BCR/ABL, IKZF deletions and FLT3-ITD as the targets for relapsed/refractory B-cell acute lymphoblastic leukemia treatment: Blinatumomab combined with Tyrosine kinase inhibitors and ATRA
Andrey N. Sokolov1, Elena N. Parovichnikova1, Vera V. Troitskaya1, Larisa A. Kuzmina1, Irina V. Galtseva1, Sergei M. Kulikov1, Sergey N. Bondarenko2, Irina A. Lukyanova1, Tatiana I. Lobanova1, Ekaterina I. Usikova1, Ksenia I. Zarubina1, Olga A. Gavrilina1, Julia O. Davidova1, Nikolai M. Kapranov1, Valeriy G. Savchenko1
1 National Research Center for Hematology of the Ministry of Healthcare of the Russian Federation, Moscow, Russia
2 Raisa Gorbacheva Memorial Research Institute of Pediatric Oncology, Hematology and Transplantation, Pavlov University,
St. Petersburg, Russia
Correspondence
Dr. Andrey N. Sokolov, National Research Center for Hematology, 4A Novyi Zykovskii Lane, 125167, Moscow, Russia
Phone: +7 (495) 612 4592
E-mail: sokolov.a@blood.ru
Accepted 27 March 2020
Summary
Bispecific monoclonal antibody blinatumomab is targeting CD19, being applied for treatment of acute lymphoblastic leukemia (ALL). Several additional targets could be used for combined chemo-free treatment with thyrosine kinase inhibitors: BCR-ABL, FLT3 and IKZF1 deletions are amongst them. In the following study, we aimed to assess toxicity and clinical effectiveness of the combination of blinatumomab and several thyrosine kinase inhibitors.
Patients and methods
From October 2015 to October 2018, we treated 11 relapsed/refractory (R/R) ALL patients (pts). The blinatumomab treatment consisted of 4-5 cycles with 2-week intervals (28 mcg/day by continuous infusion during 28 days per cycle with 9 mcg/day during the first week of the first cycle). Seven BCR-ABL-positive and 2 IKZF1-deleted pts received initially dasatinib at 140 mg/day, one case, with FLT3-ITD received sorafenib (800 mg/day). One BCR-ABL-positive pt with T315I mutation was administered ponatinib (45 mg/day). Pts with IKZF1 deletions received ATRA (45 mg/m2/day for 4 weeks) of the 1st blinatumomab cycle and during first 2 weeks of subsequent blinatumomab cycles.
Results
In the patients responding to blinatumomab treatment, we observed a statistically significant increment of absolute values in T-helper (p=0.0034), T-cytotoxic (p<0.0001) and NK (p=0.0006) cell subpopulations in peripheral blood over the entire treatment period. T-regulatory and double-negative T-cells as potentially inhibitors of T cell response to blinatumomab remained within low values of normal ranges. Hypogammaglobulinemia was observed in 8 of 11 pts. CR was achieved in 10 pts after 1st cycle of blinatumomab, progressive disease was detected in 1 pt. Nine cases of complete molecular remissions (MolCR) and one cytogenetic complete remission were achieved in ten CR pts. Nine allo-BMT and one auto-BMT were performed in 10 CR pts. Three CNS relapses after allo-BMT and one molecular relapse after auto-BMT were diagnosed. One pt died from septic shock after allo-BMT.
Conclusion
Blinatumomab combined with TKI has high therapeutic potential as induction remission treatment in targeted ALL population without conventional chemotherapy. High rate of potential CNS relapses could be decreased with more intensive intrathecal prophylaxis.
Keywords
Acute lymphoblastic leukemia, blinatumomab, tyrosine kinase inhibitors.
Introduction
Bispecific monoclonal antibodies for targeting tumor cells have a long story from 1980's to produce approved drug in 2014 [1-3]. Several trials for relapsed/refractory acute lymphoblastic leukemia (R/R ALL) treatment including ALCANTARA for Philadelphia chromosome-positive (Ph-positive) R/R ALL were performed and showed clinical effectiveness and even an advantage over chemotherapy (TOWER Study) [4-8]. Recently published results on blinatumomab combined with TKI for therapy of Ph-positive R/R ALL characterized this approach to be safe and effective [11]. Combination of Blinatumomab and TKI could elicit lower toxicity and improve primary results in managing heavily pretreated R/R ALL patients. In preclinical studies, retinoids have shown antileukemic activity in IKZF-deleted ALL [12]. We previously reported about effective combination of blinatumomab with tyrosine kinase inhibitors (TKI) for the treatment of Ph-positive and FLT3-ITD R/R ALL and blinatumomab with TKI and all-trans retinoic acid in IKZF-deleted R/R ALL patients [9, 10]. The aim of our study was to present the data on 11 R/R ALL patients treated with Blinatumomab and TKI+/-ATRA, omitting simultaneous standard chemotherapy.
Patients and methods
Eleven patients (pts) with R/R ALL were treated with Blinatumomab + TKI/TKI+ATRA at the National Research Center for Hematology, Moscow, Russia, and in Raisa Gorbacheva Memorial Institute of Pediatric Oncology, Hematology and Transplantation, Saint Petersburg, Russia, from October 2015 to October 2018. The study was approved by the Institutional Review Board. The treatment was administered after the patient has signed informed consent. Blinatumomab was provided by Amgen as part of the expanded access program. The treatment consisted of 4-5 cycles of blinatumomab 28 mcg/day by continuous infusion for 4 weeks each cycle. Over 1st week of 1st cycle, Blinatumomab was administered at the dose of 9 mcg/day. The 2-week intervals followed between the rounds of blinatumomab treatment. All the patients were administered one of TKIs: 7 Ph-positive and 2 IKZF1-deleted ALL pts were initially treated with dasatinib (140 mg/day) per os, 1 FLT3-ITD ALL patient received sorafenib (800 mg/day) per os, and one Ph-positive ALL patient with a T315I mutation received ponatinib (45 mg/day). All the TKIs were administered continuously, from the 1st day of starting blinatumomab. All-trans-retinoic acid (ATRA) at a dose of 45 mg/m2/day was administered per os in the IKZF1-deleted pts during 4 weeks of the 1st blinatumomab cycle, and during first two weeks of subsequent blinatumomab cycles.
Complete remission (CR) was diagnosed if less than 5% of blasts were present in bone marrow. Cytogenetic remission (CyR) was diagnosed in the absence of BCR-ABL positive nuclei per 200 nuclei by fluorescence in situ hybridization (FISH). Molecular CR (MolCR) was diagnosed if BCR-ABL/ABL at a ratio of <0.01 was detected in bone marrow samples by RT-qPCR. The CD3+/CD4+/CD8- T-helper, CD3+/CD4-/CD8+ T-cytotoxic, CD3+/CD4-/CD8- T-Double-negative, CD3+/CD4+/CD25+ T-regulatory, CD3-/CD56+ NK subpopulations were measured in peripheral blood lymphocytes by flow cytometry weekly during blinatumomab treatment in all the pts (1 to 16 samples, 4 points per each blinatumomab cycle). Serum immunoglobulins (Ig) G, M and A were measured during each cycle of blinatumomab (a total of 4 sampling points).
The SAS software was used for statistical evaluation using regression analysis. The MIXED SAS procedure was used to perform repeated measures analysis and to estimate parameters of linear regression of average time-dependent trend.
Results
Median follow-up was 23 months (19 to 36 months). Median age is 32 years (24 to 49 years). Eight pts were females and 3, males. 7 pts received 4 cycles; 1 pt, 5 cycles; 2 pts underwent 2 cycles, and 1 pt was subjected to 1 cycle of blinatumomab treatment. Nine patients had febrile reactions during first two weeks at the 1st cycle of blinatumomab. No one cycle of blinatumomab therapy was not interrupted. Neurological toxicity (1-2 grades) was observed in 2 cases manifesting as headaches in 1 patient, and ulnar neuropathy in 1 case. One patient treated with sorafenib has hand-foot skin syndrome. The syndrome completely resolved after 2 weeks interruption of sorafenib treatment.
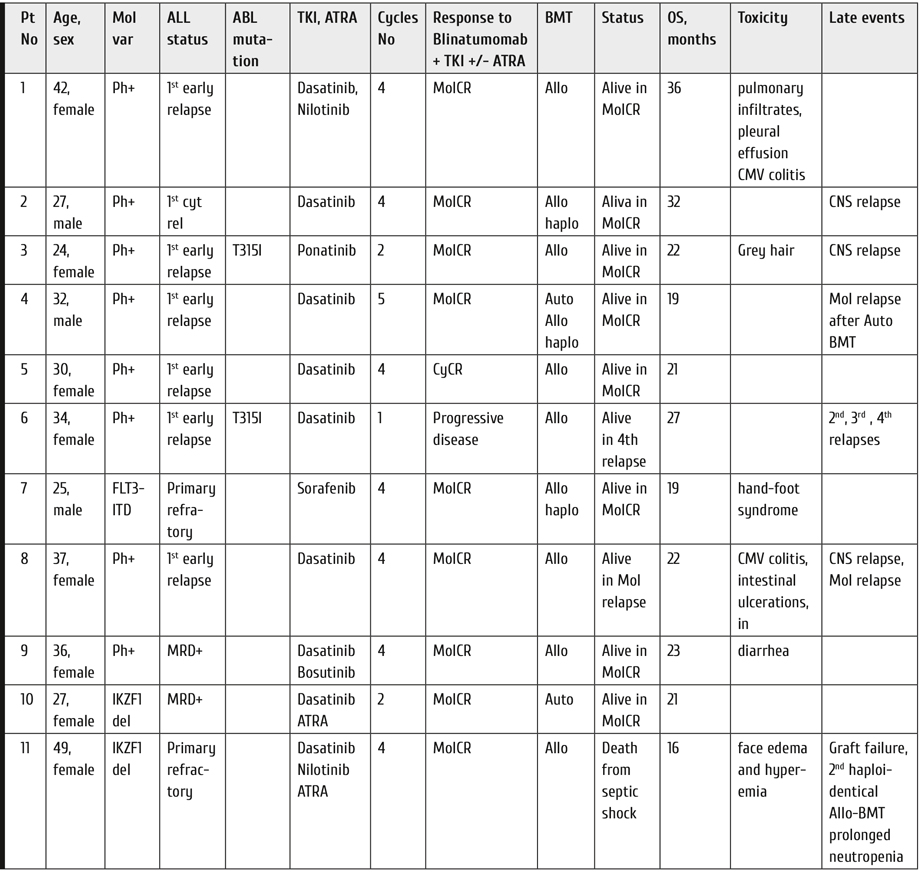
Pulmonary infiltrates and pleural effusion in one dasatinib-treated case were completely resolved after switching to nilotinib. Diarrhea associated with dasatinib therapy was observed in 3 patients and resolved after its replacement with bosutinib in 2 cases, and with nilotinib in 1 patient. CMV-associated colitis was diagnosed in 2 cases using virus-specific PCR in stool samples. Massive intestinal bleeding and multiple intestinal ulceration were observed in one patient with CMV colitis, as confirmed by colonoscopy. Facial edema and hyperemia were evident in 1 patient upon dasatinib treatment. These symptoms resolved after passage from dasatinib to nilotinib. Greyness of hair was detected in one patient treated with ponatinib. The main clinical characteristics of individual patients and the events are listed in Table 1.
Table 1. Basic clinical characteristics of blinatumomab + TKI-treated ALL patients, response to therapy, and adverse effects
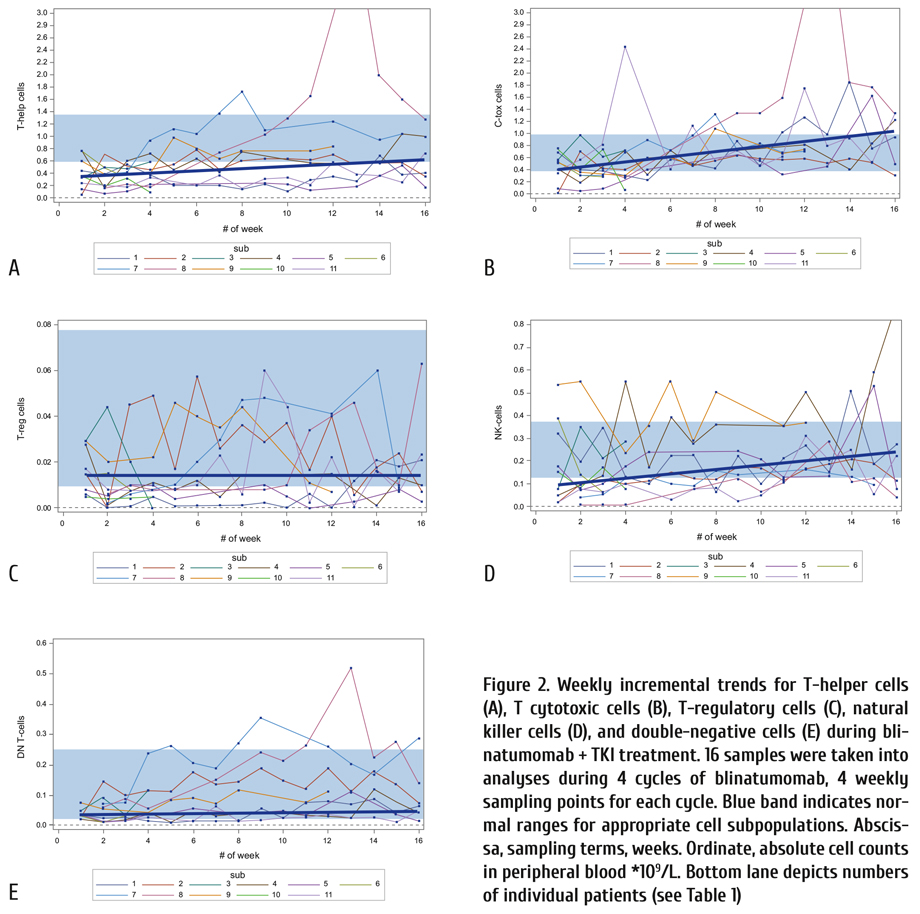
The weekly performed counts of T-cytotoxic, NK, T-helper and T-regulatory cells in peripheral blood were decreased during the 1st blinatumomab cycle. T-cytotoxic and NK cells returned to normal ranges over the 2nd to 4th blinatumomab cycles. T-regulatory cell counts remained decreased or approached low-normal limits at all terms, except of 2nd blinatumomab cycle (Fig. 1).
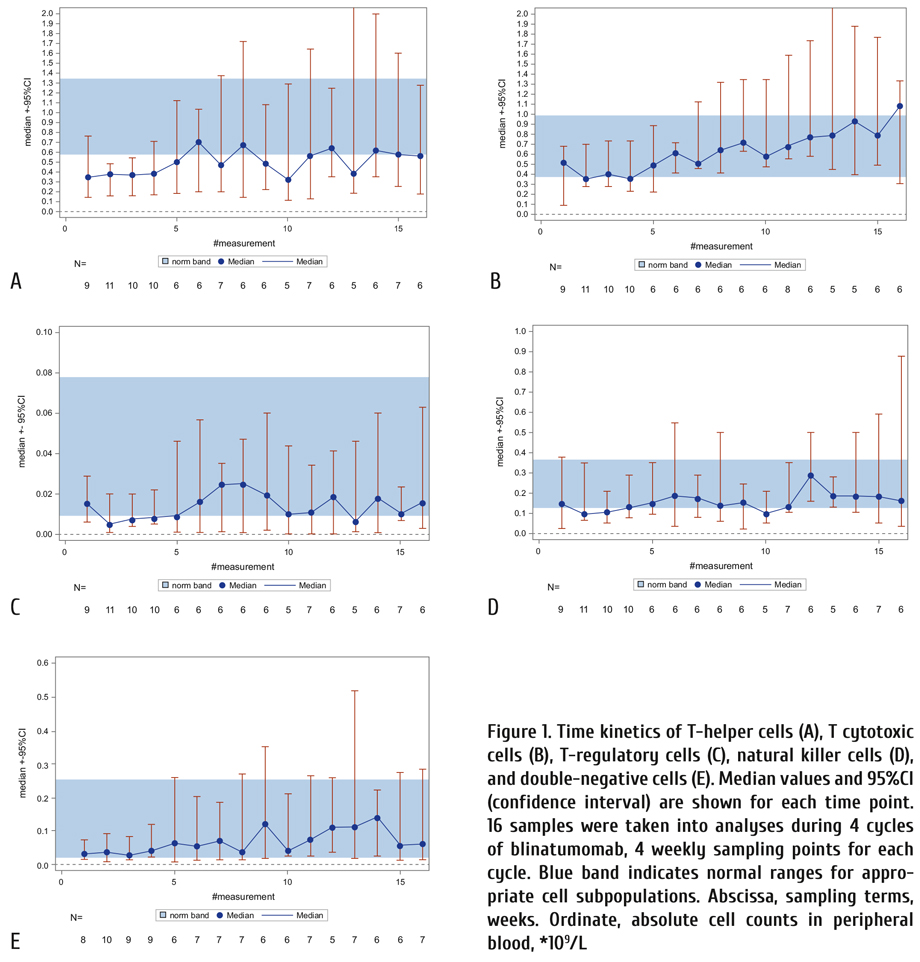
Table 2. Weekly gaining effect in distinct T-cell subpopulations. Each sampling point was measured once a week (four points per cycle measured weekly) during 4 cycles of blinatumomab
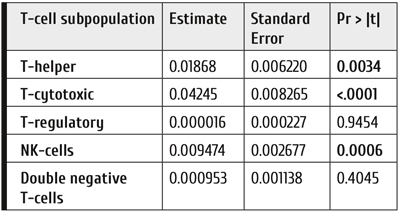
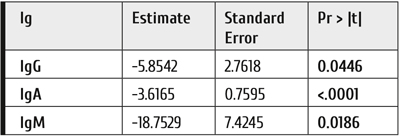
Table 3. Weekly decrement in serum IgG, IgA and IgM upon blinatumomab therapy. Each measurement was performed at every treatment cycle (four points weekly over 4 cycles)
Regression analysis (the MIXED procedure in SAS system) was performed for each cell subpopulation, in order to detect significant changes of the T cell subpopulation kinetics (Table 2 and Fig. 2 a-e). As seen in table 2 in T-helper, T-cytotoxic and NK-subpopulations the weekly gaining effect was statistically significant.
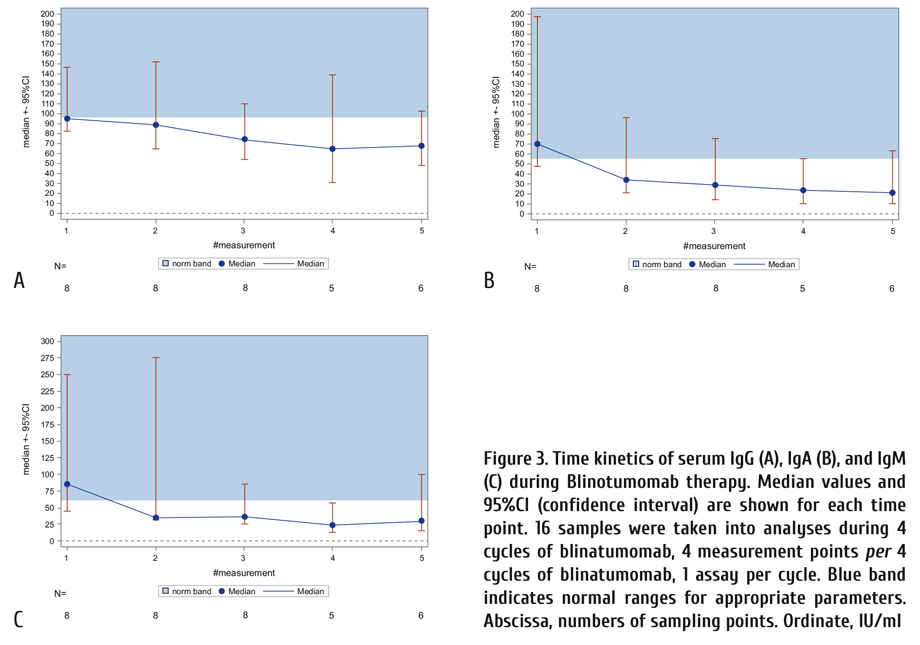
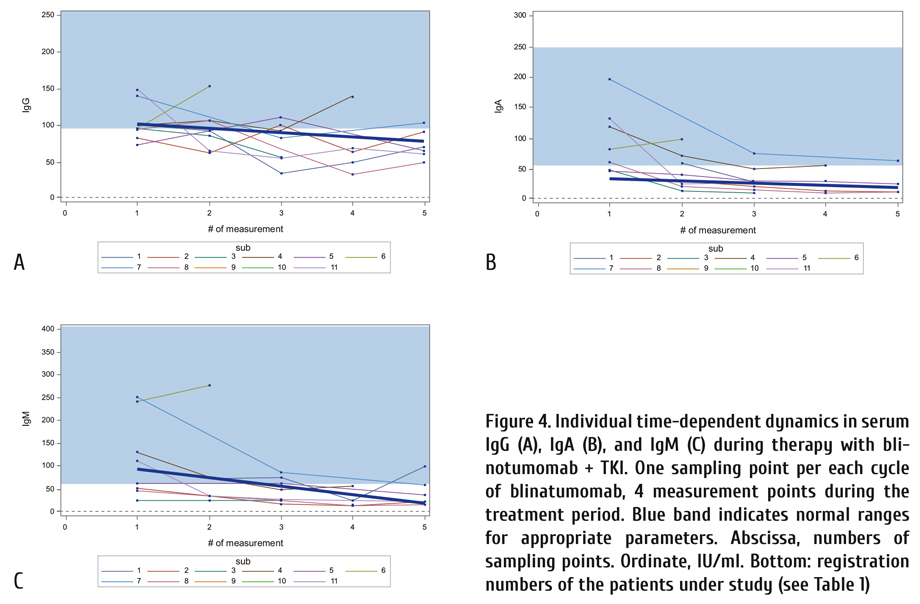
Hypogammaglobulinemia during blinatumomab treatment was frequently observed (Fig. 3), and, in eight patients, treatment with intravenous human normal immunoglobulin was used. To check if the IgG, IgA and IgM kinetics were statistically significant, the regression analysis (the MIXED procedure in SAS system) was performed for each Ig (Table 3 and Fig. 4). As seen in Table 3, a gradual decrease in immunoglobulins with each cycle of blinatumomab was statistically significant for IgG, IgA and IgM. Fig. 4 shows the statistically significant effects of Blinatumomab treatment upon IgG (p=0.0446), IgA (p<.0001), and IgM (p=0.0186) (Table 3).
In 10 cases of 11, complete remission (CR) was achieved after 1st blimatumomab cycle. Progression of the disease was observed in 1 patient during 1st cycle of blinatumomab treatment, thus urging us to stop this therapy. Molecular CR (MolCR) was achieved in 9 cases, and cytogenetic CR was detected in 1 patient during consequent blinatumomab cycles. Allogeneic BMT was performed in 9 cases, and auto-BMT, in 1 patient with MolCR. Overt rapid hematological relapse was diagnosed in 1 patient under bosutinib maintenance therapy while waiting for alloBMT. Subsequent MolCR was achieved in the patient with bortezomib-based chemotherapy + dasatinib. One cytogenetic relapse was observed in 1 patient with complete cytogenetic remission before alloBMT. One patient treated with dasatinib as maintenance therapy after auto-BMT had molecular relapse, and second MolCR was achieved after Blinatumomab retreatment + dasatinib + ATRA. Allo-BMT from haploidentical donor was performed in this case. One patient treated with ponatinib and one patient receiving dasatinib maintenance after allo-BMT had CNS relapse and CNS lesions that regressed after intrathecal chemotherapy and cranial irradiation. One patient in MolCR died from septic shock 5 months after allo-BMT.
Discussion
Each patient in the study received combined treatment with blimatumomab immunotherapy and TKI target therapy. The treatment was well tolerated and complications were rare and curable. Hypogammaglobulinemia was common during blinatumomab treatment reflecting strong mature B-cell depletion on anti CD19 treatment. High rate of hypogammaglobulinemia lead to high rate of CMV infection, that was severe in 1 case. Rapid CR achievement and granulocyte recovery permits to treat almost all patients from 2nd to 4th cycles in outpatient settings. Nine molCR and one CyR with only one case of progressive disease permit to recognize this approach as highly effective, with low toxicity profile. Complementary treatment with ATRA in IKZF-deleted pts was also effective strategy though the number of such cases is too small. TKI treatment allows to perform prolonged maintenance, in order to control remaining leukemic populations in some cases. Though the rate of relapses is high, i.e., one half of the pts. However, a cohort of patients had extremely high risk of subsequent relapses and our approach did not exclude this risk entirely. In a single case, replacement of effective TKIs due to toxicity resulted in overt hematological relapse.
Prolonged neutropenia after Allo-BMT resulted in postponing of TKI maintenance and, in all these cases, the dose of eventually administered TKI was lowered by half. Heavily pre-treated patients have higher post-Allo-BMT toxicity, and the maintenance therapy after BMT was not proper. Auto-BMT in Ph-positive patient was not a curative strategy, though in IKZF-deleted patient, AutoBMT with lower toxicity regimen enables us to perform adequate maintenance with two agents, i.e., TKI and ATRA. Recently published results of combined treatment with blinatumomab and TKIs in Ph-positive relapsed ALL had also shown high rates of subsequent remissions and OS values (73% to 75%) in a small cohort of patients [11]. Statistical evaluation of changes observed for different lymphoid subpopulations revealed a strong evidence for T-cytotoxic and NK cells recovery in the course of effective combined treatment with blinatumomab and TKI. Duell et al. have demonstrated that lower frequency of T-regulatory cells correlates with higher response to blinatumomab in B-ALL patients [13]. T-regulatory and double-negative cells may potentially inhibit cytotoxic and other effector lymphocytes subpopulations and we observed their fluctuation within lower values of absolute peripheral blood counts in responders to the drug. Rapid and strong B-cell depletion as demonstrated by Zugmaier et al. [14], could explain the dropping immunoglobulin synthesis and prolonged hypogammaglobulinemia in most patients treated with blinatumomab.
Conclusion
Combined treatment with blinatumomab and TKI has acceptable and curable toxicity and demonstrates high rate of MolCR in high risk R/R ALL pts. The results are promising, with respect of using this treatment as induction and consolidation therapy without standard chemotherapy. IKZF deletions and FLT3-ITD are the new targets for chemo-free combined immunotherapy and TKI in ALL patients.
Acknowledgements
We thank Amgen for blinatumomab providing. We thank the Russian Acute Leukemia Study Group, National Hematology Society of Russia and also Margarita Anukhina for data management.
References
- Perez P, Hoffman RW, Shaw S, Bluestone JA, Segal DM. Specific targeting of cytotoxic T cells by anti-T3 linked to anti-target cell antibody. Nature. 1985; 316:354-356.
- Baagen A, Van De Griend R, Clark M, Geerars A, Bast B, De Gast B. Killing of human leukaemia/lymphoma B cells by activated cytotoxic T lymphocytes in the presence of a bispecific monoclonal antibody (mCD3/mCD19). Clin Exp Immunol. 1992; 90: 368-375.
- Przepiorka D, Ko C-W, Deisseroth A, Yancey CL, Candau-Chacon R, Chiu H-J, Gehrke BJ, Gomez-Broughton C, Kane RC, Kirshner S, Mehrotra N, Ricks TK, Schmiel D, Song P, Zhao P, Zhou Q, Farrell AT, Pazdur R. FDA Approval: Blinatumomab. Clin Cancer Res. 2015; 21(18):4035-4039.
- Topp MS, Gokbuget N, Stein AS, Zugmaier G, O'Brien S, Bargou RC, Dombret H, Fielding AK, Heffner L, Larson RA, Neumann S, Foà R, Litzow M, Ribera JM, Rambaldi A, Schiller G. Safety and activity of Blinatumomab for adult patients with relapsed or refractory B-precursor acute lymphoblastic leukaemia: A multicentre, single-arm phase 2 study. Lancet Oncol. 2015;16:57-66.
- Kantarjian H, Stein A, Gokbuget N, Fielding AK, Schuh AC, Ribera J-M, Wei A, Dombret H, Foà R, Bassan R, Arslan Ö, Sanz MA, et al. Blinatumomab versus chemotherapy for advanced acute lymphoblastic leukemia. N Eng J Med. 2017;376:836-847.
- Martinelli G, Boissel N, Chevallier P, Ottmann O, Gökbuget N, Topp MS, Fielding AK, Rambaldi A, Ritchie EK, Papayannidis C, Sterling LR, Benjamin J, Stein A. Complete hematologic and molecular response in adult patients with relapsed/refractory Philadelphia chromosome-positive B-precursor acute lymphoblastic leukemia following treatment with Blinatumomab: Results from a phase II, single-arm, multicenter study. J Clin Oncol. 2017;35:1795-1802.
- von Stackelberg A, Locatelli F, Zugmaier G, Handgretinger R, Trippett TM, Rizzari C, Bader P, O'Brien MM, Brethon B, Bhojwani D, Schlegel PG, Borkhardt A, Rheingold SR, Cooper TM, Zwaan CM et al. Phase I/phase II study of Blinatumomab in pediatric patients with relapsed/refractory acute lymphoblastic leukemia. J Clin Oncol. 2016;34(36):4381-4389.
- Gokbuget N, Dombret H, Ribera JM, Fielding AK, Advani A, Bassan R, Chia V, Doubek M, Giebel S, Hoelzer D, Ifrah N, Katz A, Kelsh M, Martinelli G, Morgades M, O'Brien S et al. International reference analysis of outcomes in adults with B-precursor Ph-negative relapsed/refractory acute lymphoblastic leukemia. Haematologica. 2016; 101:1524-1533.
- Sokolov A, Parovichnikova E, Troitskaya V, Galtseva I, Firsova M, Davidova J, Kapranov N, Savchenko V. Combined Blinatumomab + Dasatinib/Ibrutinib therapy of relapsed acute lymphoblastic leukemia patients – antileukemic effect on the T-helper and T-regulatory cells reduction background. Haematologica. 2016; 101: 354-355 (E867).
- Sokolov AN, Parovichnikova EN, Troitskaya VV, Kuzmina LA, Galtseva IV, Kulikov SM, Bondarenko SN, Davidova JO, Kapranov NM, Lukyanova IA, Lobanova TI, Usikova EI, Zarubina KI, Savchenko VG. Blinatumomab + tyrosine kinase inhibitors with no chemotherapy in BCR-ABL-positive or IKZF1-deleted or FLT3-ITD-positive relapsed/refractory acute lymphoblastic leukemia patients: high molecular remission rate and toxicity profile. Blood. 2017;130:3884.
- Assi R, Kantarjian H, Short NJ, Daver N, Takahashi K, Garcia-Manero G, DiNardo C, Burger J, Cortes J, Jain N, Wierda W, Chamoun S, Konopleva M, Jabbour E. Safety and efficacy of blinatumomab in combination with a tyrosine kinase inhibitor for the treatment of relapsed Philadelphia chromosome-positive leukemia. Clin Lymphoma Myeloma Leuk. 2017;17(12):897-901.
- Churchman ML, Low J, Qu C, Paietta EM, Kasper LH, Chang Y, Payne-Turner D, Althoff MJ, Song G, Chen SC, Ma J, Rusch M, McGoldrick D, Edmonson M, Gupta P, Wang YD et al. Efficacy of retinoids in IKZF1-mutated BCR-ABL1 acute lymphoblastic leukemia. Cancer Cell. 2015;28(3):343-356.
- Duell J, Dittrich M, Bedke T, Mueller T, Eisele F, Rosenwald A, Rasche L, Hartmann E, Dandekar T, Einsele H, Topp MS. Frequency of regulatory T cells determines the outcome of the T-cell-engaging antibody blinatumomab in patients with B-precursor ALL. Leukemia. (2017);31, 2181-2190.
- Zugmaier G, Gokbuget N, Klinger M, Viardot A, Stelljes M, Neumann S, Horst H-A, Marks R, Faul C, Diedrich H, Reichle A, Brüggemann M, Holland C, Schmidt M, Einsele H, Bargou RC, Topp MS. Long-term survival and T-cell kinetics in relapsed/refractory ALL patients who achieved MRD response after blinatumomab treatment. Blood. 2015;126(24):2578-2584.
Accepted 27 March 2020


