survival of the organ graft. Moreover, in most patients, the immunosuppressive regimen is changed after allogeneic HSCT from a regimen typical for SOT to an HSCT-specific regimen, which could be suboptimal in this situation.
In summary, SOT can represent a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic HSCT and experience long-term survival without loss of organ function.
Acknowledgements
The authors declare no conflicts of interest.
References
- Basak GW, Wiktor-Jedrzejczak W, Labopin M, Schoemans H, Ljungman P, Kobbe G, Beguin Y, Lang P, Koenecke C, Sykora KW, te Boome L, van Biezen A, van der Werf S, Mohty M, de Witte T, Marsh J, Dreger P, Kröger N, Duarte R, Ruutu T. Allogeneic hematopoietic stem cell transplantation in solid organ transplant recipients: a retrospective, multicenter study of the EBMT. Am J Transplant 2015; 15: 705-14.
- Chiang KY, Lazarus HM. Should we be performing more combined hematopoietic stem cell plus solid organ transplants? Bone Marrow Transplant 2003; 31: 633-42.
- European Transplant Coordinators Organization. International donation and transplantation activity 2012. Available from: http://www.europeantransplantcoordinators.org.
- Fandrich F. Cell therapy approaches aiming at minimization immunosuppression in solid organ transplantation. Curr Opin Organ Transplant 2010; 15: 703-8.
- Holm AM, Riise GC, Hansson L, Brinch L, Bjortuft O, Iversen M, Simonsen S, Floisand Y. Lung transplantation for bronchiolitis obliterans syndrome after allo-SCT. Bone Marrow Transplantation 2013a; 48: 703-7.
- Holm AM, Riise GC, Brinch L, Bjortuft O, Iversen M, Simonsen S, Floisand Y. Lung transplantation for bronchiolitis obliterans after allogeneic hematopoietic stem cell transplantation: unsolved questions. Transplantation 2013b; 96: e21-e22.
- Koenecke C, Hertenstein B, Schetelig J, van Biezen A, Dammann E, Gratwohl A, Ganser A, Schleuning M, Bornhäuser M, Jacobsen N., Kröger N, Niederwieser D, de Witte T, Ruutu T. Solid organ transplantation after allogeneic hematopoietic stem cell transplantation: a retrospective, multicenter study of the EBMT. Am J Transplant 2010; 10: 1897-906.
- Passweg JR, Baldomero H, Bader P, Bonini C, Cesaro S, Dreger P, Duarte RF, Dufour C, Falkenburg JHF, Farge-Bancel D, Gennery A, Kröger N, Lanza F, Nagler A, Sureda A, Mohty M for the European Society for Blood and Marrow Transplantation (EBMT). Hematopoietic SCT in Europe 2013: recent trends in the use of alternative donors showing more haploidentical donors but fewer cord blood transplants. Bone Marrow Transplant advance online publication, February 2, 2015; doi:10.1038/bmt.2014.312
- Vogl UM, Nagayama K, Bojic M, Hoda MAR, Klepetko W, Jaksch P, Dekan S, Siersch V, Mitterbauer M, Schellongowski P, Greinix HT, Petkov V, Schulenburg A, Kalhs P, Rabitsch W. Lung transplantation for bronchiolitis obliterans after allogeneic hematopoietic stem cell transplantation: a single-center experience. Transplantation 2013; 95: 623-28.
Тапани Рууту1, Христиан Кенеке2, Гжегож В. Басак3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "118" ["VALUE"]=> array(2) { ["TEXT"]=> string(860) "<p class="Autor_place_work-Rus"><sup>1</sup>Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;</p> <p class="Autor_place_work-Rus"><sup>2</sup>Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;</p> <p class="Autor_place_work-Rus"><sup>3</sup>Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(758) "1Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;
2Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;
3Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "119" ["VALUE"]=> array(2) { ["TEXT"]=> string(7408) "<h2>Резюме</h2> <p class="Summery_Rus ParaOverride-6" lang="ru-RU">Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО. </p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(7236) "Резюме
Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО.
Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.
У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.
Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.
Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "15" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-14-18" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-14-18" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "120" ["VALUE"]=> array(2) { ["TEXT"]=> string(169) "<p class="Autor">Tapani Ruutu<sup>1</sup>, Christian Koenecke<sup>2</sup> and Grzegorz W. Basak<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(111) "Tapani Ruutu1, Christian Koenecke2 and Grzegorz W. Basak3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "19" ["VALUE"]=> array(2) { ["TEXT"]=> string(434) "<sup>1</sup>Helsinki University Central Hospital, Comprehensive Cancer Center, Stem Cell Transplantation Unit, Helsinki, Finland;<br> <sup>2</sup>Hannover Medical School, Department of Hematology, Hemostasis, Oncology and Stem-Cell Transplantation, Hannover, Germany;<br> <sup>3</sup>The Medical University of Warsaw, Department of Hematology, Oncology and Internal Diseases, Poland" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(386) "1Helsinki University Central Hospital, Comprehensive Cancer Center, Stem Cell Transplantation Unit, Helsinki, Finland;2Hannover Medical School, Department of Hematology, Hemostasis, Oncology and Stem-Cell Transplantation, Hannover, Germany;
3The Medical University of Warsaw, Department of Hematology, Oncology and Internal Diseases, Poland" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "42" ["VALUE"]=> array(2) { ["TEXT"]=> string(1032) "<h2>Summary</h2> <p> The present review is largely based on two surveys on patients who have undergone both an allogeneic hematopoietic stem cell transplantation (HSCT) and a solid organ transplantation (SOT), carried out by the European Society for Blood and Marrow Transplantation (EBMT). Some additional references to the literature are included. From these sources of data it can be summarized that SOT represents a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic SCT and experience long-term survival without loss of organ function. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1008) "
Summary
The present review is largely based on two surveys on patients who have undergone both an allogeneic hematopoietic stem cell transplantation (HSCT) and a solid organ transplantation (SOT), carried out by the European Society for Blood and Marrow Transplantation (EBMT). Some additional references to the literature are included. From these sources of data it can be summarized that SOT represents a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic SCT and experience long-term survival without loss of organ function.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "20" ["VALUE"]=> string(102) "Allogeneic hematopoietic stem cell transplantation and solid organ transplantation in the same patient" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(102) "Allogeneic hematopoietic stem cell transplantation and solid organ transplantation in the same patient" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1193" ["VALUE"]=> string(2) "10" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "10" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1194" ["VALUE"]=> string(2) "11" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "11" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(14) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "120" ["VALUE"]=> array(2) { ["TEXT"]=> string(169) "<p class="Autor">Tapani Ruutu<sup>1</sup>, Christian Koenecke<sup>2</sup> and Grzegorz W. Basak<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(111) "Tapani Ruutu1, Christian Koenecke2 and Grzegorz W. Basak3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(111) "Tapani Ruutu1, Christian Koenecke2 and Grzegorz W. Basak3
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "42" ["VALUE"]=> array(2) { ["TEXT"]=> string(1032) "<h2>Summary</h2> <p> The present review is largely based on two surveys on patients who have undergone both an allogeneic hematopoietic stem cell transplantation (HSCT) and a solid organ transplantation (SOT), carried out by the European Society for Blood and Marrow Transplantation (EBMT). Some additional references to the literature are included. From these sources of data it can be summarized that SOT represents a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic SCT and experience long-term survival without loss of organ function. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1008) "Summary
The present review is largely based on two surveys on patients who have undergone both an allogeneic hematopoietic stem cell transplantation (HSCT) and a solid organ transplantation (SOT), carried out by the European Society for Blood and Marrow Transplantation (EBMT). Some additional references to the literature are included. From these sources of data it can be summarized that SOT represents a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic SCT and experience long-term survival without loss of organ function.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1008) "Summary
The present review is largely based on two surveys on patients who have undergone both an allogeneic hematopoietic stem cell transplantation (HSCT) and a solid organ transplantation (SOT), carried out by the European Society for Blood and Marrow Transplantation (EBMT). Some additional references to the literature are included. From these sources of data it can be summarized that SOT represents a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic SCT and experience long-term survival without loss of organ function.
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "15" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-14-18" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-14-18" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-14-18" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "20" ["VALUE"]=> string(102) "Allogeneic hematopoietic stem cell transplantation and solid organ transplantation in the same patient" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(102) "Allogeneic hematopoietic stem cell transplantation and solid organ transplantation in the same patient" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(102) "Allogeneic hematopoietic stem cell transplantation and solid organ transplantation in the same patient" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "19" ["VALUE"]=> array(2) { ["TEXT"]=> string(434) "<sup>1</sup>Helsinki University Central Hospital, Comprehensive Cancer Center, Stem Cell Transplantation Unit, Helsinki, Finland;<br> <sup>2</sup>Hannover Medical School, Department of Hematology, Hemostasis, Oncology and Stem-Cell Transplantation, Hannover, Germany;<br> <sup>3</sup>The Medical University of Warsaw, Department of Hematology, Oncology and Internal Diseases, Poland" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(386) "1Helsinki University Central Hospital, Comprehensive Cancer Center, Stem Cell Transplantation Unit, Helsinki, Finland;2Hannover Medical School, Department of Hematology, Hemostasis, Oncology and Stem-Cell Transplantation, Hannover, Germany;
3The Medical University of Warsaw, Department of Hematology, Oncology and Internal Diseases, Poland" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(386) "1Helsinki University Central Hospital, Comprehensive Cancer Center, Stem Cell Transplantation Unit, Helsinki, Finland;
2Hannover Medical School, Department of Hematology, Hemostasis, Oncology and Stem-Cell Transplantation, Hannover, Germany;
3The Medical University of Warsaw, Department of Hematology, Oncology and Internal Diseases, Poland" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(3) { [0]=> string(2) "39" [1]=> string(2) "40" [2]=> string(2) "41" } ["VALUE"]=> array(3) { [0]=> string(1) "8" [1]=> string(2) "10" [2]=> string(1) "7" } ["DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(3) { [0]=> string(1) "8" [1]=> string(2) "10" [2]=> string(1) "7" } ["~DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(3) { [0]=> string(59) "Christian Koenecke" [1]=> string(59) "Grzegorz W. Basak" [2]=> string(53) "Tapani Ruutu" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "14" ["VALUE"]=> array(2) { ["TEXT"]=> string(225) "<p class="Autor_Rus" lang="ru-RU">Тапани Рууту<sup>1</sup>, Христиан Кенеке<sup>2</sup>, Гжегож В. Басак<sup>3</sup></p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(157) "
Тапани Рууту1, Христиан Кенеке2, Гжегож В. Басак3
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(157) "Тапани Рууту1, Христиан Кенеке2, Гжегож В. Басак3
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "43" ["VALUE"]=> string(19) "08.03.2015 10:43:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.03.2015 10:43:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.03.2015 10:43:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "44" ["VALUE"]=> string(19) "23.06.2015 10:43:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "23.06.2015 10:43:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "23.06.2015 10:43:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "867" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(5) { [0]=> string(4) "1188" [1]=> string(4) "1189" [2]=> string(4) "1190" [3]=> string(4) "1191" [4]=> string(4) "1192" } ["VALUE"]=> array(5) { [0]=> string(2) "21" [1]=> string(2) "22" [2]=> string(2) "23" [3]=> string(2) "24" [4]=> string(2) "25" } ["DESCRIPTION"]=> array(5) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(5) { [0]=> string(2) "21" [1]=> string(2) "22" [2]=> string(2) "23" [3]=> string(2) "24" [4]=> string(2) "25" } ["~DESCRIPTION"]=> array(5) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(5) { [0]=> string(136) "аллогенная трансплантация гемопоэтических клеток" [1]=> string(82) "трансплантация почек" [2]=> string(84) "трансплантация печени" [3]=> string(84) "трансплантация сердца" [4]=> string(102) "комбинированные трансплантации" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(2) "13" ["VALUE"]=> string(1) "7" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(1) "7" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(53) "Tapani Ruutu" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "119" ["VALUE"]=> array(2) { ["TEXT"]=> string(7408) "<h2>Резюме</h2> <p class="Summery_Rus ParaOverride-6" lang="ru-RU">Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО. </p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(7236) "Резюме
Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО.
Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.
У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.
Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.
Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(7236) "Резюме
Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО.
Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.
У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.
Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.
Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа.
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "118" ["VALUE"]=> array(2) { ["TEXT"]=> string(860) "<p class="Autor_place_work-Rus"><sup>1</sup>Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;</p> <p class="Autor_place_work-Rus"><sup>2</sup>Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;</p> <p class="Autor_place_work-Rus"><sup>3</sup>Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(758) "1Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;
2Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;
3Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(758) "1Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;
2Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;
3Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша
" } } } [6]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "2" ["~IBLOCK_SECTION_ID"]=> string(1) "2" ["ID"]=> string(2) "32" ["~ID"]=> string(2) "32" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(282) "Оценка минимальной остаточной болезни, таргетная терапия и трансплантация стволовых клеток: как их сочетать при остром лимфобластном лейкозе у взрослых" ["~NAME"]=> string(282) "Оценка минимальной остаточной болезни, таргетная терапия и трансплантация стволовых клеток: как их сочетать при остром лимфобластном лейкозе у взрослых" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:42:11" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:42:11" ["DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-19-23/" ["~DETAIL_PAGE_URL"]=> string(65) "/ru/archive/Volume-4/Regular-articles/1866-8836-2015-4-1-2-19-23/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(23718) "Introduction
Progress in adult acute lymphoblastic leukemia (ALL) in recent years is based on new diagnostic procedures, particularly the evaluation of Minimal Residual Disease (MRD), and detection of novel genetic aberrations.
At the therapeutic site the instrumentarium has been extended with targeted therapy; either with tyrosine kinase inhibitors (TKI) in Ph/bcr-abl+ ALL or, more recently, with immunotherapeutic approaches [7].
Minimal Residual Disease
There exist standard methods and definitions of MRD in ALL, in order to detect leukemic blast cells (LBC) not assessable by microscopic examination of bone marrow. Therefore, molecular complete remission (MolCR) is defined as ≤ 0,01% = ≤1 LBC in 10.000 normal cells. The molecular methods include flow cytometry (FC), or molecular biology (nucleic acid-based) approaches. Appropriate sensitivity thresholds are: 10-3-10-4 for FC, and 10-5, for RT PCR (e.g., bcr/abl detection) [4]. Clonal gene rearrangements of immunoglobulin heavy chain (IgH) or T-cell receptor (TCR-β, δ, γ) are as sensitive as 10-4. In sum, the quantitative MDR biomarkers are applicable in >90% of ALL cases.
The best time point for MRD evaluation and MRD-based treatment stratification is shown to be ca. 14-16 weeks after induction/consolidation treatment, according to the most studies. A molecular response by the week 16 after Consolidation I is most informative, with highest molecular CR rates, in order to predict outcomes of CR in standard-risk (Ph-negative) ALL, according to the GMALL Studies (06/99-07/03).
Failure of treatment by molecular criteria identifies now the worst ALL subgroup. In cases of MRD-positivity after induction/consolidation, stem cell transplantation (SCT) is considered as an option which provides sufficient increase in disease-free survival in adult ALL (standard and high risk groups) [1]. Preparation for SCT requires fast donor search, reserving place for potential haplo-, or cord blood SCT. Reduction of MRD load before SCT is quite desirable.
Pre-SCT tumor load reduction:
window studies
Reduction of MRD load before SCT is quite desirable. What approaches should be considered when treating patients positive for MRD before SCT? The so-called window studies with new cytostatic drugs (TKIs or MoABs) are aimed to reduce the tumor load before SCT. These studies allow to explore clinical effects of new drugs, measured quantitatively by MRD levels. One of those window studies was done with Nelarabine (Atriance/ Arranon), a T cell-specific drug, in relapsed/refractory T-ALL/T-LBL [5]. In this study, the CR rate was >40%, but the rate of MRD-negativity was even higher, thus allowing more MRD-negative patients to receive a transplant. Also, TKI as well as immunotherapeutic approaches have been explored in this situation.
Overall, window studies in ALL seem to be the best place for exploring new drugs. According to regulations from authorities, the novel drugs are initially explored in refractory/relapsing ALL, but it seems that some of the new drugs should be preferentially tested in the MRD-positive situation, since they might be more active if a patient has only a smaller tumor load.
The question whether it is useful to reduce the tumor load before SCT arises particularly in Ph+ ALL. It could be demonstrated in several studies that the TKI treatment during induction and consolidation increases the molecular CR rate measured by the quantitative RT-PCR bcr-abl assay to 50-70%, as compared to only 5% with chemotherapy [2]. However, it is not quite clear in Ph/bcr-abl+ ALL whether TKI post-treatment can compensate for MRD positivity before SCT. Nevertheless, in one randomized and several confirmatory studies, it has been convincingly demonstrated that a TKI treatment post-SCT is of benefit, even in patients who are MRD-negative after SCT. The TKI treatment, mostly with Imatinib, but also other TKIs, improved the outcome. Another question concerns duration of the TKI treatment. Different options are suggested for the following therapeutic regimens: (1) until bcr-abl-negativity for 2-3 time points; (2) for 2.5 years as maintenance therapy in B-lineage ALL, or forever (a discussed item).
Ph+ ALL in the era of TKI
Ph+ ALL adult studies have demonstrated a substantial advantage for SCT in CR1 with an overall survival of 60-70%. In one childhood study, intensive chemotherapy + TKI was sufficient to achieve a similar cure rate compared to a cohort with sibling- or unrelated donor transplant [11]. However, it has to be considered that Ph+ ALL in childhood is slightly different from adults, since many more additional cytogenetic aberrations are present in adult Ph+ALL. Some studies in adults, particularly with Dasatinib, currently explore whether a reasonable cure rate can be achieved without SCT. It seems, however, that the fraction of adult Ph+ ALL patients without a SCT is ~30-40%, all the other patients in these studies were later transplanted in cases of becoming bcr-abl-positive, or relapse, or in second CR. Thus, a randomized study is required in adult ALL in order to learn whether SCT is still needed in bcr/abl-negative patients in CR1.
Moreover, there is a newly discovered subtype, BCR-ABL-like ALL. For these cases, either a TKI, or a JAK2 inhibitor is indicated, depending on genetic aberrations [10].
For the newly discovered early T cell precursor (ETP) ALL, there are no new drugs proposed, except of Nelarabine evaluation, and those patients are candidates for allo-SCT in CR1, since they have a poor prognosis.
Immunotherapeutic approaches
in ALL
Several surface antigens, representing the differentiation steps in B-lineage ALL, express antigens which could be targeted by antibodies. The available drugs include monoclonal anti-CD20 antibody (Rituximab), anti-CD22 (Inotuzumab Ozogamicin, IO), the bispecific CD3/CD19-directed antibody (Blinatumomab), or Chimeric Antigen Receptor modified T (CART) cells, directed against CD19 (Table 2).
The results with Rituximab are most convincing in adult Burkitt leukemia/lymphoma, where CD20-expression is >90%. Addition of Rituximab to intensive chemotherapy has resulted in a survival rate of >80% [8]. CD20 is also positive in ~40% of cells in сommon/pre-B ALL . When referring to GMALL study 07/2003, the Rituximab addition (day -1, 375mg/m2 for eight administrations) has further improved the outcomes of standard-risk patients, by about 15%, to ~70%. The reason is a faster and higher MRD-negativity which is translated to increased disease-free survival. The question remains open, if Rituximab addition is also of benefit in high-risk patients, being candidates for a SCT in CR1.
Anti-CD22 antibody has been studied in relapsed/refractory ALL with a good CR rate, whereby a high percentage of those patients achieved a molecular remission [9]. Interestingly, this medication has been also piloted in a small study with elderly patients where the antibody was added to a reduced chemotherapy (Mini-HyperCVAD), yielding promising results. However, the follow-up in this trial was extremely short.
Blinatumomab is a novel bispecific construct that reacts simultaneously with normal CD3 T cells and CD19 ALL cells, creating a tight intercellular connection followed by T cell–mediated cytotoxicity directed against CD19 blast cells (BiTE mechanism). An appropriate Phase 2 study was carried out in pre-B ALL patients being in hematological CR, but with molecular failure or molecular relapse after ≥ 3 cycles of chemotherapy (n=21). The endpoints included a complete molecular response (CMR), time to hematologic relapse, as well as incidence and severity of adverse events [12]. As a result, long-term remissions were achieved in some patients without SCT or any other treatment [13]. Very promising studies were performed with Blinatunomab in refractory/relapsed, or MRD-positive ALL patients. In heavily pre-treated cases, MRD was again chosen as primary endpoint, i.e., conversion from MRD positivity to MRD negativity ≤10-4 is clearly defined and measurable within weeks to months [6].
A novel option represents chimeric antigen receptor-modified T cells (CART), autologous T cells expressing a CD19-specific CD28/CD3ζ, dual-signaling, second-generation chimeric antigen receptor (CAR) termed as 19-28z. The CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory ALL [3].
Conclusions
Evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies.
Targeted therapy with TKIs, either first-generation drug (Imatinib), or second-generation agents (Dasatinib/Nilotinib), has substantially improved the outcome for adult Ph+ ALL patients, eventually, by increased molecular remission rates and substantial improvement of survival to 60-70% after SCT.
Maintenance therapy with TKI is recommended after SCT, whereby its optimal duration is so far not known.
Nearly all Ph+/bcr-abl+ patients relapsing after chemo or SCT have specific mutations of the fusion gene, in particular, T351I. Such pharmaceutical products as the new third-generation TKI, Ponatinib, or other substances have to be explored, aiming to overcome drug resistance caused by such mutations.
Immunotherapeutic approaches offer new treatment options, required especially in adult ALL. Anti-CD20 Rituximab, as well as anti-CD22 Inotuzumab Ozogamicin, have been successfully explored in refractory/relapsed ALL, MRD-positive clinical situations, and also in cases of de novo treatment.
A new approach is to activate the patients’ own T-cells to be directed against the targeted leukemic blast cells. Blinatumomab, a bispecific antibody, has shown its efficiency in MRD-positive patients, refractory/relapsed disease, and in ongoing studies concerning de novo induction/consolidation therapy.
A novel option concerns potential treatment with Chimeric Antigen Receptor (CAR)- modified T cells, where autologous T-cells against CD19-bearing leukemic cells could be generated. The results are promising, although small groups of patients, short follow-up terms, and considerable treatment-associated toxicity still leave many questions open.
|
Surface |
All Subtype |
Expression >20% of LBC |
Monoclonal Antibody |
|
|
Thiel* |
Raponi N 516* |
|||
|
CD20 |
B-precursor |
41% 86% |
22-30% 100% |
Rituximab |
|
CD52 |
B-precursor |
79% 77% |
Alemtuzumab |
|
|
CD22 |
B-precursor |
60-85% 69% |
93-96% 100% |
Epratuzumab Inotuzumab Ozogamicin |
|
CD33 |
B-precursor |
23% 9% 40% |
17-26% |
Gemtuzumab* Ozogamicin |
|
CD19 |
B-precursor |
95% 94% |
100% 100% |
Blinatumomab |
* Data from the German Multicentre Study Group for Adult ALL (GMALL) central Immunophenotyping, E. Thiel, S. Schwartz, Berlin, Germany (personal communication).
** Raponi et al. Leukemia&lymphoma. 2011 52 (6): 1098-17.
Table 1. Expression of surface antigens for potential antibody therapy in ALL
References
- Bassan R, Spinelli O, Oldani E, Intermesoli T, Tosi M, Peruta B, Rossi G, Borlenghi E, Pogliani EM, Terruzzi E, Fabris P, Cassibba V, Lambertenghi-Deliliers G, Cortelezzi A, Bosi A, Gianfaldoni G, Ciceri F, Bernardi M, Gallamini A, Mattei D, Di Bona E, Romani C, Scattolin AM, Barbui T, Rambaldi A. Improved risk classification for risk-specific therapy based on the molecular study of minimal residual disease (MRD) in adult acute lymphoblastic leukemia (ALL). Blood. 2009; 113(18): 4153-62.
- Bassan R, Hoelzer D. Modern therapy of acute lymphoblastic leukemia. J Clin Oncol. 2011; 29(5): 532-43.
- Brentjens RJ, Davila ML, Riviere I, Park J, Wang X, Cowell LG, Bartido S, Stefanski J, Taylor C, Olszewska M, Borquez-Ojeda O, Qu J, Wasielewska T, He Q, Bernal Y, Rijo IV, Hedvat C, Kobos R, Curran K, Steinherz P, Jurcic J, Rosenblat T, Maslak P, Frattini M, Sadelain M. CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Sci Transl Med. 2013; 5(177):177ra38.
- Brüggemann M1, Schrauder A, Raff T, Pfeifer H, Dworzak M, Ottmann OG, Asnafi V, Baruchel A, Bassan R, Benoit Y, Biondi A, Cavé H, Dombret H, Fielding AK, Foà R, Gökbuget N, Goldstone AH, Goulden N, Henze G, Hoelzer D, Janka-Schaub GE, Macintyre EA, Pieters R, Rambaldi A, Ribera JM, Schmiegelow K, Spinelli O, Stary J, von Stackelberg A, Kneba M, Schrappe M, van Dongen JJ; European Working Group for Adult Acute Lymphoblastic Leukemia (EWALL); International Berlin-Frankfurt-Münster Study Group (I-BFM-SG). Standardized MRD quantification in European ALL trials: proceedings of the Second International Symposium on MRD assessment in Kiel, Germany, 18-20 September 2008. Leukemia. 2010; 24(3): 521-35.
- Gökbuget N, Basara N, Baurmann H, Beck J, Brüggemann M, Diedrich H, Güldenzoph B, Hartung G, Horst HA, Hüttmann A, Kobbe G, Naumann R, Ratei R, Reichle A, Serve H, Stelljes M, Viardot A, Wattad M, Hoelzer D. High single-drug activity of nelarabine in relapsed T-lymphoblastic leukemia/lymphoma offers curative option with subsequent stem cell transplantation. Blood. 2011; 118(13): 3504-3511.
- Handgretinger R, Zugmaier G, Henze G, Kreyenberg H, Lang P, von Stackelberg A. Complete remission after blinatumomab-induced donor T-cell activation in three pediatric patients with post-transplant relapsed acute lymphoblastic leukemia. Leukemia. 2011; 25(1): 181-184.
- Hoelzer D, Gökbuget N. Chemoimmunotherapy in acute lymphoblastic leukemia. Blood Rev. 2012; 26(1): 25-32.
- Hoelzer D, Walewski J, Döhner H, Viardot A, Hiddemann W, Spiekermann K, Serve H, Dührsen U, Hüttmann A, Thi el E, Dengler J, Kneba M, Schaich M, Schmidt-Wolf IG, Beck J, Hertenstein B, Reichle A, Domanska-Czyz K, Fietkau R, Horst HA, Rieder H, Schwartz S, Burmeister T, Gökbuget N; German Multicenter Study Group for Adult Acute Lymphoblastic Leukemia. Improved outcome of adult Burkitt lymphoma/leukemia with rituximab and chemotherapy: report of a large prospective multicenter trial. Blood 2014; 124 (26): 3870-9.
- Kantarjian H, Thomas D, Jorgensen J, Jabbour E, Kebriaei P, Rytting M, York S, Ravandi F, Kwari M, Faderl S, Rios MB, Cortes J, Fayad L, Tarnai R, Wang SA, Champlin R, Advani A, O’Brien S. Inotuzumab ozogamicin, an anti-CD22-calecheamicin conjugate, for refractory and relapsed acute lymphocytic leukaemia: a phase 2 study. Lancet Oncol 2012; 13(4): 403-11.
- Roberts KG, Li Y, Payne-Turner D, Harvey RC, Yang YL, Pei D, McCastlain K, Ding L, Lu C, Song G, Ma J, Becksfort J, Rusch M, Chen SC, Easton J, Cheng J, Boggs K, Santiago-Morales N, Iacobucci I, Fulton RS, Wen J, Valentine M, Cheng C, Paugh SW, Devidas M, Chen IM, Reshmi S, Smith A, Hedlund E, Gupta P, Nagahawatte P, Wu G, Chen X, Yergeau D, Vadodaria B, Mulder H, Winick NJ, Larsen EC, Carroll WL, Heerema NA, Carroll AJ, Grayson G, Tasian SK, Moore AS, Keller F, Frei-Jones M, Whitlock JA, Raetz EA, White DL, Hughes TP, Guidry Auvil JM, Smith MA, Marcucci G, Bloomfield CD, Mrózek K, Kohlschmidt J, Stock W, Kornblau SM, Konopleva M, Paietta E, Pui CH, Jeha S, Relling MV, Evans WE, Gerhard DS, Gastier-Foster JM, Mardis E, Wilson RK, Loh ML, Downing JR, Hunger SP, Willman CL, Zhang J, Mullighan CG. Targetable kinase-activating lesions in Ph-like acute lymphoblastic leukemia. N Engl J Med 2014; 371(11): 1005-15.
- Schultz KR, Carroll A, Heerema NA, Bowman WP, Aledo A, Slayton WB, Sather H, Devidas M, Zheng HW, Davies SM, Gaynon PS, Trigg M, Rutledge R, Jorstad D, Winick N, Borowitz MJ, Hunger SP, Carroll WL, Camitta B. Children’s Oncology Group. Long-term follow-up of imatinib in pediatric Philadelphia chromosome-positive acute lymphoblastic leukemia: Children’s Oncology Group study AALL0031. Leukemia 2014; 28(7): 1467-71.
- Topp MS, Kufer P, Gökbuget N, Goebeler M, Klinger M, Neumann S, Horst HA, Raff T, Viardot A, Schmid M, Stelljes M, Schaich M, Degenhard E, Köhne-Volland R, Brüggemann M, Ottmann O, Pfeifer H, Burmeister T, Nagorsen D, Schmidt M, Lutterbuese R, Reinhardt C, Baeuerle PA, Kneba M, Einsele H, Riethmüller G, Hoelzer D, Zugmaier G, Bargou RC. Targeted therapy with the T-cell-engaging antibody blinatumomab of chemotherapy-refractory minimal residual disease in B-lineage acute lymphoblastic leukemia patients results in high response rate and prolonged leukemia-free survival. J Clin Oncol 2011; 29(18): 2493-8.
- Topp MS, Gökbuget N, Zugmaier G, Degenhard E, Goebeler ME, Klinger M, Neumann SA, Horst HA, Raff T, Viardot A, Stelljes M, Schaich M, Köhne-Volland R, Brüggemann M, Ottmann OG, Burmeister T, Baeuerle PA, Nagorsen D, Schmidt M, Einsele H, Riethmüller G, Kneba M, Hoelzer D, Kufer P, Bargou RC. Long-term follow-up of hematologic relapse-free survival in a phase 2 study of blinatumomab in patients with MRD in B-lineage ALL. Blood 2012; 120(26): 5185-7.
Introduction
Progress in adult acute lymphoblastic leukemia (ALL) in recent years is based on new diagnostic procedures, particularly the evaluation of Minimal Residual Disease (MRD), and detection of novel genetic aberrations.
At the therapeutic site the instrumentarium has been extended with targeted therapy; either with tyrosine kinase inhibitors (TKI) in Ph/bcr-abl+ ALL or, more recently, with immunotherapeutic approaches [7].
Minimal Residual Disease
There exist standard methods and definitions of MRD in ALL, in order to detect leukemic blast cells (LBC) not assessable by microscopic examination of bone marrow. Therefore, molecular complete remission (MolCR) is defined as ≤ 0,01% = ≤1 LBC in 10.000 normal cells. The molecular methods include flow cytometry (FC), or molecular biology (nucleic acid-based) approaches. Appropriate sensitivity thresholds are: 10-3-10-4 for FC, and 10-5, for RT PCR (e.g., bcr/abl detection) [4]. Clonal gene rearrangements of immunoglobulin heavy chain (IgH) or T-cell receptor (TCR-β, δ, γ) are as sensitive as 10-4. In sum, the quantitative MDR biomarkers are applicable in >90% of ALL cases.
The best time point for MRD evaluation and MRD-based treatment stratification is shown to be ca. 14-16 weeks after induction/consolidation treatment, according to the most studies. A molecular response by the week 16 after Consolidation I is most informative, with highest molecular CR rates, in order to predict outcomes of CR in standard-risk (Ph-negative) ALL, according to the GMALL Studies (06/99-07/03).
Failure of treatment by molecular criteria identifies now the worst ALL subgroup. In cases of MRD-positivity after induction/consolidation, stem cell transplantation (SCT) is considered as an option which provides sufficient increase in disease-free survival in adult ALL (standard and high risk groups) [1]. Preparation for SCT requires fast donor search, reserving place for potential haplo-, or cord blood SCT. Reduction of MRD load before SCT is quite desirable.
Pre-SCT tumor load reduction:
window studies
Reduction of MRD load before SCT is quite desirable. What approaches should be considered when treating patients positive for MRD before SCT? The so-called window studies with new cytostatic drugs (TKIs or MoABs) are aimed to reduce the tumor load before SCT. These studies allow to explore clinical effects of new drugs, measured quantitatively by MRD levels. One of those window studies was done with Nelarabine (Atriance/ Arranon), a T cell-specific drug, in relapsed/refractory T-ALL/T-LBL [5]. In this study, the CR rate was >40%, but the rate of MRD-negativity was even higher, thus allowing more MRD-negative patients to receive a transplant. Also, TKI as well as immunotherapeutic approaches have been explored in this situation.
Overall, window studies in ALL seem to be the best place for exploring new drugs. According to regulations from authorities, the novel drugs are initially explored in refractory/relapsing ALL, but it seems that some of the new drugs should be preferentially tested in the MRD-positive situation, since they might be more active if a patient has only a smaller tumor load.
The question whether it is useful to reduce the tumor load before SCT arises particularly in Ph+ ALL. It could be demonstrated in several studies that the TKI treatment during induction and consolidation increases the molecular CR rate measured by the quantitative RT-PCR bcr-abl assay to 50-70%, as compared to only 5% with chemotherapy [2]. However, it is not quite clear in Ph/bcr-abl+ ALL whether TKI post-treatment can compensate for MRD positivity before SCT. Nevertheless, in one randomized and several confirmatory studies, it has been convincingly demonstrated that a TKI treatment post-SCT is of benefit, even in patients who are MRD-negative after SCT. The TKI treatment, mostly with Imatinib, but also other TKIs, improved the outcome. Another question concerns duration of the TKI treatment. Different options are suggested for the following therapeutic regimens: (1) until bcr-abl-negativity for 2-3 time points; (2) for 2.5 years as maintenance therapy in B-lineage ALL, or forever (a discussed item).
Ph+ ALL in the era of TKI
Ph+ ALL adult studies have demonstrated a substantial advantage for SCT in CR1 with an overall survival of 60-70%. In one childhood study, intensive chemotherapy + TKI was sufficient to achieve a similar cure rate compared to a cohort with sibling- or unrelated donor transplant [11]. However, it has to be considered that Ph+ ALL in childhood is slightly different from adults, since many more additional cytogenetic aberrations are present in adult Ph+ALL. Some studies in adults, particularly with Dasatinib, currently explore whether a reasonable cure rate can be achieved without SCT. It seems, however, that the fraction of adult Ph+ ALL patients without a SCT is ~30-40%, all the other patients in these studies were later transplanted in cases of becoming bcr-abl-positive, or relapse, or in second CR. Thus, a randomized study is required in adult ALL in order to learn whether SCT is still needed in bcr/abl-negative patients in CR1.
Moreover, there is a newly discovered subtype, BCR-ABL-like ALL. For these cases, either a TKI, or a JAK2 inhibitor is indicated, depending on genetic aberrations [10].
For the newly discovered early T cell precursor (ETP) ALL, there are no new drugs proposed, except of Nelarabine evaluation, and those patients are candidates for allo-SCT in CR1, since they have a poor prognosis.
Immunotherapeutic approaches
in ALL
Several surface antigens, representing the differentiation steps in B-lineage ALL, express antigens which could be targeted by antibodies. The available drugs include monoclonal anti-CD20 antibody (Rituximab), anti-CD22 (Inotuzumab Ozogamicin, IO), the bispecific CD3/CD19-directed antibody (Blinatumomab), or Chimeric Antigen Receptor modified T (CART) cells, directed against CD19 (Table 2).
The results with Rituximab are most convincing in adult Burkitt leukemia/lymphoma, where CD20-expression is >90%. Addition of Rituximab to intensive chemotherapy has resulted in a survival rate of >80% [8]. CD20 is also positive in ~40% of cells in сommon/pre-B ALL . When referring to GMALL study 07/2003, the Rituximab addition (day -1, 375mg/m2 for eight administrations) has further improved the outcomes of standard-risk patients, by about 15%, to ~70%. The reason is a faster and higher MRD-negativity which is translated to increased disease-free survival. The question remains open, if Rituximab addition is also of benefit in high-risk patients, being candidates for a SCT in CR1.
Anti-CD22 antibody has been studied in relapsed/refractory ALL with a good CR rate, whereby a high percentage of those patients achieved a molecular remission [9]. Interestingly, this medication has been also piloted in a small study with elderly patients where the antibody was added to a reduced chemotherapy (Mini-HyperCVAD), yielding promising results. However, the follow-up in this trial was extremely short.
Blinatumomab is a novel bispecific construct that reacts simultaneously with normal CD3 T cells and CD19 ALL cells, creating a tight intercellular connection followed by T cell–mediated cytotoxicity directed against CD19 blast cells (BiTE mechanism). An appropriate Phase 2 study was carried out in pre-B ALL patients being in hematological CR, but with molecular failure or molecular relapse after ≥ 3 cycles of chemotherapy (n=21). The endpoints included a complete molecular response (CMR), time to hematologic relapse, as well as incidence and severity of adverse events [12]. As a result, long-term remissions were achieved in some patients without SCT or any other treatment [13]. Very promising studies were performed with Blinatunomab in refractory/relapsed, or MRD-positive ALL patients. In heavily pre-treated cases, MRD was again chosen as primary endpoint, i.e., conversion from MRD positivity to MRD negativity ≤10-4 is clearly defined and measurable within weeks to months [6].
A novel option represents chimeric antigen receptor-modified T cells (CART), autologous T cells expressing a CD19-specific CD28/CD3ζ, dual-signaling, second-generation chimeric antigen receptor (CAR) termed as 19-28z. The CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory ALL [3].
Conclusions
Evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies.
Targeted therapy with TKIs, either first-generation drug (Imatinib), or second-generation agents (Dasatinib/Nilotinib), has substantially improved the outcome for adult Ph+ ALL patients, eventually, by increased molecular remission rates and substantial improvement of survival to 60-70% after SCT.
Maintenance therapy with TKI is recommended after SCT, whereby its optimal duration is so far not known.
Nearly all Ph+/bcr-abl+ patients relapsing after chemo or SCT have specific mutations of the fusion gene, in particular, T351I. Such pharmaceutical products as the new third-generation TKI, Ponatinib, or other substances have to be explored, aiming to overcome drug resistance caused by such mutations.
Immunotherapeutic approaches offer new treatment options, required especially in adult ALL. Anti-CD20 Rituximab, as well as anti-CD22 Inotuzumab Ozogamicin, have been successfully explored in refractory/relapsed ALL, MRD-positive clinical situations, and also in cases of de novo treatment.
A new approach is to activate the patients’ own T-cells to be directed against the targeted leukemic blast cells. Blinatumomab, a bispecific antibody, has shown its efficiency in MRD-positive patients, refractory/relapsed disease, and in ongoing studies concerning de novo induction/consolidation therapy.
A novel option concerns potential treatment with Chimeric Antigen Receptor (CAR)- modified T cells, where autologous T-cells against CD19-bearing leukemic cells could be generated. The results are promising, although small groups of patients, short follow-up terms, and considerable treatment-associated toxicity still leave many questions open.
|
Surface |
All Subtype |
Expression >20% of LBC |
Monoclonal Antibody |
|
|
Thiel* |
Raponi N 516* |
|||
|
CD20 |
B-precursor |
41% 86% |
22-30% 100% |
Rituximab |
|
CD52 |
B-precursor |
79% 77% |
Alemtuzumab |
|
|
CD22 |
B-precursor |
60-85% 69% |
93-96% 100% |
Epratuzumab Inotuzumab Ozogamicin |
|
CD33 |
B-precursor |
23% 9% 40% |
17-26% |
Gemtuzumab* Ozogamicin |
|
CD19 |
B-precursor |
95% 94% |
100% 100% |
Blinatumomab |
* Data from the German Multicentre Study Group for Adult ALL (GMALL) central Immunophenotyping, E. Thiel, S. Schwartz, Berlin, Germany (personal communication).
** Raponi et al. Leukemia&lymphoma. 2011 52 (6): 1098-17.
Table 1. Expression of surface antigens for potential antibody therapy in ALL
References
- Bassan R, Spinelli O, Oldani E, Intermesoli T, Tosi M, Peruta B, Rossi G, Borlenghi E, Pogliani EM, Terruzzi E, Fabris P, Cassibba V, Lambertenghi-Deliliers G, Cortelezzi A, Bosi A, Gianfaldoni G, Ciceri F, Bernardi M, Gallamini A, Mattei D, Di Bona E, Romani C, Scattolin AM, Barbui T, Rambaldi A. Improved risk classification for risk-specific therapy based on the molecular study of minimal residual disease (MRD) in adult acute lymphoblastic leukemia (ALL). Blood. 2009; 113(18): 4153-62.
- Bassan R, Hoelzer D. Modern therapy of acute lymphoblastic leukemia. J Clin Oncol. 2011; 29(5): 532-43.
- Brentjens RJ, Davila ML, Riviere I, Park J, Wang X, Cowell LG, Bartido S, Stefanski J, Taylor C, Olszewska M, Borquez-Ojeda O, Qu J, Wasielewska T, He Q, Bernal Y, Rijo IV, Hedvat C, Kobos R, Curran K, Steinherz P, Jurcic J, Rosenblat T, Maslak P, Frattini M, Sadelain M. CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Sci Transl Med. 2013; 5(177):177ra38.
- Brüggemann M1, Schrauder A, Raff T, Pfeifer H, Dworzak M, Ottmann OG, Asnafi V, Baruchel A, Bassan R, Benoit Y, Biondi A, Cavé H, Dombret H, Fielding AK, Foà R, Gökbuget N, Goldstone AH, Goulden N, Henze G, Hoelzer D, Janka-Schaub GE, Macintyre EA, Pieters R, Rambaldi A, Ribera JM, Schmiegelow K, Spinelli O, Stary J, von Stackelberg A, Kneba M, Schrappe M, van Dongen JJ; European Working Group for Adult Acute Lymphoblastic Leukemia (EWALL); International Berlin-Frankfurt-Münster Study Group (I-BFM-SG). Standardized MRD quantification in European ALL trials: proceedings of the Second International Symposium on MRD assessment in Kiel, Germany, 18-20 September 2008. Leukemia. 2010; 24(3): 521-35.
- Gökbuget N, Basara N, Baurmann H, Beck J, Brüggemann M, Diedrich H, Güldenzoph B, Hartung G, Horst HA, Hüttmann A, Kobbe G, Naumann R, Ratei R, Reichle A, Serve H, Stelljes M, Viardot A, Wattad M, Hoelzer D. High single-drug activity of nelarabine in relapsed T-lymphoblastic leukemia/lymphoma offers curative option with subsequent stem cell transplantation. Blood. 2011; 118(13): 3504-3511.
- Handgretinger R, Zugmaier G, Henze G, Kreyenberg H, Lang P, von Stackelberg A. Complete remission after blinatumomab-induced donor T-cell activation in three pediatric patients with post-transplant relapsed acute lymphoblastic leukemia. Leukemia. 2011; 25(1): 181-184.
- Hoelzer D, Gökbuget N. Chemoimmunotherapy in acute lymphoblastic leukemia. Blood Rev. 2012; 26(1): 25-32.
- Hoelzer D, Walewski J, Döhner H, Viardot A, Hiddemann W, Spiekermann K, Serve H, Dührsen U, Hüttmann A, Thi el E, Dengler J, Kneba M, Schaich M, Schmidt-Wolf IG, Beck J, Hertenstein B, Reichle A, Domanska-Czyz K, Fietkau R, Horst HA, Rieder H, Schwartz S, Burmeister T, Gökbuget N; German Multicenter Study Group for Adult Acute Lymphoblastic Leukemia. Improved outcome of adult Burkitt lymphoma/leukemia with rituximab and chemotherapy: report of a large prospective multicenter trial. Blood 2014; 124 (26): 3870-9.
- Kantarjian H, Thomas D, Jorgensen J, Jabbour E, Kebriaei P, Rytting M, York S, Ravandi F, Kwari M, Faderl S, Rios MB, Cortes J, Fayad L, Tarnai R, Wang SA, Champlin R, Advani A, O’Brien S. Inotuzumab ozogamicin, an anti-CD22-calecheamicin conjugate, for refractory and relapsed acute lymphocytic leukaemia: a phase 2 study. Lancet Oncol 2012; 13(4): 403-11.
- Roberts KG, Li Y, Payne-Turner D, Harvey RC, Yang YL, Pei D, McCastlain K, Ding L, Lu C, Song G, Ma J, Becksfort J, Rusch M, Chen SC, Easton J, Cheng J, Boggs K, Santiago-Morales N, Iacobucci I, Fulton RS, Wen J, Valentine M, Cheng C, Paugh SW, Devidas M, Chen IM, Reshmi S, Smith A, Hedlund E, Gupta P, Nagahawatte P, Wu G, Chen X, Yergeau D, Vadodaria B, Mulder H, Winick NJ, Larsen EC, Carroll WL, Heerema NA, Carroll AJ, Grayson G, Tasian SK, Moore AS, Keller F, Frei-Jones M, Whitlock JA, Raetz EA, White DL, Hughes TP, Guidry Auvil JM, Smith MA, Marcucci G, Bloomfield CD, Mrózek K, Kohlschmidt J, Stock W, Kornblau SM, Konopleva M, Paietta E, Pui CH, Jeha S, Relling MV, Evans WE, Gerhard DS, Gastier-Foster JM, Mardis E, Wilson RK, Loh ML, Downing JR, Hunger SP, Willman CL, Zhang J, Mullighan CG. Targetable kinase-activating lesions in Ph-like acute lymphoblastic leukemia. N Engl J Med 2014; 371(11): 1005-15.
- Schultz KR, Carroll A, Heerema NA, Bowman WP, Aledo A, Slayton WB, Sather H, Devidas M, Zheng HW, Davies SM, Gaynon PS, Trigg M, Rutledge R, Jorstad D, Winick N, Borowitz MJ, Hunger SP, Carroll WL, Camitta B. Children’s Oncology Group. Long-term follow-up of imatinib in pediatric Philadelphia chromosome-positive acute lymphoblastic leukemia: Children’s Oncology Group study AALL0031. Leukemia 2014; 28(7): 1467-71.
- Topp MS, Kufer P, Gökbuget N, Goebeler M, Klinger M, Neumann S, Horst HA, Raff T, Viardot A, Schmid M, Stelljes M, Schaich M, Degenhard E, Köhne-Volland R, Brüggemann M, Ottmann O, Pfeifer H, Burmeister T, Nagorsen D, Schmidt M, Lutterbuese R, Reinhardt C, Baeuerle PA, Kneba M, Einsele H, Riethmüller G, Hoelzer D, Zugmaier G, Bargou RC. Targeted therapy with the T-cell-engaging antibody blinatumomab of chemotherapy-refractory minimal residual disease in B-lineage acute lymphoblastic leukemia patients results in high response rate and prolonged leukemia-free survival. J Clin Oncol 2011; 29(18): 2493-8.
- Topp MS, Gökbuget N, Zugmaier G, Degenhard E, Goebeler ME, Klinger M, Neumann SA, Horst HA, Raff T, Viardot A, Stelljes M, Schaich M, Köhne-Volland R, Brüggemann M, Ottmann OG, Burmeister T, Baeuerle PA, Nagorsen D, Schmidt M, Einsele H, Riethmüller G, Kneba M, Hoelzer D, Kufer P, Bargou RC. Long-term follow-up of hematologic relapse-free survival in a phase 2 study of blinatumomab in patients with MRD in B-lineage ALL. Blood 2012; 120(26): 5185-7.
Дитер Хельцер
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "146" ["VALUE"]=> array(2) { ["TEXT"]=> string(152) "<p class="Autor_place_work-Rus">Университет Й.-В. Гете, Франкфурт-на Майне, Германия </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(130) "Университет Й.-В. Гете, Франкфурт-на Майне, Германия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "147" ["VALUE"]=> array(2) { ["TEXT"]=> string(3222) "<p class="Summery_Rus" lang="ru-RU">Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка. </p> <p class="Summery_Rus" lang="ru-RU">Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена. </p> " ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3158) "Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка.
Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "148" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-19-23" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-19-23" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "149" ["VALUE"]=> array(2) { ["TEXT"]=> string(58) "<p class="Autor">Dieter Hoelzer </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(36) "Dieter Hoelzer
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "150" ["VALUE"]=> array(2) { ["TEXT"]=> string(89) "<p class="Autor_place_work">J. W. Goethe University, Frankfurt </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(67) "J. W. Goethe University, Frankfurt
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "151" ["VALUE"]=> array(2) { ["TEXT"]=> string(1776) "<h2>Summery</h2> <p class="Summery"> There exist standard molecular methods of minimal residual disease (MRD) evaluation in acute lymphoblastic leukemia (ALL), in order to detect leukemic blast cells (LBC) not assessable by microscopy of bone marrow. The best time point for MRD evaluation and MRD-based treatment stratification in ALL is shown to be ca.14-16 weeks after induction/ consolidation treatment. Reduction of MRD load before SCT, as a next step of therapy, is quite desirable. E.g., induction and consolidation treatment with tyrosine kinase inhibitors (NKI) increase the molecular CR rate compared to conventional chemotherapy, as measured by the quantitative RT-PCR assays of bcr/abl fusion oncogene. Failure of treatment by molecular criteria identifies the worst ALL subgroup. Several window studies in ALL with new cytostatic drugs (TKIs or MoABs) were aimed to reduce the tumor load before SCT. Moreover, novel immunotherapeutic approaches include application of monoclonal antibodies against specific surface antigens typical to certain differentiation steps in B-lineage. </p> <p class="Summery"> Hence, evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies. Targeted therapy with TKI has improved the outcome for adult Ph+ ALL patients substantially, evidently by an increased molecular remission rate, and a substantial improvement of survival after SCT. Meanwhile, maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. Maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1720) "Summery
There exist standard molecular methods of minimal residual disease (MRD) evaluation in acute lymphoblastic leukemia (ALL), in order to detect leukemic blast cells (LBC) not assessable by microscopy of bone marrow. The best time point for MRD evaluation and MRD-based treatment stratification in ALL is shown to be ca.14-16 weeks after induction/ consolidation treatment. Reduction of MRD load before SCT, as a next step of therapy, is quite desirable. E.g., induction and consolidation treatment with tyrosine kinase inhibitors (NKI) increase the molecular CR rate compared to conventional chemotherapy, as measured by the quantitative RT-PCR assays of bcr/abl fusion oncogene. Failure of treatment by molecular criteria identifies the worst ALL subgroup. Several window studies in ALL with new cytostatic drugs (TKIs or MoABs) were aimed to reduce the tumor load before SCT. Moreover, novel immunotherapeutic approaches include application of monoclonal antibodies against specific surface antigens typical to certain differentiation steps in B-lineage.
Hence, evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies. Targeted therapy with TKI has improved the outcome for adult Ph+ ALL patients substantially, evidently by an increased molecular remission rate, and a substantial improvement of survival after SCT. Meanwhile, maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. Maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "152" ["VALUE"]=> string(91) "MRD evaluation, targeted therapy and stem cell transplantation: how to combine in adult ALL" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(91) "MRD evaluation, targeted therapy and stem cell transplantation: how to combine in adult ALL" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1201" ["VALUE"]=> string(2) "12" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "12" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1202" ["VALUE"]=> string(2) "13" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "13" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(14) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "149" ["VALUE"]=> array(2) { ["TEXT"]=> string(58) "<p class="Autor">Dieter Hoelzer </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(36) "Dieter Hoelzer
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(36) "Dieter Hoelzer
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "151" ["VALUE"]=> array(2) { ["TEXT"]=> string(1776) "<h2>Summery</h2> <p class="Summery"> There exist standard molecular methods of minimal residual disease (MRD) evaluation in acute lymphoblastic leukemia (ALL), in order to detect leukemic blast cells (LBC) not assessable by microscopy of bone marrow. The best time point for MRD evaluation and MRD-based treatment stratification in ALL is shown to be ca.14-16 weeks after induction/ consolidation treatment. Reduction of MRD load before SCT, as a next step of therapy, is quite desirable. E.g., induction and consolidation treatment with tyrosine kinase inhibitors (NKI) increase the molecular CR rate compared to conventional chemotherapy, as measured by the quantitative RT-PCR assays of bcr/abl fusion oncogene. Failure of treatment by molecular criteria identifies the worst ALL subgroup. Several window studies in ALL with new cytostatic drugs (TKIs or MoABs) were aimed to reduce the tumor load before SCT. Moreover, novel immunotherapeutic approaches include application of monoclonal antibodies against specific surface antigens typical to certain differentiation steps in B-lineage. </p> <p class="Summery"> Hence, evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies. Targeted therapy with TKI has improved the outcome for adult Ph+ ALL patients substantially, evidently by an increased molecular remission rate, and a substantial improvement of survival after SCT. Meanwhile, maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. Maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1720) "Summery
There exist standard molecular methods of minimal residual disease (MRD) evaluation in acute lymphoblastic leukemia (ALL), in order to detect leukemic blast cells (LBC) not assessable by microscopy of bone marrow. The best time point for MRD evaluation and MRD-based treatment stratification in ALL is shown to be ca.14-16 weeks after induction/ consolidation treatment. Reduction of MRD load before SCT, as a next step of therapy, is quite desirable. E.g., induction and consolidation treatment with tyrosine kinase inhibitors (NKI) increase the molecular CR rate compared to conventional chemotherapy, as measured by the quantitative RT-PCR assays of bcr/abl fusion oncogene. Failure of treatment by molecular criteria identifies the worst ALL subgroup. Several window studies in ALL with new cytostatic drugs (TKIs or MoABs) were aimed to reduce the tumor load before SCT. Moreover, novel immunotherapeutic approaches include application of monoclonal antibodies against specific surface antigens typical to certain differentiation steps in B-lineage.
Hence, evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies. Targeted therapy with TKI has improved the outcome for adult Ph+ ALL patients substantially, evidently by an increased molecular remission rate, and a substantial improvement of survival after SCT. Meanwhile, maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. Maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1720) "Summery
There exist standard molecular methods of minimal residual disease (MRD) evaluation in acute lymphoblastic leukemia (ALL), in order to detect leukemic blast cells (LBC) not assessable by microscopy of bone marrow. The best time point for MRD evaluation and MRD-based treatment stratification in ALL is shown to be ca.14-16 weeks after induction/ consolidation treatment. Reduction of MRD load before SCT, as a next step of therapy, is quite desirable. E.g., induction and consolidation treatment with tyrosine kinase inhibitors (NKI) increase the molecular CR rate compared to conventional chemotherapy, as measured by the quantitative RT-PCR assays of bcr/abl fusion oncogene. Failure of treatment by molecular criteria identifies the worst ALL subgroup. Several window studies in ALL with new cytostatic drugs (TKIs or MoABs) were aimed to reduce the tumor load before SCT. Moreover, novel immunotherapeutic approaches include application of monoclonal antibodies against specific surface antigens typical to certain differentiation steps in B-lineage.
Hence, evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies. Targeted therapy with TKI has improved the outcome for adult Ph+ ALL patients substantially, evidently by an increased molecular remission rate, and a substantial improvement of survival after SCT. Meanwhile, maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. Maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known.
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "148" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-19-23" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-19-23" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-19-23" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "152" ["VALUE"]=> string(91) "MRD evaluation, targeted therapy and stem cell transplantation: how to combine in adult ALL" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(91) "MRD evaluation, targeted therapy and stem cell transplantation: how to combine in adult ALL" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(91) "MRD evaluation, targeted therapy and stem cell transplantation: how to combine in adult ALL" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "150" ["VALUE"]=> array(2) { ["TEXT"]=> string(89) "<p class="Autor_place_work">J. W. Goethe University, Frankfurt </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(67) "J. W. Goethe University, Frankfurt
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(67) "J. W. Goethe University, Frankfurt
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(3) "144" } ["VALUE"]=> array(1) { [0]=> string(2) "26" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(2) "26" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Dieter Hoelzer" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "145" ["VALUE"]=> array(2) { ["TEXT"]=> string(95) "<p class="Autor_Rus" lang="ru-RU">Дитер Хельцер</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(63) "Дитер Хельцер
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(63) "Дитер Хельцер
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "141" ["VALUE"]=> string(19) "13.04.2015 10:43:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "13.04.2015 10:43:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "13.04.2015 10:43:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "142" ["VALUE"]=> string(19) "05.06.2015 10:43:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "05.06.2015 10:43:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "05.06.2015 10:43:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "879" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(6) { [0]=> string(4) "1195" [1]=> string(4) "1196" [2]=> string(4) "1197" [3]=> string(4) "1198" [4]=> string(4) "1199" [5]=> string(4) "1200" } ["VALUE"]=> array(6) { [0]=> string(2) "27" [1]=> string(2) "28" [2]=> string(2) "29" [3]=> string(2) "30" [4]=> string(2) "31" [5]=> string(2) "18" } ["DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(6) { [0]=> string(2) "27" [1]=> string(2) "28" [2]=> string(2) "29" [3]=> string(2) "30" [4]=> string(2) "31" [5]=> string(2) "18" } ["~DESCRIPTION"]=> array(6) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(6) { [0]=> string(95) "острый лимфобластный лейкоз" [1]=> string(101) "минимальная остаточная болезнь" [2]=> string(88) "ингибиторы тирозинкиназ" [3]=> string(88) "моноклональные антитела" [4]=> string(84) "молекулярная ремиссия" [5]=> string(78) "клинические исходы" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "143" ["VALUE"]=> string(2) "26" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "26" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Dieter Hoelzer" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "147" ["VALUE"]=> array(2) { ["TEXT"]=> string(3222) "<p class="Summery_Rus" lang="ru-RU">Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка. </p> <p class="Summery_Rus" lang="ru-RU">Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена. </p> " ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3158) "Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка.
Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(3158) "Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка.
Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена.
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "146" ["VALUE"]=> array(2) { ["TEXT"]=> string(152) "<p class="Autor_place_work-Rus">Университет Й.-В. Гете, Франкфурт-на Майне, Германия </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(130) "Университет Й.-В. Гете, Франкфурт-на Майне, Германия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(130) "Университет Й.-В. Гете, Франкфурт-на Майне, Германия
" } } } [7]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "3" ["~IBLOCK_SECTION_ID"]=> string(1) "3" ["ID"]=> string(3) "101" ["~ID"]=> string(3) "101" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(191) "От хряща к раковым опухолям: трансляционные исследования в норвежском Центре изучения стволовых клеток" ["~NAME"]=> string(191) "От хряща к раковым опухолям: трансляционные исследования в норвежском Центре изучения стволовых клеток" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:48:59" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:48:59" ["DETAIL_PAGE_URL"]=> string(62) "/ru/archive/Volume-4/short-reports/1866-8836-2015-4-1-2-66-68/" ["~DETAIL_PAGE_URL"]=> string(62) "/ru/archive/Volume-4/short-reports/1866-8836-2015-4-1-2-66-68/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(10862) "The report presents research activities at the Norwegian Center for Stem Cell Research located at Oslo University Hospital and the Institute of Basic Medical Sciences, University of Oslo. The Center´s research focuses on hiPS cell production, differentiation, characterization and genetic modification (TALEN and CRISPR/CAS approaches), the role of epigenetics and DNA repair in stem cell differentiation, as well as neural imaging and functional assessment (including neuro-optogenetics). The University of Oslo Medical Faculty is establishing bilateral agreements with research and teaching institutions in St. Petersburg.
Repair of hyaline cartilage is among the current priorities in experimental and clinical research at the Center, in projects headed by group leader Jan Brinchmann. In vitro expanded chondrocytes are used for hyaline cartilage replacement, but they typically give rise to fibrous cartilage. The Brinchmann lab has implicated several factors relevant to in vitro chondrogenesis of human mesenchymal stem cells, as shown by high throughput mRNA profiling (Brinchmann et al., 2012) and is now collaborating with group leader Judith Staerk to use TALEN/CRISPR technology for targeted genetic manipulation. The CRISPR/Cas system can be used to direct Cas9 to specific genomic regions where it introduces DNA double-strand breaks. The regulatory system involves a non-coding guide RNA (gRNA), tracrRNA and the Cas9 protein. Staerk´s group has used this system to develop human iPS/ES cells with fluorescent reporters in the Brachyury, Flk1, CD34 and CD45 genetic loci, and is employing these in in vitro models of myelodysplastic syndrome, including genetic modifications introduced into hematopoietic stem cells. The Staerk group is also differentiating hES cells into blood cell precursors, and is also working on the expansion and maintenance of umbilical cord blood CD34+ cells.
The search for physiologically relevant tissue models includes the development of 3D cell culture systems representing new technological platforms for in vitro tissue engineering. Group leaders Gareth Sullivan and Joel Glover are applying 3D cell printing technology to develop multicellular assemblies of liver and neural tissue. Such 3D cellular systems applied to human stem cells and their derivatives can be utilized to investigate various heritable disorders affecting hepatocytes, neurons, cardiomyocytes etc.
In the field of oncology, the Center´s efforts are currently focused on dendritic cell-based vaccine for glioblastoma, in a clinical project led by group leader Iver Langmoen together with group leaders Gunnar Kvalheim and Brinchmann.Therapeutic vaccination against autologous cancer stem cells has been used for decades. However, one may expect better efficiency of such treatment using gliioblastoma mRNA-transfected dendritic cells from glioblastoma patients. A Phase I/II trial of vaccine therapy with hTERT, survivin and glioblastoma stem cell-derived mRNA-transfected dendritic cells has been conducted. Among positive effects of such therapy are decreased tumor size and increased median progression-free survival time (PFS), which was 19.9 months (in patients treated with transfected dendritic cells) treatment) versus 7.9 (with standard treatment).
The Center maintains two GMP cell production facilities for the establishment of autologous cell cultures and mRNA amplification, enabling GMP clinical production of human stem cells and their differentiated progeny performed under highly controlled conditions corresponding to EU Directives and Regulations.
Translational stem cell research has been defined as an area of national priority in Norway, leading to the establishment of the Center by an initiative from the Ministry of Health. The Center also maintains the National Core Facility for Production, Maintenance and Characterization of Human Pluripotent Stem Cells, the only such facility in Norway. This facility began using iPS cell technology in 2012 and its services are available to Norwegian and foreign researchers.
References
- Herlofsen SR, Bryne JC, Høiby T, Wang L, Issner R, Zhang X, Coyne MJ, Boyle P, Gu H, Meza-Zepeda LA, Collas P, Mikkelsen TS, Brinchmann JE. Genome-wide map of quantified epigenetic changes during in vitro chondrogenic differentiation of primary human mesenchymal stem cells. BMC Genomics. 2013 Feb 15;14:105. doi: 10.1186/1471-2164-14-105.
- Vik-Mo EO, Nyakas M, Mikkelsen BV, Moe MC, Due-Tønnesen P, Suso EM, Sæbøe-Larssen S, Sandberg C, Brinchmann JE, Helseth E, Rasmussen AM, Lote K, Aamdal S, Gaudernack G, Kvalheim G, Langmoen IA. Therapeutic vaccination against autologous cancer stem cells with mRNA-transfected dendritic cells in patients with glioblastoma. Cancer Immunol Immunother. 2013 Sep; 62(9):1499-1509.
The report presents research activities at the Norwegian Center for Stem Cell Research located at Oslo University Hospital and the Institute of Basic Medical Sciences, University of Oslo. The Center´s research focuses on hiPS cell production, differentiation, characterization and genetic modification (TALEN and CRISPR/CAS approaches), the role of epigenetics and DNA repair in stem cell differentiation, as well as neural imaging and functional assessment (including neuro-optogenetics). The University of Oslo Medical Faculty is establishing bilateral agreements with research and teaching institutions in St. Petersburg.
Repair of hyaline cartilage is among the current priorities in experimental and clinical research at the Center, in projects headed by group leader Jan Brinchmann. In vitro expanded chondrocytes are used for hyaline cartilage replacement, but they typically give rise to fibrous cartilage. The Brinchmann lab has implicated several factors relevant to in vitro chondrogenesis of human mesenchymal stem cells, as shown by high throughput mRNA profiling (Brinchmann et al., 2012) and is now collaborating with group leader Judith Staerk to use TALEN/CRISPR technology for targeted genetic manipulation. The CRISPR/Cas system can be used to direct Cas9 to specific genomic regions where it introduces DNA double-strand breaks. The regulatory system involves a non-coding guide RNA (gRNA), tracrRNA and the Cas9 protein. Staerk´s group has used this system to develop human iPS/ES cells with fluorescent reporters in the Brachyury, Flk1, CD34 and CD45 genetic loci, and is employing these in in vitro models of myelodysplastic syndrome, including genetic modifications introduced into hematopoietic stem cells. The Staerk group is also differentiating hES cells into blood cell precursors, and is also working on the expansion and maintenance of umbilical cord blood CD34+ cells.
The search for physiologically relevant tissue models includes the development of 3D cell culture systems representing new technological platforms for in vitro tissue engineering. Group leaders Gareth Sullivan and Joel Glover are applying 3D cell printing technology to develop multicellular assemblies of liver and neural tissue. Such 3D cellular systems applied to human stem cells and their derivatives can be utilized to investigate various heritable disorders affecting hepatocytes, neurons, cardiomyocytes etc.
In the field of oncology, the Center´s efforts are currently focused on dendritic cell-based vaccine for glioblastoma, in a clinical project led by group leader Iver Langmoen together with group leaders Gunnar Kvalheim and Brinchmann.Therapeutic vaccination against autologous cancer stem cells has been used for decades. However, one may expect better efficiency of such treatment using gliioblastoma mRNA-transfected dendritic cells from glioblastoma patients. A Phase I/II trial of vaccine therapy with hTERT, survivin and glioblastoma stem cell-derived mRNA-transfected dendritic cells has been conducted. Among positive effects of such therapy are decreased tumor size and increased median progression-free survival time (PFS), which was 19.9 months (in patients treated with transfected dendritic cells) treatment) versus 7.9 (with standard treatment).
The Center maintains two GMP cell production facilities for the establishment of autologous cell cultures and mRNA amplification, enabling GMP clinical production of human stem cells and their differentiated progeny performed under highly controlled conditions corresponding to EU Directives and Regulations.
Translational stem cell research has been defined as an area of national priority in Norway, leading to the establishment of the Center by an initiative from the Ministry of Health. The Center also maintains the National Core Facility for Production, Maintenance and Characterization of Human Pluripotent Stem Cells, the only such facility in Norway. This facility began using iPS cell technology in 2012 and its services are available to Norwegian and foreign researchers.
References
- Herlofsen SR, Bryne JC, Høiby T, Wang L, Issner R, Zhang X, Coyne MJ, Boyle P, Gu H, Meza-Zepeda LA, Collas P, Mikkelsen TS, Brinchmann JE. Genome-wide map of quantified epigenetic changes during in vitro chondrogenic differentiation of primary human mesenchymal stem cells. BMC Genomics. 2013 Feb 15;14:105. doi: 10.1186/1471-2164-14-105.
- Vik-Mo EO, Nyakas M, Mikkelsen BV, Moe MC, Due-Tønnesen P, Suso EM, Sæbøe-Larssen S, Sandberg C, Brinchmann JE, Helseth E, Rasmussen AM, Lote K, Aamdal S, Gaudernack G, Kvalheim G, Langmoen IA. Therapeutic vaccination against autologous cancer stem cells with mRNA-transfected dendritic cells in patients with glioblastoma. Cancer Immunol Immunother. 2013 Sep; 62(9):1499-1509.
Джоэл Гловер
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "565" ["VALUE"]=> array(2) { ["TEXT"]=> string(238) "<span class="CharOverride-18" lang="en-GB">Институт фундаментальных медицинских наук, Медицинский факультет Университета Осло</span>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(206) "Институт фундаментальных медицинских наук, Медицинский факультет Университета Осло" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "566" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-66-68" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-66-68" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "567" ["VALUE"]=> array(2) { ["TEXT"]=> string(57) "<p class="Autor">Joel C. Glover</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(35) "Joel C. Glover
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "568" ["VALUE"]=> array(2) { ["TEXT"]=> string(129) "<p class="Autor_place_work">Institute of Basic Medical Sciences, The University of Oslo Medical Faculty</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(107) "Institute of Basic Medical Sciences, The University of Oslo Medical Faculty
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "569" ["VALUE"]=> string(95) "From cartilage to cancer: Translational research at the Norwegian Center for Stem Cell Research" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(95) "From cartilage to cancer: Translational research at the Norwegian Center for Stem Cell Research" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> &array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1011" ["VALUE"]=> array(2) { ["TEXT"]=> string(8123) "<p> Доклад представляет исследовательскую деятельность Норвежского центра изучения стволовых клеток, расположенного в Университетском госпитале Осло и Институте фундаментальных медицинских наук университета Осло. Работы Центра сосредоточены на продукции индуцированных полипотентных клеток, их дифференцировке, характеризации и генной модификации (методики TALEN и CRISPR/CAS), роли эпигенетики и репарации ДНК в дифференцировке стволовых клеток, а также в нейровизуализации и функциональной оценке, включая нейро-оптогенетику. Медицинский факультет Университета Осло заключает двусторонние соглашения с исследовательскими и учебными организациями Санкт-Петербурга. </p> <p> Репарация гиалинового хряща сейчас является одной из основных задач экспериментальных и клинических исследований Центра в рамках проектов (руководитель – Ян Бринчманн). Размноженные <em>in vitro</em> хондроциты используются для замещения гиалинового хряща, но обычно они развиваются в фиброзный хрящ. Лаборатория Бринчманна выявила несколько факторов, относящихся к хондрогенезу мезенхимных стволовых клеток человека <em>in vitro</em>, что было показано с помощью высокоразрешающего типирования мРНК (Brinchmann et al., 2012). В настоящее время идет сотрудничество с руководителем группы Джудит Стерк по применению технологий TALEN/CRISPR для направленных генетических манипуляций. Система CRISPR/Cas может использоваться для адресации Cas9 в конкретные области генома, где она осуществляет двунитевые разрезы ДНК. Регулирующая система включает в себя некодирующую «ведущую» РНК (gRNA), tracrRNA и белок Cas9. Группа Стерк применила эту систему для разработки человеческих полипотентных стволовых клеток (iPS/ES) с флуоресцентными маркерами в генных локусах Brachyury, Flk1, CD34 и CD45 и внедрила их в моделях <em>in vitro</em> миелодиспластического синдрома, включая генные модификации гемопоэтических стволовых клеток. Группа Стерк также осуществляет дифференцировку эмбриональных клеток человека в кроветворные предшественники, а также работает по экспансии и поддержании культур CD34+ клеток пуповинной крови. </p> <p> Поиск физиологически адекватных моделей тканей включает и разработку трехмерных систем клеточных культур, являющихся новыми технологическими платформами для тканевой инженерии <em>in vitro</em>. Руководители групп Гаррет Салливэн и Джоэл Гловер применяют трехмерную принтерную технологию для создания многоклеточных структур печеночной и нервной ткани. Такие трехмерные клеточные системы в аспекте стволовых клеток человека и их производных могут быть использованы для изучения различных наследственных заболеваний, поражающих гепатоциты, нейроны, кардиомиоциты и т.д. </p> <p> В области онкологии, усилия Центра в настоящее время сконцентрированы на дендритоклеточной вакцине для лечения глиобластомы в клиническом проекте, руководимом Ивером Лангменом, совместно с руководителями групп Гуннаром Квалхеймом и Бринчманном. Терапевтическая вакцинация против аутологичных стволовых раковых клеток применяется уже десятилетиями. Однако можно ожидать лучшей эффективности такого лечения, используя дендритные клетки, трансфицированные мРНК из клеток глиобластомы от пациентов. Проведена фаза I/II испытаний вакцинотерапии с применением дендритных клеток, трансфицированных мРНК hTERT, сурвивина из клеток глиобластомы. Среди позитивных эффектов такой терапии - уменьшение размера опухоли и увеличение средней выживаемости без прогрессии заболевания (19,9 мес. у больных леченных вакциной из дендритных клеток) по сравнению с 7,9 мес. при стандартном лечении. </p> <p> Центр имеет два блока для производства клеток по стандартам GMP в целях культивирования аутологичных клеток и амплификации мРНК, обеспечивающих производство человеческих стволовых клеток и их дифференцированных производных в условиях строгого контроля, согласно директивам и правилам Европейского Союза. </p> <p> Трансляционные исследования стволовых клеток определены среди национальных приоритетов в Норвегии, что ведет к обустройству Центра по инициативе Министерства здравоохранении. Центр также поддерживает Национальную лабораторию по производству, хранению и оценке плюрипотентных стволовых клеток человека – единственную подобную структуру в Норвегии. Это учреждение стало применять технологию индуцируемых плюрипотентных стволовых клеток (iPS) в 2012 г., и его услуги доступны норвежским и зарубежным исследователям. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(8003) "Доклад представляет исследовательскую деятельность Норвежского центра изучения стволовых клеток, расположенного в Университетском госпитале Осло и Институте фундаментальных медицинских наук университета Осло. Работы Центра сосредоточены на продукции индуцированных полипотентных клеток, их дифференцировке, характеризации и генной модификации (методики TALEN и CRISPR/CAS), роли эпигенетики и репарации ДНК в дифференцировке стволовых клеток, а также в нейровизуализации и функциональной оценке, включая нейро-оптогенетику. Медицинский факультет Университета Осло заключает двусторонние соглашения с исследовательскими и учебными организациями Санкт-Петербурга.
Репарация гиалинового хряща сейчас является одной из основных задач экспериментальных и клинических исследований Центра в рамках проектов (руководитель – Ян Бринчманн). Размноженные in vitro хондроциты используются для замещения гиалинового хряща, но обычно они развиваются в фиброзный хрящ. Лаборатория Бринчманна выявила несколько факторов, относящихся к хондрогенезу мезенхимных стволовых клеток человека in vitro, что было показано с помощью высокоразрешающего типирования мРНК (Brinchmann et al., 2012). В настоящее время идет сотрудничество с руководителем группы Джудит Стерк по применению технологий TALEN/CRISPR для направленных генетических манипуляций. Система CRISPR/Cas может использоваться для адресации Cas9 в конкретные области генома, где она осуществляет двунитевые разрезы ДНК. Регулирующая система включает в себя некодирующую «ведущую» РНК (gRNA), tracrRNA и белок Cas9. Группа Стерк применила эту систему для разработки человеческих полипотентных стволовых клеток (iPS/ES) с флуоресцентными маркерами в генных локусах Brachyury, Flk1, CD34 и CD45 и внедрила их в моделях in vitro миелодиспластического синдрома, включая генные модификации гемопоэтических стволовых клеток. Группа Стерк также осуществляет дифференцировку эмбриональных клеток человека в кроветворные предшественники, а также работает по экспансии и поддержании культур CD34+ клеток пуповинной крови.
Поиск физиологически адекватных моделей тканей включает и разработку трехмерных систем клеточных культур, являющихся новыми технологическими платформами для тканевой инженерии in vitro. Руководители групп Гаррет Салливэн и Джоэл Гловер применяют трехмерную принтерную технологию для создания многоклеточных структур печеночной и нервной ткани. Такие трехмерные клеточные системы в аспекте стволовых клеток человека и их производных могут быть использованы для изучения различных наследственных заболеваний, поражающих гепатоциты, нейроны, кардиомиоциты и т.д.
В области онкологии, усилия Центра в настоящее время сконцентрированы на дендритоклеточной вакцине для лечения глиобластомы в клиническом проекте, руководимом Ивером Лангменом, совместно с руководителями групп Гуннаром Квалхеймом и Бринчманном. Терапевтическая вакцинация против аутологичных стволовых раковых клеток применяется уже десятилетиями. Однако можно ожидать лучшей эффективности такого лечения, используя дендритные клетки, трансфицированные мРНК из клеток глиобластомы от пациентов. Проведена фаза I/II испытаний вакцинотерапии с применением дендритных клеток, трансфицированных мРНК hTERT, сурвивина из клеток глиобластомы. Среди позитивных эффектов такой терапии - уменьшение размера опухоли и увеличение средней выживаемости без прогрессии заболевания (19,9 мес. у больных леченных вакциной из дендритных клеток) по сравнению с 7,9 мес. при стандартном лечении.
Центр имеет два блока для производства клеток по стандартам GMP в целях культивирования аутологичных клеток и амплификации мРНК, обеспечивающих производство человеческих стволовых клеток и их дифференцированных производных в условиях строгого контроля, согласно директивам и правилам Европейского Союза.
Трансляционные исследования стволовых клеток определены среди национальных приоритетов в Норвегии, что ведет к обустройству Центра по инициативе Министерства здравоохранении. Центр также поддерживает Национальную лабораторию по производству, хранению и оценке плюрипотентных стволовых клеток человека – единственную подобную структуру в Норвегии. Это учреждение стало применять технологию индуцируемых плюрипотентных стволовых клеток (iPS) в 2012 г., и его услуги доступны норвежским и зарубежным исследователям.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1250" ["VALUE"]=> string(2) "26" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "26" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1251" ["VALUE"]=> string(2) "27" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "27" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(13) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "567" ["VALUE"]=> array(2) { ["TEXT"]=> string(57) "<p class="Autor">Joel C. Glover</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(35) "Joel C. Glover
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(35) "Joel C. Glover
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "566" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-66-68" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-66-68" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-66-68" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "569" ["VALUE"]=> string(95) "From cartilage to cancer: Translational research at the Norwegian Center for Stem Cell Research" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(95) "From cartilage to cancer: Translational research at the Norwegian Center for Stem Cell Research" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(95) "From cartilage to cancer: Translational research at the Norwegian Center for Stem Cell Research" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "568" ["VALUE"]=> array(2) { ["TEXT"]=> string(129) "<p class="Autor_place_work">Institute of Basic Medical Sciences, The University of Oslo Medical Faculty</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(107) "Institute of Basic Medical Sciences, The University of Oslo Medical Faculty
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(107) "Institute of Basic Medical Sciences, The University of Oslo Medical Faculty
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(3) "563" } ["VALUE"]=> array(1) { [0]=> string(2) "97" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(2) "97" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Joel C. Glover" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "564" ["VALUE"]=> array(2) { ["TEXT"]=> string(93) "<p class="Autor_Rus" lang="ru-RU">Джоэл Гловер</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(61) "Джоэл Гловер
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(61) "Джоэл Гловер
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "560" ["VALUE"]=> string(19) "06.04.2015 17:19:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "06.04.2015 17:19:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "06.04.2015 17:19:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "561" ["VALUE"]=> string(19) "05.06.2015 17:20:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "05.06.2015 17:20:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "05.06.2015 17:20:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "906" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(3) { [0]=> string(4) "1247" [1]=> string(4) "1248" [2]=> string(4) "1249" } ["VALUE"]=> array(3) { [0]=> string(2) "98" [1]=> string(2) "99" [2]=> string(3) "100" } ["DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(3) { [0]=> string(2) "98" [1]=> string(2) "99" [2]=> string(3) "100" } ["~DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(3) { [0]=> string(74) "стволовые клетки" [1]=> string(63) "хондроциты" [2]=> string(75) "генная инженерия" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "562" ["VALUE"]=> string(2) "97" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "97" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Joel C. Glover" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "565" ["VALUE"]=> array(2) { ["TEXT"]=> string(238) "<span class="CharOverride-18" lang="en-GB">Институт фундаментальных медицинских наук, Медицинский факультет Университета Осло</span>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(206) "Институт фундаментальных медицинских наук, Медицинский факультет Университета Осло" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(206) "Институт фундаментальных медицинских наук, Медицинский факультет Университета Осло" } ["FULL_TEXT_RU"]=> array(37) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1011" ["VALUE"]=> array(2) { ["TEXT"]=> string(8123) "<p> Доклад представляет исследовательскую деятельность Норвежского центра изучения стволовых клеток, расположенного в Университетском госпитале Осло и Институте фундаментальных медицинских наук университета Осло. Работы Центра сосредоточены на продукции индуцированных полипотентных клеток, их дифференцировке, характеризации и генной модификации (методики TALEN и CRISPR/CAS), роли эпигенетики и репарации ДНК в дифференцировке стволовых клеток, а также в нейровизуализации и функциональной оценке, включая нейро-оптогенетику. Медицинский факультет Университета Осло заключает двусторонние соглашения с исследовательскими и учебными организациями Санкт-Петербурга. </p> <p> Репарация гиалинового хряща сейчас является одной из основных задач экспериментальных и клинических исследований Центра в рамках проектов (руководитель – Ян Бринчманн). Размноженные <em>in vitro</em> хондроциты используются для замещения гиалинового хряща, но обычно они развиваются в фиброзный хрящ. Лаборатория Бринчманна выявила несколько факторов, относящихся к хондрогенезу мезенхимных стволовых клеток человека <em>in vitro</em>, что было показано с помощью высокоразрешающего типирования мРНК (Brinchmann et al., 2012). В настоящее время идет сотрудничество с руководителем группы Джудит Стерк по применению технологий TALEN/CRISPR для направленных генетических манипуляций. Система CRISPR/Cas может использоваться для адресации Cas9 в конкретные области генома, где она осуществляет двунитевые разрезы ДНК. Регулирующая система включает в себя некодирующую «ведущую» РНК (gRNA), tracrRNA и белок Cas9. Группа Стерк применила эту систему для разработки человеческих полипотентных стволовых клеток (iPS/ES) с флуоресцентными маркерами в генных локусах Brachyury, Flk1, CD34 и CD45 и внедрила их в моделях <em>in vitro</em> миелодиспластического синдрома, включая генные модификации гемопоэтических стволовых клеток. Группа Стерк также осуществляет дифференцировку эмбриональных клеток человека в кроветворные предшественники, а также работает по экспансии и поддержании культур CD34+ клеток пуповинной крови. </p> <p> Поиск физиологически адекватных моделей тканей включает и разработку трехмерных систем клеточных культур, являющихся новыми технологическими платформами для тканевой инженерии <em>in vitro</em>. Руководители групп Гаррет Салливэн и Джоэл Гловер применяют трехмерную принтерную технологию для создания многоклеточных структур печеночной и нервной ткани. Такие трехмерные клеточные системы в аспекте стволовых клеток человека и их производных могут быть использованы для изучения различных наследственных заболеваний, поражающих гепатоциты, нейроны, кардиомиоциты и т.д. </p> <p> В области онкологии, усилия Центра в настоящее время сконцентрированы на дендритоклеточной вакцине для лечения глиобластомы в клиническом проекте, руководимом Ивером Лангменом, совместно с руководителями групп Гуннаром Квалхеймом и Бринчманном. Терапевтическая вакцинация против аутологичных стволовых раковых клеток применяется уже десятилетиями. Однако можно ожидать лучшей эффективности такого лечения, используя дендритные клетки, трансфицированные мРНК из клеток глиобластомы от пациентов. Проведена фаза I/II испытаний вакцинотерапии с применением дендритных клеток, трансфицированных мРНК hTERT, сурвивина из клеток глиобластомы. Среди позитивных эффектов такой терапии - уменьшение размера опухоли и увеличение средней выживаемости без прогрессии заболевания (19,9 мес. у больных леченных вакциной из дендритных клеток) по сравнению с 7,9 мес. при стандартном лечении. </p> <p> Центр имеет два блока для производства клеток по стандартам GMP в целях культивирования аутологичных клеток и амплификации мРНК, обеспечивающих производство человеческих стволовых клеток и их дифференцированных производных в условиях строгого контроля, согласно директивам и правилам Европейского Союза. </p> <p> Трансляционные исследования стволовых клеток определены среди национальных приоритетов в Норвегии, что ведет к обустройству Центра по инициативе Министерства здравоохранении. Центр также поддерживает Национальную лабораторию по производству, хранению и оценке плюрипотентных стволовых клеток человека – единственную подобную структуру в Норвегии. Это учреждение стало применять технологию индуцируемых плюрипотентных стволовых клеток (iPS) в 2012 г., и его услуги доступны норвежским и зарубежным исследователям. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(8003) "Доклад представляет исследовательскую деятельность Норвежского центра изучения стволовых клеток, расположенного в Университетском госпитале Осло и Институте фундаментальных медицинских наук университета Осло. Работы Центра сосредоточены на продукции индуцированных полипотентных клеток, их дифференцировке, характеризации и генной модификации (методики TALEN и CRISPR/CAS), роли эпигенетики и репарации ДНК в дифференцировке стволовых клеток, а также в нейровизуализации и функциональной оценке, включая нейро-оптогенетику. Медицинский факультет Университета Осло заключает двусторонние соглашения с исследовательскими и учебными организациями Санкт-Петербурга.
Репарация гиалинового хряща сейчас является одной из основных задач экспериментальных и клинических исследований Центра в рамках проектов (руководитель – Ян Бринчманн). Размноженные in vitro хондроциты используются для замещения гиалинового хряща, но обычно они развиваются в фиброзный хрящ. Лаборатория Бринчманна выявила несколько факторов, относящихся к хондрогенезу мезенхимных стволовых клеток человека in vitro, что было показано с помощью высокоразрешающего типирования мРНК (Brinchmann et al., 2012). В настоящее время идет сотрудничество с руководителем группы Джудит Стерк по применению технологий TALEN/CRISPR для направленных генетических манипуляций. Система CRISPR/Cas может использоваться для адресации Cas9 в конкретные области генома, где она осуществляет двунитевые разрезы ДНК. Регулирующая система включает в себя некодирующую «ведущую» РНК (gRNA), tracrRNA и белок Cas9. Группа Стерк применила эту систему для разработки человеческих полипотентных стволовых клеток (iPS/ES) с флуоресцентными маркерами в генных локусах Brachyury, Flk1, CD34 и CD45 и внедрила их в моделях in vitro миелодиспластического синдрома, включая генные модификации гемопоэтических стволовых клеток. Группа Стерк также осуществляет дифференцировку эмбриональных клеток человека в кроветворные предшественники, а также работает по экспансии и поддержании культур CD34+ клеток пуповинной крови.
Поиск физиологически адекватных моделей тканей включает и разработку трехмерных систем клеточных культур, являющихся новыми технологическими платформами для тканевой инженерии in vitro. Руководители групп Гаррет Салливэн и Джоэл Гловер применяют трехмерную принтерную технологию для создания многоклеточных структур печеночной и нервной ткани. Такие трехмерные клеточные системы в аспекте стволовых клеток человека и их производных могут быть использованы для изучения различных наследственных заболеваний, поражающих гепатоциты, нейроны, кардиомиоциты и т.д.
В области онкологии, усилия Центра в настоящее время сконцентрированы на дендритоклеточной вакцине для лечения глиобластомы в клиническом проекте, руководимом Ивером Лангменом, совместно с руководителями групп Гуннаром Квалхеймом и Бринчманном. Терапевтическая вакцинация против аутологичных стволовых раковых клеток применяется уже десятилетиями. Однако можно ожидать лучшей эффективности такого лечения, используя дендритные клетки, трансфицированные мРНК из клеток глиобластомы от пациентов. Проведена фаза I/II испытаний вакцинотерапии с применением дендритных клеток, трансфицированных мРНК hTERT, сурвивина из клеток глиобластомы. Среди позитивных эффектов такой терапии - уменьшение размера опухоли и увеличение средней выживаемости без прогрессии заболевания (19,9 мес. у больных леченных вакциной из дендритных клеток) по сравнению с 7,9 мес. при стандартном лечении.
Центр имеет два блока для производства клеток по стандартам GMP в целях культивирования аутологичных клеток и амплификации мРНК, обеспечивающих производство человеческих стволовых клеток и их дифференцированных производных в условиях строгого контроля, согласно директивам и правилам Европейского Союза.
Трансляционные исследования стволовых клеток определены среди национальных приоритетов в Норвегии, что ведет к обустройству Центра по инициативе Министерства здравоохранении. Центр также поддерживает Национальную лабораторию по производству, хранению и оценке плюрипотентных стволовых клеток человека – единственную подобную структуру в Норвегии. Это учреждение стало применять технологию индуцируемых плюрипотентных стволовых клеток (iPS) в 2012 г., и его услуги доступны норвежским и зарубежным исследователям.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(8003) "Доклад представляет исследовательскую деятельность Норвежского центра изучения стволовых клеток, расположенного в Университетском госпитале Осло и Институте фундаментальных медицинских наук университета Осло. Работы Центра сосредоточены на продукции индуцированных полипотентных клеток, их дифференцировке, характеризации и генной модификации (методики TALEN и CRISPR/CAS), роли эпигенетики и репарации ДНК в дифференцировке стволовых клеток, а также в нейровизуализации и функциональной оценке, включая нейро-оптогенетику. Медицинский факультет Университета Осло заключает двусторонние соглашения с исследовательскими и учебными организациями Санкт-Петербурга.
Репарация гиалинового хряща сейчас является одной из основных задач экспериментальных и клинических исследований Центра в рамках проектов (руководитель – Ян Бринчманн). Размноженные in vitro хондроциты используются для замещения гиалинового хряща, но обычно они развиваются в фиброзный хрящ. Лаборатория Бринчманна выявила несколько факторов, относящихся к хондрогенезу мезенхимных стволовых клеток человека in vitro, что было показано с помощью высокоразрешающего типирования мРНК (Brinchmann et al., 2012). В настоящее время идет сотрудничество с руководителем группы Джудит Стерк по применению технологий TALEN/CRISPR для направленных генетических манипуляций. Система CRISPR/Cas может использоваться для адресации Cas9 в конкретные области генома, где она осуществляет двунитевые разрезы ДНК. Регулирующая система включает в себя некодирующую «ведущую» РНК (gRNA), tracrRNA и белок Cas9. Группа Стерк применила эту систему для разработки человеческих полипотентных стволовых клеток (iPS/ES) с флуоресцентными маркерами в генных локусах Brachyury, Flk1, CD34 и CD45 и внедрила их в моделях in vitro миелодиспластического синдрома, включая генные модификации гемопоэтических стволовых клеток. Группа Стерк также осуществляет дифференцировку эмбриональных клеток человека в кроветворные предшественники, а также работает по экспансии и поддержании культур CD34+ клеток пуповинной крови.
Поиск физиологически адекватных моделей тканей включает и разработку трехмерных систем клеточных культур, являющихся новыми технологическими платформами для тканевой инженерии in vitro. Руководители групп Гаррет Салливэн и Джоэл Гловер применяют трехмерную принтерную технологию для создания многоклеточных структур печеночной и нервной ткани. Такие трехмерные клеточные системы в аспекте стволовых клеток человека и их производных могут быть использованы для изучения различных наследственных заболеваний, поражающих гепатоциты, нейроны, кардиомиоциты и т.д.
В области онкологии, усилия Центра в настоящее время сконцентрированы на дендритоклеточной вакцине для лечения глиобластомы в клиническом проекте, руководимом Ивером Лангменом, совместно с руководителями групп Гуннаром Квалхеймом и Бринчманном. Терапевтическая вакцинация против аутологичных стволовых раковых клеток применяется уже десятилетиями. Однако можно ожидать лучшей эффективности такого лечения, используя дендритные клетки, трансфицированные мРНК из клеток глиобластомы от пациентов. Проведена фаза I/II испытаний вакцинотерапии с применением дендритных клеток, трансфицированных мРНК hTERT, сурвивина из клеток глиобластомы. Среди позитивных эффектов такой терапии - уменьшение размера опухоли и увеличение средней выживаемости без прогрессии заболевания (19,9 мес. у больных леченных вакциной из дендритных клеток) по сравнению с 7,9 мес. при стандартном лечении.
Центр имеет два блока для производства клеток по стандартам GMP в целях культивирования аутологичных клеток и амплификации мРНК, обеспечивающих производство человеческих стволовых клеток и их дифференцированных производных в условиях строгого контроля, согласно директивам и правилам Европейского Союза.
Трансляционные исследования стволовых клеток определены среди национальных приоритетов в Норвегии, что ведет к обустройству Центра по инициативе Министерства здравоохранении. Центр также поддерживает Национальную лабораторию по производству, хранению и оценке плюрипотентных стволовых клеток человека – единственную подобную структуру в Норвегии. Это учреждение стало применять технологию индуцируемых плюрипотентных стволовых клеток (iPS) в 2012 г., и его услуги доступны норвежским и зарубежным исследователям.
" } } } [8]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "3" ["~IBLOCK_SECTION_ID"]=> string(1) "3" ["ID"]=> string(2) "92" ["~ID"]=> string(2) "92" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(226) "Терапия бластного криза при хроническом миелоидном лейкозе (ХМЛ) и роль трансплантации стволовых кроветворных клеток (ТСК)" ["~NAME"]=> string(226) "Терапия бластного криза при хроническом миелоидном лейкозе (ХМЛ) и роль трансплантации стволовых кроветворных клеток (ТСК)" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:46:26" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:46:26" ["DETAIL_PAGE_URL"]=> string(62) "/ru/archive/Volume-4/short-reports/1866-8836-2015-4-1-2-58-61/" ["~DETAIL_PAGE_URL"]=> string(62) "/ru/archive/Volume-4/short-reports/1866-8836-2015-4-1-2-58-61/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(9547) "Progression of chronic myeloid leukemia to blast crisis (CML BC) is still a phenomenon that is only incompletely understood. In up to 90% of BC patients, additional chromosomal aberrations (ACA) are reported. In up to 77% mutations are detected by means of deep genome sequencing. In gene expression profiles blast crisis appears as a disease distinct from CML. Treatment continues to be mostly unsuccessful unless allo SCT is offered. Treatment failure indicates point of no return. Additional chromosomal aberrations (ACA) are associated with CML blast crisis, being non-random in chromosomal distribution. Major route ACA are +8 (34%), +Ph (30%), i(17q) (20%), +19 (13%), +21 (7%), +17 (5%), monosomy 7 (5%). Temporal order of secondary changes varies, preferred pathway i(17q), +8, +Ph, +19.
There exist certain diagnostic criteria for CML acceleration phase (CML AP) and BC. I.e., AP is characterized by 15 – 29% blasts in blood or marrow (WHO criteria, 10 – 19%); > 20% basophils in blood; persistent thrombocytopenia unrelated to therapy; unresponsiveness to therapy. The blast crisis is registered by >30% blasts in blood or marrow (WHO, 20%); extramedullary blastic infiltrates; varying degrees of fever, anemia, splenomegaly, leukocytosis. Different means of blast crisis prevention are considered while analyzing the studies of 1983 to 2013. Special attention is drawn to tyrosine kinase inhibitors (TKIs, imatinib, nilotinib, dasatinib) in blast crisis. Introduction of imatinib led to a small increase of patient survival (up to 20% ). Most long term survivors are those that have been transplanted (28/39, ca. 72%). European Leukemia Net (ELN) presented analysis of allo-HSCT results in CML blast crisis.
Several approaches are considered. I.e., HSCT should be always used as a second-line treatment in blast phase, irrespective of the response to TKIs. It is recommended “always” in accelerated phase, if the response to TKI is less than optimal, and, as third-line therapy, if the response to second-line TKI is less than optimal. The value and the meaning of “Always” depend on transplant risk (age, comorbidities, performance status, donor, etc.).
Induction of 2nd chronic phase (CP), or remission with TKI alone or in combination with intensive chemotherapy was studied at various regimens by several study groups, i.e.: IM 800 mg + VCR + Dexa (DIV), Rea et al., 2006 (LBC) (n = 13) IM + mitoxantrone / etoposide + AraC (Frühauf et al., 2007), (MBC) ( n= 16) IM + Dauno-AraC (Deau et al., 2011)(n = 36) Dasatinib + FLAG-IDA (Milojkovic et al., 2012), (n = 4) SCT with HLA identical related or matched unrelated donor was performed at EBMT score of 0 to 4, and standard conditioning. Maintenance TKI treatment conditions after SCT have been studied by several groups (Hehlmann et al., Blood, 2012; Rea et al., 2006; Frühauf et al., Cancer 2007; Deau et al., 2011; Milojkovic et al., 2012). Application of AlloHSCT as a 2nd line therapy was studied by CML Study IV (84 patients). HSCT after imatinib failure in 1st CP was accompanied by a 94% survival rate, whereas HSCT performed in advanced phase of CML yielded a 3-year survival of 59% (Saußele et al., 2010). Similar results were published by Oyekunle et al. (2013).
Experience with blast crisis treatment was summarized for CML Study IV (n=1551 patients). The main regimen was imatinib 400 mg + AraC or intensive chemotherapy. A special assessment of CML study IV concerned the survival rates after allo-HSCT in blast crisis dependent on pretreatment, but patient numbers were too small for firm conclusions.
Comparisons were made for myeloid vs. lymphoid BC. Treatment of lymphoid type BC was associated somewhat longer median survival than myeloid-type BC. Further data analysis is in progress. Investigational trials in this field are underway (Table 1).
|
Biological effects |
Drugs/compounds |
|
PP2A activation |
Fingolimod (FTY720) |
|
SET antagonist OP449 |
|
|
CIP2A inhibitor |
|
|
Self renewal of LSC |
BCL6 + TK inhibitors |
|
HIF1α inhibitor |
|
|
Smoothened inhibitors (in combination with TKI) |
|
|
Jak2 inhibitor (in combination with TKI) |
|
|
Activation of apoptosis |
BCL2-inhibitor ABT-737 |
|
Triptolide |
|
|
Dual-kinase inhibitor ON044580 |
|
|
MEK inhibitor PD184352 + farnesyltransferase inhibitor BMS-214662 |
|
|
Others |
Peg-IFN, HDAC inhibitors, Hsp90 inhibitors |
Abbreviations, TKI: tyrosine kinase inhibitor; PP2A: protein phosphatase 2A; LSC: leukemia stem cells; MEK: mitogen-activated protein kinase; HIF: hypoxia induced factor; HDAC: histone deacetylase; Hsp: heat shock protein.
Table 1. Investigational approaches in CML blast crisis
References
- Deau B, Nicolini FE, Guilhot J, Huguet F, Guerci A, Legros L, Pautas C, Berthou C, Guyotat D, Cony-Makhoul P, Gardembas M, Michallet M, Hayette S, Cayuela JM, Weiss IR, Réa D, Castaigne S, Mahon FX, Guilhot F, Rousselot P. The addition of daunorubicin to imatinib mesylate in combination with cytarabine improves the response rate and the survival of patients with myeloid blast crisis chronic myelogenous leukemia (AFR01 study). Leuk Res. 2011; 35(6):777-82.
- Fruehauf S, Topaly J, Buss EC, Fischer T, Ottmann OG, Emmerich B, Müller MC, Schuld P, Balleisen L, Hehlmann R, Ho AD, Hochhaus A. Imatinib combined with mitoxantrone/etoposide and cytarabine is an effective induction therapy for patients with chronic myeloid leukemia in myeloid blast crisis. Cancer. 2007; 109(8):1543
- Hehlmann R. How I treat CML blast crisis. Blood. 2012; 120(4): 737‐747.
Progression of chronic myeloid leukemia to blast crisis (CML BC) is still a phenomenon that is only incompletely understood. In up to 90% of BC patients, additional chromosomal aberrations (ACA) are reported. In up to 77% mutations are detected by means of deep genome sequencing. In gene expression profiles blast crisis appears as a disease distinct from CML. Treatment continues to be mostly unsuccessful unless allo SCT is offered. Treatment failure indicates point of no return. Additional chromosomal aberrations (ACA) are associated with CML blast crisis, being non-random in chromosomal distribution. Major route ACA are +8 (34%), +Ph (30%), i(17q) (20%), +19 (13%), +21 (7%), +17 (5%), monosomy 7 (5%). Temporal order of secondary changes varies, preferred pathway i(17q), +8, +Ph, +19.
There exist certain diagnostic criteria for CML acceleration phase (CML AP) and BC. I.e., AP is characterized by 15 – 29% blasts in blood or marrow (WHO criteria, 10 – 19%); > 20% basophils in blood; persistent thrombocytopenia unrelated to therapy; unresponsiveness to therapy. The blast crisis is registered by >30% blasts in blood or marrow (WHO, 20%); extramedullary blastic infiltrates; varying degrees of fever, anemia, splenomegaly, leukocytosis. Different means of blast crisis prevention are considered while analyzing the studies of 1983 to 2013. Special attention is drawn to tyrosine kinase inhibitors (TKIs, imatinib, nilotinib, dasatinib) in blast crisis. Introduction of imatinib led to a small increase of patient survival (up to 20% ). Most long term survivors are those that have been transplanted (28/39, ca. 72%). European Leukemia Net (ELN) presented analysis of allo-HSCT results in CML blast crisis.
Several approaches are considered. I.e., HSCT should be always used as a second-line treatment in blast phase, irrespective of the response to TKIs. It is recommended “always” in accelerated phase, if the response to TKI is less than optimal, and, as third-line therapy, if the response to second-line TKI is less than optimal. The value and the meaning of “Always” depend on transplant risk (age, comorbidities, performance status, donor, etc.).
Induction of 2nd chronic phase (CP), or remission with TKI alone or in combination with intensive chemotherapy was studied at various regimens by several study groups, i.e.: IM 800 mg + VCR + Dexa (DIV), Rea et al., 2006 (LBC) (n = 13) IM + mitoxantrone / etoposide + AraC (Frühauf et al., 2007), (MBC) ( n= 16) IM + Dauno-AraC (Deau et al., 2011)(n = 36) Dasatinib + FLAG-IDA (Milojkovic et al., 2012), (n = 4) SCT with HLA identical related or matched unrelated donor was performed at EBMT score of 0 to 4, and standard conditioning. Maintenance TKI treatment conditions after SCT have been studied by several groups (Hehlmann et al., Blood, 2012; Rea et al., 2006; Frühauf et al., Cancer 2007; Deau et al., 2011; Milojkovic et al., 2012). Application of AlloHSCT as a 2nd line therapy was studied by CML Study IV (84 patients). HSCT after imatinib failure in 1st CP was accompanied by a 94% survival rate, whereas HSCT performed in advanced phase of CML yielded a 3-year survival of 59% (Saußele et al., 2010). Similar results were published by Oyekunle et al. (2013).
Experience with blast crisis treatment was summarized for CML Study IV (n=1551 patients). The main regimen was imatinib 400 mg + AraC or intensive chemotherapy. A special assessment of CML study IV concerned the survival rates after allo-HSCT in blast crisis dependent on pretreatment, but patient numbers were too small for firm conclusions.
Comparisons were made for myeloid vs. lymphoid BC. Treatment of lymphoid type BC was associated somewhat longer median survival than myeloid-type BC. Further data analysis is in progress. Investigational trials in this field are underway (Table 1).
|
Biological effects |
Drugs/compounds |
|
PP2A activation |
Fingolimod (FTY720) |
|
SET antagonist OP449 |
|
|
CIP2A inhibitor |
|
|
Self renewal of LSC |
BCL6 + TK inhibitors |
|
HIF1α inhibitor |
|
|
Smoothened inhibitors (in combination with TKI) |
|
|
Jak2 inhibitor (in combination with TKI) |
|
|
Activation of apoptosis |
BCL2-inhibitor ABT-737 |
|
Triptolide |
|
|
Dual-kinase inhibitor ON044580 |
|
|
MEK inhibitor PD184352 + farnesyltransferase inhibitor BMS-214662 |
|
|
Others |
Peg-IFN, HDAC inhibitors, Hsp90 inhibitors |
Abbreviations, TKI: tyrosine kinase inhibitor; PP2A: protein phosphatase 2A; LSC: leukemia stem cells; MEK: mitogen-activated protein kinase; HIF: hypoxia induced factor; HDAC: histone deacetylase; Hsp: heat shock protein.
Table 1. Investigational approaches in CML blast crisis
References
- Deau B, Nicolini FE, Guilhot J, Huguet F, Guerci A, Legros L, Pautas C, Berthou C, Guyotat D, Cony-Makhoul P, Gardembas M, Michallet M, Hayette S, Cayuela JM, Weiss IR, Réa D, Castaigne S, Mahon FX, Guilhot F, Rousselot P. The addition of daunorubicin to imatinib mesylate in combination with cytarabine improves the response rate and the survival of patients with myeloid blast crisis chronic myelogenous leukemia (AFR01 study). Leuk Res. 2011; 35(6):777-82.
- Fruehauf S, Topaly J, Buss EC, Fischer T, Ottmann OG, Emmerich B, Müller MC, Schuld P, Balleisen L, Hehlmann R, Ho AD, Hochhaus A. Imatinib combined with mitoxantrone/etoposide and cytarabine is an effective induction therapy for patients with chronic myeloid leukemia in myeloid blast crisis. Cancer. 2007; 109(8):1543
- Hehlmann R. How I treat CML blast crisis. Blood. 2012; 120(4): 737‐747.
Рюдигер Хельманн
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "508" ["VALUE"]=> array(2) { ["TEXT"]=> string(135) "<p class="Autor_place_work-Rus"> Гейдельбергский университет, Германия </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(113) "Гейдельбергский университет, Германия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "509" ["VALUE"]=> array(2) { ["TEXT"]=> string(1564) "<h2>Резюме</h2> <ul> <li class="bullets">Встречаемость бластного криза низка – 5,6% после 8 лет</li> <li class="bullets">Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК</li> <li class="bullets">Лечение бластного криза в исследовании <span lang="en-US">CML</span> <span lang="en-US">Study</span> <span lang="en-US">IV</span> является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу. </li> <li class="bullets">Пока отсутствуют рекомендации по специфическому лекарственному лечению. </li> <li class="bullets">Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ. </li> <li class="bullets ParaOverride-5">Европейская организация <span lang="en-US">ELN</span> рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.</li> </ul>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1320) "Резюме
- Встречаемость бластного криза низка – 5,6% после 8 лет
- Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК
- Лечение бластного криза в исследовании CML Study IV является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу.
- Пока отсутствуют рекомендации по специфическому лекарственному лечению.
- Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ.
- Европейская организация ELN рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.
Rüdiger Hehlmann
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "512" ["VALUE"]=> array(2) { ["TEXT"]=> string(113) "<span class="CharOverride-5" lang="en-US">Universität Heidelberg, Germany</span>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(81) "Universität Heidelberg, Germany" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "513" ["VALUE"]=> array(2) { ["TEXT"]=> string(595) "<h2>Resume</h2> <ul> <li> Incidence of BC is low, with 5.6% after 8 years. </li> <li> Survival after BC not much improved with TKI. </li> <li> Treatment of BC in CML study IV is heterogeneous as expected without specific recommendations in the study protocol. </li> <li> No recommendation of a specific drug treatment is possible. </li> <li> Transplantation carries the best long term prognosis in BC. </li> <li> Allo SCT always recommended in BC by ELN. </li> </ul>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(499) "Resume
- Incidence of BC is low, with 5.6% after 8 years.
- Survival after BC not much improved with TKI.
- Treatment of BC in CML study IV is heterogeneous as expected without specific recommendations in the study protocol.
- No recommendation of a specific drug treatment is possible.
- Transplantation carries the best long term prognosis in BC.
- Allo SCT always recommended in BC by ELN.
Прогрессия хронического миелоидного лейкоза (ХМЛ) в бластный криз все еще является недостаточно изученным феноменом. Сообщается о наличии дополнительных хромосомных аберраций у пациентов с бластным кризом ХМЛ (до 90% случаев).
До 77% таких мутаций выявлены посредством глубокого геномного секвенирования. Согласно данным об профиле генной экспрессии, бластный кризис, видимо, является заболеванием, отличным от ХМЛ. Продолжение лечения, большей частью безуспешно, несмотря на возможность трансплантации гемопоэтических клеток (ТСК). Неудача терапии означает точку невозврата. Дополнительные хромосомные аберрации ассоциированы с развитием бластного криза, будучи неслучайными по распределению в хромосомах. Наиболее частыми аберрациями здесь являются: +8 (34%); +Ph (30%); i(17q) (20%); +19 (13%); +21 (7%); +17 (5%); моносомия 7 (5%). Временной порядок появления вторичных аномалий различен, чаще; i(17q), +8, +Ph, +19. Существуют определенные диагностические критерии для фазы акселерации (ФА) ХМЛ и бластного криза, т.е. ФА характеризуется 15 – 29% бластов в крови или костном мозге (по критериям ВОЗ – 10 – 19%), > 20% базофилов в крови, стойкой тромбоцитемией, независимо от лечения, нечувствительностью к терапии. Бластный криз диагностируется при >30% бластов в крови или костном мозге (по ВОЗ – 20%); экстрамедуллярной бластной инфильтрации, лихорадке различной степени, анемии, спленомегалии, лейкоцитозе. Рассматриваются различные средства предотвращения бластного криза при анализе исследований с 1983 по 2013 гг. Особое внимание уделяется ингибиторам тирозинкиназ (ИТК – иматиниб, нилотиниб, дазатиниб) для лечения бластного криза ХМЛ. Внедрение иматиниба приводило к небольшому повышению выживаемости больных (до 20% ). Наиболее долгоживущие пациенты – те, которым проводилась ТСК (28/39, ок. 72%).
Европейская организация European Leukemia Net (ELN) представила анализ результатов алло-ТГСК при бластном кризисе ХМЛ. Рассмотрены несколько подходов, т.е. ТСК должна применяться всегда в качестве второй линии терапии бластного криза, независимо от ответа на ИТК. Также всегда рекомендуется поступать в фазе акселерации, если ответ на ИТК недостаточен и, в качестве третьей линии терапии – если недостаточен ответ при лечении препаратами второй линии.
Оценка и значение понятия «Всегда» зависят от факторов индивидуального риска трансплантации (возраст, сопутствующие заболевания, физический статус, донор и др.).
Индукция 2-й хронической фазы или ремиссия только на ИТК или в комбинации с интенсивной химиотерапией изучалась несколькими группами авторов при различных режимах, а именно:
- Иматиниб 800 mg + Винкристин + Дексаметазон (DIV) (Rea et al., 2006) (LBC) (n = 13)
- Иматиниб + митоксантрон/этопозид + AraC (Frühauf et al., 2007), (MBC) ( n= 16)
- Иматиниб + дауномицин + AraC (Deau et al., 2011)
(n = 36) - Дазатиниб + FLAG-Идарубицин (Milojkovic et al., 2012), (n = 4)
Трансплантация гемопоэтических клеток от HLA-идентичного родственного тлт совместимого неродственного донора проводилась при статусе больных от 0 до 4 и стандартном кондиционировании. Режимы поддерживающей терапии ИТК изучались несколькими группами (Hehlmann et al., Blood, 2012; Rea et al., 2006; Frühauf et al., Cancer 2007; Deau et al., 2011; Milojkovic et al., 2012).
Применение алло-ТСК в качестве терапии второй линии оценивалось в исследовании CML Study IV (84 случая).
Выполнение ТСК после неудачной терапии иматинибом в 1-й хронической фазе сопровождалось выживаемостью 94%, тогда как ТСК в развернутой фазе ХМЛ приводило к 3-летней выживаемости 59% (Saußele et al., 2010). Сходные результаты были опубликованы Oyekunle et al. (2013).
Опыт лечения бластного криза был обобщен в исследовании CML Study IV (1551 пациентов).
Основным режимом было лечение Иматинибом (400 mg) + AraC и интенсивная химиотерапия. Специальная оценка в CML Study IV касалась уровней выживаемости после алло-ТГСК в бластном кризе, в зависимости от «предлеченности» больного crisis, однако количество пациентов было слишком малым для надежных выводов. Были проведены сравнения для бластных кризов миелоидного и лимфоидного типов. Лечение лимфоидного бластного криза было ассоциировано с несколько более длительным средним сроком жизни, нежели при миелоидном типе бластного криза. Дальнейший анализ данных продолжается. В разработке находятся и экспериментальные подходы в этой области терапии (Табл. 1)
|
Биологические эффекты |
Препараты/соединения |
|
Активация PP2A |
Fingolimod (FTY720) |
|
Антагонист SET OP449 |
|
|
Ингибитор CIP2A |
|
|
Самообновление ЛСК |
BCL6 + ингибиторы TK |
|
Ингибитор HIF1α |
|
|
Более мягкие ингибиторы (в сочетании с ИТК) |
|
|
Ингибитор Jak2 (в сочетании с ИТК) |
|
|
Активация апоптоза |
Ингибитор BCL2 ABT-737 |
|
Триптолид |
|
|
Двойной ингибитор киназы ON044580 |
|
|
Ингибитор MEK PD184352 + фарнезиотрансферазы Ингибитор BMS-214662 |
|
|
Прочее |
Пегилированный интерферон, ингибиторы гистондеацетилазы, ингибиторы Нsp90 |
Сокращения: ИТК: ингибитор тирозинкиназы; PP2A: протеинфосфатаза 2A; LSC: лейкозные стволовые клетки; MEK: митоген-активируемая протеинкиназа; HIF: фактор, индуцированный гипоксией; HDAC: гистондеацетилаза; Hsp: белок теплового шока.
Таблица 1. Экспериментальные походы к лечению бластного криза ХМЛ
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1239" ["VALUE"]=> string(2) "22" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "22" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1240" ["VALUE"]=> string(2) "23" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "23" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(15) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "511" ["VALUE"]=> array(2) { ["TEXT"]=> string(61) "<p class="Autor">Rüdiger Hehlmann </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(39) "Rüdiger Hehlmann
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(39) "Rüdiger Hehlmann
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "513" ["VALUE"]=> array(2) { ["TEXT"]=> string(595) "<h2>Resume</h2> <ul> <li> Incidence of BC is low, with 5.6% after 8 years. </li> <li> Survival after BC not much improved with TKI. </li> <li> Treatment of BC in CML study IV is heterogeneous as expected without specific recommendations in the study protocol. </li> <li> No recommendation of a specific drug treatment is possible. </li> <li> Transplantation carries the best long term prognosis in BC. </li> <li> Allo SCT always recommended in BC by ELN. </li> </ul>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(499) "Resume
- Incidence of BC is low, with 5.6% after 8 years.
- Survival after BC not much improved with TKI.
- Treatment of BC in CML study IV is heterogeneous as expected without specific recommendations in the study protocol.
- No recommendation of a specific drug treatment is possible.
- Transplantation carries the best long term prognosis in BC.
- Allo SCT always recommended in BC by ELN.
Resume
- Incidence of BC is low, with 5.6% after 8 years.
- Survival after BC not much improved with TKI.
- Treatment of BC in CML study IV is heterogeneous as expected without specific recommendations in the study protocol.
- No recommendation of a specific drug treatment is possible.
- Transplantation carries the best long term prognosis in BC.
- Allo SCT always recommended in BC by ELN.
Рюдигер Хельманн
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(75) "Рюдигер Хельманн
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "503" ["VALUE"]=> string(19) "27.03.2015 16:45:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "27.03.2015 16:45:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "27.03.2015 16:45:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "504" ["VALUE"]=> string(19) "05.06.2015 16:46:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "05.06.2015 16:46:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "05.06.2015 16:46:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "916" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(4) { [0]=> string(4) "1235" [1]=> string(4) "1236" [2]=> string(4) "1237" [3]=> string(4) "1238" } ["VALUE"]=> array(4) { [0]=> string(2) "88" [1]=> string(2) "89" [2]=> string(2) "15" [3]=> string(2) "91" } ["DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(4) { [0]=> string(2) "88" [1]=> string(2) "89" [2]=> string(2) "15" [3]=> string(2) "91" } ["~DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(4) { [0]=> string(99) "хронический миелоидный лейкоз" [1]=> string(68) "бластный криз" [2]=> string(134) "трансплантация гемопоэтических стволовых клеток" [3]=> string(92) "экспериментальная терапия" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "505" ["VALUE"]=> string(2) "87" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "87" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(59) "Rüdiger Hehlmann" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "509" ["VALUE"]=> array(2) { ["TEXT"]=> string(1564) "<h2>Резюме</h2> <ul> <li class="bullets">Встречаемость бластного криза низка – 5,6% после 8 лет</li> <li class="bullets">Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК</li> <li class="bullets">Лечение бластного криза в исследовании <span lang="en-US">CML</span> <span lang="en-US">Study</span> <span lang="en-US">IV</span> является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу. </li> <li class="bullets">Пока отсутствуют рекомендации по специфическому лекарственному лечению. </li> <li class="bullets">Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ. </li> <li class="bullets ParaOverride-5">Европейская организация <span lang="en-US">ELN</span> рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.</li> </ul>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1320) "Резюме
- Встречаемость бластного криза низка – 5,6% после 8 лет
- Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК
- Лечение бластного криза в исследовании CML Study IV является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу.
- Пока отсутствуют рекомендации по специфическому лекарственному лечению.
- Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ.
- Европейская организация ELN рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.
Резюме
- Встречаемость бластного криза низка – 5,6% после 8 лет
- Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК
- Лечение бластного криза в исследовании CML Study IV является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу.
- Пока отсутствуют рекомендации по специфическому лекарственному лечению.
- Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ.
- Европейская организация ELN рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.
Гейдельбергский университет, Германия
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(113) "Гейдельбергский университет, Германия
" } ["FULL_TEXT_RU"]=> array(37) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1021" ["VALUE"]=> array(2) { ["TEXT"]=> string(19154) "<p class="text"> Прогрессия хронического миелоидного лейкоза (ХМЛ) в бластный криз все еще является недостаточно изученным феноменом. Сообщается о наличии дополнительных хромосомных аберраций у пациентов с бластным кризом ХМЛ (до 90% случаев). </p> <p class="text"> До 77% таких мутаций выявлены посредством глубокого геномного секвенирования. Согласно данным об профиле генной экспрессии, бластный кризис, видимо, является заболеванием, отличным от ХМЛ. Продолжение лечения, большей частью безуспешно, несмотря на возможность трансплантации гемопоэтических клеток (ТСК). Неудача терапии означает точку невозврата. Дополнительные хромосомные аберрации ассоциированы с развитием бластного криза, будучи неслучайными по распределению в хромосомах. Наиболее частыми аберрациями здесь являются: +8 (34%); +<span lang="en-US">Ph</span> (30%); <span lang="en-US">i</span>(17<span lang="en-US">q</span>) (20%); +19 (13%); +21 (7%); +17 (5%); моносомия 7 (5%). Временной порядок появления вторичных аномалий различен, чаще; <span lang="en-US">i</span>(17<span lang="en-US">q</span>), +8, +<span lang="en-US">Ph</span>, +19. Существуют определенные диагностические критерии для фазы акселерации (ФА) ХМЛ и бластного криза, т.е. ФА характеризуется 15 – 29% бластов в крови или костном мозге (по критериям ВОЗ – 10 – 19%), > 20% базофилов в крови, стойкой тромбоцитемией, независимо от лечения, нечувствительностью к терапии. Бластный криз диагностируется при >30% бластов в крови или костном мозге (по ВОЗ – 20%); экстрамедуллярной бластной инфильтрации, лихорадке различной степени, анемии, спленомегалии, лейкоцитозе. Рассматриваются различные средства предотвращения бластного криза при анализе исследований с 1983 по 2013 гг. Особое внимание уделяется ингибиторам тирозинкиназ (ИТК – иматиниб, нилотиниб, дазатиниб) для лечения бластного криза ХМЛ. Внедрение иматиниба приводило к небольшому повышению выживаемости больных (до 20% ). Наиболее долгоживущие пациенты – те, которым проводилась ТСК (28/39, ок. 72%). </p> <p class="text"> Европейская организация <span lang="en-US">European</span> <span lang="en-US">Leukemia</span> <span lang="en-US">Net</span> (<span lang="en-US">ELN</span>) представила анализ результатов алло-ТГСК при бластном кризисе ХМЛ. Рассмотрены несколько подходов, т.е. ТСК должна применяться всегда в качестве второй линии терапии бластного криза, независимо от ответа на ИТК. Также всегда рекомендуется поступать в фазе акселерации, если ответ на ИТК недостаточен и, в качестве третьей линии терапии – если недостаточен ответ при лечении препаратами второй линии. </p> <p class="text"> Оценка и значение понятия «Всегда» зависят от факторов индивидуального риска трансплантации (возраст, сопутствующие заболевания, физический статус, донор и др.). </p> <p class="text ParaOverride-2"> Индукция 2-й хронической фазы или ремиссия только на ИТК или в комбинации с интенсивной химиотерапией изучалась несколькими группами авторов при различных режимах, а именно: </p> <ul> <li class="bullets">Иматиниб 800 <span lang="de-DE">mg</span> + Винкристин + Дексаметазон (<span lang="de-DE">DIV</span>) (<span lang="de-DE">Rea</span> <span lang="de-DE">et</span> <span lang="de-DE">al</span>., 2006) (<span lang="de-DE">LBC</span>) (<span lang="de-DE">n</span> = 13)</li> <li class="bullets">Иматиниб + митоксантрон/этопозид + <span lang="de-DE">AraC</span> (<span lang="de-DE">Fr</span>ü<span lang="de-DE">hauf</span> <span lang="de-DE">et</span> <span lang="de-DE">al</span>., 2007), (<span lang="de-DE">MBC</span>) ( <span lang="de-DE">n</span>= 16)</li> <li class="bullets">Иматиниб<span lang="fr-FR"> + </span>дауномицин + <span lang="fr-FR">AraC (Deau et al., 2011)<br> (n = 36)</span></li> <li class="bullets ParaOverride-5">Дазатиниб<span lang="fr-FR"> + FLAG-</span>Идарубицин<span lang="fr-FR"> (Milojkovic et al., 2012), (n = 4)</span></li> </ul> <p class="text"> Трансплантация<span lang="fr-FR"> </span>гемопоэтических<span lang="fr-FR"> </span>клеток<span lang="fr-FR"> </span>от<span lang="fr-FR"> HLA-</span>идентичного<span lang="fr-FR"> </span>родственного<span lang="fr-FR"> </span>тлт<span lang="fr-FR"> </span>совместимого<span lang="fr-FR"> </span>неродственного<span lang="fr-FR"> </span>донора<span lang="fr-FR"> </span>проводилась<span lang="fr-FR"> </span>при<span lang="fr-FR"> </span>статусе<span lang="fr-FR"> </span>больных<span lang="fr-FR"> </span>от<span lang="fr-FR"> 0 </span>до<span lang="fr-FR"> 4 </span>и стандартном кондиционировании. Режимы поддерживающей терапии ИТК изучались несколькими группами (<span lang="en-US">Hehlmann</span> <span lang="en-US">et</span> <span lang="en-US">al</span>., <span lang="en-US">Blood</span>, 2012; <span lang="en-US">Rea</span> <span lang="en-US">et</span> <span lang="en-US">al</span>., 2006; <span lang="en-US">Fr</span>ü<span lang="en-US">hauf</span> <span lang="en-US">et</span> <span lang="en-US">al</span>., <span lang="en-US">Cancer</span> <span lang="fr-FR">2007; Deau et al., 2011; Milojkovic et al., 2012).</span> </p> <p class="text"> Применение алло-ТСК в качестве терапии второй линии оценивалось в исследовании <span lang="en-US">CML</span> <span lang="en-US">Study</span> <span lang="en-US">IV</span> (84 случая). </p> <p class="text"> Выполнение ТСК после неудачной терапии иматинибом в 1-й хронической фазе сопровождалось выживаемостью 94%, тогда как ТСК в развернутой фазе ХМЛ приводило к 3-летней выживаемости 59% (<span lang="en-US">Sau</span>ß<span lang="en-US">ele</span> <span lang="en-US">et</span> <span lang="en-US">al</span>., 2010). Сходные результаты были опубликованы <span lang="en-US">Oyekunle</span> <span lang="en-US">et</span> <span lang="en-US">al</span>. (2013). </p> <p class="text"> Опыт лечения бластного криза был обобщен в исследовании <span lang="en-US">CML</span> <span lang="en-US">Study</span> <span lang="en-US">IV</span> (1551 пациентов). </p> <p class="text"> Основным режимом было лечение Иматинибом (400 <span lang="en-US">mg</span>) + <span lang="en-US">AraC</span> и интенсивная химиотерапия. Специальная оценка в <span lang="en-US">CML</span> <span lang="en-US">Study</span> <span lang="en-US">IV</span> касалась уровней выживаемости после алло-ТГСК в бластном кризе, в зависимости от «предлеченности» больного <span lang="en-US">crisis</span>, однако количество пациентов было слишком малым для надежных выводов. Были проведены сравнения для бластных кризов миелоидного и лимфоидного типов. Лечение лимфоидного бластного криза было ассоциировано с несколько более длительным средним сроком жизни, нежели при миелоидном типе бластного криза. Дальнейший анализ данных продолжается. В разработке находятся и экспериментальные подходы в этой области терапии (Табл. 1) </p> <table id="table013" class="No-Table-Style TableOverride-4"> <colgroup> <col class="_idGenTableRowColumn-8"> <col class="_idGenTableRowColumn-25"> </colgroup> <tbody> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> <p class="Table_text"> Биологические эффекты </p> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Препараты<span lang="en-US">/</span>соединения </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> <p class="Table_text"> Активация PP2A </p> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Fingolimod (FTY720) </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Антагонист SET OP449 </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Ингибитор CIP2A </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> <p class="Table_text"> Самообновление ЛСК </p> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> BCL6 + ингибиторы TK </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Ингибитор HIF1<span class="CharOverride-8">α</span> </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Более мягкие ингибиторы (в сочетании с ИТК) </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Ингибитор Jak2 (в сочетании с ИТК) </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> <p class="Table_text"> Активация апоптоза </p> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Ингибитор BCL2 ABT-737 </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Триптолид </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-4"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Двойной ингибитор киназы ON044580 </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-5"> <td class="No-Table-Style CellOverride-22"> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Ингибитор MEK PD184352 + фарнезиотрансферазы </p> <p class="Table_text"> Ингибитор BMS-214662 </p> </td> </tr> <tr class="No-Table-Style _idGenTableRowColumn-5"> <td class="No-Table-Style CellOverride-22"> <p class="Table_text"> Прочее </p> </td> <td class="No-Table-Style CellOverride-23"> <p class="Table_text"> Пегилированный интерферон, ингибиторы гистондеацетилазы, ингибиторы Нsp90 </p> </td> </tr> </tbody> </table> <p class="text"> <span class="CharOverride-4">Сокращения: ИТК: ингибитор тирозинкиназы; </span><span class="CharOverride-4" lang="en-US">PP</span><span class="CharOverride-4">2</span><span class="CharOverride-4" lang="en-US">A</span><span class="CharOverride-4">: протеинфосфатаза 2</span><span class="CharOverride-4" lang="en-US">A</span><span class="CharOverride-4">; </span><span class="CharOverride-4" lang="en-US">LSC</span><span class="CharOverride-4">: лейкозные стволовые клетки; </span><span class="CharOverride-4" lang="en-US">MEK</span><span class="CharOverride-4">: митоген-активируемая протеинкиназа; </span><span class="CharOverride-4" lang="en-US">HIF</span><span class="CharOverride-4">: фактор, индуцированный гипоксией; </span><span class="CharOverride-4" lang="en-US">HDAC</span><span class="CharOverride-4">: гистондеацетилаза; </span><span class="CharOverride-4" lang="en-US">Hsp</span><span class="CharOverride-4">: белок теплового шока.</span> </p> <p class="Table_sign"> Таблица 1. Экспериментальные походы к лечению бластного криза ХМЛ </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(15242) "Прогрессия хронического миелоидного лейкоза (ХМЛ) в бластный криз все еще является недостаточно изученным феноменом. Сообщается о наличии дополнительных хромосомных аберраций у пациентов с бластным кризом ХМЛ (до 90% случаев).
До 77% таких мутаций выявлены посредством глубокого геномного секвенирования. Согласно данным об профиле генной экспрессии, бластный кризис, видимо, является заболеванием, отличным от ХМЛ. Продолжение лечения, большей частью безуспешно, несмотря на возможность трансплантации гемопоэтических клеток (ТСК). Неудача терапии означает точку невозврата. Дополнительные хромосомные аберрации ассоциированы с развитием бластного криза, будучи неслучайными по распределению в хромосомах. Наиболее частыми аберрациями здесь являются: +8 (34%); +Ph (30%); i(17q) (20%); +19 (13%); +21 (7%); +17 (5%); моносомия 7 (5%). Временной порядок появления вторичных аномалий различен, чаще; i(17q), +8, +Ph, +19. Существуют определенные диагностические критерии для фазы акселерации (ФА) ХМЛ и бластного криза, т.е. ФА характеризуется 15 – 29% бластов в крови или костном мозге (по критериям ВОЗ – 10 – 19%), > 20% базофилов в крови, стойкой тромбоцитемией, независимо от лечения, нечувствительностью к терапии. Бластный криз диагностируется при >30% бластов в крови или костном мозге (по ВОЗ – 20%); экстрамедуллярной бластной инфильтрации, лихорадке различной степени, анемии, спленомегалии, лейкоцитозе. Рассматриваются различные средства предотвращения бластного криза при анализе исследований с 1983 по 2013 гг. Особое внимание уделяется ингибиторам тирозинкиназ (ИТК – иматиниб, нилотиниб, дазатиниб) для лечения бластного криза ХМЛ. Внедрение иматиниба приводило к небольшому повышению выживаемости больных (до 20% ). Наиболее долгоживущие пациенты – те, которым проводилась ТСК (28/39, ок. 72%).
Европейская организация European Leukemia Net (ELN) представила анализ результатов алло-ТГСК при бластном кризисе ХМЛ. Рассмотрены несколько подходов, т.е. ТСК должна применяться всегда в качестве второй линии терапии бластного криза, независимо от ответа на ИТК. Также всегда рекомендуется поступать в фазе акселерации, если ответ на ИТК недостаточен и, в качестве третьей линии терапии – если недостаточен ответ при лечении препаратами второй линии.
Оценка и значение понятия «Всегда» зависят от факторов индивидуального риска трансплантации (возраст, сопутствующие заболевания, физический статус, донор и др.).
Индукция 2-й хронической фазы или ремиссия только на ИТК или в комбинации с интенсивной химиотерапией изучалась несколькими группами авторов при различных режимах, а именно:
- Иматиниб 800 mg + Винкристин + Дексаметазон (DIV) (Rea et al., 2006) (LBC) (n = 13)
- Иматиниб + митоксантрон/этопозид + AraC (Frühauf et al., 2007), (MBC) ( n= 16)
- Иматиниб + дауномицин + AraC (Deau et al., 2011)
(n = 36) - Дазатиниб + FLAG-Идарубицин (Milojkovic et al., 2012), (n = 4)
Трансплантация гемопоэтических клеток от HLA-идентичного родственного тлт совместимого неродственного донора проводилась при статусе больных от 0 до 4 и стандартном кондиционировании. Режимы поддерживающей терапии ИТК изучались несколькими группами (Hehlmann et al., Blood, 2012; Rea et al., 2006; Frühauf et al., Cancer 2007; Deau et al., 2011; Milojkovic et al., 2012).
Применение алло-ТСК в качестве терапии второй линии оценивалось в исследовании CML Study IV (84 случая).
Выполнение ТСК после неудачной терапии иматинибом в 1-й хронической фазе сопровождалось выживаемостью 94%, тогда как ТСК в развернутой фазе ХМЛ приводило к 3-летней выживаемости 59% (Saußele et al., 2010). Сходные результаты были опубликованы Oyekunle et al. (2013).
Опыт лечения бластного криза был обобщен в исследовании CML Study IV (1551 пациентов).
Основным режимом было лечение Иматинибом (400 mg) + AraC и интенсивная химиотерапия. Специальная оценка в CML Study IV касалась уровней выживаемости после алло-ТГСК в бластном кризе, в зависимости от «предлеченности» больного crisis, однако количество пациентов было слишком малым для надежных выводов. Были проведены сравнения для бластных кризов миелоидного и лимфоидного типов. Лечение лимфоидного бластного криза было ассоциировано с несколько более длительным средним сроком жизни, нежели при миелоидном типе бластного криза. Дальнейший анализ данных продолжается. В разработке находятся и экспериментальные подходы в этой области терапии (Табл. 1)
|
Биологические эффекты |
Препараты/соединения |
|
Активация PP2A |
Fingolimod (FTY720) |
|
Антагонист SET OP449 |
|
|
Ингибитор CIP2A |
|
|
Самообновление ЛСК |
BCL6 + ингибиторы TK |
|
Ингибитор HIF1α |
|
|
Более мягкие ингибиторы (в сочетании с ИТК) |
|
|
Ингибитор Jak2 (в сочетании с ИТК) |
|
|
Активация апоптоза |
Ингибитор BCL2 ABT-737 |
|
Триптолид |
|
|
Двойной ингибитор киназы ON044580 |
|
|
Ингибитор MEK PD184352 + фарнезиотрансферазы Ингибитор BMS-214662 |
|
|
Прочее |
Пегилированный интерферон, ингибиторы гистондеацетилазы, ингибиторы Нsp90 |
Сокращения: ИТК: ингибитор тирозинкиназы; PP2A: протеинфосфатаза 2A; LSC: лейкозные стволовые клетки; MEK: митоген-активируемая протеинкиназа; HIF: фактор, индуцированный гипоксией; HDAC: гистондеацетилаза; Hsp: белок теплового шока.
Таблица 1. Экспериментальные походы к лечению бластного криза ХМЛ
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(15242) "Прогрессия хронического миелоидного лейкоза (ХМЛ) в бластный криз все еще является недостаточно изученным феноменом. Сообщается о наличии дополнительных хромосомных аберраций у пациентов с бластным кризом ХМЛ (до 90% случаев).
До 77% таких мутаций выявлены посредством глубокого геномного секвенирования. Согласно данным об профиле генной экспрессии, бластный кризис, видимо, является заболеванием, отличным от ХМЛ. Продолжение лечения, большей частью безуспешно, несмотря на возможность трансплантации гемопоэтических клеток (ТСК). Неудача терапии означает точку невозврата. Дополнительные хромосомные аберрации ассоциированы с развитием бластного криза, будучи неслучайными по распределению в хромосомах. Наиболее частыми аберрациями здесь являются: +8 (34%); +Ph (30%); i(17q) (20%); +19 (13%); +21 (7%); +17 (5%); моносомия 7 (5%). Временной порядок появления вторичных аномалий различен, чаще; i(17q), +8, +Ph, +19. Существуют определенные диагностические критерии для фазы акселерации (ФА) ХМЛ и бластного криза, т.е. ФА характеризуется 15 – 29% бластов в крови или костном мозге (по критериям ВОЗ – 10 – 19%), > 20% базофилов в крови, стойкой тромбоцитемией, независимо от лечения, нечувствительностью к терапии. Бластный криз диагностируется при >30% бластов в крови или костном мозге (по ВОЗ – 20%); экстрамедуллярной бластной инфильтрации, лихорадке различной степени, анемии, спленомегалии, лейкоцитозе. Рассматриваются различные средства предотвращения бластного криза при анализе исследований с 1983 по 2013 гг. Особое внимание уделяется ингибиторам тирозинкиназ (ИТК – иматиниб, нилотиниб, дазатиниб) для лечения бластного криза ХМЛ. Внедрение иматиниба приводило к небольшому повышению выживаемости больных (до 20% ). Наиболее долгоживущие пациенты – те, которым проводилась ТСК (28/39, ок. 72%).
Европейская организация European Leukemia Net (ELN) представила анализ результатов алло-ТГСК при бластном кризисе ХМЛ. Рассмотрены несколько подходов, т.е. ТСК должна применяться всегда в качестве второй линии терапии бластного криза, независимо от ответа на ИТК. Также всегда рекомендуется поступать в фазе акселерации, если ответ на ИТК недостаточен и, в качестве третьей линии терапии – если недостаточен ответ при лечении препаратами второй линии.
Оценка и значение понятия «Всегда» зависят от факторов индивидуального риска трансплантации (возраст, сопутствующие заболевания, физический статус, донор и др.).
Индукция 2-й хронической фазы или ремиссия только на ИТК или в комбинации с интенсивной химиотерапией изучалась несколькими группами авторов при различных режимах, а именно:
- Иматиниб 800 mg + Винкристин + Дексаметазон (DIV) (Rea et al., 2006) (LBC) (n = 13)
- Иматиниб + митоксантрон/этопозид + AraC (Frühauf et al., 2007), (MBC) ( n= 16)
- Иматиниб + дауномицин + AraC (Deau et al., 2011)
(n = 36) - Дазатиниб + FLAG-Идарубицин (Milojkovic et al., 2012), (n = 4)
Трансплантация гемопоэтических клеток от HLA-идентичного родственного тлт совместимого неродственного донора проводилась при статусе больных от 0 до 4 и стандартном кондиционировании. Режимы поддерживающей терапии ИТК изучались несколькими группами (Hehlmann et al., Blood, 2012; Rea et al., 2006; Frühauf et al., Cancer 2007; Deau et al., 2011; Milojkovic et al., 2012).
Применение алло-ТСК в качестве терапии второй линии оценивалось в исследовании CML Study IV (84 случая).
Выполнение ТСК после неудачной терапии иматинибом в 1-й хронической фазе сопровождалось выживаемостью 94%, тогда как ТСК в развернутой фазе ХМЛ приводило к 3-летней выживаемости 59% (Saußele et al., 2010). Сходные результаты были опубликованы Oyekunle et al. (2013).
Опыт лечения бластного криза был обобщен в исследовании CML Study IV (1551 пациентов).
Основным режимом было лечение Иматинибом (400 mg) + AraC и интенсивная химиотерапия. Специальная оценка в CML Study IV касалась уровней выживаемости после алло-ТГСК в бластном кризе, в зависимости от «предлеченности» больного crisis, однако количество пациентов было слишком малым для надежных выводов. Были проведены сравнения для бластных кризов миелоидного и лимфоидного типов. Лечение лимфоидного бластного криза было ассоциировано с несколько более длительным средним сроком жизни, нежели при миелоидном типе бластного криза. Дальнейший анализ данных продолжается. В разработке находятся и экспериментальные подходы в этой области терапии (Табл. 1)
|
Биологические эффекты |
Препараты/соединения |
|
Активация PP2A |
Fingolimod (FTY720) |
|
Антагонист SET OP449 |
|
|
Ингибитор CIP2A |
|
|
Самообновление ЛСК |
BCL6 + ингибиторы TK |
|
Ингибитор HIF1α |
|
|
Более мягкие ингибиторы (в сочетании с ИТК) |
|
|
Ингибитор Jak2 (в сочетании с ИТК) |
|
|
Активация апоптоза |
Ингибитор BCL2 ABT-737 |
|
Триптолид |
|
|
Двойной ингибитор киназы ON044580 |
|
|
Ингибитор MEK PD184352 + фарнезиотрансферазы Ингибитор BMS-214662 |
|
|
Прочее |
Пегилированный интерферон, ингибиторы гистондеацетилазы, ингибиторы Нsp90 |
Сокращения: ИТК: ингибитор тирозинкиназы; PP2A: протеинфосфатаза 2A; LSC: лейкозные стволовые клетки; MEK: митоген-активируемая протеинкиназа; HIF: фактор, индуцированный гипоксией; HDAC: гистондеацетилаза; Hsp: белок теплового шока.
Таблица 1. Экспериментальные походы к лечению бластного криза ХМЛ
" } } } [9]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(1) "3" ["~IBLOCK_SECTION_ID"]=> string(1) "3" ["ID"]=> string(2) "96" ["~ID"]=> string(2) "96" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(178) "Клетки пуповинной крови как естественный источник донорства для лечения ВИЧ-инфекции и лейкозов" ["~NAME"]=> string(178) "Клетки пуповинной крови как естественный источник донорства для лечения ВИЧ-инфекции и лейкозов" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(19) "09.09.2015 16:46:58" ["~TIMESTAMP_X"]=> string(19) "09.09.2015 16:46:58" ["DETAIL_PAGE_URL"]=> string(62) "/ru/archive/Volume-4/short-reports/1866-8836-2015-4-1-2-62-65/" ["~DETAIL_PAGE_URL"]=> string(62) "/ru/archive/Volume-4/short-reports/1866-8836-2015-4-1-2-62-65/" ["LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["~LIST_PAGE_URL"]=> string(12) "/ru/archive/" ["DETAIL_TEXT"]=> string(12550) "In February 2007, Hütter et al performed an allogeneic hematopoietic stem cell transplantation (HSCT) in a patient with acute myeloid leukemia (AML) who has been co-infected with HIV. The HSCT was performed using peripheral blood stem cells from an adult donor. The patient, known as “The Berlin Patient”, was cured of HIV as well as his AML [1]. This “magic” cure inspired many hematologists to more thoroughly investigate the prospects of cure for patients suffering from leukemia and co-infection with of HIV.
The rationale for such treatment is based on the assumption that (A) HIV primarily infects the hematopoetic system; and (B) that an HSCT replaces the infected hematopoiesis with an un-infected bone marrow. Uninfected littermates of the new bone marrow will then again repopulate the host in all different compartments of the body. However, a major challenge remains the reinfection of donor cells after HSCT. In particular typical reservoirs of HIV like monocytes are usually replaced not until months after HSCT through the new donor. Persisting host monocytes are consequently a source for HIV and threat for reinfection of the new donor. A graft-versus-host disease (GVHD) may therefore be an essential factor for eliminating residual HIV reservoirs after HSCT.
To prevent HIV reinfection of the new donor in the patients, one may use a donor with a natural deletion in CCR5, which blocks entry for the most common HIV strain. This genetic trait is found in <1% of general population. Therefore, a search for patient two has been challenging. In this case, the patient needs to have an indication for an HSCT, to be co-infected with HIV, and HIV must selectively be restricted to the receptor CCR5. The frequency of CCR5-del32/del32 donors is usually ≤1% in Caucasians and much less in other ethnic groups. Hence, the transplant patients usually have only a small number of available donors. When adult donors are used, a very close HLA match with the patient is required (7-8/8). Due to these limitations, the second patient was acquired only many years later in 2014 [3,8], unfortunately, with subsequent failure in terms of HIV control, most likely due to the fact that the virus already used another entry port like CXCR4.
Utilizing cord blood donors in the last decade as standard donor for many transplantations opened an avenue to a new potential source of donors for HIV infected patients. Firstly, although not well understood, a lower HLA matching between cord blood units and patients is sufficient for a good outcome of HSCT [9]. These less restricted matching criteria increase substantially the chance to find a donor in the very same genetic pool. Vice versa, if a cord blood unit with a unique trait like CCR5-del32/del32 is identified, it can be theoretically used for more patients. Increasing the pool of an inventory of CCR5-del32/del32 umbilical cord blood units will therefore provide as off-the-shelf product a rapid and greatly improved probability of finding an appropriately HLA-matched donor with an adequate cell dose for a patient with HIV infection with CCR5 tropism and in need of an HSCT. A theoretic inventory for a minimal required number del32/del32 CB units was performed recently [7] showing that it is very likely to identify one HLA matched homozygous CCR5-del32 cord blood unit for a patient with appropriate clinical indications for HSCT. However, stem cells per cord blood unit are small and one unit is frequently not sufficient to appropriately engraft an adult patient in time. Therefore, cord blood transplantations in adults utilize usually two cord blood units in order to overcome the limitation of little numbers in stem cells per cord blood unit. As simplistic and smart this strategy seems to be at a first sight for patients without co-infection of HIV, as problematic it is for patients with HIV: It is very unlikely to find two CCR5-del32 cord blood units and outgrowth of the CCR5-del32 unit would be then left to chance. One solution might come from combining cord blood and haplo transplantation. The haplo product, once deeply T cell depleted can be considered in this strategy as a bridge to long term engraftment of the cord blood unit as pioneered by Spanish colleagues [6]. Therapeutic prospects of the combined haplo cord blood transplantation include a safer and more rapid engraftment of neutrophils, thus providing better protection against infections. Combining haplo and cord blood donors may be justified even with a suitable donor for defined indications. Others showed that the combined haplo and cord blood transplantation have an acceptable safety profile which is comparable to MUD donors [4, 5]. However, the most recent development of single cord blood expansion protocols might provide a new avenue to pursue such transplantations with only one CCR5-del32 cord blood unit.
Beside a careful evaluation of donor choices an additional important consideration arises from the perspective of HIV positive patients: Although HIV infection is nowadays regarded as a chronic disease in the era of effective HAART, quality of life of HIV-infected patients is usually substantially impaired. A study examining the frequency of suicides in HIV positive patients from 1988 to 2008 followed 15,275 HIV-infected patients up for a median duration of 4.7 years. Suicide rates in HIV-infected individuals were more than 3 times higher than the general population [2], indeed reflecting unfortunately many restrictions experienced by HIV infected individuals during daily life.
Guiding a transplantation procedure if no state of the art is available might benefit from utilizing JACIE guidelines, a system implemented to ensure quality and improve state-of-the-art transplantations. I.e., introduction of additional quality procedures such as an “alternative transplantation procedure” with a separate informed consent and quality controls are included in our JACIE-accredited transplantation program at the UMC Utrecht. A standard informed consent for biobanking (ethical approval) is applied for all allogeneic stem cell transplantation procedures and facilitates maximizing the acquired information regardless of the outcome of the transplantation. Multiple patients have now been transplanted with a combined haplo and cord blood protocol in Europe, while one patient received a CCR del32/32 unit at our center. The outcome of this transplantation will be reported separately.
Conclusions
CCR5-del32/del32 donors are clearly the preferential option for patients with hematological malignancies and HIV co-infection. Extending the pool of CCR5-del32/del32 cord blood units is urgently needed. Combined haplo- and cord blood transplantation or single cord blood expansion protocols can become platforms for patients with hematological malignancies and HIV co-infection. However, HSCT puts the patient at a high risk, thus cannot be considered as solution for a functional cure of HIV. Beside curing a patient of HIV, this type of transplantation allows studying HIV repertoires which is important to develop mechanisms of cure for HIV.
Our and other cases started a very interesting international collaboration; the “epistem-project”: http://www.epistem-project.org, funded by AMFAR, a European Project to guide the therapy and investigate the potential for HIV cure by allogeneic stem cell transplantation. Its areas of investigations are as follows: (1) Increasing the number of suitable del32/del32 CB units by testing systematically European cord blood banks; (2) Providing advice during treatment (donor choice, ethical aspects, drug-drug interaction, etc.); (3) Improving the understanding of biology for HIV cure by providing a standardized sampling protocol which will allow comparable studies of viral reservoirs, characterization of infecting virus, and evaluation of immune responses after allo SCT between different transplantation centers.
References
- Hutter G, Nowak D, Mossner M, Ganepola S, Mussig A, Allers K, Schneider T, Hofmann J, Kucherer C, Blau O. Long-term control of HIV by CCR5 Delta32/Delta32 stem-cell transplantation. N Engl J Med 2009; 360: 692-8.
- Keiser O, Spoerri A, Brinkhof MW, Hasse B, Gayet-Ageron A, Tissot F, Christen A, Battegay M, Schmid P, Bernasconi E et al. Suicide in HIV-infected individuals and the general population in Switzerland, 1988-2008. Am J Psychiat 2010; 167: 143-50.
- Kordelas L, Verheyen J, Beelen DW, Horn PA, Heinold A, Kaiser R, Trenschel R, Schadendorf D, Dittmer U, Esser S et al. Shift of HIV tropism in stem-cell transplantation with CCR5 Delta32 mutation. New Engl J Med 2014; 371: 880-2.
- Kwon M, Balsalobre P, Serrano D, Perez CA, Buno I, Anguita J, Gayoso J, ez-Martin JL. Single Cord Blood Combined with HLA-Mismatched Third Party Donor Cells: Comparable Results to Matched Unrelated Donor Transplantation in High-Risk Patients with Hematologic Disorders. Biol Blood Marrow Transplant 2013; 19(1): 143-9.
- Liu H, Rich ES, Godley L, Odenike O, Joseph L, Marino S, Kline J, Nguyen V, Cunningham, J, Larson RA et al. Reduced-intensity conditioning with combined haploidentical and cord blood transplantation results in rapid engraftment, low GVHD, and durable remissions. Blood 2011; 118: 6438-45.
- Magro E, Regidor C, Cabrera R, Sanjuán I, Forès R, Garcia-Marco JA, Ruiz E, Gil S, Bautista G, Millán I, Madrigal A, Fernandez MN. Early hematopoietic recovery after single unit unrelated cord blood transplantation in adults supported by co-infusion of mobilized stem cells from a third party donor. Haematologica 2006; 91(5): 640-8.
- Petz LD, Redei I, Bryson Y, Regan D, Kurtzberg J, Shpall E, Gutman J, Querol S, Clark P, Tonai R et al. Hematopoietic cell transplantation with cord blood for cure of HIV infections. Biol Blood Marrow Transplant 2013; 19: 393-7.
- Verheyen J, Esser S, Kordelas L. More on shift of HIV tropism in stem-cell transplantation with CCR5 delta32/delta32 mutation. New Engl J Med 2014; 371: 2438.
- Wagner JE, Jr, Eapen M, Carter S, Wang Y, Schultz KR, Wal, DA, Bunin N, Delaney C, Haut P, Margolis D et al. One-unit versus two-unit cord-blood transplantation for hematologic cancers. New Engl J Med 2014; 371: 1685-94.
In February 2007, Hütter et al performed an allogeneic hematopoietic stem cell transplantation (HSCT) in a patient with acute myeloid leukemia (AML) who has been co-infected with HIV. The HSCT was performed using peripheral blood stem cells from an adult donor. The patient, known as “The Berlin Patient”, was cured of HIV as well as his AML [1]. This “magic” cure inspired many hematologists to more thoroughly investigate the prospects of cure for patients suffering from leukemia and co-infection with of HIV.
The rationale for such treatment is based on the assumption that (A) HIV primarily infects the hematopoetic system; and (B) that an HSCT replaces the infected hematopoiesis with an un-infected bone marrow. Uninfected littermates of the new bone marrow will then again repopulate the host in all different compartments of the body. However, a major challenge remains the reinfection of donor cells after HSCT. In particular typical reservoirs of HIV like monocytes are usually replaced not until months after HSCT through the new donor. Persisting host monocytes are consequently a source for HIV and threat for reinfection of the new donor. A graft-versus-host disease (GVHD) may therefore be an essential factor for eliminating residual HIV reservoirs after HSCT.
To prevent HIV reinfection of the new donor in the patients, one may use a donor with a natural deletion in CCR5, which blocks entry for the most common HIV strain. This genetic trait is found in <1% of general population. Therefore, a search for patient two has been challenging. In this case, the patient needs to have an indication for an HSCT, to be co-infected with HIV, and HIV must selectively be restricted to the receptor CCR5. The frequency of CCR5-del32/del32 donors is usually ≤1% in Caucasians and much less in other ethnic groups. Hence, the transplant patients usually have only a small number of available donors. When adult donors are used, a very close HLA match with the patient is required (7-8/8). Due to these limitations, the second patient was acquired only many years later in 2014 [3,8], unfortunately, with subsequent failure in terms of HIV control, most likely due to the fact that the virus already used another entry port like CXCR4.
Utilizing cord blood donors in the last decade as standard donor for many transplantations opened an avenue to a new potential source of donors for HIV infected patients. Firstly, although not well understood, a lower HLA matching between cord blood units and patients is sufficient for a good outcome of HSCT [9]. These less restricted matching criteria increase substantially the chance to find a donor in the very same genetic pool. Vice versa, if a cord blood unit with a unique trait like CCR5-del32/del32 is identified, it can be theoretically used for more patients. Increasing the pool of an inventory of CCR5-del32/del32 umbilical cord blood units will therefore provide as off-the-shelf product a rapid and greatly improved probability of finding an appropriately HLA-matched donor with an adequate cell dose for a patient with HIV infection with CCR5 tropism and in need of an HSCT. A theoretic inventory for a minimal required number del32/del32 CB units was performed recently [7] showing that it is very likely to identify one HLA matched homozygous CCR5-del32 cord blood unit for a patient with appropriate clinical indications for HSCT. However, stem cells per cord blood unit are small and one unit is frequently not sufficient to appropriately engraft an adult patient in time. Therefore, cord blood transplantations in adults utilize usually two cord blood units in order to overcome the limitation of little numbers in stem cells per cord blood unit. As simplistic and smart this strategy seems to be at a first sight for patients without co-infection of HIV, as problematic it is for patients with HIV: It is very unlikely to find two CCR5-del32 cord blood units and outgrowth of the CCR5-del32 unit would be then left to chance. One solution might come from combining cord blood and haplo transplantation. The haplo product, once deeply T cell depleted can be considered in this strategy as a bridge to long term engraftment of the cord blood unit as pioneered by Spanish colleagues [6]. Therapeutic prospects of the combined haplo cord blood transplantation include a safer and more rapid engraftment of neutrophils, thus providing better protection against infections. Combining haplo and cord blood donors may be justified even with a suitable donor for defined indications. Others showed that the combined haplo and cord blood transplantation have an acceptable safety profile which is comparable to MUD donors [4, 5]. However, the most recent development of single cord blood expansion protocols might provide a new avenue to pursue such transplantations with only one CCR5-del32 cord blood unit.
Beside a careful evaluation of donor choices an additional important consideration arises from the perspective of HIV positive patients: Although HIV infection is nowadays regarded as a chronic disease in the era of effective HAART, quality of life of HIV-infected patients is usually substantially impaired. A study examining the frequency of suicides in HIV positive patients from 1988 to 2008 followed 15,275 HIV-infected patients up for a median duration of 4.7 years. Suicide rates in HIV-infected individuals were more than 3 times higher than the general population [2], indeed reflecting unfortunately many restrictions experienced by HIV infected individuals during daily life.
Guiding a transplantation procedure if no state of the art is available might benefit from utilizing JACIE guidelines, a system implemented to ensure quality and improve state-of-the-art transplantations. I.e., introduction of additional quality procedures such as an “alternative transplantation procedure” with a separate informed consent and quality controls are included in our JACIE-accredited transplantation program at the UMC Utrecht. A standard informed consent for biobanking (ethical approval) is applied for all allogeneic stem cell transplantation procedures and facilitates maximizing the acquired information regardless of the outcome of the transplantation. Multiple patients have now been transplanted with a combined haplo and cord blood protocol in Europe, while one patient received a CCR del32/32 unit at our center. The outcome of this transplantation will be reported separately.
Conclusions
CCR5-del32/del32 donors are clearly the preferential option for patients with hematological malignancies and HIV co-infection. Extending the pool of CCR5-del32/del32 cord blood units is urgently needed. Combined haplo- and cord blood transplantation or single cord blood expansion protocols can become platforms for patients with hematological malignancies and HIV co-infection. However, HSCT puts the patient at a high risk, thus cannot be considered as solution for a functional cure of HIV. Beside curing a patient of HIV, this type of transplantation allows studying HIV repertoires which is important to develop mechanisms of cure for HIV.
Our and other cases started a very interesting international collaboration; the “epistem-project”: http://www.epistem-project.org, funded by AMFAR, a European Project to guide the therapy and investigate the potential for HIV cure by allogeneic stem cell transplantation. Its areas of investigations are as follows: (1) Increasing the number of suitable del32/del32 CB units by testing systematically European cord blood banks; (2) Providing advice during treatment (donor choice, ethical aspects, drug-drug interaction, etc.); (3) Improving the understanding of biology for HIV cure by providing a standardized sampling protocol which will allow comparable studies of viral reservoirs, characterization of infecting virus, and evaluation of immune responses after allo SCT between different transplantation centers.
References
- Hutter G, Nowak D, Mossner M, Ganepola S, Mussig A, Allers K, Schneider T, Hofmann J, Kucherer C, Blau O. Long-term control of HIV by CCR5 Delta32/Delta32 stem-cell transplantation. N Engl J Med 2009; 360: 692-8.
- Keiser O, Spoerri A, Brinkhof MW, Hasse B, Gayet-Ageron A, Tissot F, Christen A, Battegay M, Schmid P, Bernasconi E et al. Suicide in HIV-infected individuals and the general population in Switzerland, 1988-2008. Am J Psychiat 2010; 167: 143-50.
- Kordelas L, Verheyen J, Beelen DW, Horn PA, Heinold A, Kaiser R, Trenschel R, Schadendorf D, Dittmer U, Esser S et al. Shift of HIV tropism in stem-cell transplantation with CCR5 Delta32 mutation. New Engl J Med 2014; 371: 880-2.
- Kwon M, Balsalobre P, Serrano D, Perez CA, Buno I, Anguita J, Gayoso J, ez-Martin JL. Single Cord Blood Combined with HLA-Mismatched Third Party Donor Cells: Comparable Results to Matched Unrelated Donor Transplantation in High-Risk Patients with Hematologic Disorders. Biol Blood Marrow Transplant 2013; 19(1): 143-9.
- Liu H, Rich ES, Godley L, Odenike O, Joseph L, Marino S, Kline J, Nguyen V, Cunningham, J, Larson RA et al. Reduced-intensity conditioning with combined haploidentical and cord blood transplantation results in rapid engraftment, low GVHD, and durable remissions. Blood 2011; 118: 6438-45.
- Magro E, Regidor C, Cabrera R, Sanjuán I, Forès R, Garcia-Marco JA, Ruiz E, Gil S, Bautista G, Millán I, Madrigal A, Fernandez MN. Early hematopoietic recovery after single unit unrelated cord blood transplantation in adults supported by co-infusion of mobilized stem cells from a third party donor. Haematologica 2006; 91(5): 640-8.
- Petz LD, Redei I, Bryson Y, Regan D, Kurtzberg J, Shpall E, Gutman J, Querol S, Clark P, Tonai R et al. Hematopoietic cell transplantation with cord blood for cure of HIV infections. Biol Blood Marrow Transplant 2013; 19: 393-7.
- Verheyen J, Esser S, Kordelas L. More on shift of HIV tropism in stem-cell transplantation with CCR5 delta32/delta32 mutation. New Engl J Med 2014; 371: 2438.
- Wagner JE, Jr, Eapen M, Carter S, Wang Y, Schultz KR, Wal, DA, Bunin N, Delaney C, Haut P, Margolis D et al. One-unit versus two-unit cord-blood transplantation for hematologic cancers. New Engl J Med 2014; 371: 1685-94.
Юрген Кубалл
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "535" ["VALUE"]=> array(2) { ["TEXT"]=> string(158) "<p class="Autor_place_work-Rus">Университетский медицинский центр, Утрехт, Нидерланды</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(136) "Университетский медицинский центр, Утрехт, Нидерланды
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "536" ["VALUE"]=> array(2) { ["TEXT"]=> string(1122) "<h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1078) "Резюме
В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "537" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-62-65" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-62-65" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "538" ["VALUE"]=> array(2) { ["TEXT"]=> string(58) "<p class="Autor">Jürgen Kuball </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(36) "Jürgen Kuball
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "539" ["VALUE"]=> array(2) { ["TEXT"]=> string(101) "<p class="Autor_place_work">University Medical Center, Utrecht, Netherlands</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(79) "University Medical Center, Utrecht, Netherlands
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "540" ["VALUE"]=> string(62) "Cord blood as natural donor source for curing HIV and Leukemia" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(62) "Cord blood as natural donor source for curing HIV and Leukemia" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1016" ["VALUE"]=> array(2) { ["TEXT"]=> string(14465) "<p>Подобное лечение основано на том, что, во-первых, ВИЧ первично поражает систему гемопоэза и, во-вторых, что при ГТСК происходит замещение инфицированных гемопоэтических клеток неинфицированным костным мозгом. Незараженное потомство нового костного мозга затем заселяет организм пациента в различных зонах организма. Однако основной проблемой остается неинфекция донорских клеток после ТГСК. В частности, типичные «резервуары» ВИЧ, такие, как популяции моноцитов, обычно замещаются донорскими клетками лишь спустя месяцы после ТГСК. Персистирующие донорские моноциты впоследствии являются потенциальным источником ВИЧ-реинфекции клеток донора. Поэтому реакция «трансплантат против хозяина» может быть существенным фактором устранения остаточных клеток-носителей ВИЧ после ТГСК.</p> <p>Чтобы предотвратить реинфекцию ВИЧ донорских клеток в организме пациента, можно привлечь донора с естественной делецией гена CCR5, при которой блокируется вход в клетку наиболее частого типа ВИЧ. Этотгенетический признак имеется у <1% населения. Поэтому поиск такого донора затруднителен. В данном случае у пациента должны быть серьезные показания к ТГСК , у него должна быть также ВИЧ-инфекция, и заражение вирусом должно зависеть от рецептора CCR5. Частота мутации <em>CCR5</em>-del32/del32 среди европейцев ≤1% и еще ниже – в других этнических группах. Таким образом, подобные больные обычно имеют малое количество доступных доноров. Если используют материал от взрослых доноров, то требуется очень близкое совпадение по HLA (7-8/8). Из-за этих ограничений, второй пациент для аналогичной ТГСК был найден лишь через несколько лет, в 2014 г. (Kordelas et al., 2014; Verheyen et al., 2014) К сожалению, результат ТГСК был негативным из-за рецидива ВИЧ-инфекции. Скорее всего, реинфекция реализовалась через другой рецептор, например, CXCR4.</p> <p>Стволовые клетки из пуповинной крови (ПСК) в качестве стандартного донорского материала для ТГСК, стали в последнее десятилетие новым потенциальным источником гемопоэтических клеток для ВИЧ-инфицированных больных. Прежде всего, для хорошего исхода ТГСК здесь достаточно меньшего совпадения по HLA между ПСК и клетками пациента (Wagner et al., 2014). Эти менее строгие критерии подбора существенно повышают шансы найти донора в том же генетическом пуле. С другой стороны, если выявлена партия ПСК с уникальным признаком, вроде <em>CCR5</em>-del32/del32, то она теоретически может быть использована для нескольких больных. Поэтому увеличение пула образцов ПСК с наличием <em>CCR5</em>-del32/del32 обеспечит появление трансплантатов для того, чтобы повысить вероятность более быстрого и качественного подбора HLA-совместимого донора для больного с ВИЧ-инфекцией, если эта инфекция имеет тропизм к CCR5, и больному требуется ТГСК. Теоретический расчет минимального числа доз ПСК с del32/del32 проводился недавно (Petz et al., 2013), и было показана высокая вероятность нахождения образца, гомозиготного по <em>CCR5</em>-del32 и HLA-совместимого с пациентом, имеющим клинические показания к ТГСК. Однако число стволовых клеток на 1 дозу ПСК весьма мало, и одной дозы часто недостаточно для своевременного приживления у взрослого пациента. Поэтому ТГСК у взрослых лиц требуют обычно 2 доз ПСК, чтобы преодолеть ограничения малых доз ПСК в пуповинной крови. Хотя эта стратегия кажется простой и удобной для пациентов без ВИЧ-инфекции, ее применение проблематично у больных с ВИЧ-инфекцией. Очень маловероятен подбор двух доз ПСК с мутацией <em>CCR5</em>-del32, и преимущественный рост клеток с <em>CCR5</em>-del32 будет зависеть от случая. Решением вопроса может быть сочетание ТГСК пуповинных клеток и гаплоидентичной ТГСК. Последний, при высоком уровне его очистки от Т-клеток, может рассматриваться в качестве «мостика» к долгосрочному приживлению ПСК, как впервые показали испанские коллеги (Magro E et al., 2006). Лечебные перспективы комбинированной трансплантации гаплоидентичных и пуповинных клеток касаются более безопасного и быстрого приживления нейтрофилов, что дает лучшую защиту от инфекций. Такой вариант ТГСК может быть обоснован даже при наличии пригодного донора по основным показаниям. Некоторые авторы показали, что комбинированная гапло-ТГСК и пересадка ПСК имеет приемлемый уровень безопасности, сравнимый с ТГСК от неродственных доноров (Kwon et al., 2012; Liu et al., 2011). Однако новейшие протоколы размножения пуповинных стволовых клеток могут проложить новый путь для осуществления таких ТГСК при наличии лишь одной дозы ПСК с <em>CCR5</em>-del32. </p> <p>Кроме тщательной оценки выбора доноров, возникает еще одно важное соображение, касающееся будущего ВИЧ-позитивныъ больных. Хотя ВИЧ-инфекция сейчас рассматривается как хроническое заболевание в эру эффективной специфической терапии, качество жизни ВИЧ-инфицированных больных обычно существенно нарушено. Исследование частоты самоубийств среди ВИЧ-положительных больных с 1988 по 2008 гг. включало 15275 ВИЧ-инфицированных лиц в длительные сроки (медиана – 4,7 г.) Частота суицидов среди этого контингента была более чем в 3 раза выше, нежели в населении в целом (Keiser et al., 2010), отражая, на самом деле, влияние многих ограничений, касающихся ВИЧ-инфицированных лиц в повседневной жизни. </p> <p>Проведению трансплантаций при отсутствии должного опыта в этой области может помочь использование рекомендаций JACIE– системы, предназначенной для обеспечения качества и улучшения состояния знаний по данному вопросу. Таким образом, введение дополнительных качественных категорий, таких, как «альтернативная процедура трансплантации» с отдельным информированным согласием и контролем качества, включены в нашу трансплантационную программу, аккредитованную JACIE, в Университетской клинике Утрехта. Стандартное информированное согласие для биобанкирования (этическое одобрение) применяется для всех процедур алло-ТГСК и обеспечивает максимум получаемой информации независимо от ее исхода. Многие пациенты в Европе, теперь получают трансплантацию по комбинированному протоколу с гапло- и пуповинной ТГСК, в т.ч. один пациент получил трансплантацию клеток с CCR del32/32 в нашем центре. Об исходе этой ТГСК будет сообщено дополнительно.. </p> <h2>Выводы </h2> <p>Доноры с мутацией<em> CCR5</em>-del32/del32, очевидно, являются предпочтительными для пациентов с гематологическими новообразованиями и сопутствующей ВИЧ-инфекцией. Настоятельно необходимо расширение пула образцов пуповинной крови с<em> CCR5</em>-del32/del32. Комбинированная трансплантация гаплоидентичных и пуповинных стволовых клеток, или протоколы с размножением стволовых клеток из одного образца пуповинной крови могут стать основой для лечения онкогематологических больных с ВИЧ-инфекцией. Однако ТГСК представляет собой высокий риск для больного и поэтому не может рассматриваться как оптимальное решение для функционального излечения ВИЧ-инфекции. Наряду с излечением ВИЧ-инфицированного больного, этот тип ТГСК позволяет исследование вариантов ВИЧ, важных для разработки механизмов лечения ВИЧ-инфекции. С нашего и других клинических случаев началось очень интересное международное сотрудничество – проект Epistem (<a href="http://www.epistem-project.org">http://www.epistem-project.org</a>), основанный AMFAR – европейский проект проведения терапии и изучения потенциала излечения ВИЧ-инфекции путем аллогенной трансплантации гемопоэтических клеток. Областями исследований являются: (1) Повышение числа пригодных для ТГСК образцов ПСК с del32/del32, путем систематического тестирования европейских банков пуповинной крови; (2) Выдача советов в процессе лечения (выбор донора, этические аспекты, взаимодействия между препаратами и т.д.); (3) Улучшение понимания биологических механизмов излечения ВИЧ-инфекции путем выработки стандартизированного клинического протокола, который обеспечит сравнимость исследований вирусных резервуаров, характеристик инфицирующего вируса и оценки иммунного ответа после алло-ТГСК по различным трансплантационным центрам</p> " ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(14247) "Подобное лечение основано на том, что, во-первых, ВИЧ первично поражает систему гемопоэза и, во-вторых, что при ГТСК происходит замещение инфицированных гемопоэтических клеток неинфицированным костным мозгом. Незараженное потомство нового костного мозга затем заселяет организм пациента в различных зонах организма. Однако основной проблемой остается неинфекция донорских клеток после ТГСК. В частности, типичные «резервуары» ВИЧ, такие, как популяции моноцитов, обычно замещаются донорскими клетками лишь спустя месяцы после ТГСК. Персистирующие донорские моноциты впоследствии являются потенциальным источником ВИЧ-реинфекции клеток донора. Поэтому реакция «трансплантат против хозяина» может быть существенным фактором устранения остаточных клеток-носителей ВИЧ после ТГСК.
Чтобы предотвратить реинфекцию ВИЧ донорских клеток в организме пациента, можно привлечь донора с естественной делецией гена CCR5, при которой блокируется вход в клетку наиболее частого типа ВИЧ. Этотгенетический признак имеется у <1% населения. Поэтому поиск такого донора затруднителен. В данном случае у пациента должны быть серьезные показания к ТГСК , у него должна быть также ВИЧ-инфекция, и заражение вирусом должно зависеть от рецептора CCR5. Частота мутации CCR5-del32/del32 среди европейцев ≤1% и еще ниже – в других этнических группах. Таким образом, подобные больные обычно имеют малое количество доступных доноров. Если используют материал от взрослых доноров, то требуется очень близкое совпадение по HLA (7-8/8). Из-за этих ограничений, второй пациент для аналогичной ТГСК был найден лишь через несколько лет, в 2014 г. (Kordelas et al., 2014; Verheyen et al., 2014) К сожалению, результат ТГСК был негативным из-за рецидива ВИЧ-инфекции. Скорее всего, реинфекция реализовалась через другой рецептор, например, CXCR4.
Стволовые клетки из пуповинной крови (ПСК) в качестве стандартного донорского материала для ТГСК, стали в последнее десятилетие новым потенциальным источником гемопоэтических клеток для ВИЧ-инфицированных больных. Прежде всего, для хорошего исхода ТГСК здесь достаточно меньшего совпадения по HLA между ПСК и клетками пациента (Wagner et al., 2014). Эти менее строгие критерии подбора существенно повышают шансы найти донора в том же генетическом пуле. С другой стороны, если выявлена партия ПСК с уникальным признаком, вроде CCR5-del32/del32, то она теоретически может быть использована для нескольких больных. Поэтому увеличение пула образцов ПСК с наличием CCR5-del32/del32 обеспечит появление трансплантатов для того, чтобы повысить вероятность более быстрого и качественного подбора HLA-совместимого донора для больного с ВИЧ-инфекцией, если эта инфекция имеет тропизм к CCR5, и больному требуется ТГСК. Теоретический расчет минимального числа доз ПСК с del32/del32 проводился недавно (Petz et al., 2013), и было показана высокая вероятность нахождения образца, гомозиготного по CCR5-del32 и HLA-совместимого с пациентом, имеющим клинические показания к ТГСК. Однако число стволовых клеток на 1 дозу ПСК весьма мало, и одной дозы часто недостаточно для своевременного приживления у взрослого пациента. Поэтому ТГСК у взрослых лиц требуют обычно 2 доз ПСК, чтобы преодолеть ограничения малых доз ПСК в пуповинной крови. Хотя эта стратегия кажется простой и удобной для пациентов без ВИЧ-инфекции, ее применение проблематично у больных с ВИЧ-инфекцией. Очень маловероятен подбор двух доз ПСК с мутацией CCR5-del32, и преимущественный рост клеток с CCR5-del32 будет зависеть от случая. Решением вопроса может быть сочетание ТГСК пуповинных клеток и гаплоидентичной ТГСК. Последний, при высоком уровне его очистки от Т-клеток, может рассматриваться в качестве «мостика» к долгосрочному приживлению ПСК, как впервые показали испанские коллеги (Magro E et al., 2006). Лечебные перспективы комбинированной трансплантации гаплоидентичных и пуповинных клеток касаются более безопасного и быстрого приживления нейтрофилов, что дает лучшую защиту от инфекций. Такой вариант ТГСК может быть обоснован даже при наличии пригодного донора по основным показаниям. Некоторые авторы показали, что комбинированная гапло-ТГСК и пересадка ПСК имеет приемлемый уровень безопасности, сравнимый с ТГСК от неродственных доноров (Kwon et al., 2012; Liu et al., 2011). Однако новейшие протоколы размножения пуповинных стволовых клеток могут проложить новый путь для осуществления таких ТГСК при наличии лишь одной дозы ПСК с CCR5-del32.
Кроме тщательной оценки выбора доноров, возникает еще одно важное соображение, касающееся будущего ВИЧ-позитивныъ больных. Хотя ВИЧ-инфекция сейчас рассматривается как хроническое заболевание в эру эффективной специфической терапии, качество жизни ВИЧ-инфицированных больных обычно существенно нарушено. Исследование частоты самоубийств среди ВИЧ-положительных больных с 1988 по 2008 гг. включало 15275 ВИЧ-инфицированных лиц в длительные сроки (медиана – 4,7 г.) Частота суицидов среди этого контингента была более чем в 3 раза выше, нежели в населении в целом (Keiser et al., 2010), отражая, на самом деле, влияние многих ограничений, касающихся ВИЧ-инфицированных лиц в повседневной жизни.
Проведению трансплантаций при отсутствии должного опыта в этой области может помочь использование рекомендаций JACIE– системы, предназначенной для обеспечения качества и улучшения состояния знаний по данному вопросу. Таким образом, введение дополнительных качественных категорий, таких, как «альтернативная процедура трансплантации» с отдельным информированным согласием и контролем качества, включены в нашу трансплантационную программу, аккредитованную JACIE, в Университетской клинике Утрехта. Стандартное информированное согласие для биобанкирования (этическое одобрение) применяется для всех процедур алло-ТГСК и обеспечивает максимум получаемой информации независимо от ее исхода. Многие пациенты в Европе, теперь получают трансплантацию по комбинированному протоколу с гапло- и пуповинной ТГСК, в т.ч. один пациент получил трансплантацию клеток с CCR del32/32 в нашем центре. Об исходе этой ТГСК будет сообщено дополнительно..
Выводы
Доноры с мутацией CCR5-del32/del32, очевидно, являются предпочтительными для пациентов с гематологическими новообразованиями и сопутствующей ВИЧ-инфекцией. Настоятельно необходимо расширение пула образцов пуповинной крови с CCR5-del32/del32. Комбинированная трансплантация гаплоидентичных и пуповинных стволовых клеток, или протоколы с размножением стволовых клеток из одного образца пуповинной крови могут стать основой для лечения онкогематологических больных с ВИЧ-инфекцией. Однако ТГСК представляет собой высокий риск для больного и поэтому не может рассматриваться как оптимальное решение для функционального излечения ВИЧ-инфекции. Наряду с излечением ВИЧ-инфицированного больного, этот тип ТГСК позволяет исследование вариантов ВИЧ, важных для разработки механизмов лечения ВИЧ-инфекции. С нашего и других клинических случаев началось очень интересное международное сотрудничество – проект Epistem (http://www.epistem-project.org), основанный AMFAR – европейский проект проведения терапии и изучения потенциала излечения ВИЧ-инфекции путем аллогенной трансплантации гемопоэтических клеток. Областями исследований являются: (1) Повышение числа пригодных для ТГСК образцов ПСК с del32/del32, путем систематического тестирования европейских банков пуповинной крови; (2) Выдача советов в процессе лечения (выбор донора, этические аспекты, взаимодействия между препаратами и т.д.); (3) Улучшение понимания биологических механизмов излечения ВИЧ-инфекции путем выработки стандартизированного клинического протокола, который обеспечит сравнимость исследований вирусных резервуаров, характеристик инфицирующего вируса и оценки иммунного ответа после алло-ТГСК по различным трансплантационным центрам
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1245" ["VALUE"]=> string(2) "24" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "24" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1246" ["VALUE"]=> string(2) "25" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "25" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(14) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "538" ["VALUE"]=> array(2) { ["TEXT"]=> string(58) "<p class="Autor">Jürgen Kuball </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(36) "Jürgen Kuball
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(36) "Jürgen Kuball
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "537" ["VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-62-65" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-62-65" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(35) "10.18620/1866-8836-2015-4-1-2-62-65" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "540" ["VALUE"]=> string(62) "Cord blood as natural donor source for curing HIV and Leukemia" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(62) "Cord blood as natural donor source for curing HIV and Leukemia" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(62) "Cord blood as natural donor source for curing HIV and Leukemia" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "539" ["VALUE"]=> array(2) { ["TEXT"]=> string(101) "<p class="Autor_place_work">University Medical Center, Utrecht, Netherlands</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(79) "University Medical Center, Utrecht, Netherlands
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(79) "University Medical Center, Utrecht, Netherlands
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(3) "533" } ["VALUE"]=> array(1) { [0]=> string(2) "93" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(2) "93" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Jürgen Kuball" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "534" ["VALUE"]=> array(2) { ["TEXT"]=> string(93) "<p class="Autor_Rus" lang="ru-RU">Юрген Кубалл</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(61) "Юрген Кубалл
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(61) "Юрген Кубалл
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "530" ["VALUE"]=> string(19) "06.04.2015 16:57:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "06.04.2015 16:57:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "06.04.2015 16:57:00" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "531" ["VALUE"]=> string(19) "05.06.2015 16:57:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "05.06.2015 16:57:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "05.06.2015 16:57:00" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "911" ["VALUE"]=> string(19) "08.09.2015 17:36:00" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(19) "08.09.2015 17:36:00" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(24) "08.09.2015 17:36:00" } ["KEYWORDS"]=> array(38) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(4) { [0]=> string(4) "1241" [1]=> string(4) "1242" [2]=> string(4) "1243" [3]=> string(4) "1244" } ["VALUE"]=> array(4) { [0]=> string(2) "44" [1]=> string(2) "94" [2]=> string(2) "95" [3]=> string(2) "58" } ["DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(4) { [0]=> string(2) "44" [1]=> string(2) "94" [2]=> string(2) "95" [3]=> string(2) "58" } ["~DESCRIPTION"]=> array(4) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" } ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(4) { [0]=> string(49) "ВИЧ" [1]=> string(57) "лейкозы" [2]=> string(87) "клетки пуповинной крови" [3]=> string(103) "трансплантация стволовых клеток" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "532" ["VALUE"]=> string(2) "93" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(2) "93" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Jürgen Kuball" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "536" ["VALUE"]=> array(2) { ["TEXT"]=> string(1122) "<h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией. </p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1078) "Резюме
В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией.
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1078) "Резюме
В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией.
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(3) "535" ["VALUE"]=> array(2) { ["TEXT"]=> string(158) "<p class="Autor_place_work-Rus">Университетский медицинский центр, Утрехт, Нидерланды</p>" ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(136) "Университетский медицинский центр, Утрехт, Нидерланды
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(136) "Университетский медицинский центр, Утрехт, Нидерланды
" } ["FULL_TEXT_RU"]=> array(37) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(4) "1016" ["VALUE"]=> array(2) { ["TEXT"]=> string(14465) "<p>Подобное лечение основано на том, что, во-первых, ВИЧ первично поражает систему гемопоэза и, во-вторых, что при ГТСК происходит замещение инфицированных гемопоэтических клеток неинфицированным костным мозгом. Незараженное потомство нового костного мозга затем заселяет организм пациента в различных зонах организма. Однако основной проблемой остается неинфекция донорских клеток после ТГСК. В частности, типичные «резервуары» ВИЧ, такие, как популяции моноцитов, обычно замещаются донорскими клетками лишь спустя месяцы после ТГСК. Персистирующие донорские моноциты впоследствии являются потенциальным источником ВИЧ-реинфекции клеток донора. Поэтому реакция «трансплантат против хозяина» может быть существенным фактором устранения остаточных клеток-носителей ВИЧ после ТГСК.</p> <p>Чтобы предотвратить реинфекцию ВИЧ донорских клеток в организме пациента, можно привлечь донора с естественной делецией гена CCR5, при которой блокируется вход в клетку наиболее частого типа ВИЧ. Этотгенетический признак имеется у <1% населения. Поэтому поиск такого донора затруднителен. В данном случае у пациента должны быть серьезные показания к ТГСК , у него должна быть также ВИЧ-инфекция, и заражение вирусом должно зависеть от рецептора CCR5. Частота мутации <em>CCR5</em>-del32/del32 среди европейцев ≤1% и еще ниже – в других этнических группах. Таким образом, подобные больные обычно имеют малое количество доступных доноров. Если используют материал от взрослых доноров, то требуется очень близкое совпадение по HLA (7-8/8). Из-за этих ограничений, второй пациент для аналогичной ТГСК был найден лишь через несколько лет, в 2014 г. (Kordelas et al., 2014; Verheyen et al., 2014) К сожалению, результат ТГСК был негативным из-за рецидива ВИЧ-инфекции. Скорее всего, реинфекция реализовалась через другой рецептор, например, CXCR4.</p> <p>Стволовые клетки из пуповинной крови (ПСК) в качестве стандартного донорского материала для ТГСК, стали в последнее десятилетие новым потенциальным источником гемопоэтических клеток для ВИЧ-инфицированных больных. Прежде всего, для хорошего исхода ТГСК здесь достаточно меньшего совпадения по HLA между ПСК и клетками пациента (Wagner et al., 2014). Эти менее строгие критерии подбора существенно повышают шансы найти донора в том же генетическом пуле. С другой стороны, если выявлена партия ПСК с уникальным признаком, вроде <em>CCR5</em>-del32/del32, то она теоретически может быть использована для нескольких больных. Поэтому увеличение пула образцов ПСК с наличием <em>CCR5</em>-del32/del32 обеспечит появление трансплантатов для того, чтобы повысить вероятность более быстрого и качественного подбора HLA-совместимого донора для больного с ВИЧ-инфекцией, если эта инфекция имеет тропизм к CCR5, и больному требуется ТГСК. Теоретический расчет минимального числа доз ПСК с del32/del32 проводился недавно (Petz et al., 2013), и было показана высокая вероятность нахождения образца, гомозиготного по <em>CCR5</em>-del32 и HLA-совместимого с пациентом, имеющим клинические показания к ТГСК. Однако число стволовых клеток на 1 дозу ПСК весьма мало, и одной дозы часто недостаточно для своевременного приживления у взрослого пациента. Поэтому ТГСК у взрослых лиц требуют обычно 2 доз ПСК, чтобы преодолеть ограничения малых доз ПСК в пуповинной крови. Хотя эта стратегия кажется простой и удобной для пациентов без ВИЧ-инфекции, ее применение проблематично у больных с ВИЧ-инфекцией. Очень маловероятен подбор двух доз ПСК с мутацией <em>CCR5</em>-del32, и преимущественный рост клеток с <em>CCR5</em>-del32 будет зависеть от случая. Решением вопроса может быть сочетание ТГСК пуповинных клеток и гаплоидентичной ТГСК. Последний, при высоком уровне его очистки от Т-клеток, может рассматриваться в качестве «мостика» к долгосрочному приживлению ПСК, как впервые показали испанские коллеги (Magro E et al., 2006). Лечебные перспективы комбинированной трансплантации гаплоидентичных и пуповинных клеток касаются более безопасного и быстрого приживления нейтрофилов, что дает лучшую защиту от инфекций. Такой вариант ТГСК может быть обоснован даже при наличии пригодного донора по основным показаниям. Некоторые авторы показали, что комбинированная гапло-ТГСК и пересадка ПСК имеет приемлемый уровень безопасности, сравнимый с ТГСК от неродственных доноров (Kwon et al., 2012; Liu et al., 2011). Однако новейшие протоколы размножения пуповинных стволовых клеток могут проложить новый путь для осуществления таких ТГСК при наличии лишь одной дозы ПСК с <em>CCR5</em>-del32. </p> <p>Кроме тщательной оценки выбора доноров, возникает еще одно важное соображение, касающееся будущего ВИЧ-позитивныъ больных. Хотя ВИЧ-инфекция сейчас рассматривается как хроническое заболевание в эру эффективной специфической терапии, качество жизни ВИЧ-инфицированных больных обычно существенно нарушено. Исследование частоты самоубийств среди ВИЧ-положительных больных с 1988 по 2008 гг. включало 15275 ВИЧ-инфицированных лиц в длительные сроки (медиана – 4,7 г.) Частота суицидов среди этого контингента была более чем в 3 раза выше, нежели в населении в целом (Keiser et al., 2010), отражая, на самом деле, влияние многих ограничений, касающихся ВИЧ-инфицированных лиц в повседневной жизни. </p> <p>Проведению трансплантаций при отсутствии должного опыта в этой области может помочь использование рекомендаций JACIE– системы, предназначенной для обеспечения качества и улучшения состояния знаний по данному вопросу. Таким образом, введение дополнительных качественных категорий, таких, как «альтернативная процедура трансплантации» с отдельным информированным согласием и контролем качества, включены в нашу трансплантационную программу, аккредитованную JACIE, в Университетской клинике Утрехта. Стандартное информированное согласие для биобанкирования (этическое одобрение) применяется для всех процедур алло-ТГСК и обеспечивает максимум получаемой информации независимо от ее исхода. Многие пациенты в Европе, теперь получают трансплантацию по комбинированному протоколу с гапло- и пуповинной ТГСК, в т.ч. один пациент получил трансплантацию клеток с CCR del32/32 в нашем центре. Об исходе этой ТГСК будет сообщено дополнительно.. </p> <h2>Выводы </h2> <p>Доноры с мутацией<em> CCR5</em>-del32/del32, очевидно, являются предпочтительными для пациентов с гематологическими новообразованиями и сопутствующей ВИЧ-инфекцией. Настоятельно необходимо расширение пула образцов пуповинной крови с<em> CCR5</em>-del32/del32. Комбинированная трансплантация гаплоидентичных и пуповинных стволовых клеток, или протоколы с размножением стволовых клеток из одного образца пуповинной крови могут стать основой для лечения онкогематологических больных с ВИЧ-инфекцией. Однако ТГСК представляет собой высокий риск для больного и поэтому не может рассматриваться как оптимальное решение для функционального излечения ВИЧ-инфекции. Наряду с излечением ВИЧ-инфицированного больного, этот тип ТГСК позволяет исследование вариантов ВИЧ, важных для разработки механизмов лечения ВИЧ-инфекции. С нашего и других клинических случаев началось очень интересное международное сотрудничество – проект Epistem (<a href="http://www.epistem-project.org">http://www.epistem-project.org</a>), основанный AMFAR – европейский проект проведения терапии и изучения потенциала излечения ВИЧ-инфекции путем аллогенной трансплантации гемопоэтических клеток. Областями исследований являются: (1) Повышение числа пригодных для ТГСК образцов ПСК с del32/del32, путем систематического тестирования европейских банков пуповинной крови; (2) Выдача советов в процессе лечения (выбор донора, этические аспекты, взаимодействия между препаратами и т.д.); (3) Улучшение понимания биологических механизмов излечения ВИЧ-инфекции путем выработки стандартизированного клинического протокола, который обеспечит сравнимость исследований вирусных резервуаров, характеристик инфицирующего вируса и оценки иммунного ответа после алло-ТГСК по различным трансплантационным центрам</p> " ["TYPE"]=> string(4) "html" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(14247) "Подобное лечение основано на том, что, во-первых, ВИЧ первично поражает систему гемопоэза и, во-вторых, что при ГТСК происходит замещение инфицированных гемопоэтических клеток неинфицированным костным мозгом. Незараженное потомство нового костного мозга затем заселяет организм пациента в различных зонах организма. Однако основной проблемой остается неинфекция донорских клеток после ТГСК. В частности, типичные «резервуары» ВИЧ, такие, как популяции моноцитов, обычно замещаются донорскими клетками лишь спустя месяцы после ТГСК. Персистирующие донорские моноциты впоследствии являются потенциальным источником ВИЧ-реинфекции клеток донора. Поэтому реакция «трансплантат против хозяина» может быть существенным фактором устранения остаточных клеток-носителей ВИЧ после ТГСК.
Чтобы предотвратить реинфекцию ВИЧ донорских клеток в организме пациента, можно привлечь донора с естественной делецией гена CCR5, при которой блокируется вход в клетку наиболее частого типа ВИЧ. Этотгенетический признак имеется у <1% населения. Поэтому поиск такого донора затруднителен. В данном случае у пациента должны быть серьезные показания к ТГСК , у него должна быть также ВИЧ-инфекция, и заражение вирусом должно зависеть от рецептора CCR5. Частота мутации CCR5-del32/del32 среди европейцев ≤1% и еще ниже – в других этнических группах. Таким образом, подобные больные обычно имеют малое количество доступных доноров. Если используют материал от взрослых доноров, то требуется очень близкое совпадение по HLA (7-8/8). Из-за этих ограничений, второй пациент для аналогичной ТГСК был найден лишь через несколько лет, в 2014 г. (Kordelas et al., 2014; Verheyen et al., 2014) К сожалению, результат ТГСК был негативным из-за рецидива ВИЧ-инфекции. Скорее всего, реинфекция реализовалась через другой рецептор, например, CXCR4.
Стволовые клетки из пуповинной крови (ПСК) в качестве стандартного донорского материала для ТГСК, стали в последнее десятилетие новым потенциальным источником гемопоэтических клеток для ВИЧ-инфицированных больных. Прежде всего, для хорошего исхода ТГСК здесь достаточно меньшего совпадения по HLA между ПСК и клетками пациента (Wagner et al., 2014). Эти менее строгие критерии подбора существенно повышают шансы найти донора в том же генетическом пуле. С другой стороны, если выявлена партия ПСК с уникальным признаком, вроде CCR5-del32/del32, то она теоретически может быть использована для нескольких больных. Поэтому увеличение пула образцов ПСК с наличием CCR5-del32/del32 обеспечит появление трансплантатов для того, чтобы повысить вероятность более быстрого и качественного подбора HLA-совместимого донора для больного с ВИЧ-инфекцией, если эта инфекция имеет тропизм к CCR5, и больному требуется ТГСК. Теоретический расчет минимального числа доз ПСК с del32/del32 проводился недавно (Petz et al., 2013), и было показана высокая вероятность нахождения образца, гомозиготного по CCR5-del32 и HLA-совместимого с пациентом, имеющим клинические показания к ТГСК. Однако число стволовых клеток на 1 дозу ПСК весьма мало, и одной дозы часто недостаточно для своевременного приживления у взрослого пациента. Поэтому ТГСК у взрослых лиц требуют обычно 2 доз ПСК, чтобы преодолеть ограничения малых доз ПСК в пуповинной крови. Хотя эта стратегия кажется простой и удобной для пациентов без ВИЧ-инфекции, ее применение проблематично у больных с ВИЧ-инфекцией. Очень маловероятен подбор двух доз ПСК с мутацией CCR5-del32, и преимущественный рост клеток с CCR5-del32 будет зависеть от случая. Решением вопроса может быть сочетание ТГСК пуповинных клеток и гаплоидентичной ТГСК. Последний, при высоком уровне его очистки от Т-клеток, может рассматриваться в качестве «мостика» к долгосрочному приживлению ПСК, как впервые показали испанские коллеги (Magro E et al., 2006). Лечебные перспективы комбинированной трансплантации гаплоидентичных и пуповинных клеток касаются более безопасного и быстрого приживления нейтрофилов, что дает лучшую защиту от инфекций. Такой вариант ТГСК может быть обоснован даже при наличии пригодного донора по основным показаниям. Некоторые авторы показали, что комбинированная гапло-ТГСК и пересадка ПСК имеет приемлемый уровень безопасности, сравнимый с ТГСК от неродственных доноров (Kwon et al., 2012; Liu et al., 2011). Однако новейшие протоколы размножения пуповинных стволовых клеток могут проложить новый путь для осуществления таких ТГСК при наличии лишь одной дозы ПСК с CCR5-del32.
Кроме тщательной оценки выбора доноров, возникает еще одно важное соображение, касающееся будущего ВИЧ-позитивныъ больных. Хотя ВИЧ-инфекция сейчас рассматривается как хроническое заболевание в эру эффективной специфической терапии, качество жизни ВИЧ-инфицированных больных обычно существенно нарушено. Исследование частоты самоубийств среди ВИЧ-положительных больных с 1988 по 2008 гг. включало 15275 ВИЧ-инфицированных лиц в длительные сроки (медиана – 4,7 г.) Частота суицидов среди этого контингента была более чем в 3 раза выше, нежели в населении в целом (Keiser et al., 2010), отражая, на самом деле, влияние многих ограничений, касающихся ВИЧ-инфицированных лиц в повседневной жизни.
Проведению трансплантаций при отсутствии должного опыта в этой области может помочь использование рекомендаций JACIE– системы, предназначенной для обеспечения качества и улучшения состояния знаний по данному вопросу. Таким образом, введение дополнительных качественных категорий, таких, как «альтернативная процедура трансплантации» с отдельным информированным согласием и контролем качества, включены в нашу трансплантационную программу, аккредитованную JACIE, в Университетской клинике Утрехта. Стандартное информированное согласие для биобанкирования (этическое одобрение) применяется для всех процедур алло-ТГСК и обеспечивает максимум получаемой информации независимо от ее исхода. Многие пациенты в Европе, теперь получают трансплантацию по комбинированному протоколу с гапло- и пуповинной ТГСК, в т.ч. один пациент получил трансплантацию клеток с CCR del32/32 в нашем центре. Об исходе этой ТГСК будет сообщено дополнительно..
Выводы
Доноры с мутацией CCR5-del32/del32, очевидно, являются предпочтительными для пациентов с гематологическими новообразованиями и сопутствующей ВИЧ-инфекцией. Настоятельно необходимо расширение пула образцов пуповинной крови с CCR5-del32/del32. Комбинированная трансплантация гаплоидентичных и пуповинных стволовых клеток, или протоколы с размножением стволовых клеток из одного образца пуповинной крови могут стать основой для лечения онкогематологических больных с ВИЧ-инфекцией. Однако ТГСК представляет собой высокий риск для больного и поэтому не может рассматриваться как оптимальное решение для функционального излечения ВИЧ-инфекции. Наряду с излечением ВИЧ-инфицированного больного, этот тип ТГСК позволяет исследование вариантов ВИЧ, важных для разработки механизмов лечения ВИЧ-инфекции. С нашего и других клинических случаев началось очень интересное международное сотрудничество – проект Epistem (http://www.epistem-project.org), основанный AMFAR – европейский проект проведения терапии и изучения потенциала излечения ВИЧ-инфекции путем аллогенной трансплантации гемопоэтических клеток. Областями исследований являются: (1) Повышение числа пригодных для ТГСК образцов ПСК с del32/del32, путем систематического тестирования европейских банков пуповинной крови; (2) Выдача советов в процессе лечения (выбор донора, этические аспекты, взаимодействия между препаратами и т.д.); (3) Улучшение понимания биологических механизмов излечения ВИЧ-инфекции путем выработки стандартизированного клинического протокола, который обеспечит сравнимость исследований вирусных резервуаров, характеристик инфицирующего вируса и оценки иммунного ответа после алло-ТГСК по различным трансплантационным центрам
" ["TYPE"]=> string(4) "html" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(14247) "Подобное лечение основано на том, что, во-первых, ВИЧ первично поражает систему гемопоэза и, во-вторых, что при ГТСК происходит замещение инфицированных гемопоэтических клеток неинфицированным костным мозгом. Незараженное потомство нового костного мозга затем заселяет организм пациента в различных зонах организма. Однако основной проблемой остается неинфекция донорских клеток после ТГСК. В частности, типичные «резервуары» ВИЧ, такие, как популяции моноцитов, обычно замещаются донорскими клетками лишь спустя месяцы после ТГСК. Персистирующие донорские моноциты впоследствии являются потенциальным источником ВИЧ-реинфекции клеток донора. Поэтому реакция «трансплантат против хозяина» может быть существенным фактором устранения остаточных клеток-носителей ВИЧ после ТГСК.
Чтобы предотвратить реинфекцию ВИЧ донорских клеток в организме пациента, можно привлечь донора с естественной делецией гена CCR5, при которой блокируется вход в клетку наиболее частого типа ВИЧ. Этотгенетический признак имеется у <1% населения. Поэтому поиск такого донора затруднителен. В данном случае у пациента должны быть серьезные показания к ТГСК , у него должна быть также ВИЧ-инфекция, и заражение вирусом должно зависеть от рецептора CCR5. Частота мутации CCR5-del32/del32 среди европейцев ≤1% и еще ниже – в других этнических группах. Таким образом, подобные больные обычно имеют малое количество доступных доноров. Если используют материал от взрослых доноров, то требуется очень близкое совпадение по HLA (7-8/8). Из-за этих ограничений, второй пациент для аналогичной ТГСК был найден лишь через несколько лет, в 2014 г. (Kordelas et al., 2014; Verheyen et al., 2014) К сожалению, результат ТГСК был негативным из-за рецидива ВИЧ-инфекции. Скорее всего, реинфекция реализовалась через другой рецептор, например, CXCR4.
Стволовые клетки из пуповинной крови (ПСК) в качестве стандартного донорского материала для ТГСК, стали в последнее десятилетие новым потенциальным источником гемопоэтических клеток для ВИЧ-инфицированных больных. Прежде всего, для хорошего исхода ТГСК здесь достаточно меньшего совпадения по HLA между ПСК и клетками пациента (Wagner et al., 2014). Эти менее строгие критерии подбора существенно повышают шансы найти донора в том же генетическом пуле. С другой стороны, если выявлена партия ПСК с уникальным признаком, вроде CCR5-del32/del32, то она теоретически может быть использована для нескольких больных. Поэтому увеличение пула образцов ПСК с наличием CCR5-del32/del32 обеспечит появление трансплантатов для того, чтобы повысить вероятность более быстрого и качественного подбора HLA-совместимого донора для больного с ВИЧ-инфекцией, если эта инфекция имеет тропизм к CCR5, и больному требуется ТГСК. Теоретический расчет минимального числа доз ПСК с del32/del32 проводился недавно (Petz et al., 2013), и было показана высокая вероятность нахождения образца, гомозиготного по CCR5-del32 и HLA-совместимого с пациентом, имеющим клинические показания к ТГСК. Однако число стволовых клеток на 1 дозу ПСК весьма мало, и одной дозы часто недостаточно для своевременного приживления у взрослого пациента. Поэтому ТГСК у взрослых лиц требуют обычно 2 доз ПСК, чтобы преодолеть ограничения малых доз ПСК в пуповинной крови. Хотя эта стратегия кажется простой и удобной для пациентов без ВИЧ-инфекции, ее применение проблематично у больных с ВИЧ-инфекцией. Очень маловероятен подбор двух доз ПСК с мутацией CCR5-del32, и преимущественный рост клеток с CCR5-del32 будет зависеть от случая. Решением вопроса может быть сочетание ТГСК пуповинных клеток и гаплоидентичной ТГСК. Последний, при высоком уровне его очистки от Т-клеток, может рассматриваться в качестве «мостика» к долгосрочному приживлению ПСК, как впервые показали испанские коллеги (Magro E et al., 2006). Лечебные перспективы комбинированной трансплантации гаплоидентичных и пуповинных клеток касаются более безопасного и быстрого приживления нейтрофилов, что дает лучшую защиту от инфекций. Такой вариант ТГСК может быть обоснован даже при наличии пригодного донора по основным показаниям. Некоторые авторы показали, что комбинированная гапло-ТГСК и пересадка ПСК имеет приемлемый уровень безопасности, сравнимый с ТГСК от неродственных доноров (Kwon et al., 2012; Liu et al., 2011). Однако новейшие протоколы размножения пуповинных стволовых клеток могут проложить новый путь для осуществления таких ТГСК при наличии лишь одной дозы ПСК с CCR5-del32.
Кроме тщательной оценки выбора доноров, возникает еще одно важное соображение, касающееся будущего ВИЧ-позитивныъ больных. Хотя ВИЧ-инфекция сейчас рассматривается как хроническое заболевание в эру эффективной специфической терапии, качество жизни ВИЧ-инфицированных больных обычно существенно нарушено. Исследование частоты самоубийств среди ВИЧ-положительных больных с 1988 по 2008 гг. включало 15275 ВИЧ-инфицированных лиц в длительные сроки (медиана – 4,7 г.) Частота суицидов среди этого контингента была более чем в 3 раза выше, нежели в населении в целом (Keiser et al., 2010), отражая, на самом деле, влияние многих ограничений, касающихся ВИЧ-инфицированных лиц в повседневной жизни.
Проведению трансплантаций при отсутствии должного опыта в этой области может помочь использование рекомендаций JACIE– системы, предназначенной для обеспечения качества и улучшения состояния знаний по данному вопросу. Таким образом, введение дополнительных качественных категорий, таких, как «альтернативная процедура трансплантации» с отдельным информированным согласием и контролем качества, включены в нашу трансплантационную программу, аккредитованную JACIE, в Университетской клинике Утрехта. Стандартное информированное согласие для биобанкирования (этическое одобрение) применяется для всех процедур алло-ТГСК и обеспечивает максимум получаемой информации независимо от ее исхода. Многие пациенты в Европе, теперь получают трансплантацию по комбинированному протоколу с гапло- и пуповинной ТГСК, в т.ч. один пациент получил трансплантацию клеток с CCR del32/32 в нашем центре. Об исходе этой ТГСК будет сообщено дополнительно..
Выводы
Доноры с мутацией CCR5-del32/del32, очевидно, являются предпочтительными для пациентов с гематологическими новообразованиями и сопутствующей ВИЧ-инфекцией. Настоятельно необходимо расширение пула образцов пуповинной крови с CCR5-del32/del32. Комбинированная трансплантация гаплоидентичных и пуповинных стволовых клеток, или протоколы с размножением стволовых клеток из одного образца пуповинной крови могут стать основой для лечения онкогематологических больных с ВИЧ-инфекцией. Однако ТГСК представляет собой высокий риск для больного и поэтому не может рассматриваться как оптимальное решение для функционального излечения ВИЧ-инфекции. Наряду с излечением ВИЧ-инфицированного больного, этот тип ТГСК позволяет исследование вариантов ВИЧ, важных для разработки механизмов лечения ВИЧ-инфекции. С нашего и других клинических случаев началось очень интересное международное сотрудничество – проект Epistem (http://www.epistem-project.org), основанный AMFAR – европейский проект проведения терапии и изучения потенциала излечения ВИЧ-инфекции путем аллогенной трансплантации гемопоэтических клеток. Областями исследований являются: (1) Повышение числа пригодных для ТГСК образцов ПСК с del32/del32, путем систематического тестирования европейских банков пуповинной крови; (2) Выдача советов в процессе лечения (выбор донора, этические аспекты, взаимодействия между препаратами и т.д.); (3) Улучшение понимания биологических механизмов излечения ВИЧ-инфекции путем выработки стандартизированного клинического протокола, который обеспечит сравнимость исследований вирусных резервуаров, характеристик инфицирующего вируса и оценки иммунного ответа после алло-ТГСК по различным трансплантационным центрам
" } } } }01.08.2015

Афанасьев Б. В. (Санкт-Петербург, Россия)
Вагемакер Г (Роттердам, Нидерланды)
Цандер А. Р. (Гамбург, Германия)
Фезе Б. (Гамбург, Германия)
Чухловин А. Б. (Санкт-Петербург, Россия)
Алейникова О. В. (Минск, Беларусь)
Баум К. (Ганновер, Германия)
Билько Н. М. (Киев, Украина)
Борсет М. (Трондхейм, Норвегия)
Бюхнер Т. (Мюнстер, Германия)
Галибин О. В. (Санкт-Петербург, Россия)
Грицаев С. В. (Санкт-Петербург, Россия)
Зубаровская Л. С. (Санкт-Петербург, Россия)
Климко Н. Н. (Санкт-Петербург, Россия)
Кольб Х. (Мюнхен, Германия)
Крегер Н. (Гамбург, Германия)
Кулагин А. Д. (Санкт-Петербург, Россия)
Ланге К. (Гамбург, Германия)
Мамаев Н. Н. (Санкт-Петербург, Россия)
Михайлова Н. Б. (Санкт-Петербург, Россия)
Моисеев И. С. (Санкт-Петербург, Россия)
Наглер А. (Тель-Авив, Израиль)
Немков А. С. (Санкт-Петербург, Россия)
Парамонов И. В. (Киров, Россия)
Румянцев А. Г. (Москва, Россия)
Савченко В. Г. (Москва, Россия)
Смирнов А. В. (Санкт-Петербург, Россия)
Усс А. Л. (Минск, Беларусь)
Фиббе В. (Лейден, Нидерланды)
Хельтцер Д. (Франкфурт-на Майне, Германия)
Чечеткин А. В. (Санкт-Петербург, Россия)
Алексей Б. Чухловин
Большинство статей, опубликованных в этом выпуске журнала CTT (том 4, № 1-2, 2015), как и ранее, касаются вопросов клинической онкогематологии. Кроме того, мы рады представить как клинические, так и экспериментальные работы, где обсуждаются новые и актуальные аспекты трансплантации и клеточной терапии.
- Химиотерапия злокачественных новообразований у пациентов старших возрастов приобретает все большую значимость, ввиду увеличения числа подобных клинических ситуаций. Соответствующие рекомендации пока далеки от совершенства. Поэтому статья проф. А. Цандера и соавторов касается некоторых ключевых аспектов цитостатической терапии у пожилых пациентов.
- Ряд специальных вопросов комбинированной клеточной трансплантации обсуждается в статье проф. Руту и соавт., где представлены весьма убедительные данные о возможных взаимодействиях пересадки гемопоэтических стволовых клеток и солидных органов от того же донора.
- Важные аспекты применения трансплантации гемопоэтических клеток, ингибиторов тирозинкиназы и иммунотерапии в рамках схем комбинированного лечения острого лимфобластного лейкоза рассматриваются в статье проф. Д. Хельцера
- ВИЧ-инфекция нередко осложняется вторичными злокачественными новообразованиями. Работа группы из Санкт-Петербурга касается разработки стратегии лечения ВИЧ-инфицированных больных с лейкозами или лимфомами на фоне активного антиретровирусного лечения.
- Раздел врожденных и наследственных заболеваний содержит статью проф. А. Алейниковой и соавт., содержащую собственные данные авторов об относительно редком иммунодефиците типа Ниймеген, который встречается более часто в некоторых областях Беларуси и представляет собой клиническую патологию, перспективную для применения трансплантации гемопоэтических стволовых клеток (ТГСК).
- Вопросы внедрения лабораторных маркеров в трансплантации гемопоэтических стволовых клеток рассматриваются в статье И.С.Моисеева и соавт., где отмечается потенциальная ценность определения уровней фактора до ТГСК, с целью прогнозирования тяжелых осложнений трансплантации и ранних рецидивов злокачественного заболевания.
- Доклинические модели клеточной трансплантации всегда оживленно обсуждаются клиницистами. Статья, представленная коллективом из Санкт-Петербургского государственного медицинского университета им. акад. И. Павлова и Института цитологии РАН касается ряда биологических эффектов в отношении течения и исходов экспериментального инфаркта миокарда, наблюдаемых при введении мезенхимных стволовых клеток (МСК) и мононуклеарной фракции клеток костного мозга. Местные инъекции МСК представляют собой, по-видимому, более предпочтительный вариант.
- Краткое сообщение проф. Р. Хелльмана касается ряда перспективных подходов к преодолению бластного криза при хроническом миелоидном лейкозе, в аспекте применения некоторых недавно испытанных терапевтических схем и новых экпериментальных способов лечения.
- Сообщение проф. Ю. Кубалла описывает современное состояние и перспективы использования стволовых клеток пуповинной крови в качестве возможного средства эффективного лечения ВИЧ-ассоциированных лейкозов, в связи с рядом благоприятных характеристик этого вида стволовых клеток.
- Особое внимание следует уделять будущему клеточной инженерии, особенно в области индуцибельных полипотентных стволовых клеток человека. Последние активно изучаются коллективом из Осло (Норвегия) с целью создания функционирующих хрящевых структур, сходных с нормальными тканями.
Регулярные статьи
Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,
Владимир Н. Вавилов, Борис В. Афанасьев
Владимир В. Давыденко1, Андрей А. Матюков1, Тимур Д. Власов1, Наталия В. Цупкина2, Анатолий Н. Ялфимов3, Георгий П. Пинаев2, Халида К. Аминева1
Аксель Р. Цандер1, Рене Дж. Хорнунг2, Ханс П. Липп3
Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова
Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская
Тапани Рууту1, Христиан Кенеке2, Гжегож В. Басак3
Регулярные статьи
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1218
[1] => 1219
[2] => 1220
[3] => 1221
[4] => 1222
[5] => 1223
[6] => 1224
)
[VALUE] => Array
(
[0] => 15
[1] => 66
[2] => 67
[3] => 68
[4] => 69
[5] => 70
[6] => 71
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 15
[1] => 66
[2] => 67
[3] => 68
[4] => 69
[5] => 70
[6] => 71
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 375
[VALUE] => 08.04.2015 15:05:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.04.2015 15:05:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 376
[VALUE] => 12.06.2015 15:05:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 12.06.2015 15:05:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 887
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 377
[VALUE] => 60
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 60
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 378
[1] => 379
[2] => 380
[3] => 381
[4] => 382
[5] => 383
[6] => 384
[7] => 385
)
[VALUE] => Array
(
[0] => 64
[1] => 34
[2] => 62
[3] => 37
[4] => 60
[5] => 63
[6] => 61
[7] => 65
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
[7] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 64
[1] => 34
[2] => 62
[3] => 37
[4] => 60
[5] => 63
[6] => 61
[7] => 65
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
[7] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 386
[VALUE] => Array
(
[TEXT] => <p class="Autor_Rus" lang="ru-RU">Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,<br>Владимир Н. Вавилов, Борис В. Афанасьев</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,
Владимир Н. Вавилов, Борис В. Афанасьев
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 387
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">НИИ детской онкологии, гематологии и трансплантологии им. Р. М. Горбачевой, Первый Санкт-Петербургский государственный медицинский университет им. И. П. Павлова, Санкт-Петербург, Россия </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => НИИ детской онкологии, гематологии и трансплантологии им. Р. М. Горбачевой, Первый Санкт-Петербургский государственный медицинский университет им. И. П. Павлова, Санкт-Петербург, Россия
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 388
[VALUE] => Array
(
[TEXT] => <p class="Summery_Rus" lang="ru-RU">В ряде исследований проводилось изучение прогностического значения маркеров повреждения эндотелия для анализа риска различных исходов аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК). При этом, однако, редко сравнивали информативность различных лабораторных маркеров при длительных сроках наблюдения. В настоящей работе мы оценивали прогностическую значимость фактора роста сосудистого эндотелия (<span lang="en-US">VEGF</span>) в плазме крови и содержания циркулирующих эндотелиальных клеток (ЦЭК) как возможных факторов, ассоциированных с ранней и поздней смертностью, не связанной с рецидивами. Учитывая известный негативный прогностический эффект экспрессии <span lang="en-US">VEGF</span> при онкогематологических заболеваниях, леченных цитостатической терапией, другой целью работы была оценка ассоциаций между уровнями <span lang="en-US">VEGF</span> и частотой рецидивов после алло-ТГСК. Уровни <span lang="en-US">VEGF</span> анализировали у 91 пациента перед началом кондиционирующей терапии, в день трансплантации и в день приживления трансплантата. Содержание ЦЭК в крови определяли у 55 больных из той же группы и в те же сроки. Как уровни <span lang="en-US">VEGF</span>, так и содержание ЦЭК коррелировали с ранней, но не более поздней нерецидивной смертностью. Высокие уровни <span lang="en-US">VEGF</span> в день 0 при использовании мультивариантного анализа были ассоциированы с более высокой однолетней безрецидивной выживаемостью (55% против 22%; <span lang="en-US">HR</span> 3,15, 95%; <span lang="en-US">CI</span> 1,34-7,40, <span lang="en-US">p</span>=0,009), тогда как высокое содержание ЦЭК до кондиционирования было ассоциировано с повышенной безрецидивной выживаемостью при унивариантном (69% против 20%, <span lang="en-US">p</span>=0,001), но не многофакторном анализе (95%<span lang="en-US">CI</span> 0.84-5.76, <span lang="en-US">p</span>=0,102). Высокие уровни <span lang="en-US">VEGF</span> <span lang="en-US">A</span> перед кондиционированием были ассоциированы с повышенной частотой рецидивов в течение 1 года (55% против 22%, <span lang="en-US">p</span>=0,001, <span lang="en-US">HR</span> 3,15, 95%<span lang="en-US">CI</span> 1,34-7,40), но не были связаны с поздними рецидивами и общей 3-летней выживаемостью (50% против 42%, соответственно, <span lang="en-US">p</span>=0.60), поскольку многие пациенты были успешно пролечены после рецидива. </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => В ряде исследований проводилось изучение прогностического значения маркеров повреждения эндотелия для анализа риска различных исходов аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК). При этом, однако, редко сравнивали информативность различных лабораторных маркеров при длительных сроках наблюдения. В настоящей работе мы оценивали прогностическую значимость фактора роста сосудистого эндотелия (VEGF) в плазме крови и содержания циркулирующих эндотелиальных клеток (ЦЭК) как возможных факторов, ассоциированных с ранней и поздней смертностью, не связанной с рецидивами. Учитывая известный негативный прогностический эффект экспрессии VEGF при онкогематологических заболеваниях, леченных цитостатической терапией, другой целью работы была оценка ассоциаций между уровнями VEGF и частотой рецидивов после алло-ТГСК. Уровни VEGF анализировали у 91 пациента перед началом кондиционирующей терапии, в день трансплантации и в день приживления трансплантата. Содержание ЦЭК в крови определяли у 55 больных из той же группы и в те же сроки. Как уровни VEGF, так и содержание ЦЭК коррелировали с ранней, но не более поздней нерецидивной смертностью. Высокие уровни VEGF в день 0 при использовании мультивариантного анализа были ассоциированы с более высокой однолетней безрецидивной выживаемостью (55% против 22%; HR 3,15, 95%; CI 1,34-7,40, p=0,009), тогда как высокое содержание ЦЭК до кондиционирования было ассоциировано с повышенной безрецидивной выживаемостью при унивариантном (69% против 20%, p=0,001), но не многофакторном анализе (95%CI 0.84-5.76, p=0,102). Высокие уровни VEGF A перед кондиционированием были ассоциированы с повышенной частотой рецидивов в течение 1 года (55% против 22%, p=0,001, HR 3,15, 95%CI 1,34-7,40), но не были связаны с поздними рецидивами и общей 3-летней выживаемостью (50% против 42%, соответственно, p=0.60), поскольку многие пациенты были успешно пролечены после рецидива.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 389
[VALUE] => 10.18620/1866-8836-2015-4-1-2-38-46
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-38-46
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 390
[VALUE] => Array
(
[TEXT] => <p class="Autor ParaOverride-3">Ivan S. Moiseev, Sergej V. Lapin, Elena A. Surkova, Margarita Y. Lerner, Elena V. Babenko, Alexandra A. Sipol, <br>Vladimir N. Vavilov, Boris V. Afanasyev</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Ivan S. Moiseev, Sergej V. Lapin, Elena A. Surkova, Margarita Y. Lerner, Elena V. Babenko, Alexandra A. Sipol,
Vladimir N. Vavilov, Boris V. Afanasyev
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 391
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, The First St.Petersburg State I. Pavlov Medical University </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation, The First St.Petersburg State I. Pavlov Medical University
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 392
[VALUE] => Array
(
[TEXT] => <h2>Summery</h2>
<p class="Summery">
A number of studies evaluated predictive value of endothelial damage markers on outcomes of allogeneic hematopoietic stem cell transplantation (alloHSCT), but they were rarely measured in combination and with long follow up. In this study we evaluated predictive value of vascular endothelial growth factor (VEGF) and circulating endothelial cells (CEC) on early and late non-relapse mortality (NRM). Given the known negative prognostic impact of VEGF expression in hematologic malignancies undergoing chemotherapy, the second goal was to access impact of VEGF level on relapse incidence after alloHSCT. Level of VEGF was analyzed in 91 consecutive patients before the start of conditioning, on day 0 and on the day of engraftment. CEC were measured in 55 consecutive patients from the same study group at the same time points. Both VEGF and CEC were predicted early, but not late NRM. High level of VEGF on day 0 in multivariate analysis was associated with increased 1-year NRM (55% vs 22%, HR 3.15, 95%CI 1.34-7.40, p=0.009), while high level of CEC before conditioning was associated with increased 1-year NRM in univariate (69% vs 20%, p=0.001), but not multivariate analysis (95%CI 0.84-5.76, p=0.102). High VEGF A level before conditioning was associated with increased 1-year relapse rate (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40), but had no impact on late relapses and 3-year overall survival (50% vs 42% respectively, p=0.60), as a large proportion of patients were successfully salvaged after relapse. CEC were not a significant prognostic factor for relapse (p=0.09). No correlation was found between VEGF and CEC at any time point (p>0.05), indicating that they may represent different aspects of endothelial dysfunction. In conclusion, VEGF and CEC are valuable biomarkers to predict early NRM, and VEGF is also a predictive factor of early relapse after alloHSCT.
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Summery
A number of studies evaluated predictive value of endothelial damage markers on outcomes of allogeneic hematopoietic stem cell transplantation (alloHSCT), but they were rarely measured in combination and with long follow up. In this study we evaluated predictive value of vascular endothelial growth factor (VEGF) and circulating endothelial cells (CEC) on early and late non-relapse mortality (NRM). Given the known negative prognostic impact of VEGF expression in hematologic malignancies undergoing chemotherapy, the second goal was to access impact of VEGF level on relapse incidence after alloHSCT. Level of VEGF was analyzed in 91 consecutive patients before the start of conditioning, on day 0 and on the day of engraftment. CEC were measured in 55 consecutive patients from the same study group at the same time points. Both VEGF and CEC were predicted early, but not late NRM. High level of VEGF on day 0 in multivariate analysis was associated with increased 1-year NRM (55% vs 22%, HR 3.15, 95%CI 1.34-7.40, p=0.009), while high level of CEC before conditioning was associated with increased 1-year NRM in univariate (69% vs 20%, p=0.001), but not multivariate analysis (95%CI 0.84-5.76, p=0.102). High VEGF A level before conditioning was associated with increased 1-year relapse rate (55% vs 22%, p=0.001, HR 3.15, 95%CI 1.34-7.40), but had no impact on late relapses and 3-year overall survival (50% vs 42% respectively, p=0.60), as a large proportion of patients were successfully salvaged after relapse. CEC were not a significant prognostic factor for relapse (p=0.09). No correlation was found between VEGF and CEC at any time point (p>0.05), indicating that they may represent different aspects of endothelial dysfunction. In conclusion, VEGF and CEC are valuable biomarkers to predict early NRM, and VEGF is also a predictive factor of early relapse after alloHSCT.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 393
[VALUE] => Prognostic significance of vascular endothelial growth factor and circulating endothelial cells for early and late outcomes of allogeneic hematopoietic stem cell transplantation
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Prognostic significance of vascular endothelial growth factor and circulating endothelial cells for early and late outcomes of allogeneic hematopoietic stem cell transplantation
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1225
[VALUE] => 18
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 18
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1226
[VALUE] => 19
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 19
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Иван С. Моисеев, Сергей В. Лапин, Елена А. Суркова, Маргарита Ю. Лернер, Елена В. Бабенко, Александра А. Сипол,
Владимир Н. Вавилов, Борис В. Афанасьев
НИИ детской онкологии, гематологии и трансплантологии им. Р. М. Горбачевой, Первый Санкт-Петербургский государственный медицинский университет им. И. П. Павлова, Санкт-Петербург, Россия
В ряде исследований проводилось изучение прогностического значения маркеров повреждения эндотелия для анализа риска различных исходов аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК). При этом, однако, редко сравнивали информативность различных лабораторных маркеров при длительных сроках наблюдения. В настоящей работе мы оценивали прогностическую значимость фактора роста сосудистого эндотелия (VEGF) в плазме крови и содержания циркулирующих эндотелиальных клеток (ЦЭК) как возможных факторов, ассоциированных с ранней и поздней смертностью, не связанной с рецидивами. Учитывая известный негативный прогностический эффект экспрессии VEGF при онкогематологических заболеваниях, леченных цитостатической терапией, другой целью работы была оценка ассоциаций между уровнями VEGF и частотой рецидивов после алло-ТГСК. Уровни VEGF анализировали у 91 пациента перед началом кондиционирующей терапии, в день трансплантации и в день приживления трансплантата. Содержание ЦЭК в крови определяли у 55 больных из той же группы и в те же сроки. Как уровни VEGF, так и содержание ЦЭК коррелировали с ранней, но не более поздней нерецидивной смертностью. Высокие уровни VEGF в день 0 при использовании мультивариантного анализа были ассоциированы с более высокой однолетней безрецидивной выживаемостью (55% против 22%; HR 3,15, 95%; CI 1,34-7,40, p=0,009), тогда как высокое содержание ЦЭК до кондиционирования было ассоциировано с повышенной безрецидивной выживаемостью при унивариантном (69% против 20%, p=0,001), но не многофакторном анализе (95%CI 0.84-5.76, p=0,102). Высокие уровни VEGF A перед кондиционированием были ассоциированы с повышенной частотой рецидивов в течение 1 года (55% против 22%, p=0,001, HR 3,15, 95%CI 1,34-7,40), но не были связаны с поздними рецидивами и общей 3-летней выживаемостью (50% против 42%, соответственно, p=0.60), поскольку многие пациенты были успешно пролечены после рецидива.
Регулярные статьи
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1227
[1] => 1228
[2] => 1229
[3] => 1230
[4] => 1231
[5] => 1232
)
[VALUE] => Array
(
[0] => 80
[1] => 81
[2] => 82
[3] => 83
[4] => 84
[5] => 85
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 80
[1] => 81
[2] => 82
[3] => 83
[4] => 84
[5] => 85
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 466
[VALUE] => 06.04.2015 15:21:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 06.04.2015 15:21:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 467
[VALUE] => 02.07.2015 15:21:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 02.07.2015 15:21:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 894
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 468
[VALUE] => 73
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 73
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 469
[1] => 470
[2] => 471
[3] => 472
[4] => 473
[5] => 474
[6] => 475
)
[VALUE] => Array
(
[0] => 79
[1] => 77
[2] => 74
[3] => 78
[4] => 76
[5] => 75
[6] => 73
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 79
[1] => 77
[2] => 74
[3] => 78
[4] => 76
[5] => 75
[6] => 73
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 476
[VALUE] => Array
(
[TEXT] => <p class="Autor">Владимир В. Давыденко<sup>1</sup>, Андрей А. Матюков<sup>1</sup>, Тимур Д. Власов<sup>1</sup>, Наталия В. Цупкина<sup>2</sup>, Анатолий Н. Ялфимов<sup>3</sup>, Георгий П. Пинаев<sup>2</sup>, Халида К. Аминева<sup>1</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Владимир В. Давыденко1, Андрей А. Матюков1, Тимур Д. Власов1, Наталия В. Цупкина2, Анатолий Н. Ялфимов3, Георгий П. Пинаев2, Халида К. Аминева1
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 477
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work-Rus"><sup>1</sup>Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова</p>
<p class="Autor_place_work-Rus"><sup>2</sup>Институт цитологии Российской Академии наук, Санкт-Петербург</p>
<p class="Autor_place_work-Rus"><sup>3</sup>Российский центр радиологии и хирургических технологий, Санкт-Петербург</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 1Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова
2Институт цитологии Российской Академии наук, Санкт-Петербург
3Российский центр радиологии и хирургических технологий, Санкт-Петербург
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 478
[VALUE] => Array
(
[TEXT] => <h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8<span class="CharOverride-12">+</span>0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами. </p>
<p class="Summery_H">Результаты</p>
<p class="Summery_Rus" lang="ru-RU">Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков. </p>
<p class="Summery_H">Заключение</p>
<p class="Summery_Rus" lang="ru-RU">Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов. </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Резюме
Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8+0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами.
Результаты
Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков.
Заключение
Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 479
[VALUE] => 10.18620/1866-8836-2015-4-1-2-47-57
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-47-57
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 480
[VALUE] => Array
(
[TEXT] => <p class="Autor">Vladimir V. Davydenko<sup>1</sup>, Andrey A. Matyukov<sup>1</sup>, Timur D. Vlasov<sup>1</sup>, Natalya V. Tsupkina<sup>2</sup>, Anatoly N. Yalfimov<sup>3</sup>, <br>Georgy P. Pinaev<sup>2</sup>, Khalida K. Amineva<sup>1</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Vladimir V. Davydenko1, Andrey A. Matyukov1, Timur D. Vlasov1, Natalya V. Tsupkina2, Anatoly N. Yalfimov3,
Georgy P. Pinaev2, Khalida K. Amineva1
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 481
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work"><span class="CharOverride-2" lang="en-US">1</span><span lang="en-US">FirstSt.Petersburg State I.Pavlov Medical University </span></p>
<p class="Autor_place_work"><span class="CharOverride-2" lang="en-US">2</span><span lang="en-US">Institute of Cytology, Russian Academy of Sciences, St.Petersburg</span></p>
<p class="Autor_place_work"><span class="CharOverride-2" lang="en-US">3</span><span lang="en-US">Russian Center of Radiology and Surgical Technologies, St.Petersburg</span></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 1FirstSt.Petersburg State I.Pavlov Medical University
2Institute of Cytology, Russian Academy of Sciences, St.Petersburg
3Russian Center of Radiology and Surgical Technologies, St.Petersburg
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 482
[VALUE] => Array
(
[TEXT] => <h2>Summary</h2><p class="Summery">Over the last decade, different cell therapy options have been tested to improve treatment of myocardial infarction (MI), including cardiomyoplastics. Autologous bone marrow is a widely used source of therapeutic cell preparations, i.e., freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchymal stromal cells (MMSC). The aim of our pilot study was to compare short- and long-term consequences of intramyocardial MF and MMSC transplantation upon clinical course and outcome of experimental MI. Materials and methods: The experiments were performed with male Chinchilla rabbits of 2.8<span class="CharOverride-12">+</span>0.2 kg weight. MI was modelled by ligation of anterior descendent left coronary artery. Mononuclear cell fraction was obtained from the bone marrow aspirate. MMSC cell culture was grown by MF cell passages in МЕМ medium with 10% fetal calf serum. Intramyocardial injections of MF or MMSC suspensions were performed into 6 points of the infarcted area. The surviving animals were divided in four groups, each consisting of 13 rabbits: group 1 (controls), group 2 (placebo-treated), group 3 (MMSC injections), and group 4 (MF injections). Electrocardiography (ECG) and echo-cardiography were carried out in all animals before surgery, during 1 mo and 1 year after surgery. Myocardial perfusion rates were assessed with SPECT technique. IM dimensions (perfusion areas) were determined by means of staining heart sections with 2,3,5-TTC. Routine histology of myocardial sections was also performed. Vascularization rates of different myocardial areas were assessed in similar way. </p>
<p class="Summery_H">Results</p>
<p class="Summery">Intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit experimental MI during the acute phase has changed natural process development and resulted in principally different morpho-functional outcomes. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, the animals, treated with MMSC or MF showed less impaired perfusion rates than in control or placebo groups (p<0.05). 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged myocardium in MMSC and MF-treated groups. These changes were confirmed by perfusion tomoscyntigraphy of myocardium at 1.5 and 12 months after surgery. Histological studies have shown that, after MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles. One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all functional parameters (LV ejection fraction; EDSLV, end LV diastolic size; blood flow rates in ascending aorta) at 12 months post-surgery (p<0.05), and absence of akinetic areas. </p>
<p class="Summery_H">Conclusions </p>
<p class="Summery">MMSC injections were associated with pronounced therapeutic effect, by reducing myocardium damage area. By the contrary, MF transplantation showed a negative effect, expanding myocardium damage area and impairing systolic function indices. Both MMSC and MF intramyocardial transplantation display neoangiogenesis stimulation and perfusion improvement in rabbit experimental infarction area. </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Summary
Over the last decade, different cell therapy options have been tested to improve treatment of myocardial infarction (MI), including cardiomyoplastics. Autologous bone marrow is a widely used source of therapeutic cell preparations, i.e., freshly isolated mononuclear cell fraction (MF), or cultured multipotent mesenchymal stromal cells (MMSC). The aim of our pilot study was to compare short- and long-term consequences of intramyocardial MF and MMSC transplantation upon clinical course and outcome of experimental MI. Materials and methods: The experiments were performed with male Chinchilla rabbits of 2.8+0.2 kg weight. MI was modelled by ligation of anterior descendent left coronary artery. Mononuclear cell fraction was obtained from the bone marrow aspirate. MMSC cell culture was grown by MF cell passages in МЕМ medium with 10% fetal calf serum. Intramyocardial injections of MF or MMSC suspensions were performed into 6 points of the infarcted area. The surviving animals were divided in four groups, each consisting of 13 rabbits: group 1 (controls), group 2 (placebo-treated), group 3 (MMSC injections), and group 4 (MF injections). Electrocardiography (ECG) and echo-cardiography were carried out in all animals before surgery, during 1 mo and 1 year after surgery. Myocardial perfusion rates were assessed with SPECT technique. IM dimensions (perfusion areas) were determined by means of staining heart sections with 2,3,5-TTC. Routine histology of myocardial sections was also performed. Vascularization rates of different myocardial areas were assessed in similar way.
Results
Intramyocardial transplantation of autologous bone marrow cells (MF and MMSC) into the area of rabbit experimental MI during the acute phase has changed natural process development and resulted in principally different morpho-functional outcomes. Ten days after coronary occlusion, all animals exhibited pronounced perfusion decrease in infarcted anterior wall of LV (p<0,05). However, the animals, treated with MMSC or MF showed less impaired perfusion rates than in control or placebo groups (p<0.05). 1.5 months after treatment, a gradual recovery of mean perfusion rates was observed in damaged myocardium in MMSC and MF-treated groups. These changes were confirmed by perfusion tomoscyntigraphy of myocardium at 1.5 and 12 months after surgery. Histological studies have shown that, after MMSC transplantation, a pattern of microfocal cardiosclerosis was observed, followed by recovery of myocardial structure, whereas MF injections were followed by development of fibrotic aneurism affecting both left and right ventricles. One year after surgical intervention, a more expressed positive effect of MMSC transplantation was observed, i.e., nearly full recovery of all functional parameters (LV ejection fraction; EDSLV, end LV diastolic size; blood flow rates in ascending aorta) at 12 months post-surgery (p<0.05), and absence of akinetic areas.
Conclusions
MMSC injections were associated with pronounced therapeutic effect, by reducing myocardium damage area. By the contrary, MF transplantation showed a negative effect, expanding myocardium damage area and impairing systolic function indices. Both MMSC and MF intramyocardial transplantation display neoangiogenesis stimulation and perfusion improvement in rabbit experimental infarction area.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 483
[VALUE] => Comparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Comparative effects of intramyocardial autotransplantation of different bone marrow cells upon outcomes of experimental myocardial infarction in rabbits
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1233
[VALUE] => 20
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 20
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1234
[VALUE] => 21
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 21
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Владимир В. Давыденко1, Андрей А. Матюков1, Тимур Д. Власов1, Наталия В. Цупкина2, Анатолий Н. Ялфимов3, Георгий П. Пинаев2, Халида К. Аминева1
1Первый Санкт-Петербургский государственный медицинский Университет им. И.П.Павлова
2Институт цитологии Российской Академии наук, Санкт-Петербург
3Российский центр радиологии и хирургических технологий, Санкт-Петербург
Резюме
Введение. На протяжении последних 10 лет изучались различные варианты клеточной терапии, направленной на улучшение результатов лечения инфаркта миокарда (ИМ), включая кардиомиопластику. Аутологичный костный мозг широко применяется в качестве источника изолированных препаратов клеток, в т.ч. свежеполученные мононуклеарные клетки (МНК) и культивированные мультипотентные мезенхимные стволовые клетки (ММСК). Целью нашего пилотного исследования было сравнение кратко- и долгосрочных эффектов интрамиокардиального введения МНК и ММСК на клиническое течение и исходы экспериментального ИМ. Материалы и методы. Эксперименты проводили на кроликах Шиншилла весом 2.8+0.2 кг. ИМ моделировали путем лигирования передней нисходящей левой коронарной артерии. Фракцию МНК получали из аспирата костного мозга. Культуру ММСК выращивали путем пассажей МНК в среде Игла с 10% фетальной телячьей сыворотки. Инъекции суспензий МНК и ММСК осуществляли в 6 точек области инфаркта. Выжившие животные были разделены на 4 группы (по 13 в каждой): группа 1 (контроль); группа 2 (плацебо); группа 3 (введение ММСК), и группа 4 (введение МНК). ЭКГ и эхо-КГ проводились всем животным од хирургического вмешательства, а также через 1 мес. и 1 год после него. Показатели перфузии миокарда оценивали с помощью технологии SPECT. Размеры зоны ИМ (зоны перфузии) определяли посредством окрашивания срезов сердечной ткани с помощью 2,3,5-ТТС. Также проводили рутинные гистологические исследования срезов миокарда. Степень васкуляризации различных областей миокарда оценивали морфологическими методами.
Результаты
Внутрисердечная пересадка аутологичных клеток костного мозга (МНК и ММСК) в области экспериментального ИМ у кроликов в его острой фазе приводила к модификации его естественного развития и вызывала принципиально различные морфофункциональные исходы. Через 10 дней после коронарной окклюзии у всех животных отмечалось резкое снижение перфузии передней стенки левого желудочка миокарда. (p<0,05). В то же время у животных, леченых ММСК или МНК, уровни перфузии были снижены в меньшей мере, нежели в контроле и группе плацебо (p<0.05). Спустя 1,5 мес. после лечения наблюдалось постепенное восстановление средних уровней перфузии поврежденного миокарда в группах, леченных ММСК и МНК. Эти изменения подтверждены перфузионной томосцинтиграфией миокарда через 1,5 и 12 месяцев после ИМ. Гистологические исследования показали, что после трансплантации ММСК отмечалась картина микроочагового кардиосклероза, а впоследствии – восстановлении структуры миокарда, тогда как после инъекций МНК наблюдалось развитие фибротической аневризмы, поражающей как левый, так и правый желудочек. Через год после хирургического вмешательства отмечен более выраженный положительный эффект трансплантации при введении ММСК, т.е. почти полное восстановление по всем функциональным параметрам (фракция выброса левого желудочка, показатель EDSLV, конечный диастолический размер левого желудочка, скорость кровотока в восходящей аорте) через 12 мес. после операции (p<0.05), а также отсутствие акинетических участков.
Заключение
Инъекции ММСК были ассоциированы с выраженным терапевтическим эффектом, а именно – снижением области повреждения миокарда. Напротив, трансплантация МНК сопровождалась негативным эффектом, с расширением области поражения миокарда и нарушением систолических функций. Трансплантация ММНК, и МНК приводят к стимуляции неоангиогенеза и улучшению перфузии в области экспериментального ИМ у кроликов.
Регулярные статьи
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1180
[1] => 1181
[2] => 1182
[3] => 1183
[4] => 1184
[5] => 1185
)
[VALUE] => Array
(
[0] => 15
[1] => 16
[2] => 17
[3] => 18
[4] => 19
[5] => 20
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 15
[1] => 16
[2] => 17
[3] => 18
[4] => 19
[5] => 20
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 923
[VALUE] => 25.01.2015 17:40:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 25.01.2015 17:40:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 924
[VALUE] => 23.06.2015 17:40:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 23.06.2015 17:40:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 925
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 21
[VALUE] => 11
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 11
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 24
[1] => 25
[2] => 84
)
[VALUE] => Array
(
[0] => 11
[1] => 12
[2] => 14
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 11
[1] => 12
[2] => 14
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 97
[VALUE] => Array
(
[TEXT] => <p class="Autor_Rus" lang="ru-RU">Аксель Р. Цандер<sup>1</sup>, Рене Дж. Хорнунг<sup>2</sup>, Ханс П. Липп<sup>3</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Аксель Р. Цандер1, Рене Дж. Хорнунг2, Ханс П. Липп3
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 98
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work-Rus"><sup>1</sup>Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия </p>
<p class="Autor_place_work-Rus"><sup>2</sup>Университетский медицинский центр Гамбург-Эппендорф, Германия</p>
<p class="Autor_place_work-Rus"><sup>3</sup><span class="affiliation">Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия</span></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 1Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия
2Университетский медицинский центр Гамбург-Эппендорф, Германия
3Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 99
[VALUE] => Array
(
[TEXT] => <h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.</p>
<p class="Summery_Rus" lang="ru-RU">Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (<span class="CharOverride-4">Hypericum perforatum</span>), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.</p>
<p class="Summery_Rus" lang="ru-RU">Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов. </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Резюме
Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.
Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (Hypericum perforatum), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.
Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 22
[VALUE] => 10.18620/1866-8836-2015-4-1-2-8-13
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-8-13
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 100
[VALUE] => Array
(
[TEXT] => <p class="Autor">Axel R. Zander<sup>1</sup>, René J. Hornung<sup>2</sup>, Hans-Peter Lipp<sup>3</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Axel R. Zander1, René J. Hornung2, Hans-Peter Lipp3
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 101
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">Research Department Cell and Gene Therapy, Clinic for Stem Cell Transplantation, University Medical Centre Hamburg-Eppendorf, Hamburg, Germany<sup>1</sup></p><p class="Autor_place_work">University Medical Centre Hamburg-Eppendorf, Hamburg, Germany<sup>2</sup></p>
<p class="Autor_place_work">Department of Hospital Pharmacy, University Tübingen, Tübingen, Germany<sup>3</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Research Department Cell and Gene Therapy, Clinic for Stem Cell Transplantation, University Medical Centre Hamburg-Eppendorf, Hamburg, Germany1
University Medical Centre Hamburg-Eppendorf, Hamburg, Germany2
Department of Hospital Pharmacy, University Tübingen, Tübingen, Germany3
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 102
[VALUE] => Array
(
[TEXT] => <h2 class="Summery">
Summary</h2>
<p class="Summery">
Physiological changes and deficiencies in cognitive processes in the elderly have an influence on therapy and drug dosage compliance. The consequences of differences for the outcome of especially chemotherapies are neither well nor systematically studied. Existing studies though could actually demonstrate age-related differences in clinical pharmacokinetics. Another problem is the increased number of prescribed drugs that are often necessary when getting older (polypharmacy) and their interference with over-the-counter drugs (OTC) and complementary and alternative medicine (CAM). While they are often seen as harmless since they require no prescription or are of “natural origin”, they can contain pharmaceutical active agents. For example green tea is reported to prevent prostate cancer and pre-menopausal breast cancer and is therefore often recommended to cancer patients, but also contains Epigallocatechin gallate (EGCg) an active substance which decreases the bio-availability of the anti-cancer drugs Bortezomid or Sunitinib. Conclusion: a further and more systematic study of age-related differences in the outcome of chemotherapies in the elderly is necessary. Here especially the kidney function requires adaption of treatment regimen. Furthermore the interactions with other drugs, in particular over-the-counter and alternative medicine, need to be better understood and communicated.
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] =>
Summary
Physiological changes and deficiencies in cognitive processes in the elderly have an influence on therapy and drug dosage compliance. The consequences of differences for the outcome of especially chemotherapies are neither well nor systematically studied. Existing studies though could actually demonstrate age-related differences in clinical pharmacokinetics. Another problem is the increased number of prescribed drugs that are often necessary when getting older (polypharmacy) and their interference with over-the-counter drugs (OTC) and complementary and alternative medicine (CAM). While they are often seen as harmless since they require no prescription or are of “natural origin”, they can contain pharmaceutical active agents. For example green tea is reported to prevent prostate cancer and pre-menopausal breast cancer and is therefore often recommended to cancer patients, but also contains Epigallocatechin gallate (EGCg) an active substance which decreases the bio-availability of the anti-cancer drugs Bortezomid or Sunitinib. Conclusion: a further and more systematic study of age-related differences in the outcome of chemotherapies in the elderly is necessary. Here especially the kidney function requires adaption of treatment regimen. Furthermore the interactions with other drugs, in particular over-the-counter and alternative medicine, need to be better understood and communicated.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 23
[VALUE] => Chemotherapy in the elderly – How intense should treatment be?
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Chemotherapy in the elderly – How intense should treatment be?
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1186
[VALUE] => 8
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 8
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1187
[VALUE] => 9
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 9
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Аксель Р. Цандер1, Рене Дж. Хорнунг2, Ханс П. Липп3
1Отдел трансплантации стволовых клеток, Университетский медицинский центр Гамбург-Эппендорф, Гамбург, Германия
2Университетский медицинский центр Гамбург-Эппендорф, Германия
3Отдел госпитальной фармации, Университет Тюбинген, Тюбинген, Германия
Резюме
Исходы химиотерапии у лиц пожилого возраста зависят от возрастных изменений функций различных органов. Наряду со снижением содержания воды и повышением доли жиров в теле, отмечено снижение нормальной функции органов: сердечного выброса – на 1%, кровотока печени – на 1%, кровотока почек – на 1% ежегодно. Снижение кислотности в желудке и моторики кишечника может приводить к снижению биодоступности многих препаратов. Нарушения краткосрочной памяти ведут к ошибкам дозировки и проблемам с соблюдением режима приема препаратов. Эти нарушения и дефицит когнитивных процессов у лиц пожилого возраста оказывают влияние на терапию и дозировку препаратов. Последствия возрастных различий, в особенности, для исходов химиотерапии, не подвергались систематическому изучению. Существующие исследования указывают, однако, на возрастные различия в клинической фармакокинетике. Однако имеются методические рекомендации международного Общества по гериатрической онкологии по дозировке ряда противораковых препаратов в зависимости от показателей клиренса креатинина у больных. Обсуждается вопрос о кратности приема кардиотоксических препаратов (например, доксорубицина) в зависимости от возраста.
Другие проблемы состоят в возрастающем числе прописанных препаратов, которые часто нужны в старшем возрасте (полифармация) и их взаимодействии с другими, безрецептурными препаратами и средствами комплементарной и альтернативной медицины. Хотя они часто считаются безвредными, так они не требуют рецепта или являются натуральными продуктами, они могут содержать фармакологически активные агенты, влияющие на метаболизм химиотерапевтических препаратов. В качестве примера приводятся препараты зверобоя (Hypericum perforatum), который является индукторами Cyp3A. Его применение совместно с Иматинибом приводит к значительному повышению его клиренса из организма. Миеются также данные о повышении гематотоксического действия этопозида на фоне приема препаратов Эхинацеи Рассматриваются также возможные модифицирующие эффекты зеленого чая, о котором известно, что он предотвращает рак простаты и пременопаузальный рак молочной железы и поэтому часто назначается онкологическим больным. В то же время он содержит эпигаллокатехин-галлат в качестве активной субстанции, которая снижает биодоступность, например, противоракового препарата бортезомиба.
Таким образом, следует учитывать возможные потенцирующие и ингибирующие эффекты многих безрецептурных препаратов на противоопухолевое воздействие многих химиотерапевтических препаратов. Необходимо собирать и систематизировать сведения о соответствующих побочных эффектах от больных пожилого возраста с целью большей адаптации дозировок к возрасту пациентов. На последующем этапе можно включать пожилых больных в клинические исследования и планировать специальные исследования по химиотерапии пациентов старших возрастов.
Регулярные статьи
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1212
[1] => 1213
[2] => 1214
[3] => 1215
)
[VALUE] => Array
(
[0] => 54
[1] => 56
[2] => 57
[3] => 58
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 54
[1] => 56
[2] => 57
[3] => 58
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 290
[VALUE] => 27.02.2015 14:23:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 27.02.2015 14:23:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 291
[VALUE] => 12.06.2015 14:23:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 12.06.2015 14:23:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 872
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 292
[VALUE] => 51
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 51
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 293
[1] => 294
[2] => 295
)
[VALUE] => Array
(
[0] => 52
[1] => 51
[2] => 53
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 52
[1] => 51
[2] => 53
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 296
[VALUE] => Array
(
[TEXT] => <p class="Autor">Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 297
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 298
[VALUE] => Array
(
[TEXT] => <p class="Summery">Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.</p>
<p class="Summery">Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии. </p>
<p class="Summery">Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена <span lang="en-US">NBN</span>. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.</p>
<p class="Summery">Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661<span lang="en-US">delACAAA</span> в гене <span lang="en-US">NBN</span> и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (<span lang="en-US">III</span> стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.</p>
<p class="Summery">Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.
Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии.
Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена NBN. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.
Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661delACAAA в гене NBN и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (III стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.
Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 299
[VALUE] => 10.18620/1866-8836-2015-4-1-2-31-37
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-31-37
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 300
[VALUE] => Array
(
[TEXT] => <p class="Autor">Olga V. Aleinikova, Alina S. Fedorova, Svetlana O. Sharapova</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Olga V. Aleinikova, Alina S. Fedorova, Svetlana O. Sharapova
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 301
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">Belarusian Research Center for Pediatric Oncology, Hematology and Immunology, Minsk Region, Belarus</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Belarusian Research Center for Pediatric Oncology, Hematology and Immunology, Minsk Region, Belarus
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 302
[VALUE] => Array
(
[TEXT] => <h2>Summery </h2>
<p class="Summery">
Introduction: Nijmegen breakage syndrome (NBS) is characterized by chromosome instability, combined immunodeficiency, radiosensitivity and high predisposition to lymphoid malignancy. A specific therapy is not available, however, hematopoietic stem cell transplantation (HSCT) is considered for NBS patients with refractory or recurrent leukemia or lymphoma.
</p>
<p class="Summery">
Purpose: We aimed to present Belarusian data in NBS diagnosis and management and to discuss indications for allo-HSCT treatment.
</p>
<p class="Summery">
Patients and Methods: A total of 238 patients were registered with primary immune deficiency (PID), including 19 cases of NBS. DNA was analyzed for mutation in NBN gene by direct sequencing of exon 6. Histological classification of lymphoid neoplasms was performed according to World Health Organization classification (2008). The patients were treated according to modified pediatric regimens or individually.
</p>
<p class="Summery">
Results: NBS accounted for 8.0% of all PID cases and was diagnosed at the age from 0.3 to 21.6 years (median 7.1). Mutation 657-661delACAAA in NBN gene and combined immunodeficiency of various degrees was confirmed in all patients. Lymphoid malignancy developed in 9 (47.4%) NBS patients ageing from 4.3 to 21.6 years (median 10.7). Acute leukemia was diagnosed in 4 patients, and stage III non-Hodgkin’s lymphoma in 5. Lymphoma/leukemia were in 7 out of 9 cases of T-cell origin. Complete remission (CR) was achieved in 66.7% of the patients.. Events were: death from infections in induction or in CR1 in 3 patients, progression/relapse in 3, second lymphoma in 1. Totally 7 NBS patients died, all after the development of malignancies. Two patients with T-mature lymphoma/leukemia did not respond to induction chemotherapy, were treated with unrelated HSCT in the 1CT and alive disease free within 6 and 13 months after transplantation. HSCT from a sibling donor was performed 9.8 years ago in a boy without malignancy but with infectious and autoimmune complications. They all received reduced-intensity conditioning regimens, which were well tolerated.
</p>
<p class="Summery">
Conclusions:<span class="CharOverride-10"> </span>NBS needs to be diagnosed early. With respect to progressive immunodeficiency and high risk of lymphoid malignancies with uncertain curative prospective, an allo-HSCT approach with reduced-intensity conditioning could be proposed as a treatment option for NBS patients with severe defects of immune function, and for all NBS patients with lymphoid malignancy in 1<sup>st</sup> complete remission.
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Summery
Introduction: Nijmegen breakage syndrome (NBS) is characterized by chromosome instability, combined immunodeficiency, radiosensitivity and high predisposition to lymphoid malignancy. A specific therapy is not available, however, hematopoietic stem cell transplantation (HSCT) is considered for NBS patients with refractory or recurrent leukemia or lymphoma.
Purpose: We aimed to present Belarusian data in NBS diagnosis and management and to discuss indications for allo-HSCT treatment.
Patients and Methods: A total of 238 patients were registered with primary immune deficiency (PID), including 19 cases of NBS. DNA was analyzed for mutation in NBN gene by direct sequencing of exon 6. Histological classification of lymphoid neoplasms was performed according to World Health Organization classification (2008). The patients were treated according to modified pediatric regimens or individually.
Results: NBS accounted for 8.0% of all PID cases and was diagnosed at the age from 0.3 to 21.6 years (median 7.1). Mutation 657-661delACAAA in NBN gene and combined immunodeficiency of various degrees was confirmed in all patients. Lymphoid malignancy developed in 9 (47.4%) NBS patients ageing from 4.3 to 21.6 years (median 10.7). Acute leukemia was diagnosed in 4 patients, and stage III non-Hodgkin’s lymphoma in 5. Lymphoma/leukemia were in 7 out of 9 cases of T-cell origin. Complete remission (CR) was achieved in 66.7% of the patients.. Events were: death from infections in induction or in CR1 in 3 patients, progression/relapse in 3, second lymphoma in 1. Totally 7 NBS patients died, all after the development of malignancies. Two patients with T-mature lymphoma/leukemia did not respond to induction chemotherapy, were treated with unrelated HSCT in the 1CT and alive disease free within 6 and 13 months after transplantation. HSCT from a sibling donor was performed 9.8 years ago in a boy without malignancy but with infectious and autoimmune complications. They all received reduced-intensity conditioning regimens, which were well tolerated.
Conclusions: NBS needs to be diagnosed early. With respect to progressive immunodeficiency and high risk of lymphoid malignancies with uncertain curative prospective, an allo-HSCT approach with reduced-intensity conditioning could be proposed as a treatment option for NBS patients with severe defects of immune function, and for all NBS patients with lymphoid malignancy in 1st complete remission.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 303
[VALUE] => Should Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Should Allogeneic Hematopoietic Stem Cell Transplantation be a Treatment Option for Patients with Nijmegen Breakage Syndrome? Belarusian Experience
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1216
[VALUE] => 16
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 16
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1217
[VALUE] => 17
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 17
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Ольга В. Алейникова, Алина С. Фёдорова, Светлана О. Шарапова
Республиканский научно-практический центр детской онкологии, гематологии и иммунологии, Минский район, Беларусь
Актуальность: Синдром Ниймеген (СН) характеризуется хромосомной нестабильностью, комбинированным иммунодефицитом, повышенной чувствительностью к радиоактивному излучению и предрасположенностью к развитию лимфоидных неоплазий. Специфических методов лечения СН нет, но считается оправданным проведение трансплантации гемопоэтических стволовых клеток (ТГСК) пациентам с рецидивами или с рефрактерными формами лимфомы/лейкоза.
Цель: анализ данных по диагностике и лечению белорусских пациентов с СН и обсуждение показаний к проведению аллогенной трансплантации при этой патологии.
Пациенты и методы: Диагноз первичного иммунодефициты (ПИД) установлен у 238 пациентов, включая 19 случаев СН. Анализ ДНК проводился методом прямого секвенирования 6 экзона гена NBN. Гистологическая верификация лимфоидных неоплазий проводилась в соответствии с классификацией ВОЗ 2008 года. Пациенты получали протокольную или индивидуальную химиотерапию.
Результаты: СН составил 8.0% от всех случаев ПИД и был диагностирован в возрасте от 0.3 до 21.6 лет (медиана – 7.1). Наличие мутации 657-661delACAAA в гене NBN и комбинированного иммунодефицита было подтверждено у всех пациентов. Злокачественные лимфопролиферативные заболевания развились у 9 (47.4%) пациентов с СН в возрасте от 4.3 до 21.6 лет (медиана – 10.7), Т-клеточные в большинстве (77.8%) случаев, острый лейкоз – у 4, неходжкинская лимфома (III стадия) – у 5. Полная ремиссия (ПР) была достигнута у 66.7% пациентов. События на лечении: смерть от инфекций на этапе индукции или в ПР – 3, прогрессирование/рецидив – 3, вторая лимфома – 1. Всего умерли 7 пациентов с СН, все после развития гемобластоза. Двоим пациентам с Т-зрелой лимфомой/лейкозом, не ответившим на индукционную химиотерапию, была проведена неродственная ТГСК в 1ПР. Эти пациенты живы, без признаков рецидива 6 и 13 месяцев после трансплантации. Также ТГСК от совместимого родственного донора была проведена 9.8 лет назад мальчику без опухоли, но с инфекционными и аутоиммунными осложнениями. Всем троим пациентам было проведено немиелоаблативное кондиционирование, без тяжёлых осложнений.
Заключение: СН должен диагностироваться рано. Учитывая прогрессирующую иммунологическую недостаточность и высокий риск развития лимфоидных неоплазий с неопределённым потенциалом излечения, мы считаем оправданным проведение аллогенной ТГСК с немиелоаблативным режимом кондиционирования пациентам с СН с тяжелой иммунологической недостаточностью или с лимфомой/лейкозом в 1ПР.
Регулярные статьи
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1203
[1] => 1204
[2] => 1205
[3] => 1206
[4] => 1207
[5] => 1208
[6] => 1209
)
[VALUE] => Array
(
[0] => 43
[1] => 44
[2] => 45
[3] => 46
[4] => 47
[5] => 48
[6] => 49
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 43
[1] => 44
[2] => 45
[3] => 46
[4] => 47
[5] => 48
[6] => 49
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 224
[VALUE] => 13.04.2015 13:38:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 13.04.2015 13:38:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 225
[VALUE] => 12.06.2015 13:39:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 12.06.2015 13:39:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 902
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 226
[VALUE] => 33
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 33
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 227
[1] => 228
[2] => 229
[3] => 230
[4] => 231
[5] => 232
[6] => 233
[7] => 234
[8] => 235
[9] => 236
[10] => 237
)
[VALUE] => Array
(
[0] => 39
[1] => 34
[2] => 33
[3] => 38
[4] => 11
[5] => 37
[6] => 36
[7] => 40
[8] => 42
[9] => 35
[10] => 41
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
[7] =>
[8] =>
[9] =>
[10] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 39
[1] => 34
[2] => 33
[3] => 38
[4] => 11
[5] => 37
[6] => 36
[7] => 40
[8] => 42
[9] => 35
[10] => 41
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
[7] =>
[8] =>
[9] =>
[10] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 238
[VALUE] => Array
(
[TEXT] => <p class="Autor">Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская<sup>
</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 239
[VALUE] => Array
(
[TEXT] => <p class="Summery_Rus" lang="ru-RU">Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти <span lang="en-US">HLA</span>-совместимого донора с гомозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32. Алло-ТГСК от донора без мутации гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена <span lang="en-US">CCR</span>5 <span lang="en-US">del</span> 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена CCR5 del 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена CCR5 del 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти HLA-совместимого донора с гомозиготной мутацией гена CCR5 del 32. Алло-ТГСК от донора без мутации гена CCR5 del 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена CCR5 del 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 240
[VALUE] => 10.18620/1866-8836-2015-4-1-2-24-30
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-24-30
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 241
[VALUE] => Array
(
[TEXT] => <p class="Autor">Boris V. Afanasyev<sup>1</sup>, Marina Popova<sup>1</sup>, Sergey Bondarenko<sup>1</sup>, Ilya Zyuzgin<sup>2</sup>, Elena Babenko<sup>1</sup>, Aleksander Alyanskiy<sup>1</sup>, Susanne Morsch<sup>3</sup>, Jan van Lunzen<sup>4</sup>, Boris Fehse<sup>5</sup>, Axel R. Zander <sup>5</sup>, Ludmila S. Zubarovskaya<sup>1</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Boris V. Afanasyev1, Marina Popova1, Sergey Bondarenko1, Ilya Zyuzgin2, Elena Babenko1, Aleksander Alyanskiy1, Susanne Morsch3, Jan van Lunzen4, Boris Fehse5, Axel R. Zander 5, Ludmila S. Zubarovskaya1
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 242
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">
<sup>1</sup>Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation,
</p>
<p class="Autor_place_work">
First Pavlov State Medical University of Saint-Petersburg, Russia
</p>
<p class="Autor_place_work">
<sup>2</sup>Oncology, Hematology and BMT department, Petrov Research Institute of Oncology, Saint-Petersburg, Russia
</p>
<p class="Autor_place_work">
<sup>3</sup>Stefan Morsch Stiftung, Birkenfeld, Germany
</p>
<p class="Autor_place_work">
<sup>4</sup>Infectious Diseases Unit, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
</p>
<p class="Autor_place_work">
<sup>5</sup>Clinic for Stem Cell Transplantation, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
</p>
<p class="Autor_place_work">
Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation
</p>
<p class="Autor_place_work">
First Pavlov State Medical University of Saint-Petersburg, Russia
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] =>
1Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation,
First Pavlov State Medical University of Saint-Petersburg, Russia
2Oncology, Hematology and BMT department, Petrov Research Institute of Oncology, Saint-Petersburg, Russia
3Stefan Morsch Stiftung, Birkenfeld, Germany
4Infectious Diseases Unit, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
5Clinic for Stem Cell Transplantation, University Medical Center Hamburg-Eppendorf, Hamburg, Germany
Raisa Gorbacheva Memorial Institute of Children Oncology, Hematology and Transplantation
First Pavlov State Medical University of Saint-Petersburg, Russia
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 243
[VALUE] => Array
(
[TEXT] => <h2 class="Summery"> <span style="font-family: Arial, sans-serif;">Summery</span><br>
</h2>
<p class="Summery">
Introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown with only limited case reports and small series. Most of these patients are potentially curable from hematological malignancies by allo-HSCT. Allo-HSCT from donor with homozygote CCR5 del 32 mutation can cure from the both diseases: HIV and cancer that was demonstrated by the Berlin patient. Prevalence of this mutation is low and this way seems unacceptable in most HIV-positive patients with high-risk hematologic malignancies. Allo-HSCT from donor without CCR5 mutation with ongoing HAART has looked more promising but has failed which was reported as Boston patients. But other aspects including donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and new agent therapy in HIV-patients maintain interest to allo-HSCT as a potential cure procedure. It was not reported an allo-HSCT from donor with heterozygote CCR5 del 32 mutation. An application of HAART in post-transplant period can be used not only for HIV control also as a component of GvHD prophylaxis. We report on three HIV-infected patients with high-risk acute leukemia which have undergone an allo-HSCT and donor lymphocyte infusions (DLI) to treat post-allo-HSCT relapse in Saint-Petersburg.
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Summery
Introduction of highly active antiretroviral therapy (HAART) in 1996 changed the situation with human immunodeficiency virus (HIV) infection management. HIV-infected patients remain at an increased risk of hematologic malignances for which hematopoietic stem cell transplantation (HSCT) is considered standard therapy. Chemotherapy (CT), including high-dose CT with autologous hematopoietic stem cell transplantation (auto-HSCT) in patients with HIV-associated lymphomas and well-controlled HIV infection on HAART has similar outcomes compared with patients without HIV infection. However, the outcome of HIV-patients after allogeneic hematopoietic stem cells transplantation (allo-HSCT) is unknown with only limited case reports and small series. Most of these patients are potentially curable from hematological malignancies by allo-HSCT. Allo-HSCT from donor with homozygote CCR5 del 32 mutation can cure from the both diseases: HIV and cancer that was demonstrated by the Berlin patient. Prevalence of this mutation is low and this way seems unacceptable in most HIV-positive patients with high-risk hematologic malignancies. Allo-HSCT from donor without CCR5 mutation with ongoing HAART has looked more promising but has failed which was reported as Boston patients. But other aspects including donor type, conditioning regimen, graft-versus-host disease (GvHD) prophylaxis, post-transplant immunoadoptive and new agent therapy in HIV-patients maintain interest to allo-HSCT as a potential cure procedure. It was not reported an allo-HSCT from donor with heterozygote CCR5 del 32 mutation. An application of HAART in post-transplant period can be used not only for HIV control also as a component of GvHD prophylaxis. We report on three HIV-infected patients with high-risk acute leukemia which have undergone an allo-HSCT and donor lymphocyte infusions (DLI) to treat post-allo-HSCT relapse in Saint-Petersburg.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 244
[VALUE] => Saint-Petersburg experience of allogeneic hematopoietic stem cell transplantation in patients with acute leukemia and human immunodeficiency virus
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Saint-Petersburg experience of allogeneic hematopoietic stem cell transplantation in patients with acute leukemia and human immunodeficiency virus
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1210
[VALUE] => 14
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 14
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1211
[VALUE] => 15
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 15
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Борис В. Афанасьев, Марина Попова, Сергей Бондаренко, Илья Зюзгин, Елена Бабенко, Александр Алянский, Сюзанна Морш, Ян ван Лунзен, Борис Фезе, Аксель Цандер, Людмила С. Зубаровская
Внедрение высокоактивной антиретровирусной терапии (ВААРТ) в 1996 году изменило ситуацию с лечением ВИЧ-инфекции. Несмотря на широкое применение ВААРТ, пациенты с ВИЧ по-прежнему относятся к группе высокого риска развития злокачественных опухолей кроветворной и лимфатической ткани. Трансплантация гемопоэтических стволовых клеток (ТГСК) является стандартным лечением для большинства этих опухолей. Противоопухолевая химиотерапия (ПХТ), включая высокодозную ПХТ с аутологичной ТГСК, так же эффективна как у пациентов без ВИЧ при применении ВААРТ. В то время как результаты аллогенной ТГСК (алло-ТГСК) неизвестны, публикации ограничены отдельными случаями или небольшими группами пациентов. Часть пациентов потенциально могут быть излечены от двух заболеваний при проведении алло-ТГСК от донора с гомозиготной мутацией гена CCR5 del 32: злокачественная опухоль и ВИЧ, что было продемонстрировано у «Берлинского пациента». Встречаемость мутации гена CCR5 del 32 в популяции невысока, такой способ лечения малоперспективен для большинства пациентов с ВИЧ и онкогематологическим заболеванием из-за низкой вероятности найти HLA-совместимого донора с гомозиготной мутацией гена CCR5 del 32. Алло-ТГСК от донора без мутации гена CCR5 del 32 на фоне ВААРТ выглядело более перспективным, но опыт «Бостонских пациентов» продемонстрировал неэффективность такого подхода. При этом, другие аспекты, включающие тип донора, режим кондиционирования и профилактики РТПХ, посттрансплантационную иммуноадоптивную терапию, поддерживают интерес к алло-ТГСК у пациентов с ВИЧ, как потенциального метода излечения от двух заболеваний. Нет опубликованных данных об алло-ТГСК от донора с гетерозиготной мутацией гена CCR5 del 32, а ВААРТ в посттрансплантационном периоде может быть использована в качестве компонента профилактики РТПХ. Мы представляем собственный опыт алло-ТГСК у пациентов с острыми лейкозами и ВИЧ-инфекцией, выполненные в Санкт-Петербурге.
Регулярные статьи
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1188
[1] => 1189
[2] => 1190
[3] => 1191
[4] => 1192
)
[VALUE] => Array
(
[0] => 21
[1] => 22
[2] => 23
[3] => 24
[4] => 25
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 21
[1] => 22
[2] => 23
[3] => 24
[4] => 25
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 43
[VALUE] => 08.03.2015 10:43:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.03.2015 10:43:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 44
[VALUE] => 23.06.2015 10:43:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 23.06.2015 10:43:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 867
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 13
[VALUE] => 7
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 7
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 39
[1] => 40
[2] => 41
)
[VALUE] => Array
(
[0] => 8
[1] => 10
[2] => 7
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 8
[1] => 10
[2] => 7
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 14
[VALUE] => Array
(
[TEXT] => <p class="Autor_Rus" lang="ru-RU">Тапани Рууту<sup>1</sup>, Христиан Кенеке<sup>2</sup>, Гжегож В. Басак<sup>3</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Тапани Рууту1, Христиан Кенеке2, Гжегож В. Басак3
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 118
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work-Rus"><sup>1</sup>Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;</p>
<p class="Autor_place_work-Rus"><sup>2</sup>Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;</p>
<p class="Autor_place_work-Rus"><sup>3</sup>Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 1Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;
2Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;
3Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 119
[VALUE] => Array
(
[TEXT] => <h2>Резюме</h2>
<p class="Summery_Rus ParaOverride-6" lang="ru-RU">Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО. </p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.</p><p class="Summery_Rus ParaOverride-6" lang="ru-RU">Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа. </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Резюме
Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО.
Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.
У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.
Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.
Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 15
[VALUE] => 10.18620/1866-8836-2015-4-1-2-14-18
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-14-18
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 120
[VALUE] => Array
(
[TEXT] => <p class="Autor">Tapani Ruutu<sup>1</sup>, Christian Koenecke<sup>2</sup> and Grzegorz W. Basak<sup>3</sup></p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Tapani Ruutu1, Christian Koenecke2 and Grzegorz W. Basak3
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19
[VALUE] => Array
(
[TEXT] => <sup>1</sup>Helsinki University Central Hospital, Comprehensive Cancer Center, Stem Cell Transplantation Unit, Helsinki, Finland;<br>
<sup>2</sup>Hannover Medical School, Department of Hematology, Hemostasis, Oncology and Stem-Cell Transplantation, Hannover, Germany;<br>
<sup>3</sup>The Medical University of Warsaw, Department of Hematology, Oncology and Internal Diseases, Poland
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 1Helsinki University Central Hospital, Comprehensive Cancer Center, Stem Cell Transplantation Unit, Helsinki, Finland;
2Hannover Medical School, Department of Hematology, Hemostasis, Oncology and Stem-Cell Transplantation, Hannover, Germany;
3The Medical University of Warsaw, Department of Hematology, Oncology and Internal Diseases, Poland
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 42
[VALUE] => Array
(
[TEXT] => <h2>Summary</h2>
<p>
The present review is largely based on two surveys on patients who have undergone both an allogeneic hematopoietic stem cell transplantation (HSCT) and a solid organ transplantation (SOT), carried out by the European Society for Blood and Marrow Transplantation (EBMT). Some additional references to the literature are included. From these sources of data it can be summarized that SOT represents a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic SCT and experience long-term survival without loss of organ function.
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Summary
The present review is largely based on two surveys on patients who have undergone both an allogeneic hematopoietic stem cell transplantation (HSCT) and a solid organ transplantation (SOT), carried out by the European Society for Blood and Marrow Transplantation (EBMT). Some additional references to the literature are included. From these sources of data it can be summarized that SOT represents a valuable treatment strategy in HSCT recipients who develop an organ failure. In stringently selected young patients, the overall and organ survivals appear to be comparable to patients undergoing SOT for other causes. Complications, such as infections and graft rejection are frequent but usually manageable. Thus, SOT offers a viable therapeutic option for selected patients with single organ failure after HSCT. Also, selected SOT recipients suffering from hematologic disorders may benefit from allogeneic SCT and experience long-term survival without loss of organ function.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 20
[VALUE] => Allogeneic hematopoietic stem cell transplantation and solid organ transplantation in the same patient
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Allogeneic hematopoietic stem cell transplantation and solid organ transplantation in the same patient
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1193
[VALUE] => 10
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1194
[VALUE] => 11
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 11
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Тапани Рууту1, Христиан Кенеке2, Гжегож В. Басак3
1Центральный госпиталь Университета Хельсинки, Центр исследований рака, Отделение трансплантации стволовых клеток, Хельсинки, Финляндия;
2Высшая медицинская Школа Ганновера, Отдел Гематологии и гемостаза, Ганновер, Германия;
3Варшавский медицинский университет, Отдел гематологии, онкологии и внутренних болезней, Варшава, Польша
Резюме
Трансплантация солидных органов (ТСО) широко применяется для лечения пациентов с органной недостаточностью терминальной степени. Аллогенная трансплантация гемопоэтических стволовых клеток (ТГСК) представляет собой метод интенсивной терапии , который сам по себе часто вызывает повреждение и недостаточность различных органов, что является потенциальным показанием к ТСО.
Настоящий обзор основан, в основном, на нескольких небольших исследованиях больных, которым выполнялась как ТГСК, так и ТСО, проведенных под эгидой Европейского общества трансплантации костного мозга в группе. Так, Koenecke et al. опубликовали сводку по 107 трансплантационным центрам, где проведено 67000 аллогенных ТГСК с 1984 по 2007 гг. Из них, В 28 центрах были выполнены 45 ТСО в связи с органной недостаточностью после ТГСК, в том числе 15 пересадок почек, 15 – печени, 13 – легких lung, 1 – сердца. Кроме того, рассматриваются и данные о ряде других исследований, в частности анализ результатов трансплантации легких, выполненных в связи с облитерирующим альвеолитом на фоне хронической реакции «трансплантат против хозяина» после аллогенной ТГСК, проведенной для лечения онкогематологических заболеваний (Holm et al., 2013). Средний срок от ТГСКT до пересадки легких составил 8,2 года (от 0,7 до 16 лет) при возрасте пациентов от 16 до 55 лет. При средних сроках наблюдения 4,2 года, выживаемость больных составила 90% через 1 год и 75% через 5 лет после пересадки легких.
У реципиентов кроветворных клеток с применением ТСО после ТГСК, весьма вероятны иммунологические осложнения. Стратегии иммуносупрессии, принятые при этих двух типах трансплантации, существенно различаются. Однако частота отторжения трансплантата незначительно отличается от той, которая наблюдается у пациентов после пересадки солидных органов. Возникновение или отсутствие реакции «трансплантат против хозяина» несущественно влияет на конечный исход.
Существует множество вероятных механизмов отторжения трансплантата в этих ситуациях. Так, иммунный ответ может быть направлен против чужеродных молекул HLA, так как HLA-совместимость кроветворного трансплантата с тканями реципиента намного выше, чем совместимость донорского органа. Однако можно предположить, что алло-ТГСК может оказать и толерогенный эффект, позволяющий сохранить солидный орган без иммуносупрессии. Кондиционирование перед аллогенной ТГСК и инфекционные осложнения могут повысить иммуногенность пересаженного органа посредством повышения уровней презентации антигенов, повышения костимулирующих сигналов, изменений свойств сосудистого эндотелия и ингибируюших влияний Т-регуляторных клеток. В то же время большинство донорских органов подобраны к пациенту по группам крови, что не требуется для доноров гемопоэтических клеток. Таким образом, большинство кроветворных трансплантатов несовместимы с тканями солидного органа, что может повлиять на его переживание. Кроме того, у большинства больных после ТСО и ТГСК иммуносупрессивные режимы изменяются на протоколы, применяемые при алло-ТГСК, что может быть недостаточным в данной ситуации.
Исходя из вышесказанного, можно заключить, что ТСО представляет собой полезную тактику лечения у пациентов после ТГСК с осложнениями в виде органной недостаточности. При тщательном отборе молодых пациентов, общая выживаемость и переживание органа, по-видимому, сравнимы с показателями общего контингента больных после ТСО. Часты осложнения, такие, как инфекции и отторжение трансплантата, но они обычно поддаются терапии. Следовательно, ТСО является важным вариантом лечения для некоторых пациентов с органной недостаточностью после ТГСК. Кроме того, некоторые реципиенты солидных органов при развитии гематологических заболеваний могут выиграть от аллогенной ТГСК и жить в течение длительных сроков без утраты функций органа.
Регулярные статьи
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1195
[1] => 1196
[2] => 1197
[3] => 1198
[4] => 1199
[5] => 1200
)
[VALUE] => Array
(
[0] => 27
[1] => 28
[2] => 29
[3] => 30
[4] => 31
[5] => 18
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 27
[1] => 28
[2] => 29
[3] => 30
[4] => 31
[5] => 18
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 141
[VALUE] => 13.04.2015 10:43:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 13.04.2015 10:43:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 142
[VALUE] => 05.06.2015 10:43:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 05.06.2015 10:43:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 879
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 143
[VALUE] => 26
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 26
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 144
)
[VALUE] => Array
(
[0] => 26
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 26
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 145
[VALUE] => Array
(
[TEXT] => <p class="Autor_Rus" lang="ru-RU">Дитер Хельцер</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Дитер Хельцер
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 146
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work-Rus">Университет Й.-В. Гете, Франкфурт-на Майне, Германия </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Университет Й.-В. Гете, Франкфурт-на Майне, Германия
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 147
[VALUE] => Array
(
[TEXT] => <p class="Summery_Rus" lang="ru-RU">Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка. </p>
<p class="Summery_Rus" lang="ru-RU">Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена. </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка.
Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 148
[VALUE] => 10.18620/1866-8836-2015-4-1-2-19-23
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-19-23
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 149
[VALUE] => Array
(
[TEXT] => <p class="Autor">Dieter Hoelzer </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Dieter Hoelzer
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 150
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">J. W. Goethe University, Frankfurt </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => J. W. Goethe University, Frankfurt
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 151
[VALUE] => Array
(
[TEXT] => <h2>Summery</h2>
<p class="Summery">
There exist standard molecular methods of minimal residual disease (MRD) evaluation in acute lymphoblastic leukemia (ALL), in order to detect leukemic blast cells (LBC) not assessable by microscopy of bone marrow. The best time point for MRD evaluation and MRD-based treatment stratification in ALL is shown to be ca.14-16 weeks after induction/ consolidation treatment. Reduction of MRD load before SCT, as a next step of therapy, is quite desirable. E.g., induction and consolidation treatment with tyrosine kinase inhibitors (NKI) increase the molecular CR rate compared to conventional chemotherapy, as measured by the quantitative RT-PCR assays of bcr/abl fusion oncogene. Failure of treatment by molecular criteria identifies the worst ALL subgroup. Several window studies in ALL with new cytostatic drugs (TKIs or MoABs) were aimed to reduce the tumor load before SCT. Moreover, novel immunotherapeutic approaches include application of monoclonal antibodies against specific surface antigens typical to certain differentiation steps in B-lineage.
</p>
<p class="Summery">
Hence, evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies. Targeted therapy with TKI has improved the outcome for adult Ph+ ALL patients substantially, evidently by an increased molecular remission rate, and a substantial improvement of survival after SCT. Meanwhile, maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. Maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known.
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Summery
There exist standard molecular methods of minimal residual disease (MRD) evaluation in acute lymphoblastic leukemia (ALL), in order to detect leukemic blast cells (LBC) not assessable by microscopy of bone marrow. The best time point for MRD evaluation and MRD-based treatment stratification in ALL is shown to be ca.14-16 weeks after induction/ consolidation treatment. Reduction of MRD load before SCT, as a next step of therapy, is quite desirable. E.g., induction and consolidation treatment with tyrosine kinase inhibitors (NKI) increase the molecular CR rate compared to conventional chemotherapy, as measured by the quantitative RT-PCR assays of bcr/abl fusion oncogene. Failure of treatment by molecular criteria identifies the worst ALL subgroup. Several window studies in ALL with new cytostatic drugs (TKIs or MoABs) were aimed to reduce the tumor load before SCT. Moreover, novel immunotherapeutic approaches include application of monoclonal antibodies against specific surface antigens typical to certain differentiation steps in B-lineage.
Hence, evaluation of minimal residual disease is a new parameter for treatment stratification. The conversion of MRD-positivity to MRD-negativity is also a new endpoint for studies. Targeted therapy with TKI has improved the outcome for adult Ph+ ALL patients substantially, evidently by an increased molecular remission rate, and a substantial improvement of survival after SCT. Meanwhile, maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known. Maintenance with a TKI is recommended after SCT, whereby the optimal duration is so far not known.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 152
[VALUE] => MRD evaluation, targeted therapy and stem cell transplantation: how to combine in adult ALL
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => MRD evaluation, targeted therapy and stem cell transplantation: how to combine in adult ALL
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1201
[VALUE] => 12
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 12
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1202
[VALUE] => 13
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 13
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Дитер Хельцер
Университет Й.-В. Гете, Франкфурт-на Майне, Германия
Существуют стандартные молекулярные методы и оценки минимальной остаточной болезни (MОД) при остром лимфобластном лейкозе (ОЛЛ), чтобы выявлять лейкозные костном мозге бласты, не выявляемые с помощью микроскопии. Наилучший период для оценки МОД и основанной на ней стратификации терапии при ОЛЛ – примерно 14-16 недель после индукции/консолидации. Снижение уровня МОД весьма желательно после трансплантации гемопоэтических стволовых клеток (ТГСК) как следующего этапа лечения. Например, индукция и консолидация ремиссии ингибиторами тирозинкиназы (ИТК) повышает частоту молекулярной ремиссии, в сравнении с обычной химиотерапией, по данным количественной ПЦР онкогена bcr/abl. Неудачный исход лечения по молекулярным критериям идентифицирует подгруппу ОЛЛ с худшими исходами. Несколько «интервальных» исследований при ОЛЛ с применением новых цитостатиков (ИТК и моноклональных антител) были направлены на снижение опухолевой нагрузки перед ТГСК. Кроме того, новые иммунотерапевтические подходы включают в себя применение антител к специфическим поверхностным антигенам, характерным для определенных этапов дифференцировки В-клеточного ростка.
Таким образом, оценка МОД является новым параметром для назначения схем лечения. Переход от МОД-позитивности к МОД-негативности также является отдельным критерием исхода в клинических исследованиях. Целевая терапия ИТК значительно улучшила исходы лечения взрослых пациентов с Ph+ ОЛЛ по более высоким показателям частоты молекулярной ремиссии и существенному увеличению выживаемости после ТГСК. В то же время, после ТГСК рекомендуется поддерживающая терапия ИТК причем ее оптимальная длительность до сих пор не выяснена.
Короткие сообщения
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1247
[1] => 1248
[2] => 1249
)
[VALUE] => Array
(
[0] => 98
[1] => 99
[2] => 100
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 98
[1] => 99
[2] => 100
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 560
[VALUE] => 06.04.2015 17:19:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 06.04.2015 17:19:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 561
[VALUE] => 05.06.2015 17:20:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 05.06.2015 17:20:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 906
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 562
[VALUE] => 97
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 97
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 563
)
[VALUE] => Array
(
[0] => 97
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 97
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 564
[VALUE] => Array
(
[TEXT] => <p class="Autor_Rus" lang="ru-RU">Джоэл Гловер</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Джоэл Гловер
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 565
[VALUE] => Array
(
[TEXT] => <span class="CharOverride-18" lang="en-GB">Институт фундаментальных медицинских наук, Медицинский факультет Университета Осло</span>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Институт фундаментальных медицинских наук, Медицинский факультет Университета Осло
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 566
[VALUE] => 10.18620/1866-8836-2015-4-1-2-66-68
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-66-68
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 567
[VALUE] => Array
(
[TEXT] => <p class="Autor">Joel C. Glover</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Joel C. Glover
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 568
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">Institute of Basic Medical Sciences, The University of Oslo Medical Faculty</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Institute of Basic Medical Sciences, The University of Oslo Medical Faculty
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 569
[VALUE] => From cartilage to cancer: Translational research at the Norwegian Center for Stem Cell Research
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => From cartilage to cancer: Translational research at the Norwegian Center for Stem Cell Research
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 1011
[VALUE] => Array
(
[TEXT] => <p>
Доклад представляет исследовательскую деятельность Норвежского центра изучения стволовых клеток, расположенного в Университетском госпитале Осло и Институте фундаментальных медицинских наук университета Осло. Работы Центра сосредоточены на продукции индуцированных полипотентных клеток, их дифференцировке, характеризации и генной модификации (методики TALEN и CRISPR/CAS), роли эпигенетики и репарации ДНК в дифференцировке стволовых клеток, а также в нейровизуализации и функциональной оценке, включая нейро-оптогенетику. Медицинский факультет Университета Осло заключает двусторонние соглашения с исследовательскими и учебными организациями Санкт-Петербурга.
</p>
<p>
Репарация гиалинового хряща сейчас является одной из основных задач экспериментальных и клинических исследований Центра в рамках проектов (руководитель – Ян Бринчманн). Размноженные <em>in vitro</em> хондроциты используются для замещения гиалинового хряща, но обычно они развиваются в фиброзный хрящ. Лаборатория Бринчманна выявила несколько факторов, относящихся к хондрогенезу мезенхимных стволовых клеток человека <em>in vitro</em>, что было показано с помощью высокоразрешающего типирования мРНК (Brinchmann et al., 2012). В настоящее время идет сотрудничество с руководителем группы Джудит Стерк по применению технологий TALEN/CRISPR для направленных генетических манипуляций. Система CRISPR/Cas может использоваться для адресации Cas9 в конкретные области генома, где она осуществляет двунитевые разрезы ДНК. Регулирующая система включает в себя некодирующую «ведущую» РНК (gRNA), tracrRNA и белок Cas9. Группа Стерк применила эту систему для разработки человеческих полипотентных стволовых клеток (iPS/ES) с флуоресцентными маркерами в генных локусах Brachyury, Flk1, CD34 и CD45 и внедрила их в моделях <em>in vitro</em> миелодиспластического синдрома, включая генные модификации гемопоэтических стволовых клеток. Группа Стерк также осуществляет дифференцировку эмбриональных клеток человека в кроветворные предшественники, а также работает по экспансии и поддержании культур CD34+ клеток пуповинной крови.
</p>
<p>
Поиск физиологически адекватных моделей тканей включает и разработку трехмерных систем клеточных культур, являющихся новыми технологическими платформами для тканевой инженерии <em>in vitro</em>. Руководители групп Гаррет Салливэн и Джоэл Гловер применяют трехмерную принтерную технологию для создания многоклеточных структур печеночной и нервной ткани. Такие трехмерные клеточные системы в аспекте стволовых клеток человека и их производных могут быть использованы для изучения различных наследственных заболеваний, поражающих гепатоциты, нейроны, кардиомиоциты и т.д.
</p>
<p>
В области онкологии, усилия Центра в настоящее время сконцентрированы на дендритоклеточной вакцине для лечения глиобластомы в клиническом проекте, руководимом Ивером Лангменом, совместно с руководителями групп Гуннаром Квалхеймом и Бринчманном. Терапевтическая вакцинация против аутологичных стволовых раковых клеток применяется уже десятилетиями. Однако можно ожидать лучшей эффективности такого лечения, используя дендритные клетки, трансфицированные мРНК из клеток глиобластомы от пациентов. Проведена фаза I/II испытаний вакцинотерапии с применением дендритных клеток, трансфицированных мРНК hTERT, сурвивина из клеток глиобластомы. Среди позитивных эффектов такой терапии - уменьшение размера опухоли и увеличение средней выживаемости без прогрессии заболевания (19,9 мес. у больных леченных вакциной из дендритных клеток) по сравнению с 7,9 мес. при стандартном лечении.
</p>
<p>
Центр имеет два блока для производства клеток по стандартам GMP в целях культивирования аутологичных клеток и амплификации мРНК, обеспечивающих производство человеческих стволовых клеток и их дифференцированных производных в условиях строгого контроля, согласно директивам и правилам Европейского Союза.
</p>
<p>
Трансляционные исследования стволовых клеток определены среди национальных приоритетов в Норвегии, что ведет к обустройству Центра по инициативе Министерства здравоохранении. Центр также поддерживает Национальную лабораторию по производству, хранению и оценке плюрипотентных стволовых клеток человека – единственную подобную структуру в Норвегии. Это учреждение стало применять технологию индуцируемых плюрипотентных стволовых клеток (iPS) в 2012 г., и его услуги доступны норвежским и зарубежным исследователям.
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] =>
Доклад представляет исследовательскую деятельность Норвежского центра изучения стволовых клеток, расположенного в Университетском госпитале Осло и Институте фундаментальных медицинских наук университета Осло. Работы Центра сосредоточены на продукции индуцированных полипотентных клеток, их дифференцировке, характеризации и генной модификации (методики TALEN и CRISPR/CAS), роли эпигенетики и репарации ДНК в дифференцировке стволовых клеток, а также в нейровизуализации и функциональной оценке, включая нейро-оптогенетику. Медицинский факультет Университета Осло заключает двусторонние соглашения с исследовательскими и учебными организациями Санкт-Петербурга.
Репарация гиалинового хряща сейчас является одной из основных задач экспериментальных и клинических исследований Центра в рамках проектов (руководитель – Ян Бринчманн). Размноженные in vitro хондроциты используются для замещения гиалинового хряща, но обычно они развиваются в фиброзный хрящ. Лаборатория Бринчманна выявила несколько факторов, относящихся к хондрогенезу мезенхимных стволовых клеток человека in vitro, что было показано с помощью высокоразрешающего типирования мРНК (Brinchmann et al., 2012). В настоящее время идет сотрудничество с руководителем группы Джудит Стерк по применению технологий TALEN/CRISPR для направленных генетических манипуляций. Система CRISPR/Cas может использоваться для адресации Cas9 в конкретные области генома, где она осуществляет двунитевые разрезы ДНК. Регулирующая система включает в себя некодирующую «ведущую» РНК (gRNA), tracrRNA и белок Cas9. Группа Стерк применила эту систему для разработки человеческих полипотентных стволовых клеток (iPS/ES) с флуоресцентными маркерами в генных локусах Brachyury, Flk1, CD34 и CD45 и внедрила их в моделях in vitro миелодиспластического синдрома, включая генные модификации гемопоэтических стволовых клеток. Группа Стерк также осуществляет дифференцировку эмбриональных клеток человека в кроветворные предшественники, а также работает по экспансии и поддержании культур CD34+ клеток пуповинной крови.
Поиск физиологически адекватных моделей тканей включает и разработку трехмерных систем клеточных культур, являющихся новыми технологическими платформами для тканевой инженерии in vitro. Руководители групп Гаррет Салливэн и Джоэл Гловер применяют трехмерную принтерную технологию для создания многоклеточных структур печеночной и нервной ткани. Такие трехмерные клеточные системы в аспекте стволовых клеток человека и их производных могут быть использованы для изучения различных наследственных заболеваний, поражающих гепатоциты, нейроны, кардиомиоциты и т.д.
В области онкологии, усилия Центра в настоящее время сконцентрированы на дендритоклеточной вакцине для лечения глиобластомы в клиническом проекте, руководимом Ивером Лангменом, совместно с руководителями групп Гуннаром Квалхеймом и Бринчманном. Терапевтическая вакцинация против аутологичных стволовых раковых клеток применяется уже десятилетиями. Однако можно ожидать лучшей эффективности такого лечения, используя дендритные клетки, трансфицированные мРНК из клеток глиобластомы от пациентов. Проведена фаза I/II испытаний вакцинотерапии с применением дендритных клеток, трансфицированных мРНК hTERT, сурвивина из клеток глиобластомы. Среди позитивных эффектов такой терапии - уменьшение размера опухоли и увеличение средней выживаемости без прогрессии заболевания (19,9 мес. у больных леченных вакциной из дендритных клеток) по сравнению с 7,9 мес. при стандартном лечении.
Центр имеет два блока для производства клеток по стандартам GMP в целях культивирования аутологичных клеток и амплификации мРНК, обеспечивающих производство человеческих стволовых клеток и их дифференцированных производных в условиях строгого контроля, согласно директивам и правилам Европейского Союза.
Трансляционные исследования стволовых клеток определены среди национальных приоритетов в Норвегии, что ведет к обустройству Центра по инициативе Министерства здравоохранении. Центр также поддерживает Национальную лабораторию по производству, хранению и оценке плюрипотентных стволовых клеток человека – единственную подобную структуру в Норвегии. Это учреждение стало применять технологию индуцируемых плюрипотентных стволовых клеток (iPS) в 2012 г., и его услуги доступны норвежским и зарубежным исследователям.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1250
[VALUE] => 26
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 26
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1251
[VALUE] => 27
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 27
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Джоэл Гловер
Короткие сообщения
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1235
[1] => 1236
[2] => 1237
[3] => 1238
)
[VALUE] => Array
(
[0] => 88
[1] => 89
[2] => 15
[3] => 91
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 88
[1] => 89
[2] => 15
[3] => 91
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 503
[VALUE] => 27.03.2015 16:45:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 27.03.2015 16:45:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 504
[VALUE] => 05.06.2015 16:46:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 05.06.2015 16:46:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 916
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 505
[VALUE] => 87
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 87
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 506
)
[VALUE] => Array
(
[0] => 87
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 87
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 507
[VALUE] => Array
(
[TEXT] => <p class="Autor_Rus" lang="ru-RU">
Рюдигер Хельманн
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] =>
Рюдигер Хельманн
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 508
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work-Rus">
Гейдельбергский университет, Германия
</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] =>
Гейдельбергский университет, Германия
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 509
[VALUE] => Array
(
[TEXT] => <h2>Резюме</h2>
<ul>
<li class="bullets">Встречаемость бластного криза низка – 5,6% после 8 лет</li>
<li class="bullets">Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК</li>
<li class="bullets">Лечение бластного криза в исследовании <span lang="en-US">CML</span> <span lang="en-US">Study</span> <span lang="en-US">IV</span> является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу. </li>
<li class="bullets">Пока отсутствуют рекомендации по специфическому лекарственному лечению. </li>
<li class="bullets">Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ. </li>
<li class="bullets ParaOverride-5">Европейская организация <span lang="en-US">ELN</span> рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.</li>
</ul>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Резюме
- Встречаемость бластного криза низка – 5,6% после 8 лет
- Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК
- Лечение бластного криза в исследовании CML Study IV является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу.
- Пока отсутствуют рекомендации по специфическому лекарственному лечению.
- Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ.
- Европейская организация ELN рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.
Rüdiger Hehlmann
[TYPE] => html ) [~DESCRIPTION] => [~NAME] => Author [~DEFAULT_VALUE] => Array ( [TEXT] => [TYPE] => HTML ) ) [ORGANIZATION_EN] => Array ( [ID] => 38 [TIMESTAMP_X] => 2015-09-02 18:02:59 [IBLOCK_ID] => 2 [NAME] => Organization [ACTIVE] => Y [SORT] => 500 [CODE] => ORGANIZATION_EN [DEFAULT_VALUE] => Array ( [TEXT] => [TYPE] => HTML ) [PROPERTY_TYPE] => S [ROW_COUNT] => 1 [COL_COUNT] => 30 [LIST_TYPE] => L [MULTIPLE] => N [XML_ID] => 38 [FILE_TYPE] => [MULTIPLE_CNT] => 5 [TMP_ID] => [LINK_IBLOCK_ID] => 0 [WITH_DESCRIPTION] => N [SEARCHABLE] => N [FILTRABLE] => N [IS_REQUIRED] => N [VERSION] => 1 [USER_TYPE] => HTML [USER_TYPE_SETTINGS] => Array ( [height] => 200 ) [HINT] => [PROPERTY_VALUE_ID] => 512 [VALUE] => Array ( [TEXT] => <span class="CharOverride-5" lang="en-US">Universität Heidelberg, Germany</span> [TYPE] => html ) [DESCRIPTION] => [VALUE_ENUM] => [VALUE_XML_ID] => [VALUE_SORT] => [~VALUE] => Array ( [TEXT] => Universität Heidelberg, Germany [TYPE] => html ) [~DESCRIPTION] => [~NAME] => Organization [~DEFAULT_VALUE] => Array ( [TEXT] => [TYPE] => HTML ) ) [SUMMARY_EN] => Array ( [ID] => 39 [TIMESTAMP_X] => 2015-09-02 18:02:59 [IBLOCK_ID] => 2 [NAME] => Description / Summary [ACTIVE] => Y [SORT] => 500 [CODE] => SUMMARY_EN [DEFAULT_VALUE] => Array ( [TEXT] => [TYPE] => HTML ) [PROPERTY_TYPE] => S [ROW_COUNT] => 1 [COL_COUNT] => 30 [LIST_TYPE] => L [MULTIPLE] => N [XML_ID] => 39 [FILE_TYPE] => [MULTIPLE_CNT] => 5 [TMP_ID] => [LINK_IBLOCK_ID] => 0 [WITH_DESCRIPTION] => N [SEARCHABLE] => N [FILTRABLE] => N [IS_REQUIRED] => N [VERSION] => 1 [USER_TYPE] => HTML [USER_TYPE_SETTINGS] => Array ( [height] => 200 ) [HINT] => [PROPERTY_VALUE_ID] => 513 [VALUE] => Array ( [TEXT] => <h2>Resume</h2> <ul> <li> Incidence of BC is low, with 5.6% after 8 years. </li> <li> Survival after BC not much improved with TKI. </li> <li> Treatment of BC in CML study IV is heterogeneous as expected without specific recommendations in the study protocol. </li> <li> No recommendation of a specific drug treatment is possible. </li> <li> Transplantation carries the best long term prognosis in BC. </li> <li> Allo SCT always recommended in BC by ELN. </li> </ul> [TYPE] => html ) [DESCRIPTION] => [VALUE_ENUM] => [VALUE_XML_ID] => [VALUE_SORT] => [~VALUE] => Array ( [TEXT] =>Resume
- Incidence of BC is low, with 5.6% after 8 years.
- Survival after BC not much improved with TKI.
- Treatment of BC in CML study IV is heterogeneous as expected without specific recommendations in the study protocol.
- No recommendation of a specific drug treatment is possible.
- Transplantation carries the best long term prognosis in BC.
- Allo SCT always recommended in BC by ELN.
Прогрессия хронического миелоидного лейкоза (ХМЛ) в бластный криз все еще является недостаточно изученным феноменом. Сообщается о наличии дополнительных хромосомных аберраций у пациентов с бластным кризом ХМЛ (до 90% случаев).
До 77% таких мутаций выявлены посредством глубокого геномного секвенирования. Согласно данным об профиле генной экспрессии, бластный кризис, видимо, является заболеванием, отличным от ХМЛ. Продолжение лечения, большей частью безуспешно, несмотря на возможность трансплантации гемопоэтических клеток (ТСК). Неудача терапии означает точку невозврата. Дополнительные хромосомные аберрации ассоциированы с развитием бластного криза, будучи неслучайными по распределению в хромосомах. Наиболее частыми аберрациями здесь являются: +8 (34%); +Ph (30%); i(17q) (20%); +19 (13%); +21 (7%); +17 (5%); моносомия 7 (5%). Временной порядок появления вторичных аномалий различен, чаще; i(17q), +8, +Ph, +19. Существуют определенные диагностические критерии для фазы акселерации (ФА) ХМЛ и бластного криза, т.е. ФА характеризуется 15 – 29% бластов в крови или костном мозге (по критериям ВОЗ – 10 – 19%), > 20% базофилов в крови, стойкой тромбоцитемией, независимо от лечения, нечувствительностью к терапии. Бластный криз диагностируется при >30% бластов в крови или костном мозге (по ВОЗ – 20%); экстрамедуллярной бластной инфильтрации, лихорадке различной степени, анемии, спленомегалии, лейкоцитозе. Рассматриваются различные средства предотвращения бластного криза при анализе исследований с 1983 по 2013 гг. Особое внимание уделяется ингибиторам тирозинкиназ (ИТК – иматиниб, нилотиниб, дазатиниб) для лечения бластного криза ХМЛ. Внедрение иматиниба приводило к небольшому повышению выживаемости больных (до 20% ). Наиболее долгоживущие пациенты – те, которым проводилась ТСК (28/39, ок. 72%).
Европейская организация European Leukemia Net (ELN) представила анализ результатов алло-ТГСК при бластном кризисе ХМЛ. Рассмотрены несколько подходов, т.е. ТСК должна применяться всегда в качестве второй линии терапии бластного криза, независимо от ответа на ИТК. Также всегда рекомендуется поступать в фазе акселерации, если ответ на ИТК недостаточен и, в качестве третьей линии терапии – если недостаточен ответ при лечении препаратами второй линии.
Оценка и значение понятия «Всегда» зависят от факторов индивидуального риска трансплантации (возраст, сопутствующие заболевания, физический статус, донор и др.).
Индукция 2-й хронической фазы или ремиссия только на ИТК или в комбинации с интенсивной химиотерапией изучалась несколькими группами авторов при различных режимах, а именно:
- Иматиниб 800 mg + Винкристин + Дексаметазон (DIV) (Rea et al., 2006) (LBC) (n = 13)
- Иматиниб + митоксантрон/этопозид + AraC (Frühauf et al., 2007), (MBC) ( n= 16)
- Иматиниб + дауномицин + AraC (Deau et al., 2011)
(n = 36) - Дазатиниб + FLAG-Идарубицин (Milojkovic et al., 2012), (n = 4)
Трансплантация гемопоэтических клеток от HLA-идентичного родственного тлт совместимого неродственного донора проводилась при статусе больных от 0 до 4 и стандартном кондиционировании. Режимы поддерживающей терапии ИТК изучались несколькими группами (Hehlmann et al., Blood, 2012; Rea et al., 2006; Frühauf et al., Cancer 2007; Deau et al., 2011; Milojkovic et al., 2012).
Применение алло-ТСК в качестве терапии второй линии оценивалось в исследовании CML Study IV (84 случая).
Выполнение ТСК после неудачной терапии иматинибом в 1-й хронической фазе сопровождалось выживаемостью 94%, тогда как ТСК в развернутой фазе ХМЛ приводило к 3-летней выживаемости 59% (Saußele et al., 2010). Сходные результаты были опубликованы Oyekunle et al. (2013).
Опыт лечения бластного криза был обобщен в исследовании CML Study IV (1551 пациентов).
Основным режимом было лечение Иматинибом (400 mg) + AraC и интенсивная химиотерапия. Специальная оценка в CML Study IV касалась уровней выживаемости после алло-ТГСК в бластном кризе, в зависимости от «предлеченности» больного crisis, однако количество пациентов было слишком малым для надежных выводов. Были проведены сравнения для бластных кризов миелоидного и лимфоидного типов. Лечение лимфоидного бластного криза было ассоциировано с несколько более длительным средним сроком жизни, нежели при миелоидном типе бластного криза. Дальнейший анализ данных продолжается. В разработке находятся и экспериментальные подходы в этой области терапии (Табл. 1)
|
Биологические эффекты |
Препараты/соединения |
|
Активация PP2A |
Fingolimod (FTY720) |
|
Антагонист SET OP449 |
|
|
Ингибитор CIP2A |
|
|
Самообновление ЛСК |
BCL6 + ингибиторы TK |
|
Ингибитор HIF1α |
|
|
Более мягкие ингибиторы (в сочетании с ИТК) |
|
|
Ингибитор Jak2 (в сочетании с ИТК) |
|
|
Активация апоптоза |
Ингибитор BCL2 ABT-737 |
|
Триптолид |
|
|
Двойной ингибитор киназы ON044580 |
|
|
Ингибитор MEK PD184352 + фарнезиотрансферазы Ингибитор BMS-214662 |
|
|
Прочее |
Пегилированный интерферон, ингибиторы гистондеацетилазы, ингибиторы Нsp90 |
Сокращения: ИТК: ингибитор тирозинкиназы; PP2A: протеинфосфатаза 2A; LSC: лейкозные стволовые клетки; MEK: митоген-активируемая протеинкиназа; HIF: фактор, индуцированный гипоксией; HDAC: гистондеацетилаза; Hsp: белок теплового шока.
Таблица 1. Экспериментальные походы к лечению бластного криза ХМЛ
[TYPE] => html ) [~DESCRIPTION] => [~NAME] => Полный текст [~DEFAULT_VALUE] => Array ( [TEXT] => [TYPE] => HTML ) ) [PDF_RU] => Array ( [ID] => 43 [TIMESTAMP_X] => 2015-09-09 16:05:20 [IBLOCK_ID] => 2 [NAME] => PDF RUS [ACTIVE] => Y [SORT] => 500 [CODE] => PDF_RU [DEFAULT_VALUE] => [PROPERTY_TYPE] => F [ROW_COUNT] => 1 [COL_COUNT] => 30 [LIST_TYPE] => L [MULTIPLE] => N [XML_ID] => 43 [FILE_TYPE] => doc, txt, rtf, pdf [MULTIPLE_CNT] => 5 [TMP_ID] => [LINK_IBLOCK_ID] => 0 [WITH_DESCRIPTION] => N [SEARCHABLE] => N [FILTRABLE] => N [IS_REQUIRED] => N [VERSION] => 1 [USER_TYPE] => [USER_TYPE_SETTINGS] => [HINT] => [PROPERTY_VALUE_ID] => 1239 [VALUE] => 22 [DESCRIPTION] => [VALUE_ENUM] => [VALUE_XML_ID] => [VALUE_SORT] => [~VALUE] => 22 [~DESCRIPTION] => [~NAME] => PDF RUS [~DEFAULT_VALUE] => ) [PDF_EN] => Array ( [ID] => 44 [TIMESTAMP_X] => 2015-09-09 16:05:20 [IBLOCK_ID] => 2 [NAME] => PDF ENG [ACTIVE] => Y [SORT] => 500 [CODE] => PDF_EN [DEFAULT_VALUE] => [PROPERTY_TYPE] => F [ROW_COUNT] => 1 [COL_COUNT] => 30 [LIST_TYPE] => L [MULTIPLE] => N [XML_ID] => 44 [FILE_TYPE] => doc, txt, rtf, pdf [MULTIPLE_CNT] => 5 [TMP_ID] => [LINK_IBLOCK_ID] => 0 [WITH_DESCRIPTION] => N [SEARCHABLE] => N [FILTRABLE] => N [IS_REQUIRED] => N [VERSION] => 1 [USER_TYPE] => [USER_TYPE_SETTINGS] => [HINT] => [PROPERTY_VALUE_ID] => 1240 [VALUE] => 23 [DESCRIPTION] => [VALUE_ENUM] => [VALUE_XML_ID] => [VALUE_SORT] => [~VALUE] => 23 [~DESCRIPTION] => [~NAME] => PDF ENG [~DEFAULT_VALUE] => ) [NAME_LONG] => Array ( [ID] => 45 [TIMESTAMP_X] => 2023-04-13 00:55:00 [IBLOCK_ID] => 2 [NAME] => Название (для очень длинных заголовков) [ACTIVE] => Y [SORT] => 500 [CODE] => NAME_LONG [DEFAULT_VALUE] => Array ( [TYPE] => HTML [TEXT] => ) [PROPERTY_TYPE] => S [ROW_COUNT] => 1 [COL_COUNT] => 30 [LIST_TYPE] => L [MULTIPLE] => N [XML_ID] => 45 [FILE_TYPE] => [MULTIPLE_CNT] => 5 [TMP_ID] => [LINK_IBLOCK_ID] => 0 [WITH_DESCRIPTION] => N [SEARCHABLE] => N [FILTRABLE] => N [IS_REQUIRED] => N [VERSION] => 1 [USER_TYPE] => HTML [USER_TYPE_SETTINGS] => Array ( [height] => 80 ) [HINT] => [PROPERTY_VALUE_ID] => [VALUE] => [DESCRIPTION] => [VALUE_ENUM] => [VALUE_XML_ID] => [VALUE_SORT] => [~VALUE] => [~DESCRIPTION] => [~NAME] => Название (для очень длинных заголовков) [~DEFAULT_VALUE] => Array ( [TYPE] => HTML [TEXT] => ) ) )Рюдигер Хельманн
Гейдельбергский университет, Германия
Резюме
- Встречаемость бластного криза низка – 5,6% после 8 лет
- Выживаемость после бластного криза не увеличилась значительно с внедрением ИТК
- Лечение бластного криза в исследовании CML Study IV является разнородным, как ожидается, без особых рекомендаций по исследовательскому протоколу.
- Пока отсутствуют рекомендации по специфическому лекарственному лечению.
- Трансплантация стволовых кроветворных клеток дает лучший долгосрочный прогноз при бластном кризе ХМЛ.
- Европейская организация ELN рекомендует применять Алло-ТСК всегда при бластном кризе ХМЛ.
Короткие сообщения
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 1241
[1] => 1242
[2] => 1243
[3] => 1244
)
[VALUE] => Array
(
[0] => 44
[1] => 94
[2] => 95
[3] => 58
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 44
[1] => 94
[2] => 95
[3] => 58
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
)
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 530
[VALUE] => 06.04.2015 16:57:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 06.04.2015 16:57:00
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 531
[VALUE] => 05.06.2015 16:57:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 05.06.2015 16:57:00
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 911
[VALUE] => 08.09.2015 17:36:00
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08.09.2015 17:36:00
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 532
[VALUE] => 93
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 93
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 533
)
[VALUE] => Array
(
[0] => 93
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 93
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 534
[VALUE] => Array
(
[TEXT] => <p class="Autor_Rus" lang="ru-RU">Юрген Кубалл</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Юрген Кубалл
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 535
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work-Rus">Университетский медицинский центр, Утрехт, Нидерланды</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Университетский медицинский центр, Утрехт, Нидерланды
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 536
[VALUE] => Array
(
[TEXT] => <h2>Резюме</h2><p class="Summery_Rus" lang="ru-RU">В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией. </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Резюме
В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией.
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 537
[VALUE] => 10.18620/1866-8836-2015-4-1-2-62-65
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.18620/1866-8836-2015-4-1-2-62-65
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 538
[VALUE] => Array
(
[TEXT] => <p class="Autor">Jürgen Kuball </p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Jürgen Kuball
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 539
[VALUE] => Array
(
[TEXT] => <p class="Autor_place_work">University Medical Center, Utrecht, Netherlands</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => University Medical Center, Utrecht, Netherlands
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 540
[VALUE] => Cord blood as natural donor source for curing HIV and Leukemia
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Cord blood as natural donor source for curing HIV and Leukemia
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 1016
[VALUE] => Array
(
[TEXT] => <p>Подобное лечение основано на том, что, во-первых, ВИЧ первично поражает систему гемопоэза и, во-вторых, что при ГТСК происходит замещение инфицированных гемопоэтических клеток неинфицированным костным мозгом. Незараженное потомство нового костного мозга затем заселяет организм пациента в различных зонах организма. Однако основной проблемой остается неинфекция донорских клеток после ТГСК. В частности, типичные «резервуары» ВИЧ, такие, как популяции моноцитов, обычно замещаются донорскими клетками лишь спустя месяцы после ТГСК. Персистирующие донорские моноциты впоследствии являются потенциальным источником ВИЧ-реинфекции клеток донора. Поэтому реакция «трансплантат против хозяина» может быть существенным фактором устранения остаточных клеток-носителей ВИЧ после ТГСК.</p>
<p>Чтобы предотвратить реинфекцию ВИЧ донорских клеток в организме пациента, можно привлечь донора с естественной делецией гена CCR5, при которой блокируется вход в клетку наиболее частого типа ВИЧ. Этотгенетический признак имеется у <1% населения. Поэтому поиск такого донора затруднителен. В данном случае у пациента должны быть серьезные показания к ТГСК , у него должна быть также ВИЧ-инфекция, и заражение вирусом должно зависеть от рецептора CCR5. Частота мутации <em>CCR5</em>-del32/del32 среди европейцев ≤1% и еще ниже – в других этнических группах. Таким образом, подобные больные обычно имеют малое количество доступных доноров. Если используют материал от взрослых доноров, то требуется очень близкое совпадение по HLA (7-8/8). Из-за этих ограничений, второй пациент для аналогичной ТГСК был найден лишь через несколько лет, в 2014 г. (Kordelas et al., 2014; Verheyen et al., 2014) К сожалению, результат ТГСК был негативным из-за рецидива ВИЧ-инфекции. Скорее всего, реинфекция реализовалась через другой рецептор, например, CXCR4.</p>
<p>Стволовые клетки из пуповинной крови (ПСК) в качестве стандартного донорского материала для ТГСК, стали в последнее десятилетие новым потенциальным источником гемопоэтических клеток для ВИЧ-инфицированных больных. Прежде всего, для хорошего исхода ТГСК здесь достаточно меньшего совпадения по HLA между ПСК и клетками пациента (Wagner et al., 2014). Эти менее строгие критерии подбора существенно повышают шансы найти донора в том же генетическом пуле. С другой стороны, если выявлена партия ПСК с уникальным признаком, вроде <em>CCR5</em>-del32/del32, то она теоретически может быть использована для нескольких больных. Поэтому увеличение пула образцов ПСК с наличием <em>CCR5</em>-del32/del32 обеспечит появление трансплантатов для того, чтобы повысить вероятность более быстрого и качественного подбора HLA-совместимого донора для больного с ВИЧ-инфекцией, если эта инфекция имеет тропизм к CCR5, и больному требуется ТГСК. Теоретический расчет минимального числа доз ПСК с del32/del32 проводился недавно (Petz et al., 2013), и было показана высокая вероятность нахождения образца, гомозиготного по <em>CCR5</em>-del32 и HLA-совместимого с пациентом, имеющим клинические показания к ТГСК. Однако число стволовых клеток на 1 дозу ПСК весьма мало, и одной дозы часто недостаточно для своевременного приживления у взрослого пациента. Поэтому ТГСК у взрослых лиц требуют обычно 2 доз ПСК, чтобы преодолеть ограничения малых доз ПСК в пуповинной крови. Хотя эта стратегия кажется простой и удобной для пациентов без ВИЧ-инфекции, ее применение проблематично у больных с ВИЧ-инфекцией. Очень маловероятен подбор двух доз ПСК с мутацией <em>CCR5</em>-del32, и преимущественный рост клеток с <em>CCR5</em>-del32 будет зависеть от случая. Решением вопроса может быть сочетание ТГСК пуповинных клеток и гаплоидентичной ТГСК. Последний, при высоком уровне его очистки от Т-клеток, может рассматриваться в качестве «мостика» к долгосрочному приживлению ПСК, как впервые показали испанские коллеги (Magro E et al., 2006). Лечебные перспективы комбинированной трансплантации гаплоидентичных и пуповинных клеток касаются более безопасного и быстрого приживления нейтрофилов, что дает лучшую защиту от инфекций. Такой вариант ТГСК может быть обоснован даже при наличии пригодного донора по основным показаниям. Некоторые авторы показали, что комбинированная гапло-ТГСК и пересадка ПСК имеет приемлемый уровень безопасности, сравнимый с ТГСК от неродственных доноров (Kwon et al., 2012; Liu et al., 2011). Однако новейшие протоколы размножения пуповинных стволовых клеток могут проложить новый путь для осуществления таких ТГСК при наличии лишь одной дозы ПСК с <em>CCR5</em>-del32. </p>
<p>Кроме тщательной оценки выбора доноров, возникает еще одно важное соображение, касающееся будущего ВИЧ-позитивныъ больных. Хотя ВИЧ-инфекция сейчас рассматривается как хроническое заболевание в эру эффективной специфической терапии, качество жизни ВИЧ-инфицированных больных обычно существенно нарушено. Исследование частоты самоубийств среди ВИЧ-положительных больных с 1988 по 2008 гг. включало 15275 ВИЧ-инфицированных лиц в длительные сроки (медиана – 4,7 г.) Частота суицидов среди этого контингента была более чем в 3 раза выше, нежели в населении в целом (Keiser et al., 2010), отражая, на самом деле, влияние многих ограничений, касающихся ВИЧ-инфицированных лиц в повседневной жизни. </p>
<p>Проведению трансплантаций при отсутствии должного опыта в этой области может помочь использование рекомендаций JACIE– системы, предназначенной для обеспечения качества и улучшения состояния знаний по данному вопросу. Таким образом, введение дополнительных качественных категорий, таких, как «альтернативная процедура трансплантации» с отдельным информированным согласием и контролем качества, включены в нашу трансплантационную программу, аккредитованную JACIE, в Университетской клинике Утрехта. Стандартное информированное согласие для биобанкирования (этическое одобрение) применяется для всех процедур алло-ТГСК и обеспечивает максимум получаемой информации независимо от ее исхода. Многие пациенты в Европе, теперь получают трансплантацию по комбинированному протоколу с гапло- и пуповинной ТГСК, в т.ч. один пациент получил трансплантацию клеток с CCR del32/32 в нашем центре. Об исходе этой ТГСК будет сообщено дополнительно.. </p>
<h2>Выводы </h2>
<p>Доноры с мутацией<em> CCR5</em>-del32/del32, очевидно, являются предпочтительными для пациентов с гематологическими новообразованиями и сопутствующей ВИЧ-инфекцией. Настоятельно необходимо расширение пула образцов пуповинной крови с<em> CCR5</em>-del32/del32. Комбинированная трансплантация гаплоидентичных и пуповинных стволовых клеток, или протоколы с размножением стволовых клеток из одного образца пуповинной крови могут стать основой для лечения онкогематологических больных с ВИЧ-инфекцией. Однако ТГСК представляет собой высокий риск для больного и поэтому не может рассматриваться как оптимальное решение для функционального излечения ВИЧ-инфекции. Наряду с излечением ВИЧ-инфицированного больного, этот тип ТГСК позволяет исследование вариантов ВИЧ, важных для разработки механизмов лечения ВИЧ-инфекции. С нашего и других клинических случаев началось очень интересное международное сотрудничество – проект Epistem (<a href="http://www.epistem-project.org">http://www.epistem-project.org</a>), основанный AMFAR – европейский проект проведения терапии и изучения потенциала излечения ВИЧ-инфекции путем аллогенной трансплантации гемопоэтических клеток. Областями исследований являются: (1) Повышение числа пригодных для ТГСК образцов ПСК с del32/del32, путем систематического тестирования европейских банков пуповинной крови; (2) Выдача советов в процессе лечения (выбор донора, этические аспекты, взаимодействия между препаратами и т.д.); (3) Улучшение понимания биологических механизмов излечения ВИЧ-инфекции путем выработки стандартизированного клинического протокола, который обеспечит сравнимость исследований вирусных резервуаров, характеристик инфицирующего вируса и оценки иммунного ответа после алло-ТГСК по различным трансплантационным центрам</p>
[TYPE] => html
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Подобное лечение основано на том, что, во-первых, ВИЧ первично поражает систему гемопоэза и, во-вторых, что при ГТСК происходит замещение инфицированных гемопоэтических клеток неинфицированным костным мозгом. Незараженное потомство нового костного мозга затем заселяет организм пациента в различных зонах организма. Однако основной проблемой остается неинфекция донорских клеток после ТГСК. В частности, типичные «резервуары» ВИЧ, такие, как популяции моноцитов, обычно замещаются донорскими клетками лишь спустя месяцы после ТГСК. Персистирующие донорские моноциты впоследствии являются потенциальным источником ВИЧ-реинфекции клеток донора. Поэтому реакция «трансплантат против хозяина» может быть существенным фактором устранения остаточных клеток-носителей ВИЧ после ТГСК.
Чтобы предотвратить реинфекцию ВИЧ донорских клеток в организме пациента, можно привлечь донора с естественной делецией гена CCR5, при которой блокируется вход в клетку наиболее частого типа ВИЧ. Этотгенетический признак имеется у <1% населения. Поэтому поиск такого донора затруднителен. В данном случае у пациента должны быть серьезные показания к ТГСК , у него должна быть также ВИЧ-инфекция, и заражение вирусом должно зависеть от рецептора CCR5. Частота мутации CCR5-del32/del32 среди европейцев ≤1% и еще ниже – в других этнических группах. Таким образом, подобные больные обычно имеют малое количество доступных доноров. Если используют материал от взрослых доноров, то требуется очень близкое совпадение по HLA (7-8/8). Из-за этих ограничений, второй пациент для аналогичной ТГСК был найден лишь через несколько лет, в 2014 г. (Kordelas et al., 2014; Verheyen et al., 2014) К сожалению, результат ТГСК был негативным из-за рецидива ВИЧ-инфекции. Скорее всего, реинфекция реализовалась через другой рецептор, например, CXCR4.
Стволовые клетки из пуповинной крови (ПСК) в качестве стандартного донорского материала для ТГСК, стали в последнее десятилетие новым потенциальным источником гемопоэтических клеток для ВИЧ-инфицированных больных. Прежде всего, для хорошего исхода ТГСК здесь достаточно меньшего совпадения по HLA между ПСК и клетками пациента (Wagner et al., 2014). Эти менее строгие критерии подбора существенно повышают шансы найти донора в том же генетическом пуле. С другой стороны, если выявлена партия ПСК с уникальным признаком, вроде CCR5-del32/del32, то она теоретически может быть использована для нескольких больных. Поэтому увеличение пула образцов ПСК с наличием CCR5-del32/del32 обеспечит появление трансплантатов для того, чтобы повысить вероятность более быстрого и качественного подбора HLA-совместимого донора для больного с ВИЧ-инфекцией, если эта инфекция имеет тропизм к CCR5, и больному требуется ТГСК. Теоретический расчет минимального числа доз ПСК с del32/del32 проводился недавно (Petz et al., 2013), и было показана высокая вероятность нахождения образца, гомозиготного по CCR5-del32 и HLA-совместимого с пациентом, имеющим клинические показания к ТГСК. Однако число стволовых клеток на 1 дозу ПСК весьма мало, и одной дозы часто недостаточно для своевременного приживления у взрослого пациента. Поэтому ТГСК у взрослых лиц требуют обычно 2 доз ПСК, чтобы преодолеть ограничения малых доз ПСК в пуповинной крови. Хотя эта стратегия кажется простой и удобной для пациентов без ВИЧ-инфекции, ее применение проблематично у больных с ВИЧ-инфекцией. Очень маловероятен подбор двух доз ПСК с мутацией CCR5-del32, и преимущественный рост клеток с CCR5-del32 будет зависеть от случая. Решением вопроса может быть сочетание ТГСК пуповинных клеток и гаплоидентичной ТГСК. Последний, при высоком уровне его очистки от Т-клеток, может рассматриваться в качестве «мостика» к долгосрочному приживлению ПСК, как впервые показали испанские коллеги (Magro E et al., 2006). Лечебные перспективы комбинированной трансплантации гаплоидентичных и пуповинных клеток касаются более безопасного и быстрого приживления нейтрофилов, что дает лучшую защиту от инфекций. Такой вариант ТГСК может быть обоснован даже при наличии пригодного донора по основным показаниям. Некоторые авторы показали, что комбинированная гапло-ТГСК и пересадка ПСК имеет приемлемый уровень безопасности, сравнимый с ТГСК от неродственных доноров (Kwon et al., 2012; Liu et al., 2011). Однако новейшие протоколы размножения пуповинных стволовых клеток могут проложить новый путь для осуществления таких ТГСК при наличии лишь одной дозы ПСК с CCR5-del32.
Кроме тщательной оценки выбора доноров, возникает еще одно важное соображение, касающееся будущего ВИЧ-позитивныъ больных. Хотя ВИЧ-инфекция сейчас рассматривается как хроническое заболевание в эру эффективной специфической терапии, качество жизни ВИЧ-инфицированных больных обычно существенно нарушено. Исследование частоты самоубийств среди ВИЧ-положительных больных с 1988 по 2008 гг. включало 15275 ВИЧ-инфицированных лиц в длительные сроки (медиана – 4,7 г.) Частота суицидов среди этого контингента была более чем в 3 раза выше, нежели в населении в целом (Keiser et al., 2010), отражая, на самом деле, влияние многих ограничений, касающихся ВИЧ-инфицированных лиц в повседневной жизни.
Проведению трансплантаций при отсутствии должного опыта в этой области может помочь использование рекомендаций JACIE– системы, предназначенной для обеспечения качества и улучшения состояния знаний по данному вопросу. Таким образом, введение дополнительных качественных категорий, таких, как «альтернативная процедура трансплантации» с отдельным информированным согласием и контролем качества, включены в нашу трансплантационную программу, аккредитованную JACIE, в Университетской клинике Утрехта. Стандартное информированное согласие для биобанкирования (этическое одобрение) применяется для всех процедур алло-ТГСК и обеспечивает максимум получаемой информации независимо от ее исхода. Многие пациенты в Европе, теперь получают трансплантацию по комбинированному протоколу с гапло- и пуповинной ТГСК, в т.ч. один пациент получил трансплантацию клеток с CCR del32/32 в нашем центре. Об исходе этой ТГСК будет сообщено дополнительно..
Выводы
Доноры с мутацией CCR5-del32/del32, очевидно, являются предпочтительными для пациентов с гематологическими новообразованиями и сопутствующей ВИЧ-инфекцией. Настоятельно необходимо расширение пула образцов пуповинной крови с CCR5-del32/del32. Комбинированная трансплантация гаплоидентичных и пуповинных стволовых клеток, или протоколы с размножением стволовых клеток из одного образца пуповинной крови могут стать основой для лечения онкогематологических больных с ВИЧ-инфекцией. Однако ТГСК представляет собой высокий риск для больного и поэтому не может рассматриваться как оптимальное решение для функционального излечения ВИЧ-инфекции. Наряду с излечением ВИЧ-инфицированного больного, этот тип ТГСК позволяет исследование вариантов ВИЧ, важных для разработки механизмов лечения ВИЧ-инфекции. С нашего и других клинических случаев началось очень интересное международное сотрудничество – проект Epistem (http://www.epistem-project.org), основанный AMFAR – европейский проект проведения терапии и изучения потенциала излечения ВИЧ-инфекции путем аллогенной трансплантации гемопоэтических клеток. Областями исследований являются: (1) Повышение числа пригодных для ТГСК образцов ПСК с del32/del32, путем систематического тестирования европейских банков пуповинной крови; (2) Выдача советов в процессе лечения (выбор донора, этические аспекты, взаимодействия между препаратами и т.д.); (3) Улучшение понимания биологических механизмов излечения ВИЧ-инфекции путем выработки стандартизированного клинического протокола, который обеспечит сравнимость исследований вирусных резервуаров, характеристик инфицирующего вируса и оценки иммунного ответа после алло-ТГСК по различным трансплантационным центрам
[TYPE] => html
)
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1245
[VALUE] => 24
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 24
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 1246
[VALUE] => 25
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 25
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Юрген Кубалл
Университетский медицинский центр, Утрехт, Нидерланды
Резюме
В феврале 2007 года Хюттер и соавт. осуществили аллогенную транплантацию гемопоэтических стволовых клеток(ТГСК) больному с острым миелобластным лейкозом (ОМЛ) и наличием ВИЧ-инфекции. При этом была проведена трансплантация периферических стволовых клеток от взрослого донора. Этот больной, известный как «берлинский пациент», был излечен как от ВИЧ-инфекции, а также от ОМЛ. (Hutter et al., 2009). Это «магическое» излечение побудило многих гематологов более детально исследовать перспективы лечения пациентов, страдающих от лейкозов в сочеатнии с ВИЧ-инфекцией.

