Case Report
The patient, a five-year-old boy, was first noted to have pancytopenia at 24 months of age. An evaluation (Duke University Medical Center) showed the following hematologic values: hemoglobin concentration, 9.5 g per deciliter; white-cell count, 4.3 x 109 per liter, with 22 percent granulocytes, 62 percent lymphocytes, 3 percent monocytes, 1 percent eosinophils, and 8 percent basophils; platelet count, 62 x 109 per liter; and reticulocyte level, 2.3 percent. The bone marrow was hypocellular. The patient had the classic malformations of Fanconi's anemia, including retarded growth (5th to 10th percentile), a rudimentary extra thumb on the left hand, the absence of a left kidney, and hypospadias. Testing of the patient's cells with diepoxybutane, performed at 24 months (Rockefeller University), confirmed the diagnosis of Fanconi's anemia. The parents were healthy, and there was no consanguinity or past history of blood disorders in the family. The patient had been treated with danazol (300 mg per day for six months), with a progressive decrease in the blood-cell counts. Before admission, he had received three units of filtered and irradiated packed red cells.
The patient's mother became pregnant in June 1987. Cytogenetic analysis of cultured amniotic-fluid cells (Rockefeller University) showed that the values for chromosome breakage before and after the cells were exposed to diepoxybutane were within the normal range [5]. A girl was delivered vaginally without complications in February 1988. Studies of chromosome breakage in umbilical-cord blood cells indicated that the newborn had a normal karyotype and was not affected by Fanconi's anemia (Table 1).
Table 1. Results of Cytogenetic Analysis.*
*DEB denotes diepoxybutane; its final concentration in the culture medium was 0.1 mg per milliliter in each analysis in this table.
†Analysis performed on quinacrine-stained metaphase preparations.
‡Analysis performed on Giemsa-stained metaphase preparations.
|
Source Of Cells |
Percent Donor |
Mean Chromosome |
||
|---|---|---|---|---|
|
before deb |
after deb |
before deb |
after deb |
|
|
Patient's peripheral blood on day 0 |
0 |
0 |
0.18 |
10.6 |
|
Donor's cord blood on day 0 |
100 |
100 |
0.00 |
0.02 |
|
Patient's bone marrow on day 120 |
100 |
100 |
0.04 |
0.30 |
|
Patient's peripheral blood |
30 |
52 |
0.7 |
4.0 |
|
Day 64 |
8 |
32 |
1.3 |
5.0 |
|
Day 120 |
12 |
32 |
1.9 |
6.4 |
|
Day 204 |
64 |
86 |
0.30 |
0.49 |
Prenatal HLA typing of amniotic-fluid cells (Dr. M.S. Pollack, Methodist Hospital and Baylor Medical Center, Houston) had shown that the fetus was HLA identical to the patient: the first haplotype was Al,B8,DR3, and the second haplotype A29,B44,DR3. Mixed lymphocyte cultures of cells from the patient with cells from the cord blood and peripheral blood of the donor were negative. The cord-blood cells were less reactive against a pool of allogeneic cells than were the peripheral-blood cells (incorporation of [3H]thymidine, 15,437 vs. 112,954 cpm). The ABO blood group of the donor was O Rh+, and that of the recipient B Rh+.
The patient was admitted in September 1988, with the following hematologic values: hemoglobin concentration, 6.8 g per deciliter; white-cell count, 3.1 x 109 per liter, with 7 percent granulocytes, 86 percent lymphocytes, and 5 percent monocytes; and platelet count, 18 x 109 per liter. The marrow was hypocellular, with 10 percent of normal cellularity, 24 percent myeloid cells, 2 percent erythroblast cells, 67 percent lymphocytes, and no megakaryocytes. There were no hemorrhagic or infectious complications of the patient's illness. His liver and kidney functions were normal. Serologic tests were positive for cytomegalovirus (on enzyme-linked immunosorbent assay) and negative for human immunodeficiency virus, hepatitis B, and toxoplasmosis.
The patient was isolated in a room with laminar airflow, and treatment with oral broad-spectrum nonabsorbable antibiotics (vancomycin, tobramycin, and colistin [Colimycine]) was started nine days before transplantation (on day -8). Fluconazole (50 mg per day) was administered to prevent fungal infection, and oral acyclovir (100 mg per day) to prevent herpes simplex virus infection. For pretransplantation conditioning, cyclophosphamide (5 mg per kilogram of body weight) was given intravenously for four consecutive days (from day -6 to day -3; total, 380 mg) along with hyperhydration. Irradiation was delivered to the thoracoabdominal region by a linear accelerator on day -1 (mean rate, 10.87 cGy per minute), for a total of 5 Gy over a period of 46 minutes; the abdomen received 500 cGy, and the lungs and the right liver lobe, which were shielded, received 67 cGy.
On the day of transplantation (day 0 – October 6, 1988), cryopreserved umbilical-cord blood was thawed and infused without further processing, according to predetermined optimal conditions12 (the surviving whole red cells that had not been hemolyzed belonged to group O). The patient received 0.4 x 108 nucleated cells per kilogram, of which a total of 4.37 x 105 were CFU-GM (as determined by assay in Paris). Two hours after the infusion, the patient had chills, fever, and hypotension. These symptoms soon resolved, while the patient was receiving the broad-spectrum antibiotics vancomycin and ceftazidime intravenously. For prophylaxis against graft-versus-host disease, cyclosporine was administered intravenously from day – 1 (4.5 mg per kilogram per day), according to a preliminary pharmacokinetic study. All blood products were irradiated (25 Gy).
Ethical and Regulatory Considerations
Written informed consent was obtained from the patient's parents for collecting the umbilical-cord blood and for the transplantation procedure. The treatment plan was reviewed and approved by the institutional review board for clinical investigation of the Duke University Medical Center and by the ethics committee of the Hôpital Saint-Louis. Approval for the receipt, cryopreservation, storage, and release of cord blood was received from the institutional review board of the Indiana University School of Medicine. The Food and Drug Administration considered the procedure equivalent to the storage and transplantation of bone marrow, which are currently not subject to its regulation.
Methods
Cytogenetic Studies
Chromosome-breakage studies were performed as described elsewhere [4]. Diepoxybutane was added to bone marrow cultures when they were begun, and the cultured cells were harvested after 24 hours. Peripheral blood was cultured in the presence of phytohemagglutinin for 72 hours; diepoxybutane was present in the medium during the last 48 hours of culture. The frequency of chromosome breakage before and after the addition of diepoxybutane was analyzed in Giemsa-stained metaphase preparations; the ratio of cells from the patient to cells from the donor (male:female) was determined on quinacrine-stained slides to facilitate the identification of the Y chromosome.
DNA Studies: Restriction-Fragment-Length PolymorphismDNA samples obtained for Southern blotting were digested with Taq1 (New England Biolabs, Beverly, Mass.), separated by gel electrophoresis, transferred to an Immobilon-N filter (Millipore Corp., Bedford, Mass.), hybridized, and washed as previously described [13]. The probe used was CRI-pS232 (DXS278) (Collaborative Research, Boston), which hybridizes with sequences from the X and Y chromosomes.
Collection, Storage, and Shipment of Neonatal Blood
Immediately after the birth of the patient's sister, blood was obtained from her umbilical cord and the placenta as described elsewhere [12] and transported at ambient temperature by overnight express service to a laboratory for cellular analysis, cryopreservation, and storage (Indiana University School of Medicine). A sample of cord blood was also sent elsewhere for cytogenetic analysis (Rockefeller University). After a small sample (<2 ml) had been set aside for laboratory tests, including the determination of the level of nucleated cells and the enumeration of progenitor cells, the blood was frozen without further treatment in dimethyl sulfoxide at a final concentration of 10 percent (vol/vol) as previously described [12]. Two bags of cord blood and one bag of placental blood were frozen. Samples (about 1 ml each in Nunc tubes) were similarly frozen for testing of cell recovery after thawing and for confirmation of the HLA types. The volume of blood and the numbers of nucleated and progenitor cells collected are shown in Table 2. These values were within the range associated with successful transplantation of HLA–matched allogeneic bone marrow [12]. Testing of thawed cells, including those in one tube sent from Indiana University to Duke University Medical Center (where the HLA types were confirmed), demonstrated recovery of 79 percent to 90 percent of nucleated cells; on day 14, the mean (±1 SEM) rates of recovery were 100 percent ofCFU-GM, 63±18 percent of BFU-E, and 79±15 percent of CFU-GEMM.
Table 2. Hematopoietic Progenitor Cells in Blood from the Umbilical Cord and Placenta of the Donor and Bone Marrow from the Recipient.
* The preparation for the assays has been described elsewhere [12]. The assays of the cord blood and the bone marrow on day 120 were performed in Indianapolis, and those of the bone marrow at day 0 and day 30 in Paris.
† Plus-minus values are means ± 1 SEM; ND denotes not done.
‡ The total volume of cord and placental blood collected was 160 ml and contained 1.19 x 109 nucleated cells.
§ Normal range (Indianapolis laboratory) for low-density cells. 10 to 70 for CFU-GM and 15 to 80 for BFU-E-1 and BFU-E-2.
These were mainly microclusters, with less than 20 cells per cluster.
|
Source of Cells |
Progenitor Cells† |
|
|---|---|---|
|
all densities |
low density |
|
|
Donor (cord and placental blood)‡ |
total cells x 10-5 |
|
|
Agar culture |
1.52 |
ND |
|
Day 14 CFU-GM (colonies and clusters) |
2.46 |
ND |
|
Methylcellulose culture (colonies) |
1.56 |
ND |
|
BFU-E-2 |
3.95 |
ND |
|
BFU-E-1 |
3.60 |
ND |
|
CFU-GEMM |
0.39 |
ND |
|
Recipient (bone marrow) |
cells/105 cells plated§ |
|
|
Methylcellulose culture, day 0 |
ND |
1 |
|
Day 14 CFU-GM (colonies and clusters) |
ND |
8 |
|
BFU-E-1 |
ND |
0 |
|
CFU-GEMM |
ND |
0 |
|
Methylcellulose culture, day 30 |
ND |
9 |
|
BFU-E-1 |
ND |
0 |
|
CFU-GEMM |
ND |
0 |
|
Agar culture, day 120 |
22±2 |
140±12 |
|
Day 7 CFU-GM (colonies and clusters) |
118±16 |
416±20 |
|
Day 14 CFU-GM (colonies) |
36±4 |
156±8 |
|
Day 14 CFU-GM (colonies and clusters) |
152±4 |
228±12 |
|
Methylcellulose culture, day 120 |
324±16 |
416±25 |
|
BFU-E-2 |
77±2 |
134±6 |
|
BFU-E-1 |
96±8 |
132±10 |
|
CFU-GEMM |
4±1 |
9±1 |
The two bags of frozen cord blood and the bag of placental blood were sent with an escort by air (with the approval of the airline) to the Hôpital Saint-Louis from Indiana University two weeks before transplantation. The bags were sent in a Dry Shipper container (CMC-3200 wide mouth with platform; Cryomed, New Baltimore, Mich.) maintained at -175°C, a temperature optimal for cryopreservation.
Hematopoietic Progenitor Cells in Vitro
Assays were prepared as previously described [12]. In the CFU-GM assay, colonies (>40 cells per aggregate) and clusters (3 to 40 cells per aggregate) were scored after 7 days and 14 days of incubation in agar culture medium. Large-sized colonies formed (>1000 cells). Cell counts were expressed also as colonies plus clusters, for a more accurate estimate of the total CFU-GM compartment. In the assays for BFU-E, CFU-GEMM, and CFU-GM, colonies were scored after 14 days of incubation in methylcellulose culture medium. In the BFU-E-1, CFU-GEMM, and CFU-GM assays, colonies were scored from the same plates, which included erythropoietin (1 unit per milliliter), hemin (0.1 mM), and 5637 conditioned medium (10 percent vol/vol). BFU-E-2 cells were cultured as BFU-E-1, but without 5637 conditioned medium. Each BFU-E-2 colony contained at least 50 cells or comprised at least three subcolonies, each of which contained at least 10 cells, but were usually much larger. Colonies derived from BFU-E-1 were much larger than those derived from BFU-E-2.
Thawing and Recovery of Cells
Eighty-two percent of nucleated cells of the thawed blood transfused into the patient were viable. Progenitor-cell assays performed in Paris (which differed slightly in technique from assays performed in Indianapolis) indicated that the rate of cell recovery was equal to or greater than the count of progenitor cells recorded before freezing.
Results
Clinical Findings
The clinical course of the patient was uneventful and without complications. He tolerated the pretransplantation conditioning without evident toxic effects. On day 15, a transient skin rash and fever resolved with methylprednisolone treatment (2 mg per kilogram). A skin biopsy revealed few vacuolar basal epidermal cells with a mild lymphoid infiltrate, indicative of grade I graft-versus-host disease as defined according to the Seattle classification [14]. Liver-function tests showed that the serum levels of aspartate and alanine aminotransferases were twice normal, probably as a result of the graft-versus-host disease; values returned to normal on day 47. Cytomegalovirus was repeatedly isolated from the urine, but the patient never had any signs of active infection, and all tests for viremia were negative. Five months after transplantation the patient was discharged with normal clinical and laboratory findings. The doses of cyclosporine and corticosteroids were progressively reduced, and the drugs were discontinued at six months. At present (nine months after transplantation), the patient has no chronic graft-versus-host disease and leads a normal life.
Hematologic Findings
The blood-cell counts began to return to normal (Table 3).
Table 3. Blood-Cell Counts before and after Transplantation
|
Day |
Hemoglobin |
Leukocytes |
Granulocytes |
Lymphocytes |
Platelets |
Reticuloytes |
|---|---|---|---|---|---|---|
|
g/dl |
no. of cells x 10-9 per liter |
|||||
|
-20 |
6.8 |
3.1 |
0.25 |
2.8 |
18 |
10 |
|
0 |
9.7 |
0.8 |
0.0 |
0.8 |
120 |
0 |
|
8 |
10.9 |
0.4 |
0.0 |
0.4 |
80 |
0 |
|
15 |
11.6 |
0.4 |
0.0 |
0.4 |
39 |
0 |
|
22 |
7.8 |
0.9 |
0.3 |
0.6 |
50 |
5 |
|
29 |
8.5 |
1.0 |
0.3 |
0.5 |
105 |
17 |
|
36 |
9.4 |
1.7 |
0.6 |
0.5 |
55 |
36 |
|
43 |
11.3 |
5.1 |
2.4 |
1.9 |
31 |
90 |
|
50 |
8.9 |
3.4 |
1.5 |
0.7 |
62 |
162 |
|
57 |
8.9 |
5.6 |
3.2 |
1.0 |
174 |
63 |
|
90 |
11.3 |
5.1 |
4.0 |
1.1 |
296 |
50 |
|
120 |
13.0 |
3.9 |
2.3 |
1.1 |
265 |
40 |
|
160 |
12.0 |
3.7 |
1.4 |
1.6 |
293 |
45 |
|
240 |
12.3 |
5.2 |
2.7 |
1.6 |
354 |
50 |
|
282 |
12.2 |
4.8 |
2.3 |
1.2 |
315 |
--- |
The reticulocyte and granulocyte counts had begun to rise by day 22 after transplantation. The patient received eight transfusions of packed red cells (O Rh+) and 48 units of random platelets. Red cells were last transfused on day 54, and platelets on day 43. Bone marrow aspirated on day 17 was aplastic: an evaluation on day 28 showed 20 percent cellularity, with 19 percent myeloid cells, 73 percent erythroid cells, and few megakaryocytes. On day 120, the marrow had normal cellularity, with 40 percent myeloid cells, 44 percent erythroid cells, and a normal level of megakaryocytes.
Hematopoietic Progenitor Cells
Before transplantation, the marrow contained few or no detectable progenitor cells (Table 2). At 30 days after transplantation, CFU-GM cells were detected but not BFU-E or CFU-GEMM; at 120 days, progenitors were apparent at normal to supranormal frequencies (colonies or clusters per number of cells plated).
Reconstitution by Donor Cells
Blood- Type Studies
The patient's red cells (B Rh+) disappeared progressively and became undetectable on day 90 after transplantation; 46 days after the last transfusion, 100 percent of red cells were of the donor's blood type (O Rh+) and were found to have remained so at 240 days after transplantation.
Cytogenetic Studies
Table 1 shows the results of cytogenetic studies of bone marrow aspirated on day 120 and peripheral blood obtained on days 50, 64, 120, and 204. The chromosomal complement of the bone marrow was 46,XX. No cells of the patient (male cells) in metaphase were seen among 50 quinacrine-stained or 100 Giemsa-stained cells analyzed. The chromosomebreakage frequencies were 0.04 and 0.30 breaks per cell in the base-line and diepoxybutane-treated cultures, respectively.
Through day 120 after transplantation, more than half the metaphases seen in cytogenetic preparations of phytohemagglutinin-stimulated peripheral-blood cultures were of host origin, as indicated by the presence of a Y chromosome. These cells, of lymphoid origin, had greatly elevated levels of chromosome breakage at base line and severe radiation damage, manifested by the presence of multiple dicentrics, rings, and chromosomal fragments; they were also hypersensitive to the clastogenic effect of diepoxybutane, showing multiple chromatid breaks and exchanges typical of the cells characterizing Fanconi's anemia. The cells of donor origin (female) did not have elevated levels of chromosome breakage. By day 204 (61/2 months after transplantation), the majority of peripheral-blood lymphocytes were of donor origin.
These findings reflected engraftment with the donor cells and survival of a minor population of radiationdamaged host cells in the blood – an outcome similar to that in reports of bone marrow transplantation by others [15].
DNA Studies
The CRI-pS232 probe recognizes a complex set of fragments at a highly polymorphic locus on the X chromosome, as well as a polymorphic locus on the Y chromosome [16]. In the present case, all the variable bands present in the DNA of the donor were seen in the DNA extracted from the peripheral blood of the recipient after transplantation (Fig. 1). In addition, the X and Y alleles of the recipient were seen as faint bands, indicating some chimerism in the peripheral blood, with primarily donor cells present.
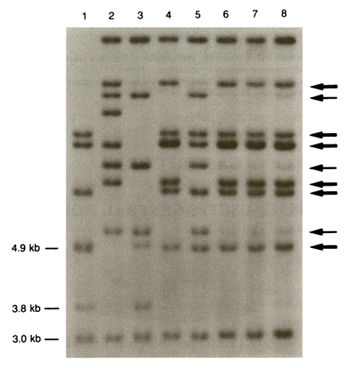
Figure 1. Southern Blot Analysis of DNA from the Patient and His Family.
DNA was extracted from the peripheral blood of the father (lane 1), the mother (lane 2), the patient before transplantation (lane 3), the patient's HI.A-identical sister (lane 4), the patient's HA non-identical sister (lane 5), and the patient on post-transplantation day 50 (lane 6), day 64 (lane 7), and day 120 (lane 8).
The DNA obtained from the patient after transplantation was primarily of donor origin. Each DNA sample was digested with the restriction enzyme Taq1 and examined with the probe CRI-pS232, which recognizes a complex set of fragments at a highly polymorphic locus on the X chromosome as well as a locus on the Y chromosome. The thick arrows indicate X-specific bands from the donor, and the thin arrows denote those from the recipient. Y-specific bands are seen at 4.9 and 3.8 kb. A constant band at 3.0 kb is seen in the DNA of all the subjects.
Discussion
Bone marrow and, under certain circumstances, the blood of adults (see references cited by Broxmeyer et al [12]) and the liver of fetuses [17] have been used in the transplantation of hematopoietic cells. The clinical and biologic data presented above show that the umbilical-cord blood of a single newborn is sufficient to induce hematopoietic reconstitution. The virtually complete occupation of the patient's myeloid system by cells from his sibling was indicated by the cytogenetic studies, blood typing, and studies of DNA polymorphisms and by the absence of undue chromosomal fragility. At present, a small percentage of lymphoid cells with chromosome damage remains in the circulation, but there has been a trend toward the elimination of these damaged cells.
There may be several reasons why cellular repopulation was somewhat delayed in our patient as compared with patients who have undergone transplantation with HLA-matched allogeneic (sibling) bone marrow. For instance, cells that have been frozen and thawed may take longer than fresh cells to seed, respond, and differentiate in their respective inducing microenvironments. Also, consistent with the relative paucity of CFU-GM on day 7 as compared with the more immature CFU-GM on day 14 [12], umbilical-cord blood may typically have a profile with immaturity and less differentiation of hematopoietic stem and progenitor cells. The modified conditioning regimen was adequate to permit complete engraftment with 0.4 x 108 total nucleated cord-blood cells per kilogram, as compared with the mean of 3 x 108 total nucleated bone marrow cells per kilogram that is usually given for bone marrow transplantation.
The use of cord blood in the treatment of Fanconi's anemia may be extended to the treatment of other conditions for which bone marrow transplantation is indicated, and demonstrates the potential of cryopreservation for prospective use of autologous blood.
In the latter respect, our success with allogeneic cord blood is particularly important, because studies in animals have shown that fewer reconstituting cells are required to restore hematopoietic function when these are syngeneic rather than allogeneic [18].
Thus, umbilical-cord blood can be considered an efficacious source of sufficient cells for clinical hematopoietic reconstitution.
Acknowledgements
We are indebted to Dr. Bo Dupont (Sloan-Kettering Institute for Cancer Research) for suggesting the clinical application in Fanconi's anemia, to Dr. Marilyn Pollack (Baylor Medical Center) for HLA typing of the amniotic cells, to Dr. Rebecca H. Buckley (Duke University) for the data from the mixed lymphocyte cultures, to Rita Ghosh, Lui Qian, and Drew Olsen (Rockefeller University) for technical help with the cytogenetic studies, to Dr. William Mann and V.S. Venkatraj (Rockeleller University) for DNA analysis, to Françoise Varrin (Paris) for technical assistance in the assessment of hematopoietic progenitors, to Ms. Linda Cheung (Indiana University) for help in preparing the manuscript, and to Collaborative Research for the probe pS232.
Supported in part by grants from the Biocyte Corporation, by grants (CA36464 and CA-36740 to Dr. Broxmeyer and CA-39827 to Dr. Boyse) from the National Cancer Institute, by a grant (HL-32987 to Dr. Auerbach) from the National Institutes of Health, and by a grant from the Pew Memorial Trust to Rockefeller University. Dr. Boyse holds a Research Professorship from the American Cancer Society, and Dr. Kurtzberg is a Special Fellow of the Leukemia Society of America. In accordance with the Journal's policy, the authors have provided the following information: Dr. Broxmeyer, Dr. Douglas, Ms. Bard, and Dr. Boyse are shareholders in Biocyte Corporation (New York), and Dr. Douglas and Dr. Boyse are members of its board of directors.
References
1. Fanconi G. Familial constitutional panmyelocytopathy, Fanconi's anemia (F.A.). L Clinical aspects. Semin Hematol. 1967;4:233-40. pmid: 6074578.
2. Schroeder TM, Tilgen D, Kruger J, Vogel F. Formal genetics of Fanconi's anemia. Hum Genet. 1976;32:257-88. pmid: 939547.
4. Auerbach AD, Wolman SR. Susceptibility of Fanconi's anaemia fibroblasts to chromosome damage by carcinogens. Nature. 1976;261:494-6. pmid: 934283.
5. Auerbach AD, Sagi M, Adler B. Fanconi anemia: prenatal diagnosis in 30 fetuses at risk. Pediatrics. 1985;76:794-800. pmid: 4058989.
6. Auerbach AD, Min Z, Ghosh R, et al. Clastogen-induced chromosomal breakage as a marker for first trimester prenatal diagnosis of Fanconi anemia. Hum Genet. 1986;73:86-8. pmid: 3458668.
8. Gluckman E, Devergie A, Dutreix J. Bone marrow transplantation for Fanconi's anemia. In: Schroeder-Kurth TM, Auerbach AD, Obe G, eds. Fanconi anemia: clinical, cytogenetic and experimental aspects. New York: Springer-Verlag. 1989:60-8.
9. Gluckman E, Devergie A, Schaison G, et al. Bone marrow transplantation in Fanconi anemia. Br J Haematol. 1980;45:557-64. pmid: 7000153.
10. Berger R, Bernheim A, Gluckman E, Gisselbrecht C. In vitro effect of cyclophosphamide metabolites on chromosomes of Fanconi anaemia patients. Br J Haematol. 1980;45:565-8. pmid: 7426437.
11. Gluckman E, Devergie A, Dutreix J. Radiosensitivity in Fanconi anaemia: application to the conditioning regimen for bone marrow transplantation. Br J Haematol. 1983;54:431-40. pmid: 6344915.
17. Gale RP, Touraine 1-L, Lucarelli G, eds. Fetal liver transplantation: proceedings of an international symposium held in Pesaro, Italy, September 29-October I, 1984. Vol. 193. Progress in clinical and biological research. New York: Alan R. Liss. 1985:327-42.
18. Balner H. Bone marrow transplantation and other treatment after radiation injury. The Hague, Netherlands: Martinus Nijhoff. 197.
© 1989 Massachusetts Medical Society. All rights reserved.
Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. PMID: 2571931
Case Report
The patient, a five-year-old boy, was first noted to have pancytopenia at 24 months of age. An evaluation (Duke University Medical Center) showed the following hematologic values: hemoglobin concentration, 9.5 g per deciliter; white-cell count, 4.3 x 109 per liter, with 22 percent granulocytes, 62 percent lymphocytes, 3 percent monocytes, 1 percent eosinophils, and 8 percent basophils; platelet count, 62 x 109 per liter; and reticulocyte level, 2.3 percent. The bone marrow was hypocellular. The patient had the classic malformations of Fanconi's anemia, including retarded growth (5th to 10th percentile), a rudimentary extra thumb on the left hand, the absence of a left kidney, and hypospadias. Testing of the patient's cells with diepoxybutane, performed at 24 months (Rockefeller University), confirmed the diagnosis of Fanconi's anemia. The parents were healthy, and there was no consanguinity or past history of blood disorders in the family. The patient had been treated with danazol (300 mg per day for six months), with a progressive decrease in the blood-cell counts. Before admission, he had received three units of filtered and irradiated packed red cells.
The patient's mother became pregnant in June 1987. Cytogenetic analysis of cultured amniotic-fluid cells (Rockefeller University) showed that the values for chromosome breakage before and after the cells were exposed to diepoxybutane were within the normal range [5]. A girl was delivered vaginally without complications in February 1988. Studies of chromosome breakage in umbilical-cord blood cells indicated that the newborn had a normal karyotype and was not affected by Fanconi's anemia (Table 1).
Table 1. Results of Cytogenetic Analysis.*
*DEB denotes diepoxybutane; its final concentration in the culture medium was 0.1 mg per milliliter in each analysis in this table.
†Analysis performed on quinacrine-stained metaphase preparations.
‡Analysis performed on Giemsa-stained metaphase preparations.
|
Source Of Cells |
Percent Donor |
Mean Chromosome |
||
|---|---|---|---|---|
|
before deb |
after deb |
before deb |
after deb |
|
|
Patient's peripheral blood on day 0 |
0 |
0 |
0.18 |
10.6 |
|
Donor's cord blood on day 0 |
100 |
100 |
0.00 |
0.02 |
|
Patient's bone marrow on day 120 |
100 |
100 |
0.04 |
0.30 |
|
Patient's peripheral blood |
30 |
52 |
0.7 |
4.0 |
|
Day 64 |
8 |
32 |
1.3 |
5.0 |
|
Day 120 |
12 |
32 |
1.9 |
6.4 |
|
Day 204 |
64 |
86 |
0.30 |
0.49 |
Prenatal HLA typing of amniotic-fluid cells (Dr. M.S. Pollack, Methodist Hospital and Baylor Medical Center, Houston) had shown that the fetus was HLA identical to the patient: the first haplotype was Al,B8,DR3, and the second haplotype A29,B44,DR3. Mixed lymphocyte cultures of cells from the patient with cells from the cord blood and peripheral blood of the donor were negative. The cord-blood cells were less reactive against a pool of allogeneic cells than were the peripheral-blood cells (incorporation of [3H]thymidine, 15,437 vs. 112,954 cpm). The ABO blood group of the donor was O Rh+, and that of the recipient B Rh+.
The patient was admitted in September 1988, with the following hematologic values: hemoglobin concentration, 6.8 g per deciliter; white-cell count, 3.1 x 109 per liter, with 7 percent granulocytes, 86 percent lymphocytes, and 5 percent monocytes; and platelet count, 18 x 109 per liter. The marrow was hypocellular, with 10 percent of normal cellularity, 24 percent myeloid cells, 2 percent erythroblast cells, 67 percent lymphocytes, and no megakaryocytes. There were no hemorrhagic or infectious complications of the patient's illness. His liver and kidney functions were normal. Serologic tests were positive for cytomegalovirus (on enzyme-linked immunosorbent assay) and negative for human immunodeficiency virus, hepatitis B, and toxoplasmosis.
The patient was isolated in a room with laminar airflow, and treatment with oral broad-spectrum nonabsorbable antibiotics (vancomycin, tobramycin, and colistin [Colimycine]) was started nine days before transplantation (on day -8). Fluconazole (50 mg per day) was administered to prevent fungal infection, and oral acyclovir (100 mg per day) to prevent herpes simplex virus infection. For pretransplantation conditioning, cyclophosphamide (5 mg per kilogram of body weight) was given intravenously for four consecutive days (from day -6 to day -3; total, 380 mg) along with hyperhydration. Irradiation was delivered to the thoracoabdominal region by a linear accelerator on day -1 (mean rate, 10.87 cGy per minute), for a total of 5 Gy over a period of 46 minutes; the abdomen received 500 cGy, and the lungs and the right liver lobe, which were shielded, received 67 cGy.
On the day of transplantation (day 0 – October 6, 1988), cryopreserved umbilical-cord blood was thawed and infused without further processing, according to predetermined optimal conditions12 (the surviving whole red cells that had not been hemolyzed belonged to group O). The patient received 0.4 x 108 nucleated cells per kilogram, of which a total of 4.37 x 105 were CFU-GM (as determined by assay in Paris). Two hours after the infusion, the patient had chills, fever, and hypotension. These symptoms soon resolved, while the patient was receiving the broad-spectrum antibiotics vancomycin and ceftazidime intravenously. For prophylaxis against graft-versus-host disease, cyclosporine was administered intravenously from day – 1 (4.5 mg per kilogram per day), according to a preliminary pharmacokinetic study. All blood products were irradiated (25 Gy).
Ethical and Regulatory Considerations
Written informed consent was obtained from the patient's parents for collecting the umbilical-cord blood and for the transplantation procedure. The treatment plan was reviewed and approved by the institutional review board for clinical investigation of the Duke University Medical Center and by the ethics committee of the Hôpital Saint-Louis. Approval for the receipt, cryopreservation, storage, and release of cord blood was received from the institutional review board of the Indiana University School of Medicine. The Food and Drug Administration considered the procedure equivalent to the storage and transplantation of bone marrow, which are currently not subject to its regulation.
Methods
Cytogenetic Studies
Chromosome-breakage studies were performed as described elsewhere [4]. Diepoxybutane was added to bone marrow cultures when they were begun, and the cultured cells were harvested after 24 hours. Peripheral blood was cultured in the presence of phytohemagglutinin for 72 hours; diepoxybutane was present in the medium during the last 48 hours of culture. The frequency of chromosome breakage before and after the addition of diepoxybutane was analyzed in Giemsa-stained metaphase preparations; the ratio of cells from the patient to cells from the donor (male:female) was determined on quinacrine-stained slides to facilitate the identification of the Y chromosome.
DNA Studies: Restriction-Fragment-Length PolymorphismDNA samples obtained for Southern blotting were digested with Taq1 (New England Biolabs, Beverly, Mass.), separated by gel electrophoresis, transferred to an Immobilon-N filter (Millipore Corp., Bedford, Mass.), hybridized, and washed as previously described [13]. The probe used was CRI-pS232 (DXS278) (Collaborative Research, Boston), which hybridizes with sequences from the X and Y chromosomes.
Collection, Storage, and Shipment of Neonatal Blood
Immediately after the birth of the patient's sister, blood was obtained from her umbilical cord and the placenta as described elsewhere [12] and transported at ambient temperature by overnight express service to a laboratory for cellular analysis, cryopreservation, and storage (Indiana University School of Medicine). A sample of cord blood was also sent elsewhere for cytogenetic analysis (Rockefeller University). After a small sample (<2 ml) had been set aside for laboratory tests, including the determination of the level of nucleated cells and the enumeration of progenitor cells, the blood was frozen without further treatment in dimethyl sulfoxide at a final concentration of 10 percent (vol/vol) as previously described [12]. Two bags of cord blood and one bag of placental blood were frozen. Samples (about 1 ml each in Nunc tubes) were similarly frozen for testing of cell recovery after thawing and for confirmation of the HLA types. The volume of blood and the numbers of nucleated and progenitor cells collected are shown in Table 2. These values were within the range associated with successful transplantation of HLA–matched allogeneic bone marrow [12]. Testing of thawed cells, including those in one tube sent from Indiana University to Duke University Medical Center (where the HLA types were confirmed), demonstrated recovery of 79 percent to 90 percent of nucleated cells; on day 14, the mean (±1 SEM) rates of recovery were 100 percent ofCFU-GM, 63±18 percent of BFU-E, and 79±15 percent of CFU-GEMM.
Table 2. Hematopoietic Progenitor Cells in Blood from the Umbilical Cord and Placenta of the Donor and Bone Marrow from the Recipient.
* The preparation for the assays has been described elsewhere [12]. The assays of the cord blood and the bone marrow on day 120 were performed in Indianapolis, and those of the bone marrow at day 0 and day 30 in Paris.
† Plus-minus values are means ± 1 SEM; ND denotes not done.
‡ The total volume of cord and placental blood collected was 160 ml and contained 1.19 x 109 nucleated cells.
§ Normal range (Indianapolis laboratory) for low-density cells. 10 to 70 for CFU-GM and 15 to 80 for BFU-E-1 and BFU-E-2.
These were mainly microclusters, with less than 20 cells per cluster.
|
Source of Cells |
Progenitor Cells† |
|
|---|---|---|
|
all densities |
low density |
|
|
Donor (cord and placental blood)‡ |
total cells x 10-5 |
|
|
Agar culture |
1.52 |
ND |
|
Day 14 CFU-GM (colonies and clusters) |
2.46 |
ND |
|
Methylcellulose culture (colonies) |
1.56 |
ND |
|
BFU-E-2 |
3.95 |
ND |
|
BFU-E-1 |
3.60 |
ND |
|
CFU-GEMM |
0.39 |
ND |
|
Recipient (bone marrow) |
cells/105 cells plated§ |
|
|
Methylcellulose culture, day 0 |
ND |
1 |
|
Day 14 CFU-GM (colonies and clusters) |
ND |
8 |
|
BFU-E-1 |
ND |
0 |
|
CFU-GEMM |
ND |
0 |
|
Methylcellulose culture, day 30 |
ND |
9 |
|
BFU-E-1 |
ND |
0 |
|
CFU-GEMM |
ND |
0 |
|
Agar culture, day 120 |
22±2 |
140±12 |
|
Day 7 CFU-GM (colonies and clusters) |
118±16 |
416±20 |
|
Day 14 CFU-GM (colonies) |
36±4 |
156±8 |
|
Day 14 CFU-GM (colonies and clusters) |
152±4 |
228±12 |
|
Methylcellulose culture, day 120 |
324±16 |
416±25 |
|
BFU-E-2 |
77±2 |
134±6 |
|
BFU-E-1 |
96±8 |
132±10 |
|
CFU-GEMM |
4±1 |
9±1 |
The two bags of frozen cord blood and the bag of placental blood were sent with an escort by air (with the approval of the airline) to the Hôpital Saint-Louis from Indiana University two weeks before transplantation. The bags were sent in a Dry Shipper container (CMC-3200 wide mouth with platform; Cryomed, New Baltimore, Mich.) maintained at -175°C, a temperature optimal for cryopreservation.
Hematopoietic Progenitor Cells in Vitro
Assays were prepared as previously described [12]. In the CFU-GM assay, colonies (>40 cells per aggregate) and clusters (3 to 40 cells per aggregate) were scored after 7 days and 14 days of incubation in agar culture medium. Large-sized colonies formed (>1000 cells). Cell counts were expressed also as colonies plus clusters, for a more accurate estimate of the total CFU-GM compartment. In the assays for BFU-E, CFU-GEMM, and CFU-GM, colonies were scored after 14 days of incubation in methylcellulose culture medium. In the BFU-E-1, CFU-GEMM, and CFU-GM assays, colonies were scored from the same plates, which included erythropoietin (1 unit per milliliter), hemin (0.1 mM), and 5637 conditioned medium (10 percent vol/vol). BFU-E-2 cells were cultured as BFU-E-1, but without 5637 conditioned medium. Each BFU-E-2 colony contained at least 50 cells or comprised at least three subcolonies, each of which contained at least 10 cells, but were usually much larger. Colonies derived from BFU-E-1 were much larger than those derived from BFU-E-2.
Thawing and Recovery of Cells
Eighty-two percent of nucleated cells of the thawed blood transfused into the patient were viable. Progenitor-cell assays performed in Paris (which differed slightly in technique from assays performed in Indianapolis) indicated that the rate of cell recovery was equal to or greater than the count of progenitor cells recorded before freezing.
Results
Clinical Findings
The clinical course of the patient was uneventful and without complications. He tolerated the pretransplantation conditioning without evident toxic effects. On day 15, a transient skin rash and fever resolved with methylprednisolone treatment (2 mg per kilogram). A skin biopsy revealed few vacuolar basal epidermal cells with a mild lymphoid infiltrate, indicative of grade I graft-versus-host disease as defined according to the Seattle classification [14]. Liver-function tests showed that the serum levels of aspartate and alanine aminotransferases were twice normal, probably as a result of the graft-versus-host disease; values returned to normal on day 47. Cytomegalovirus was repeatedly isolated from the urine, but the patient never had any signs of active infection, and all tests for viremia were negative. Five months after transplantation the patient was discharged with normal clinical and laboratory findings. The doses of cyclosporine and corticosteroids were progressively reduced, and the drugs were discontinued at six months. At present (nine months after transplantation), the patient has no chronic graft-versus-host disease and leads a normal life.
Hematologic Findings
The blood-cell counts began to return to normal (Table 3).
Table 3. Blood-Cell Counts before and after Transplantation
|
Day |
Hemoglobin |
Leukocytes |
Granulocytes |
Lymphocytes |
Platelets |
Reticuloytes |
|---|---|---|---|---|---|---|
|
g/dl |
no. of cells x 10-9 per liter |
|||||
|
-20 |
6.8 |
3.1 |
0.25 |
2.8 |
18 |
10 |
|
0 |
9.7 |
0.8 |
0.0 |
0.8 |
120 |
0 |
|
8 |
10.9 |
0.4 |
0.0 |
0.4 |
80 |
0 |
|
15 |
11.6 |
0.4 |
0.0 |
0.4 |
39 |
0 |
|
22 |
7.8 |
0.9 |
0.3 |
0.6 |
50 |
5 |
|
29 |
8.5 |
1.0 |
0.3 |
0.5 |
105 |
17 |
|
36 |
9.4 |
1.7 |
0.6 |
0.5 |
55 |
36 |
|
43 |
11.3 |
5.1 |
2.4 |
1.9 |
31 |
90 |
|
50 |
8.9 |
3.4 |
1.5 |
0.7 |
62 |
162 |
|
57 |
8.9 |
5.6 |
3.2 |
1.0 |
174 |
63 |
|
90 |
11.3 |
5.1 |
4.0 |
1.1 |
296 |
50 |
|
120 |
13.0 |
3.9 |
2.3 |
1.1 |
265 |
40 |
|
160 |
12.0 |
3.7 |
1.4 |
1.6 |
293 |
45 |
|
240 |
12.3 |
5.2 |
2.7 |
1.6 |
354 |
50 |
|
282 |
12.2 |
4.8 |
2.3 |
1.2 |
315 |
--- |
The reticulocyte and granulocyte counts had begun to rise by day 22 after transplantation. The patient received eight transfusions of packed red cells (O Rh+) and 48 units of random platelets. Red cells were last transfused on day 54, and platelets on day 43. Bone marrow aspirated on day 17 was aplastic: an evaluation on day 28 showed 20 percent cellularity, with 19 percent myeloid cells, 73 percent erythroid cells, and few megakaryocytes. On day 120, the marrow had normal cellularity, with 40 percent myeloid cells, 44 percent erythroid cells, and a normal level of megakaryocytes.
Hematopoietic Progenitor Cells
Before transplantation, the marrow contained few or no detectable progenitor cells (Table 2). At 30 days after transplantation, CFU-GM cells were detected but not BFU-E or CFU-GEMM; at 120 days, progenitors were apparent at normal to supranormal frequencies (colonies or clusters per number of cells plated).
Reconstitution by Donor Cells
Blood- Type Studies
The patient's red cells (B Rh+) disappeared progressively and became undetectable on day 90 after transplantation; 46 days after the last transfusion, 100 percent of red cells were of the donor's blood type (O Rh+) and were found to have remained so at 240 days after transplantation.
Cytogenetic Studies
Table 1 shows the results of cytogenetic studies of bone marrow aspirated on day 120 and peripheral blood obtained on days 50, 64, 120, and 204. The chromosomal complement of the bone marrow was 46,XX. No cells of the patient (male cells) in metaphase were seen among 50 quinacrine-stained or 100 Giemsa-stained cells analyzed. The chromosomebreakage frequencies were 0.04 and 0.30 breaks per cell in the base-line and diepoxybutane-treated cultures, respectively.
Through day 120 after transplantation, more than half the metaphases seen in cytogenetic preparations of phytohemagglutinin-stimulated peripheral-blood cultures were of host origin, as indicated by the presence of a Y chromosome. These cells, of lymphoid origin, had greatly elevated levels of chromosome breakage at base line and severe radiation damage, manifested by the presence of multiple dicentrics, rings, and chromosomal fragments; they were also hypersensitive to the clastogenic effect of diepoxybutane, showing multiple chromatid breaks and exchanges typical of the cells characterizing Fanconi's anemia. The cells of donor origin (female) did not have elevated levels of chromosome breakage. By day 204 (61/2 months after transplantation), the majority of peripheral-blood lymphocytes were of donor origin.
These findings reflected engraftment with the donor cells and survival of a minor population of radiationdamaged host cells in the blood – an outcome similar to that in reports of bone marrow transplantation by others [15].
DNA Studies
The CRI-pS232 probe recognizes a complex set of fragments at a highly polymorphic locus on the X chromosome, as well as a polymorphic locus on the Y chromosome [16]. In the present case, all the variable bands present in the DNA of the donor were seen in the DNA extracted from the peripheral blood of the recipient after transplantation (Fig. 1). In addition, the X and Y alleles of the recipient were seen as faint bands, indicating some chimerism in the peripheral blood, with primarily donor cells present.

Figure 1. Southern Blot Analysis of DNA from the Patient and His Family.
DNA was extracted from the peripheral blood of the father (lane 1), the mother (lane 2), the patient before transplantation (lane 3), the patient's HI.A-identical sister (lane 4), the patient's HA non-identical sister (lane 5), and the patient on post-transplantation day 50 (lane 6), day 64 (lane 7), and day 120 (lane 8).
The DNA obtained from the patient after transplantation was primarily of donor origin. Each DNA sample was digested with the restriction enzyme Taq1 and examined with the probe CRI-pS232, which recognizes a complex set of fragments at a highly polymorphic locus on the X chromosome as well as a locus on the Y chromosome. The thick arrows indicate X-specific bands from the donor, and the thin arrows denote those from the recipient. Y-specific bands are seen at 4.9 and 3.8 kb. A constant band at 3.0 kb is seen in the DNA of all the subjects.
Discussion
Bone marrow and, under certain circumstances, the blood of adults (see references cited by Broxmeyer et al [12]) and the liver of fetuses [17] have been used in the transplantation of hematopoietic cells. The clinical and biologic data presented above show that the umbilical-cord blood of a single newborn is sufficient to induce hematopoietic reconstitution. The virtually complete occupation of the patient's myeloid system by cells from his sibling was indicated by the cytogenetic studies, blood typing, and studies of DNA polymorphisms and by the absence of undue chromosomal fragility. At present, a small percentage of lymphoid cells with chromosome damage remains in the circulation, but there has been a trend toward the elimination of these damaged cells.
There may be several reasons why cellular repopulation was somewhat delayed in our patient as compared with patients who have undergone transplantation with HLA-matched allogeneic (sibling) bone marrow. For instance, cells that have been frozen and thawed may take longer than fresh cells to seed, respond, and differentiate in their respective inducing microenvironments. Also, consistent with the relative paucity of CFU-GM on day 7 as compared with the more immature CFU-GM on day 14 [12], umbilical-cord blood may typically have a profile with immaturity and less differentiation of hematopoietic stem and progenitor cells. The modified conditioning regimen was adequate to permit complete engraftment with 0.4 x 108 total nucleated cord-blood cells per kilogram, as compared with the mean of 3 x 108 total nucleated bone marrow cells per kilogram that is usually given for bone marrow transplantation.
The use of cord blood in the treatment of Fanconi's anemia may be extended to the treatment of other conditions for which bone marrow transplantation is indicated, and demonstrates the potential of cryopreservation for prospective use of autologous blood.
In the latter respect, our success with allogeneic cord blood is particularly important, because studies in animals have shown that fewer reconstituting cells are required to restore hematopoietic function when these are syngeneic rather than allogeneic [18].
Thus, umbilical-cord blood can be considered an efficacious source of sufficient cells for clinical hematopoietic reconstitution.
Acknowledgements
We are indebted to Dr. Bo Dupont (Sloan-Kettering Institute for Cancer Research) for suggesting the clinical application in Fanconi's anemia, to Dr. Marilyn Pollack (Baylor Medical Center) for HLA typing of the amniotic cells, to Dr. Rebecca H. Buckley (Duke University) for the data from the mixed lymphocyte cultures, to Rita Ghosh, Lui Qian, and Drew Olsen (Rockefeller University) for technical help with the cytogenetic studies, to Dr. William Mann and V.S. Venkatraj (Rockeleller University) for DNA analysis, to Françoise Varrin (Paris) for technical assistance in the assessment of hematopoietic progenitors, to Ms. Linda Cheung (Indiana University) for help in preparing the manuscript, and to Collaborative Research for the probe pS232.
Supported in part by grants from the Biocyte Corporation, by grants (CA36464 and CA-36740 to Dr. Broxmeyer and CA-39827 to Dr. Boyse) from the National Cancer Institute, by a grant (HL-32987 to Dr. Auerbach) from the National Institutes of Health, and by a grant from the Pew Memorial Trust to Rockefeller University. Dr. Boyse holds a Research Professorship from the American Cancer Society, and Dr. Kurtzberg is a Special Fellow of the Leukemia Society of America. In accordance with the Journal's policy, the authors have provided the following information: Dr. Broxmeyer, Dr. Douglas, Ms. Bard, and Dr. Boyse are shareholders in Biocyte Corporation (New York), and Dr. Douglas and Dr. Boyse are members of its board of directors.
References
1. Fanconi G. Familial constitutional panmyelocytopathy, Fanconi's anemia (F.A.). L Clinical aspects. Semin Hematol. 1967;4:233-40. pmid: 6074578.
2. Schroeder TM, Tilgen D, Kruger J, Vogel F. Formal genetics of Fanconi's anemia. Hum Genet. 1976;32:257-88. pmid: 939547.
4. Auerbach AD, Wolman SR. Susceptibility of Fanconi's anaemia fibroblasts to chromosome damage by carcinogens. Nature. 1976;261:494-6. pmid: 934283.
5. Auerbach AD, Sagi M, Adler B. Fanconi anemia: prenatal diagnosis in 30 fetuses at risk. Pediatrics. 1985;76:794-800. pmid: 4058989.
6. Auerbach AD, Min Z, Ghosh R, et al. Clastogen-induced chromosomal breakage as a marker for first trimester prenatal diagnosis of Fanconi anemia. Hum Genet. 1986;73:86-8. pmid: 3458668.
8. Gluckman E, Devergie A, Dutreix J. Bone marrow transplantation for Fanconi's anemia. In: Schroeder-Kurth TM, Auerbach AD, Obe G, eds. Fanconi anemia: clinical, cytogenetic and experimental aspects. New York: Springer-Verlag. 1989:60-8.
9. Gluckman E, Devergie A, Schaison G, et al. Bone marrow transplantation in Fanconi anemia. Br J Haematol. 1980;45:557-64. pmid: 7000153.
10. Berger R, Bernheim A, Gluckman E, Gisselbrecht C. In vitro effect of cyclophosphamide metabolites on chromosomes of Fanconi anaemia patients. Br J Haematol. 1980;45:565-8. pmid: 7426437.
11. Gluckman E, Devergie A, Dutreix J. Radiosensitivity in Fanconi anaemia: application to the conditioning regimen for bone marrow transplantation. Br J Haematol. 1983;54:431-40. pmid: 6344915.
17. Gale RP, Touraine 1-L, Lucarelli G, eds. Fetal liver transplantation: proceedings of an international symposium held in Pesaro, Italy, September 29-October I, 1984. Vol. 193. Progress in clinical and biological research. New York: Alan R. Liss. 1985:327-42.
18. Balner H. Bone marrow transplantation and other treatment after radiation injury. The Hague, Netherlands: Martinus Nijhoff. 197.
© 1989 Massachusetts Medical Society. All rights reserved.
Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. PMID: 2571931
Элиана Глюкман, Хэл Е. Броксмайер, Арлин Д. Ауэрбах, Генри С. Фридман, Гордон У. Дуглас, Агнес Девержи, Элен Эсперо, Доминик Тьерри, Жерар Соси, Пьер Лен, Скотт Купер, Денис Инглиш, Джоан Кюртцберг, Юдифь Бард, Эдвард А. Бойз
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18838" ["VALUE"]=> array(2) { ["TEXT"]=> string(3833) "<p class="bodytext">Клинические проявления анемии Фанкони, аутосомной рецессивной болезни, включают прогрессирующую панцитопению, предрасположенность к злокачественным опухолям и развитию аномалий, не связанных с гемопоэзом. Гиперчувствительность к кластогенным эффектам – разрывам хромосом под действием препаратов, способствующих сшивке цепей ДНК, таких как диэпоксибутан, используется как диагностический признак генотипа анемии Фанкони, как пре- так и постнатально. Пренатальное <br>HLA-типирование даёт возможность установить, является ли плод HLA-идентичным больному сиблингу. <br /><br />Мы описываем здесь восстановление гемопоэза у мальчика с тяжёлой формой анемии Фанкони, которому была введена криоконсервированная пуповинная кровь сестры, не поражённой, по данным пренатального тестирования, данным заболеванием, имевшей нормальный кариотип и HLA-идентичный фенотип. <br /><br />Мы использовали претрансплантационный режим кондиционирования, разработанный специально для таких больных; метод основан на гиперчувствительности аномальных клеток к алкилирующим агентам, вызывающих сшивки цепей ДНК, и воздействию радиации. Метод позволяет использовать пуповинную кровь и избежать забора клеток костного мозга у новорожденного сиблинга. Такое применение пуповинной крови вытекало из предположения одного из нас о том, что кровь, взятая из пуповинной вены при рождении и обычно не используемая, может восстанавливать гемопоэз – предположении, основанном на наших предварительных исследованиях, согласующихся с сообщениями о наличии гемопоэтических стволовых и мультипотентных (CFU-GEMM), эритроидных (BFU-E) и гранулоцитарно-макрофагальных (CFU-GM) клеток-предшественников в пуповинной крови человека (см. ссылки в работе Broxmeyer et al.).<br /><br /> <h3>Ключевые слова</h3> <p> анемия, апластическая терапия, консервация крови, анемия Фанкони, женская особь, плодная кровь, HLA антигены, трансплантация гемопоэтических стволовых клеток, тестирование гистосовместимости, человек, мужская особь, беременность, пренатальный диагноз, дети дошкольного возраста </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3751) "Клинические проявления анемии Фанкони, аутосомной рецессивной болезни, включают прогрессирующую панцитопению, предрасположенность к злокачественным опухолям и развитию аномалий, не связанных с гемопоэзом. Гиперчувствительность к кластогенным эффектам – разрывам хромосом под действием препаратов, способствующих сшивке цепей ДНК, таких как диэпоксибутан, используется как диагностический признак генотипа анемии Фанкони, как пре- так и постнатально. Пренатальное
HLA-типирование даёт возможность установить, является ли плод HLA-идентичным больному сиблингу.
Мы описываем здесь восстановление гемопоэза у мальчика с тяжёлой формой анемии Фанкони, которому была введена криоконсервированная пуповинная кровь сестры, не поражённой, по данным пренатального тестирования, данным заболеванием, имевшей нормальный кариотип и HLA-идентичный фенотип.
Мы использовали претрансплантационный режим кондиционирования, разработанный специально для таких больных; метод основан на гиперчувствительности аномальных клеток к алкилирующим агентам, вызывающих сшивки цепей ДНК, и воздействию радиации. Метод позволяет использовать пуповинную кровь и избежать забора клеток костного мозга у новорожденного сиблинга. Такое применение пуповинной крови вытекало из предположения одного из нас о том, что кровь, взятая из пуповинной вены при рождении и обычно не используемая, может восстанавливать гемопоэз – предположении, основанном на наших предварительных исследованиях, согласующихся с сообщениями о наличии гемопоэтических стволовых и мультипотентных (CFU-GEMM), эритроидных (BFU-E) и гранулоцитарно-макрофагальных (CFU-GM) клеток-предшественников в пуповинной крови человека (см. ссылки в работе Broxmeyer et al.).
Ключевые слова
анемия, апластическая терапия, консервация крови, анемия Фанкони, женская особь, плодная кровь, HLA антигены, трансплантация гемопоэтических стволовых клеток, тестирование гистосовместимости, человек, мужская особь, беременность, пренатальный диагноз, дети дошкольного возраста
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18839" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000079.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000079.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18871" ["VALUE"]=> array(2) { ["TEXT"]=> string(1035) "<p><strong>Eliane Gluckman</strong><sup>1</sup><strong>, Hal E. Broxmeyer</strong><sup>2</sup><strong>, Arleen D. Auerbach</strong><sup>3</sup><strong>, Henry S. Friedman</strong><sup>4</sup><strong>, Gordon W. Douglas</strong><sup>5</sup><strong>, Agnes Devergie</strong><sup>1</sup><strong>, Helene Esperou</strong><sup>1</sup><strong>, Dominique Thierry</strong><sup>6</sup><strong>, Gerard Socie<sup>1</sup>, Pierre Lehn</strong><sup>1</sup><strong>, Scott Cooper</strong><sup>2</sup><strong>, Denis English</strong><sup>2</sup><strong>, Joanne Kurtzberg</strong><sup>4</sup><strong>, Judith Bard</strong><sup>7</sup><strong>, and Edward A. Boyse</strong><sup>7</sup></p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(675) "Eliane Gluckman1, Hal E. Broxmeyer2, Arleen D. Auerbach3, Henry S. Friedman4, Gordon W. Douglas5, Agnes Devergie1, Helene Esperou1, Dominique Thierry6, Gerard Socie1, Pierre Lehn1, Scott Cooper2, Denis English2, Joanne Kurtzberg4, Judith Bard7, and Edward A. Boyse7
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18872" ["VALUE"]=> array(2) { ["TEXT"]=> string(826) "<p class="bodytext"><sup>1</sup>Bone Marrow Transplant Unit, Hôpital Saint-Louis, Paris, France; <sup>2</sup>Departments of Medicine (Hematology/Oncology), Microbiology and Immunology, Pathology, and the Walther Oncology Center, Indiana University School of Medicine, Indianapolis, USA; <sup>3</sup>Laboratory for Investigative Dermatology, Rockefeller University, New York, USA; <sup>4</sup>Department of Pediatrics (Hematology/Oncology), Duke University Medical Center, Durham, N.C., USA; <sup>5</sup>Department of Obstetrics and Gynecology, New York University Medical Center, New York, USA; <sup>6</sup>Central Nuclear Agency, Paris, France; <sup>7</sup>Memorial Sloan-Kettering Cancer Center, New York, USA. </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(720) "1Bone Marrow Transplant Unit, Hôpital Saint-Louis, Paris, France; 2Departments of Medicine (Hematology/Oncology), Microbiology and Immunology, Pathology, and the Walther Oncology Center, Indiana University School of Medicine, Indianapolis, USA; 3Laboratory for Investigative Dermatology, Rockefeller University, New York, USA; 4Department of Pediatrics (Hematology/Oncology), Duke University Medical Center, Durham, N.C., USA; 5Department of Obstetrics and Gynecology, New York University Medical Center, New York, USA; 6Central Nuclear Agency, Paris, France; 7Memorial Sloan-Kettering Cancer Center, New York, USA.
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18873" ["VALUE"]=> array(2) { ["TEXT"]=> string(2204) "<p class="bodytext">The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].<br />We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.<br />This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).<br /><br /> <h3>Keywords </h3> <p>anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child </p> <p class="bodytext">© 1989 Massachusetts Medical Society. All rights reserved.<br />Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931 </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2112) "The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].
We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.
This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).
Keywords
anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child
© 1989 Massachusetts Medical Society. All rights reserved.
Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931
Eliane Gluckman1, Hal E. Broxmeyer2, Arleen D. Auerbach3, Henry S. Friedman4, Gordon W. Douglas5, Agnes Devergie1, Helene Esperou1, Dominique Thierry6, Gerard Socie1, Pierre Lehn1, Scott Cooper2, Denis English2, Joanne Kurtzberg4, Judith Bard7, and Edward A. Boyse7
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(675) "Eliane Gluckman1, Hal E. Broxmeyer2, Arleen D. Auerbach3, Henry S. Friedman4, Gordon W. Douglas5, Agnes Devergie1, Helene Esperou1, Dominique Thierry6, Gerard Socie1, Pierre Lehn1, Scott Cooper2, Denis English2, Joanne Kurtzberg4, Judith Bard7, and Edward A. Boyse7
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18873" ["VALUE"]=> array(2) { ["TEXT"]=> string(2204) "<p class="bodytext">The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].<br />We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.<br />This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).<br /><br /> <h3>Keywords </h3> <p>anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child </p> <p class="bodytext">© 1989 Massachusetts Medical Society. All rights reserved.<br />Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931 </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2112) "The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].
We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.
This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).
Keywords
anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child
© 1989 Massachusetts Medical Society. All rights reserved.
Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931
The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].
We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.
This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).
Keywords
anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child
© 1989 Massachusetts Medical Society. All rights reserved.
Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931
1Bone Marrow Transplant Unit, Hôpital Saint-Louis, Paris, France; 2Departments of Medicine (Hematology/Oncology), Microbiology and Immunology, Pathology, and the Walther Oncology Center, Indiana University School of Medicine, Indianapolis, USA; 3Laboratory for Investigative Dermatology, Rockefeller University, New York, USA; 4Department of Pediatrics (Hematology/Oncology), Duke University Medical Center, Durham, N.C., USA; 5Department of Obstetrics and Gynecology, New York University Medical Center, New York, USA; 6Central Nuclear Agency, Paris, France; 7Memorial Sloan-Kettering Cancer Center, New York, USA.
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(720) "1Bone Marrow Transplant Unit, Hôpital Saint-Louis, Paris, France; 2Departments of Medicine (Hematology/Oncology), Microbiology and Immunology, Pathology, and the Walther Oncology Center, Indiana University School of Medicine, Indianapolis, USA; 3Laboratory for Investigative Dermatology, Rockefeller University, New York, USA; 4Department of Pediatrics (Hematology/Oncology), Duke University Medical Center, Durham, N.C., USA; 5Department of Obstetrics and Gynecology, New York University Medical Center, New York, USA; 6Central Nuclear Agency, Paris, France; 7Memorial Sloan-Kettering Cancer Center, New York, USA.
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(15) { [0]=> string(5) "18890" [1]=> string(5) "18891" [2]=> string(5) "18892" [3]=> string(5) "18893" [4]=> string(5) "18894" [5]=> string(5) "18895" [6]=> string(5) "18896" [7]=> string(5) "18897" [8]=> string(5) "18898" [9]=> string(5) "18899" [10]=> string(5) "18900" [11]=> string(5) "18901" [12]=> string(5) "18902" [13]=> string(5) "18903" [14]=> string(5) "18904" } ["VALUE"]=> array(15) { [0]=> string(4) "1407" [1]=> string(4) "1408" [2]=> string(4) "1409" [3]=> string(4) "1410" [4]=> string(4) "1411" [5]=> string(4) "1412" [6]=> string(4) "1413" [7]=> string(4) "1414" [8]=> string(4) "1415" [9]=> string(4) "1416" [10]=> string(4) "1417" [11]=> string(4) "1418" [12]=> string(4) "1419" [13]=> string(4) "1420" [14]=> string(4) "1421" } ["DESCRIPTION"]=> array(15) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" [7]=> string(0) "" [8]=> string(0) "" [9]=> string(0) "" [10]=> string(0) "" [11]=> string(0) "" [12]=> string(0) "" [13]=> string(0) "" [14]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(15) { [0]=> string(4) "1407" [1]=> string(4) "1408" [2]=> string(4) "1409" [3]=> string(4) "1410" [4]=> string(4) "1411" [5]=> string(4) "1412" [6]=> string(4) "1413" [7]=> string(4) "1414" [8]=> string(4) "1415" [9]=> string(4) "1416" [10]=> string(4) "1417" [11]=> string(4) "1418" [12]=> string(4) "1419" [13]=> string(4) "1420" [14]=> string(4) "1421" } ["~DESCRIPTION"]=> array(15) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" [3]=> string(0) "" [4]=> string(0) "" [5]=> string(0) "" [6]=> string(0) "" [7]=> string(0) "" [8]=> string(0) "" [9]=> string(0) "" [10]=> string(0) "" [11]=> string(0) "" [12]=> string(0) "" [13]=> string(0) "" [14]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(15) { [0]=> string(59) "Eliane Gluckman" [1]=> string(60) "Hal E. Broxmeyer" [2]=> string(62) "Arleen D. Auerbach" [3]=> string(61) "Henry S. Friedman" [4]=> string(61) "Gordon W. Douglas" [5]=> string(58) "Agnes Devergie" [6]=> string(58) "Helene Esperou" [7]=> string(61) "Dominique Thierry" [8]=> string(56) "Gerard Socie" [9]=> string(55) "Pierre Lehn" [10]=> string(56) "Scott Cooper" [11]=> string(57) "Denis English" [12]=> string(60) "Joanne Kurtzberg" [13]=> string(55) "Judith Bard" [14]=> string(59) "Edward A. Boyse" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18837" ["VALUE"]=> array(2) { ["TEXT"]=> string(416) "<p>Элиана Глюкман, Хэл Е. Броксмайер, Арлин Д. Ауэрбах, Генри С. Фридман, Гордон У. Дуглас, Агнес Девержи, Элен Эсперо, Доминик Тьерри, Жерар Соси, Пьер Лен, Скотт Купер, Денис Инглиш, Джоан Кюртцберг, Юдифь Бард, Эдвард А. Бойз</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(404) "Элиана Глюкман, Хэл Е. Броксмайер, Арлин Д. Ауэрбах, Генри С. Фридман, Гордон У. Дуглас, Агнес Девержи, Элен Эсперо, Доминик Тьерри, Жерар Соси, Пьер Лен, Скотт Купер, Денис Инглиш, Джоан Кюртцберг, Юдифь Бард, Эдвард А. Бойз
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(404) "Элиана Глюкман, Хэл Е. Броксмайер, Арлин Д. Ауэрбах, Генри С. Фридман, Гордон У. Дуглас, Агнес Девержи, Элен Эсперо, Доминик Тьерри, Жерар Соси, Пьер Лен, Скотт Купер, Денис Инглиш, Джоан Кюртцберг, Юдифь Бард, Эдвард А. Бойз
" } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18838" ["VALUE"]=> array(2) { ["TEXT"]=> string(3833) "<p class="bodytext">Клинические проявления анемии Фанкони, аутосомной рецессивной болезни, включают прогрессирующую панцитопению, предрасположенность к злокачественным опухолям и развитию аномалий, не связанных с гемопоэзом. Гиперчувствительность к кластогенным эффектам – разрывам хромосом под действием препаратов, способствующих сшивке цепей ДНК, таких как диэпоксибутан, используется как диагностический признак генотипа анемии Фанкони, как пре- так и постнатально. Пренатальное <br>HLA-типирование даёт возможность установить, является ли плод HLA-идентичным больному сиблингу. <br /><br />Мы описываем здесь восстановление гемопоэза у мальчика с тяжёлой формой анемии Фанкони, которому была введена криоконсервированная пуповинная кровь сестры, не поражённой, по данным пренатального тестирования, данным заболеванием, имевшей нормальный кариотип и HLA-идентичный фенотип. <br /><br />Мы использовали претрансплантационный режим кондиционирования, разработанный специально для таких больных; метод основан на гиперчувствительности аномальных клеток к алкилирующим агентам, вызывающих сшивки цепей ДНК, и воздействию радиации. Метод позволяет использовать пуповинную кровь и избежать забора клеток костного мозга у новорожденного сиблинга. Такое применение пуповинной крови вытекало из предположения одного из нас о том, что кровь, взятая из пуповинной вены при рождении и обычно не используемая, может восстанавливать гемопоэз – предположении, основанном на наших предварительных исследованиях, согласующихся с сообщениями о наличии гемопоэтических стволовых и мультипотентных (CFU-GEMM), эритроидных (BFU-E) и гранулоцитарно-макрофагальных (CFU-GM) клеток-предшественников в пуповинной крови человека (см. ссылки в работе Broxmeyer et al.).<br /><br /> <h3>Ключевые слова</h3> <p> анемия, апластическая терапия, консервация крови, анемия Фанкони, женская особь, плодная кровь, HLA антигены, трансплантация гемопоэтических стволовых клеток, тестирование гистосовместимости, человек, мужская особь, беременность, пренатальный диагноз, дети дошкольного возраста </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3751) "Клинические проявления анемии Фанкони, аутосомной рецессивной болезни, включают прогрессирующую панцитопению, предрасположенность к злокачественным опухолям и развитию аномалий, не связанных с гемопоэзом. Гиперчувствительность к кластогенным эффектам – разрывам хромосом под действием препаратов, способствующих сшивке цепей ДНК, таких как диэпоксибутан, используется как диагностический признак генотипа анемии Фанкони, как пре- так и постнатально. Пренатальное
HLA-типирование даёт возможность установить, является ли плод HLA-идентичным больному сиблингу.
Мы описываем здесь восстановление гемопоэза у мальчика с тяжёлой формой анемии Фанкони, которому была введена криоконсервированная пуповинная кровь сестры, не поражённой, по данным пренатального тестирования, данным заболеванием, имевшей нормальный кариотип и HLA-идентичный фенотип.
Мы использовали претрансплантационный режим кондиционирования, разработанный специально для таких больных; метод основан на гиперчувствительности аномальных клеток к алкилирующим агентам, вызывающих сшивки цепей ДНК, и воздействию радиации. Метод позволяет использовать пуповинную кровь и избежать забора клеток костного мозга у новорожденного сиблинга. Такое применение пуповинной крови вытекало из предположения одного из нас о том, что кровь, взятая из пуповинной вены при рождении и обычно не используемая, может восстанавливать гемопоэз – предположении, основанном на наших предварительных исследованиях, согласующихся с сообщениями о наличии гемопоэтических стволовых и мультипотентных (CFU-GEMM), эритроидных (BFU-E) и гранулоцитарно-макрофагальных (CFU-GM) клеток-предшественников в пуповинной крови человека (см. ссылки в работе Broxmeyer et al.).
Ключевые слова
анемия, апластическая терапия, консервация крови, анемия Фанкони, женская особь, плодная кровь, HLA антигены, трансплантация гемопоэтических стволовых клеток, тестирование гистосовместимости, человек, мужская особь, беременность, пренатальный диагноз, дети дошкольного возраста
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(3751) "Клинические проявления анемии Фанкони, аутосомной рецессивной болезни, включают прогрессирующую панцитопению, предрасположенность к злокачественным опухолям и развитию аномалий, не связанных с гемопоэзом. Гиперчувствительность к кластогенным эффектам – разрывам хромосом под действием препаратов, способствующих сшивке цепей ДНК, таких как диэпоксибутан, используется как диагностический признак генотипа анемии Фанкони, как пре- так и постнатально. Пренатальное
HLA-типирование даёт возможность установить, является ли плод HLA-идентичным больному сиблингу.
Мы описываем здесь восстановление гемопоэза у мальчика с тяжёлой формой анемии Фанкони, которому была введена криоконсервированная пуповинная кровь сестры, не поражённой, по данным пренатального тестирования, данным заболеванием, имевшей нормальный кариотип и HLA-идентичный фенотип.
Мы использовали претрансплантационный режим кондиционирования, разработанный специально для таких больных; метод основан на гиперчувствительности аномальных клеток к алкилирующим агентам, вызывающих сшивки цепей ДНК, и воздействию радиации. Метод позволяет использовать пуповинную кровь и избежать забора клеток костного мозга у новорожденного сиблинга. Такое применение пуповинной крови вытекало из предположения одного из нас о том, что кровь, взятая из пуповинной вены при рождении и обычно не используемая, может восстанавливать гемопоэз – предположении, основанном на наших предварительных исследованиях, согласующихся с сообщениями о наличии гемопоэтических стволовых и мультипотентных (CFU-GEMM), эритроидных (BFU-E) и гранулоцитарно-макрофагальных (CFU-GM) клеток-предшественников в пуповинной крови человека (см. ссылки в работе Broxmeyer et al.).
Ключевые слова
анемия, апластическая терапия, консервация крови, анемия Фанкони, женская особь, плодная кровь, HLA антигены, трансплантация гемопоэтических стволовых клеток, тестирование гистосовместимости, человек, мужская особь, беременность, пренатальный диагноз, дети дошкольного возраста
" } } } [1]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "80" ["~IBLOCK_SECTION_ID"]=> string(2) "80" ["ID"]=> string(4) "1433" ["~ID"]=> string(4) "1433" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["~NAME"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "09/29/2017 02:41:24 pm" ["~TIMESTAMP_X"]=> string(22) "09/29/2017 02:41:24 pm" ["DETAIL_PAGE_URL"]=> string(111) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii/" ["~DETAIL_PAGE_URL"]=> string(111) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(28952) "Introduction
The distribution of thalassemia used to be confined to areas from the Mediterranean across the Middle East through Southern Asia to Southeast Asia: the so-called thalassemia belt [1]. At present, migration of people has spread thalassemia throughout the world. Furthermore, with the improvement of medical care, including developing countries, thalassemic children can now survive the early months of life and live long enough to require treatment. Thalassemia is, therefore, now considered to be a global health problem [2].
In Thailand, both α- and β-thalassemias as well as Hb E and Hb Constant Spring are prevalent [3]. There are more than 60 clinical syndromes resulting from various gene interactions, giving 12,000 annual births of thalassemic children. Among them, the common severe thalassemic syndromes with which patients can survive are homozygous β-thalassemia or thalassemia major, and Hb E/β-thalassemia. Hb E/β-thalassemia is the most common severe clinical syndrome in adults and is found more frequently than homozygous β-thalassemia in Thailand [4]. This syndrome is unique to Southeast Asia in general and to Thailand in particular. Clinical manifestations of this syndrome are heterogeneous: at one end, symptoms may be as severe as with thalassemia major, at the other end, patients may have only mild anemia [4]. However, those who show symptoms related to anemia during the first year of life usually have severe manifestations later on.
Therapy of severe thalassemia with regular hypertransfusion and iron chelation has dramatically improved life expectancy [5, 6], but there remain many problems related to quality of life, compliance, and expense. Hematopoietic stem cell transplantation is at present the only modality with the potential to cure thalassemia [7]. The objective of allogeneic transplantation for thalassemia is to replace thalassemic hematopoiesis by normal hematopoiesis through allogeneic stem cell transplantation. Patients require “conditioning” to eradicate thalassemic stem cells and to overcome the immunological barriers (histoincompatibility and transfusion-associated allosensitization).
Bone marrow transplantation from HLA-identical siblings in children with thalassemia
The first successful treatment of thalassemia with bone marrow transplantation from HLA-identical sibling donors was performed in 1981 in Seattle [8]. Most subsequent experience, however, has been reported by the Pesaro group [9-14], and other case series have been presented [15-23]. Most transplants for thalassemia have employed bone marrow from unaffected HLA-identical sibling donors. However, only 25–30% of patients have an HLA-matched sibling donor.
By using conditioning with busulfan, 14 mg/kg given over 4 days, followed by cyclophosphamide, 200 mg/kg over the next 4 days, the Pesaro group reported successful bone marrow transplantation in large numbers of children and identified three risk factors, which predicted outcome after transplantation [9]. These risk factors include hepatomegaly of more than 2 cm, liver histology showing portal fibrosis, and irregular (and therefore ineffective) iron chelation. On that basis patients can be classified into three risk categories: class 1 without any risk factors, class 2 with one or two risk factors, and class 3 with all risk factors.
Results in class 1 and 2 patients
The majority of transplants were performed in children in the class 1 and 2 risk groups using bone marrow from HLA-identical siblings. Overall survival was 87–90% and thalassemia-free survival 85–87% [9, 11, 15-23]. The incidence of graft rejection and transplant-related mortality was 3% and 10–13%, respectively. On the basis of these recommendations, children with severe thalassemia should undergo bone marrow transplantation if they have HLA-identical siblings, as early in life as possible.
Class 3 patients
By using busulfan at 14 mg/kg and cyclophosphamide at 200 mg/kg as conditioning, the Pesaro group reported lower overall survival (61%), thalassemia-free survival (53%) and higher transplant-related mortality (47%) [12] than that observed in class 1 and 2 patients. Conditioning comprising busulfan 14 mg/kg and lower dose of cyclophosphamide (160 or 120 mg/kg) improved the overall survival to 80%; however, the graft rejection rate was increased to 33%, giving a thalassemia-free survival of 56% [12]. This conditioning regimen is, therefore, inadequate to eradicate the marrow erythroid hyperplasia related to the disease.
A new preparative regimen was developed by the Pesaro group in an attempt to eradicate more effectively thalassemic marrow erythropoiesis [14]. This protocol comprises intensified preparation with hydroxyurea 30 mg/kg and azathioprine 3 mg/kg daily on day -45 to day -11, followed by fludarabine 20 mg/m^2/day from day -17 to day 11, and busulfan at, 14 mg/kg and cyclophosphamide at 160 mg/kg . With this approach overall survival, thalassemia-free survival, graft rejection and transplant-related mortality were 93%, 85%, 8% and 6%, respectively. Thus, the use of this regimen has improved outcome in class 3 patients to the level observed in class 1 and class 2 patients conditioned with a less intensive regimen.
Transplantation in adult patients
Early trials from the Pesaro group showed unfavorable results in adult patients, who typically had more advanced disease with marked erythroid expansion and therapy-related organ complications. With conditioning regimens comprising busulfan 14 mg/kg and cyclophosphamide 200 mg/kg in class 2, and busulfan 14–16 mg/kg and cyclophosphamide 120–160 mg/kg in class 3 patients, the overall survival, thalassemia-free survival, rejection, and transplant-related mortality were 66%, 62%, 4%, and 37%, respectively.
By using a new preparative regimen similar to that used for children with class 3 risk (cyclophosphamide dose lowered to 90 mg/kg), the overall survival, thalassemia-free survival, rejection, and transplant-related mortality were 65%, 65%, 7%, and 28%, respectively [14]. Thus, this strategy has improved transplant results in adult patients with thalassemia; however, transplant-related mortality is still significant.
Bone marrow transplantation for thalassemia in Thailand
The first successful bone marrow transplant for thalassemia in Thailand was performed in 1988 at Siriraj Hospital, Mahidol University. Subsequently, transplant programs were also developed at Ramathibodi and Chulalongkorn hospitals. By 2008, 241 patients with thalassemia had undergone bone marrow transplantation in Thailand. Of these, 48 (22%) had homozygous β-thalassemia, and 155 (72%) had severe Hb E/β-thalassemia. Patients with Hb E/β-thalassemia with anemic symptoms for the first time during the first year of life are considered to have severe disease and should undergo bone marrow transplantation if they have HLA-identical siblings. Only a few patients received hypertransfusion and iron chelation. The results showed that overall survival and thalassemia-free survival in class 1 and 2 children were 89% and 80%, respectively. However, results in class 3 children were unfavorable. By using modified conditioning with busulfan 600 mg/m2 and cyclophosphamide 200 mg/kg, outcome was improved to 90% overall survival, and 85% thalassemia-free survival [15].
Cord blood transplantation from related donors
We reported the first successful use of cord blood from an unaffected younger sibling to transplant a child with Hb E/β-thalassemia [24]. The use of cord blood circumvents the need for a donor bone marrow harvest, is associated with a lower incidence of GvHD, and allows for prompt transplantation. So far, 14 patients have undergone cord blood transplantation for thalassemia at our institution. Three patients had homozygous β-thalassemia, and 11 had Hb E/β-thalassemia. Patients were 1 to 8 (a median of 4) years old, 8 were males and 6 were females. One patient died early, and one patient failed to engraft. Twelve patients had documented engraftment, and 10 of them are surviving thalassemia-free. Two patients, both in risk class 3, rejected their grafts. Based on our experience from a single institution, we recommend that sibling cord blood transplantation should be performed only in children with class 1 or 2, not in advanced disease. An adequate cell dose of cord blood is important to guarantee success.
Data from Eurocord show a high survival rate (100%) and thalassemia-free survival of 89% for class 1, and 62% for class 2 patients [25]; however, graft rejection was high (21%), presumably reflecting the importance of cell dose, although cell dose did not predict engraftment. Graft rejection was decreased when thiotepa was added to the conditioning regimen, and when methotrexate was omitted from GvHD prophylaxis.
Transplants from donors other than HLA- identical siblings
Only 25–30% of patients have an unaffected HLA-identical sibling donor. The remaining patients may receive stem cells from alternative donors including matched unrelated donors, unrelated cord blood, and haploidentical donors. However, it should be emphasized that thalassemia is not a malignant disease, and although bone marrow transplantation can cure the disease, patients can live a long time with a satisfactory quality of life with hypertransfusion and iron chelation, and without transplantation. Transplants from donors other than HLA-identical siblings should be considered only when patients and their parents fully understand the potential risks and benefits and are motivated to perform transplantation.
Marrow transplantation from HLA-matched unrelated donors
The outcome of matched unrelated donor transplantation has improved substantially, primarily due to more refined histocompatibility typing and selection of donors on the basis of matching at the molecular level. Earlier reports using conditioning with busulfan and cyclophosphamide with or without thiotepa showed thalassemia-free survival of 66%, graft rejection of 12%, and transplant-related mortality of 19% [26]. Favorable results were also obtained in adult patients with overall survival, thalassemia-free survival, graft rejection, and transplant-related mortality of 70%, 70%, 4%, and 30%, respectively [27].
A recent report from Thailand confirms this data, showing overall survival, thalassemia-free survival, graft rejection, and transplant related mortality of 82%, 71%, 13%, and 18% respectively [28]. By 2008, 53 patients had undergone matched unrelated bone marrow transplantation (40 “full” HLA matches, 13 1 or 2 antigen mismatches) in Thailand. Of these 53 patients, 28 were in class 1, 24 in class 2, and 5 in class 3. Overall survival was 87%, and thalassemia-free survival, 80%. Thus, HLA-matched unrelated donor transplantation is an excellent option and may have success rates superior to those achieved with cord blood.
Unrelated cord blood transplantation
Unrelated cord blood transplantation is increasingly used to treat hematological malignancies [29]. The advantages of using cord blood are as follows: faster availability, acceptability of partial HLA mismatching, and low incidence of GvHD; however, engraftment is usually delayed. Recent data from 14 transplant centers showed encouraging results with overall survival and thalassemic-free survival of 77%, and 65%, respectively [30]. Results were better when transplants were performed at experienced centers (overall survival 87% and thalassemia-free survival 77%).
To overcome the cell dose barrier some centers have begun to use two partially HLA-matched cord blood units for transplantation [31].
Transplantation from haploidentical donors
Almost all patients have haploidentical donors. A recent report described a successful use of T-cell depleted CD34+ peripheral blood and bone marrow cells from haploidentical mothers in children with thalassemia [32]. However, the methodology to purify CD34+ cells and deplete T cells is sophisticated and expensive.
Graft failure and graft rejection
Graft failure and rejection is more common after transplant for thalassemia, especially in poor-risk patients, than it is in other diseases. Failure of primary engraftment with persistent aplasia is rare and has a poor prognosis, because second transplants following second course of conditioning yield poor results (overall survival 49%, thalassemia-free survival 33%) [33]. Most patients with graft rejection show autologous recovery of thalassemic hematopoiesis resulting in recurrence of the disease. Graft rejection most often occurs within the first 6 months after transplantation [34], therefore monthly determination of chimerism is recommended for the first 6 months as patients with residual detectable host cells are likely to develop graft rejection [35]. If the proportion of donor cells is declining, withdrawal of immunosuppressive drugs may allow for enhancement of donor hematopoiesis [36].
Mixed chimerism was found in one third of thalassemia patients at 2 months after transplantation. The risks of graft rejection was nearly 100%, 41%, and 13% when residual host cells accounted for more than 25%, 10–25%, and less than 10% of all cells, respectively [35]. None of the patients with complete chimerism at 2 months rejected the graft [35].
A cohort of 295 patients who underwent transplantation showed that at 2 months 95 (33%) had mixed chimerism. At 24 months 42 had become complete chimeras, 33 progressed to rejection, and 20 had persistent mixed chimerism of 30–90% donor cells [34]. These results indicated that engrafted donor cells, as evidenced by stable mixed chimerism, are adequate to cure the disease phenotype once donor-host tolerance has been established. Therefore, complete eradication of donor hematopoiesis may not be necessary for cure.
Reduced intensity conditioning and transplantation for thalassemia
The findings that stable mixed chimerism is sufficient to suppress thalassemic hematopoiesis, have provided the rationale for using reduced intensity conditioning in thalassemic patients. Such an approach can reduce the conditioning-related toxicity, especially in patients with advanced disease. Early results using reduced intensity conditioning were disappointing [37-40]. A more recent report describes the use of busulfan, 8–12 mg/kg, fludarabine, 175–210 mg/m2, antilymphocyte globulin 20–40 mg/kg with or without thiotepa, and total lymphoid irradiation for conditioning, and cyclosporine or tacrolimus and mycophenolate mofetil for GvHD prophylaxis in 8 patients with class 3 disease [41]. Initial engraftment was observed in all patients, although two patients lost donor chimerism later on. Further studies are needed.
Conclusions
Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 disease, if adequate numbers of cord blood cells from younger siblings are available.
Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed only in motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.
Acknowledgement
Dr. Issaragrisil is a Senior Research Scholar of Thailand Research Fund (grant no. RTA 488-0007) and also supported by Commission on Higher Education (grant no. CHE-RES-RG-49).
References
1. Chernoff AI. The distribution of the thalassemia gene. A historical review. Blood. 1959;14:899.
2. Weatherall DJ. Thalassemia in the next millennium. Ann NY Acad Sci. 1998;850:1-9. pmid: 9668522.
3. Wasi P. Haemoglobinopathies including thalassemia. Part 1. Tropical Asia. Clin Haematol. 1981;10:702-29. pmid: 7030550.
4. Fucharoen S, Winichagoon P. Clinical and hematologic aspects of hemoglobin E β-thalassemia. Cur Opin Hematol. 2000;7:106-12. pmid: 10698297.
5. Borgna-Pignatti C, Rugolotto S, di Stefano P, et al. Survival and complications in patients with thalassemia major treated with transfusion and defroxamine. Hematologica. 2004;89:1187-93.
7. Lucarelli G, Gaziev J. Advances in the allogeneic transplantation for thalassemia. Blood Rev. 2008;22:53-63. doi:10.1016/j.blre.2007.10.001.
8. Thomas ED, Buckner CD, Sanders J, et al. Marrow transplantation for thalassemia. Lancet. 1982;ii:227-9. pmid: 6124668.
9. Lucarelli G, Galimberti M, Polchi P, et al. Bone marrow transplantation in patients with thalassemia. N Engl j Med. 1990;322:417-21. pmid: 2300104.
14. Gaziev J, Sodani P, Polchi P, Andreant M, Lucarelli G. Bone marrow transplantation in adults with thalassemia. Treatment and long-term follow-up. Ann NY Acad Sci. 2005;1054:196-205.
15. Issaragrisil S, Suvatte V, Visuthisakchai S, et al. Bone marrow and cord blood stem cell transplantation for thalassemia in Thailand. Bone Marrow Transplant. 1997;19(2):54-6.
16. Lin HP, Chan LL, Lam SK, Ariffin W, Menaka N, Looi LM. Bone marrow transplantation for thalassemia. The experience from Malaysia. Bone Marrow Transplant. 1997;19(2):74-7.
17. Dennison D, Srivastava A, Chandy M. Bone Marrow transplantation for thalassemia in India. Bone Marrow Transplant. 1997;19(2):70.
18. Ghavamzadeh A, Bahar B, Djahani M, Kokabandeh A, Shahriari A. Bone marrow transplantation of thalassemia, the experience in Tehran (Iran). Bone Marrow Transplant. 1997;19(2):71-3.
19. Clift RA, Johnson FL. Marrow transplants for thalassemia. The USA experience. Bone Marrow Transplant. 1997;19(2):57-9.
20. Argiolu F, Sanna MA, Cossu F, et al. Bone marrow transplant in thalassemia. The experience of Cagliari. Bone Marrow Transplant. 1997;19(2):65-7.
21. Li CK, Shing MK, Chik KW, Lee V, Leung TF, Cheung PMP, Yuen PMP. Hematopoietic stem cell transplantation for thalassemia major in Hong Kong: prognostic factors and outcome. Bone Marrow Transplant. 2002;29:101-5.
22. Lawson SE, Roberts IAG, Amrolia P, Dokal I, Szydio R, Darbyshire PJ. Bone marrow transplantation for β-thalassemia major: the UK experience in two paediatric centers. Brit J Hematol. 2003;120:289-95.
23. Di Bartolomeo P, Santarone S, Di Bartolomeo, et al. Long-term results of bone marrow transplantation for thalassemia major in Pescara. Blood. 2004;104:3332.
30. Jaing T-H, Tan P, Rosenthal J, et al. Unrelated cord blood transplantation (CBT) for thalassemia. Blood. 2006;108:11.
33. Gaziev D, Polchi P, Lucarelli G et al. Second bone marrow for graft failure in patients with thalassemia. Bone Marrow Transplant. 1999;24:1299-1306.
34. Nesci S, Manna M, Lucarelli G, et al. Mixed chimerism after bone marrow transplantation in thalassemia. Ann NY Acad Sci. 1998;850:495-7. pmid: 9668594.
36. Zakrzewaki JL. Successful management of impending graft failure in a thalassemic bone marrow transplant recipient. Hematologica. 2002;87:ECR32. pmid: 12368175.
39. Jacobsohn DA, Duerst R, Tse W, Kletzel M. Reduced intensity haematopoietic stem cell transplantation for treatment of non-malignant disease children. Lancet. 2004;364:156-62. pmid: 15246728.
40. Krishnamurti L, Wu CJ, Baker S, Wagner J. Stable donor engraftment following reduced intensity hematopoietic cell transplantation for sickle disease. Biol Blood Marrow Transplant. 2006;12:39.
" ["~DETAIL_TEXT"]=> string(28952) "Introduction
The distribution of thalassemia used to be confined to areas from the Mediterranean across the Middle East through Southern Asia to Southeast Asia: the so-called thalassemia belt [1]. At present, migration of people has spread thalassemia throughout the world. Furthermore, with the improvement of medical care, including developing countries, thalassemic children can now survive the early months of life and live long enough to require treatment. Thalassemia is, therefore, now considered to be a global health problem [2].
In Thailand, both α- and β-thalassemias as well as Hb E and Hb Constant Spring are prevalent [3]. There are more than 60 clinical syndromes resulting from various gene interactions, giving 12,000 annual births of thalassemic children. Among them, the common severe thalassemic syndromes with which patients can survive are homozygous β-thalassemia or thalassemia major, and Hb E/β-thalassemia. Hb E/β-thalassemia is the most common severe clinical syndrome in adults and is found more frequently than homozygous β-thalassemia in Thailand [4]. This syndrome is unique to Southeast Asia in general and to Thailand in particular. Clinical manifestations of this syndrome are heterogeneous: at one end, symptoms may be as severe as with thalassemia major, at the other end, patients may have only mild anemia [4]. However, those who show symptoms related to anemia during the first year of life usually have severe manifestations later on.
Therapy of severe thalassemia with regular hypertransfusion and iron chelation has dramatically improved life expectancy [5, 6], but there remain many problems related to quality of life, compliance, and expense. Hematopoietic stem cell transplantation is at present the only modality with the potential to cure thalassemia [7]. The objective of allogeneic transplantation for thalassemia is to replace thalassemic hematopoiesis by normal hematopoiesis through allogeneic stem cell transplantation. Patients require “conditioning” to eradicate thalassemic stem cells and to overcome the immunological barriers (histoincompatibility and transfusion-associated allosensitization).
Bone marrow transplantation from HLA-identical siblings in children with thalassemia
The first successful treatment of thalassemia with bone marrow transplantation from HLA-identical sibling donors was performed in 1981 in Seattle [8]. Most subsequent experience, however, has been reported by the Pesaro group [9-14], and other case series have been presented [15-23]. Most transplants for thalassemia have employed bone marrow from unaffected HLA-identical sibling donors. However, only 25–30% of patients have an HLA-matched sibling donor.
By using conditioning with busulfan, 14 mg/kg given over 4 days, followed by cyclophosphamide, 200 mg/kg over the next 4 days, the Pesaro group reported successful bone marrow transplantation in large numbers of children and identified three risk factors, which predicted outcome after transplantation [9]. These risk factors include hepatomegaly of more than 2 cm, liver histology showing portal fibrosis, and irregular (and therefore ineffective) iron chelation. On that basis patients can be classified into three risk categories: class 1 without any risk factors, class 2 with one or two risk factors, and class 3 with all risk factors.
Results in class 1 and 2 patients
The majority of transplants were performed in children in the class 1 and 2 risk groups using bone marrow from HLA-identical siblings. Overall survival was 87–90% and thalassemia-free survival 85–87% [9, 11, 15-23]. The incidence of graft rejection and transplant-related mortality was 3% and 10–13%, respectively. On the basis of these recommendations, children with severe thalassemia should undergo bone marrow transplantation if they have HLA-identical siblings, as early in life as possible.
Class 3 patients
By using busulfan at 14 mg/kg and cyclophosphamide at 200 mg/kg as conditioning, the Pesaro group reported lower overall survival (61%), thalassemia-free survival (53%) and higher transplant-related mortality (47%) [12] than that observed in class 1 and 2 patients. Conditioning comprising busulfan 14 mg/kg and lower dose of cyclophosphamide (160 or 120 mg/kg) improved the overall survival to 80%; however, the graft rejection rate was increased to 33%, giving a thalassemia-free survival of 56% [12]. This conditioning regimen is, therefore, inadequate to eradicate the marrow erythroid hyperplasia related to the disease.
A new preparative regimen was developed by the Pesaro group in an attempt to eradicate more effectively thalassemic marrow erythropoiesis [14]. This protocol comprises intensified preparation with hydroxyurea 30 mg/kg and azathioprine 3 mg/kg daily on day -45 to day -11, followed by fludarabine 20 mg/m^2/day from day -17 to day 11, and busulfan at, 14 mg/kg and cyclophosphamide at 160 mg/kg . With this approach overall survival, thalassemia-free survival, graft rejection and transplant-related mortality were 93%, 85%, 8% and 6%, respectively. Thus, the use of this regimen has improved outcome in class 3 patients to the level observed in class 1 and class 2 patients conditioned with a less intensive regimen.
Transplantation in adult patients
Early trials from the Pesaro group showed unfavorable results in adult patients, who typically had more advanced disease with marked erythroid expansion and therapy-related organ complications. With conditioning regimens comprising busulfan 14 mg/kg and cyclophosphamide 200 mg/kg in class 2, and busulfan 14–16 mg/kg and cyclophosphamide 120–160 mg/kg in class 3 patients, the overall survival, thalassemia-free survival, rejection, and transplant-related mortality were 66%, 62%, 4%, and 37%, respectively.
By using a new preparative regimen similar to that used for children with class 3 risk (cyclophosphamide dose lowered to 90 mg/kg), the overall survival, thalassemia-free survival, rejection, and transplant-related mortality were 65%, 65%, 7%, and 28%, respectively [14]. Thus, this strategy has improved transplant results in adult patients with thalassemia; however, transplant-related mortality is still significant.
Bone marrow transplantation for thalassemia in Thailand
The first successful bone marrow transplant for thalassemia in Thailand was performed in 1988 at Siriraj Hospital, Mahidol University. Subsequently, transplant programs were also developed at Ramathibodi and Chulalongkorn hospitals. By 2008, 241 patients with thalassemia had undergone bone marrow transplantation in Thailand. Of these, 48 (22%) had homozygous β-thalassemia, and 155 (72%) had severe Hb E/β-thalassemia. Patients with Hb E/β-thalassemia with anemic symptoms for the first time during the first year of life are considered to have severe disease and should undergo bone marrow transplantation if they have HLA-identical siblings. Only a few patients received hypertransfusion and iron chelation. The results showed that overall survival and thalassemia-free survival in class 1 and 2 children were 89% and 80%, respectively. However, results in class 3 children were unfavorable. By using modified conditioning with busulfan 600 mg/m2 and cyclophosphamide 200 mg/kg, outcome was improved to 90% overall survival, and 85% thalassemia-free survival [15].
Cord blood transplantation from related donors
We reported the first successful use of cord blood from an unaffected younger sibling to transplant a child with Hb E/β-thalassemia [24]. The use of cord blood circumvents the need for a donor bone marrow harvest, is associated with a lower incidence of GvHD, and allows for prompt transplantation. So far, 14 patients have undergone cord blood transplantation for thalassemia at our institution. Three patients had homozygous β-thalassemia, and 11 had Hb E/β-thalassemia. Patients were 1 to 8 (a median of 4) years old, 8 were males and 6 were females. One patient died early, and one patient failed to engraft. Twelve patients had documented engraftment, and 10 of them are surviving thalassemia-free. Two patients, both in risk class 3, rejected their grafts. Based on our experience from a single institution, we recommend that sibling cord blood transplantation should be performed only in children with class 1 or 2, not in advanced disease. An adequate cell dose of cord blood is important to guarantee success.
Data from Eurocord show a high survival rate (100%) and thalassemia-free survival of 89% for class 1, and 62% for class 2 patients [25]; however, graft rejection was high (21%), presumably reflecting the importance of cell dose, although cell dose did not predict engraftment. Graft rejection was decreased when thiotepa was added to the conditioning regimen, and when methotrexate was omitted from GvHD prophylaxis.
Transplants from donors other than HLA- identical siblings
Only 25–30% of patients have an unaffected HLA-identical sibling donor. The remaining patients may receive stem cells from alternative donors including matched unrelated donors, unrelated cord blood, and haploidentical donors. However, it should be emphasized that thalassemia is not a malignant disease, and although bone marrow transplantation can cure the disease, patients can live a long time with a satisfactory quality of life with hypertransfusion and iron chelation, and without transplantation. Transplants from donors other than HLA-identical siblings should be considered only when patients and their parents fully understand the potential risks and benefits and are motivated to perform transplantation.
Marrow transplantation from HLA-matched unrelated donors
The outcome of matched unrelated donor transplantation has improved substantially, primarily due to more refined histocompatibility typing and selection of donors on the basis of matching at the molecular level. Earlier reports using conditioning with busulfan and cyclophosphamide with or without thiotepa showed thalassemia-free survival of 66%, graft rejection of 12%, and transplant-related mortality of 19% [26]. Favorable results were also obtained in adult patients with overall survival, thalassemia-free survival, graft rejection, and transplant-related mortality of 70%, 70%, 4%, and 30%, respectively [27].
A recent report from Thailand confirms this data, showing overall survival, thalassemia-free survival, graft rejection, and transplant related mortality of 82%, 71%, 13%, and 18% respectively [28]. By 2008, 53 patients had undergone matched unrelated bone marrow transplantation (40 “full” HLA matches, 13 1 or 2 antigen mismatches) in Thailand. Of these 53 patients, 28 were in class 1, 24 in class 2, and 5 in class 3. Overall survival was 87%, and thalassemia-free survival, 80%. Thus, HLA-matched unrelated donor transplantation is an excellent option and may have success rates superior to those achieved with cord blood.
Unrelated cord blood transplantation
Unrelated cord blood transplantation is increasingly used to treat hematological malignancies [29]. The advantages of using cord blood are as follows: faster availability, acceptability of partial HLA mismatching, and low incidence of GvHD; however, engraftment is usually delayed. Recent data from 14 transplant centers showed encouraging results with overall survival and thalassemic-free survival of 77%, and 65%, respectively [30]. Results were better when transplants were performed at experienced centers (overall survival 87% and thalassemia-free survival 77%).
To overcome the cell dose barrier some centers have begun to use two partially HLA-matched cord blood units for transplantation [31].
Transplantation from haploidentical donors
Almost all patients have haploidentical donors. A recent report described a successful use of T-cell depleted CD34+ peripheral blood and bone marrow cells from haploidentical mothers in children with thalassemia [32]. However, the methodology to purify CD34+ cells and deplete T cells is sophisticated and expensive.
Graft failure and graft rejection
Graft failure and rejection is more common after transplant for thalassemia, especially in poor-risk patients, than it is in other diseases. Failure of primary engraftment with persistent aplasia is rare and has a poor prognosis, because second transplants following second course of conditioning yield poor results (overall survival 49%, thalassemia-free survival 33%) [33]. Most patients with graft rejection show autologous recovery of thalassemic hematopoiesis resulting in recurrence of the disease. Graft rejection most often occurs within the first 6 months after transplantation [34], therefore monthly determination of chimerism is recommended for the first 6 months as patients with residual detectable host cells are likely to develop graft rejection [35]. If the proportion of donor cells is declining, withdrawal of immunosuppressive drugs may allow for enhancement of donor hematopoiesis [36].
Mixed chimerism was found in one third of thalassemia patients at 2 months after transplantation. The risks of graft rejection was nearly 100%, 41%, and 13% when residual host cells accounted for more than 25%, 10–25%, and less than 10% of all cells, respectively [35]. None of the patients with complete chimerism at 2 months rejected the graft [35].
A cohort of 295 patients who underwent transplantation showed that at 2 months 95 (33%) had mixed chimerism. At 24 months 42 had become complete chimeras, 33 progressed to rejection, and 20 had persistent mixed chimerism of 30–90% donor cells [34]. These results indicated that engrafted donor cells, as evidenced by stable mixed chimerism, are adequate to cure the disease phenotype once donor-host tolerance has been established. Therefore, complete eradication of donor hematopoiesis may not be necessary for cure.
Reduced intensity conditioning and transplantation for thalassemia
The findings that stable mixed chimerism is sufficient to suppress thalassemic hematopoiesis, have provided the rationale for using reduced intensity conditioning in thalassemic patients. Such an approach can reduce the conditioning-related toxicity, especially in patients with advanced disease. Early results using reduced intensity conditioning were disappointing [37-40]. A more recent report describes the use of busulfan, 8–12 mg/kg, fludarabine, 175–210 mg/m2, antilymphocyte globulin 20–40 mg/kg with or without thiotepa, and total lymphoid irradiation for conditioning, and cyclosporine or tacrolimus and mycophenolate mofetil for GvHD prophylaxis in 8 patients with class 3 disease [41]. Initial engraftment was observed in all patients, although two patients lost donor chimerism later on. Further studies are needed.
Conclusions
Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 disease, if adequate numbers of cord blood cells from younger siblings are available.
Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed only in motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.
Acknowledgement
Dr. Issaragrisil is a Senior Research Scholar of Thailand Research Fund (grant no. RTA 488-0007) and also supported by Commission on Higher Education (grant no. CHE-RES-RG-49).
References
1. Chernoff AI. The distribution of the thalassemia gene. A historical review. Blood. 1959;14:899.
2. Weatherall DJ. Thalassemia in the next millennium. Ann NY Acad Sci. 1998;850:1-9. pmid: 9668522.
3. Wasi P. Haemoglobinopathies including thalassemia. Part 1. Tropical Asia. Clin Haematol. 1981;10:702-29. pmid: 7030550.
4. Fucharoen S, Winichagoon P. Clinical and hematologic aspects of hemoglobin E β-thalassemia. Cur Opin Hematol. 2000;7:106-12. pmid: 10698297.
5. Borgna-Pignatti C, Rugolotto S, di Stefano P, et al. Survival and complications in patients with thalassemia major treated with transfusion and defroxamine. Hematologica. 2004;89:1187-93.
7. Lucarelli G, Gaziev J. Advances in the allogeneic transplantation for thalassemia. Blood Rev. 2008;22:53-63. doi:10.1016/j.blre.2007.10.001.
8. Thomas ED, Buckner CD, Sanders J, et al. Marrow transplantation for thalassemia. Lancet. 1982;ii:227-9. pmid: 6124668.
9. Lucarelli G, Galimberti M, Polchi P, et al. Bone marrow transplantation in patients with thalassemia. N Engl j Med. 1990;322:417-21. pmid: 2300104.
14. Gaziev J, Sodani P, Polchi P, Andreant M, Lucarelli G. Bone marrow transplantation in adults with thalassemia. Treatment and long-term follow-up. Ann NY Acad Sci. 2005;1054:196-205.
15. Issaragrisil S, Suvatte V, Visuthisakchai S, et al. Bone marrow and cord blood stem cell transplantation for thalassemia in Thailand. Bone Marrow Transplant. 1997;19(2):54-6.
16. Lin HP, Chan LL, Lam SK, Ariffin W, Menaka N, Looi LM. Bone marrow transplantation for thalassemia. The experience from Malaysia. Bone Marrow Transplant. 1997;19(2):74-7.
17. Dennison D, Srivastava A, Chandy M. Bone Marrow transplantation for thalassemia in India. Bone Marrow Transplant. 1997;19(2):70.
18. Ghavamzadeh A, Bahar B, Djahani M, Kokabandeh A, Shahriari A. Bone marrow transplantation of thalassemia, the experience in Tehran (Iran). Bone Marrow Transplant. 1997;19(2):71-3.
19. Clift RA, Johnson FL. Marrow transplants for thalassemia. The USA experience. Bone Marrow Transplant. 1997;19(2):57-9.
20. Argiolu F, Sanna MA, Cossu F, et al. Bone marrow transplant in thalassemia. The experience of Cagliari. Bone Marrow Transplant. 1997;19(2):65-7.
21. Li CK, Shing MK, Chik KW, Lee V, Leung TF, Cheung PMP, Yuen PMP. Hematopoietic stem cell transplantation for thalassemia major in Hong Kong: prognostic factors and outcome. Bone Marrow Transplant. 2002;29:101-5.
22. Lawson SE, Roberts IAG, Amrolia P, Dokal I, Szydio R, Darbyshire PJ. Bone marrow transplantation for β-thalassemia major: the UK experience in two paediatric centers. Brit J Hematol. 2003;120:289-95.
23. Di Bartolomeo P, Santarone S, Di Bartolomeo, et al. Long-term results of bone marrow transplantation for thalassemia major in Pescara. Blood. 2004;104:3332.
30. Jaing T-H, Tan P, Rosenthal J, et al. Unrelated cord blood transplantation (CBT) for thalassemia. Blood. 2006;108:11.
33. Gaziev D, Polchi P, Lucarelli G et al. Second bone marrow for graft failure in patients with thalassemia. Bone Marrow Transplant. 1999;24:1299-1306.
34. Nesci S, Manna M, Lucarelli G, et al. Mixed chimerism after bone marrow transplantation in thalassemia. Ann NY Acad Sci. 1998;850:495-7. pmid: 9668594.
36. Zakrzewaki JL. Successful management of impending graft failure in a thalassemic bone marrow transplant recipient. Hematologica. 2002;87:ECR32. pmid: 12368175.
39. Jacobsohn DA, Duerst R, Tse W, Kletzel M. Reduced intensity haematopoietic stem cell transplantation for treatment of non-malignant disease children. Lancet. 2004;364:156-62. pmid: 15246728.
40. Krishnamurti L, Wu CJ, Baker S, Wagner J. Stable donor engraftment following reduced intensity hematopoietic cell transplantation for sickle disease. Biol Blood Marrow Transplant. 2006;12:39.
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "500" ["~SORT"]=> string(3) "500" ["CODE"]=> string(67) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii" ["~CODE"]=> string(67) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii" ["EXTERNAL_ID"]=> string(4) "1433" ["~EXTERNAL_ID"]=> string(4) "1433" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["ELEMENT_META_KEYWORDS"]=> string(0) "" ["ELEMENT_META_DESCRIPTION"]=> string(174) "Трансплантация гемопоэтических стволовых клеток при талассемииHematopoietic stem cell transplantation for thalassemia" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(2688) "<p class="bodytext"> Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов. <br> <br> Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов. </p> <h3>Ключевые слова</h3> <p> талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества </p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_META_TITLE"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_META_KEYWORDS"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_META_DESCRIPTION"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_PICTURE_FILE_ALT"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_PICTURE_FILE_TITLE"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_PICTURE_FILE_NAME"]=> string(71) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii-img" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(119) "Трансплантация гемопоэтических стволовых клеток при талассемии" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(71) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii-img" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(71) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii-img" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(71) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-talassemii-img" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(2) "80" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> bool(false) ["VALUE"]=> bool(false) ["DESCRIPTION"]=> bool(false) ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> bool(false) ["~DESCRIPTION"]=> bool(false) ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19023" ["VALUE"]=> string(22) "01/04/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/04/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19024" ["VALUE"]=> string(22) "01/15/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/15/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19025" ["VALUE"]=> string(22) "11/17/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "11/17/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19026" ["VALUE"]=> string(4) "1432" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1432" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19040" } ["VALUE"]=> array(1) { [0]=> string(4) "1432" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1432" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19028" ["VALUE"]=> array(2) { ["TEXT"]=> string(59) " <p>Сурапол Иссарагризил</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(47) "Сурапол Иссарагризил
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19039" ["VALUE"]=> array(2) { ["TEXT"]=> string(2688) "<p class="bodytext"> Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов. <br> <br> Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов. </p> <h3>Ключевые слова</h3> <p> талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2630) "
Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов.
Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов.
Ключевые слова
талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19030" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000070.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000070.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19034" ["VALUE"]=> array(2) { ["TEXT"]=> string(39) "<p>Surapol Issaragrisil</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(27) "Surapol Issaragrisil
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19035" ["VALUE"]=> array(2) { ["TEXT"]=> string(153) "<p>Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(141) "Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19036" ["VALUE"]=> array(2) { ["TEXT"]=> string(1281) "<p class="bodytext">Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.<br /><br />Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.</p><h3>Keywords</h3> <p> thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1223) "Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.
Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.
Keywords
thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19031" ["VALUE"]=> string(55) "Hematopoietic stem cell transplantation for thalassemia" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(55) "Hematopoietic stem cell transplantation for thalassemia" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19032" ["VALUE"]=> string(3) "918" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "918" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19037" ["VALUE"]=> string(3) "919" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "919" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(12) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19034" ["VALUE"]=> array(2) { ["TEXT"]=> string(39) "<p>Surapol Issaragrisil</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(27) "Surapol Issaragrisil
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(27) "Surapol Issaragrisil
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19036" ["VALUE"]=> array(2) { ["TEXT"]=> string(1281) "<p class="bodytext">Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.<br /><br />Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.</p><h3>Keywords</h3> <p> thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1223) "Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.
Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.
Keywords
thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1223) "Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.
Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.
Keywords
thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19030" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000070.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000070.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2010-en-000070.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19031" ["VALUE"]=> string(55) "Hematopoietic stem cell transplantation for thalassemia" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(55) "Hematopoietic stem cell transplantation for thalassemia" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(55) "Hematopoietic stem cell transplantation for thalassemia" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19035" ["VALUE"]=> array(2) { ["TEXT"]=> string(153) "<p>Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(141) "Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(141) "Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19040" } ["VALUE"]=> array(1) { [0]=> string(4) "1432" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1432" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(64) "Surapol Issaragrisil" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19028" ["VALUE"]=> array(2) { ["TEXT"]=> string(59) " <p>Сурапол Иссарагризил</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(47) "Сурапол Иссарагризил
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(47) "Сурапол Иссарагризил
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19023" ["VALUE"]=> string(22) "01/04/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/04/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/04/2010 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19024" ["VALUE"]=> string(22) "01/15/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/15/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/15/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19025" ["VALUE"]=> string(22) "11/17/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "11/17/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "11/17/2010 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19026" ["VALUE"]=> string(4) "1432" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1432" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(64) "Surapol Issaragrisil" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19039" ["VALUE"]=> array(2) { ["TEXT"]=> string(2688) "<p class="bodytext"> Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов. <br> <br> Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов. </p> <h3>Ключевые слова</h3> <p> талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(2630) "
Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов.
Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов.
Ключевые слова
талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(2630) "
Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов.
Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов.
Ключевые слова
талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества
" } } } [2]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "80" ["~IBLOCK_SECTION_ID"]=> string(2) "80" ["ID"]=> string(4) "1428" ["~ID"]=> string(4) "1428" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["~NAME"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "09/27/2017 07:27:35 pm" ["~TIMESTAMP_X"]=> string(22) "09/27/2017 07:27:35 pm" ["DETAIL_PAGE_URL"]=> string(133) "/en/archive/tom-2-nomer-3-7/obzornye-stati/rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok/" ["~DETAIL_PAGE_URL"]=> string(133) "/en/archive/tom-2-nomer-3-7/obzornye-stati/rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(44832) "Early studies
Some of the most compelling evidence for the absolute requirement of a competent microenvironment (ME) to support engraftment comes from early studies in mutant mice. In particular, unequivocal studies show that both the SL/SL, or “Steel” mutant mouse which dies of anemia spontaneously, and the more viable SL/SLd mouse, which succumbs following very low doses of irradiation, cannot be rescued with an infusion of normal bone marrow cells [<38]. However, the animals could be rescued by transplantation of intact spleen tissue, which becomes the site of hematopoiesis [29]. These studies not only established the importance of the ME for stem cell engraftment, but also advanced the concept that at least some components of the ME cannot be transplanted by an intra-venous infusion of aspirated marrow cells. More recently the mutated gene product that gives rise to the Steel phenotype was shown to be kit ligand, also known as “stem cell factor” (SCF) expressed by stromal cells [12, 19].
Early seminal work by Wolf and Trentin illustrated that the ME is also critical for inducing lineage commitment. In these experiments, a section of bone with intact marrow was implanted within the spleen of a mouse prior to irradiation. After stem cell transplantation, the resulting spleen colonies that bridged the two different MEs were mixed such that there was mostly erythroid differentiation on the splenic side while myeloid differentiation predominated on the marrow side [51].
Although these early studies highlighted the important role of the ME in normal hematopoiesis, identifying the cells and secreted products that are involved in this process remains unfinished work. Specifically, the components that can support the expansion of stem cells without loss of their potential have not been defined. This may be due in part to the fact that more than one cell type and gene product participate in this regulation. In addition, even though the hematopoietic system is a liquid tissue, some ME components appear to be "fixed" stromal elements that contribute to the architecture and may have critical spatial relationships with each other that are difficult to reproduce in vitro.
For several decades in vitro studies of the ME have relied heavily on the Dexter long term culture (LTC) in which many cell types are evident [13]. LTC that are established from aspirated marrow and cultured under appropriate conditions will generate in 2-4 weeks an adherent layer that supports hematopoiesis for several months. Figure 1 shows an example of an LTC.
Figure1. Dexter Long-Term Culture (LTC): Panel A depicts a schematic representation of a typical LTC. A complex adherent layer composed of fibroblasts, endothelium, adipocytes, and macrophages which supports the production of hematopoietic cells. As hematopoietic cells mature, they are released from the adherent layer into the media. Panel B depicts a phase-contrast photomicrograph of a typical human LTC.
The adherent stromal layer in the LTC consists of fibroblasts, endothelial cells, macrophages, adipocytes, osteoclasts, and extracellular matrix. LTC, if done properly, appear to approximate the in vivo ME since the functional ramifications of the Steel defect are apparent in cultures established from SL/SLd marrow [14]. However there are limitations to this system as myeloid cell production is generally favored over erythroid, and the ever-increasing proportion of monocyte-derived macrophages, is eventually associated with the termination of cell production [10].
Stromal component of the ME
There has been considerable debate concerning the origin of the ME stromal cells. Many reports have suggested that hematopoietic cells and stromal cells have a common precursor, and in agreement with this, several reports have claimed that stromal fibroblasts as well as hematopoietic cells are replaced by donor cells after hematopoietic stem cell transplantation [23, 43]. However, many of these studies typically looked at LTC established from sex mismatched transplants and detected donor cells using standard cytogenetics or fluorescent in-situ hybridization (FISH) for sex chromatin [23]. While it is clear that adherent cells of donor origin were detected in these LTC, these reports were flawed, as they did not properly account for the macrophage component of the adherent layer. This is an important consideration, since studies have shown that even after weekly passage of adherent cells, macrophages can represent a significant proportion of the cells in a 12 week LTC (see Table 1) [5].
Table 1: Percentage of NSE + cells in LTC of normal donors
|
Weeks in culture |
||||||
|
2wk |
4wk |
6wk |
8wk |
10wk |
12wk |
|
|
Donor |
||||||
|
1 |
15.5 |
17.7 |
44.0 |
28.0 |
23.0 |
8.2 |
|
2 |
13.9 |
24.9 |
17.4 |
5.8 |
2.1 |
1.9 |
|
3 |
32.8 |
22.3 |
29.6 |
31.7 |
29.5 |
22.0 |
|
4 |
25.1 |
21.4 |
27.6 |
41.1 |
16.5 |
3.3 |
|
NSE=nonspecific esterase; LTC=long term culture |
||||||
Using histochemistry to identify and exclude the donor-derived macrophage component, our lab has determined that even after decades following successful stem cell transplantation, with 100% donor-derived hematopoietic cells, the stromal cells detected in an LTC from a transplanted patient remain of host origin, as predicted by the Steel mouse [5, 42].
The stromal component of the ME remains relatively constant and is quite resistant to currently used conditioning regimens. Therefore, after transplantation, the ME as a whole becomes chimeric; the stromal fibroblasts and endothelial cells remain host-derived while the macrophages are donor-derived [42, 48]. There are several possible explanations for this: First, unlike hematopoietic cells, the stromal fibroblasts and endothelial cells that are harvested from marrow and detectable in the transplanted product are not equipped with the surface molecules needed for trans-migrating the endothelium and homing to the ME. Pre-clinical animal studies suggest that when stromal cells are infused intravenously, they get trapped primarily in the lung and spleen (M. Mielcarek, personal communication). Second, because stromal cells are relatively resistant to chemotherapy and irradiation, the stromal cell compartment is not depleted by standard conditioning; as a result there may not be a demand for stromal cell replacement.
ME niches
After conditioning, the resident stromal cells express or secrete molecules that attract hematopoietic stem and progenitor cells, provide cell surface receptors which allow for the attachment of these cells, and secrete activities for the induction and support of various cell fates. Recently there has been considerable interest in identifying the specific cellular components that make up the stem cell niche, the specific ME unit where the hematopoietic stem cell resides and self-renews. Over the past two decades, the mouse model has been used to identify various chemokines, cell surface adhesion molecules, and cell types that contribute to this niche. There is general agreement that a number of signaling pathways including c-kit/SCF, CXCR4/CXCL12, VCAM1/VLA-4, Tie2/angipoietin, c-mpl/thrombopoietin, notch/jagged-1, and osteopontin play important roles in maintaining the stem cell niche [6, 30, 3, 16, 22, 32, 4, 27, 31, 44, 25, 35, 52, 9]. However, there is less agreement on the exact identity of the cells that make up the stem cell niche.
Compelling evidence from mouse studies suggest that the endosteal region is critical for the maintenance of hematopoietic stem and precursor cells. One prevalent model proposes that stem cell maintenance critically depends on N-cadherin-mediated binding to osteoblasts [9, 53]. This “osteoblastic niche” model was based on experiments which showed that N-cadherin-positive cells in the endosteal region are associated with cells expressing stem cell markers [9] . However, there are also reports that ablation of osteoblasts does not result in an immediate loss of stem cells, suggesting that while the stem cells may be spatially associated with osteoblasts, the osteoblasts may not be playing a significant role in their support [50, 54]. Furthermore, a recent study demonstrated that only CD146-positive mesenchymal progenitors and not osteoblasts can transfer a ME when transplanted into immunodeficient mice [39] .
Another equally compelling model proposes that hematopoietic stem cells localize close to marrow sinusoids. Evidence for this “endothelial niche” comes from experiments where cells expressing the SLAM family of surface receptors, which are highly expressed in hematopoietic stem cells, were detected in close association with vascular endothelium [24] . A third study suggested that reticular cells that express high levels of CXCL12/SDF1 (CAR cells) essentially define the stem cell niche, and these cells could be detected in both the perivascular and endosteal regions [45] .
The macrophage component of the ME
It is obvious that in vivo, stromal cells do not function in isolation, but do so in the context of other cells. One cell type that is clearly conspicuous both in vivo and in vitro (see Figure 2) is the monocyte-derived macrophage [34, 33].
Figure 2. Panel A shows a normal human bone marrow biopsy stained with macrophage-specific CD68 antibody. Panel B depicts a marrow LTC from an inducible transgenic mouse where GFP is under the control of the human CD68 promoter and is expressed exclusively in macrophages. As illustrated in the photomicrographs, CD68 positive macrophages have a significant presence in the marrow and have numerous cell processes which interact with many cell types, suggesting a crucial role in the regulation of hematopoiesis.
In vivo, monocytes are recruited from the circulation into tissues, where they can differentiate into macrophages and perform functions that are relevant to that particular tissue ME. It has long been known that macrophages play a critical role in hematopoiesis. Bessis first described the “nurse cell”, a specialized macrophage that is an important component of the erythroblast island, thought to provide structure and nutrients to developing erythroid cells [7, 11]. Osteoclasts, another specialized type of monocyte-derived macrophages, are critical in Ca+ homeostasis in the bone, which is also important for the maintenance of hematopoietic stem cells [1]. However, there is little known or even speculated about the role macrophages may play in the stem cell niche.
Available data suggest that stromal cells play a direct role in the stem cell niche by influencing cell fate decisions through the expression of proteins, such as SDF1 and Jagged, which bind progenitor surface determinants CXCR4 and Notch, respectively. While SDF1 facilitates homing and retention of cells in the marrow, Jagged transduces a signal through Notch that renders early progenitors resistant to differentiation signals [30, 3, 27, 9]. However, since the stromal cell compartment appears constant, with little turnover, it is unclear how interactions between stroma and stem cells can be modulated to allow for the dynamic range of cell production that is characteristic of hematopoiesis. In particular, the mechanisms that regulate gene expression in stromal cells have not been well defined. However, in theory the influence of a constant level of a stroma-expressed genes, e.g. Jagged, could be modulated to some extent indirectly, by down-regulating the level of its receptor, Notch, expressed by progenitors. In vitro studies using cloned human stromal cell lines suggest that this may occur.
Recent data from our laboratory indicates that functionally distinct stromal cell lines isolated from the same LTC can induce different gene expression profiles in monocytes. Specifically, the cloned stromal cell line HS27a, which expresses a number of genes associated with the stem cell niche including CXCL12, angiopoietin, Jagged 1, VCAM, induces the secretion of osteopontin by monocytes [37, 15, 20]. The osteopontin in turn down-regulates Notch expression on progenitors. It is reasonable to conclude that the reduced expression of Notch on progenitors can limit Jagged-Notch signaling, thereby making the progenitors more responsive to differentiation signals [20]. Interestingly, we also showed that the second functionally distinct stromal line, designated HS5, secretes activities that increase the production of matrix metalloproteinase 9 (MMP9) by monocytes, which would facilitate egress of the newly matured cells [21]. Since monocytes circulate and can be recruited from the blood, changes in their number and gene expression within an ME could significantly modulate stromal function.
ME and disease
Since stroma-monocyte interactions likely participate at many levels in the regulation of hematopoiesis, it would be reasonable to conclude that abnormal monocytes may contribute to the pathophysiology of hematologic malignancies. One example that we reported shows that monocytes from patients with myelodysplastic syndrome (MDS) fail to respond appropriately to stromal signals [21]. Specifically, clonally derived monocytes from patients with MDS fail to upregulate MMP-9 gene expression in response to stromal signals (see Figure 3).
Figure 3. Combined Immunohistochemistry for MMP-9 and FISH for chromosome 7. Monocytes from a healthy donor and from an MDS patient with monosomy seven were isolated and exposed to stromal signals. Cytospins were prepared and IHC for MMP-9 and FISH for chromosome 7 were performed. Panel A depicts monocytes from a healthy control which upregulate MMP-9 expression in response to stromal signals (green cytoplasmic staining) and have two copies of chromosome 7 detected by FISH (see white arrows). Panel B depicts clonal MDS monocytes identified by monosomy 7 which fail to upregulate MMP-9 expression in response to stromal signals.
The potential clinical relevance of this finding was suggested by a significant negative correlation between the proportion of abnormal monocytes and degree of marrow cellularity [21]. Given the role of MMP-9 in facilitating the egress of cells from marrow, it is reasonable to conclude that as the proportion of non-responsive monocytes increases, inducible levels of MMP-9 decline, resulting in hypercellularity. We also determined that the stromal signal from HS5 that induced MMP-9 is most likely MCP-1; however, we have not as yet identified the compromised monocyte signaling pathway that fails to respond [21]. Clearly a better delineation of signaling pathways that are responsible for normal responses between stromal cells and monocytes as well as the activities that trigger these pathways are needed.
These data suggest that macrophages can play a significant role in altering the hematopoietic ME to support the malignant/dysplastic process. This has clear implications for the success of hematopoietic stem cell transplantation, especially with the introduction of reduced intensity and so-called non-myeloablative conditioning regimens. Most of these conditioning regimens are of insufficient intensity to eliminate residual clonal host macrophages. Thus, when allogeneic stem cells are infused, they encounter a ME that remains dysregulated. This may explain the high rates of graft rejection and relapse seen in MDS patients after reduced intensity and non-myeloablative transplantation [21, 2, 28, 40, 26].
Finally, appreciating the critical role that monocyte-derived macrophages may play in the hematopoietic ME sheds new light on the “seed versus soil” debate as to the cause of hematopoietic dysplasias and aplasias, as well as graft failures. Clearly, the ME (soil) may appear abnormal, yet the defect may reside in the hematopoietic stem cell (seed)- derived monocyte, which upon entering the ME, fails to respond appropriately to stromal signals and thereby contributes to abnormal ME function. This would explain why “defective” MEs appear to be corrected by transplantation; the transplant is actually replacing the abnormal monocytes, not the stromal cells. This is not to suggest that primary stromal failures do not exist. Two examples of such failures have been observed following transplantation: one involves CMV infection and destruction of stromal cells [41, 47, 36, 46, 8], the other involves GVH-mediated anti-stroma activities [49, 18, 17]. In both cases the recipients could not be rescued by the infusion of additional stem cells, even after the anti-stroma mechanism had been eliminated.
Summary
Over the past several decades, studies have revealed the hematopoietic ME to be a complex tissue that consists of both hematopoietic and non-hematopoietic cells, extra-cellular matrix, as well as soluble and membrane bound factors, all of which act in concert to support normal hematopoiesis.
• The ME consists of both hematopoietic stem cell derived and non-hematopoietic cells.
• A viable host ME is required for successful stem cell transplantation.
• Graft failure ensues when the ME is damaged/destroyed.
• After transplantation, the ME becomes chimeric. The stromal elements of the ME remain host-derived, whereas the monocyte/macrophage component is replaced by donor cells.
• Distinct niches or “ME units” exist that are responsible for the regulation of stem cell quiescence as well as differentiation.
• The hematopoietic stem cell derived monocyte/macrophage is a critical component of the ME.
• Stromal cells activate monocytes to assume different fates, which subsequently secrete activities that regulate hematopoiesis.
• In hematologic malignancies, clonally derived monocytes contribute to the dysregulation of the ME.
Data from our lab suggest that monocyte-derived macrophages play a significant role within the ME, and that abnormal monocytes derived from a clone of malignant hematopoietic cells, can compromise ME function. Importantly, following reduced intensity conditioning, recipient macrophages can be retained, and the dysregulated ME can persist and fail to support engraftment. Clearly, further investigation is necessary to completely understand how stroma and monocytes interact to regulate normal hematopoiesis, and how these pathways are altered by abnormal cells. As our knowledge increases we will be able to develop strategies to identify and correct abnormal signaling within the ME.
Acknowledgements
This work was supported in part by PHS grants DK082783, HL099993, DK056465 from the National Institutes of Health. We thank Bonnie Larson, Helen Crawford and Sue Carbonneau for assistance with the preparation and editing of the manuscript. The authors indicate no potential conflict of interest.
References
1. Adams, G. B., K. T. Chabner, I. R. Alley, D. P. Olson, Z. M. Szczepiorkowski, M. C. Poznansky, C. H. Kos, M. R. Pollak, E. M. Brown, and D. T. Scadden. 2006. Stem cell engraftment at the endosteal niche is specified by the calcium-sensing receptor. Nature 439, (7076) (Feb 2): 599-603.
5. Awaya, N., K. Rupert, E. Bryant, and B. Torok-Storb. 2002. Failure of adult marrow-derived stem cells to generate marrow stroma after successful hematopoietic stem cell transplantation. Experimental Hematology 30, (8) (Aug): 937-42.
6. Barker, J. E. 1994. Sl/Sld hematopoietic progenitors are deficient in situ. Experimental Hematology 22, (2) (Feb): 174-7.
7. Bessis, M. 1958. Erythroblastic island, functional unity of bone marrow. Revue d'Hematologie 13, (1) (Jan-Mar): 8-11.
8. Boeckh, M., C. Hoy, and B. Torok-Storb. 1998. Occult cytomegalovirus infection of marrow stroma. Clinical Infectious Diseases : An Official Publication of the Infectious Diseases Society of America 26, (1) (Jan): 209-10.
10. Chabannon, C., and B. Torok-Storb. 1992. Stem cell-stromal cell interactions. Current Topics in Microbiology and Immunology 177, : 123-36.
12. Copeland, N. G., D. J. Gilbert, B. C. Cho, P. J. Donovan, N. A. Jenkins, D. Cosman, D. Anderson, S. D. Lyman, and D. E. Williams. 1990. Mast cell growth factor maps near the steel locus on mouse chromosome 10 and is deleted in a number of steel alleles. Cell 63, (1) (Oct 5): 175-83.
13. Dexter, T. M., T. D. Allen, and L. G. Lajtha. 1977. Conditions controlling the proliferation of haemopoietic stem cells in vitro. Journal of Cellular Physiology 91, (3) (Jun): 335-44.
14. Dexter, T. M., and M. A. Moore. 1977. In vitro duplication and "cure" of haemopoietic defects in genetically anaemic mice. Nature 269, (5627) (Sep 29): 412-4.
17. Hirabayashi, N. 1981. Studies on graft versus host (GvH) reactions. I. impairment of hemopoietic stroma in mice suffering from GvH disease. Experimental Hematology 9, (2) (Feb): 101-10.
18. Hows, J. M. 1991. Mechanisms of graft failure after human marrow transplantation: A review. Immunology Letters 29, (1-2) (Jul): 77-80.
19. Huang, E., K. Nocka, D. R. Beier, T. Y. Chu, J. Buck, H. W. Lahm, D. Wellner, P. Leder, and P. Besmer. 1990. The hematopoietic growth factor KL is encoded by the sl locus and is the ligand of the c-kit receptor, the gene product of the W locus. Cell 63, (1) (Oct 5): 225-33.
22. Jiang, Y., H. Bonig, T. Ulyanova, K. Chang, and T. Papayannopoulou. 2009. On the adaptation of endosteal stem cell niche function in response to stress. Blood 114, (18) (Oct 29): 3773-82.
23. Keating, A., J. W. Singer, P. D. Killen, G. E. Striker, A. C. Salo, J. Sanders, E. D. Thomas, D. Thorning, and P. J. Fialkow. 1982. Donor origin of the in vitro haematopoietic microenvironment after marrow transplantation in man. Nature 298, (5871) (Jul 15): 280-3.
30. Nagasawa, T. 2000. A chemokine, SDF-1/PBSF, and its receptor, CXC chemokine receptor 4, as mediators of hematopoiesis. International Journal of Hematology 72, (4) (Dec): 408-11.
33. Pillai, M. M., B. Hayes, and B. Torok-Storb. 2009. Inducible transgenes under the control of the hCD68 promoter identifies mouse macrophages with a distribution that differs from the F4/80 - and CSF-1R-expressing populations. Experimental Hematology 37, (12) (Dec): 1387-92.
36. Randolph-Habecker, J., M. Iwata, and B. Torok-Storb. 2002. Cytomegalovirus mediated myelosuppression. Journal of Clinical Virology : The Official Publication of the Pan American Society for Clinical Virology 25 Suppl 2, (Aug): S51-6.
38. Russell, E. S. 1979. Hereditary anemias of the mouse: A review for geneticists. Advances in Genetics 20, : 357-459.
40. Scott, B. L., B. M. Sandmaier, B. Storer, M. B. Maris, M. L. Sorror, D. G. Maloney, T. R. Chauncey, R. Storb, and H. J. Deeg. 2006. Myeloablative vs nonmyeloablative allogeneic transplantation for patients with myelodysplastic syndrome or acute myelogenous leukemia with multilineage dysplasia: A retrospective analysis. Leukemia : Official Journal of the Leukemia Society of America, Leukemia Research Fund, U.K 20, (1) (Jan): 128-35.
42. Simmons, P. J., D. Przepiorka, E. D. Thomas, and B. Torok-Storb. 1987. Host origin of marrow stromal cells following allogeneic bone marrow transplantation. Nature 328, (6129) (Jul 30-Aug 5): 429-32.
43. Singer, J. W., A. Keating, J. Cuttner, A. M. Gown, R. Jacobson, P. D. Killen, J. W. Moohr, V. Najfeld, J. Powell, and J. Sanders. 1984. Evidence for a stem cell common to hematopoiesis and its in vitro microenvironment: Studies of patients with clonal hematopoietic neoplasia. Leukemia Research 8, (4): 535-45.
48. Torok-Storb, B., and L. Holmberg. 1994. Role of marrow microenvironment in engraftment and maintenance of allogeneic hematopoietic stem cells. Bone Marrow Transplantation 14 Suppl 4, : S71-3.
49. Torok-Storb, B., P. Simmons, and D. Przepiorka. 1987. Impairment of hemopoiesis in human allografts. Transplantation Proceedings 19, (6 Suppl 7) (Dec): 33-7.
" ["~DETAIL_TEXT"]=> string(44832) "Early studies
Some of the most compelling evidence for the absolute requirement of a competent microenvironment (ME) to support engraftment comes from early studies in mutant mice. In particular, unequivocal studies show that both the SL/SL, or “Steel” mutant mouse which dies of anemia spontaneously, and the more viable SL/SLd mouse, which succumbs following very low doses of irradiation, cannot be rescued with an infusion of normal bone marrow cells [<38]. However, the animals could be rescued by transplantation of intact spleen tissue, which becomes the site of hematopoiesis [29]. These studies not only established the importance of the ME for stem cell engraftment, but also advanced the concept that at least some components of the ME cannot be transplanted by an intra-venous infusion of aspirated marrow cells. More recently the mutated gene product that gives rise to the Steel phenotype was shown to be kit ligand, also known as “stem cell factor” (SCF) expressed by stromal cells [12, 19].
Early seminal work by Wolf and Trentin illustrated that the ME is also critical for inducing lineage commitment. In these experiments, a section of bone with intact marrow was implanted within the spleen of a mouse prior to irradiation. After stem cell transplantation, the resulting spleen colonies that bridged the two different MEs were mixed such that there was mostly erythroid differentiation on the splenic side while myeloid differentiation predominated on the marrow side [51].
Although these early studies highlighted the important role of the ME in normal hematopoiesis, identifying the cells and secreted products that are involved in this process remains unfinished work. Specifically, the components that can support the expansion of stem cells without loss of their potential have not been defined. This may be due in part to the fact that more than one cell type and gene product participate in this regulation. In addition, even though the hematopoietic system is a liquid tissue, some ME components appear to be "fixed" stromal elements that contribute to the architecture and may have critical spatial relationships with each other that are difficult to reproduce in vitro.
For several decades in vitro studies of the ME have relied heavily on the Dexter long term culture (LTC) in which many cell types are evident [13]. LTC that are established from aspirated marrow and cultured under appropriate conditions will generate in 2-4 weeks an adherent layer that supports hematopoiesis for several months. Figure 1 shows an example of an LTC.
Figure1. Dexter Long-Term Culture (LTC): Panel A depicts a schematic representation of a typical LTC. A complex adherent layer composed of fibroblasts, endothelium, adipocytes, and macrophages which supports the production of hematopoietic cells. As hematopoietic cells mature, they are released from the adherent layer into the media. Panel B depicts a phase-contrast photomicrograph of a typical human LTC.

The adherent stromal layer in the LTC consists of fibroblasts, endothelial cells, macrophages, adipocytes, osteoclasts, and extracellular matrix. LTC, if done properly, appear to approximate the in vivo ME since the functional ramifications of the Steel defect are apparent in cultures established from SL/SLd marrow [14]. However there are limitations to this system as myeloid cell production is generally favored over erythroid, and the ever-increasing proportion of monocyte-derived macrophages, is eventually associated with the termination of cell production [10].
Stromal component of the ME
There has been considerable debate concerning the origin of the ME stromal cells. Many reports have suggested that hematopoietic cells and stromal cells have a common precursor, and in agreement with this, several reports have claimed that stromal fibroblasts as well as hematopoietic cells are replaced by donor cells after hematopoietic stem cell transplantation [23, 43]. However, many of these studies typically looked at LTC established from sex mismatched transplants and detected donor cells using standard cytogenetics or fluorescent in-situ hybridization (FISH) for sex chromatin [23]. While it is clear that adherent cells of donor origin were detected in these LTC, these reports were flawed, as they did not properly account for the macrophage component of the adherent layer. This is an important consideration, since studies have shown that even after weekly passage of adherent cells, macrophages can represent a significant proportion of the cells in a 12 week LTC (see Table 1) [5].
Table 1: Percentage of NSE + cells in LTC of normal donors
|
Weeks in culture |
||||||
|
2wk |
4wk |
6wk |
8wk |
10wk |
12wk |
|
|
Donor |
||||||
|
1 |
15.5 |
17.7 |
44.0 |
28.0 |
23.0 |
8.2 |
|
2 |
13.9 |
24.9 |
17.4 |
5.8 |
2.1 |
1.9 |
|
3 |
32.8 |
22.3 |
29.6 |
31.7 |
29.5 |
22.0 |
|
4 |
25.1 |
21.4 |
27.6 |
41.1 |
16.5 |
3.3 |
|
NSE=nonspecific esterase; LTC=long term culture |
||||||
Using histochemistry to identify and exclude the donor-derived macrophage component, our lab has determined that even after decades following successful stem cell transplantation, with 100% donor-derived hematopoietic cells, the stromal cells detected in an LTC from a transplanted patient remain of host origin, as predicted by the Steel mouse [5, 42].
The stromal component of the ME remains relatively constant and is quite resistant to currently used conditioning regimens. Therefore, after transplantation, the ME as a whole becomes chimeric; the stromal fibroblasts and endothelial cells remain host-derived while the macrophages are donor-derived [42, 48]. There are several possible explanations for this: First, unlike hematopoietic cells, the stromal fibroblasts and endothelial cells that are harvested from marrow and detectable in the transplanted product are not equipped with the surface molecules needed for trans-migrating the endothelium and homing to the ME. Pre-clinical animal studies suggest that when stromal cells are infused intravenously, they get trapped primarily in the lung and spleen (M. Mielcarek, personal communication). Second, because stromal cells are relatively resistant to chemotherapy and irradiation, the stromal cell compartment is not depleted by standard conditioning; as a result there may not be a demand for stromal cell replacement.
ME niches
After conditioning, the resident stromal cells express or secrete molecules that attract hematopoietic stem and progenitor cells, provide cell surface receptors which allow for the attachment of these cells, and secrete activities for the induction and support of various cell fates. Recently there has been considerable interest in identifying the specific cellular components that make up the stem cell niche, the specific ME unit where the hematopoietic stem cell resides and self-renews. Over the past two decades, the mouse model has been used to identify various chemokines, cell surface adhesion molecules, and cell types that contribute to this niche. There is general agreement that a number of signaling pathways including c-kit/SCF, CXCR4/CXCL12, VCAM1/VLA-4, Tie2/angipoietin, c-mpl/thrombopoietin, notch/jagged-1, and osteopontin play important roles in maintaining the stem cell niche [6, 30, 3, 16, 22, 32, 4, 27, 31, 44, 25, 35, 52, 9]. However, there is less agreement on the exact identity of the cells that make up the stem cell niche.
Compelling evidence from mouse studies suggest that the endosteal region is critical for the maintenance of hematopoietic stem and precursor cells. One prevalent model proposes that stem cell maintenance critically depends on N-cadherin-mediated binding to osteoblasts [9, 53]. This “osteoblastic niche” model was based on experiments which showed that N-cadherin-positive cells in the endosteal region are associated with cells expressing stem cell markers [9] . However, there are also reports that ablation of osteoblasts does not result in an immediate loss of stem cells, suggesting that while the stem cells may be spatially associated with osteoblasts, the osteoblasts may not be playing a significant role in their support [50, 54]. Furthermore, a recent study demonstrated that only CD146-positive mesenchymal progenitors and not osteoblasts can transfer a ME when transplanted into immunodeficient mice [39] .
Another equally compelling model proposes that hematopoietic stem cells localize close to marrow sinusoids. Evidence for this “endothelial niche” comes from experiments where cells expressing the SLAM family of surface receptors, which are highly expressed in hematopoietic stem cells, were detected in close association with vascular endothelium [24] . A third study suggested that reticular cells that express high levels of CXCL12/SDF1 (CAR cells) essentially define the stem cell niche, and these cells could be detected in both the perivascular and endosteal regions [45] .
The macrophage component of the ME
It is obvious that in vivo, stromal cells do not function in isolation, but do so in the context of other cells. One cell type that is clearly conspicuous both in vivo and in vitro (see Figure 2) is the monocyte-derived macrophage [34, 33].
Figure 2. Panel A shows a normal human bone marrow biopsy stained with macrophage-specific CD68 antibody. Panel B depicts a marrow LTC from an inducible transgenic mouse where GFP is under the control of the human CD68 promoter and is expressed exclusively in macrophages. As illustrated in the photomicrographs, CD68 positive macrophages have a significant presence in the marrow and have numerous cell processes which interact with many cell types, suggesting a crucial role in the regulation of hematopoiesis.

In vivo, monocytes are recruited from the circulation into tissues, where they can differentiate into macrophages and perform functions that are relevant to that particular tissue ME. It has long been known that macrophages play a critical role in hematopoiesis. Bessis first described the “nurse cell”, a specialized macrophage that is an important component of the erythroblast island, thought to provide structure and nutrients to developing erythroid cells [7, 11]. Osteoclasts, another specialized type of monocyte-derived macrophages, are critical in Ca+ homeostasis in the bone, which is also important for the maintenance of hematopoietic stem cells [1]. However, there is little known or even speculated about the role macrophages may play in the stem cell niche.
Available data suggest that stromal cells play a direct role in the stem cell niche by influencing cell fate decisions through the expression of proteins, such as SDF1 and Jagged, which bind progenitor surface determinants CXCR4 and Notch, respectively. While SDF1 facilitates homing and retention of cells in the marrow, Jagged transduces a signal through Notch that renders early progenitors resistant to differentiation signals [30, 3, 27, 9]. However, since the stromal cell compartment appears constant, with little turnover, it is unclear how interactions between stroma and stem cells can be modulated to allow for the dynamic range of cell production that is characteristic of hematopoiesis. In particular, the mechanisms that regulate gene expression in stromal cells have not been well defined. However, in theory the influence of a constant level of a stroma-expressed genes, e.g. Jagged, could be modulated to some extent indirectly, by down-regulating the level of its receptor, Notch, expressed by progenitors. In vitro studies using cloned human stromal cell lines suggest that this may occur.
Recent data from our laboratory indicates that functionally distinct stromal cell lines isolated from the same LTC can induce different gene expression profiles in monocytes. Specifically, the cloned stromal cell line HS27a, which expresses a number of genes associated with the stem cell niche including CXCL12, angiopoietin, Jagged 1, VCAM, induces the secretion of osteopontin by monocytes [37, 15, 20]. The osteopontin in turn down-regulates Notch expression on progenitors. It is reasonable to conclude that the reduced expression of Notch on progenitors can limit Jagged-Notch signaling, thereby making the progenitors more responsive to differentiation signals [20]. Interestingly, we also showed that the second functionally distinct stromal line, designated HS5, secretes activities that increase the production of matrix metalloproteinase 9 (MMP9) by monocytes, which would facilitate egress of the newly matured cells [21]. Since monocytes circulate and can be recruited from the blood, changes in their number and gene expression within an ME could significantly modulate stromal function.
ME and disease
Since stroma-monocyte interactions likely participate at many levels in the regulation of hematopoiesis, it would be reasonable to conclude that abnormal monocytes may contribute to the pathophysiology of hematologic malignancies. One example that we reported shows that monocytes from patients with myelodysplastic syndrome (MDS) fail to respond appropriately to stromal signals [21]. Specifically, clonally derived monocytes from patients with MDS fail to upregulate MMP-9 gene expression in response to stromal signals (see Figure 3).
Figure 3. Combined Immunohistochemistry for MMP-9 and FISH for chromosome 7. Monocytes from a healthy donor and from an MDS patient with monosomy seven were isolated and exposed to stromal signals. Cytospins were prepared and IHC for MMP-9 and FISH for chromosome 7 were performed. Panel A depicts monocytes from a healthy control which upregulate MMP-9 expression in response to stromal signals (green cytoplasmic staining) and have two copies of chromosome 7 detected by FISH (see white arrows). Panel B depicts clonal MDS monocytes identified by monosomy 7 which fail to upregulate MMP-9 expression in response to stromal signals.

The potential clinical relevance of this finding was suggested by a significant negative correlation between the proportion of abnormal monocytes and degree of marrow cellularity [21]. Given the role of MMP-9 in facilitating the egress of cells from marrow, it is reasonable to conclude that as the proportion of non-responsive monocytes increases, inducible levels of MMP-9 decline, resulting in hypercellularity. We also determined that the stromal signal from HS5 that induced MMP-9 is most likely MCP-1; however, we have not as yet identified the compromised monocyte signaling pathway that fails to respond [21]. Clearly a better delineation of signaling pathways that are responsible for normal responses between stromal cells and monocytes as well as the activities that trigger these pathways are needed.
These data suggest that macrophages can play a significant role in altering the hematopoietic ME to support the malignant/dysplastic process. This has clear implications for the success of hematopoietic stem cell transplantation, especially with the introduction of reduced intensity and so-called non-myeloablative conditioning regimens. Most of these conditioning regimens are of insufficient intensity to eliminate residual clonal host macrophages. Thus, when allogeneic stem cells are infused, they encounter a ME that remains dysregulated. This may explain the high rates of graft rejection and relapse seen in MDS patients after reduced intensity and non-myeloablative transplantation [21, 2, 28, 40, 26].
Finally, appreciating the critical role that monocyte-derived macrophages may play in the hematopoietic ME sheds new light on the “seed versus soil” debate as to the cause of hematopoietic dysplasias and aplasias, as well as graft failures. Clearly, the ME (soil) may appear abnormal, yet the defect may reside in the hematopoietic stem cell (seed)- derived monocyte, which upon entering the ME, fails to respond appropriately to stromal signals and thereby contributes to abnormal ME function. This would explain why “defective” MEs appear to be corrected by transplantation; the transplant is actually replacing the abnormal monocytes, not the stromal cells. This is not to suggest that primary stromal failures do not exist. Two examples of such failures have been observed following transplantation: one involves CMV infection and destruction of stromal cells [41, 47, 36, 46, 8], the other involves GVH-mediated anti-stroma activities [49, 18, 17]. In both cases the recipients could not be rescued by the infusion of additional stem cells, even after the anti-stroma mechanism had been eliminated.
Summary
Over the past several decades, studies have revealed the hematopoietic ME to be a complex tissue that consists of both hematopoietic and non-hematopoietic cells, extra-cellular matrix, as well as soluble and membrane bound factors, all of which act in concert to support normal hematopoiesis.
• The ME consists of both hematopoietic stem cell derived and non-hematopoietic cells.
• A viable host ME is required for successful stem cell transplantation.
• Graft failure ensues when the ME is damaged/destroyed.
• After transplantation, the ME becomes chimeric. The stromal elements of the ME remain host-derived, whereas the monocyte/macrophage component is replaced by donor cells.
• Distinct niches or “ME units” exist that are responsible for the regulation of stem cell quiescence as well as differentiation.
• The hematopoietic stem cell derived monocyte/macrophage is a critical component of the ME.
• Stromal cells activate monocytes to assume different fates, which subsequently secrete activities that regulate hematopoiesis.
• In hematologic malignancies, clonally derived monocytes contribute to the dysregulation of the ME.
Data from our lab suggest that monocyte-derived macrophages play a significant role within the ME, and that abnormal monocytes derived from a clone of malignant hematopoietic cells, can compromise ME function. Importantly, following reduced intensity conditioning, recipient macrophages can be retained, and the dysregulated ME can persist and fail to support engraftment. Clearly, further investigation is necessary to completely understand how stroma and monocytes interact to regulate normal hematopoiesis, and how these pathways are altered by abnormal cells. As our knowledge increases we will be able to develop strategies to identify and correct abnormal signaling within the ME.
Acknowledgements
This work was supported in part by PHS grants DK082783, HL099993, DK056465 from the National Institutes of Health. We thank Bonnie Larson, Helen Crawford and Sue Carbonneau for assistance with the preparation and editing of the manuscript. The authors indicate no potential conflict of interest.
References
1. Adams, G. B., K. T. Chabner, I. R. Alley, D. P. Olson, Z. M. Szczepiorkowski, M. C. Poznansky, C. H. Kos, M. R. Pollak, E. M. Brown, and D. T. Scadden. 2006. Stem cell engraftment at the endosteal niche is specified by the calcium-sensing receptor. Nature 439, (7076) (Feb 2): 599-603.
5. Awaya, N., K. Rupert, E. Bryant, and B. Torok-Storb. 2002. Failure of adult marrow-derived stem cells to generate marrow stroma after successful hematopoietic stem cell transplantation. Experimental Hematology 30, (8) (Aug): 937-42.
6. Barker, J. E. 1994. Sl/Sld hematopoietic progenitors are deficient in situ. Experimental Hematology 22, (2) (Feb): 174-7.
7. Bessis, M. 1958. Erythroblastic island, functional unity of bone marrow. Revue d'Hematologie 13, (1) (Jan-Mar): 8-11.
8. Boeckh, M., C. Hoy, and B. Torok-Storb. 1998. Occult cytomegalovirus infection of marrow stroma. Clinical Infectious Diseases : An Official Publication of the Infectious Diseases Society of America 26, (1) (Jan): 209-10.
10. Chabannon, C., and B. Torok-Storb. 1992. Stem cell-stromal cell interactions. Current Topics in Microbiology and Immunology 177, : 123-36.
12. Copeland, N. G., D. J. Gilbert, B. C. Cho, P. J. Donovan, N. A. Jenkins, D. Cosman, D. Anderson, S. D. Lyman, and D. E. Williams. 1990. Mast cell growth factor maps near the steel locus on mouse chromosome 10 and is deleted in a number of steel alleles. Cell 63, (1) (Oct 5): 175-83.
13. Dexter, T. M., T. D. Allen, and L. G. Lajtha. 1977. Conditions controlling the proliferation of haemopoietic stem cells in vitro. Journal of Cellular Physiology 91, (3) (Jun): 335-44.
14. Dexter, T. M., and M. A. Moore. 1977. In vitro duplication and "cure" of haemopoietic defects in genetically anaemic mice. Nature 269, (5627) (Sep 29): 412-4.
17. Hirabayashi, N. 1981. Studies on graft versus host (GvH) reactions. I. impairment of hemopoietic stroma in mice suffering from GvH disease. Experimental Hematology 9, (2) (Feb): 101-10.
18. Hows, J. M. 1991. Mechanisms of graft failure after human marrow transplantation: A review. Immunology Letters 29, (1-2) (Jul): 77-80.
19. Huang, E., K. Nocka, D. R. Beier, T. Y. Chu, J. Buck, H. W. Lahm, D. Wellner, P. Leder, and P. Besmer. 1990. The hematopoietic growth factor KL is encoded by the sl locus and is the ligand of the c-kit receptor, the gene product of the W locus. Cell 63, (1) (Oct 5): 225-33.
22. Jiang, Y., H. Bonig, T. Ulyanova, K. Chang, and T. Papayannopoulou. 2009. On the adaptation of endosteal stem cell niche function in response to stress. Blood 114, (18) (Oct 29): 3773-82.
23. Keating, A., J. W. Singer, P. D. Killen, G. E. Striker, A. C. Salo, J. Sanders, E. D. Thomas, D. Thorning, and P. J. Fialkow. 1982. Donor origin of the in vitro haematopoietic microenvironment after marrow transplantation in man. Nature 298, (5871) (Jul 15): 280-3.
30. Nagasawa, T. 2000. A chemokine, SDF-1/PBSF, and its receptor, CXC chemokine receptor 4, as mediators of hematopoiesis. International Journal of Hematology 72, (4) (Dec): 408-11.
33. Pillai, M. M., B. Hayes, and B. Torok-Storb. 2009. Inducible transgenes under the control of the hCD68 promoter identifies mouse macrophages with a distribution that differs from the F4/80 - and CSF-1R-expressing populations. Experimental Hematology 37, (12) (Dec): 1387-92.
36. Randolph-Habecker, J., M. Iwata, and B. Torok-Storb. 2002. Cytomegalovirus mediated myelosuppression. Journal of Clinical Virology : The Official Publication of the Pan American Society for Clinical Virology 25 Suppl 2, (Aug): S51-6.
38. Russell, E. S. 1979. Hereditary anemias of the mouse: A review for geneticists. Advances in Genetics 20, : 357-459.
40. Scott, B. L., B. M. Sandmaier, B. Storer, M. B. Maris, M. L. Sorror, D. G. Maloney, T. R. Chauncey, R. Storb, and H. J. Deeg. 2006. Myeloablative vs nonmyeloablative allogeneic transplantation for patients with myelodysplastic syndrome or acute myelogenous leukemia with multilineage dysplasia: A retrospective analysis. Leukemia : Official Journal of the Leukemia Society of America, Leukemia Research Fund, U.K 20, (1) (Jan): 128-35.
42. Simmons, P. J., D. Przepiorka, E. D. Thomas, and B. Torok-Storb. 1987. Host origin of marrow stromal cells following allogeneic bone marrow transplantation. Nature 328, (6129) (Jul 30-Aug 5): 429-32.
43. Singer, J. W., A. Keating, J. Cuttner, A. M. Gown, R. Jacobson, P. D. Killen, J. W. Moohr, V. Najfeld, J. Powell, and J. Sanders. 1984. Evidence for a stem cell common to hematopoiesis and its in vitro microenvironment: Studies of patients with clonal hematopoietic neoplasia. Leukemia Research 8, (4): 535-45.
48. Torok-Storb, B., and L. Holmberg. 1994. Role of marrow microenvironment in engraftment and maintenance of allogeneic hematopoietic stem cells. Bone Marrow Transplantation 14 Suppl 4, : S71-3.
49. Torok-Storb, B., P. Simmons, and D. Przepiorka. 1987. Impairment of hemopoiesis in human allografts. Transplantation Proceedings 19, (6 Suppl 7) (Dec): 33-7.
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "500" ["~SORT"]=> string(3) "500" ["CODE"]=> string(89) "rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok" ["~CODE"]=> string(89) "rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok" ["EXTERNAL_ID"]=> string(4) "1428" ["~EXTERNAL_ID"]=> string(4) "1428" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["ELEMENT_META_KEYWORDS"]=> string(0) "" ["ELEMENT_META_DESCRIPTION"]=> string(242) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клетокThe role of the marrow microenvironment in hematopoietic stem cell transplantation" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(1534) "<p class="bodytext"><span lang="RU">Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.</p> <h3>Ключевые слова</h3> <p> гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг</p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_META_TITLE"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_META_KEYWORDS"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_META_DESCRIPTION"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_PICTURE_FILE_ALT"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_PICTURE_FILE_TITLE"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_PICTURE_FILE_NAME"]=> string(93) "rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-img" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(160) "Роль микроокружения костного мозга в трансплантации гемопоэтических стволовых клеток" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(93) "rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-img" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(93) "rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-img" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(93) "rol-mikrookruzheniya-kostnogo-mozga-v-transplantatsii-gemopoeticheskikh-stvolovykh-kletok-img" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(2) "80" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> bool(false) ["VALUE"]=> bool(false) ["DESCRIPTION"]=> bool(false) ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> bool(false) ["~DESCRIPTION"]=> bool(false) ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18953" ["VALUE"]=> string(22) "12/08/2009 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "12/08/2009 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18954" ["VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18955" ["VALUE"]=> string(22) "04/29/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "04/29/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18956" ["VALUE"]=> string(4) "1426" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1426" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(2) { [0]=> string(5) "18970" [1]=> string(5) "18971" } ["VALUE"]=> array(2) { [0]=> string(4) "1426" [1]=> string(4) "1427" } ["DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { [0]=> string(4) "1426" [1]=> string(4) "1427" } ["~DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18959" ["VALUE"]=> array(2) { ["TEXT"]=> string(99) "<p>Аравинд Рамакришнан, Биверли Дж.Торок-Шторб</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(87) "Аравинд Рамакришнан, Биверли Дж.Торок-Шторб
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18960" ["VALUE"]=> array(2) { ["TEXT"]=> string(1534) "<p class="bodytext"><span lang="RU">Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.</p> <h3>Ключевые слова</h3> <p> гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1472) "Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.
Ключевые слова
гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18961" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000072.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000072.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18965" ["VALUE"]=> array(2) { ["TEXT"]=> string(76) "<p>Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(64) "Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18966" ["VALUE"]=> array(2) { ["TEXT"]=> string(104) "<p>Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(92) "Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18967" ["VALUE"]=> array(2) { ["TEXT"]=> string(771) "<p class="bodytext">The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages. </p> <h3>Keywords</h3> <p> hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(725) "The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages.
Keywords
hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18962" ["VALUE"]=> string(82) "The role of the marrow microenvironment in hematopoietic stem cell transplantation" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(82) "The role of the marrow microenvironment in hematopoietic stem cell transplantation" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18968" ["VALUE"]=> string(3) "914" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "914" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18969" ["VALUE"]=> string(3) "915" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "915" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(12) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18965" ["VALUE"]=> array(2) { ["TEXT"]=> string(76) "<p>Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(64) "Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(64) "Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18967" ["VALUE"]=> array(2) { ["TEXT"]=> string(771) "<p class="bodytext">The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages. </p> <h3>Keywords</h3> <p> hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(725) "The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages.
Keywords
hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(725) "The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages.
Keywords
hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18961" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000072.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000072.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2010-en-000072.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18962" ["VALUE"]=> string(82) "The role of the marrow microenvironment in hematopoietic stem cell transplantation" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(82) "The role of the marrow microenvironment in hematopoietic stem cell transplantation" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(82) "The role of the marrow microenvironment in hematopoietic stem cell transplantation" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18966" ["VALUE"]=> array(2) { ["TEXT"]=> string(104) "<p>Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(92) "Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(92) "Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(2) { [0]=> string(5) "18970" [1]=> string(5) "18971" } ["VALUE"]=> array(2) { [0]=> string(4) "1426" [1]=> string(4) "1427" } ["DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { [0]=> string(4) "1426" [1]=> string(4) "1427" } ["~DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(2) { [0]=> string(64) "Aravind Ramakrishnan" [1]=> string(66) "Beverly J. Torok-Storb" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18959" ["VALUE"]=> array(2) { ["TEXT"]=> string(99) "<p>Аравинд Рамакришнан, Биверли Дж.Торок-Шторб</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(87) "Аравинд Рамакришнан, Биверли Дж.Торок-Шторб
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(87) "Аравинд Рамакришнан, Биверли Дж.Торок-Шторб
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18953" ["VALUE"]=> string(22) "12/08/2009 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "12/08/2009 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "12/08/2009 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18954" ["VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/25/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18955" ["VALUE"]=> string(22) "04/29/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "04/29/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "04/29/2010 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18956" ["VALUE"]=> string(4) "1426" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1426" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(64) "Aravind Ramakrishnan" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18960" ["VALUE"]=> array(2) { ["TEXT"]=> string(1534) "<p class="bodytext"><span lang="RU">Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.</p> <h3>Ключевые слова</h3> <p> гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1472) "Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.
Ключевые слова
гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1472) "Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.
Ключевые слова
гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг
" } } } [3]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "80" ["~IBLOCK_SECTION_ID"]=> string(2) "80" ["ID"]=> string(4) "1431" ["~ID"]=> string(4) "1431" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(165) "Трансплантация гемопоэтических стволовых клеток при метаболических болезнях накопления" ["~NAME"]=> string(165) "Трансплантация гемопоэтических стволовых клеток при метаболических болезнях накопления" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "09/29/2017 01:25:39 pm" ["~TIMESTAMP_X"]=> string(22) "09/29/2017 01:25:39 pm" ["DETAIL_PAGE_URL"]=> string(140) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-metabolicheskikh-boleznyakh-nakopleniya/" ["~DETAIL_PAGE_URL"]=> string(140) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-pri-metabolicheskikh-boleznyakh-nakopleniya/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(70682) "1. Introduction
Hematopoietic cell transplantation (HCT) is a prototypic stem cell therapy, and has been a life-saving measure for tens of thousands of patients. Over its relatively short history, the study of transplantation has shown that the transfer of relatively few cells can lead to the development of a fully functional lympho-hematopoietic system in the recipient, that bidirectional immunologic tolerance between post-natal tissues is possible, and that cancer can be eradicated by immunologic means.
After the seminal insight that cells with two different enzyme deficiencies can complement each other [1], a paradigm shift occurred, according to which stem cell transfer is applicable to equally fatal but non-malignant disorders [2]. This has translated into the establishment of transplantation as the standard of care for some of these enzyme disorders; monitoring of hundreds of patients with congenital metabolic disorders after transplantation has shown that long-lasting cross correction can be achieved. Conceptually, these benefits have been limited to congenital defects of enzymes, but there is no intellectual barrier to applying this strategy to other diseases where structural proteins are deficient, such as in extracellular matrix disorders.
In this review, we intend to present experiences with hematopoietic cell transplantation that have established its functionality and benefits for children with congenital metabolic storage diseases, and to describe some limitations and open questions regarding HCT for these conditions.
2. Conditioning regimens and graft sources
HCT for malignant as well as non-malignant diseases has traditionally been preceded by myeloablative doses of total body irradiation (TBI) and chemotherapy, or more commonly in the non-malignant setting, with myeloablative doses of busulfan combined with cyclophosphamide [3-6]. These regimens were also originally designed to be effective in treating the underlying malignancy, particularly leukemia, as well as providing intensive immunosuppression to prevent graft rejection. Although effective at achieving durable engraftment in most patients, intensive chemotherapy leads to a significant risk of short-term morbidity and a 10–30% risk of transplant-related mortality in patients with inborn errors of metabolism (IEM) [7]. Additionally, exposure to high doses of these agents can lead to a risk of significant late effects (cataracts, endocrinopathies, pulmonary and cardiac abnormalities, and new malignancies) as discussed later in this chapter. For these reasons, many parents and non-transplant physicians have been unwilling to accept the risks of HCT for children with IEM.
The demonstration that stable mixed chimerism could be achieved with sub-lethal doses of TBI (approximately one-sixth of the dose administered with standard TBI) and immunosuppression with cyclosporine and mycophenolate mofetil led to the widespread development of so-called non-myeloablative or reduced intensity conditioning regimens [8]. While these regimens were initially intended for patients who were ineligible for standard high dose conditioning, the fact that these regimens avoid many of the major short and long term toxicities associated with HCT has made this approach very attractive for use in children with non-malignant disorders. Fludarabine, a relatively new chemotherapeutic agent that has been widely used for conditioning, is highly immunosuppressive and has limited non-hematologic toxicity [9]. It has been used with low-dose TBI or without TBI in combination with busulfan, melphalan, or other agents. The use of these regimens in patients who are “chemotherapy naive” and who have normal immune systems, such as patients with IEM, has been very limited and associated with high rates of graft rejection. Additionally, measures commonly employed with reduced intensity conditioning to improve or boost engraftment, such as donor lymphocyte infusions, are associated with a high risk of acute and chronic graft vs. host disease (GVHD). Despite these issues, the use of reduced intensity conditioning in patients with IEM is a desirable goal, and research continues to refine these regimens with the objective of optimizing engraftment and minimizing toxicity.
The other consideration regarding HCT for patients with IEM is graft source. Obviously the preference is for HLA-matched sibling donors, but this is an option for only a minority of patients. The availability may be even lower for this patient group because siblings can also be affected with the disease. Certainly many of the potential matched sibling donors may be carriers of the disease in question. The question as to whether an alternative donor should be used preferentially over a sibling shown to be a carrier remains unanswered. Alternative unrelated donor sources (bone marrow, peripheral blood stem cells, cord blood) have been routinely utilized with good results. Acute and chronic GVHD is the major limitation to the use of alternative donors, and in these patients with non-malignant disorders there is no benefit to be derived from GVHD. Methods employed to reduce the risk of GVHD include T cell depletion (TCD) and possibly the use of umbilical cord blood. Both of these methods appear to be effective in reducing the risk of GVHD, but each carries with it a higher risk of graft rejection as well as a higher risk of infectious complications (particularly from viruses).
3. Lysosomal storage diseases
3.1. Mucopolysaccharidoses
Mucopolysaccharidoses are autosomal recessive disorders characterized by deficiencies of enzymes needed for the stepwise catabolism of complex sugars termed glycosaminoglycans (GAG) [10-12]. Some of these conditions predominantly affect the viscera; the others are both neuronopathic and visceral. Many of them also exhibit a dynamic range from a less severe phenotype associated with hypomorphic mutations to severe ones generally associated with null mutations.
3.1.1. Mucopolysaccharidosis type I (Hurler Syndrome)
In mucopolysaccharidosis type I (MPS I), the deficiency of α-L-iduronidase (IDUA) results in lysosomal accumulation of the GAG heparan sulfate and dermatan sulfate. This in turn leads to progressive cellular and multi-organ dysfunction. While the clinical findings may be apparent at birth, the manifestations of the disease and onset of symptoms usually occur by six months of age. Multiple organ systems are affected, and many of these patients present with or develop hepatosplenomegaly, cardiac disease, umbilical or inguinal hernia, obstructive airway disease, chronic rhinitis and otitis, skeletal deformities, hydrocephalus, neurocognitive deterioration, and corneal clouding. If left untreated, death occurs between 5 and 10 years of age, primarily from cardiac causes.
Treatments focus on approaches to replace the missing IDUA. This can be achieved either by exogenous administration of IDUA or through the endogenous production of IDUA following stable engraftment of normal cells producing enzyme within the affected individual. The former is achieved by enzyme replacement therapy (ERT) available for MPS I since 2003 [13], and the latter by HCT, which was first shown to hold promise in 1980 [2]. The therapeutic basis for both treatment options is that IDUA can be taken up by recipient cells via the mannose-6-phosphate receptor and then be translocated to lysosomes where it mediates the hydrolysis of GAG.
HCT has been accepted as a standard of care for patients with severe forms of MPS I (Hurler Syndrome). Initially, unaffected HLA-genotypically-identical bone marrow donors were considered the optimal donors, but results with matched unrelated donors, and especially with cord blood, are encouraging. As a result of better availability of improved methods for HLA typing and supportive care, the early engraftment and survival rates have improved, and currently may be as high as 85% in institutions specializing in transplantation for metabolic storage diseases [5, 14-19].
Remarkably, donor-derived cells engraft even within the brain, thereby providing a source of enzyme to the central nervous system and halting the neurocognitive decline in most patients [20]. This is in addition to correction of most of the visceral signs of pathology, including cardiovascular function, organomegaly, and lung disease. In contrast, the heart valves and skeletal abnormalities are largely unaffected by this therapy.
ERT has been introduced for treatment of less severe visceral forms of MPS I, and is currently the standard of care in patients without neurologic disease, since IDUA does not cross the blood-brain barrier [21]. Recent data on a combination of ERT with HCT are encouraging, however, and appear to support the possibility that combination therapy is in fact the new standard of care for patients with Hurler Syndrome [22-24]. The rationale for this approach is based on identifying risks in the pre-transplant course that are associated with increased morbidity and mortality during and after HCT [7]. Most prominent among these risks are upper and lower lung disease. It follows that if the enzyme can be provided for a sufficient time before transplantation, GAG storage in viscera can be partially cleared, and may result in fewer complications during HCT. The possibility that pre-transplant enzyme replacement therapy will result in increased graft failure because of generation of antibodies against donor cells has not been borne out. Of note, some advocate the use of combination therapy primarily for patients with higher risk disease. We and others, however, offer combination therapy for all patients with MPS I who are considered for HCT, because of the low risks associated with enzyme therapy and the potential that it may decrease life-threatening complications after HCT. In addition, it is possible that decreases in GAG, after enzyme replacement therapy, but before the HCT, can create a more permissive environment in the bone marrow niche for donor engraftment when compared to the patients who did not receive ERT.
3.1.2. Other mucopolysaccharidoses
In contrast to Hurler Syndrome, HCT has not been shown to significantly alter the natural history of patients with severe mucopolysaccharidosis type II (Hunter Syndrome). The attenuated phenotypes may benefit from stem cell therapy, but for yet unknown reasons, children with severe MPS II phenotype do not appear to gain neurocognitive benefit from the transplant. Whether transplantation before the onset of symptoms, such as in the neonatal period, may improve outcomes is as yet unclear.
Similarly, early results with HCT using allogeneic grafts have not been very encouraging in patients with Sanfilippo Syndrome (MPS III). Only limited published data exist regarding transplant results, but available data suggest that, in contrast to MPS I, the neurologic deterioration of MPS III patients is not alleviated by transplantation.
Morquio Syndrome (MPS IV), is characterized by significant musculoskeletal disease with less prominent neurologic changes, and so far has not been shown to benefit from HCT.
In contrast, the visceral findings of Maroteaux-Lamy Syndrome (MPS VI) have been shown to improve with HCT. However, the availability of enzyme replacement therapy for MPS VI limits the need for HCT.
Finally, Sly Syndrome (MPS VII), which results in bone deformities, developmental delays, and organomegaly, has been treated with HCT with some positive response [25-27].
Thus, individual mucopolysaccharidoses differ substantially with regards to their responses to HCT and ERT. While HCT, especially in combination with ERT, is a standard of care for severe MPS I (Hurler Syndrome), the efficacy of standard methods of transplantation for MPS II and MPS III has not been established.
4. Sphingolipidoses
The glycosphingolipids are an important component of the cell membrane, consisting of polysaccharide bound to lipid, primarily ceramide, which is incorporated into the membrane [28]. The polysaccharide portion contributes to cell interactions, adhesion, and signaling, in addition to other functions [29]. Degradation is accomplished through the action of lysosomal acid hydrolases, which serve to remove the carbohydrate moiety. Collectively the glycosphingolipid disorders are the most common cause of neurogenerative diseases (incidence approximately 1:18,000) in children [28]. With the exception of Fabry disease, these disorders are inherited in an autosomal recessive pattern. Based on the enzyme defect and substrate accumulation, these disorders are often divided into GM1 gangliosidosis, GM2 gangliosidoses (Tay-Sachs disease and Sandhoff disease), Fabry disease, multiple sulfatase deficiency, Gaucher disease, Niemann-Pick A and B, Farber disease, metachromatic leukodystrophy (MLD) and globoid cell leukodystrophy (GLD, also known as Krabbe disease). Most data regarding transplantation for these disorders relate to experience with MLD and GLD. These disorders will be discussed individually.
4.1. Metachromatic leukodystrophy
Metachromatic leukodystrophy (MLD) results from a decrease in arylsulfatase A (ARSA) activity, leading to the accumulation of the substrate cerebroside 3-sulfate, a component of myelin [30]. Decreased ARSA activity leads to demyelination of the white matter of the central nervous system (CNS) as well as the peripheral nerves [31]. Arylsulfatase A deficiency leading to MLD occurs with an overall incidence of approximately 1:40,000 births, while a higher frequency may be observed in specific populations [31-33]. There is significant phenotypic variation in MLD. In patients with the “late-infantile” form of the disease, neurological deterioration is initially observed within the first several years of life. Death generally ensues several years from diagnosis. Symptoms are associated with both central and peripheral demyelination, and motor-related difficulties are often apparent earlier than loss of cognition and language skills. The juvenile form of the disease has an onset from 4 years of age through adolescence [34-35]. Clinical manifestations of juvenile MLD are similar to the infantile form, although the rate of progression is slower. The adult form of the disease may become apparent as late as the seventh decade, and represents approximately 20% of cases of MLD [36]. Rather than presenting with motor-related difficulties, patients with late-onset disease may have emotional lability, progressive dementia, psychosis, and difficulties with substance abuse. There is a phenotype-genotype correlation in MLD, with more severe mutations resulting in more rapid accumulation of sulfatides and disease progression [37].
Krivit reported the results of the first transplant for MLD in 1990 [38]. Subsequently, reports of the success of transplantation for MLD generally have been limited to a small numbers of patients, and these data are difficult to assess due to variations in phenotype (late-infantile, juvenile, or adult forms) as well as the state of the disease at the time of transplantation [34]. Assessment of these outcomes is further limited by the lack of a universal standard for clinically assessing these patients both prior to and after transplantation. Obtaining such data will be critical to determining the utility of therapy, as asymptomatic patients or those early in their disease course are more likely to have better outcomes [16]. Similarly, those with less severe phenotypes may respond better to therapy. In regards to symptomatic late-infantile disease, while sulfatide levels decrease in urine and cerebrospinal fluid and the rate of progression may be less than observed in untreated siblings, the available data do not support the claim that transplantation has the capacity to stabilize disease [39]. The inability to deliver sufficient amounts of enzyme into the CNS is likely a primary limitation, as enzyme delivery is dependent on engraftment of cells such as the microglial population in the brain, which may take months following transplant [12, 27, 34]. In addition, despite engraftment of allogeneic cells, patients with infantile disease also appear to have progressive peripheral disease. Whether asymptomatic patients identified by neonatal screening or by family history who would be predicted to develop infantile disease can benefit from transplantation within the newborn period is debatable. Data available to address this question suggest that these patients continue to have progressive motor disabilities [34, 40-41]. In contrast, reports of the outcome of transplantation of later-onset disease (juvenile and adult forms) suggest that stabilization of the central nervous system may be achieved, even if patients are symptomatic at the time of transplantation [39,42-43]. As may be expected, the rate of decline prior to transplantation and the status of the disease at transplant are likely to affect outcomes [44].
4.2. Globoid cell leukodystrophy
The disorder known as globoid cell leukodystrophy (GLD) was initially described in 1916 by Krabbe, who reported infants developing spasticity and sclerosis of the brain [45]. Krabbe also described the characteristic “globoid cell” present in the white matter of affected patients. In 1970 the enzyme defect responsible for GLD was identified as the lysosomal enzyme galactocerebroside β-galactosidase (GALC) [46], also commonly referred to as galactocerebrosidase. In 1990 Zlotogora localized the gene to chromosome 14 [47], and the gene was cloned by Wenger’s laboratory in 1993 [48]. The primary substrate that accumulates in GLD is galactocerebroside, which is degraded by GALC to ceramide and galactose [49]. The metabolite psychosine accumulates as well in GLD, as it is a substrate for GALC [35]. Psychosine has been thought to contribute to cytotoxicity of cells in the CNS, including oligodendrocytes [50-52].
Globoid cell leukodystrophy has an incidence of 1:70,000–100,000, and presents with a varied phenotype, similar to MLD. Historically, 85–90% of patients with GLD develop symptoms as infants [35]. Patients with infantile GLD characteristically become increasingly irritable, with increased sensitivity to stimuli, developmental arrest and subsequent regression [35]. Protein levels in the cerebro-spinal fluid are high. Hypertonicity is apparent, with feeding difficulties and visual changes; increased deep tendon reflexes and seizures may be observed. Death generally results within a few years of the onset of symptoms. Other patients have less severe disease, and have been divided into late infantile (onset from 6 months to 3 years) and juvenile forms (ages 3–8 years), while some patients are not diagnosed until their second or third decades, and occasionally later [35]. As might be expected, these later onset patients have a less rapidly progressive disease course.
The first description of the outcomes of GLD patients treated by allogeneic transplantation were provided by Krivit et al in 1998 [53]. Four of the 5 patients reported had late onset disease, while one had typical infantile GLD. For the older patients, the patients appeared to stabilize, or even improve, in regards to their disease. The patient with infantile disease was transplanted at 2 months of age. By now there is sufficient experience with transplantation of symptomatic patients with infantile disease to state that transplantation is not effective at arresting disease progression, although the clinical course may be attenuated [39]. In addressing this question, Escolar reported a staging system for clinically assessing patients with GLD in the pre-transplant period, and correlated this to outcomes [54]. There has recently been great interest in the outcomes of patients with presumed infantile GLD if these patients are transplanted in the neonatal period [55]. These very young and asymptomatic patients who would be predicted to have a severe phenotype, clearly have a different clinical course after transplantation than would be expected without transplantation [56]. Based on this observation, there has been significant discussion regarding the use of newborn screening as a means of identifying these patients prior to the onset of symptoms [57, 58]. However, it remains unclear how patients who have severe genotypes and are transplanted in the first weeks of life will do as they age [55]. It is of interest that many of the difficulties these patients face are motor limitations, and this is likely at least in part due to peripheral nerve demyelination. Such a finding would be in keeping with observations in the twitcher mice, a model for GLD [59-61]. Thus far there has not been universal agreement to move towards neonatal screening for GLD with the intention of identifying and transplanting patients predicted to have severe disease soon after delivery, although screening is currently being done in New York, and is likely to be in place soon in several other US states. It should be noted that due to the severe time limitations in attempting to transplant asymptomatic neonates, a large proportion of these infants will require cord blood grafts. This has been suggested to be a preferred graft source, not only because of the expediency of moving to transplantation, but also because of the possibility of an increased ability of cord blood to transdifferentiate into a variety of non-hematopoietic stem cells or progenitor cells [16]. Additional clinical information will be required to determine if this will be the case.
The efficacy of transplantation in patients with later onset GLD remains less well delineated than would be expected. It has previously been stated that patients with later onset disease are likely to benefit from transplantation [62]. In some cases, improvement has been reported [26]. However, data related to large series of patients focused on the function and neurocognitive outcomes are not available. It would be important to review the genotypic findings of an individual diagnosed by GALC activity to determine whether it is reasonable to pursue transplantation in an asymptomatic patient, as it is not necessarily clear what the anticipated course will be. However, if a patient with later-onset disease is early in the course of the disease, transplantation seems a reasonable option. It has been suggested that for a number of these diseases, multi-institutional trials with standard methods of analysis would prove very beneficial to the field [63], and despite the difficulties inherent in developing and funding these large trials that could require decades to complete, it is difficult to argue with this view.
Other related lysosomal disorders have been treated with transplantation, although less data are available than for MLD and GLD. Niemann-Pick A and B result from a deficiency in sphingomyelinase. In Niemann-Pick A rapid neurologic progression is often observed. For these patients, who are severely affected and deteriorating rapidly, there are insufficient data to confirm that transplantation modifies the course of neurologic disease. In Niemann-Pick B, there is little published data, but our group and others have observed improvement in the marrow and lung pathology of these patients after transplant [64-65]. Niemann-Pick C has been shown to have 2 subtypes, both associated with accumulation of cholesterol. Niemann-Pick C1 is the most frequent form, but is not due to a lysosomal enzyme defect and therefore is less likely to respond to transplantation. In contrast, Niemann-Pick C2 disease is associated with a deficit in a lysosomal enzyme [66]. While it has been reported that there is an insufficient response of Niemann-Pick C to transplantation [67], the ability to separate the genotypes has only recently become available. Although it might be expected that type C2 may respond to transplantation, results have not been reported in individuals confirmed to have this genotype. As the C2 genotype is much less common than C1, genetic analysis prior to intervention will be of importance.
GM1 gangliosidosis is characterized by seizures and psychomotor deficits, and has infantile, juvenile, and adult onset forms [35, 68]. While little information is available regarding the utility of transplantation, a report describing a juvenile patient suggests there is little benefit from transplantation [69]. GM2 gangliosidosis disorders (Tay-Sachs and Sandhoff) are due to abnormalities within the hexosaminidase (HEX) gene [68]. In the case of Tay-Sachs, HEX A is deficient, while in Sandhoff HEX A and B are deficient. Unfortunately in most cases these disorders are rapidly progressive, and there is little information to suggest that symptomatic patients benefit from transplantation [40, 70]. However, it is as yet unclear as to whether those with late-onset disease or newborns predicted to have early-onset disease would benefit. Gaucher disease has been shown to benefit from transplantation [71-74], but as there is enzyme replacement therapy available for Gaucher, there is little enthusiasm for the morbidity and mortality associated with transplantation for this disorder. However, as the neuropathic form of Gaucher does not benefit from ERT [75], there may be interest in evaluating transplantation in patients with Gaucher who show evidence of neurologic deterioration [40]. Fabry disease is an X-linked disorder of the lysosomal enzyme α-galactosidase A, which results in accumulation of substrate in the kidneys, heart, eyes, and blood vessels, but does not have a significant neurological component. As enzyme replacement therapy is available for Fabry, there is currently no enthusiasm for transplantation [41].
4.3. Adrenoleukodystrophy
While GLD and MLD are autosomal recessive lysosomal enzyme deficiencies, adrenoleukodystrophy (ALD) is an X-linked disorder of the peroxisome that results in abnormal metabolism of very long chain fatty acids (VLCFA) due to decreased beta-oxidation. These VLCFA accumulate in the testes, adrenal gland, and white matter of the central nervous system [76]. For reasons that are not clear, approximately 40% of individuals with ALD under 20 years of age show a clinical course of rapid neurologic deterioration [77]. This condition, representing the cerebral form of ALD, is an inflammatory process present in the CNS, with a mixed cellular infiltrative process, although CD8+ T cells are prominent [78-79]. Eichler stated that the bulk of the inflammation occurs behind the area in which demyelination is seen, and he proposed that the infiltrative process occurs in response to demyelination rather than being its cause [80]. The beneficial effects of HCT are thought to be related at least in part to elimination of the active inflammation present in the CNS, although recent early findings of a gene therapy approach suggest that there is a corrective process provided by hematopoietically-derived cells [81]. Another important issue in regards to the early identification of ALD relates to adrenal insufficiency. Primary adrenal insufficiency (AI), or Addison’s disease, which precedes cerebral manifestations of ALD, occurs with an estimated prevalence of 43% in asymptomatic boys with X-ALD [82]. In our center’s experience, 7 boys who have been evaluated for transplantation for cerebral ALD since 2002 had previously been diagnosed with adrenal insufficiency, but VLCFA testing was not performed expeditiously, resulting in a delay in diagnosis and presumably disease progression that either rendered the patient ineligible for transplantation or put him at higher risk for a poor outcome (Polgreen et al., unpublished observations).
Transplantation early in the course of cerebral ALD has been shown to stabilize the disease process, although it is clear that in more advanced patients the outcome is inferior [4]. An MRI scoring system was developed by Loes to quantitate the extent of the disease [83], and this allows the identification of patients who are at high risk for poor outcomes of transplantation. Due to the importance of the extent of disease in the ability of transplantation to arrest the disease process [84], it is recommended that boys with biochemically proven ALD be monitored with serial MRI scans, and to proceed with transplantation when patients show evidence of early progression to cerebral disease [4]. It is not known whether transplantation plays any role in preventing the evolution of other manifestations of ALD, such as the peripheral nervous system condition termed adrenomyeloneuropathy (AMN). In addition, there are no data to show that transplantation prior to the onset of cerebral ALD will prevent its occurrence. Therefore the risks of transplantation are not justified in patients without evidence of evolving cerebral ALD, as a majority of boys will not develop cerebral ALD [85]. The use of Lorenzo’s oil in patients who have not yet developed cerebral ALD may decrease the risk of its occurrence [86].
5. Oligosaccharidosis: Mannosidosis
Alpha-mannosidosis presents with hepatosplenomegaly, vomiting, immune deficiency, and dysostosis multiplex. Affected patients also have mental retardation and ocular clouding. Approximately 20 patients have been transplanted to date, some of whom had pulmonary and airway complications during the first several months after HCT. Remarkably, the mental development as well as cardiopulmonary function appear to have been preserved, suggesting that HCT is a valid treatment option for alpha-mannosidosis [87].
6. Enzyme localization defect: Mucolipidosis Type II (I-Cell Disease)
Mucolipidosis Type II results from a defect in a phosphotransferase that is integral to the localization of numerous lysosomal hydrolyses. In the absence of this targeting mechanism, these lysosomal enzymes are secreted rather than retained in the lysosome. This results in lysosomal substrate accumulation, while extremely high serum levels of these enzymes are observed in the plasma. The phenotype resembles MPS I, but the response to HCT has been much less favorable [88]. It remains to be determined whether early identification of these patients, before the damage to visceral and neuronal tissue is irreversible and profound, and expedient transplantation may improve outcomes.
7. Late effects after HCT for Metabolic Storage Disease
As discussed previously, the majority of patients with IEM who undergo HCT do so following traditional high-dose, chemotherapy-based conditioning regimens. The combination of busulfan and cyclophosphamide is the most common regimen utilized. Patients with IEM are unique, however, in that they also have to face the potential of long-term complications related to their underlying disease that may not be reversed or prevented by successful HCT. One can assume that they are at the same risk as other patients going through HCT for the common conditions seen after exposure to high-dose chemotherapy in the conditioning regimen, but there are little data that describe those findings. Additionally, there may be unique long-term effects of some of the preparative regimens in patients with IEM, but again for the most part these have not been reported to date. Limited long-term follow-up data in some subsets of IEM patients (Hurler’s syndrome in particular) related to amelioration of disease-associated conditions are available and will be briefly summarized.
Endocrine issues. There are minimal IEM-specific data, but some patients have been found to have primary ovarian failure [19]. It is unclear if this is related to the disease or HCT since both may contribute. Other endocrine issues seen in children after HCT include gonadal failure in males, hypothyroidism, and growth failure. While some of these conditions may be more frequently encountered after exposure to TBI, they can also be seen with non-TBI containing regimens. Patients with Hurler’s syndrome have growth problems to begin with, and while some reports suggest that linear growth may be maintained early after HCT, others suggest growth may not be maintained on a long-term basis [19, 89].
Pulmonary. Patients with IEM have high rates of pulmonary complications during HCT that may be related to a pro-inflammatory state within the lung [90]. While busulfan can lead to pulmonary fibrosis, this is not a common complication in children after HCT. In patients with Hurler’s it has been demonstrated that they do have relief of their obstructive airway symptoms and improvement in sleep apnea with improved pulmonary function [19, 91]. A reduction in the risk of pulmonary deterioration in a patient successfully transplanted for I-cell disease has also been reported [92].
Cardiac. Long-term cardiovascular complications are rarely associated with exposure to cyclophosphamide and busulfan alone. Certainly for several of the IEM disorders, progressive cardiac dysfunction is common. For patients with Hurler’s, long-term follow-up after HCT has shown that myocardial function is preserved and hypertrophy has been seen to regress, and patients have not developed heart failure or coronary artery disease. However, mitral and aortic valve deformities have persisted and frequently progressed [93].
Neuropsychological and cognitive function. In the absence of exposure to radiation during conditioning, children typically do not have significant neuropsychological sequelae secondary to HCT. In the case of children with IEM, post-HCT neurologic outcome depends upon the specific disease, age at time of HCT, specific genotype of the disease, cognitive status at the time of HCT, engraftment status, and donor enzyme activity after HCT. The goal, of course, is to perform HCT early in the course of the disease before any extensive neurologic damage or deterioration has occurred. When this can be done, neurocognitive function can be stabilized (or in some cases improved) and further progressive neurologic deterioration can be prevented [5, 19, 89,91, 94].
Bone and joints. HCT conditioning can affect bone health leading to osteopenia and osteoporosis. This may be reversible on its own over time or may require further intervention with vitamin D and calcium supplementation or occasionally treatment with bisphosphonates. These effects have not been studied to date in children with IEM. Other disease-specific orthopedic complications, such as odontoid dysplasia in patients with Hurler’s, have been shown to improve over time [95]. However, other complications such as genu valgum, carpel tunnel syndrome, and acetabular dysplasia have not improved after HCT and frequently require surgical intervention [96-97].
Post-transplant malignancies. It has been well described that patients after HCT are at life-long increased risk of developing malignancies that is estimated at nearly 10-fold greater than that in the general population [98-99]. Whether this same risk applies to patients with IEM is not known, but we are aware of some patients who have developed malignancies years after HCT.
Late Mortality. After allogeneic HCT patients have twice the risk of mortality of the general population [100]. Data submitted for publication from the Center for International Blood and Marrow Transplant Research demonstrate that patients with IEM have a higher risk of mortality between 2–6 yrs after HCT and that this increased risk persists even 6 yrs after HCT. This increased risk is highest in patients who have received unrelated or HLA non-identical related donor transplants. Causes of death include GVHD, infection, and organ failure.
Summary
Obtaining clear data regarding the outcomes of transplantation in patients with IEM has proven difficult due to the rarity of these diseases, their variable phenotypes/genotypes, and differences in stem cell sources, preparative regimens, supportive therapy, and assessment of “successful” outcomes. Multi-institution trials with a common approach and outcome measures will be important in this regard. In earlier years HCT in these populations used standardized regimens designed for patients with malignant disorders. For disorders such as Hurler’s syndrome and early cerebral ALD, this approach has been successful. However, for other disorders, the ability to achieve satisfactory outcomes with standard transplant regimens has proven elusive. Reduced-intensity conditioning strategies may prove more successful in decreasing morbidity and mortality, particularly in patients with ongoing neurologic injury. It is anticipated that future investigations will test the use of combination therapy with or without transplantation, including substrate inhibition [101-102], chaperone therapy [103-105], enzyme replacement [24, 106], modification of anti-inflammatory therapy [107], or biologic response modifiers [108-110]. In addition, the interest in neonatal screening will provide the opportunity to intervene early in the course of these diseases, as this appears critical in achieving optimal outcomes [4, 111-114]. Finally, modifying the transplant procedure, using selectively expanded cell populations, or using cytokine manipulation may enhance microglial engraftment [115-118], which could make a substantial difference in the delivery of enzyme to the CNS. Significant progress is required to enhance transplant results and to determine optimal therapy in individuals with these devastating congenital disorders.
References
1. Fratantoni JC, Hall CW, Neufeld EF. Hurler and Hunter syndromes: mutual correction of the defect in cultured fibroblasts. Science. 1968;162:570-572.
2. Hobbs JR, Hugh-Jones K, Barrett AJ, et al. Reversal of clinical features of Hurler's disease and biochemical improvement after treatment by bone-marrow transplantation. Lancet. 1981;2:709-712.
3. Jacobson P, Park JJ, DeFor TE, et al. Oral busulfan pharmacokinetics and engraftment in children with Hurler syndrome and other inherited metabolic storage diseases undergoing hematopoietic cell transplantation. Bone Marrow Transplant. 2001;27:855-861.
4. Peters C, Charnas LR, Tan Y, et al. Cerebral X-linked adrenoleukodystrophy: the international hematopoietic cell transplantation experience from 1982 to 1999. Blood. 2004;104:881-888.
5. Peters C, Shapiro EG, Anderson J, et al. Hurler syndrome: II. Outcome of HLA-genotypically identical sibling and HLA-haploidentical related donor bone marrow transplantation in fifty-four children. The Storage Disease Collaborative Study Group. Blood. 1998;91:2601-2608.
6. Peters C, Balthazor M, Shapiro EG, et al. Outcome of unrelated donor bone marrow transplantation in 40 children with Hurler syndrome. Blood. 1996;87:4894-4902.
10. Neufeld EF. Lysosomal storage diseases. Annu Rev Biochem. 1991;60:257-280.
11. Muenzer J. The mucopolysaccharidoses: a heterogeneous group of disorders with variable pediatric presentations. J Pediatr. 2004;144:S27-34.
12. Orchard PJ, Blazar BR, Wagner J, Charnas L, Krivit W, Tolar J. Hematopoietic cell therapy for metabolic disease. J Pediatr. 2007;151:340-346.
13. Kakkis ED, Muenzer J, Tiller GE, et al. Enzyme-replacement therapy in mucopolysaccharidosis I. N Engl J Med. 2001;344:182-188.
14. Boelens JJ, Rocha V, Aldenhoven M, et al. Risk factor analysis of outcomes after unrelated cord blood transplantation in patients with hurler syndrome. Biol Blood Marrow Transplant. 2009;15:618-625.
15. Aldenhoven M, Boelens JJ, de Koning TJ. The clinical outcome of Hurler syndrome after stem cell transplantation. Biol Blood Marrow Transplant. 2008;14:485-498.
16. Prasad VK, Kurtzberg J. Cord blood and bone marrow transplantation in inherited metabolic diseases: scientific basis, current status and future directions. Br J Haematol. 2009.
17. Prasad VK, Kurtzberg J. Umbilical cord blood transplantation for non-malignant diseases. Bone Marrow Transplant. 2009;44:643-651.
18. Prasad VK, Mendizabal A, Parikh SH, et al. Unrelated donor umbilical cord blood transplantation for inherited metabolic disorders in 159 pediatric patients from a single center: influence of cellular composition of the graft on transplantation outcomes. Blood. 2008;112:2979-2989.
19. Vellodi A, Young EP, Cooper A, et al. Bone marrow transplantation for mucopolysaccharidosis type I: experience of two British centres. Arch Dis Child. 1997;76:92-99.
20. Krivit W, Sung JH, Shapiro EG, Lockman LA. Microglia: the effector cell for reconstitution of the central nervous system following bone marrow transplantation for lysosomal and peroxisomal storage diseases. Cell Transplant. 1995;4:385-392.
21. Wraith JE. The first 5 years of clinical experience with laronidase enzyme replacement therapy for mucopolysaccharidosis I. Expert Opin Pharmacother. 2005;6:489-506.
22. Wynn RF, Mercer J, Page J, Carr TF, Jones S, Wraith JE. Use of enzyme replacement therapy (Laronidase) before hematopoietic stem cell transplantation for mucopolysaccharidosis I: experience in 18 patients. J Pediatr. 2009;154:135-139.
23. Cox-Brinkman J, Boelens JJ, Wraith JE, et al. Haematopoietic cell transplantation (HCT) in combination with enzyme replacement therapy (ERT) in patients with Hurler syndrome. Bone Marrow Transplant. 2006;38:17-21.
24. Tolar J, Grewal SS, Bjoraker KJ, et al. Combination of enzyme replacement and hematopoietic stem cell transplantation as therapy for Hurler syndrome. Bone Marrow Transplant. 2008;41:531-535.
25. Klein KA, Krivit W, Whitley CB, et al. Poor cognitive outcome of eleven children with Sanfilippo syndrome after bone marrow transplantation and successful engraftment. Bone Marrow Transplant. 1995;15:S176-181.
26. Krivit W. Allogeneic stem cell transplantation for the treatment of lysosomal and peroxisomal metabolic diseases. Springer Semin Immunopathol. 2004;26:119-132.
27. Peters C, Krivit W. Hematopoietic cell transplantation for mucopolysaccharidosis IIB (Hunter syndrome). Bone Marrow Transplant. 2000;25:1097-1099.
29. Watts RW. A historical perspective of the glycosphingolipids and sphingolipidoses. Philos Trans R Soc Lond B Biol Sci. 2003;358:975-983.
30. Gieselmann V, Polten A, Kreysing J, von Figura K. Molecular genetics of metachromatic leukodystrophy. J Inherit Metab Dis. 1994;17:500-509.
31. Eng B, Nakamura LN, O'Reilly N, et al. Identification of nine novel arylsulfatase a (ARSA) gene mutations in patients with metachromatic leukodystrophy (MLD). Hum Mutat. 2003;22:418-419.
32. Heinisch U, Zlotogora J, Kafert S, Gieselmann V. Multiple mutations are responsible for the high frequency of metachromatic leukodystrophy in a small geographic area. Am J Hum Genet. 1995;56:51-57.
33. Zlotogora J, Bach G, Bosenberg C, Barak Y, von Figura K, Gieselmann V. Molecular basis of late infantile metachromatic leukodystrophy in the Habbanite Jews. Hum Mutat. 1995;5:137-143.
34. Biffi A, Lucchini G, Rovelli A, Sessa M. Metachromatic leukodystrophy: an overview of current and prospective treatments. Bone Marrow Transplant. 2008;42 Suppl 2:S2-6.
35. Scriver CR, Beaudet AL, Sly WS, Valle D. The Metabolic and Molecular Bases of Inherited Disease. Vol. III (ed 8th). New York: McGraw-Hill; 2001.
36. Sedel F, Tourbah A, Fontaine B, et al. Leukoencephalopathies associated with inborn errors of metabolism in adults. J Inherit Metab Dis. 2008;31:295-307.
37. Gieselmann V. Metachromatic leukodystrophy: genetics, pathogenesis and therapeutic options. Acta Paediatr Suppl. 2008;97:15-21.
38. Krivit W, Shapiro E, Kennedy W, et al. Treatment of late infantile metachromatic leukodystrophy by bone marrow transplantation. N Engl J Med. 1990;322:28-32.
39. Krivit W, Aubourg P, Shapiro E, Peters C. Bone marrow transplantation for globoid cell leukodystrophy, adrenoleukodystrophy, metachromatic leukodystrophy, and Hurler syndrome. Curr Opin Hematol. 1999;6:377-382.
40. Peters C, Steward CG. Hematopoietic cell transplantation for inherited metabolic diseases: an overview of outcomes and practice guidelines. Bone Marrow Transplant. 2003;31:229-239.
41. Peters C. Hematopoietic Stem Cell Transplantation for Storage Diseases. In: Appelbaum FR, Forman SJ, Negrin RS, eds. Thomas' Hematopoietic Cell Transplantation: Stem Cell Transplantation (ed 4). Oxford, UK: Wiley, John & Sons, Incorporated; 2009:1136-1162.
42. Gorg M, Wilck W, Granitzny B, et al. Stabilization of juvenile metachromatic leukodystrophy after bone marrow transplantation: a 13-year follow-up. J Child Neurol. 2007;22:1139-1142.
43. Solders G, Celsing G, Hagenfeldt L, Ljungman P, Isberg B, Ringden O. Improved peripheral nerve conduction, EEG and verbal IQ after bone marrow transplantation for adult metachromatic leukodystrophy. Bone Marrow Transplant. 1998;22:1119-1122.
44. Pierson TM, Bonnemann CG, Finkel RS, Bunin N, Tennekoon GI. Umbilical cord blood transplantation for juvenile metachromatic leukodystrophy. Ann Neurol. 2008;64:583-587.
45. Krabbe K. A new familial, infantile form of diffuse brain sclerosis. Brain. 1916;39:74-114.
46. Suzuki K, Suzuki Y. Globoid cell leucodystrophy (Krabbe's disease): deficiency of galactocerebroside beta-galactosidase. Proc Natl Acad Sci U S A. 1970;66:302-309.
48. Chen YQ, Rafi MA, de Gala G, Wenger DA. Cloning and expression of cDNA encoding human galactocerebrosidase, the enzyme deficient in globoid cell leukodystrophy. Hum Mol Genet. 1993;2:1841-1845.
49. Tatsumi N, Inui K, Sakai N, et al. Molecular defects in Krabbe disease. Hum Mol Genet. 1995;4:1865-1868.
50. Igisu H, Suzuki K. Progressive accumulation of toxic metabolite in a genetic leukodystrophy. Science. 1984;224:753-755.
51. Suzuki K. Twenty five years of the "psychosine hypothesis": a personal perspective of its history and present status. Neurochem Res. 1998;23:251-259.
52. White AB, Givogri MI, Lopez-Rosas A, et al. Psychosine accumulates in membrane microdomains in the brain of krabbe patients, disrupting the raft architecture. J Neurosci. 2009;29:6068-6077.
55. Duffner PK, Caviness VS, Jr., Erbe RW, et al. The long-term outcomes of presymptomatic infants transplanted for Krabbe disease: Report of the workshop held on July 11 and 12, 2008, Holiday Valley, New York. Genet Med. 2009.
57. Duffner PK, Caggana M, Orsini JJ, et al. Newborn screening for Krabbe disease: the New York State model. Pediatr Neurol. 2009;40:245-252; discussion 253-245.
58. Meikle PJ, Grasby DJ, Dean CJ, et al. Newborn screening for lysosomal storage disorders. Mol Genet Metab. 2006;88:307-314.
59. Kagitani-Shimono K, Mohri I, Yagi T, Taniike M, Suzuki K. Peripheral neuropathy in the twitcher mouse: accumulation of extracellular matrix in the endoneurium and aberrant expression of ion channels. Acta Neuropathol. 2008;115:577-587.
60. Kondo A, Hoogerbrugge PM, Suzuki K, Poorthuis BJ, Van Bekkum DW. Pathology of the peripheral nerve in the twitcher mouse following bone marrow transplantation. Brain Res. 1988;460:178-183.
61. Luzi P, Rafi MA, Zaka M, et al. Biochemical and pathological evaluation of long-lived mice with globoid cell leukodystrophy after bone marrow transplantation. Mol Genet Metab. 2005;86:150-159.
63. Cartier N, Aubourg P. Hematopoietic stem cell gene therapy in Hurler syndrome, globoid cell leukodystrophy, metachromatic leukodystrophy and X-adrenoleukodystrophy. Curr Opin Mol Ther. 2008;10:471-478.
64. Victor S, Coulter JB, Besley GT, et al. Niemann-Pick disease: sixteen-year follow-up of allogeneic bone marrow transplantation in a type B variant. J Inherit Metab Dis. 2003;26:775-785.
65. Shah AJ, Kapoor N, Crooks GM, et al. Successful hematopoietic stem cell transplantation for Niemann-Pick disease type B. Pediatrics. 2005;116:1022-1025.
66. Walkley SU, Suzuki K. Consequences of NPC1 and NPC2 loss of function in mammalian neurons. Biochim Biophys Acta. 2004;1685:48-62.
68. Walkley SU. Secondary accumulation of gangliosides in lysosomal storage disorders. Semin Cell Dev Biol. 2004;15:433-444.
69. Shield JP, Stone J, Steward CG. Bone marrow transplantation correcting beta-galactosidase activity does not influence neurological outcome in juvenile GM1-gangliosidosis. J Inherit Metab Dis. 2005;28:797-798.
71. Starer F, Sargent JD, Hobbs JR. Regression of the radiological changes of Gaucher's disease following bone marrow transplantation. Br J Radiol. 1987;60:1189-1195.
72. Ringden O, Groth CG, Erikson A, et al. Long-term follow-up of the first successful bone marrow transplantation in Gaucher disease. Transplantation. 1988;46:66-70.
73. Svennerholm L, Erikson A, Groth CG, Ringden O, Mansson JE. Norrbottnian type of Gaucher disease--clinical, biochemical and molecular biology aspects: successful treatment with bone marrow transplantation. Dev Neurosci. 1991;13:345-351.
74. Tsai P, Lipton JM, Sahdev I, et al. Allogenic bone marrow transplantation in severe Gaucher disease. Pediatr Res. 1992;31:503-507.
75. Goker-Alpan O, Wiggs EA, Eblan MJ, et al. Cognitive outcome in treated patients with chronic neuronopathic Gaucher disease. J Pediatr. 2008;153:89-94.
76. Krasemann EW, Meier V, Korenke GC, Hunneman DH, Hanefeld F. Identification of mutations in the ALD-gene of 20 families with adrenoleukodystrophy/adrenomyeloneuropathy. Hum Genet. 1996;97:194-197.
77. Berger J, Gartner J. X-linked adrenoleukodystrophy: clinical, biochemical and pathogenetic aspects. Biochim Biophys Acta. 2006;1763:1721-1732.
78. Ito M, Blumberg BM, Mock DJ, et al. Potential environmental and host participants in the early white matter lesion of adreno-leukodystrophy: morphologic evidence for CD8 cytotoxic T cells, cytolysis of oligodendrocytes, and CD1-mediated lipid antigen presentation. J Neuropathol Exp Neurol. 2001;60:1004-1019.
79. Powers JM, Moser HW, Moser AB, Ma CK, Elias SB, Norum RA. Pathologic findings in adrenoleukodystrophy heterozygotes. Arch Pathol Lab Med. 1987;111:151-153.
80. Eichler F, Van Haren K. Immune response in leukodystrophies. Pediatr Neurol. 2007;37:235-244.
81. Cartier N, Hacein-Bey-Abina S, Bartholomae CC, et al. Hematopoietic stem cell gene therapy with a lentiviral vector in X-linked adrenoleukodystrophy. Science. 2009;326:818-823.
82. Dubey P, Raymond GV, Moser AB, Kharkar S, Bezman L, Moser HW. Adrenal insufficiency in asymptomatic adrenoleukodystrophy patients identified by very long-chain fatty acid screening. J Pediatr. 2005;146:528-532.
83. Loes DJ, Fatemi A, Melhem ER, et al. Analysis of MRI patterns aids prediction of progression in X-linked adrenoleukodystrophy. Neurology. 2003;61:369-374.
84. Mahmood A, Raymond GV, Dubey P, Peters C, Moser HW. Survival analysis of haematopoietic cell transplantation for childhood cerebral X-linked adrenoleukodystrophy: a comparison study. Lancet Neurol. 2007;6:687-692.
85. Mahmood A, Dubey P, Moser HW, Moser A. X-linked adrenoleukodystrophy: Therapeutic approaches to distinct phenotypes. Pediatr Transplant. 2005;9:55-62.
87. Grewal SS, Shapiro EG, Krivit W, et al. Effective treatment of alpha-mannosidosis by allogeneic hematopoietic stem cell transplantation. J Pediatr. 2004;144:569-573.
91. Whitley CB, Belani KG, Chang PN, et al. Long-term outcome of Hurler syndrome following bone marrow transplantation. Am J Med Genet. 1993;46:209-218.
93. Braunlin EA, Stauffer NR, Peters CH, et al. Usefulness of bone marrow transplantation in the Hurler syndrome. Am J Cardiol. 2003;92:882-886.
94. Shapiro EG, Lockman LA, Balthazor M, Krivit W. Neuropsychological outcomes of several storage diseases with and without bone marrow transplantation. J Inherit Metab Dis. 1995;18:413-429.
95. Hite SH, Peters C, Krivit W. Correction of odontoid dysplasia following bone-marrow transplantation and engraftment (in Hurler syndrome MPS 1H). Pediatr Radiol. 2000;30:464-470.
96. Field RE, Buchanan JA, Copplemans MG, Aichroth PM. Bone-marrow transplantation in Hurler's syndrome. Effect on skeletal development. J Bone Joint Surg Br. 1994;76:975-981.
97. Wraith JE, Alani SM. Carpal tunnel syndrome in the mucopolysaccharidoses and related disorders. Arch Dis Child. 1990;65:962-963.
98. Baker KS, DeFor TE, Burns LJ, Ramsay NK, Neglia JP, Robison LL. New malignancies after blood or marrow stem-cell transplantation in children and adults: incidence and risk factors. J Clin Oncol. 2003;21:1352-1358.
99. Bhatia S, Ramsay NK, Steinbuch M, et al. Malignant neoplasms following bone marrow transplantation. Blood. 1996;87:3633-3639.
101. Desnick RJ. Enzyme replacement and enhancement therapies for lysosomal diseases. J Inherit Metab Dis. 2004;27:385-410.
102. Cox TM. Substrate reduction therapy for lysosomal storage diseases. Acta Paediatr Suppl. 2005;94:69-75; discussion 57.
103. Gregersen N, Bolund L, Bross P. Protein misfolding, aggregation, and degradation in disease. Mol Biotechnol. 2005;31:141-150.
104. Desnick RJ, Schuchman EH. Enzyme replacement and enhancement therapies: lessons from lysosomal disorders. Nat Rev Genet. 2002;3:954-966.
105. Hoffmann B, Mayatepek E. Neurological manifestations in lysosomal storage disorders - from pathology to first therapeutic possibilities. Neuropediatrics. 2005;36:285-289.
106. Vellodi A. Lysosomal storage disorders. Br J Haematol. 2005;128:413-431.
108. Spagnoli A, Longobardi L, O'Rear L. Cartilage disorders: potential therapeutic use of mesenchymal stem cells. Endocr Dev. 2005;9:17-30.
109. Young PP, Fantz CR, Sands MS. VEGF disrupts the neonatal blood-brain barrier and increases life span after non-ablative BMT in a murine model of congenital neurodegeneration caused by a lysosomal enzyme deficiency. Exp Neurol. 2004;188:104-114.
110. Zaka M, Rafi MA, Rao HZ, Luzi P, Wenger DA. Insulin-like growth factor-1 provides protection against psychosine-induced apoptosis in cultured mouse oligodendrocyte progenitor cells using primarily the PI3K/Akt pathway. Mol Cell Neurosci. 2005;30:398-407.
111. Li Y, Scott CR, Chamoles NA, et al. Direct multiplex assay of lysosomal enzymes in dried blood spots for newborn screening. Clin Chem. 2004;50:1785-1796.
112. Meikle PJ, Ranieri E, Simonsen H, et al. Newborn screening for lysosomal storage disorders: clinical evaluation of a two-tier strategy. Pediatrics. 2004;114:909-916.
113. Millington DS. Newborn screening for lysosomal storage disorders. Clin Chem. 2005;51:808-809.
114. Staba SL, Escolar ML, Poe M, et al. Cord-blood transplants from unrelated donors in patients with Hurler's syndrome. N Engl J Med. 2004;350:1960-1969.
115. Davoust N, Vuaillat C, Androdias G, Nataf S. From bone marrow to microglia: barriers and avenues. Trends Immunol. 2008;29:227-234.
116. D'Mello C, Le T, Swain MG. Cerebral microglia recruit monocytes into the brain in response to tumor necrosis factoralpha signaling during peripheral organ inflammation. J Neurosci. 2009;29:2089-2102.
117. Hall AA, Herrera Y, Ajmo CT, Jr., Cuevas J, Pennypacker KR. Sigma receptors suppress multiple aspects of microglial activation. Glia. 2009;57:744-754.
118. Semple BD, Bye N, Rancan M, Ziebell JM, Morganti-Kossmann MC. Role of CCL2 (MCP-1) in traumatic brain injury (TBI): evidence from severe TBI patients and CCL2-/- mice. J Cereb Blood Flow Metab. 2009.
1. Introduction
Hematopoietic cell transplantation (HCT) is a prototypic stem cell therapy, and has been a life-saving measure for tens of thousands of patients. Over its relatively short history, the study of transplantation has shown that the transfer of relatively few cells can lead to the development of a fully functional lympho-hematopoietic system in the recipient, that bidirectional immunologic tolerance between post-natal tissues is possible, and that cancer can be eradicated by immunologic means.
After the seminal insight that cells with two different enzyme deficiencies can complement each other [1], a paradigm shift occurred, according to which stem cell transfer is applicable to equally fatal but non-malignant disorders [2]. This has translated into the establishment of transplantation as the standard of care for some of these enzyme disorders; monitoring of hundreds of patients with congenital metabolic disorders after transplantation has shown that long-lasting cross correction can be achieved. Conceptually, these benefits have been limited to congenital defects of enzymes, but there is no intellectual barrier to applying this strategy to other diseases where structural proteins are deficient, such as in extracellular matrix disorders.
In this review, we intend to present experiences with hematopoietic cell transplantation that have established its functionality and benefits for children with congenital metabolic storage diseases, and to describe some limitations and open questions regarding HCT for these conditions.
2. Conditioning regimens and graft sources
HCT for malignant as well as non-malignant diseases has traditionally been preceded by myeloablative doses of total body irradiation (TBI) and chemotherapy, or more commonly in the non-malignant setting, with myeloablative doses of busulfan combined with cyclophosphamide [3-6]. These regimens were also originally designed to be effective in treating the underlying malignancy, particularly leukemia, as well as providing intensive immunosuppression to prevent graft rejection. Although effective at achieving durable engraftment in most patients, intensive chemotherapy leads to a significant risk of short-term morbidity and a 10–30% risk of transplant-related mortality in patients with inborn errors of metabolism (IEM) [7]. Additionally, exposure to high doses of these agents can lead to a risk of significant late effects (cataracts, endocrinopathies, pulmonary and cardiac abnormalities, and new malignancies) as discussed later in this chapter. For these reasons, many parents and non-transplant physicians have been unwilling to accept the risks of HCT for children with IEM.
The demonstration that stable mixed chimerism could be achieved with sub-lethal doses of TBI (approximately one-sixth of the dose administered with standard TBI) and immunosuppression with cyclosporine and mycophenolate mofetil led to the widespread development of so-called non-myeloablative or reduced intensity conditioning regimens [8]. While these regimens were initially intended for patients who were ineligible for standard high dose conditioning, the fact that these regimens avoid many of the major short and long term toxicities associated with HCT has made this approach very attractive for use in children with non-malignant disorders. Fludarabine, a relatively new chemotherapeutic agent that has been widely used for conditioning, is highly immunosuppressive and has limited non-hematologic toxicity [9]. It has been used with low-dose TBI or without TBI in combination with busulfan, melphalan, or other agents. The use of these regimens in patients who are “chemotherapy naive” and who have normal immune systems, such as patients with IEM, has been very limited and associated with high rates of graft rejection. Additionally, measures commonly employed with reduced intensity conditioning to improve or boost engraftment, such as donor lymphocyte infusions, are associated with a high risk of acute and chronic graft vs. host disease (GVHD). Despite these issues, the use of reduced intensity conditioning in patients with IEM is a desirable goal, and research continues to refine these regimens with the objective of optimizing engraftment and minimizing toxicity.
The other consideration regarding HCT for patients with IEM is graft source. Obviously the preference is for HLA-matched sibling donors, but this is an option for only a minority of patients. The availability may be even lower for this patient group because siblings can also be affected with the disease. Certainly many of the potential matched sibling donors may be carriers of the disease in question. The question as to whether an alternative donor should be used preferentially over a sibling shown to be a carrier remains unanswered. Alternative unrelated donor sources (bone marrow, peripheral blood stem cells, cord blood) have been routinely utilized with good results. Acute and chronic GVHD is the major limitation to the use of alternative donors, and in these patients with non-malignant disorders there is no benefit to be derived from GVHD. Methods employed to reduce the risk of GVHD include T cell depletion (TCD) and possibly the use of umbilical cord blood. Both of these methods appear to be effective in reducing the risk of GVHD, but each carries with it a higher risk of graft rejection as well as a higher risk of infectious complications (particularly from viruses).
3. Lysosomal storage diseases
3.1. Mucopolysaccharidoses
Mucopolysaccharidoses are autosomal recessive disorders characterized by deficiencies of enzymes needed for the stepwise catabolism of complex sugars termed glycosaminoglycans (GAG) [10-12]. Some of these conditions predominantly affect the viscera; the others are both neuronopathic and visceral. Many of them also exhibit a dynamic range from a less severe phenotype associated with hypomorphic mutations to severe ones generally associated with null mutations.
3.1.1. Mucopolysaccharidosis type I (Hurler Syndrome)
In mucopolysaccharidosis type I (MPS I), the deficiency of α-L-iduronidase (IDUA) results in lysosomal accumulation of the GAG heparan sulfate and dermatan sulfate. This in turn leads to progressive cellular and multi-organ dysfunction. While the clinical findings may be apparent at birth, the manifestations of the disease and onset of symptoms usually occur by six months of age. Multiple organ systems are affected, and many of these patients present with or develop hepatosplenomegaly, cardiac disease, umbilical or inguinal hernia, obstructive airway disease, chronic rhinitis and otitis, skeletal deformities, hydrocephalus, neurocognitive deterioration, and corneal clouding. If left untreated, death occurs between 5 and 10 years of age, primarily from cardiac causes.
Treatments focus on approaches to replace the missing IDUA. This can be achieved either by exogenous administration of IDUA or through the endogenous production of IDUA following stable engraftment of normal cells producing enzyme within the affected individual. The former is achieved by enzyme replacement therapy (ERT) available for MPS I since 2003 [13], and the latter by HCT, which was first shown to hold promise in 1980 [2]. The therapeutic basis for both treatment options is that IDUA can be taken up by recipient cells via the mannose-6-phosphate receptor and then be translocated to lysosomes where it mediates the hydrolysis of GAG.
HCT has been accepted as a standard of care for patients with severe forms of MPS I (Hurler Syndrome). Initially, unaffected HLA-genotypically-identical bone marrow donors were considered the optimal donors, but results with matched unrelated donors, and especially with cord blood, are encouraging. As a result of better availability of improved methods for HLA typing and supportive care, the early engraftment and survival rates have improved, and currently may be as high as 85% in institutions specializing in transplantation for metabolic storage diseases [5, 14-19].
Remarkably, donor-derived cells engraft even within the brain, thereby providing a source of enzyme to the central nervous system and halting the neurocognitive decline in most patients [20]. This is in addition to correction of most of the visceral signs of pathology, including cardiovascular function, organomegaly, and lung disease. In contrast, the heart valves and skeletal abnormalities are largely unaffected by this therapy.
ERT has been introduced for treatment of less severe visceral forms of MPS I, and is currently the standard of care in patients without neurologic disease, since IDUA does not cross the blood-brain barrier [21]. Recent data on a combination of ERT with HCT are encouraging, however, and appear to support the possibility that combination therapy is in fact the new standard of care for patients with Hurler Syndrome [22-24]. The rationale for this approach is based on identifying risks in the pre-transplant course that are associated with increased morbidity and mortality during and after HCT [7]. Most prominent among these risks are upper and lower lung disease. It follows that if the enzyme can be provided for a sufficient time before transplantation, GAG storage in viscera can be partially cleared, and may result in fewer complications during HCT. The possibility that pre-transplant enzyme replacement therapy will result in increased graft failure because of generation of antibodies against donor cells has not been borne out. Of note, some advocate the use of combination therapy primarily for patients with higher risk disease. We and others, however, offer combination therapy for all patients with MPS I who are considered for HCT, because of the low risks associated with enzyme therapy and the potential that it may decrease life-threatening complications after HCT. In addition, it is possible that decreases in GAG, after enzyme replacement therapy, but before the HCT, can create a more permissive environment in the bone marrow niche for donor engraftment when compared to the patients who did not receive ERT.
3.1.2. Other mucopolysaccharidoses
In contrast to Hurler Syndrome, HCT has not been shown to significantly alter the natural history of patients with severe mucopolysaccharidosis type II (Hunter Syndrome). The attenuated phenotypes may benefit from stem cell therapy, but for yet unknown reasons, children with severe MPS II phenotype do not appear to gain neurocognitive benefit from the transplant. Whether transplantation before the onset of symptoms, such as in the neonatal period, may improve outcomes is as yet unclear.
Similarly, early results with HCT using allogeneic grafts have not been very encouraging in patients with Sanfilippo Syndrome (MPS III). Only limited published data exist regarding transplant results, but available data suggest that, in contrast to MPS I, the neurologic deterioration of MPS III patients is not alleviated by transplantation.
Morquio Syndrome (MPS IV), is characterized by significant musculoskeletal disease with less prominent neurologic changes, and so far has not been shown to benefit from HCT.
In contrast, the visceral findings of Maroteaux-Lamy Syndrome (MPS VI) have been shown to improve with HCT. However, the availability of enzyme replacement therapy for MPS VI limits the need for HCT.
Finally, Sly Syndrome (MPS VII), which results in bone deformities, developmental delays, and organomegaly, has been treated with HCT with some positive response [25-27].
Thus, individual mucopolysaccharidoses differ substantially with regards to their responses to HCT and ERT. While HCT, especially in combination with ERT, is a standard of care for severe MPS I (Hurler Syndrome), the efficacy of standard methods of transplantation for MPS II and MPS III has not been established.
4. Sphingolipidoses
The glycosphingolipids are an important component of the cell membrane, consisting of polysaccharide bound to lipid, primarily ceramide, which is incorporated into the membrane [28]. The polysaccharide portion contributes to cell interactions, adhesion, and signaling, in addition to other functions [29]. Degradation is accomplished through the action of lysosomal acid hydrolases, which serve to remove the carbohydrate moiety. Collectively the glycosphingolipid disorders are the most common cause of neurogenerative diseases (incidence approximately 1:18,000) in children [28]. With the exception of Fabry disease, these disorders are inherited in an autosomal recessive pattern. Based on the enzyme defect and substrate accumulation, these disorders are often divided into GM1 gangliosidosis, GM2 gangliosidoses (Tay-Sachs disease and Sandhoff disease), Fabry disease, multiple sulfatase deficiency, Gaucher disease, Niemann-Pick A and B, Farber disease, metachromatic leukodystrophy (MLD) and globoid cell leukodystrophy (GLD, also known as Krabbe disease). Most data regarding transplantation for these disorders relate to experience with MLD and GLD. These disorders will be discussed individually.
4.1. Metachromatic leukodystrophy
Metachromatic leukodystrophy (MLD) results from a decrease in arylsulfatase A (ARSA) activity, leading to the accumulation of the substrate cerebroside 3-sulfate, a component of myelin [30]. Decreased ARSA activity leads to demyelination of the white matter of the central nervous system (CNS) as well as the peripheral nerves [31]. Arylsulfatase A deficiency leading to MLD occurs with an overall incidence of approximately 1:40,000 births, while a higher frequency may be observed in specific populations [31-33]. There is significant phenotypic variation in MLD. In patients with the “late-infantile” form of the disease, neurological deterioration is initially observed within the first several years of life. Death generally ensues several years from diagnosis. Symptoms are associated with both central and peripheral demyelination, and motor-related difficulties are often apparent earlier than loss of cognition and language skills. The juvenile form of the disease has an onset from 4 years of age through adolescence [34-35]. Clinical manifestations of juvenile MLD are similar to the infantile form, although the rate of progression is slower. The adult form of the disease may become apparent as late as the seventh decade, and represents approximately 20% of cases of MLD [36]. Rather than presenting with motor-related difficulties, patients with late-onset disease may have emotional lability, progressive dementia, psychosis, and difficulties with substance abuse. There is a phenotype-genotype correlation in MLD, with more severe mutations resulting in more rapid accumulation of sulfatides and disease progression [37].
Krivit reported the results of the first transplant for MLD in 1990 [38]. Subsequently, reports of the success of transplantation for MLD generally have been limited to a small numbers of patients, and these data are difficult to assess due to variations in phenotype (late-infantile, juvenile, or adult forms) as well as the state of the disease at the time of transplantation [34]. Assessment of these outcomes is further limited by the lack of a universal standard for clinically assessing these patients both prior to and after transplantation. Obtaining such data will be critical to determining the utility of therapy, as asymptomatic patients or those early in their disease course are more likely to have better outcomes [16]. Similarly, those with less severe phenotypes may respond better to therapy. In regards to symptomatic late-infantile disease, while sulfatide levels decrease in urine and cerebrospinal fluid and the rate of progression may be less than observed in untreated siblings, the available data do not support the claim that transplantation has the capacity to stabilize disease [39]. The inability to deliver sufficient amounts of enzyme into the CNS is likely a primary limitation, as enzyme delivery is dependent on engraftment of cells such as the microglial population in the brain, which may take months following transplant [12, 27, 34]. In addition, despite engraftment of allogeneic cells, patients with infantile disease also appear to have progressive peripheral disease. Whether asymptomatic patients identified by neonatal screening or by family history who would be predicted to develop infantile disease can benefit from transplantation within the newborn period is debatable. Data available to address this question suggest that these patients continue to have progressive motor disabilities [34, 40-41]. In contrast, reports of the outcome of transplantation of later-onset disease (juvenile and adult forms) suggest that stabilization of the central nervous system may be achieved, even if patients are symptomatic at the time of transplantation [39,42-43]. As may be expected, the rate of decline prior to transplantation and the status of the disease at transplant are likely to affect outcomes [44].
4.2. Globoid cell leukodystrophy
The disorder known as globoid cell leukodystrophy (GLD) was initially described in 1916 by Krabbe, who reported infants developing spasticity and sclerosis of the brain [45]. Krabbe also described the characteristic “globoid cell” present in the white matter of affected patients. In 1970 the enzyme defect responsible for GLD was identified as the lysosomal enzyme galactocerebroside β-galactosidase (GALC) [46], also commonly referred to as galactocerebrosidase. In 1990 Zlotogora localized the gene to chromosome 14 [47], and the gene was cloned by Wenger’s laboratory in 1993 [48]. The primary substrate that accumulates in GLD is galactocerebroside, which is degraded by GALC to ceramide and galactose [49]. The metabolite psychosine accumulates as well in GLD, as it is a substrate for GALC [35]. Psychosine has been thought to contribute to cytotoxicity of cells in the CNS, including oligodendrocytes [50-52].
Globoid cell leukodystrophy has an incidence of 1:70,000–100,000, and presents with a varied phenotype, similar to MLD. Historically, 85–90% of patients with GLD develop symptoms as infants [35]. Patients with infantile GLD characteristically become increasingly irritable, with increased sensitivity to stimuli, developmental arrest and subsequent regression [35]. Protein levels in the cerebro-spinal fluid are high. Hypertonicity is apparent, with feeding difficulties and visual changes; increased deep tendon reflexes and seizures may be observed. Death generally results within a few years of the onset of symptoms. Other patients have less severe disease, and have been divided into late infantile (onset from 6 months to 3 years) and juvenile forms (ages 3–8 years), while some patients are not diagnosed until their second or third decades, and occasionally later [35]. As might be expected, these later onset patients have a less rapidly progressive disease course.
The first description of the outcomes of GLD patients treated by allogeneic transplantation were provided by Krivit et al in 1998 [53]. Four of the 5 patients reported had late onset disease, while one had typical infantile GLD. For the older patients, the patients appeared to stabilize, or even improve, in regards to their disease. The patient with infantile disease was transplanted at 2 months of age. By now there is sufficient experience with transplantation of symptomatic patients with infantile disease to state that transplantation is not effective at arresting disease progression, although the clinical course may be attenuated [39]. In addressing this question, Escolar reported a staging system for clinically assessing patients with GLD in the pre-transplant period, and correlated this to outcomes [54]. There has recently been great interest in the outcomes of patients with presumed infantile GLD if these patients are transplanted in the neonatal period [55]. These very young and asymptomatic patients who would be predicted to have a severe phenotype, clearly have a different clinical course after transplantation than would be expected without transplantation [56]. Based on this observation, there has been significant discussion regarding the use of newborn screening as a means of identifying these patients prior to the onset of symptoms [57, 58]. However, it remains unclear how patients who have severe genotypes and are transplanted in the first weeks of life will do as they age [55]. It is of interest that many of the difficulties these patients face are motor limitations, and this is likely at least in part due to peripheral nerve demyelination. Such a finding would be in keeping with observations in the twitcher mice, a model for GLD [59-61]. Thus far there has not been universal agreement to move towards neonatal screening for GLD with the intention of identifying and transplanting patients predicted to have severe disease soon after delivery, although screening is currently being done in New York, and is likely to be in place soon in several other US states. It should be noted that due to the severe time limitations in attempting to transplant asymptomatic neonates, a large proportion of these infants will require cord blood grafts. This has been suggested to be a preferred graft source, not only because of the expediency of moving to transplantation, but also because of the possibility of an increased ability of cord blood to transdifferentiate into a variety of non-hematopoietic stem cells or progenitor cells [16]. Additional clinical information will be required to determine if this will be the case.
The efficacy of transplantation in patients with later onset GLD remains less well delineated than would be expected. It has previously been stated that patients with later onset disease are likely to benefit from transplantation [62]. In some cases, improvement has been reported [26]. However, data related to large series of patients focused on the function and neurocognitive outcomes are not available. It would be important to review the genotypic findings of an individual diagnosed by GALC activity to determine whether it is reasonable to pursue transplantation in an asymptomatic patient, as it is not necessarily clear what the anticipated course will be. However, if a patient with later-onset disease is early in the course of the disease, transplantation seems a reasonable option. It has been suggested that for a number of these diseases, multi-institutional trials with standard methods of analysis would prove very beneficial to the field [63], and despite the difficulties inherent in developing and funding these large trials that could require decades to complete, it is difficult to argue with this view.
Other related lysosomal disorders have been treated with transplantation, although less data are available than for MLD and GLD. Niemann-Pick A and B result from a deficiency in sphingomyelinase. In Niemann-Pick A rapid neurologic progression is often observed. For these patients, who are severely affected and deteriorating rapidly, there are insufficient data to confirm that transplantation modifies the course of neurologic disease. In Niemann-Pick B, there is little published data, but our group and others have observed improvement in the marrow and lung pathology of these patients after transplant [64-65]. Niemann-Pick C has been shown to have 2 subtypes, both associated with accumulation of cholesterol. Niemann-Pick C1 is the most frequent form, but is not due to a lysosomal enzyme defect and therefore is less likely to respond to transplantation. In contrast, Niemann-Pick C2 disease is associated with a deficit in a lysosomal enzyme [66]. While it has been reported that there is an insufficient response of Niemann-Pick C to transplantation [67], the ability to separate the genotypes has only recently become available. Although it might be expected that type C2 may respond to transplantation, results have not been reported in individuals confirmed to have this genotype. As the C2 genotype is much less common than C1, genetic analysis prior to intervention will be of importance.
GM1 gangliosidosis is characterized by seizures and psychomotor deficits, and has infantile, juvenile, and adult onset forms [35, 68]. While little information is available regarding the utility of transplantation, a report describing a juvenile patient suggests there is little benefit from transplantation [69]. GM2 gangliosidosis disorders (Tay-Sachs and Sandhoff) are due to abnormalities within the hexosaminidase (HEX) gene [68]. In the case of Tay-Sachs, HEX A is deficient, while in Sandhoff HEX A and B are deficient. Unfortunately in most cases these disorders are rapidly progressive, and there is little information to suggest that symptomatic patients benefit from transplantation [40, 70]. However, it is as yet unclear as to whether those with late-onset disease or newborns predicted to have early-onset disease would benefit. Gaucher disease has been shown to benefit from transplantation [71-74], but as there is enzyme replacement therapy available for Gaucher, there is little enthusiasm for the morbidity and mortality associated with transplantation for this disorder. However, as the neuropathic form of Gaucher does not benefit from ERT [75], there may be interest in evaluating transplantation in patients with Gaucher who show evidence of neurologic deterioration [40]. Fabry disease is an X-linked disorder of the lysosomal enzyme α-galactosidase A, which results in accumulation of substrate in the kidneys, heart, eyes, and blood vessels, but does not have a significant neurological component. As enzyme replacement therapy is available for Fabry, there is currently no enthusiasm for transplantation [41].
4.3. Adrenoleukodystrophy
While GLD and MLD are autosomal recessive lysosomal enzyme deficiencies, adrenoleukodystrophy (ALD) is an X-linked disorder of the peroxisome that results in abnormal metabolism of very long chain fatty acids (VLCFA) due to decreased beta-oxidation. These VLCFA accumulate in the testes, adrenal gland, and white matter of the central nervous system [76]. For reasons that are not clear, approximately 40% of individuals with ALD under 20 years of age show a clinical course of rapid neurologic deterioration [77]. This condition, representing the cerebral form of ALD, is an inflammatory process present in the CNS, with a mixed cellular infiltrative process, although CD8+ T cells are prominent [78-79]. Eichler stated that the bulk of the inflammation occurs behind the area in which demyelination is seen, and he proposed that the infiltrative process occurs in response to demyelination rather than being its cause [80]. The beneficial effects of HCT are thought to be related at least in part to elimination of the active inflammation present in the CNS, although recent early findings of a gene therapy approach suggest that there is a corrective process provided by hematopoietically-derived cells [81]. Another important issue in regards to the early identification of ALD relates to adrenal insufficiency. Primary adrenal insufficiency (AI), or Addison’s disease, which precedes cerebral manifestations of ALD, occurs with an estimated prevalence of 43% in asymptomatic boys with X-ALD [82]. In our center’s experience, 7 boys who have been evaluated for transplantation for cerebral ALD since 2002 had previously been diagnosed with adrenal insufficiency, but VLCFA testing was not performed expeditiously, resulting in a delay in diagnosis and presumably disease progression that either rendered the patient ineligible for transplantation or put him at higher risk for a poor outcome (Polgreen et al., unpublished observations).
Transplantation early in the course of cerebral ALD has been shown to stabilize the disease process, although it is clear that in more advanced patients the outcome is inferior [4]. An MRI scoring system was developed by Loes to quantitate the extent of the disease [83], and this allows the identification of patients who are at high risk for poor outcomes of transplantation. Due to the importance of the extent of disease in the ability of transplantation to arrest the disease process [84], it is recommended that boys with biochemically proven ALD be monitored with serial MRI scans, and to proceed with transplantation when patients show evidence of early progression to cerebral disease [4]. It is not known whether transplantation plays any role in preventing the evolution of other manifestations of ALD, such as the peripheral nervous system condition termed adrenomyeloneuropathy (AMN). In addition, there are no data to show that transplantation prior to the onset of cerebral ALD will prevent its occurrence. Therefore the risks of transplantation are not justified in patients without evidence of evolving cerebral ALD, as a majority of boys will not develop cerebral ALD [85]. The use of Lorenzo’s oil in patients who have not yet developed cerebral ALD may decrease the risk of its occurrence [86].
5. Oligosaccharidosis: Mannosidosis
Alpha-mannosidosis presents with hepatosplenomegaly, vomiting, immune deficiency, and dysostosis multiplex. Affected patients also have mental retardation and ocular clouding. Approximately 20 patients have been transplanted to date, some of whom had pulmonary and airway complications during the first several months after HCT. Remarkably, the mental development as well as cardiopulmonary function appear to have been preserved, suggesting that HCT is a valid treatment option for alpha-mannosidosis [87].
6. Enzyme localization defect: Mucolipidosis Type II (I-Cell Disease)
Mucolipidosis Type II results from a defect in a phosphotransferase that is integral to the localization of numerous lysosomal hydrolyses. In the absence of this targeting mechanism, these lysosomal enzymes are secreted rather than retained in the lysosome. This results in lysosomal substrate accumulation, while extremely high serum levels of these enzymes are observed in the plasma. The phenotype resembles MPS I, but the response to HCT has been much less favorable [88]. It remains to be determined whether early identification of these patients, before the damage to visceral and neuronal tissue is irreversible and profound, and expedient transplantation may improve outcomes.
7. Late effects after HCT for Metabolic Storage Disease
As discussed previously, the majority of patients with IEM who undergo HCT do so following traditional high-dose, chemotherapy-based conditioning regimens. The combination of busulfan and cyclophosphamide is the most common regimen utilized. Patients with IEM are unique, however, in that they also have to face the potential of long-term complications related to their underlying disease that may not be reversed or prevented by successful HCT. One can assume that they are at the same risk as other patients going through HCT for the common conditions seen after exposure to high-dose chemotherapy in the conditioning regimen, but there are little data that describe those findings. Additionally, there may be unique long-term effects of some of the preparative regimens in patients with IEM, but again for the most part these have not been reported to date. Limited long-term follow-up data in some subsets of IEM patients (Hurler’s syndrome in particular) related to amelioration of disease-associated conditions are available and will be briefly summarized.
Endocrine issues. There are minimal IEM-specific data, but some patients have been found to have primary ovarian failure [19]. It is unclear if this is related to the disease or HCT since both may contribute. Other endocrine issues seen in children after HCT include gonadal failure in males, hypothyroidism, and growth failure. While some of these conditions may be more frequently encountered after exposure to TBI, they can also be seen with non-TBI containing regimens. Patients with Hurler’s syndrome have growth problems to begin with, and while some reports suggest that linear growth may be maintained early after HCT, others suggest growth may not be maintained on a long-term basis [19, 89].
Pulmonary. Patients with IEM have high rates of pulmonary complications during HCT that may be related to a pro-inflammatory state within the lung [90]. While busulfan can lead to pulmonary fibrosis, this is not a common complication in children after HCT. In patients with Hurler’s it has been demonstrated that they do have relief of their obstructive airway symptoms and improvement in sleep apnea with improved pulmonary function [19, 91]. A reduction in the risk of pulmonary deterioration in a patient successfully transplanted for I-cell disease has also been reported [92].
Cardiac. Long-term cardiovascular complications are rarely associated with exposure to cyclophosphamide and busulfan alone. Certainly for several of the IEM disorders, progressive cardiac dysfunction is common. For patients with Hurler’s, long-term follow-up after HCT has shown that myocardial function is preserved and hypertrophy has been seen to regress, and patients have not developed heart failure or coronary artery disease. However, mitral and aortic valve deformities have persisted and frequently progressed [93].
Neuropsychological and cognitive function. In the absence of exposure to radiation during conditioning, children typically do not have significant neuropsychological sequelae secondary to HCT. In the case of children with IEM, post-HCT neurologic outcome depends upon the specific disease, age at time of HCT, specific genotype of the disease, cognitive status at the time of HCT, engraftment status, and donor enzyme activity after HCT. The goal, of course, is to perform HCT early in the course of the disease before any extensive neurologic damage or deterioration has occurred. When this can be done, neurocognitive function can be stabilized (or in some cases improved) and further progressive neurologic deterioration can be prevented [5, 19, 89,91, 94].
Bone and joints. HCT conditioning can affect bone health leading to osteopenia and osteoporosis. This may be reversible on its own over time or may require further intervention with vitamin D and calcium supplementation or occasionally treatment with bisphosphonates. These effects have not been studied to date in children with IEM. Other disease-specific orthopedic complications, such as odontoid dysplasia in patients with Hurler’s, have been shown to improve over time [95]. However, other complications such as genu valgum, carpel tunnel syndrome, and acetabular dysplasia have not improved after HCT and frequently require surgical intervention [96-97].
Post-transplant malignancies. It has been well described that patients after HCT are at life-long increased risk of developing malignancies that is estimated at nearly 10-fold greater than that in the general population [98-99]. Whether this same risk applies to patients with IEM is not known, but we are aware of some patients who have developed malignancies years after HCT.
Late Mortality. After allogeneic HCT patients have twice the risk of mortality of the general population [100]. Data submitted for publication from the Center for International Blood and Marrow Transplant Research demonstrate that patients with IEM have a higher risk of mortality between 2–6 yrs after HCT and that this increased risk persists even 6 yrs after HCT. This increased risk is highest in patients who have received unrelated or HLA non-identical related donor transplants. Causes of death include GVHD, infection, and organ failure.
Summary
Obtaining clear data regarding the outcomes of transplantation in patients with IEM has proven difficult due to the rarity of these diseases, their variable phenotypes/genotypes, and differences in stem cell sources, preparative regimens, supportive therapy, and assessment of “successful” outcomes. Multi-institution trials with a common approach and outcome measures will be important in this regard. In earlier years HCT in these populations used standardized regimens designed for patients with malignant disorders. For disorders such as Hurler’s syndrome and early cerebral ALD, this approach has been successful. However, for other disorders, the ability to achieve satisfactory outcomes with standard transplant regimens has proven elusive. Reduced-intensity conditioning strategies may prove more successful in decreasing morbidity and mortality, particularly in patients with ongoing neurologic injury. It is anticipated that future investigations will test the use of combination therapy with or without transplantation, including substrate inhibition [101-102], chaperone therapy [103-105], enzyme replacement [24, 106], modification of anti-inflammatory therapy [107], or biologic response modifiers [108-110]. In addition, the interest in neonatal screening will provide the opportunity to intervene early in the course of these diseases, as this appears critical in achieving optimal outcomes [4, 111-114]. Finally, modifying the transplant procedure, using selectively expanded cell populations, or using cytokine manipulation may enhance microglial engraftment [115-118], which could make a substantial difference in the delivery of enzyme to the CNS. Significant progress is required to enhance transplant results and to determine optimal therapy in individuals with these devastating congenital disorders.
References
1. Fratantoni JC, Hall CW, Neufeld EF. Hurler and Hunter syndromes: mutual correction of the defect in cultured fibroblasts. Science. 1968;162:570-572.
2. Hobbs JR, Hugh-Jones K, Barrett AJ, et al. Reversal of clinical features of Hurler's disease and biochemical improvement after treatment by bone-marrow transplantation. Lancet. 1981;2:709-712.
3. Jacobson P, Park JJ, DeFor TE, et al. Oral busulfan pharmacokinetics and engraftment in children with Hurler syndrome and other inherited metabolic storage diseases undergoing hematopoietic cell transplantation. Bone Marrow Transplant. 2001;27:855-861.
4. Peters C, Charnas LR, Tan Y, et al. Cerebral X-linked adrenoleukodystrophy: the international hematopoietic cell transplantation experience from 1982 to 1999. Blood. 2004;104:881-888.
5. Peters C, Shapiro EG, Anderson J, et al. Hurler syndrome: II. Outcome of HLA-genotypically identical sibling and HLA-haploidentical related donor bone marrow transplantation in fifty-four children. The Storage Disease Collaborative Study Group. Blood. 1998;91:2601-2608.
6. Peters C, Balthazor M, Shapiro EG, et al. Outcome of unrelated donor bone marrow transplantation in 40 children with Hurler syndrome. Blood. 1996;87:4894-4902.
10. Neufeld EF. Lysosomal storage diseases. Annu Rev Biochem. 1991;60:257-280.
11. Muenzer J. The mucopolysaccharidoses: a heterogeneous group of disorders with variable pediatric presentations. J Pediatr. 2004;144:S27-34.
12. Orchard PJ, Blazar BR, Wagner J, Charnas L, Krivit W, Tolar J. Hematopoietic cell therapy for metabolic disease. J Pediatr. 2007;151:340-346.
13. Kakkis ED, Muenzer J, Tiller GE, et al. Enzyme-replacement therapy in mucopolysaccharidosis I. N Engl J Med. 2001;344:182-188.
14. Boelens JJ, Rocha V, Aldenhoven M, et al. Risk factor analysis of outcomes after unrelated cord blood transplantation in patients with hurler syndrome. Biol Blood Marrow Transplant. 2009;15:618-625.
15. Aldenhoven M, Boelens JJ, de Koning TJ. The clinical outcome of Hurler syndrome after stem cell transplantation. Biol Blood Marrow Transplant. 2008;14:485-498.
16. Prasad VK, Kurtzberg J. Cord blood and bone marrow transplantation in inherited metabolic diseases: scientific basis, current status and future directions. Br J Haematol. 2009.
17. Prasad VK, Kurtzberg J. Umbilical cord blood transplantation for non-malignant diseases. Bone Marrow Transplant. 2009;44:643-651.
18. Prasad VK, Mendizabal A, Parikh SH, et al. Unrelated donor umbilical cord blood transplantation for inherited metabolic disorders in 159 pediatric patients from a single center: influence of cellular composition of the graft on transplantation outcomes. Blood. 2008;112:2979-2989.
19. Vellodi A, Young EP, Cooper A, et al. Bone marrow transplantation for mucopolysaccharidosis type I: experience of two British centres. Arch Dis Child. 1997;76:92-99.
20. Krivit W, Sung JH, Shapiro EG, Lockman LA. Microglia: the effector cell for reconstitution of the central nervous system following bone marrow transplantation for lysosomal and peroxisomal storage diseases. Cell Transplant. 1995;4:385-392.
21. Wraith JE. The first 5 years of clinical experience with laronidase enzyme replacement therapy for mucopolysaccharidosis I. Expert Opin Pharmacother. 2005;6:489-506.
22. Wynn RF, Mercer J, Page J, Carr TF, Jones S, Wraith JE. Use of enzyme replacement therapy (Laronidase) before hematopoietic stem cell transplantation for mucopolysaccharidosis I: experience in 18 patients. J Pediatr. 2009;154:135-139.
23. Cox-Brinkman J, Boelens JJ, Wraith JE, et al. Haematopoietic cell transplantation (HCT) in combination with enzyme replacement therapy (ERT) in patients with Hurler syndrome. Bone Marrow Transplant. 2006;38:17-21.
24. Tolar J, Grewal SS, Bjoraker KJ, et al. Combination of enzyme replacement and hematopoietic stem cell transplantation as therapy for Hurler syndrome. Bone Marrow Transplant. 2008;41:531-535.
25. Klein KA, Krivit W, Whitley CB, et al. Poor cognitive outcome of eleven children with Sanfilippo syndrome after bone marrow transplantation and successful engraftment. Bone Marrow Transplant. 1995;15:S176-181.
26. Krivit W. Allogeneic stem cell transplantation for the treatment of lysosomal and peroxisomal metabolic diseases. Springer Semin Immunopathol. 2004;26:119-132.
27. Peters C, Krivit W. Hematopoietic cell transplantation for mucopolysaccharidosis IIB (Hunter syndrome). Bone Marrow Transplant. 2000;25:1097-1099.
29. Watts RW. A historical perspective of the glycosphingolipids and sphingolipidoses. Philos Trans R Soc Lond B Biol Sci. 2003;358:975-983.
30. Gieselmann V, Polten A, Kreysing J, von Figura K. Molecular genetics of metachromatic leukodystrophy. J Inherit Metab Dis. 1994;17:500-509.
31. Eng B, Nakamura LN, O'Reilly N, et al. Identification of nine novel arylsulfatase a (ARSA) gene mutations in patients with metachromatic leukodystrophy (MLD). Hum Mutat. 2003;22:418-419.
32. Heinisch U, Zlotogora J, Kafert S, Gieselmann V. Multiple mutations are responsible for the high frequency of metachromatic leukodystrophy in a small geographic area. Am J Hum Genet. 1995;56:51-57.
33. Zlotogora J, Bach G, Bosenberg C, Barak Y, von Figura K, Gieselmann V. Molecular basis of late infantile metachromatic leukodystrophy in the Habbanite Jews. Hum Mutat. 1995;5:137-143.
34. Biffi A, Lucchini G, Rovelli A, Sessa M. Metachromatic leukodystrophy: an overview of current and prospective treatments. Bone Marrow Transplant. 2008;42 Suppl 2:S2-6.
35. Scriver CR, Beaudet AL, Sly WS, Valle D. The Metabolic and Molecular Bases of Inherited Disease. Vol. III (ed 8th). New York: McGraw-Hill; 2001.
36. Sedel F, Tourbah A, Fontaine B, et al. Leukoencephalopathies associated with inborn errors of metabolism in adults. J Inherit Metab Dis. 2008;31:295-307.
37. Gieselmann V. Metachromatic leukodystrophy: genetics, pathogenesis and therapeutic options. Acta Paediatr Suppl. 2008;97:15-21.
38. Krivit W, Shapiro E, Kennedy W, et al. Treatment of late infantile metachromatic leukodystrophy by bone marrow transplantation. N Engl J Med. 1990;322:28-32.
39. Krivit W, Aubourg P, Shapiro E, Peters C. Bone marrow transplantation for globoid cell leukodystrophy, adrenoleukodystrophy, metachromatic leukodystrophy, and Hurler syndrome. Curr Opin Hematol. 1999;6:377-382.
40. Peters C, Steward CG. Hematopoietic cell transplantation for inherited metabolic diseases: an overview of outcomes and practice guidelines. Bone Marrow Transplant. 2003;31:229-239.
41. Peters C. Hematopoietic Stem Cell Transplantation for Storage Diseases. In: Appelbaum FR, Forman SJ, Negrin RS, eds. Thomas' Hematopoietic Cell Transplantation: Stem Cell Transplantation (ed 4). Oxford, UK: Wiley, John & Sons, Incorporated; 2009:1136-1162.
42. Gorg M, Wilck W, Granitzny B, et al. Stabilization of juvenile metachromatic leukodystrophy after bone marrow transplantation: a 13-year follow-up. J Child Neurol. 2007;22:1139-1142.
43. Solders G, Celsing G, Hagenfeldt L, Ljungman P, Isberg B, Ringden O. Improved peripheral nerve conduction, EEG and verbal IQ after bone marrow transplantation for adult metachromatic leukodystrophy. Bone Marrow Transplant. 1998;22:1119-1122.
44. Pierson TM, Bonnemann CG, Finkel RS, Bunin N, Tennekoon GI. Umbilical cord blood transplantation for juvenile metachromatic leukodystrophy. Ann Neurol. 2008;64:583-587.
45. Krabbe K. A new familial, infantile form of diffuse brain sclerosis. Brain. 1916;39:74-114.
46. Suzuki K, Suzuki Y. Globoid cell leucodystrophy (Krabbe's disease): deficiency of galactocerebroside beta-galactosidase. Proc Natl Acad Sci U S A. 1970;66:302-309.
48. Chen YQ, Rafi MA, de Gala G, Wenger DA. Cloning and expression of cDNA encoding human galactocerebrosidase, the enzyme deficient in globoid cell leukodystrophy. Hum Mol Genet. 1993;2:1841-1845.
49. Tatsumi N, Inui K, Sakai N, et al. Molecular defects in Krabbe disease. Hum Mol Genet. 1995;4:1865-1868.
50. Igisu H, Suzuki K. Progressive accumulation of toxic metabolite in a genetic leukodystrophy. Science. 1984;224:753-755.
51. Suzuki K. Twenty five years of the "psychosine hypothesis": a personal perspective of its history and present status. Neurochem Res. 1998;23:251-259.
52. White AB, Givogri MI, Lopez-Rosas A, et al. Psychosine accumulates in membrane microdomains in the brain of krabbe patients, disrupting the raft architecture. J Neurosci. 2009;29:6068-6077.
55. Duffner PK, Caviness VS, Jr., Erbe RW, et al. The long-term outcomes of presymptomatic infants transplanted for Krabbe disease: Report of the workshop held on July 11 and 12, 2008, Holiday Valley, New York. Genet Med. 2009.
57. Duffner PK, Caggana M, Orsini JJ, et al. Newborn screening for Krabbe disease: the New York State model. Pediatr Neurol. 2009;40:245-252; discussion 253-245.
58. Meikle PJ, Grasby DJ, Dean CJ, et al. Newborn screening for lysosomal storage disorders. Mol Genet Metab. 2006;88:307-314.
59. Kagitani-Shimono K, Mohri I, Yagi T, Taniike M, Suzuki K. Peripheral neuropathy in the twitcher mouse: accumulation of extracellular matrix in the endoneurium and aberrant expression of ion channels. Acta Neuropathol. 2008;115:577-587.
60. Kondo A, Hoogerbrugge PM, Suzuki K, Poorthuis BJ, Van Bekkum DW. Pathology of the peripheral nerve in the twitcher mouse following bone marrow transplantation. Brain Res. 1988;460:178-183.
61. Luzi P, Rafi MA, Zaka M, et al. Biochemical and pathological evaluation of long-lived mice with globoid cell leukodystrophy after bone marrow transplantation. Mol Genet Metab. 2005;86:150-159.
63. Cartier N, Aubourg P. Hematopoietic stem cell gene therapy in Hurler syndrome, globoid cell leukodystrophy, metachromatic leukodystrophy and X-adrenoleukodystrophy. Curr Opin Mol Ther. 2008;10:471-478.
64. Victor S, Coulter JB, Besley GT, et al. Niemann-Pick disease: sixteen-year follow-up of allogeneic bone marrow transplantation in a type B variant. J Inherit Metab Dis. 2003;26:775-785.
65. Shah AJ, Kapoor N, Crooks GM, et al. Successful hematopoietic stem cell transplantation for Niemann-Pick disease type B. Pediatrics. 2005;116:1022-1025.
66. Walkley SU, Suzuki K. Consequences of NPC1 and NPC2 loss of function in mammalian neurons. Biochim Biophys Acta. 2004;1685:48-62.
68. Walkley SU. Secondary accumulation of gangliosides in lysosomal storage disorders. Semin Cell Dev Biol. 2004;15:433-444.
69. Shield JP, Stone J, Steward CG. Bone marrow transplantation correcting beta-galactosidase activity does not influence neurological outcome in juvenile GM1-gangliosidosis. J Inherit Metab Dis. 2005;28:797-798.
71. Starer F, Sargent JD, Hobbs JR. Regression of the radiological changes of Gaucher's disease following bone marrow transplantation. Br J Radiol. 1987;60:1189-1195.
72. Ringden O, Groth CG, Erikson A, et al. Long-term follow-up of the first successful bone marrow transplantation in Gaucher disease. Transplantation. 1988;46:66-70.
73. Svennerholm L, Erikson A, Groth CG, Ringden O, Mansson JE. Norrbottnian type of Gaucher disease--clinical, biochemical and molecular biology aspects: successful treatment with bone marrow transplantation. Dev Neurosci. 1991;13:345-351.
74. Tsai P, Lipton JM, Sahdev I, et al. Allogenic bone marrow transplantation in severe Gaucher disease. Pediatr Res. 1992;31:503-507.
75. Goker-Alpan O, Wiggs EA, Eblan MJ, et al. Cognitive outcome in treated patients with chronic neuronopathic Gaucher disease. J Pediatr. 2008;153:89-94.
76. Krasemann EW, Meier V, Korenke GC, Hunneman DH, Hanefeld F. Identification of mutations in the ALD-gene of 20 families with adrenoleukodystrophy/adrenomyeloneuropathy. Hum Genet. 1996;97:194-197.
77. Berger J, Gartner J. X-linked adrenoleukodystrophy: clinical, biochemical and pathogenetic aspects. Biochim Biophys Acta. 2006;1763:1721-1732.
78. Ito M, Blumberg BM, Mock DJ, et al. Potential environmental and host participants in the early white matter lesion of adreno-leukodystrophy: morphologic evidence for CD8 cytotoxic T cells, cytolysis of oligodendrocytes, and CD1-mediated lipid antigen presentation. J Neuropathol Exp Neurol. 2001;60:1004-1019.
79. Powers JM, Moser HW, Moser AB, Ma CK, Elias SB, Norum RA. Pathologic findings in adrenoleukodystrophy heterozygotes. Arch Pathol Lab Med. 1987;111:151-153.
80. Eichler F, Van Haren K. Immune response in leukodystrophies. Pediatr Neurol. 2007;37:235-244.
81. Cartier N, Hacein-Bey-Abina S, Bartholomae CC, et al. Hematopoietic stem cell gene therapy with a lentiviral vector in X-linked adrenoleukodystrophy. Science. 2009;326:818-823.
82. Dubey P, Raymond GV, Moser AB, Kharkar S, Bezman L, Moser HW. Adrenal insufficiency in asymptomatic adrenoleukodystrophy patients identified by very long-chain fatty acid screening. J Pediatr. 2005;146:528-532.
83. Loes DJ, Fatemi A, Melhem ER, et al. Analysis of MRI patterns aids prediction of progression in X-linked adrenoleukodystrophy. Neurology. 2003;61:369-374.
84. Mahmood A, Raymond GV, Dubey P, Peters C, Moser HW. Survival analysis of haematopoietic cell transplantation for childhood cerebral X-linked adrenoleukodystrophy: a comparison study. Lancet Neurol. 2007;6:687-692.
85. Mahmood A, Dubey P, Moser HW, Moser A. X-linked adrenoleukodystrophy: Therapeutic approaches to distinct phenotypes. Pediatr Transplant. 2005;9:55-62.
87. Grewal SS, Shapiro EG, Krivit W, et al. Effective treatment of alpha-mannosidosis by allogeneic hematopoietic stem cell transplantation. J Pediatr. 2004;144:569-573.
91. Whitley CB, Belani KG, Chang PN, et al. Long-term outcome of Hurler syndrome following bone marrow transplantation. Am J Med Genet. 1993;46:209-218.
93. Braunlin EA, Stauffer NR, Peters CH, et al. Usefulness of bone marrow transplantation in the Hurler syndrome. Am J Cardiol. 2003;92:882-886.
94. Shapiro EG, Lockman LA, Balthazor M, Krivit W. Neuropsychological outcomes of several storage diseases with and without bone marrow transplantation. J Inherit Metab Dis. 1995;18:413-429.
95. Hite SH, Peters C, Krivit W. Correction of odontoid dysplasia following bone-marrow transplantation and engraftment (in Hurler syndrome MPS 1H). Pediatr Radiol. 2000;30:464-470.
96. Field RE, Buchanan JA, Copplemans MG, Aichroth PM. Bone-marrow transplantation in Hurler's syndrome. Effect on skeletal development. J Bone Joint Surg Br. 1994;76:975-981.
97. Wraith JE, Alani SM. Carpal tunnel syndrome in the mucopolysaccharidoses and related disorders. Arch Dis Child. 1990;65:962-963.
98. Baker KS, DeFor TE, Burns LJ, Ramsay NK, Neglia JP, Robison LL. New malignancies after blood or marrow stem-cell transplantation in children and adults: incidence and risk factors. J Clin Oncol. 2003;21:1352-1358.
99. Bhatia S, Ramsay NK, Steinbuch M, et al. Malignant neoplasms following bone marrow transplantation. Blood. 1996;87:3633-3639.
101. Desnick RJ. Enzyme replacement and enhancement therapies for lysosomal diseases. J Inherit Metab Dis. 2004;27:385-410.
102. Cox TM. Substrate reduction therapy for lysosomal storage diseases. Acta Paediatr Suppl. 2005;94:69-75; discussion 57.
103. Gregersen N, Bolund L, Bross P. Protein misfolding, aggregation, and degradation in disease. Mol Biotechnol. 2005;31:141-150.
104. Desnick RJ, Schuchman EH. Enzyme replacement and enhancement therapies: lessons from lysosomal disorders. Nat Rev Genet. 2002;3:954-966.
105. Hoffmann B, Mayatepek E. Neurological manifestations in lysosomal storage disorders - from pathology to first therapeutic possibilities. Neuropediatrics. 2005;36:285-289.
106. Vellodi A. Lysosomal storage disorders. Br J Haematol. 2005;128:413-431.
108. Spagnoli A, Longobardi L, O'Rear L. Cartilage disorders: potential therapeutic use of mesenchymal stem cells. Endocr Dev. 2005;9:17-30.
109. Young PP, Fantz CR, Sands MS. VEGF disrupts the neonatal blood-brain barrier and increases life span after non-ablative BMT in a murine model of congenital neurodegeneration caused by a lysosomal enzyme deficiency. Exp Neurol. 2004;188:104-114.
110. Zaka M, Rafi MA, Rao HZ, Luzi P, Wenger DA. Insulin-like growth factor-1 provides protection against psychosine-induced apoptosis in cultured mouse oligodendrocyte progenitor cells using primarily the PI3K/Akt pathway. Mol Cell Neurosci. 2005;30:398-407.
111. Li Y, Scott CR, Chamoles NA, et al. Direct multiplex assay of lysosomal enzymes in dried blood spots for newborn screening. Clin Chem. 2004;50:1785-1796.
112. Meikle PJ, Ranieri E, Simonsen H, et al. Newborn screening for lysosomal storage disorders: clinical evaluation of a two-tier strategy. Pediatrics. 2004;114:909-916.
113. Millington DS. Newborn screening for lysosomal storage disorders. Clin Chem. 2005;51:808-809.
114. Staba SL, Escolar ML, Poe M, et al. Cord-blood transplants from unrelated donors in patients with Hurler's syndrome. N Engl J Med. 2004;350:1960-1969.
115. Davoust N, Vuaillat C, Androdias G, Nataf S. From bone marrow to microglia: barriers and avenues. Trends Immunol. 2008;29:227-234.
116. D'Mello C, Le T, Swain MG. Cerebral microglia recruit monocytes into the brain in response to tumor necrosis factoralpha signaling during peripheral organ inflammation. J Neurosci. 2009;29:2089-2102.
117. Hall AA, Herrera Y, Ajmo CT, Jr., Cuevas J, Pennypacker KR. Sigma receptors suppress multiple aspects of microglial activation. Glia. 2009;57:744-754.
118. Semple BD, Bye N, Rancan M, Ziebell JM, Morganti-Kossmann MC. Role of CCL2 (MCP-1) in traumatic brain injury (TBI): evidence from severe TBI patients and CCL2-/- mice. J Cereb Blood Flow Metab. 2009.
Якуб Толар, К.Скотт Бэйкер, Пол Дж. Орчард
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18998" ["VALUE"]=> array(2) { ["TEXT"]=> string(5243) "<p class="bodytext">В данной обзорной статье представлены сведения о трансплантации гемопоэтических стволовых клеток (ТГСК) у детей с врожденными метаболическими болезнями накопления (ВМБН), и о нерешенных вопросах ТГСК при этих состояниях. Обсуждаются как миелоаблативные, так и менее интенсивные режимы кондиционирования. Показана выгода стандартизированного подхода к ТГСК при болезни Хурлера и ранней адренолейкодистрофии (АЛД) головного мозга. Режимы кондиционирования со сниженной интенсивностью могут оказаться более успешными в плане снижения смертности и развития осложнений, особенно у больных с развивающимся неврологическим дефектом. В ситуациях с ТГСК при наследственных заболеваниях можно ожидать, что потенциальные доноры-сибсы могут быть носителями мутации данного гена. Нерешенная проблема состоит в том, может ли альтернативный донор иметь преимущество в сравнении с сибсом, который может быть носителем заболевания. Обычно применяют стволовые неродственные донорские клетки из различных источников (костного мозга, периферических клеток, пуповинной крови) с хорошими результатами. Рассматривается эффективность энзим-заместительной терапии по сравнению с ТГСК в качестве подходящего лечения при менее тяжелых формах мукополисахаридозов (МПС), и ТГСК признано стандартом терапии для больных с тяжелыми клиническими формами МПС типа I. В противоположность синдрому Хурлера, ТГСК не выявила существенного влияния у больных с тяжелым МПС типа II (синдром Хантера), т.е. дети с тяжелой формой МПС типа II, по-видимому, не имеют преимуществ в нейрокогнитивном развитии при ТГСК. Что касается метахроматической или глобоидноклеточной лейкодистрофии, то данные об эффективности ТГСК здесь более скудные. Получение четких данных об исходах ТГСК у больных с ВМБН оказалось сложной задачей из-за редкости этих заболеваний, вариабельности их генотипов и фенотипов, различий в источниках стволовых клеток, кондиционирующих режимах и оценке «успешных» результатов. Дальнейшие исследования установят полезность комбинированной терапии с/без трансплантации, включая субстратное ингибирование, терапию шаперонами, энзимотерапию и т.д. Кроме того, интерес к неонатальному скринингу обеспечит раннее вмешательство в течение этих болезней, т.к. это очень важно для получения оптимальных результатов. Наконец, модификация процедуры ТГСК или применение селективно размножающихся клеточных популяций, или обработка цитокинами могут усилить приживление микроглии, что может существенно облегчить достаку энзимов в центральную нервную систему. В это отношении будут важны многоцентровые исследования с общим подходом и оценкой клинических исходов. </p> <h3>Ключевые слова</h3> <p>наследственные болезни накопления, мукополисахаридозы, трансплантация гемопоэтических клеток, режимы кондиционирования, клинический эффект </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(5197) "В данной обзорной статье представлены сведения о трансплантации гемопоэтических стволовых клеток (ТГСК) у детей с врожденными метаболическими болезнями накопления (ВМБН), и о нерешенных вопросах ТГСК при этих состояниях. Обсуждаются как миелоаблативные, так и менее интенсивные режимы кондиционирования. Показана выгода стандартизированного подхода к ТГСК при болезни Хурлера и ранней адренолейкодистрофии (АЛД) головного мозга. Режимы кондиционирования со сниженной интенсивностью могут оказаться более успешными в плане снижения смертности и развития осложнений, особенно у больных с развивающимся неврологическим дефектом. В ситуациях с ТГСК при наследственных заболеваниях можно ожидать, что потенциальные доноры-сибсы могут быть носителями мутации данного гена. Нерешенная проблема состоит в том, может ли альтернативный донор иметь преимущество в сравнении с сибсом, который может быть носителем заболевания. Обычно применяют стволовые неродственные донорские клетки из различных источников (костного мозга, периферических клеток, пуповинной крови) с хорошими результатами. Рассматривается эффективность энзим-заместительной терапии по сравнению с ТГСК в качестве подходящего лечения при менее тяжелых формах мукополисахаридозов (МПС), и ТГСК признано стандартом терапии для больных с тяжелыми клиническими формами МПС типа I. В противоположность синдрому Хурлера, ТГСК не выявила существенного влияния у больных с тяжелым МПС типа II (синдром Хантера), т.е. дети с тяжелой формой МПС типа II, по-видимому, не имеют преимуществ в нейрокогнитивном развитии при ТГСК. Что касается метахроматической или глобоидноклеточной лейкодистрофии, то данные об эффективности ТГСК здесь более скудные. Получение четких данных об исходах ТГСК у больных с ВМБН оказалось сложной задачей из-за редкости этих заболеваний, вариабельности их генотипов и фенотипов, различий в источниках стволовых клеток, кондиционирующих режимах и оценке «успешных» результатов. Дальнейшие исследования установят полезность комбинированной терапии с/без трансплантации, включая субстратное ингибирование, терапию шаперонами, энзимотерапию и т.д. Кроме того, интерес к неонатальному скринингу обеспечит раннее вмешательство в течение этих болезней, т.к. это очень важно для получения оптимальных результатов. Наконец, модификация процедуры ТГСК или применение селективно размножающихся клеточных популяций, или обработка цитокинами могут усилить приживление микроглии, что может существенно облегчить достаку энзимов в центральную нервную систему. В это отношении будут важны многоцентровые исследования с общим подходом и оценкой клинических исходов.
Ключевые слова
наследственные болезни накопления, мукополисахаридозы, трансплантация гемопоэтических клеток, режимы кондиционирования, клинический эффект
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18999" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000075.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000075.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19005" ["VALUE"]=> array(2) { ["TEXT"]=> string(170) "<p>Jakub Tolar, M.D., Ph.D.<sup>1</sup>, K. Scott Baker, M.D.<sup>2</sup>, Paul J. Orchard, M.D.<sup>1</sup></p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(122) "Jakub Tolar, M.D., Ph.D.1, K. Scott Baker, M.D.2, Paul J. Orchard, M.D.1
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19006" ["VALUE"]=> array(2) { ["TEXT"]=> string(320) "<p class="bodytext"><sup>1</sup>Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; <sup>2</sup>Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(274) "1Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; 2Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19007" ["VALUE"]=> array(2) { ["TEXT"]=> string(1514) "<p class="bodytext">Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.</p> <h3>Keywords</h3> <p> hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1468) "Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.
Keywords
hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19000" ["VALUE"]=> string(70) "Hematopoietic stem cell transplantation for metabolic storage diseases" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(70) "Hematopoietic stem cell transplantation for metabolic storage diseases" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19001" ["VALUE"]=> string(3) "916" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "916" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19011" ["VALUE"]=> string(3) "917" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "917" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(12) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19005" ["VALUE"]=> array(2) { ["TEXT"]=> string(170) "<p>Jakub Tolar, M.D., Ph.D.<sup>1</sup>, K. Scott Baker, M.D.<sup>2</sup>, Paul J. Orchard, M.D.<sup>1</sup></p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(122) "Jakub Tolar, M.D., Ph.D.1, K. Scott Baker, M.D.2, Paul J. Orchard, M.D.1
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(122) "Jakub Tolar, M.D., Ph.D.1, K. Scott Baker, M.D.2, Paul J. Orchard, M.D.1
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19007" ["VALUE"]=> array(2) { ["TEXT"]=> string(1514) "<p class="bodytext">Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.</p> <h3>Keywords</h3> <p> hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1468) "Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.
Keywords
hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1468) "Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.
Keywords
hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18999" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000075.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000075.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2010-en-000075.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19000" ["VALUE"]=> string(70) "Hematopoietic stem cell transplantation for metabolic storage diseases" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(70) "Hematopoietic stem cell transplantation for metabolic storage diseases" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(70) "Hematopoietic stem cell transplantation for metabolic storage diseases" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19006" ["VALUE"]=> array(2) { ["TEXT"]=> string(320) "<p class="bodytext"><sup>1</sup>Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; <sup>2</sup>Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(274) "1Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; 2Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(274) "1Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; 2Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(3) { [0]=> string(5) "19012" [1]=> string(5) "19013" [2]=> string(5) "19014" } ["VALUE"]=> array(3) { [0]=> string(4) "1429" [1]=> string(4) "1291" [2]=> string(4) "1430" } ["DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(3) { [0]=> string(4) "1429" [1]=> string(4) "1291" [2]=> string(4) "1430" } ["~DESCRIPTION"]=> array(3) { [0]=> string(0) "" [1]=> string(0) "" [2]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(3) { [0]=> string(55) "Jakub Tolar" [1]=> string(58) "K. Scott Baker" [2]=> string(59) "Paul J. Orchard" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18997" ["VALUE"]=> array(2) { ["TEXT"]=> string(93) "<p>Якуб Толар, К.Скотт Бэйкер, Пол Дж. Орчард</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(81) "Якуб Толар, К.Скотт Бэйкер, Пол Дж. Орчард
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(81) "Якуб Толар, К.Скотт Бэйкер, Пол Дж. Орчард
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18990" ["VALUE"]=> string(22) "01/11/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/11/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/11/2010 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18991" ["VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/25/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18992" ["VALUE"]=> string(22) "03/22/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "03/22/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "03/22/2010 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18993" ["VALUE"]=> string(4) "1429" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1429" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(55) "Jakub Tolar" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18998" ["VALUE"]=> array(2) { ["TEXT"]=> string(5243) "<p class="bodytext">В данной обзорной статье представлены сведения о трансплантации гемопоэтических стволовых клеток (ТГСК) у детей с врожденными метаболическими болезнями накопления (ВМБН), и о нерешенных вопросах ТГСК при этих состояниях. Обсуждаются как миелоаблативные, так и менее интенсивные режимы кондиционирования. Показана выгода стандартизированного подхода к ТГСК при болезни Хурлера и ранней адренолейкодистрофии (АЛД) головного мозга. Режимы кондиционирования со сниженной интенсивностью могут оказаться более успешными в плане снижения смертности и развития осложнений, особенно у больных с развивающимся неврологическим дефектом. В ситуациях с ТГСК при наследственных заболеваниях можно ожидать, что потенциальные доноры-сибсы могут быть носителями мутации данного гена. Нерешенная проблема состоит в том, может ли альтернативный донор иметь преимущество в сравнении с сибсом, который может быть носителем заболевания. Обычно применяют стволовые неродственные донорские клетки из различных источников (костного мозга, периферических клеток, пуповинной крови) с хорошими результатами. Рассматривается эффективность энзим-заместительной терапии по сравнению с ТГСК в качестве подходящего лечения при менее тяжелых формах мукополисахаридозов (МПС), и ТГСК признано стандартом терапии для больных с тяжелыми клиническими формами МПС типа I. В противоположность синдрому Хурлера, ТГСК не выявила существенного влияния у больных с тяжелым МПС типа II (синдром Хантера), т.е. дети с тяжелой формой МПС типа II, по-видимому, не имеют преимуществ в нейрокогнитивном развитии при ТГСК. Что касается метахроматической или глобоидноклеточной лейкодистрофии, то данные об эффективности ТГСК здесь более скудные. Получение четких данных об исходах ТГСК у больных с ВМБН оказалось сложной задачей из-за редкости этих заболеваний, вариабельности их генотипов и фенотипов, различий в источниках стволовых клеток, кондиционирующих режимах и оценке «успешных» результатов. Дальнейшие исследования установят полезность комбинированной терапии с/без трансплантации, включая субстратное ингибирование, терапию шаперонами, энзимотерапию и т.д. Кроме того, интерес к неонатальному скринингу обеспечит раннее вмешательство в течение этих болезней, т.к. это очень важно для получения оптимальных результатов. Наконец, модификация процедуры ТГСК или применение селективно размножающихся клеточных популяций, или обработка цитокинами могут усилить приживление микроглии, что может существенно облегчить достаку энзимов в центральную нервную систему. В это отношении будут важны многоцентровые исследования с общим подходом и оценкой клинических исходов. </p> <h3>Ключевые слова</h3> <p>наследственные болезни накопления, мукополисахаридозы, трансплантация гемопоэтических клеток, режимы кондиционирования, клинический эффект </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(5197) "В данной обзорной статье представлены сведения о трансплантации гемопоэтических стволовых клеток (ТГСК) у детей с врожденными метаболическими болезнями накопления (ВМБН), и о нерешенных вопросах ТГСК при этих состояниях. Обсуждаются как миелоаблативные, так и менее интенсивные режимы кондиционирования. Показана выгода стандартизированного подхода к ТГСК при болезни Хурлера и ранней адренолейкодистрофии (АЛД) головного мозга. Режимы кондиционирования со сниженной интенсивностью могут оказаться более успешными в плане снижения смертности и развития осложнений, особенно у больных с развивающимся неврологическим дефектом. В ситуациях с ТГСК при наследственных заболеваниях можно ожидать, что потенциальные доноры-сибсы могут быть носителями мутации данного гена. Нерешенная проблема состоит в том, может ли альтернативный донор иметь преимущество в сравнении с сибсом, который может быть носителем заболевания. Обычно применяют стволовые неродственные донорские клетки из различных источников (костного мозга, периферических клеток, пуповинной крови) с хорошими результатами. Рассматривается эффективность энзим-заместительной терапии по сравнению с ТГСК в качестве подходящего лечения при менее тяжелых формах мукополисахаридозов (МПС), и ТГСК признано стандартом терапии для больных с тяжелыми клиническими формами МПС типа I. В противоположность синдрому Хурлера, ТГСК не выявила существенного влияния у больных с тяжелым МПС типа II (синдром Хантера), т.е. дети с тяжелой формой МПС типа II, по-видимому, не имеют преимуществ в нейрокогнитивном развитии при ТГСК. Что касается метахроматической или глобоидноклеточной лейкодистрофии, то данные об эффективности ТГСК здесь более скудные. Получение четких данных об исходах ТГСК у больных с ВМБН оказалось сложной задачей из-за редкости этих заболеваний, вариабельности их генотипов и фенотипов, различий в источниках стволовых клеток, кондиционирующих режимах и оценке «успешных» результатов. Дальнейшие исследования установят полезность комбинированной терапии с/без трансплантации, включая субстратное ингибирование, терапию шаперонами, энзимотерапию и т.д. Кроме того, интерес к неонатальному скринингу обеспечит раннее вмешательство в течение этих болезней, т.к. это очень важно для получения оптимальных результатов. Наконец, модификация процедуры ТГСК или применение селективно размножающихся клеточных популяций, или обработка цитокинами могут усилить приживление микроглии, что может существенно облегчить достаку энзимов в центральную нервную систему. В это отношении будут важны многоцентровые исследования с общим подходом и оценкой клинических исходов.
Ключевые слова
наследственные болезни накопления, мукополисахаридозы, трансплантация гемопоэтических клеток, режимы кондиционирования, клинический эффект
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(5197) "В данной обзорной статье представлены сведения о трансплантации гемопоэтических стволовых клеток (ТГСК) у детей с врожденными метаболическими болезнями накопления (ВМБН), и о нерешенных вопросах ТГСК при этих состояниях. Обсуждаются как миелоаблативные, так и менее интенсивные режимы кондиционирования. Показана выгода стандартизированного подхода к ТГСК при болезни Хурлера и ранней адренолейкодистрофии (АЛД) головного мозга. Режимы кондиционирования со сниженной интенсивностью могут оказаться более успешными в плане снижения смертности и развития осложнений, особенно у больных с развивающимся неврологическим дефектом. В ситуациях с ТГСК при наследственных заболеваниях можно ожидать, что потенциальные доноры-сибсы могут быть носителями мутации данного гена. Нерешенная проблема состоит в том, может ли альтернативный донор иметь преимущество в сравнении с сибсом, который может быть носителем заболевания. Обычно применяют стволовые неродственные донорские клетки из различных источников (костного мозга, периферических клеток, пуповинной крови) с хорошими результатами. Рассматривается эффективность энзим-заместительной терапии по сравнению с ТГСК в качестве подходящего лечения при менее тяжелых формах мукополисахаридозов (МПС), и ТГСК признано стандартом терапии для больных с тяжелыми клиническими формами МПС типа I. В противоположность синдрому Хурлера, ТГСК не выявила существенного влияния у больных с тяжелым МПС типа II (синдром Хантера), т.е. дети с тяжелой формой МПС типа II, по-видимому, не имеют преимуществ в нейрокогнитивном развитии при ТГСК. Что касается метахроматической или глобоидноклеточной лейкодистрофии, то данные об эффективности ТГСК здесь более скудные. Получение четких данных об исходах ТГСК у больных с ВМБН оказалось сложной задачей из-за редкости этих заболеваний, вариабельности их генотипов и фенотипов, различий в источниках стволовых клеток, кондиционирующих режимах и оценке «успешных» результатов. Дальнейшие исследования установят полезность комбинированной терапии с/без трансплантации, включая субстратное ингибирование, терапию шаперонами, энзимотерапию и т.д. Кроме того, интерес к неонатальному скринингу обеспечит раннее вмешательство в течение этих болезней, т.к. это очень важно для получения оптимальных результатов. Наконец, модификация процедуры ТГСК или применение селективно размножающихся клеточных популяций, или обработка цитокинами могут усилить приживление микроглии, что может существенно облегчить достаку энзимов в центральную нервную систему. В это отношении будут важны многоцентровые исследования с общим подходом и оценкой клинических исходов.
Ключевые слова
наследственные болезни накопления, мукополисахаридозы, трансплантация гемопоэтических клеток, режимы кондиционирования, клинический эффект
" } } } [4]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "80" ["~IBLOCK_SECTION_ID"]=> string(2) "80" ["ID"]=> string(4) "1438" ["~ID"]=> string(4) "1438" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["~NAME"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "10/18/2017 03:01:36 pm" ["~TIMESTAMP_X"]=> string(22) "10/18/2017 03:01:36 pm" ["DETAIL_PAGE_URL"]=> string(140) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov/" ["~DETAIL_PAGE_URL"]=> string(140) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(84798) "General principles of hematopoietic cell transplantation for primary immune deficiency diseases
The primitive hematopoietic stem cell (HSC) has the capability for self-renewal and differentiation, characteristics that allow transplantation of small numbers of HSC sufficient for complete restoration of the hematopoietic system of another individual. Transplanted HSC ultimately will differentiate into multiple lineages, including erythrocyte, monocyte/macrophage, granulocyte, megakaryocyte, and lymphoid cells. Thus hematopoietic cell transplantation (HCT) has the potential to cure disorders resulting from defects in the pluripotent progenitor cells as well as defects in single hematopoietic lineages. Primary immune deficiency syndromes are a group of disorders that primarily affect a single lineage, e.g., lymphoid or myeloid lineage, and can be cured with HCT. The goal of HCT for treatment of most primary immune deficiency disorders is to restore sufficient numbers of normal donor cells in the affected lineage(s); donor reconstitution of an unaffected lineage is not required for cure of the disease.
The barrier to successful allogeneic HCT is determined by differences in major or minor histocompatibility antigens between donor and recipient, resulting in bi-directional immunologically mediated graft-vs.-host (GVH) and host-vs.-graft (HVG) reactions. The barrier to engraftment is further determined by the capacity of host immune cells to generate a response to alloantigens. In addition, it has been postulated that host cell occupancy of a specific hematopoietic cell niche functions as a “space-occupying” barrier to engraftment. The strength of the opposing GVH reaction is determined by the number of alloreactive T cells in the graft. The conventional strategy to overcome this bi-directional barrier has relied upon three elements: first, elimination of host alloreactivity with agents capable of immunoablation and myeloablation; second, infusion of donor HSCs to rescue the patient from lethal myeloablation; and third, control of donor alloreactivity with post-transplant immune suppression or by elimination of T cells from the donor graft.
When these general principles are applied to the treatment of specific primary immune deficiency disorders, several distinct concepts emerge. First, syndromes that cause profound immune deficiency may not require a conditioning regimen, as there is no immunological resistance to engraftment. That said, there appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly when the MHC barrier is increased, i.e. in the situation of HLA-mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. Accordingly, the intensity of the conditioning regimen generally is determined not only by the degree of human leukocyte antigen (HLA) disparity, but also by the magnitude of T cell deficiency and the occupancy of niches thought to be required for engraftment by host cells. Wiskott-Aldrich syndrome (WAS) exemplifies this concept in a different way: a successful allograft must generate normal platelets as well as functional T cells; hence the conditioning regimen must provide some degree of myeloablation. Second, the immune defect may be corrected by partial reconstitution of normal immune cells — in other words full donor chimerism of the affected cell subset may not be required. A natural model is the absence of immune deficiency in most female carriers of X-linked immune deficiencies. This concept may add further justification for limiting the intensity of the conditioning regimen. Third, there is no potential benefit for GVH alloreactivity among patients with an immune deficiency, in contrast to patients with hematological malignancy in whom a graft-vs.-leukemia effect might be advantageous. Thus HCT protocols generally employ intensive post-grafting immune suppression or deplete alloreactive T cells from the graft, so as to minimize the risk of GVH disease (GVHD). The strong preference to avoid GVHD also forms the basis for the general disinclination to transplant peripheral blood stem cells, which contain approximately 10 times the number of T cells in the graft compared to bone marrow. The potential risk for life-threatening GVHD often enters into the determination of whether HCT should be undertaken in a specific patient, and the degree of disparate HLA or minor histocompatibility antigens among available donors must be balanced against the effectiveness of alternative therapies, such as enzyme replacement, intravenous immune globulin, prophylactic antibiotics, and other medical treatments.
Severe combined immune deficiency (SCID)
SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes in which the lymphocyte subsets may or may not be present, and if present, may or may not be functional, and which may pose a barrier to engraftment (Table 1) [1].
Table 1. Lymphocyte phenotype in the SCID syndromes
|
Lymphocyte phenotype |
Mutation or deficiency |
||
|---|---|---|---|
|
T |
B |
NK |
|
|
- |
- |
- |
Adenosine deaminase |
|
- |
- |
+ |
RAG1 or RAG2 |
|
- |
- |
+ |
Artemis |
|
- |
+ |
- |
Common γ chain |
|
- |
+ |
- |
Jak3 |
|
- |
+ |
+/- |
CD45 deficiency |
|
- |
+ |
+ |
IL-7Rα-chain |
|
- |
+ |
+ |
CD3γ/CD3ε/CD3ζ deficiency |
Since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. As mentioned above, elimination of occupancy of a B cell niche may require conditioning, particularly with haploidentical grafts; alternatively, establishment of “split” mixed chimerism (donor T / host B cells) may be sufficient to ameliorate the T cell dysfunction and allow the X-SCID patient to be supported with IVIG, similar to a patient with agammaglobulinemia. Lui et al recently showed that resistance to B cell engraftment in B+ SCID appears to be at the level of the pro-B cell, thus suggesting a potential role for targeting early B cell progenitors in lieu of high intensity conditioning [2].
Other biological factors associated with the SCID phenotype may influence the barrier to engraftment. NK cells, which are relatively radio resistant and may survive intensive conditioning regimens, have been shown to mediate graft rejection [3, 4]. The Perugia team has shown that donor NK alloreactivity is enhanced in the absence of T cells in the graft. Although this concept has been exploited to engineer donor grafts with enhanced anti-host NK activity, it may have implications for the reciprocal situation where T cells are lacking in the host. Particularly in the situation where the donor lacks inhibitory ligands, NK cells theoretically could pose an additional immune barrier to engraftment into a patient with SCID. This concept is supported by a murine model of Artemis deficiency, wherein NK-mediated graft rejection has been observed [5]. Another potential barrier is the presence of maternal T cells that have “engrafted” in the fetus in utero, often seen in patients with X-SCID. Maternal T cells can be detected using the standard methods for assessing chimerism, such as sex-chromosome specific fluorescent in situ hybridization (FISH) probes or polymerase chain reaction (PCR) detection of maternal-specific genetic polymorphisms, termed variable number tandem repeat (VNTR) sequences [6, 7]. High-levels of maternal T cells have been associated with resistance to engraftment of haploidentical cells when no conditioning is given [8, 9]. Thus, it is reasonable to consider use of a conditioning regimen in SCID patients with NK cells or maternal T cells. In the absence of a conditioning regimen, some reports have suggested that very large dose CD34+-selected peripheral blood stem cell (PBSC) grafts may help overcome graft rejection, although it may not facilitate B cell reconstitution [10].
One of the difficulties in analyzing the outcome of HCT in SCID patients is the relative rarity of the condition, which prohibits conducting large single center studies of a specific modality over a short period of time. Most reports with large numbers of patients represent either retrospective analyses of registry data, or single center studies conducted over a long period of time. Studies confined to a single phenotype or pilot studies of novel approaches generally have too few patients for meaningful assessment. The largest series of analyses has been reported by the European cooperative groups. In 1990 a retrospective study included 183 SCID patients given marrow transplants [11]. Among the 70 patients given grafts from HLA-identical siblings, 65 of whom were not given a preparative regimen, long term survival was 70%, and the majority of patients achieved stable engraftment of T and B lymphocytes. Factors that correlated with improved chances of survival included lack of infection prior to HCT and isolation of the patient in a protective environment. Clinical improvement was observed in all patients, including those with partial donor cell engraftment. In contrast to these results, less than 60% of patients given haploidentical grafts survived. The analysis definitively showed the important role of conditioning in establishing donor engraftment of T-depleted HLA-mismatched haploidentical marrow. Graft failure occurred in 50% of unconditioned patients compared to 14% of conditioned patients, and the rate of engraftment improved proportionately with increased intensity of the regimen. Immunological recovery, including B cell recovery, was also facilitated by the preparative regimen, and the frequency of late deaths related to poor immunological reconstitution was reduced. However, the benefit of a preparative regimen for establishing donor cell engraftment was negated by an increase in regimen-related complications and did not improve overall survival.
Over time, the outcome of HCT for SCID has improved, as novel supportive care and alternative donor sources have been used. Survival for recipients of HLA-identical sibling grafts now approaches 90%, and in the 2003 retrospective study by the European Group for Blood and Marrow Transplantation (EBMT), outcome for recipients of HLA-phenotypically identical grafts was not statistically significantly different from that for genotypically HLA-identical donors [12]. This analysis also showed a significant improvement over time for recipients of T-depleted haploidentical grafts, from approximately 60% to almost 80% survival (p=.0007) by the late 1990s. The most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT, with a 2-fold increase in risk for patients aged 6–12 years, and an 8-fold increase in risk for patients >12 years when compared with patients given HCT before 6 years of age. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype (64% vs. 36%, p=.0007), protected environment (57% vs. 15%, p=.0001), and lack of pulmonary infections before HCT (59% vs. 38%, p=.0001). Use of a conditioning regimen was associated with improved survival for B- SCID patients, although the difference was not statistically significant. More recently, Fischer and colleagues analyzed a large cohort of SCID patients to determine factors that correlated with good clinical outcomes (survival and amelioration of clinical immune deficiency) [13]. Graft source was significant, and risk for poor outcome was 3.7-fold higher for recipients of haploidentical and 4.8-fold higher for phenotypically HLA-identical (related or unrelated) compared to HLA-identical sibling grafts. Establishment of donor myeloid cells correlated with better survival, presumably because donor chimerism of the myeloid lineage correlated with donor origin of lymphocytes. Lack of CD4+ cell reconstitution and persistent need for IVIG were both significantly associated with poor outcome. Finally, the type of SCID appears to affect outcome, as specifically those with Artemis mutations have a 6-fold higher risk for poor outcome. These patients had a higher incidence of chronic papilloma virus infections, malnutrition, and chronic GVHD. Other studies indicate that survival generally is higher among B+ compared to B- SCID patients, particularly after alternative donor HCT [14].
Most other centers report comparable results, although in smaller series. The general experience is that genotypically HLA-identical marrow transplantation restores T cell immunity in >90% of unconditioned SCID patients, although B cell reconstitution occurs in only half of these patients [8, 15]. Despite the use of preparative regimens, recipients of T-depleted haploidentical marrow have delayed immune reconstitution, with 3–6 months required for development of antigen responsive T cells, and commonly multiple marrow infusions are needed [16]. B lymphocyte reconstitution is generally suboptimal and most patients require continued immunoglobulin support. The EBMT analysis found long-term functional T cells in about 80% of recipients of HLA-sibling grafts and 90% of B+ SCID recipients of haploidentical grafts; in contrast, functional T cells were observed in only 66% of B- SCID patients (p=.002). Long-term B cell function was less robust in all cohorts: 88% of B+ and 63% of B- SCID recipients of HLA-identical sibling grafts, and 66% of B+ and 44% of B- SCID recipients of haploidentical grafts, respectively. Certain SCID phenotypes may require a preparative regimen, for example patients with reticular dysgenesis given T-depleted grafts appear to have improved outcome if given high intensity conditioning with subsequent reconstitution of normal myeloid cells [17]. B- SCID patients also appear to benefit from conditioning [14].
The role of conditioning for unrelated grafts is the same as for T-depleted haploidentical grafts, in that it may facilitate establishment of donor B lymphocyte chimerism, however, that benefit may be offset by regimen-related toxicities. In 1992 Filipovich and colleagues reported their initial experience with unrelated marrow grafts for 8 SCID patients, of whom 5 were given high intensity conditioning [18]. Graft rejection occurred in 2 of the 3 unconditioned patients, although both survived long term after a second transplant with high intensity conditioning. Among the conditioned patients, 2 died within the first 100 days after HCT, while the others survived long term with improved immune function. Subsequently larger series have shown excellent outcome after high intensity conditioning followed by HLA-matched unrelated grafts, with about 80% survival [19, 20]. Compared to haploidentical recipients, unrelated marrow recipients had significantly lower risk for interstitial pneumonitis, graft failure, acute and chronic GVHD, and abnormal T cell receptor diversity [19]. Thus, immune reconstitution after T-replete unrelated donor transplantation appears to be faster compared to T-depleted haploidentical HCT, and often normal B cell function is achieved.
Outcomes for unrelated umbilical cord blood have been reported in small series and appears equivalent to that of matched unrelated marrow. Bhattacharya et al reported success in establishing well-matched (6/6 or 10/10 HLA match) umbilical cord blood grafts without conditioning [21]. The median time to achieving an absolute T cell count of more than 200 cells/ml among 5 surviving SCID patients was about 60 days, and mixed or full donor B cell engraftment was observed in 4 of these. Diaz reported 11 SCID patients, 9 given high intensity and 2 given reduced intensity conditioning, 7 and 1 of these, respectively, survive long term [22]. High intensity conditioning generally has been employed in recipients of HLA-mismatched cord blood units, with comparable results [20].
The condition of the patient before HCT correlates strongly with the risk of death after HCT irrespective of the graft source. In particular, infections and pulmonary disease are associated with significantly worse outcomes [12, 14, 23]. The most common cause of death in the first 6 months after HCT is infection, thus it is not surprising that pre-existing infection is detrimental to success. Indeed, a pre-existing pulmonary infection confers a 2-to 3-fold increased risk of death following HCT [14]. Therefore, every patient with SCID should have a thorough evaluation for infection and occult pulmonary disease. Liver enzyme elevations may indicate maternal T cell-mediated GVHD or underlying liver dysfunction, the latter is commonly associated with untreated ADA deficiency. Enzyme replacement therapy with polyethylene glycol (PEG) conjugated adenosine deaminase improves T cell function [24]. Since functional T cells pose an immunological barrier to engraftment, the general practice has been to stop PEG-ADA several weeks before HCT in order to “T-deplete” the recipient. However PEG-ADA also prevents or improves the liver injury found in ADA deficiency, thus, early stopping may result in hepatitis and increase the risk for post-transplant liver toxicity during the time required to establish endogenous enzyme production. A reasonable approach is to continue PEG-ADA unless no conditioning is contemplated, in which case pre-transplant discontinuation is warranted. Age of the patient is another important factor associated with survival. The best outcomes are reported for SCID patients given allogeneic transplant within the first year of life [12]. Older patients are more likely to have infections and organ dysfunction that contribute to higher mortality.
The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age. Buckley and colleagues reported better survival and the establishment of long-term functional T cells in patients with SCID who received HCT before 28 days of life (overall survival ((OS) 95%) compared to patients who were older (OS 74%) [25]. Survival of 21 SCID infants, given no conditioning and transplanted with haploidentical T cell depleted marrow grafts before 28 days of age (neonatal cohort), was 95% compared to 74% of 96 older infants. Thymopoiesis, as measured by T cell receptor excision circles (TREC), was improved in the neonatal transplant cohort, however, no comparative improvement in B cell function was observed. Acute GVHD grades III–IV developed in only 16% of patients who received grafts mismatched for 2 or 3 HLA antigens. Several factors probably contributed to the improved survival observed in patients less than 28 days old. In particular, younger patients are less likely to have opportunistic infections and subsequent co-morbidities, malnutrition, and failure to thrive, all of which have been associated with increased mortality following HCT, but may also contribute to decreased thymic function. These results show that T cell depleted haploidentical marrow grafts are feasible at a very early age and that there is little benefit in delaying HCT in order to identify a better matched donor.
Once established, donor progenitor cells develop and mature in the vestigial thymus of the SCID patient. Buckley and colleagues demonstrated that T cell receptor (TCR) gene rearrangement occurs in donor T cell precursors resulting in the generation of naïve T cells [25, 26, 27]. Measurements of TCR repertoire show development of a broad diversity within the donor T cell pool, which persists over time. Patel and colleagues reported that thymopoiesis, as measured by TRECs and naïve CD4 cells, declined exponentially over time after HCT. Several studies have suggested that late graft failure or deterioration of thymopoiesis may jeopardize long-term T cell function [28]. In contrast, recent studies have shown that thymic output of T cells and T cell diversity remain normal for decades after HCT in approximately 80% of patients [29, 30]. The degree of early T cell reconstitution appears to be strongly associated with the long-term stability of T cell function, thus, patients at most risk for poor T cell function or loss of T cell grafts are those with low numbers of TRECs and naïve-CD4 cells within the first few years after HCT [13, 31]. Alain Fischer’s team in Paris found that donor chimerism of the myeloid lineage correlated with higher CD4+ T cell counts long term, and that donor myeloid chimerism was limited to patients who received high intensity conditioning. Other factors that may be associated with higher risk for poor long-term T cell reconstitution are SCID phenotypes that lack B cells, presence of NK cells, and possibly young age at time of HCT. As noted above, long term B cell reconstitution is common only among patients given high intensity conditioning regimens [13, 15].
Primary T cell immunodeficiencies other than SCID
Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Nonetheless, the immune dysfunction leads to progressive decline from opportunistic infections, autoimmune phenomena, and a propensity to develop malignancies, particularly lymphoma. Several of the genetic mutations implicated in SCID also have been found to be present in patients with PTCD, thus termed “leaky SCID”. New genetic mutations also have been characterized, while the genetic causes in many patients remain unrecognized [32, 33, 34]. The more common of these rare disorders are listed in Table 2.
Table 2. Primary T cell immunodeficiency syndromes commonly referred for HCT
Abbreviations:
HIGM, Hyper IgM;
HLA, Human leukocyte antigen;
HSM, hepatosplenomegaly;
IPEX, Immunodeficiency-polyendocrinopathy-enteropathy X-linked;
XLP, X-linked lymphoproliferative
|
Syndrome |
Mutation |
Clinical features |
Laboratory features |
|---|---|---|---|
|
Omenn’s |
RAG1 or RAG2 |
HSM |
Eosinophilia |
|
ZAP70 |
ZAP70 |
CD8+ lymphopenia |
|
|
HIGM |
CD40L or CD40 |
X-linked |
High IgM & low IgG levels |
|
Common Variable Immunodeficiency |
Unknown |
Autoimmunity |
Low IgG |
|
Cartilage Hair Hypoplasia |
endoribonuclease RMRP |
Dwarfism |
|
|
Wiskott Aldrich |
WASP |
Eczema |
Thrombocytopenia |
|
IPEX |
FOXP3 |
X-linked |
|
|
XLP |
SH2D1A |
X-linked |
Hypogammaglobulinemia |
|
Bare Lymphocyte syndrome (Class II HLA deficiency) |
RFXANK, RFX5, RFSAP, CIITA |
Pulmonary infection |
Hypogammaglobulinemia |
|
Class I HLA deficiency |
TAP1 or TAP2 |
CD8 lymphopenia |
|
|
DiGeorge syndrome |
10p13 or 22q11.2 |
Hypocalcemia |
CD3 lymphopenia |
Until gene therapy is perfected, allogeneic marrow transplantation remains the only curative therapy available for these disorders. In general, conventional regimens have included both immunoablative and myeloablative agents to overcome residual immune barriers to engraftment and to ensure multi-lineage chimerism. The combination of busulfan (1 mg/kg x 16 doses) and cyclophosphamide (200 mg/kg total dose), with or without anti-thymocyte globulin is the most commonly used regimen. Our experience indicates that busulfan is metabolized faster in young patients, therefore in order to optimize engraftment it is prudent to adjust the daily doses to achieve steady state concentration (Css) of >200 ng/ml in recipients of HLA-identical sibling grafts and >400 ng/ml in recipients of HLA-matched unrelated grafts [35].
In 2003 the EBMT reported a retrospective analysis of outcome for patients with primary immunodeficiency disease other than SCID [12, 36]. A higher incidence of engraftment was reported in patients who received HLA-identical sibling grafts (99%), compared to those who received haploidentical or unrelated donor grafts (75–80%). In addition, survival at 3 years was better for patients who received HLA-identical sibling grafts (71%) compared to haploidentical grafts [42% (p=.0006)]. Survival after HLA-matched unrelated donor grafts was 59%, which was not statistically significantly different from the HLA-identical sibling cohort. The main cause of death following HCT was infection.
Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Overall survival was 63% and 35% after HLA-identical sibling grafts or mismatched grafts, respectively [12, 36]. Unfortunately, and in contrast to the results for SCID, the EBMT study found no improvement in survival of the non-SCID cohorts over the two decades included in the analysis, thus highlighting important differences and problems associated with PTCD compared to SCID. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT. Given that a conditioning regimen is necessary to ensure engraftment, the associated risks for organ toxicity, hemorrhage, and infection are compounded by these co-morbidities. Several studies have associated inferior survival with presence of co-morbidities, including opportunistic infections, Epstein-Barr virus lymphoproliferation, and pulmonary dysfunction [8, 23]. Among boys with X-linked hyper-IgM (XHIM) excessive mortality has been associated with the presence of pulmonary infection or liver disease at time of HCT [37].
In theory, split chimerism (donor T/host B chimerism) or partial donor T cell chimerism should be sufficient to ameliorate the immune dysfunction in most types of PTCD. Accordingly, reducing the intensity of conditioning may be a strategy to reduce regimen-related toxicity without sacrificing immune reconstitution. Specific factors associated with the molecular defect must be taken into consideration, as partial chimerism may not be sufficient for some defects. DiGeorge syndrome and the Bare Lymphocyte syndromes (BLS) pose particular challenges, because the T cell deficiency results from inadequate thymopoiesis, caused by absence of the thymus or absence of HLA molecules on the thymic epithelial cells, respectively. The molecular defects that cause BLS block the transcription of HLA genes; therefore antigen-presenting cells also are defective. Hence, donor chimerism must be established in B cell and dendritic cell lineages. In both disorders, absence of thymic function may prevent formation of naïve donor T cells; therefore full chimerism provides the most likely chance that a broad range of donor antigen-specific memory cells may be established long term.
Molecular deficits that allow T cell proliferation, but preclude intercellular interactions, such as X-linked hyper-IgM (XHIM) syndrome or Immune Dysregulation-Polyendocrinopathy-Enteropathy X-linked (IPEX) syndrome, generally require conditioning in order to prevent T cell mediated graft rejection; however, partial T cell chimerism appears to restore immune function as well as full donor chimerism [38, 39]. The autoimmune manifestations of the IPEX syndrome are caused by absence of CD4+CD25+ FOXP3+ regulatory T cells (Tregs), important for sustaining self-tolerance. Normal numbers of FOXP3 expressing CD4+CD25+ cells have been observed in boys with mixed donor/host chimerism, and several case reports indicate that mixed chimerism is sufficient to ameliorate many of the manifestations of IPEX, including the enteropathy, anemia, failure to thrive, and the susceptibility to infections. Curiously, we and others have observed improvement in diabetes, although in theory autoimmune-mediated islet cell destruction happens well before HCT is carried out [38]. The most common cause of the XHIM syndrome is a mutation in the CD40 ligand gene, which is expressed by T cells and provides a critical signal for B cells to switch antibody production from IgM to IgG subtypes. Theoretically, the introduction of some normal CD40 ligand-expressing T cells should be sufficient to reverse the disease, even if B cells of host origin remain. Amelioration of disease symptoms with mixed chimerism has been observed for some boys treated for XHIM, although no detailed analysis of B cell function was reported [40, 41].
Wiskott-Aldrich Syndrome (WAS). HCT offers significantly improved survival chances for patients with WAS, without which about 50% will die from infection, autoimmune disease, or lymphoproliferative disease by the third decade of life [42]. The WAS mutation affects lymphoid and hematopoietic compartments, both of which are corrected by HCT. Accordingly most patients are conditioned with both immunosuppression and high dose chemotherapy to facilitate multilineage donor cell engraftment. Figure 1 shows cell counts in a patient who was too ill with opportunistic infections to receive high dose conditioning and became a split chimera after reduced intensity conditioning and unrelated marrow transplantation. Following transplantation the T cell immune defect was corrected, but thrombocytopenia persisted as did host CD33+ cells. After the infections resolved, a second graft was given with a high intensity (directed at myeloid cells), but without immunoablative preparative regimen, resulting in amelioration of thrombocytopenia as the CD33+ compartment converted to donor type. The importance of achieving full donor chimerism was shown recently in a retrospective analysis of results in 96 patients, which showed an almost 2-fold reduction in mortality among patients with full chimerism compared to those with mixed or split chimerism [43]. Mixed chimerism also is associated with a significantly higher risk for developing autoimmune manifestations after HCT.
Figure 1. Correction of thrombocytopenia in Wiskott-Aldrich correlates with donor chimerism of CD33+ cell subset
At 30 days after hematopoietic cell transplant, a high proportion of both CD3 (gray line) and CD33 (black line) subsets mark as donor origin. Over time, the proportion of donor CD3 cells remains stable, while the proportion of donor CD33 cells decreases. The platelet count (black dashed line) reaches a normal level when the CD33 donor chimerism is high, and falls proportionately with the fall in donor CD33 chimerism.

HCT using HLA-identical sibling marrow grafts is highly successful in treating WAS, with approximately 88% event-free survival [43]. The combination of busulfan (1 mg/kg x 16 doses) and cyclophosphamide (200 mg/kg total dose), with or without anti-thymocyte globulin is the most commonly used conditioning regimen. Busulfan is metabolized faster in younger patients, therefore it is prudent to monitor levels and target the dose to achieve a Css of greater than 200 ng/ml to assure engraftment [35]. An EBMT analysis determined that patient age, disease severity, and splenectomy, among other factors, did not affect outcome [43].
Results of alternative donor HCT for treatment of WAS have improved over time, particularly for recipients of unrelated marrow grafts. Most recent studies have shown approximately 70%–78% long-term survival [43, 44]. In a 2001 study facilitated by the International Bone Marrow Transplant Registry (IBMTR), age of 5 years or older was associated with an increased risk of mortality after HCT. Survival for patients younger than 5 years was about the same as for recipients of HLA-identical sibling grafts. In addition, several studies found comparable survival rates among recipients of HLA-matched related and unrelated grafts [44, 45]. The most commonly used regimen was a combination of busulfan, cyclophosphamide, and ATG. In our experience, targeting the dose of busulfan to achieve a C SS above 400 ng/ml facilitates engraftment [35].
Encouraging results have also been reported for umbilical cord blood transplants, but most information comes from case reports or part of smaller series of patients with immune deficiencies. Among 15 patients reported by Ozsahin, et al, event-free survival was approximately 70%, similar to recipients of unrelated marrow grafts [44]. Most patients in these reports were conditioned with the combination of busulfan, cyclophosphamide, and antithymocyte globulin, which the Japanese group found to be an important factor for improved survival when compared to other regimens [44]. Reconstitution of immunity after cord blood approximates that observed with unrelated marrow grafts.
There is more information about haploidentical transplants for WAS, although the historical results are less encouraging. The EBMT study showed a 4–5-fold increase in mortality after haploidentical compared to HLA-identical sibling grafts [43]. Others have reported similar results [36, 44, 46]. These reports show a high incidence of graft failure and poor immune reconstitution following T-depleted haploidentical marrow grafts. The Tubingen team provided a promising case report of “mega-dose” purified CD34+ haploidentical grafts used to overcome the barrier to engraftment without engendering GVHD [47].
Inherited immune defects not primarily affecting T cells
A wide range of rare immune deficiency syndromes result from defects in B lymphocytes, NK cells, or nonlymphocytic subsets including neutrophils (Table 3).
Table 3. Histiocytic and myeloid immune deficiency syndromes commonly referred for HCT
Abbreviations:
FHL, Familial hemophagocytic lymphohistiocytosis;
LCH, Langerhans cell histiocytosis
|
Syndrome |
Mutation |
Clinical features |
Laboratory features |
|---|---|---|---|
|
Histiocytic disorders |
|||
|
FHL |
PRF1 |
Fever |
Pancytopenia |
|
Multifocal LCH |
unknown |
Bone lesions |
Anemia |
|
Myeloid disorders |
|||
|
Chronic Granulomatous Disease |
p91PHOX |
Pneumonia |
Catalase-positive bacteria |
|
Chediak-Higashi Syndrome |
CHS1 |
Pyogenic infections |
Neutropenia |
|
Leukocyte Adhesion defect |
β-2 integrin |
Bacterial infections |
Leukocytosis |
|
Kostmann’s neutropenia |
GCSF-R |
Bacteremia/sepsis |
Neutropenia |
|
Shwachman-Diamond Syndrome |
Unknown |
Pancreatic enzyme deficiency |
Neutropenia |
The individual immune defects predispose the patients to specific infections, for example with Aspergillus in patients with chronic granulomatous disease (CGD) or staphylococcus aureus in leukocyte adhesion deficiency (LAD)-I, and are associated with distinctive co-morbidities, such as infiltrative pulmonary or central nervous system disease in hemophagocytic lymphohistiocytosis (HLH) or recalcitrant colitis in CGD. As above, the decision to treat with HCT must take into consideration the prognosis of the disorder with available supportive care, the presence of co-morbidities that might increase the risk of mortality following HCT, and the availability of a suitable donor. Unfortunately, because these diseases are rare, meaningful prospective studies reporting on large series of patients with a single disease entity are not available. Within the European retrospective study, survival for specific subsets, 48 patients with phagocytic disorders, and 90 patients with hemophagocytic disorders, was reported to be approximately 70% and 68%, respectively, for recipients of HLA-identical sibling grafts. The small number of patients with phagocytic cell disorders had a similar outcome after transplantation of unrelated marrow, in contrast to patients with hemophagocytic disorders in whom survival was only 28% after unrelated grafts.
Studies that include larger numbers of patients with single diagnoses are limited to a few disorders such as CGD and HLH. The prognosis for CGD patients has improved considerably with more aggressive use of gamma-interferon and antibiotic prophylaxis. HCT is indicated for patients with recurrent life-threatening infections or organ dysfunction caused by refractory granulomatous disease [48]. A series of patients transplanted with HLA-identical sibling marrow (n=10) or unrelated marrow or cord blood (n=10) was reported recently from the United Kingdom [49]. Most patients were conditioned with busulfan and cyclophosphamide, and alemtuzumab was given to recipients of unrelated grafts. Survival was reported to be 90% with a median follow-up of 61 months; one patient in each group died from disseminated infection. Neutrophil oxidative burst was normalized in patients with mixed as well as full donor chimerism. Del Giudice et al published a review of case reports and small series of patients with CGD that included several long-term survivors with stable mixed chimerism, consistent with the notion that a small proportion of normal cells improves disease symptoms [50].
Without HCT, the prognosis for patients with HLH is poor even with intensive supportive care and anti-inflammatory regimens that include etoposide, cyclosporine, and prednisone [51, 52]. The outcome is considerably improved when HCT is performed after control of the initial inflammatory state is gained and infiltrative disease has resolved. The HLH 94 protocol reported 50–60% overall survival for the 113 children entered into the study; overall survival was 65% for the subgroup of 65 children given HCT. The study results suggested that intrathecal chemotherapy plays an important role in gaining disease control [52]. A retrospective analysis of 91 patients in the CIBMTR registry given unrelated marrow grafts found 53% overall survival [53]. Most patients were conditioned with busulfan, cyclophosphamide, and etoposide, with or without ATG. Survival was worse among the small subgroup with active disease at time of HCT, as well as among recipients of HLA-mismatched grafts. Disease manifestations resolved among patients with mixed as well as full donor chimerism. Early mortality (before day 100) was 32%, however, suggesting that a reduced intensity conditioning regimen might be of benefit.
Development of reduced toxicity regimens
Conditioning regimens that do not employ agents at doses resulting in long-lasting marrow aplasia are referred to as reduced intensity conditioning (RIC) regimens. Until recently, those regimens have been used routinely for only two conditions: severe aplastic anemia and SCID. Regimens for aplastic anemia have included immunosuppressive agents alone to overcome the allo-immune rejection responses, since these patients are thought to have "unoccupied" marrow space. These reduced intensity regimens have resulted in a markedly lower incidence of both early and late complications [54, 55]. SCID patients have no immune system capable of rejecting the graft, and therefore do not require conditioning except in the instances discussed above [11].
As the power of the graft vs. leukemia (GVL) effect became evident in the late 1970s and early 1980s, subsequent studies found that donor lymphocyte infusions (DLI) could be used to treat leukemic relapse after HCT [56>, 57]. The success of DLI set the stage for the introduction of reduced intensity conditioning for HCT, based on the hypothesis that the graft itself created the needed space through a subclinical GVH reaction directed toward recipient hematopoietic cells. Based on insights from animal models and armed with new potent immunosuppressive agents such as 2-CDA and fludarabine, investigators in Texas, Israel, Seattle, Boston, and Washington, DC pioneered less toxic regimens that facilitated partial or full chimerism in most patients [58, 59, 60, 61, 62, 63, 64].
These studies demonstrated that intensive immunosuppression alone following stem cell infusion was sufficient to establish full or partial donor chimerism and that conditioning was not required for creation of marrow space. The extent of donor cell engraftment following low intensity regimens depends on multiple factors, including the degree of intensity of the preparative regimen, the source of hematopoietic cells (marrow vs. peripheral blood stem cells), the degree of HLA-matching, and the extent of T cell depletion. Most low intensity protocols use PBSC to facilitate engraftment and enhance GVL reactions, as the product may contain 10-fold greater numbers of T cells and 4-fold greater number of hematopoietic stem cells compared to marrow [65].
There are several reasons for the further development of low intensity regimens for the establishment of mixed chimerism in patients with Non-SCID primary immune deficiency disorders. First, the potential risks of high dose conditioning regimens include early treatment related mortality and late effects, such as infertility, hormonal dysfunction, growth failure, and secondary malignancies. These risks may deter patients and families from seeking treatment before co-morbidities arise. Second, as discussed earlier, the risk for regimen-related mortality increases significantly among patients with disseminated infection, pulmonary disease or other organ dysfunction. Third, reversal of disease symptoms with partial chimerism, which may be achievable with low intensity conditioning, has been demonstrated in a number of studies [36, 66].
The main challenge in translating the success of protocols using RIC to patients with primary immune deficiency is the reliance on PBSC grafts, which may be difficult (or impossible) to collect from pediatric donors; also it confers a high risk of GVHD. Some progress has been made using marrow or CD34+ selected PBSC. Some results with HLA-matched related or unrelated marrow using RIC are summarized in Table 4.
Table 4. Intensity conditioning regimens and transplant outcome in immunodeficiency syndromes
Abbreviations:
ATG, anti-thymocyte globulin;
BM, bone marrow;
CB, cord blood;
CGD, chronic granulomatous disease;
DLI, donor lymphocyte infusion;
EBV-LPD, Epstein Barr virus lymphoproliferative disease; Flu, fludarabine;
HCT, hematopoietic cell transplant;
IPEX, Immunodeficiency-polyendocrinopathy-enteropathy X-linked;
Mel, melphalan;
MSD, matched sibling donor;
PBSC, peripheral blood stem cells;
PID, primary immune deficiency (nonSCID);
SCID, severe combined immune deficiency;
SC-M, severe co-morbities;
TBI, total body irradiation
Author | Diagnosis | Regimen | Donor | Rejection (No.) | Survival (No.) | FU (mo) |
|---|---|---|---|---|---|---|
Reduced Intensity Conditioning | ||||||
(Rao et al. 2005 [67]) | 27 PID/ 6 SCID | Flu/ Mel/Campath | BM | 0 | 31 | |
(Amrolia et al. 2000 [68]) | 6 ID/ 2 SCID | Flu/ Mel/ ATG | 0 | 7 | 6-18 | |
(Rao et al. 2007 [38]) | 4 IPEX | Flu/ Mel/Campath | BM | 0 | 4 | 6-25 |
(Cohen et al. 2007 [69]) | 7 PID/ EBV-LPD | Flu/ Mel/Campath | BM or PBSC | 0 | 7 | 0 |
Minimal Toxicity (non-myeloablative) Conditioning | ||||||
(Horwitz et al. 2001 [70]) | 10 CGD | Flu/ Cy/ ATG | CD34+ PBSC | 1 | 7 | 16-26 |
(Burroughs et al. 2007 [71]) | 10 PID+SC-M | Flu / 2 Gy TBI | PBSC | 1 | 7 | 9-96 |
A high rate of engraftment of marrow grafts has been reported after the combination of fludarabine and melphalan plus, an in vivo T-depleting agent, such as ATG or Campath®, and appears to be associated with low mortality rates [38, 67, 68, 70]. The combination of cyclophosphamide, fludarabine, and ATG has been studied as a low-intensity regimen to facilitate engraftment of CD34+ selected PBSC [70]. In the latter study, the benefit of in vivo and ex vivo T-depletion for reducing GVHD was at least partially abrogated by the use of DLI to improve the level of donor cell chimerism. The Seattle group has studied the combination of fludarabine and low-dose TBI in patients who would be expected to have very poor survival following conventional conditioning for HCT, such as those with disseminated opportunistic infections, mechanical ventilation, or other organ damage. No regimen-related mortality was observed in the first cohort given 2 Gy TBI, however chronic GVHD was observed in 70% of patients, presumably related to the use of PBSC grafts [71]. The substitution of marrow for PBSC in the subsequent cohort appears promising, and early mortality has not been increased despite increasing the dose of TBI to 4 Gy (Figure 2). Taken together, these studies suggest that low-intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
Figure 2. Survival of patients with severe infections or pulmonary disease after reduced intensity conditioning HCT is improved with bone marrow as the sole source of allogeneic hematopoietic cells.
The first cohort of patients (dashed line) was conditioned with fludarabine and 2 Gy total body irradiation and most patients received peripheral blood stem cell grafts. The second cohort (solid line) was conditioned with fludarabine and 4 Gy total body irradiation and was given marrow grafts.

Acknowledgements
This work was supported by National Institute of Health grant NHLBI grant HL36444 and National Cancer Institute grant CA18029.
References
3. Ohlen C, Hoglund P, Sentman, CL, Carbone E, et al. Inhibition of natural killer cell-mediated bone marrow graft rejection by allogeneic major histocompatibility complex class I, but not class II molecules. European Journal of Immunology. 1995;25;1286-1291.
4. George T, Yu, YY, Liu, J, Davenport C, et al. Allorecognition by murine natural killer cells: lysis of T-lymphoblasts and rejection of bone-marrow grafts (Review). Immunological Reviews. 1997;155;29-40.
6. Morisaki H, Morisaki T, Nakahori Y, Ogura H, et al. Genotypic analysis using a Y-chromosome-specific probe following bone marrow transplantation. American Journal of Hematology. 1988;27:30-33. pmid: 3281450.
8. O'Reilly RJ, Keever CA, Small TN, Brochstein J. The use of HLA-non-identical T-cell-depleted marrow transplants for correction of severe combined immunodeficiency disease. Immunodeficiency Reviews. 1989;1:273-309. pmid: 2698644.
11. Fischer A, Landais P, Friedrich W, Morgan G, et al. European experience of bone-marrow transplantation for severe combined immunodeficiency. Lancet. 1990;336:850-854. pmid: 1976883.
12. Antoine C, Muller S, Cant A, Cavazzana-Calvo M, et al. European Group for Blood and Marrow Transplantation & European Society for Immunodeficiency. Long-term survival and transplantation of haemopoietic stem cells for immunodeficiencies: report of the European experience 1968-99. Lancet. 2003;361:553-560.
14. Bertrand Y, Landais P, Friedrich W, Gerritsen B, et al. Influence of severe combined immunodeficiency phenotype on the outcome of HLA non-identical, T-cell-depleted bone marrow transplantation: a retrospective European survey from the European group for bone marrow transplantation and the European Society for immunodeficiency. Journal of Pediatrics. 1999;134:740-748.
23. Filipovich AH. Stem cell transplantation from unrelated donors for correction of primary immunodeficiencies. Immunology and Allergy Clinics NA. 1996;16:377-392.
24. Chan B, Wara D, Bastian J, Hershfield MS, et al. Long-term efficacy of enzyme replacement therapy for adenosine deaminase (ADA)-deficient severe combined immunodeficiency (SCID). Clinical Immunology. 2005;117:133-143.
29. Sarzotti-Kelsoe M, Win CM, Parrott RE, Cooney M, et al. Thymic output, T-cell diversity, and T-cell function in long-term human SCID chimeras. Blood. 2009;114:1445-1453. pmid: 19433858.
32. Liston A, Enders A, Siggs OM. Unravelling the association of partial T-cell immunodeficiency and immune dysregulation (Review). Nature Reviews Immunology. 2008;8:545-558. pmid: 18551129.
33. Cunningham-Rundles C, Ponda PP. Molecular defects in T- and B-cell primary immunodeficiency diseases (Review). Nature Reviews Immunology. 2005;5:880-892.
34. Fischer A. Primary T-lymphocyte immunodeficiencies (Review). Clinical Reviews in Allergy and Immunology. 2001;20:3-26. pmid: 11269227.
35. Slattery JT, Sanders JE, Buckner CD, Schaffer RL, et al. Graft-rejection and toxicity following bone marrow transplantation in relation to busulfan pharmacokinetics. Bone Marrow Transplantation. 1995;16:31-42. pmid: 7581127.
41. Khawaja K, Gennery AR, Flood TJ. Bone marrow transplantation for CD40 ligand deficiency: a single centre experience. Archives of Disease in Childhood. 2001;84:508-511. pmid: 11369571.
44. Ozsahin H, Le Deist F, Benkerrou M, Cavazzana-Calvo M, et al. Bone marrow transplantation in 26 patients with Wiskott-Aldrich syndrome from a single center. Journal of Pediatrics. 1996;129:238-244. pmid: 8765621.
46. Bock M, Maiwald M, Kappe R. Polymerase chain reaction-based detection of dermatophyte DNA with a fungus-specific primer system. Mycoses. 1994;37:79-84. pmid: 7845424.
50. Del Giudice I, Iori AP, Mengarelli A, Testi AM, et al. Allogeneic stem cell transplant from HLA-identical sibling for chronic granulomatous disease and review of the literature (Review). Annals of Hematology. 2003;82:189-192.
51. Sung L, King, SM, Carcao M, Trebo M, Weitzman, S.S. Adverse outcomes in primary hemophagocytic lymphohistiocytosis. Journal of Pediatric Hematology/Oncology. 2002;24:550-554.
55. Storb R, Thomas ED, Buckner CD, Clift RA, et al. Marrow transplantation in thirty "untransfused" patients with severe aplastic anemia. Annals of Internal Medicine. 1980;92:30-36. pmid: 6985782.
61. Khouri IF, Keating M, Körbling M, Przepiorka D, et al. Transplant-lite: induction of graft-versus-malignancy using fludarabine-based nonablative chemotherapy and allogeneic blood progenitor-cell transplantation as treatment for lymphoid malignancies. Journal of Clinical Oncology. 1998;16:2817-2824. pmid: 9704734.
64. Sykes M, Preffer F, McAfee S, Saidman SL, et al. Mixed lymphohaemopoietic chimerism and graft-versus-lymphoma effects after non-myeloablative therapy and HLA-mismatched bone-marrow transplantation. Lancet. 1999;353:1755-1759. pmid: 10347989.
" ["~DETAIL_TEXT"]=> string(84798) "General principles of hematopoietic cell transplantation for primary immune deficiency diseases
The primitive hematopoietic stem cell (HSC) has the capability for self-renewal and differentiation, characteristics that allow transplantation of small numbers of HSC sufficient for complete restoration of the hematopoietic system of another individual. Transplanted HSC ultimately will differentiate into multiple lineages, including erythrocyte, monocyte/macrophage, granulocyte, megakaryocyte, and lymphoid cells. Thus hematopoietic cell transplantation (HCT) has the potential to cure disorders resulting from defects in the pluripotent progenitor cells as well as defects in single hematopoietic lineages. Primary immune deficiency syndromes are a group of disorders that primarily affect a single lineage, e.g., lymphoid or myeloid lineage, and can be cured with HCT. The goal of HCT for treatment of most primary immune deficiency disorders is to restore sufficient numbers of normal donor cells in the affected lineage(s); donor reconstitution of an unaffected lineage is not required for cure of the disease.
The barrier to successful allogeneic HCT is determined by differences in major or minor histocompatibility antigens between donor and recipient, resulting in bi-directional immunologically mediated graft-vs.-host (GVH) and host-vs.-graft (HVG) reactions. The barrier to engraftment is further determined by the capacity of host immune cells to generate a response to alloantigens. In addition, it has been postulated that host cell occupancy of a specific hematopoietic cell niche functions as a “space-occupying” barrier to engraftment. The strength of the opposing GVH reaction is determined by the number of alloreactive T cells in the graft. The conventional strategy to overcome this bi-directional barrier has relied upon three elements: first, elimination of host alloreactivity with agents capable of immunoablation and myeloablation; second, infusion of donor HSCs to rescue the patient from lethal myeloablation; and third, control of donor alloreactivity with post-transplant immune suppression or by elimination of T cells from the donor graft.
When these general principles are applied to the treatment of specific primary immune deficiency disorders, several distinct concepts emerge. First, syndromes that cause profound immune deficiency may not require a conditioning regimen, as there is no immunological resistance to engraftment. That said, there appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly when the MHC barrier is increased, i.e. in the situation of HLA-mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. Accordingly, the intensity of the conditioning regimen generally is determined not only by the degree of human leukocyte antigen (HLA) disparity, but also by the magnitude of T cell deficiency and the occupancy of niches thought to be required for engraftment by host cells. Wiskott-Aldrich syndrome (WAS) exemplifies this concept in a different way: a successful allograft must generate normal platelets as well as functional T cells; hence the conditioning regimen must provide some degree of myeloablation. Second, the immune defect may be corrected by partial reconstitution of normal immune cells — in other words full donor chimerism of the affected cell subset may not be required. A natural model is the absence of immune deficiency in most female carriers of X-linked immune deficiencies. This concept may add further justification for limiting the intensity of the conditioning regimen. Third, there is no potential benefit for GVH alloreactivity among patients with an immune deficiency, in contrast to patients with hematological malignancy in whom a graft-vs.-leukemia effect might be advantageous. Thus HCT protocols generally employ intensive post-grafting immune suppression or deplete alloreactive T cells from the graft, so as to minimize the risk of GVH disease (GVHD). The strong preference to avoid GVHD also forms the basis for the general disinclination to transplant peripheral blood stem cells, which contain approximately 10 times the number of T cells in the graft compared to bone marrow. The potential risk for life-threatening GVHD often enters into the determination of whether HCT should be undertaken in a specific patient, and the degree of disparate HLA or minor histocompatibility antigens among available donors must be balanced against the effectiveness of alternative therapies, such as enzyme replacement, intravenous immune globulin, prophylactic antibiotics, and other medical treatments.
Severe combined immune deficiency (SCID)
SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes in which the lymphocyte subsets may or may not be present, and if present, may or may not be functional, and which may pose a barrier to engraftment (Table 1) [1].
Table 1. Lymphocyte phenotype in the SCID syndromes
|
Lymphocyte phenotype |
Mutation or deficiency |
||
|---|---|---|---|
|
T |
B |
NK |
|
|
- |
- |
- |
Adenosine deaminase |
|
- |
- |
+ |
RAG1 or RAG2 |
|
- |
- |
+ |
Artemis |
|
- |
+ |
- |
Common γ chain |
|
- |
+ |
- |
Jak3 |
|
- |
+ |
+/- |
CD45 deficiency |
|
- |
+ |
+ |
IL-7Rα-chain |
|
- |
+ |
+ |
CD3γ/CD3ε/CD3ζ deficiency |
Since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. As mentioned above, elimination of occupancy of a B cell niche may require conditioning, particularly with haploidentical grafts; alternatively, establishment of “split” mixed chimerism (donor T / host B cells) may be sufficient to ameliorate the T cell dysfunction and allow the X-SCID patient to be supported with IVIG, similar to a patient with agammaglobulinemia. Lui et al recently showed that resistance to B cell engraftment in B+ SCID appears to be at the level of the pro-B cell, thus suggesting a potential role for targeting early B cell progenitors in lieu of high intensity conditioning [2].
Other biological factors associated with the SCID phenotype may influence the barrier to engraftment. NK cells, which are relatively radio resistant and may survive intensive conditioning regimens, have been shown to mediate graft rejection [3, 4]. The Perugia team has shown that donor NK alloreactivity is enhanced in the absence of T cells in the graft. Although this concept has been exploited to engineer donor grafts with enhanced anti-host NK activity, it may have implications for the reciprocal situation where T cells are lacking in the host. Particularly in the situation where the donor lacks inhibitory ligands, NK cells theoretically could pose an additional immune barrier to engraftment into a patient with SCID. This concept is supported by a murine model of Artemis deficiency, wherein NK-mediated graft rejection has been observed [5]. Another potential barrier is the presence of maternal T cells that have “engrafted” in the fetus in utero, often seen in patients with X-SCID. Maternal T cells can be detected using the standard methods for assessing chimerism, such as sex-chromosome specific fluorescent in situ hybridization (FISH) probes or polymerase chain reaction (PCR) detection of maternal-specific genetic polymorphisms, termed variable number tandem repeat (VNTR) sequences [6, 7]. High-levels of maternal T cells have been associated with resistance to engraftment of haploidentical cells when no conditioning is given [8, 9]. Thus, it is reasonable to consider use of a conditioning regimen in SCID patients with NK cells or maternal T cells. In the absence of a conditioning regimen, some reports have suggested that very large dose CD34+-selected peripheral blood stem cell (PBSC) grafts may help overcome graft rejection, although it may not facilitate B cell reconstitution [10].
One of the difficulties in analyzing the outcome of HCT in SCID patients is the relative rarity of the condition, which prohibits conducting large single center studies of a specific modality over a short period of time. Most reports with large numbers of patients represent either retrospective analyses of registry data, or single center studies conducted over a long period of time. Studies confined to a single phenotype or pilot studies of novel approaches generally have too few patients for meaningful assessment. The largest series of analyses has been reported by the European cooperative groups. In 1990 a retrospective study included 183 SCID patients given marrow transplants [11]. Among the 70 patients given grafts from HLA-identical siblings, 65 of whom were not given a preparative regimen, long term survival was 70%, and the majority of patients achieved stable engraftment of T and B lymphocytes. Factors that correlated with improved chances of survival included lack of infection prior to HCT and isolation of the patient in a protective environment. Clinical improvement was observed in all patients, including those with partial donor cell engraftment. In contrast to these results, less than 60% of patients given haploidentical grafts survived. The analysis definitively showed the important role of conditioning in establishing donor engraftment of T-depleted HLA-mismatched haploidentical marrow. Graft failure occurred in 50% of unconditioned patients compared to 14% of conditioned patients, and the rate of engraftment improved proportionately with increased intensity of the regimen. Immunological recovery, including B cell recovery, was also facilitated by the preparative regimen, and the frequency of late deaths related to poor immunological reconstitution was reduced. However, the benefit of a preparative regimen for establishing donor cell engraftment was negated by an increase in regimen-related complications and did not improve overall survival.
Over time, the outcome of HCT for SCID has improved, as novel supportive care and alternative donor sources have been used. Survival for recipients of HLA-identical sibling grafts now approaches 90%, and in the 2003 retrospective study by the European Group for Blood and Marrow Transplantation (EBMT), outcome for recipients of HLA-phenotypically identical grafts was not statistically significantly different from that for genotypically HLA-identical donors [12]. This analysis also showed a significant improvement over time for recipients of T-depleted haploidentical grafts, from approximately 60% to almost 80% survival (p=.0007) by the late 1990s. The most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT, with a 2-fold increase in risk for patients aged 6–12 years, and an 8-fold increase in risk for patients >12 years when compared with patients given HCT before 6 years of age. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype (64% vs. 36%, p=.0007), protected environment (57% vs. 15%, p=.0001), and lack of pulmonary infections before HCT (59% vs. 38%, p=.0001). Use of a conditioning regimen was associated with improved survival for B- SCID patients, although the difference was not statistically significant. More recently, Fischer and colleagues analyzed a large cohort of SCID patients to determine factors that correlated with good clinical outcomes (survival and amelioration of clinical immune deficiency) [13]. Graft source was significant, and risk for poor outcome was 3.7-fold higher for recipients of haploidentical and 4.8-fold higher for phenotypically HLA-identical (related or unrelated) compared to HLA-identical sibling grafts. Establishment of donor myeloid cells correlated with better survival, presumably because donor chimerism of the myeloid lineage correlated with donor origin of lymphocytes. Lack of CD4+ cell reconstitution and persistent need for IVIG were both significantly associated with poor outcome. Finally, the type of SCID appears to affect outcome, as specifically those with Artemis mutations have a 6-fold higher risk for poor outcome. These patients had a higher incidence of chronic papilloma virus infections, malnutrition, and chronic GVHD. Other studies indicate that survival generally is higher among B+ compared to B- SCID patients, particularly after alternative donor HCT [14].
Most other centers report comparable results, although in smaller series. The general experience is that genotypically HLA-identical marrow transplantation restores T cell immunity in >90% of unconditioned SCID patients, although B cell reconstitution occurs in only half of these patients [8, 15]. Despite the use of preparative regimens, recipients of T-depleted haploidentical marrow have delayed immune reconstitution, with 3–6 months required for development of antigen responsive T cells, and commonly multiple marrow infusions are needed [16]. B lymphocyte reconstitution is generally suboptimal and most patients require continued immunoglobulin support. The EBMT analysis found long-term functional T cells in about 80% of recipients of HLA-sibling grafts and 90% of B+ SCID recipients of haploidentical grafts; in contrast, functional T cells were observed in only 66% of B- SCID patients (p=.002). Long-term B cell function was less robust in all cohorts: 88% of B+ and 63% of B- SCID recipients of HLA-identical sibling grafts, and 66% of B+ and 44% of B- SCID recipients of haploidentical grafts, respectively. Certain SCID phenotypes may require a preparative regimen, for example patients with reticular dysgenesis given T-depleted grafts appear to have improved outcome if given high intensity conditioning with subsequent reconstitution of normal myeloid cells [17]. B- SCID patients also appear to benefit from conditioning [14].
The role of conditioning for unrelated grafts is the same as for T-depleted haploidentical grafts, in that it may facilitate establishment of donor B lymphocyte chimerism, however, that benefit may be offset by regimen-related toxicities. In 1992 Filipovich and colleagues reported their initial experience with unrelated marrow grafts for 8 SCID patients, of whom 5 were given high intensity conditioning [18]. Graft rejection occurred in 2 of the 3 unconditioned patients, although both survived long term after a second transplant with high intensity conditioning. Among the conditioned patients, 2 died within the first 100 days after HCT, while the others survived long term with improved immune function. Subsequently larger series have shown excellent outcome after high intensity conditioning followed by HLA-matched unrelated grafts, with about 80% survival [19, 20]. Compared to haploidentical recipients, unrelated marrow recipients had significantly lower risk for interstitial pneumonitis, graft failure, acute and chronic GVHD, and abnormal T cell receptor diversity [19]. Thus, immune reconstitution after T-replete unrelated donor transplantation appears to be faster compared to T-depleted haploidentical HCT, and often normal B cell function is achieved.
Outcomes for unrelated umbilical cord blood have been reported in small series and appears equivalent to that of matched unrelated marrow. Bhattacharya et al reported success in establishing well-matched (6/6 or 10/10 HLA match) umbilical cord blood grafts without conditioning [21]. The median time to achieving an absolute T cell count of more than 200 cells/ml among 5 surviving SCID patients was about 60 days, and mixed or full donor B cell engraftment was observed in 4 of these. Diaz reported 11 SCID patients, 9 given high intensity and 2 given reduced intensity conditioning, 7 and 1 of these, respectively, survive long term [22]. High intensity conditioning generally has been employed in recipients of HLA-mismatched cord blood units, with comparable results [20].
The condition of the patient before HCT correlates strongly with the risk of death after HCT irrespective of the graft source. In particular, infections and pulmonary disease are associated with significantly worse outcomes [12, 14, 23]. The most common cause of death in the first 6 months after HCT is infection, thus it is not surprising that pre-existing infection is detrimental to success. Indeed, a pre-existing pulmonary infection confers a 2-to 3-fold increased risk of death following HCT [14]. Therefore, every patient with SCID should have a thorough evaluation for infection and occult pulmonary disease. Liver enzyme elevations may indicate maternal T cell-mediated GVHD or underlying liver dysfunction, the latter is commonly associated with untreated ADA deficiency. Enzyme replacement therapy with polyethylene glycol (PEG) conjugated adenosine deaminase improves T cell function [24]. Since functional T cells pose an immunological barrier to engraftment, the general practice has been to stop PEG-ADA several weeks before HCT in order to “T-deplete” the recipient. However PEG-ADA also prevents or improves the liver injury found in ADA deficiency, thus, early stopping may result in hepatitis and increase the risk for post-transplant liver toxicity during the time required to establish endogenous enzyme production. A reasonable approach is to continue PEG-ADA unless no conditioning is contemplated, in which case pre-transplant discontinuation is warranted. Age of the patient is another important factor associated with survival. The best outcomes are reported for SCID patients given allogeneic transplant within the first year of life [12]. Older patients are more likely to have infections and organ dysfunction that contribute to higher mortality.
The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age. Buckley and colleagues reported better survival and the establishment of long-term functional T cells in patients with SCID who received HCT before 28 days of life (overall survival ((OS) 95%) compared to patients who were older (OS 74%) [25]. Survival of 21 SCID infants, given no conditioning and transplanted with haploidentical T cell depleted marrow grafts before 28 days of age (neonatal cohort), was 95% compared to 74% of 96 older infants. Thymopoiesis, as measured by T cell receptor excision circles (TREC), was improved in the neonatal transplant cohort, however, no comparative improvement in B cell function was observed. Acute GVHD grades III–IV developed in only 16% of patients who received grafts mismatched for 2 or 3 HLA antigens. Several factors probably contributed to the improved survival observed in patients less than 28 days old. In particular, younger patients are less likely to have opportunistic infections and subsequent co-morbidities, malnutrition, and failure to thrive, all of which have been associated with increased mortality following HCT, but may also contribute to decreased thymic function. These results show that T cell depleted haploidentical marrow grafts are feasible at a very early age and that there is little benefit in delaying HCT in order to identify a better matched donor.
Once established, donor progenitor cells develop and mature in the vestigial thymus of the SCID patient. Buckley and colleagues demonstrated that T cell receptor (TCR) gene rearrangement occurs in donor T cell precursors resulting in the generation of naïve T cells [25, 26, 27]. Measurements of TCR repertoire show development of a broad diversity within the donor T cell pool, which persists over time. Patel and colleagues reported that thymopoiesis, as measured by TRECs and naïve CD4 cells, declined exponentially over time after HCT. Several studies have suggested that late graft failure or deterioration of thymopoiesis may jeopardize long-term T cell function [28]. In contrast, recent studies have shown that thymic output of T cells and T cell diversity remain normal for decades after HCT in approximately 80% of patients [29, 30]. The degree of early T cell reconstitution appears to be strongly associated with the long-term stability of T cell function, thus, patients at most risk for poor T cell function or loss of T cell grafts are those with low numbers of TRECs and naïve-CD4 cells within the first few years after HCT [13, 31]. Alain Fischer’s team in Paris found that donor chimerism of the myeloid lineage correlated with higher CD4+ T cell counts long term, and that donor myeloid chimerism was limited to patients who received high intensity conditioning. Other factors that may be associated with higher risk for poor long-term T cell reconstitution are SCID phenotypes that lack B cells, presence of NK cells, and possibly young age at time of HCT. As noted above, long term B cell reconstitution is common only among patients given high intensity conditioning regimens [13, 15].
Primary T cell immunodeficiencies other than SCID
Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Nonetheless, the immune dysfunction leads to progressive decline from opportunistic infections, autoimmune phenomena, and a propensity to develop malignancies, particularly lymphoma. Several of the genetic mutations implicated in SCID also have been found to be present in patients with PTCD, thus termed “leaky SCID”. New genetic mutations also have been characterized, while the genetic causes in many patients remain unrecognized [32, 33, 34]. The more common of these rare disorders are listed in Table 2.
Table 2. Primary T cell immunodeficiency syndromes commonly referred for HCT
Abbreviations:
HIGM, Hyper IgM;
HLA, Human leukocyte antigen;
HSM, hepatosplenomegaly;
IPEX, Immunodeficiency-polyendocrinopathy-enteropathy X-linked;
XLP, X-linked lymphoproliferative
|
Syndrome |
Mutation |
Clinical features |
Laboratory features |
|---|---|---|---|
|
Omenn’s |
RAG1 or RAG2 |
HSM |
Eosinophilia |
|
ZAP70 |
ZAP70 |
CD8+ lymphopenia |
|
|
HIGM |
CD40L or CD40 |
X-linked |
High IgM & low IgG levels |
|
Common Variable Immunodeficiency |
Unknown |
Autoimmunity |
Low IgG |
|
Cartilage Hair Hypoplasia |
endoribonuclease RMRP |
Dwarfism |
|
|
Wiskott Aldrich |
WASP |
Eczema |
Thrombocytopenia |
|
IPEX |
FOXP3 |
X-linked |
|
|
XLP |
SH2D1A |
X-linked |
Hypogammaglobulinemia |
|
Bare Lymphocyte syndrome (Class II HLA deficiency) |
RFXANK, RFX5, RFSAP, CIITA |
Pulmonary infection |
Hypogammaglobulinemia |
|
Class I HLA deficiency |
TAP1 or TAP2 |
CD8 lymphopenia |
|
|
DiGeorge syndrome |
10p13 or 22q11.2 |
Hypocalcemia |
CD3 lymphopenia |
Until gene therapy is perfected, allogeneic marrow transplantation remains the only curative therapy available for these disorders. In general, conventional regimens have included both immunoablative and myeloablative agents to overcome residual immune barriers to engraftment and to ensure multi-lineage chimerism. The combination of busulfan (1 mg/kg x 16 doses) and cyclophosphamide (200 mg/kg total dose), with or without anti-thymocyte globulin is the most commonly used regimen. Our experience indicates that busulfan is metabolized faster in young patients, therefore in order to optimize engraftment it is prudent to adjust the daily doses to achieve steady state concentration (Css) of >200 ng/ml in recipients of HLA-identical sibling grafts and >400 ng/ml in recipients of HLA-matched unrelated grafts [35].
In 2003 the EBMT reported a retrospective analysis of outcome for patients with primary immunodeficiency disease other than SCID [12, 36]. A higher incidence of engraftment was reported in patients who received HLA-identical sibling grafts (99%), compared to those who received haploidentical or unrelated donor grafts (75–80%). In addition, survival at 3 years was better for patients who received HLA-identical sibling grafts (71%) compared to haploidentical grafts [42% (p=.0006)]. Survival after HLA-matched unrelated donor grafts was 59%, which was not statistically significantly different from the HLA-identical sibling cohort. The main cause of death following HCT was infection.
Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Overall survival was 63% and 35% after HLA-identical sibling grafts or mismatched grafts, respectively [12, 36]. Unfortunately, and in contrast to the results for SCID, the EBMT study found no improvement in survival of the non-SCID cohorts over the two decades included in the analysis, thus highlighting important differences and problems associated with PTCD compared to SCID. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT. Given that a conditioning regimen is necessary to ensure engraftment, the associated risks for organ toxicity, hemorrhage, and infection are compounded by these co-morbidities. Several studies have associated inferior survival with presence of co-morbidities, including opportunistic infections, Epstein-Barr virus lymphoproliferation, and pulmonary dysfunction [8, 23]. Among boys with X-linked hyper-IgM (XHIM) excessive mortality has been associated with the presence of pulmonary infection or liver disease at time of HCT [37].
In theory, split chimerism (donor T/host B chimerism) or partial donor T cell chimerism should be sufficient to ameliorate the immune dysfunction in most types of PTCD. Accordingly, reducing the intensity of conditioning may be a strategy to reduce regimen-related toxicity without sacrificing immune reconstitution. Specific factors associated with the molecular defect must be taken into consideration, as partial chimerism may not be sufficient for some defects. DiGeorge syndrome and the Bare Lymphocyte syndromes (BLS) pose particular challenges, because the T cell deficiency results from inadequate thymopoiesis, caused by absence of the thymus or absence of HLA molecules on the thymic epithelial cells, respectively. The molecular defects that cause BLS block the transcription of HLA genes; therefore antigen-presenting cells also are defective. Hence, donor chimerism must be established in B cell and dendritic cell lineages. In both disorders, absence of thymic function may prevent formation of naïve donor T cells; therefore full chimerism provides the most likely chance that a broad range of donor antigen-specific memory cells may be established long term.
Molecular deficits that allow T cell proliferation, but preclude intercellular interactions, such as X-linked hyper-IgM (XHIM) syndrome or Immune Dysregulation-Polyendocrinopathy-Enteropathy X-linked (IPEX) syndrome, generally require conditioning in order to prevent T cell mediated graft rejection; however, partial T cell chimerism appears to restore immune function as well as full donor chimerism [38, 39]. The autoimmune manifestations of the IPEX syndrome are caused by absence of CD4+CD25+ FOXP3+ regulatory T cells (Tregs), important for sustaining self-tolerance. Normal numbers of FOXP3 expressing CD4+CD25+ cells have been observed in boys with mixed donor/host chimerism, and several case reports indicate that mixed chimerism is sufficient to ameliorate many of the manifestations of IPEX, including the enteropathy, anemia, failure to thrive, and the susceptibility to infections. Curiously, we and others have observed improvement in diabetes, although in theory autoimmune-mediated islet cell destruction happens well before HCT is carried out [38]. The most common cause of the XHIM syndrome is a mutation in the CD40 ligand gene, which is expressed by T cells and provides a critical signal for B cells to switch antibody production from IgM to IgG subtypes. Theoretically, the introduction of some normal CD40 ligand-expressing T cells should be sufficient to reverse the disease, even if B cells of host origin remain. Amelioration of disease symptoms with mixed chimerism has been observed for some boys treated for XHIM, although no detailed analysis of B cell function was reported [40, 41].
Wiskott-Aldrich Syndrome (WAS). HCT offers significantly improved survival chances for patients with WAS, without which about 50% will die from infection, autoimmune disease, or lymphoproliferative disease by the third decade of life [42]. The WAS mutation affects lymphoid and hematopoietic compartments, both of which are corrected by HCT. Accordingly most patients are conditioned with both immunosuppression and high dose chemotherapy to facilitate multilineage donor cell engraftment. Figure 1 shows cell counts in a patient who was too ill with opportunistic infections to receive high dose conditioning and became a split chimera after reduced intensity conditioning and unrelated marrow transplantation. Following transplantation the T cell immune defect was corrected, but thrombocytopenia persisted as did host CD33+ cells. After the infections resolved, a second graft was given with a high intensity (directed at myeloid cells), but without immunoablative preparative regimen, resulting in amelioration of thrombocytopenia as the CD33+ compartment converted to donor type. The importance of achieving full donor chimerism was shown recently in a retrospective analysis of results in 96 patients, which showed an almost 2-fold reduction in mortality among patients with full chimerism compared to those with mixed or split chimerism [43]. Mixed chimerism also is associated with a significantly higher risk for developing autoimmune manifestations after HCT.
Figure 1. Correction of thrombocytopenia in Wiskott-Aldrich correlates with donor chimerism of CD33+ cell subset
At 30 days after hematopoietic cell transplant, a high proportion of both CD3 (gray line) and CD33 (black line) subsets mark as donor origin. Over time, the proportion of donor CD3 cells remains stable, while the proportion of donor CD33 cells decreases. The platelet count (black dashed line) reaches a normal level when the CD33 donor chimerism is high, and falls proportionately with the fall in donor CD33 chimerism.

HCT using HLA-identical sibling marrow grafts is highly successful in treating WAS, with approximately 88% event-free survival [43]. The combination of busulfan (1 mg/kg x 16 doses) and cyclophosphamide (200 mg/kg total dose), with or without anti-thymocyte globulin is the most commonly used conditioning regimen. Busulfan is metabolized faster in younger patients, therefore it is prudent to monitor levels and target the dose to achieve a Css of greater than 200 ng/ml to assure engraftment [35]. An EBMT analysis determined that patient age, disease severity, and splenectomy, among other factors, did not affect outcome [43].
Results of alternative donor HCT for treatment of WAS have improved over time, particularly for recipients of unrelated marrow grafts. Most recent studies have shown approximately 70%–78% long-term survival [43, 44]. In a 2001 study facilitated by the International Bone Marrow Transplant Registry (IBMTR), age of 5 years or older was associated with an increased risk of mortality after HCT. Survival for patients younger than 5 years was about the same as for recipients of HLA-identical sibling grafts. In addition, several studies found comparable survival rates among recipients of HLA-matched related and unrelated grafts [44, 45]. The most commonly used regimen was a combination of busulfan, cyclophosphamide, and ATG. In our experience, targeting the dose of busulfan to achieve a C SS above 400 ng/ml facilitates engraftment [35].
Encouraging results have also been reported for umbilical cord blood transplants, but most information comes from case reports or part of smaller series of patients with immune deficiencies. Among 15 patients reported by Ozsahin, et al, event-free survival was approximately 70%, similar to recipients of unrelated marrow grafts [44]. Most patients in these reports were conditioned with the combination of busulfan, cyclophosphamide, and antithymocyte globulin, which the Japanese group found to be an important factor for improved survival when compared to other regimens [44]. Reconstitution of immunity after cord blood approximates that observed with unrelated marrow grafts.
There is more information about haploidentical transplants for WAS, although the historical results are less encouraging. The EBMT study showed a 4–5-fold increase in mortality after haploidentical compared to HLA-identical sibling grafts [43]. Others have reported similar results [36, 44, 46]. These reports show a high incidence of graft failure and poor immune reconstitution following T-depleted haploidentical marrow grafts. The Tubingen team provided a promising case report of “mega-dose” purified CD34+ haploidentical grafts used to overcome the barrier to engraftment without engendering GVHD [47].
Inherited immune defects not primarily affecting T cells
A wide range of rare immune deficiency syndromes result from defects in B lymphocytes, NK cells, or nonlymphocytic subsets including neutrophils (Table 3).
Table 3. Histiocytic and myeloid immune deficiency syndromes commonly referred for HCT
Abbreviations:
FHL, Familial hemophagocytic lymphohistiocytosis;
LCH, Langerhans cell histiocytosis
|
Syndrome |
Mutation |
Clinical features |
Laboratory features |
|---|---|---|---|
|
Histiocytic disorders |
|||
|
FHL |
PRF1 |
Fever |
Pancytopenia |
|
Multifocal LCH |
unknown |
Bone lesions |
Anemia |
|
Myeloid disorders |
|||
|
Chronic Granulomatous Disease |
p91PHOX |
Pneumonia |
Catalase-positive bacteria |
|
Chediak-Higashi Syndrome |
CHS1 |
Pyogenic infections |
Neutropenia |
|
Leukocyte Adhesion defect |
β-2 integrin |
Bacterial infections |
Leukocytosis |
|
Kostmann’s neutropenia |
GCSF-R |
Bacteremia/sepsis |
Neutropenia |
|
Shwachman-Diamond Syndrome |
Unknown |
Pancreatic enzyme deficiency |
Neutropenia |
The individual immune defects predispose the patients to specific infections, for example with Aspergillus in patients with chronic granulomatous disease (CGD) or staphylococcus aureus in leukocyte adhesion deficiency (LAD)-I, and are associated with distinctive co-morbidities, such as infiltrative pulmonary or central nervous system disease in hemophagocytic lymphohistiocytosis (HLH) or recalcitrant colitis in CGD. As above, the decision to treat with HCT must take into consideration the prognosis of the disorder with available supportive care, the presence of co-morbidities that might increase the risk of mortality following HCT, and the availability of a suitable donor. Unfortunately, because these diseases are rare, meaningful prospective studies reporting on large series of patients with a single disease entity are not available. Within the European retrospective study, survival for specific subsets, 48 patients with phagocytic disorders, and 90 patients with hemophagocytic disorders, was reported to be approximately 70% and 68%, respectively, for recipients of HLA-identical sibling grafts. The small number of patients with phagocytic cell disorders had a similar outcome after transplantation of unrelated marrow, in contrast to patients with hemophagocytic disorders in whom survival was only 28% after unrelated grafts.
Studies that include larger numbers of patients with single diagnoses are limited to a few disorders such as CGD and HLH. The prognosis for CGD patients has improved considerably with more aggressive use of gamma-interferon and antibiotic prophylaxis. HCT is indicated for patients with recurrent life-threatening infections or organ dysfunction caused by refractory granulomatous disease [48]. A series of patients transplanted with HLA-identical sibling marrow (n=10) or unrelated marrow or cord blood (n=10) was reported recently from the United Kingdom [49]. Most patients were conditioned with busulfan and cyclophosphamide, and alemtuzumab was given to recipients of unrelated grafts. Survival was reported to be 90% with a median follow-up of 61 months; one patient in each group died from disseminated infection. Neutrophil oxidative burst was normalized in patients with mixed as well as full donor chimerism. Del Giudice et al published a review of case reports and small series of patients with CGD that included several long-term survivors with stable mixed chimerism, consistent with the notion that a small proportion of normal cells improves disease symptoms [50].
Without HCT, the prognosis for patients with HLH is poor even with intensive supportive care and anti-inflammatory regimens that include etoposide, cyclosporine, and prednisone [51, 52]. The outcome is considerably improved when HCT is performed after control of the initial inflammatory state is gained and infiltrative disease has resolved. The HLH 94 protocol reported 50–60% overall survival for the 113 children entered into the study; overall survival was 65% for the subgroup of 65 children given HCT. The study results suggested that intrathecal chemotherapy plays an important role in gaining disease control [52]. A retrospective analysis of 91 patients in the CIBMTR registry given unrelated marrow grafts found 53% overall survival [53]. Most patients were conditioned with busulfan, cyclophosphamide, and etoposide, with or without ATG. Survival was worse among the small subgroup with active disease at time of HCT, as well as among recipients of HLA-mismatched grafts. Disease manifestations resolved among patients with mixed as well as full donor chimerism. Early mortality (before day 100) was 32%, however, suggesting that a reduced intensity conditioning regimen might be of benefit.
Development of reduced toxicity regimens
Conditioning regimens that do not employ agents at doses resulting in long-lasting marrow aplasia are referred to as reduced intensity conditioning (RIC) regimens. Until recently, those regimens have been used routinely for only two conditions: severe aplastic anemia and SCID. Regimens for aplastic anemia have included immunosuppressive agents alone to overcome the allo-immune rejection responses, since these patients are thought to have "unoccupied" marrow space. These reduced intensity regimens have resulted in a markedly lower incidence of both early and late complications [54, 55]. SCID patients have no immune system capable of rejecting the graft, and therefore do not require conditioning except in the instances discussed above [11].
As the power of the graft vs. leukemia (GVL) effect became evident in the late 1970s and early 1980s, subsequent studies found that donor lymphocyte infusions (DLI) could be used to treat leukemic relapse after HCT [56>, 57]. The success of DLI set the stage for the introduction of reduced intensity conditioning for HCT, based on the hypothesis that the graft itself created the needed space through a subclinical GVH reaction directed toward recipient hematopoietic cells. Based on insights from animal models and armed with new potent immunosuppressive agents such as 2-CDA and fludarabine, investigators in Texas, Israel, Seattle, Boston, and Washington, DC pioneered less toxic regimens that facilitated partial or full chimerism in most patients [58, 59, 60, 61, 62, 63, 64].
These studies demonstrated that intensive immunosuppression alone following stem cell infusion was sufficient to establish full or partial donor chimerism and that conditioning was not required for creation of marrow space. The extent of donor cell engraftment following low intensity regimens depends on multiple factors, including the degree of intensity of the preparative regimen, the source of hematopoietic cells (marrow vs. peripheral blood stem cells), the degree of HLA-matching, and the extent of T cell depletion. Most low intensity protocols use PBSC to facilitate engraftment and enhance GVL reactions, as the product may contain 10-fold greater numbers of T cells and 4-fold greater number of hematopoietic stem cells compared to marrow [65].
There are several reasons for the further development of low intensity regimens for the establishment of mixed chimerism in patients with Non-SCID primary immune deficiency disorders. First, the potential risks of high dose conditioning regimens include early treatment related mortality and late effects, such as infertility, hormonal dysfunction, growth failure, and secondary malignancies. These risks may deter patients and families from seeking treatment before co-morbidities arise. Second, as discussed earlier, the risk for regimen-related mortality increases significantly among patients with disseminated infection, pulmonary disease or other organ dysfunction. Third, reversal of disease symptoms with partial chimerism, which may be achievable with low intensity conditioning, has been demonstrated in a number of studies [36, 66].
The main challenge in translating the success of protocols using RIC to patients with primary immune deficiency is the reliance on PBSC grafts, which may be difficult (or impossible) to collect from pediatric donors; also it confers a high risk of GVHD. Some progress has been made using marrow or CD34+ selected PBSC. Some results with HLA-matched related or unrelated marrow using RIC are summarized in Table 4.
Table 4. Intensity conditioning regimens and transplant outcome in immunodeficiency syndromes
Abbreviations:
ATG, anti-thymocyte globulin;
BM, bone marrow;
CB, cord blood;
CGD, chronic granulomatous disease;
DLI, donor lymphocyte infusion;
EBV-LPD, Epstein Barr virus lymphoproliferative disease; Flu, fludarabine;
HCT, hematopoietic cell transplant;
IPEX, Immunodeficiency-polyendocrinopathy-enteropathy X-linked;
Mel, melphalan;
MSD, matched sibling donor;
PBSC, peripheral blood stem cells;
PID, primary immune deficiency (nonSCID);
SCID, severe combined immune deficiency;
SC-M, severe co-morbities;
TBI, total body irradiation
Author | Diagnosis | Regimen | Donor | Rejection (No.) | Survival (No.) | FU (mo) |
|---|---|---|---|---|---|---|
Reduced Intensity Conditioning | ||||||
(Rao et al. 2005 [67]) | 27 PID/ 6 SCID | Flu/ Mel/Campath | BM | 0 | 31 | |
(Amrolia et al. 2000 [68]) | 6 ID/ 2 SCID | Flu/ Mel/ ATG | 0 | 7 | 6-18 | |
(Rao et al. 2007 [38]) | 4 IPEX | Flu/ Mel/Campath | BM | 0 | 4 | 6-25 |
(Cohen et al. 2007 [69]) | 7 PID/ EBV-LPD | Flu/ Mel/Campath | BM or PBSC | 0 | 7 | 0 |
Minimal Toxicity (non-myeloablative) Conditioning | ||||||
(Horwitz et al. 2001 [70]) | 10 CGD | Flu/ Cy/ ATG | CD34+ PBSC | 1 | 7 | 16-26 |
(Burroughs et al. 2007 [71]) | 10 PID+SC-M | Flu / 2 Gy TBI | PBSC | 1 | 7 | 9-96 |
A high rate of engraftment of marrow grafts has been reported after the combination of fludarabine and melphalan plus, an in vivo T-depleting agent, such as ATG or Campath®, and appears to be associated with low mortality rates [38, 67, 68, 70]. The combination of cyclophosphamide, fludarabine, and ATG has been studied as a low-intensity regimen to facilitate engraftment of CD34+ selected PBSC [70]. In the latter study, the benefit of in vivo and ex vivo T-depletion for reducing GVHD was at least partially abrogated by the use of DLI to improve the level of donor cell chimerism. The Seattle group has studied the combination of fludarabine and low-dose TBI in patients who would be expected to have very poor survival following conventional conditioning for HCT, such as those with disseminated opportunistic infections, mechanical ventilation, or other organ damage. No regimen-related mortality was observed in the first cohort given 2 Gy TBI, however chronic GVHD was observed in 70% of patients, presumably related to the use of PBSC grafts [71]. The substitution of marrow for PBSC in the subsequent cohort appears promising, and early mortality has not been increased despite increasing the dose of TBI to 4 Gy (Figure 2). Taken together, these studies suggest that low-intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
Figure 2. Survival of patients with severe infections or pulmonary disease after reduced intensity conditioning HCT is improved with bone marrow as the sole source of allogeneic hematopoietic cells.
The first cohort of patients (dashed line) was conditioned with fludarabine and 2 Gy total body irradiation and most patients received peripheral blood stem cell grafts. The second cohort (solid line) was conditioned with fludarabine and 4 Gy total body irradiation and was given marrow grafts.

Acknowledgements
This work was supported by National Institute of Health grant NHLBI grant HL36444 and National Cancer Institute grant CA18029.
References
3. Ohlen C, Hoglund P, Sentman, CL, Carbone E, et al. Inhibition of natural killer cell-mediated bone marrow graft rejection by allogeneic major histocompatibility complex class I, but not class II molecules. European Journal of Immunology. 1995;25;1286-1291.
4. George T, Yu, YY, Liu, J, Davenport C, et al. Allorecognition by murine natural killer cells: lysis of T-lymphoblasts and rejection of bone-marrow grafts (Review). Immunological Reviews. 1997;155;29-40.
6. Morisaki H, Morisaki T, Nakahori Y, Ogura H, et al. Genotypic analysis using a Y-chromosome-specific probe following bone marrow transplantation. American Journal of Hematology. 1988;27:30-33. pmid: 3281450.
8. O'Reilly RJ, Keever CA, Small TN, Brochstein J. The use of HLA-non-identical T-cell-depleted marrow transplants for correction of severe combined immunodeficiency disease. Immunodeficiency Reviews. 1989;1:273-309. pmid: 2698644.
11. Fischer A, Landais P, Friedrich W, Morgan G, et al. European experience of bone-marrow transplantation for severe combined immunodeficiency. Lancet. 1990;336:850-854. pmid: 1976883.
12. Antoine C, Muller S, Cant A, Cavazzana-Calvo M, et al. European Group for Blood and Marrow Transplantation & European Society for Immunodeficiency. Long-term survival and transplantation of haemopoietic stem cells for immunodeficiencies: report of the European experience 1968-99. Lancet. 2003;361:553-560.
14. Bertrand Y, Landais P, Friedrich W, Gerritsen B, et al. Influence of severe combined immunodeficiency phenotype on the outcome of HLA non-identical, T-cell-depleted bone marrow transplantation: a retrospective European survey from the European group for bone marrow transplantation and the European Society for immunodeficiency. Journal of Pediatrics. 1999;134:740-748.
23. Filipovich AH. Stem cell transplantation from unrelated donors for correction of primary immunodeficiencies. Immunology and Allergy Clinics NA. 1996;16:377-392.
24. Chan B, Wara D, Bastian J, Hershfield MS, et al. Long-term efficacy of enzyme replacement therapy for adenosine deaminase (ADA)-deficient severe combined immunodeficiency (SCID). Clinical Immunology. 2005;117:133-143.
29. Sarzotti-Kelsoe M, Win CM, Parrott RE, Cooney M, et al. Thymic output, T-cell diversity, and T-cell function in long-term human SCID chimeras. Blood. 2009;114:1445-1453. pmid: 19433858.
32. Liston A, Enders A, Siggs OM. Unravelling the association of partial T-cell immunodeficiency and immune dysregulation (Review). Nature Reviews Immunology. 2008;8:545-558. pmid: 18551129.
33. Cunningham-Rundles C, Ponda PP. Molecular defects in T- and B-cell primary immunodeficiency diseases (Review). Nature Reviews Immunology. 2005;5:880-892.
34. Fischer A. Primary T-lymphocyte immunodeficiencies (Review). Clinical Reviews in Allergy and Immunology. 2001;20:3-26. pmid: 11269227.
35. Slattery JT, Sanders JE, Buckner CD, Schaffer RL, et al. Graft-rejection and toxicity following bone marrow transplantation in relation to busulfan pharmacokinetics. Bone Marrow Transplantation. 1995;16:31-42. pmid: 7581127.
41. Khawaja K, Gennery AR, Flood TJ. Bone marrow transplantation for CD40 ligand deficiency: a single centre experience. Archives of Disease in Childhood. 2001;84:508-511. pmid: 11369571.
44. Ozsahin H, Le Deist F, Benkerrou M, Cavazzana-Calvo M, et al. Bone marrow transplantation in 26 patients with Wiskott-Aldrich syndrome from a single center. Journal of Pediatrics. 1996;129:238-244. pmid: 8765621.
46. Bock M, Maiwald M, Kappe R. Polymerase chain reaction-based detection of dermatophyte DNA with a fungus-specific primer system. Mycoses. 1994;37:79-84. pmid: 7845424.
50. Del Giudice I, Iori AP, Mengarelli A, Testi AM, et al. Allogeneic stem cell transplant from HLA-identical sibling for chronic granulomatous disease and review of the literature (Review). Annals of Hematology. 2003;82:189-192.
51. Sung L, King, SM, Carcao M, Trebo M, Weitzman, S.S. Adverse outcomes in primary hemophagocytic lymphohistiocytosis. Journal of Pediatric Hematology/Oncology. 2002;24:550-554.
55. Storb R, Thomas ED, Buckner CD, Clift RA, et al. Marrow transplantation in thirty "untransfused" patients with severe aplastic anemia. Annals of Internal Medicine. 1980;92:30-36. pmid: 6985782.
61. Khouri IF, Keating M, Körbling M, Przepiorka D, et al. Transplant-lite: induction of graft-versus-malignancy using fludarabine-based nonablative chemotherapy and allogeneic blood progenitor-cell transplantation as treatment for lymphoid malignancies. Journal of Clinical Oncology. 1998;16:2817-2824. pmid: 9704734.
64. Sykes M, Preffer F, McAfee S, Saidman SL, et al. Mixed lymphohaemopoietic chimerism and graft-versus-lymphoma effects after non-myeloablative therapy and HLA-mismatched bone-marrow transplantation. Lancet. 1999;353:1755-1759. pmid: 10347989.
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "500" ["~SORT"]=> string(3) "500" ["CODE"]=> string(96) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov" ["~CODE"]=> string(96) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov" ["EXTERNAL_ID"]=> string(4) "1438" ["~EXTERNAL_ID"]=> string(4) "1438" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["ELEMENT_META_KEYWORDS"]=> string(0) "" ["ELEMENT_META_DESCRIPTION"]=> string(242) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитовHematopoietic cell transplantation for treatment of primary immune deficiencies" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(7407) "<p class="bodytext">Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима. </p> <p class="bodytext">ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов. </p> <p class="bodytext">Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК. </p> <p class="bodytext">Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте. </p> <p class="bodytext">Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК. </p> <p class="bodytext">ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций. </p> <h3>Ключевые слова</h3> <p> первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы </p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_META_TITLE"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_META_KEYWORDS"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_META_DESCRIPTION"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_PICTURE_FILE_ALT"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_PICTURE_FILE_TITLE"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_PICTURE_FILE_NAME"]=> string(100) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov-img" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(163) "Трансплантация гемопоэтических стволовых клеток для лечения первичных иммунодефицитов" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(100) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov-img" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(100) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov-img" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(100) "transplantatsiya-gemopoeticheskikh-stvolovykh-kletok-dlya-lecheniya-pervichnykh-immunodefitsitov-img" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(2) "80" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> bool(false) ["VALUE"]=> bool(false) ["DESCRIPTION"]=> bool(false) ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> bool(false) ["~DESCRIPTION"]=> bool(false) ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19084" ["VALUE"]=> string(22) "02/04/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "02/04/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19085" ["VALUE"]=> string(22) "05/02/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "05/02/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19086" ["VALUE"]=> string(22) "08/31/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "08/31/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19087" ["VALUE"]=> string(4) "1437" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1437" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(2) { [0]=> string(5) "19104" [1]=> string(5) "19105" } ["VALUE"]=> array(2) { [0]=> string(4) "1436" [1]=> string(4) "1437" } ["DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { [0]=> string(4) "1436" [1]=> string(4) "1437" } ["~DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19094" ["VALUE"]=> array(2) { ["TEXT"]=> string(55) "<p>Л. Барроуз, Э. Вулфри</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(43) "Л. Барроуз, Э. Вулфри
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19095" ["VALUE"]=> array(2) { ["TEXT"]=> string(168) "<p>Центр раковых исследований Фреда Хатчинсона и Университет Вашингтона, Сиэтл, США</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(156) "Центр раковых исследований Фреда Хатчинсона и Университет Вашингтона, Сиэтл, США
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19096" ["VALUE"]=> array(2) { ["TEXT"]=> string(7407) "<p class="bodytext">Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима. </p> <p class="bodytext">ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов. </p> <p class="bodytext">Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК. </p> <p class="bodytext">Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте. </p> <p class="bodytext">Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК. </p> <p class="bodytext">ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций. </p> <h3>Ключевые слова</h3> <p> первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(7251) "Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима.
ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов.
Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК.
Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте.
Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК.
ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций.
Ключевые слова
первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19090" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000077.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000077.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19100" ["VALUE"]=> array(2) { ["TEXT"]=> string(58) "<p>Lauri Burroughs (MD), Ann Woolfrey (MD)</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(46) "Lauri Burroughs (MD), Ann Woolfrey (MD)
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19101" ["VALUE"]=> array(2) { ["TEXT"]=> string(99) "<p>Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(87) "Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19102" ["VALUE"]=> array(2) { ["TEXT"]=> string(3680) "<p class="bodytext">Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen. </p> <p class="bodytext">SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age. </p> <p class="bodytext">Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT. </p> <p class="bodytext">In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high. </p> <h3>Keywords</h3> <p>Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3568) "Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen.
SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age.
Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT.
In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
Keywords
Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19091" ["VALUE"]=> string(79) "Hematopoietic cell transplantation for treatment of primary immune deficiencies" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(79) "Hematopoietic cell transplantation for treatment of primary immune deficiencies" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19097" ["VALUE"]=> string(3) "927" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "927" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19103" ["VALUE"]=> string(3) "930" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "930" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(13) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19100" ["VALUE"]=> array(2) { ["TEXT"]=> string(58) "<p>Lauri Burroughs (MD), Ann Woolfrey (MD)</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(46) "Lauri Burroughs (MD), Ann Woolfrey (MD)
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(46) "Lauri Burroughs (MD), Ann Woolfrey (MD)
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19102" ["VALUE"]=> array(2) { ["TEXT"]=> string(3680) "<p class="bodytext">Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen. </p> <p class="bodytext">SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age. </p> <p class="bodytext">Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT. </p> <p class="bodytext">In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high. </p> <h3>Keywords</h3> <p>Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3568) "Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen.
SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age.
Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT.
In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
Keywords
Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(3568) "Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen.
SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age.
Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT.
In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
Keywords
Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19090" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000077.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000077.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2010-en-000077.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19091" ["VALUE"]=> string(79) "Hematopoietic cell transplantation for treatment of primary immune deficiencies" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(79) "Hematopoietic cell transplantation for treatment of primary immune deficiencies" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(79) "Hematopoietic cell transplantation for treatment of primary immune deficiencies" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19101" ["VALUE"]=> array(2) { ["TEXT"]=> string(99) "<p>Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(87) "Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(87) "Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(2) { [0]=> string(5) "19104" [1]=> string(5) "19105" } ["VALUE"]=> array(2) { [0]=> string(4) "1436" [1]=> string(4) "1437" } ["DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { [0]=> string(4) "1436" [1]=> string(4) "1437" } ["~DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(2) { [0]=> string(59) "Lauri Burroughs" [1]=> string(56) "Ann Woolfrey" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19094" ["VALUE"]=> array(2) { ["TEXT"]=> string(55) "<p>Л. Барроуз, Э. Вулфри</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(43) "Л. Барроуз, Э. Вулфри
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(43) "Л. Барроуз, Э. Вулфри
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19084" ["VALUE"]=> string(22) "02/04/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "02/04/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "02/04/2010 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19085" ["VALUE"]=> string(22) "05/02/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "05/02/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "05/02/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19086" ["VALUE"]=> string(22) "08/31/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "08/31/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "08/31/2010 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19087" ["VALUE"]=> string(4) "1437" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1437" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(56) "Ann Woolfrey" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19096" ["VALUE"]=> array(2) { ["TEXT"]=> string(7407) "<p class="bodytext">Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима. </p> <p class="bodytext">ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов. </p> <p class="bodytext">Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК. </p> <p class="bodytext">Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте. </p> <p class="bodytext">Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК. </p> <p class="bodytext">ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций. </p> <h3>Ключевые слова</h3> <p> первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(7251) "Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима.
ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов.
Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК.
Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте.
Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК.
ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций.
Ключевые слова
первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(7251) "Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима.
ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов.
Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК.
Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте.
Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК.
ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций.
Ключевые слова
первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы
" } ["ORGANIZATION_RU"]=> array(37) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19095" ["VALUE"]=> array(2) { ["TEXT"]=> string(168) "<p>Центр раковых исследований Фреда Хатчинсона и Университет Вашингтона, Сиэтл, США</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(156) "Центр раковых исследований Фреда Хатчинсона и Университет Вашингтона, Сиэтл, США
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(156) "Центр раковых исследований Фреда Хатчинсона и Университет Вашингтона, Сиэтл, США
" } } } [5]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "80" ["~IBLOCK_SECTION_ID"]=> string(2) "80" ["ID"]=> string(4) "1441" ["~ID"]=> string(4) "1441" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["~NAME"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "10/20/2017 03:30:59 pm" ["~TIMESTAMP_X"]=> string(22) "10/20/2017 03:30:59 pm" ["DETAIL_PAGE_URL"]=> string(114) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh/" ["~DETAIL_PAGE_URL"]=> string(114) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(107828) "High-dose immunosuppressive therapy and autologous hematopoietic cell transplantation for autoimmune diseases: clinical experience
High-dose immunosuppressive therapy regimens
Two reports were published in the mid-late 1990s on the outcomes of concomitant autoimmune diseases after high-dose cytotoxic therapy and autologous HCT for a hematological malignancy [3, 4]. A majority of the patients achieved remissions of the concomitant autoimmune diseases early after treatment, but only 5 of 15 cases had sustained responses at last follow-up in one report, and all 4 patients presented relapsed in a second report. This experience indicated that there was a substantial risk of progression of the autoimmune disease after high-dose cytotoxic/immunosuppressive therapy (HDIT) designed for treatment of a hematological malignancy. Clinical trials of HDIT and autologous HCT specifically for autoimmune diseases were designed to intensify the immunosuppressive effect compared to standard cytotoxic regimens for treating hematologic malignancies. This was achieved by depleting T cells from the autologous hematopoietic cell graft or by adding other non-cytotoxic immunosuppressive agents to the HDIT regimen for in vivo T cell depletion. The HDIT regimens that have been investigated in clinical trials have had varying intensities. High-dose cyclophosphamide as a single agent has been considered a low-intensity regimen [5]. It is highly immunosuppressive but is not myeloablative. Clinical trials of high-dose cyclophosphamide have been conducted with and without the support of autologous HCT. Regimens which included TBI or high-dose busulfan were considered high-intensity and required support with autologous HCT.
Systemic depletion of autoreactive immune effector cells was the rationale for the early clinical trials of HDIT followed by HCT for severe autoimmune diseases. These clinical trials showed high initial response rates, and a significant proportion of patients achieved sustained remissions [6, 7, 8, 9, 10]. The sustained responses observed after recovery of the lymphocyte counts at 2 years may have resulted from a late immunomodulatory effect of the HDIT regimen [11, 12, 13]. The intensity of the HDIT regimen may be important for the disease remission to be sustained. In a report from the EBMT registry, sustained responses were observed in 78% of patients after a regimen with high-intensity conditioning compared to 68% with intermediate and 30% with low-intensity conditioning regimens (p=0.0001) [5]. The analysis of the registry data, although informative, had some limitations including variability of the diagnoses, patient selection criteria, and treatments (as well as having imbalances between diagnosis and type of HDIT regimen). The possible benefits must be weighed against the risk when selecting the level of intensity of the conditioning regimens.
High-dose single agent cyclophosphamide followed by autologous HCT for hematopoietic support was reported as one of the more frequently used HDIT regimens [5]. When the doses of cyclophosphamide (100 vs. 200 mg/kg) were compared in a small study of patients with rheumatoid arthritis (RA), remissions were longer with the higher dose of cyclophosphamide [14]. However, all patients eventually relapsed regardless of the dose. Relapse rates were also high in a systemic sclerosis (SSc) study in which patients were treated with high-dose cyclophosphamide (200 mg/kg) alone. Four of 11 patients died by 18 months after treatment (three from progression), and another four patients had progressed and required secondary treatment [15]. The addition of antithymocyte globulin (ATG) to cyclophosphamide may improve the response rate and duration. Experience has continued to accrue with high-dose cyclophosphamide in combination with ATG [8, 16, 17, 18]. The regimen has been effective for inducing remissions and has been well tolerated; however, a longer follow-up is still required to assess the durability of responses. Since the regimen is not myeloablative, high-dose cyclophosphamide (200 mg/kg) as a single agent without autologous HCT has also been investigated [19, 20]. Without the support of an autologous hematopoietic cell graft after high-dose cyclophosphamide, the median time to recover neutrophil counts was about 2–3 days longer than with HCT, but the upper limit of the range was 7 days longer [8, 20]. Only 36% of the patients were reported to have durable complete remissions. In this small experience, there did not appear to be any benefit to withholding the infusion of an autologous hematopoietic cell graft.
Treatment-related mortality was 14% and 3%, respectively, in the groups reported from the EBMT registry who received the high and the low conditioning intensity regimens, but there was no significant difference in overall survival [5]. Patients with multiple sclerosis (MS) and RA had lower treatment-related mortality than patients with systemic sclerosis (SSc) and systemic lupus erythematosus (SLE) who had significant internal organ dysfunction related to their disease. Treatment with immunosuppressive agents including corticosteroids before transplant, especially in the SLE group, likely predisposed patients to the infectious complications experienced after HDIT. Better patient selection and modifications to the treatment regimen appear to have reduced the risks of treatment-related mortality in recent years [6, 9, 21]. In the SCOT clinical trial in which patients with SSc are randomized between two treatment arms, either HDIT followed by autologous HCT or pulse cyclophosphamide, there was only one treatment-related death as of late 2009 [22]. This improvement was attributed to modifications made to the treatment regimen and patient selection based on insights gained from the pilot study [7, 22].
Specific Autoimmune Diseases and High-Dose Immunosuppressive Therapy Followed by Autologous Hematopoietic Cell Transplantation
HDIT has been performed most commonly for MS, SSc, SLE, RA and juvenile idiopathic arthritis (JIA) [5], but promising results have also been observed in other autoimmune diseases.
Multiple sclerosis MS is an inflammatory disorder of the central nervous system manifesting as acute focal demyelination and axonal loss followed by sclerotic scarring. It is postulated that myelin proteins are targeted by autoreactive immune effector cells [23]. The pathology shows a predominant T cell response both in the demyelinated lesion and in perivascular spaces. Axonal injury is evident in both the MS lesions and the normal-appearing white matter. The clinical manifestations of the disease are manifold and include loss of vision from optic neuritis, diplopia, sensory loss and paresthesias, vertigo, fecal or urinary incontinence, impotence, intellectual decline, paroxysmal pain, recurrent infections, and loss of coordination or paralysis. Most MS patients (85%) present with relapsing-remitting disease, and about 50% will evolve to the secondary progressive type of MS over 10 years. The other 15% of patients have progressive disease from onset (primary). The standard for measuring outcome in studies of MS is the Kurtzke Expanded Disability Status Scale (EDSS) and, more recently, the Multiple Sclerosis Functional Composite (MSFC). At 20 years after onset, patients with MS had 85% of the expected survival. Despite responses to immunomodulating agents, no standard therapy is curative or has been demonstrated to prevent development of a progressive clinical course. Disease-modifying therapies in relapsing-remitting MS include interferon (IFN) beta-1a, IFN beta-1b, glatiramer acetate (GA), mitoxantrone and natalizumab [24]. Treatment reduced the clinical relapse rates by 30–68%, with mitoxantrone and natalizumab being more effective than IFN or GA. These agents, however, remain inadequate in completely preventing relapses and progression. There is no effective therapy for primary or secondary progressive MS.
Results from at least 11 clinical trials of HDIT and autologous HCT for MS have been reported from transplant centers in the Americas, Europe and Asia (Table 1) [8, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34]. Although there was variability in the design of each of the early clinical trials, they all included patients with advanced MS and the progressive type of the disease. All patients received high-dose combination chemotherapy or total body irradiation (TBI) and cyclophosphamide. In 10 of the 11 clinical trials, the hematopoietic cell grafts consisted of “mobilized” peripheral blood cells, and seven of the trials included T cell depletion with CD34-selection. In the clinical trials reported before 2008, the overall treatment-related mortality was 2.8% (4/145) and the progression-free survival or rate of neurological stability reported in the individual clinical trials ranged from 36–95% at 2–3 years after treatment (Table 1). Five patients (3.5%) died after progression of their disease and further loss of neurological function or other complications. In a report by Saccardi et al. of 19 MS patients with high levels of disease activity based on magnetic resonance imaging (MRI) of the brain and sustained clinical deterioration, there was a marked reduction of gadolinium (Gd)-enhancing lesions in the brain after the HDIT regimen, which was sustained up to 5 years after treatment (Table 1) [31]. Although HDIT followed by autologous HCT appears highly effective for suppressing MRI findings of MS disease activity, a significant loss of brain volume has been noted after HDIT, although this appears to stabilize at 2 years after HDIT [35, 36]. The brains of five patients, all with a progressive type of MS who had died at a median of 2 (1–18) months after HDIT, had ongoing active demyelination and acute axonal damage in MS lesions in the absence of substantial lymphocytic infiltration [37]. A mouse model of MS has demonstrated that the neuroinflammatory process after transplantation may be sustained predominantly by endogenous microglia/macrophages and that transplant earlier in the disease course was more effective [38]. The histopathology studies of the MS brain after HDIT would be consistent with the observations in the mouse model.
Table 1. Clinical trials of HDIT and autologous HCT for multiple sclerosis
ATG=antithymocyte globulin; B=BCNU; BEAM=BCNU/Etoposide/Cytosine arabinoside/melphalan; Bu=busulfan; Cy=cyclophosphamide; PFS=progression-free survival; PP=primary progressive; PR=progressive relapsing; RR=relapse-remitting; SP=secondary progressive; TBI=total body irradiation; EDSS=Expanded Disability Status Scale
*In brief, the functional levels of the Expanded Status Scale (EDSS) are graded from 0–10 points and include changes in increments of 0.5 points. An EDSS score of 0 indicates a normal neurological examination in all functional systems (FS). An EDSS score of 10 indicates death from MS. Most of the MS patients who entered these clinical trials of HDIT and autologous HCT had an EDSS score of 5.0–8.0. In general, the function of patients at these different EDSS scores are:
5.0 Ambulant 200m without aids, difficulty to work full day, FS grades 5
6.0 Intermittent or unilateral walking aid for 100m
7.0 Wheelchair-bound (walking <5m with assistance). Able to transfer and use wheelchair alone. Sometimes severe pyramidal grade 5
8.0 Bed- and chair-bound, self-care functions retained (arm function retained), sitting out of bed most of the day.
** One patient with progression of MS was started on interferon β after a relapse, developed a factor VIII inhibitor at 14 months and died at 28 months after HDIT and autologous HCT.
|
Author |
Patient n |
MS type |
Median EDSS* (range) |
Mobilization |
High-dose therapy |
T-cell Depletion |
Follow-up Median months (range) |
Treatment-/ Disease-related Mortality, |
Clinical Result |
|---|---|---|---|---|---|---|---|---|---|
|
(Fassas et al, 1997 [40]; Fassas & Nash, 2004 [32]) |
35 |
SP (19) |
6.0 |
G/GM-CSF + CY |
BEAM + ATG |
CD34 selection |
35 (3–67) |
1/1** |
PFS 81% at 5yrs |
|
(Openshaw et al, 2000 [26]) |
5 |
SP |
6.5 |
G-CSF only |
Bu/Cy |
CD34 selection |
22 (17–30) |
2/0 |
PFS 40% |
|
(Kozak et al, 2001 [34]) |
10 |
SP |
6.5 |
G-CSF + Cy |
G-CSF + Cy |
CD34 selection + monoclonals |
8 (1–18) |
0/0 |
90% stable or improved |
|
(Nash et al, 2003 [28]) |
26 |
SP (17) |
7.0 |
G-CSF + Prednisone |
TBI/Cy + ATG |
CD34 selection |
27 (2–47) |
1/1 |
76% stable or improved |
|
(Burt et al, 2003 [29]) |
21 |
SP (14) |
7.0 |
G-CSF + Cy |
TBI/Cy |
CD34 selection |
24 (12–60) |
0/2 |
62% stable or improved |
|
(Saiz et al, 2004 [33]) |
14 |
SP (9) |
6.0 |
G-CSF + Cy |
BCNU/Cy + ATG |
CD34 selection |
37 (19–55) |
0/0 |
PFS 86% |
|
(Saccardi et al, 2005 [31]) |
19 |
SP (15) |
6.5 |
G-CSF+ Cy |
BEAM + ATG |
None |
36 (12–72) |
0/0 |
PFS 95% |
|
(Samijn et al, 2006 [30]) |
14 |
SP |
6.0 |
None (marrow) |
TBI/Cy + ATG |
CD34 selection |
36 (7–36) |
0/1 |
PFS 36% |
|
(Shevchenko et al, 2008 [26]) |
50 |
SP (27) |
5.0 |
G-CSF + Cy |
BEAM + ATG |
None |
Min. follow-up |
1 (3 yrs)/0 |
PFS 72% (6 yrs) |
|
(Fagius et al, 2009 [27]) |
9 |
RR (9) |
7.0 |
G-CSF + Cy |
BEAM + ATG |
None |
29 |
0/0 |
PFS 100% |
|
(Burt et al, 2009 [18]) |
21 |
RR (21) |
3.5 |
G-CSF +Cy |
Cy +ATG |
None |
37 |
0/0 |
PFS 100% |
In the three studies reported since 2008 with a total of 80 patients, no treatment-related mortality was observed, although one patient died from acute myelogenous leukemia at 3 years after treatment (Table 1). No indication was given in the report if there were other risk factors for AML in this patient besides the transplant, such as previous treatment with mitoxantrone. In two of the more recent clinical trials, only patients with very active relapsing-remitting MS who were earlier in their disease course were included [18, 27]. Progression-free survival was observed to be 100% in both trials at a median follow-up of 2–3 years, and a marked clinical improvement was noted. Disease activity-free survival in which disease activity was defined as relapses, activity on the brain MRI, or loss of neurological function was 62% in one study [18].
Although MRI studies in the early clinical trials showed a marked and sustained reduction in Gd-enhancing brain lesions in all the groups studied compared to baseline, it was still uncertain if the continued loss of neurological function observed in some of these progressive patients was the result of a degenerative process or a failure to completely control inflammation related to the autoimmune disease. Based on the observations now in patients transplanted earlier in the course of MS and the brain histopathology studies, continued loss of neurological function is consistent with persistent microglial/macrophage activation in the MS lesions of patients with advanced disease. Future clinical trials should be done in patients with very active relapsing-remitting MS who have failed therapy while they are still early in their disease course. The NIH-sponsored HALT MS clinical trial of HDIT followed by autologous HCT for relapsing-remitting MS completed accrual in late 2009 (n=24). A 5-year follow-up is planned to assess stability of the response. Randomized clinical trials need to be completed to confirm if there is a therapeutic benefit of HDIT and autologous HCT for MS. In Europe, the Autologous Stem cell Transplantation International Multiple Sclerosis (ASTIMS) randomized clinical trial included patients with secondary progressive MS with an EDSS of 3.5–6.5. ASTIMS was closed because of poor accrual.
Systemic sclerosis
Systemic sclerosis is an uncommon disabling autoimmune disease that is characterized by two major clinical features: 1) a non-inflammatory small vessel vasculopathy and, 2) fibrosis of the skin and multiple internal organs [41]. Antinuclear antibodies occur in 95% of SSc patients and the anti-topoisomerase I antibody (Scl-70) is found in 30–40% of subjects with diffuse cutaneous SSc. Diffuse cutaneous SSc has a higher mortality than limited cutaneous SSc and is associated with substantial morbidity. Clinical manifestations include digital ischemia/skin ulcerations from the vasculopathy, both truncal and acral scleroderma, interstitial lung disease, hypertensive renal crisis, diffuse GI disease, and myocardial involvement. The modified Rodnan skin score (mRSS) and the modified Health Assessment Questionnaire Disability Index for SSc (SHAQ) are two validated tools for evaluating the degree of scleroderma and measuring the effect of disease on overall function [42].
Immunosuppressive therapies investigated for severe SSc have been inadequate or ineffective. A 12-month course of cyclophosphamide was reported to be superior to placebo in slowing the rate of progression of SSc lung disease at 12 months after start of treatment, but later follow-up showed that the overall effect was modest and not sustained at 24 months [43, 44]. However, cyclophosphamide might be considered a standard of care for individuals with SSc since no other immunosuppressive treatment has been shown in a controlled setting to be of any benefit whatsoever. Important supportive care measures for SSc patients include angiotensin-converting enzyme inhibitors for management of renal crisis, and bosentan or other agents for management of pulmonary hypertension.
A still limited number of clinical trials of HDIT and autologous HCT for SSc have been conducted. Patients included in these clinical trials had a poor prognosis based on the presence of diffuse cutaneous disease and internal organ involvement. In a single center study of high-dose cyclophosphamide as a single agent (n=10) or melphalan (n=1) and autologous HCT, major or partial responses were observed in 8 of 11 patients, but at a median of 18 months, 8 patients had relapsed or not achieved a response (Table 2) [15].
Table 2. Clinical trials of HDIT and autologous HCT for systemic sclerosis
*There was one additional death at 5 years after HDIT from lung cancer.
BL=baseline; Cy=cyclophosphamide (mobilization: 2 or 4 g/m2; treatment: 120 mg/kg in combination with TBI or 200 mg/kg if single cytotoxic agent); DLCO=diffusion capacity of the lung for carbon monoxide; EFS=event-free survival; Mel=melphalan; mRSS=modified Rodnan skin score (ranges from 0–51; increasing score indicates worsening scleroderma); PFS=progression-free survival.
Author | Patient | BL Median DLCO% (range) | BL Median mRSS (range) | Mobilization | High-dose therapy | T-cell depletion | Follow-up Median months (range) | Treatment-related/ Disease-related Mortality, | Clinical results |
|---|---|---|---|---|---|---|---|---|---|
(McSweeney et al, 2002 [45]; Nash et al, 2007 [7]) | 34 | 61 | 30 | G-CSF | TBI / Cy + ATG | CD34 selection | 48 | 8/4 | PFS – 64% |
(Farge et al, 2002 [15]) | 11 | 67 | 29 | G-CSF + Cy | G-CSF + Cy | CD34 selection (n=9) | 18 | 1/3 | 3 patients alive in remission (27%) |
(Tsukamoto et al, 2006 [46]) | 6 | 47 | 26 | G-CSF + Cy | Cy | CD34 selection | 20 | 0/0 | Improvement in skin score (P=0.05) and lung function |
(Loh et al, 2007 [48]; Milanetti et al, 2009 [47]) | 37 | ? | 25 | G-CSF + Cy | Cy + ATG | None | 24 | 4/2 | EFS 68% |
(Vonk et al, 2008) [10] | 28 | 55 | 32 | G-CSF + Cy | Cy | CD34 selection | 63 (12–90) | 2/2* | EFS (evaluable, n=26) |
Four patients (36%) had died by 18 months after HDIT. In a later study of patients who had survived at least 6 months after high-dose cyclophosphamide only and HCT (n=26), survival was 96% and event-free survival was 64% at 5 years [10]. However, about half of the patients included in this study had diffuse cutaneous disease albeit without internal organ involvement. In the North American multicenter pilot study of a more intensive HDIT regimen consisting of TBI and cyclophosphamide in patients with diffuse cutaneous disease and internal organ involvement, 17 of 27 evaluable patients (63%) who survived at least 1 year after HDIT had sustained responses (without progression or disease activation) at a median follow-up of 4 years [7]. Patients with sustained responses had required no immune-based treatment after HDIT. There was a major improvement in the degree of scleroderma as measured by mRSS and in overall function as measured by the mHAQ at final evaluation (Figure 1A and B).
Figure 1. Change in modified Rodnan skin score (mRSS), modified Health Assessment Questionnaire (mHAQ) score, and lung function after high-dose immunosuppressive therapy (HDIT) and autologous hematopoietic cell transplantation
A determination was made whether a parameter value was statistically significantly increasing or decreasing over time using a generalized estimating equation (GEE) model. The bold black solid line represents the mean value over time for the parameter of interest. The bold black dotted line represents an estimate of the modeled linear relationship between the parameter value and time and summarizes the results of the GEE models. The gray solid lines are parameter values for individual patients. The mean mRSS and mHAQ values statistically significantly decreased with time after HDIT (both P<0.0001; panels A and B, respectively). The mean values for diffusion capacity of the lung for carbon monoxide (DLCO) adjusted for hemoglobin levels did not significantly change (P=0.50, panel C), and forced vital capacity statistically significantly increased with time (P=0.01, panel D). (This figure based on a figure originally published in Blood. Nash RA, McSweeney PA, Crofford LJ, Abidi M, et al. High-dose immunosuppressive therapy and autologous hematopoietic cell transplantation for severe systemic sclerosis: long-term follow-up of the U.S. multicenter pilot study. Blood. 2007;110:1388-1396. © the American Society of Hematology.)
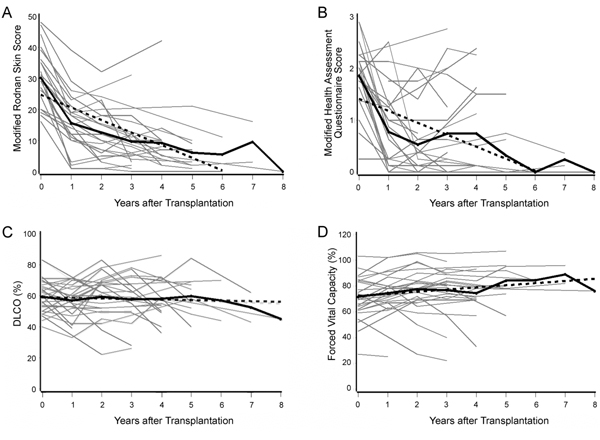
Skin biopsies confirmed that the improvement in skin score was associated with a significant decrease of dermal fibrosis (Figure 2) [7, 49].
Figure 2. Resolution of dermal fibrosis after HDIT and autologous HCT
Shown are full thickness skin biopsies from a patient in the North American pilot study for the SCOT clinical trial. Skin biopsies were collected at baseline (A and B) and then at 1 (C and D) and 5 years (E and F) after HDIT from the same location. Dermal fibrosis was evaluated after staining the skin with H&E and examined under low and high power magnification. At baseline, pan-dermal sclerosis from the dermal-epidermal border to the hypodermis (subcutaneous fat) was observed.
The reticular dermis is replaced by a dense compact collagen without normal collagen bundles or dermal appendages. (Original optic 5x. B)
As in 1A but at higher power, the straightened dermal-subcutaneous border demonstrates the abnormal, densely packed, homogenized collagen. (Original optic 20x. C)
A low power view of the skin biopsy at 1 year after HDIT shows crowded collagen bundles with focal areas of residual sclerosis but less than at baseline. (Original optic 5x. D)
A higher power view of the 1-year skin biopsy from C shows collagen bundles some of which are hypereosinophilic and straightened but overall there is no longer the appearance of homogenization. (Original optic 20x. E)
The skin biopsy at 5 years shows that the thickness of the dermis has decreased from baseline. There has been resolution of the dermal fibrosis. There is now some thinning of the collagen bundles with a relative increase in the space between the collagen bands. The dermal-epidermal border remains straightened with loss of rete ridges. (Original optic 5x. F)
A higher power view of collagen in lower reticular dermis demonstrates a change to thin wavy collagen bundles separated by increased ground substance. (Original optic 20x)
(This figure is based upon a figure originally published in Blood. Nash RA, McSweeney PA, Crofford LJ, Abidi M, et al. High-dose immunosuppressive therapy and autologous hematopoietic cell transplantation for severe systemic sclerosis: long-term follow-up of the U.S. multicenter pilot study. Blood. 2007;110:1388-1396. © the American Society of Hematology.)

Lung, heart and kidney function, in general, remained clinically stable (Figure 1C and D). Histological studies of the microvasculature of the skin also showed improvement after HDIT [50]. There was an increased capillary count in post-transplant SSc skin and interferon alpha, vascular endothelial cadherin and RGS5 had returned to normal levels. The treatment-related mortality was 23%, and progression-free survival was 64% at 5 years. Other studies have also suggested a major clinical effect of HDIT on skin and function [46, 47]. The cumulative probability of disease progression at 5 years was 48% and the cumulative probability of survival at 5 years was 72% in registry data from EBMT [21]. Two randomized clinical trials of HDIT followed by autologous HCT for SSc are currently being conducted, one in Europe (ASTIS) and the other in North America (SCOT; website: www.sclerodermatrial.org).
Systemic lupus erythematosus
Systemic lupus erythematosus (SLE) is characterized by the presence of anti-nuclear antibodies and immune complexes [51]. Disease severity may vary from mild to life threatening, and numerous organ systems may be involved. Antinuclear antibodies, anti-double stranded DNA antibodies, and anti-Smith antibodies are present in 98%, 70% and 25% of SLE patients, respectively. Overall, the 10-year survival of patients with SLE has been reported as 75–85%, with more than 90% surviving at 5 years [52]. Standard treatment options are not curative and complete sustained remissions are rare. Antimalarials such as hydroxychloroquine reduce the frequency of disease flares, and low-dose corticosteroids are used for patients in whom disease symptoms have not been controlled by more conservative measures. Agents such as cyclophosphamide, azathioprine, rituximab and mycophenolate mofetil have also been found effective in controlling disease activity [53]. The SLE Disease Activity Index (SLEDAI) is a validated tool for following disease activity [54].
Clinical trials of HDIT with and without HCT were conducted on patients with SLE who were refractory to standard therapies. In a single center study (n=50) of HDIT and HCT, patients underwent stem cell mobilization with G-CSF and cyclophosphamide, and the autologous graft was T cell-depleted by CD34-selection [8]. The HDIT regimen consisted of high-dose cyclophosphamide (200 mg/kg) and ATG. There was a significant improvement in the SLEDAI score, renal function stabilized and titers of the anti-nuclear and anti-double stranded DNA antibodies improved after HDIT. Overall and disease-free survival at 5 years was 84% and 50%, respectively. Treatment-related mortality was 4% (two patients) and both deaths occurred before HDIT. The EBMT registry reported the experience with HDIT and autologous HCT for SLE and observed significant disease responses in 31 of 50 patients, although many remained on some maintenance therapy after transplantation [55]. In comparison, a study of high-dose cyclophosphamide (200 mg/kg) without HCT (n=14) showed that only 5 patients (36%) had durable complete remissions at a median follow-up of 27 months [20]. Although this approach avoids the re-infusion of cells, the relapse rates were comparable with or without the transplant of autologous hematopoietic cells. If there is no difference in relapse rates, then transplantation of hematopoietic cells would be expected to be beneficial due to a reduction in the time to recovery of blood cell counts. Although experience is still limited, HDIT can induce a high percentage of disease responses in patients with SLE who had otherwise been refractory to standard therapy, and remissions have been durable in a significant proportion of patients.
Rheumatoid arthritis
The pathological hallmark of Rheumatoid arthritis (RA) is synovial inflammation with proliferation of macrophages and fibroblasts. If severe, the inflamed synovium develops into an invasive pannus which destroys cartilage and bone [56]. Other complications are a vasculitis, cervical spine disease, lung nodules or interstitial fibrosis, and cardiac complications including pericarditis. Risk of progression can be predicted by prognostic factors such as increased number of affected joints, a high level of C-reactive protein, presence of rheumatoid factor, and extra-articular features of the disease [56]. The risk of mortality is increased with more severe disease activity or ≥ 1 extra-articular disease manifestation [57, 58, 59]. There is a mortality of approximately 30% at 5 years for patients with the highest disease activity. Many anti-cytokine or immunomodulatory agents have been approved for the treatment of RA including methotrexate, hydroxychloroquine, sulfsalazine, leflunamide, infliximab, adalimumab, etanercept, abatacept, and anakinra. B-cell targeted therapy with rituximab has recently been shown to be effective as well. The goal of standard therapy is to relieve the signs and symptoms of the disease since none of these treatments are curative. The criteria for determining response to treatment have been defined by the American College of Rheumatology [60].
Four small clinical trials of high-dose cyclophosphamide with or without ATG for patients with RA who had failed standard treatment have been reported [14, 61, 62, 63, 64, 65]. There were early major responses in the majority of the patients, but on long-term follow-up, all 32 patients accrued to these clinical trials relapsed and required additional treatment. Although disease activity recurred, one study showed that after HDIT, there was a decrease in progression of joint damage compared to baseline [66]. No mortality was observed in any of the clinical trials. Seventy-six patients with RA who underwent HDIT and autologous HCT were available for analysis in the EBMT registry, and the outcomes were comparable to the experience reported from the clinical trials [67]. Major responses were observed in 67% of patients, with a significant reduction in the measures of disability. Most patients had restarted immunomodulatory treatment by 6 months after HDIT for persistent or recurrent disease activity. No treatment-related mortality was observed. The apparent difference in response of RA to HDIT compared to other autoimmune diseases might be related to immune or non-immune biological factors. More durable responses might be obtained with more intense HDIT regimens, but this may increase the risk for treatment-related mortality. Another strategy to decrease relapses or progression may be the addition of immunomodulatory therapy after HDIT.
Juvenile idiopathic arthritis
Juvenile idiopathic arthritis (JIA) is a heterogeneous group of chronic inflammatory diseases involving the joints and extra-articular tissues that begins before 16 years of age [68]. Severe disease has an effect on bone and joint development resulting in overgrowth or undergrowth of juxta-articular bone resulting in limb deformities. The macrophage activation syndrome is a potentially life-threatening complication in which there is uncontrolled activation and proliferation of macrophages and T cells. This complication may occur in 5–8% of patients with systemic JIA. The mortality is <1% and occurs mostly in the systemic JIA subtype [69]. One clinical trial of HDIT and autologous HCT in patients with treatment-refractory JIA (n=22) was reported with a median follow-up of 80 months [6]. The HDIT regimen consisted of TBI (400 cGy), cyclophosphamide, and ATG. Early in the clinical trial, two patients developed macrophage activation syndrome less than 1 month after HDIT and both died. Precautionary measures added to the treatment may have reduced this risk in later patients. Two other patients died after relapsing and restarting immunosuppressive treatment more than 1 year after HDIT. Overall and disease-free survival was 82% and 36%, respectively. There were significant sustained improvements in disease activity in the group based on disability and active joint scores. In a more recent report of 7 patients, 4 patients had sustained responses, 2 patients relapsed within 1–12 months of transplant, and 1 patient died at 4 months post-transplant [70]. In a report from the EBMT registry on 34 JIA patients, 18 (53%) were in complete remission without additional therapy at 12 to 60 months after HDIT [71]. In a small subset of poor prognosis JIA patients who fail to respond to standard treatment, HDIT and autologous HCT may be of benefit, although this may be associated with a substantial risk in a disease that is not per se life threatening.
Crohn’s disease
In a clinical trial of patients with treatment-refractory Crohn’s disease, 11 of 12 patients achieved sustained remissions at a median of 18 (7–37) months after HDIT without significant treatment-related toxicity or mortality [72]. In another study, 3 of 4 patients achieved clinical and endoscopic remissions at a median of 16.5 months after HDIT [73]. Longer follow-up is required to assess the durability of response.
Diabetes mellitus
An interesting clinical trial was performed in patients with recent-onset diabetes mellitus. Fourteen of 15 patients had prolonged periods of insulin independence after high-dose cyclophosphamide and autologous HCT [16]. In a follow-up to that report and with inclusion of 8 additional patients, 20 of 23 patients became insulin-independent after HDIT and 12 patients maintained that status for a mean of 31 months; 8 patients relapsed and required insulin again [74]. C-peptide levels were significantly increased after transplant compared to baseline. About 50% of patients may achieve a prolonged insulin-free period after HDIT but longer follow-up is required.
Immune reconstitution after high-dose immunosuppressive therapy
Natural killer (NK) cell counts recovered by 1 month and B and CD8+ T-cell counts recovered by 6–12 months after HDIT. There was a slower recovery of CD4+ T cell counts, which reach low–normal levels by 2 years [12]. Immune recovery at 2 years after HDIT was associated with increasing thymic-derived naïve CD4+ T cells (Figure 3) [11].
Figure 3. Central memory CD4+ T cells decreased and naïve CD4+ T cells increased at 2 years after HDIT and autologous HCT for MS
At the 2-year follow-up, the frequency of naïve CD4+ T cells in the blood had increased 118% as compared with pretherapy (P=0.032). Correspondingly, CM CD4+ T cells had decreased 38% at 2 years after therapy (P=0.008). The frequencies of the EM CD4+ T cells did not change significantly at the 2-year follow-up compared with the baseline. These data support the concept that there is significant immunomodulation at 2 years after HDIT and autologous HCT, and this may explain the observed durable clinical remissions in a significant proportion of patients with autoimmune disease. Reproduced with permission. © Muraro et al., 2005. J. Exp. Med. doi:10.1084/jem.20041679

It was also observed that there was an increase in T cell receptor excision circles (TRECs; a marker for recent thymic emigrants) in CD4+ T cells at 1 and 2 years after HDIT and a steady decrease over time in CD4+ central memory T cells. CD4+ effector memory cells were relatively increased at 6 months after HDIT, likely from homeostatic proliferation, but had recovered to normal levels by 2 years. There were no significant changes in the CD8+ T cell subsets. Several investigators have reported an increase in regulatory CD4+ FoxP3+ and CD8+FoxP3+ T cells, and broader clonal diversity than present before [11, 13, 75, 76, 77]. In association with the increased levels of naïve CD4+ T cells, there was hypertrophy of the thymus at 1 and 2 years compared to baseline especially in the younger patients (less than 43 years of age) [12]. This evidence suggested a thymic origin for the recovery of the CD4+ T-cell repertoire after HDIT and autologous HCT. Even though B-cell counts were very low in the first 3 months after HDIT, median serum levels of immunoglobulin G specific for tetanus toxoid, Hemophilus influenzae and Streptococcus pneumoniae, were normal [12]. There was recovery of the naïve B cell compartment in SLE patients by 1 year after HDIT [76]. The clinical responses to HDIT, which have persisted for 2 or more years in several autoimmune diseases, may be a result of these late immunomodulatory effects.
Allogeneic HCT for autoimmune diseases
Outcomes in patients with autoimmune diseases transplanted for another primary disease
Our first understanding of the effect of allogeneic HCT on human autoimmune diseases came from experience in transplanting patients with hematologic disorders who also suffered from autoimmune diseases (Table 3) [78, 79, 80, 81, 82, 83, 84, 85, 86, 87, 88, 89, 90, 91, 92, 93, 94,95].
Table 3. Outcomes in patients with autoimmune diseases transplanted with an allogeneic hematopoietic cell graft for another primary disease
Abbreviations: AML=acute myeloid leukemia; ALL=acute lymphoblastic leukemia; ANA=anti-nuclear antibody; CML=chronic myelogenous leukemia; LGL=large granular lymphocytes; MM=multiple myeloma; NHL=Non-Hodgkin lymphoma; SAA=severe aplastic anemia.
*Clinical remission but ANA remained positive.
†Relapse occurred in patient with mixed chimerism.
Autoimmune Disease | Hematologic Disease | Evaluable Patients (total) n | Remission of Autoimmune Disease after HCT, n | Outcome (alive at last follow-up), n | Follow-up |
|---|---|---|---|---|---|
Rheumatoid arthritis (Baldwin et al, 1977 [78]; Jacobs et al, 1986 [79]; McKendry et al, 1996 [80]; Lowenthal et al, 1993 [81]; Snowden et al, 1998 [82]; Lowenthal et al, 2006 [83]; Tapprich et al, 2003 [84]) | SAA (n=8), 1 MM | 9 | 7 (2 relapses +1 transient relapse) | 6 | 2 mos–21 yrs |
Systemic lupus erythematosus (Gur-Lavi, 1999 [85]) | SAA | 1 | 1* (ANA titer +) | 1 | 15 yrs |
Psoriatic arthritis (Yin & Jowitt, 1992 [86]; Slavin et al, 2000 [87]; Snowden et al, 1998 [82]; Eedy et al, 1990 [88]) | AML, CML (n=3) | 4 | 3 (1 relapse) | 3 | 1, 3, 5, 5 yrs |
Ulcerative colitis (Yin & Jowitt, 1992 [86]) | AML | 1 | 1 | 1 | 4 yrs |
Crohn’s disease [Lopez-Cubero et al, 1998 [89] | CML | 5 | 4† | 5 | 4.5–15.3 yrs |
Multiple sclerosis (Mandalfino et al, 2000 [90]; McAllister et al, 1997 [91]; La Nasa et al, 2004 [92]; Jeffery, 2007 [93]) | CML (n=2), LGL Leukemia, AML | 4 | 3 | 3 | 1, 2, 3, 4 yrs |
Autoimmune hepatitis (Vento et al, 1996 [94]) | ALL | 1 | 1 | 1 | 4 yrs |
Lupus anticoagulant (Olalla et al, 1999 [95]) | CML | 1 | 1 | 1 | 5 yrs |
In RA patients, sustained remissions have been observed for as long as 20 years after allogeneic HCT [83]. However, relapses were observed in 3 of the 9 reported RA patients. One of the relapses was transient with a subsequent treatment-free remission of 11 years. In one of the two sustained relapses, the HLA-identical donor was serologically positive for rheumatoid factor but without clinical disease [79]. Sustained remissions and some relapses have also been observed in patients with other concomitant autoimmune diseases after allogeneic HCT (Table 3). One patient who relapsed with Crohn’s disease had mixed hematopoietic chimerism detected at 3 months after HCT. Hinterberger et al did a literature search and identified reports of patients with an autoimmune disease who were transplanted for severe aplastic anemia or a hematologic malignancy between 1977 and 2001 [96]. Attempts were then made to update these reports. Disease-free survival after allogeneic HCT of patients with aplastic anemia (n=23) was 78% at 16 years and survival in unmaintained remission of the concomitant autoimmune disease was 64% at 13 years. The results were similar for patients with autoimmune diseases who underwent allogeneic HCT for hematologic malignancies. An association was noted between the development of GVHD and the risk for relapse of the autoimmune disease. The risk for relapse of the autoimmune disease was lower after allogeneic than after autologous HCT. There were insufficient data from the case reports/series to develop an understanding of why relapses occurred after allogeneic HCT. After allogeneic HCT from an HLA-identical sibling, one possible explanation for recurrence of the autoimmune disease may be genetic factors that are shared between the donor and recipient. Another possible explanation is the persistence of host immune cells resulting in the recurrence of disease activity.
Allogeneic hematopoietic cell transplantation for autoimmune diseases as the primary indication
The primary risks of allogeneic HCT are the morbidity and mortality associated with a delayed immune reconstitution and graft-versus-host disease (GVHD). Therefore, there has been a reluctance to consider this approach except for extreme cases of refractory autoimmune diseases. Although the risk of complications and treatment-related mortality is greater than after autologous HCT, there may be a greater potential for sustained remissions of severe autoimmune diseases after allogeneic HCT and, therefore, the possibility of an improved overall outcome. Survival after allogeneic HCT for nonmalignant hematological disorders or good-risk hematological malignancies such as chronic myelogenous leukemia in chronic phase has ranged from 85–95%. The best outcomes were observed in young patients transplanted from HLA-matched donors. No clinical trials have yet been conducted of allogeneic HCT for which an autoimmune disease was the primary indication, but a small number of cases have been reported. The largest experience has been in patients with autoimmune cytopenias [97, 98, 99, 100]. Of the seven evaluable patients reported from the EBMT registry, five were alive and in remission at a median follow-up of 41 months [97]. One patient with Evans syndrome in the report from the EBMT registry had disease progression and died. The second patient died from treatment-related complications after HCT from an HLA-haploidentical donor. Of the three case reports of Evans syndrome in the literature, one patient relapsed and died and the other two died of transplant-related complications in complete remission [98, 99, 100]. There are six cases reported of allogeneic HCT for connective tissue diseases like SSc, overlap syndrome, and RA [48, 101, 102, 103, 104]. Two patients with SSc had high-dose conditioning, one of whom was alive at 5 years in disease remission with resolution of the dermal fibrosis and severe scleroderma. The four other patients received reduced intensity conditioning regimens. All patients were alive at last follow-up and in remission. Three of these patients had stable mixed hematopoietic chimerism and no history of GVHD. Regulatory immune mechanisms associated with the establishment of mixed hematopoietic chimerism may be responsible for inducing remission of the autoimmune disease [105]. Daikeler et al. reported a case series of 35 patients who had allogeneic HCT between 1984 and 2007 for a primary indication of an autoimmune disease and were reported to the EBMT registry [106]. Responses occurred in 78% of patients, but in this heavily pre-treated population, the treatment-related mortality was 22%. Relapses were again observed in a small number of cases. These registry data had significant limitations since the patient population was very heterogeneous for both treatment and disease type, as well as the fact that the data were often incomplete. Conclusions regarding the therapeutic role of allogeneic HCT for severe autoimmune diseases await the results from prospective clinical trials conducted in carefully selected patients.
Conclusions
A high rate of remission in autoimmune diseases is observed after HDIT and autologous HCT, and a significant proportion are sustained after 4–5 years. The rate and durability of response may depend on the intensity of the HDIT regimen and the type of autoimmune disease being treated. Randomized clinical trials are now being conducted in specific autoimmune diseases. The experience with allogeneic HCT as a treatment for autoimmune diseases is still limited, but promises to be highly effective. Carefully selected patients with active autoimmune disease that is life-threatening or threatening critical organ function and refractory to standard treatment should be considered as candidates for clinical trials of allogeneic HCT or HDIT followed by autologous HCT.
Acknowledgements
Grants to acknowledge are: National MS Society- RG4183
References
1. Good RA, Ikehara S. Preclinical investigations that subserve efforts to employ bone marrow transplantation for rheumatoid or autoimmune diseases. Journal of Rheumatology. 1997;24(48);5-12.
2. Shizuru JA. The experimental basis for hematopoietic cell transplantation for autoimmune diseases. Thomas' Hematopoietic Cell Transplantation (ed. by F.R.Appelbaum, S.J.Forman, R.S.Negrin and K.G.Blume), Oxford, UK, Wiley-Blackwell. 2009. 264 p.
4. Cooley HM, Snowden JA, Grigg AP, Wicks IP. Outcome of rheumatoid arthritis and psoriasis following autologous stem cell transplantation for hematologic malignancy. Arthritis and Rheumatism. 1997;40:1712-1715.
9. Saccardi R, Kozak T, Bocelli-Tyndall C, Fassas A, et al, Autoimmune Diseases Working Party of EBMT. Autologous stem cell transplantation for progressive multiple sclerosis: update of the European Group for Blood and Marrow Transplantation autoimmune diseases working party database. Multiple Sclerosis. 2006;12:814-823.
10. Vonk MC, Marjanovic Z, van den Hoogen FH, Zohar R, et al. Long-term follow-up results after autologous haematopoietic stem cell transplantation for severe systemic sclerosis [Erratum appears in Ann Rheum Dis. 2008 Feb;67(2):280]. Annals of the Rheumatic Diseases. 2008;67:98-104.
12. Storek J, Zhao Z, Lin E, Berger T, et al. Recovery from and consequences of severe iatrogenic lymphopenia (induced to treat autoimmune diseases). Clinical Immunology. 2004;113:285-298.
15. Farge D, Marolleau JP, Zohar R, Marjanovic Z, et al, Intensification et Autogreffe dans les Maladies Auto Immunes Resistantes (ISAMAIR) Study Group. Autologous bone marrow transplantation in the treatment of refractory systemic sclerosis: early results from a French multicentre phase I-II study. British Journal of Haematology. 2002;119:726-739.
18. Burt RK, Loh Y, Cohen B, Stefoski D, et al. Autologous non-myeloablative haemopoietic stem cell transplantation in relapsing-remitting multiple sclerosis: a phase I/II study [Erratum appears in Lancet Neurol. 2009 Apr;8(4):309]. Lancet Neurology. 2009;8:244-253.
19. Brodsky RA, Chen AR, Brodsky I, Jones RJ. High-dose cyclophosphamide as salvage therapy for severe aplastic anemia. Experimental Hematology. 2004;32:435-440.
22. Mayes M, Crofford L, Csuka ME, Furst D, et al. Autologous transplantation for systemic sclerosis in North America. Report of the scleroderma: cyclophosphamide or transplantation trial. Haematopoietic Stem Cell Transplantation for Severe Autoimmune Diseases, Abstract Book. 2009;4(Abstract):12.
25. Openshaw H, Lund BT, Kashyap A, Atkinson R, et al. Peripheral blood stem cell transplantation in multiple sclerosis with busulfan and cyclophosphamide conditioning: report of toxicity and immunological monitoring. Biology of Blood and Marrow Transplantation. 2000;6:563-575.
26. Shevchenko YL, Novik AA, Kuznetsov AN, Afanasiev BV, et al. High-dose immunosuppressive therapy with autologous hematopoietic stem cell transplantation as a treatment option in multiple sclerosis. Experimental Hematology. 2008;36:922-928.
27. Fagius J, Lundgren J, Oberg G. Early highly aggressive MS successfully treated by hematopoietic stem cell transplantation. Multiple Sclerosis. 2009;15:229-237.
30. Samijn JP, te Boekhorst PA, Mondria T, van Doorn PA, et al. Intense T cell depletion followed by autologous bone marrow transplantation for severe multiple sclerosis. Journal of Neurology. Neurosurgery and Psychiatry. 2006;77:46-50.
32. Fassas A, Nash R. Stem cell transplantation for autoimmune disorders. Multiple
sclerosis. Best Pract Res Clin Haematol. 2004 Jun;17(2):247-62.
33. Saiz A, Blanco Y, Carreras E, Berenguer J, et al. Clinical and MRI outcome after autologous hematopoietic stem cell transplantation in MS. Neurology. 2004;62:282-284.
34. Kozak T, Havrdova E, Pit'ha J, Gregora E, et al. Immunoablative therapy with autologous stem cell transplantation in the treatment of poor risk multiple sclerosis. Transplantation Proceedings. 2001;33:2179-2181.
35. Chen JT, Collins DL, Atkins HL, Freedman MS, et al, Canadian MS BMT Study Group. Brain atrophy after immunoablation and stem cell transplantation in multiple sclerosis. Neurology. 2006;66:1935-1937.
36. Roccatagliata L, Rocca M, Valsasina P, Bonzano L, et al, Italian GITMO-NEURO Intergroup on Autologous Stem Cell Transplantation. The long-term effect of AHSCT on MRI measures of MS evolution: a five-year follow-up study. Multiple Sclerosis. 2007;13:1068-1070.
38. Cassiani-Ingoni R, Muraro PA, Magnus T, Reichert-Scrivner R, et al. Disease progression after bone marrow transplantation in a model of multiple sclerosis is associated with chronic microglial and glial progenitor response. Journal of Neuropathology and Experimental Neurology. 2007;66:637-649.
41. Valentini G, Black C. Systemic sclerosis (Review). Best Practice and Research in Clinical Rheumatology. 2002;16:807-816.
42. Clements PJ, Lachenbruch PA, Ng SC, Simmons M, et al. Skin score. A semiquantitative measure of cutaneous involvement that improves prediction of prognosis in systemic sclerosis. Arthritis and Rheumatism. 1990;33:1256-1263.
44. Tashkin DP, Elashoff R, Clements PJ, Roth MD, et al. Effects of 1-year treatment with cyclophosphamide on outcomes at 2 years in scleroderma lung disease. American Journal of Respiratory and Critical Care Medicine. 2007;176:1026-1034.
46. Tsukamoto H, Nagafuji K, Horiuchi T, Miyamoto T, et al. A phase I-II trial of autologous peripheral blood stem cell transplantation in the treatment of refractory autoimmune disease. Annals of the Rheumatic Diseases. 2006;65:508-514.
47. Milanetti F, Bucha J, Kwasny M, Boyce K, et al. Autologous non-myeloablative hematopoietic stem cell transplantation in patients with systemic sclerosis. Haematopoietic Stem Cell Transplantation for Severe Autoimmune Diseases, Abstract Book. 2009;9(Abstract):44-45.
51. D'Cruz DP, Khamashta MA, Hughes GR. Systemic lupus erythematosus (Review). Lancet. 2007;369:587-596.
53. Smith KG, Jones RB, Burns SM, Jayne DR. Long-term comparison of rituximab treatment for refractory systemic lupus erythematosus and vasculitis: Remission, relapse, and re-treatment. Arthritis and Rheumatism. 2006;54:2970-2982.
54. Bombardier C, Gladman DD, Urowitz MB, et al. Derivation of the SLEDAI. A disease activity index for lupus patients. The Committee on Prognosis Studies in SLE. Arthritis and Rheumatism. 1992;35:630-640.
55. Jayne D, Passweg J, Marmont A, Farge D, et al. Autologous stem cell transplantation for systemic lupus erythematosus. Lupus. 2004;13:168-176.
56. Lee DM, Weinblatt ME, Lee DM, Weinblatt ME. Rheumatoid arthritis (Review). Lancet. 2001;358:903-911.
60. Pinals RS, Masi AT, Larsen RA. Preliminary criteria for clinical remission in rheumatoid arthritis. Arthritis and Rheumatism. 1981;24:1308-1315.
61. Bingham SJ, Snowden J, McGonagle D, Richards R, et al. Autologous stem cell transplantation for rheumatoid arthritis – interim report of 6 patients. Journal of Rheumatology. 2001;64(Suppl.):21-24.
65. Pavletic SZ, Klassen LW, Pope R, O'Dell JR, et al. Treatment of relapse after autologous blood stem cell transplantation for severe rheumatoid arthritis. Journal of Rheumatology. 2001;64(Suppl.):28-31.
67. Snowden JA, Passweg J, Moore JJ, Milliken R, et al. Autologous hemopoietic stem cell transplantation in severe rheumatoid arthritis: a report from the EBMT and ABMTR. Journal of Rheumatology. 2004;31:482-488.
68. Ravelli A, Martini A. Juvenile idiopathic arthritis (Review). Lancet. 2007;369:767-778.
70. Abinun M, Flood TJ, Cant AJ, Veys P, et al. Autologous T cell depleted haematopoietic stem cell transplantation in children with severe juvenile idiopathic arthritis in the UK (2000-2007). Molecular Immunology. 2009;47:46-51.
72. Oyama Y, Craig RM, Traynor AE, Quigley K, Statkute L, Halverson A, Brush M, Verda L, Kowalska B, Krosnjar N, Kletzel M, Whitington PF, Burt RK. Autologous hematopoietic stem cell transplantation in patients with refractory Crohn's disease. Gastroenterology. 2005;128:552-563.
73. Cassinotti A, Annaloro C, Ardizzone R, Onida F, et al. Autologous haematopoietic stem cell transplantation without CD34+ cell selection in refractory Crohn's disease. Gut. 2008;57:211-217.
74. Couri CE, Oliveira MC, Stracieri AB, Moraes DA, et al. C-peptide levels and insulin independence following autologous nonmyeloablative hematopoietic stem cell transplantation in newly diagnosed type 1 diabetes mellitus. Journal of the American Medical Association. 2009;301:1573-1579.
75. Zhang L, Bertucci AM, Ramsey-Goldman R, et al. Regulatory T cell (Treg) subsets return in patients with refractory lupus following stem cell transplantation, and TGF-beta-producing CD8+ Treg cells are associated with immunological remission of lupus. Journal of Immunology. 2009;183:6346-6358.
78. Baldwin JL, Storb R, Thomas ED, Mannik M. Bone marrow transplantation in patients with gold-induced marrow aplasia. Arthritis and Rheumatism. 1977;20:1043-1048.
79. McKendry RJ, Huebsch L, Leclair B. Progression of rheumatoid arthritis following bone marrow transplantation. A case report with a 13-year followup. Arthritis and Rheumatism. 1996;39:1246-1253.
80. Jacobs P, Vincent MD, Martell RW. Prolonged remission of severe refractory rheumatoid arthritis following allogeneic bone marrow transplantation for drug-induced aplastic anemia. Bone Marrow Transplantation. 1986:1:237-239.
81. Lowenthal RM, Cohen ML, Atkinson K, Biggs JC. Apparent cure of rheumatoid arthritis by bone marrow transplantation. Journal of Rheumatology. 1993;20:137-140.
83. Lowenthal RM, Francis H, Gill DS. Twenty-year remission of rheumatoid arthritis in 2 patients after allogeneic bone marrow transplant. Journal of Rheumatology. 2006;33:812-813.
86. Yin JA, Jowitt SN. Resolution of immune-mediated diseases following allogeneic bone marrow transplantation for leukaemia. Bone Marrow Transplantation. 1992;9:31-33.
87. Slavin R, Nagler A, Varadi G, Or R. Graft vs autoimmunity following allogeneic non-myeloablative blood stem cell transplantation in a patient with chronic myelogenous leukemia and severe systemic psoriasis and psoriatic polyarthritis. Experimental Hematology. 2000;28:853-857.
89. Lopez-Cubero SO, Sullivan KM, McDonald GB. Course of Crohn's disease after allogeneic marrow transplantation. Gastroenterology. 1998;114:433-440.
90. Mandalfino P, Rice G, Smith A, Klein JL, et al. Bone marrow transplantation in multiple sclerosis. Journal of Neurology. 2000;247:691-695.
92. La Nasa G, Littera R, Cocco E, Battistini L, et al. Allogeneic hematopoietic stem cell transplantation in a patient affected by large granular lymphocyte leukemia and multiple sclerosis. Annals of Hematology. 2004;83:403-405.
93. Jeffery DR. Failure of allogeneic bone marrow transplantation to arrest disease activity in multiple sclerosis. Multiple Sclerosis. 2007;13:1071-1075.
94. Vento R, Cainelli F, Renzini C, et al. Resolution of autoimmune hepatitis after bone-marrow transplantation. Lancet. 1996;348:544-545.
102. Khorshid O, Hosing C, Bibawi R, Ueno N, et al. Nonmyeloablative stem cell transplant in a patient with advanced systemic sclerosis and systemic lupus erythematosus. Journal of Rheumatology. 2004;31:2513-2516.
" ["~DETAIL_TEXT"]=> string(107828) "High-dose immunosuppressive therapy and autologous hematopoietic cell transplantation for autoimmune diseases: clinical experience
High-dose immunosuppressive therapy regimens
Two reports were published in the mid-late 1990s on the outcomes of concomitant autoimmune diseases after high-dose cytotoxic therapy and autologous HCT for a hematological malignancy [3, 4]. A majority of the patients achieved remissions of the concomitant autoimmune diseases early after treatment, but only 5 of 15 cases had sustained responses at last follow-up in one report, and all 4 patients presented relapsed in a second report. This experience indicated that there was a substantial risk of progression of the autoimmune disease after high-dose cytotoxic/immunosuppressive therapy (HDIT) designed for treatment of a hematological malignancy. Clinical trials of HDIT and autologous HCT specifically for autoimmune diseases were designed to intensify the immunosuppressive effect compared to standard cytotoxic regimens for treating hematologic malignancies. This was achieved by depleting T cells from the autologous hematopoietic cell graft or by adding other non-cytotoxic immunosuppressive agents to the HDIT regimen for in vivo T cell depletion. The HDIT regimens that have been investigated in clinical trials have had varying intensities. High-dose cyclophosphamide as a single agent has been considered a low-intensity regimen [5]. It is highly immunosuppressive but is not myeloablative. Clinical trials of high-dose cyclophosphamide have been conducted with and without the support of autologous HCT. Regimens which included TBI or high-dose busulfan were considered high-intensity and required support with autologous HCT.
Systemic depletion of autoreactive immune effector cells was the rationale for the early clinical trials of HDIT followed by HCT for severe autoimmune diseases. These clinical trials showed high initial response rates, and a significant proportion of patients achieved sustained remissions [6, 7, 8, 9, 10]. The sustained responses observed after recovery of the lymphocyte counts at 2 years may have resulted from a late immunomodulatory effect of the HDIT regimen [11, 12, 13]. The intensity of the HDIT regimen may be important for the disease remission to be sustained. In a report from the EBMT registry, sustained responses were observed in 78% of patients after a regimen with high-intensity conditioning compared to 68% with intermediate and 30% with low-intensity conditioning regimens (p=0.0001) [5]. The analysis of the registry data, although informative, had some limitations including variability of the diagnoses, patient selection criteria, and treatments (as well as having imbalances between diagnosis and type of HDIT regimen). The possible benefits must be weighed against the risk when selecting the level of intensity of the conditioning regimens.
High-dose single agent cyclophosphamide followed by autologous HCT for hematopoietic support was reported as one of the more frequently used HDIT regimens [5]. When the doses of cyclophosphamide (100 vs. 200 mg/kg) were compared in a small study of patients with rheumatoid arthritis (RA), remissions were longer with the higher dose of cyclophosphamide [14]. However, all patients eventually relapsed regardless of the dose. Relapse rates were also high in a systemic sclerosis (SSc) study in which patients were treated with high-dose cyclophosphamide (200 mg/kg) alone. Four of 11 patients died by 18 months after treatment (three from progression), and another four patients had progressed and required secondary treatment [15]. The addition of antithymocyte globulin (ATG) to cyclophosphamide may improve the response rate and duration. Experience has continued to accrue with high-dose cyclophosphamide in combination with ATG [8, 16, 17, 18]. The regimen has been effective for inducing remissions and has been well tolerated; however, a longer follow-up is still required to assess the durability of responses. Since the regimen is not myeloablative, high-dose cyclophosphamide (200 mg/kg) as a single agent without autologous HCT has also been investigated [19, 20]. Without the support of an autologous hematopoietic cell graft after high-dose cyclophosphamide, the median time to recover neutrophil counts was about 2–3 days longer than with HCT, but the upper limit of the range was 7 days longer [8, 20]. Only 36% of the patients were reported to have durable complete remissions. In this small experience, there did not appear to be any benefit to withholding the infusion of an autologous hematopoietic cell graft.
Treatment-related mortality was 14% and 3%, respectively, in the groups reported from the EBMT registry who received the high and the low conditioning intensity regimens, but there was no significant difference in overall survival [5]. Patients with multiple sclerosis (MS) and RA had lower treatment-related mortality than patients with systemic sclerosis (SSc) and systemic lupus erythematosus (SLE) who had significant internal organ dysfunction related to their disease. Treatment with immunosuppressive agents including corticosteroids before transplant, especially in the SLE group, likely predisposed patients to the infectious complications experienced after HDIT. Better patient selection and modifications to the treatment regimen appear to have reduced the risks of treatment-related mortality in recent years [6, 9, 21]. In the SCOT clinical trial in which patients with SSc are randomized between two treatment arms, either HDIT followed by autologous HCT or pulse cyclophosphamide, there was only one treatment-related death as of late 2009 [22]. This improvement was attributed to modifications made to the treatment regimen and patient selection based on insights gained from the pilot study [7, 22].
Specific Autoimmune Diseases and High-Dose Immunosuppressive Therapy Followed by Autologous Hematopoietic Cell Transplantation
HDIT has been performed most commonly for MS, SSc, SLE, RA and juvenile idiopathic arthritis (JIA) [5], but promising results have also been observed in other autoimmune diseases.
Multiple sclerosis MS is an inflammatory disorder of the central nervous system manifesting as acute focal demyelination and axonal loss followed by sclerotic scarring. It is postulated that myelin proteins are targeted by autoreactive immune effector cells [23]. The pathology shows a predominant T cell response both in the demyelinated lesion and in perivascular spaces. Axonal injury is evident in both the MS lesions and the normal-appearing white matter. The clinical manifestations of the disease are manifold and include loss of vision from optic neuritis, diplopia, sensory loss and paresthesias, vertigo, fecal or urinary incontinence, impotence, intellectual decline, paroxysmal pain, recurrent infections, and loss of coordination or paralysis. Most MS patients (85%) present with relapsing-remitting disease, and about 50% will evolve to the secondary progressive type of MS over 10 years. The other 15% of patients have progressive disease from onset (primary). The standard for measuring outcome in studies of MS is the Kurtzke Expanded Disability Status Scale (EDSS) and, more recently, the Multiple Sclerosis Functional Composite (MSFC). At 20 years after onset, patients with MS had 85% of the expected survival. Despite responses to immunomodulating agents, no standard therapy is curative or has been demonstrated to prevent development of a progressive clinical course. Disease-modifying therapies in relapsing-remitting MS include interferon (IFN) beta-1a, IFN beta-1b, glatiramer acetate (GA), mitoxantrone and natalizumab [24]. Treatment reduced the clinical relapse rates by 30–68%, with mitoxantrone and natalizumab being more effective than IFN or GA. These agents, however, remain inadequate in completely preventing relapses and progression. There is no effective therapy for primary or secondary progressive MS.
Results from at least 11 clinical trials of HDIT and autologous HCT for MS have been reported from transplant centers in the Americas, Europe and Asia (Table 1) [8, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34]. Although there was variability in the design of each of the early clinical trials, they all included patients with advanced MS and the progressive type of the disease. All patients received high-dose combination chemotherapy or total body irradiation (TBI) and cyclophosphamide. In 10 of the 11 clinical trials, the hematopoietic cell grafts consisted of “mobilized” peripheral blood cells, and seven of the trials included T cell depletion with CD34-selection. In the clinical trials reported before 2008, the overall treatment-related mortality was 2.8% (4/145) and the progression-free survival or rate of neurological stability reported in the individual clinical trials ranged from 36–95% at 2–3 years after treatment (Table 1). Five patients (3.5%) died after progression of their disease and further loss of neurological function or other complications. In a report by Saccardi et al. of 19 MS patients with high levels of disease activity based on magnetic resonance imaging (MRI) of the brain and sustained clinical deterioration, there was a marked reduction of gadolinium (Gd)-enhancing lesions in the brain after the HDIT regimen, which was sustained up to 5 years after treatment (Table 1) [31]. Although HDIT followed by autologous HCT appears highly effective for suppressing MRI findings of MS disease activity, a significant loss of brain volume has been noted after HDIT, although this appears to stabilize at 2 years after HDIT [35, 36]. The brains of five patients, all with a progressive type of MS who had died at a median of 2 (1–18) months after HDIT, had ongoing active demyelination and acute axonal damage in MS lesions in the absence of substantial lymphocytic infiltration [37]. A mouse model of MS has demonstrated that the neuroinflammatory process after transplantation may be sustained predominantly by endogenous microglia/macrophages and that transplant earlier in the disease course was more effective [38]. The histopathology studies of the MS brain after HDIT would be consistent with the observations in the mouse model.
Table 1. Clinical trials of HDIT and autologous HCT for multiple sclerosis
ATG=antithymocyte globulin; B=BCNU; BEAM=BCNU/Etoposide/Cytosine arabinoside/melphalan; Bu=busulfan; Cy=cyclophosphamide; PFS=progression-free survival; PP=primary progressive; PR=progressive relapsing; RR=relapse-remitting; SP=secondary progressive; TBI=total body irradiation; EDSS=Expanded Disability Status Scale
*In brief, the functional levels of the Expanded Status Scale (EDSS) are graded from 0–10 points and include changes in increments of 0.5 points. An EDSS score of 0 indicates a normal neurological examination in all functional systems (FS). An EDSS score of 10 indicates death from MS. Most of the MS patients who entered these clinical trials of HDIT and autologous HCT had an EDSS score of 5.0–8.0. In general, the function of patients at these different EDSS scores are:
5.0 Ambulant 200m without aids, difficulty to work full day, FS grades 5
6.0 Intermittent or unilateral walking aid for 100m
7.0 Wheelchair-bound (walking <5m with assistance). Able to transfer and use wheelchair alone. Sometimes severe pyramidal grade 5
8.0 Bed- and chair-bound, self-care functions retained (arm function retained), sitting out of bed most of the day.
** One patient with progression of MS was started on interferon β after a relapse, developed a factor VIII inhibitor at 14 months and died at 28 months after HDIT and autologous HCT.
|
Author |
Patient n |
MS type |
Median EDSS* (range) |
Mobilization |
High-dose therapy |
T-cell Depletion |
Follow-up Median months (range) |
Treatment-/ Disease-related Mortality, |
Clinical Result |
|---|---|---|---|---|---|---|---|---|---|
|
(Fassas et al, 1997 [40]; Fassas & Nash, 2004 [32]) |
35 |
SP (19) |
6.0 |
G/GM-CSF + CY |
BEAM + ATG |
CD34 selection |
35 (3–67) |
1/1** |
PFS 81% at 5yrs |
|
(Openshaw et al, 2000 [26]) |
5 |
SP |
6.5 |
G-CSF only |
Bu/Cy |
CD34 selection |
22 (17–30) |
2/0 |
PFS 40% |
|
(Kozak et al, 2001 [34]) |
10 |
SP |
6.5 |
G-CSF + Cy |
G-CSF + Cy |
CD34 selection + monoclonals |
8 (1–18) |
0/0 |
90% stable or improved |
|
(Nash et al, 2003 [28]) |
26 |
SP (17) |
7.0 |
G-CSF + Prednisone |
TBI/Cy + ATG |
CD34 selection |
27 (2–47) |
1/1 |
76% stable or improved |
|
(Burt et al, 2003 [29]) |
21 |
SP (14) |
7.0 |
G-CSF + Cy |
TBI/Cy |
CD34 selection |
24 (12–60) |
0/2 |
62% stable or improved |
|
(Saiz et al, 2004 [33]) |
14 |
SP (9) |
6.0 |
G-CSF + Cy |
BCNU/Cy + ATG |
CD34 selection |
37 (19–55) |
0/0 |
PFS 86% |
|
(Saccardi et al, 2005 [31]) |
19 |
SP (15) |
6.5 |
G-CSF+ Cy |
BEAM + ATG |
None |
36 (12–72) |
0/0 |
PFS 95% |
|
(Samijn et al, 2006 [30]) |
14 |
SP |
6.0 |
None (marrow) |
TBI/Cy + ATG |
CD34 selection |
36 (7–36) |
0/1 |
PFS 36% |
|
(Shevchenko et al, 2008 [26]) |
50 |
SP (27) |
5.0 |
G-CSF + Cy |
BEAM + ATG |
None |
Min. follow-up |
1 (3 yrs)/0 |
PFS 72% (6 yrs) |
|
(Fagius et al, 2009 [27]) |
9 |
RR (9) |
7.0 |
G-CSF + Cy |
BEAM + ATG |
None |
29 |
0/0 |
PFS 100% |
|
(Burt et al, 2009 [18]) |
21 |
RR (21) |
3.5 |
G-CSF +Cy |
Cy +ATG |
None |
37 |
0/0 |
PFS 100% |
In the three studies reported since 2008 with a total of 80 patients, no treatment-related mortality was observed, although one patient died from acute myelogenous leukemia at 3 years after treatment (Table 1). No indication was given in the report if there were other risk factors for AML in this patient besides the transplant, such as previous treatment with mitoxantrone. In two of the more recent clinical trials, only patients with very active relapsing-remitting MS who were earlier in their disease course were included [18, 27]. Progression-free survival was observed to be 100% in both trials at a median follow-up of 2–3 years, and a marked clinical improvement was noted. Disease activity-free survival in which disease activity was defined as relapses, activity on the brain MRI, or loss of neurological function was 62% in one study [18].
Although MRI studies in the early clinical trials showed a marked and sustained reduction in Gd-enhancing brain lesions in all the groups studied compared to baseline, it was still uncertain if the continued loss of neurological function observed in some of these progressive patients was the result of a degenerative process or a failure to completely control inflammation related to the autoimmune disease. Based on the observations now in patients transplanted earlier in the course of MS and the brain histopathology studies, continued loss of neurological function is consistent with persistent microglial/macrophage activation in the MS lesions of patients with advanced disease. Future clinical trials should be done in patients with very active relapsing-remitting MS who have failed therapy while they are still early in their disease course. The NIH-sponsored HALT MS clinical trial of HDIT followed by autologous HCT for relapsing-remitting MS completed accrual in late 2009 (n=24). A 5-year follow-up is planned to assess stability of the response. Randomized clinical trials need to be completed to confirm if there is a therapeutic benefit of HDIT and autologous HCT for MS. In Europe, the Autologous Stem cell Transplantation International Multiple Sclerosis (ASTIMS) randomized clinical trial included patients with secondary progressive MS with an EDSS of 3.5–6.5. ASTIMS was closed because of poor accrual.
Systemic sclerosis
Systemic sclerosis is an uncommon disabling autoimmune disease that is characterized by two major clinical features: 1) a non-inflammatory small vessel vasculopathy and, 2) fibrosis of the skin and multiple internal organs [41]. Antinuclear antibodies occur in 95% of SSc patients and the anti-topoisomerase I antibody (Scl-70) is found in 30–40% of subjects with diffuse cutaneous SSc. Diffuse cutaneous SSc has a higher mortality than limited cutaneous SSc and is associated with substantial morbidity. Clinical manifestations include digital ischemia/skin ulcerations from the vasculopathy, both truncal and acral scleroderma, interstitial lung disease, hypertensive renal crisis, diffuse GI disease, and myocardial involvement. The modified Rodnan skin score (mRSS) and the modified Health Assessment Questionnaire Disability Index for SSc (SHAQ) are two validated tools for evaluating the degree of scleroderma and measuring the effect of disease on overall function [42].
Immunosuppressive therapies investigated for severe SSc have been inadequate or ineffective. A 12-month course of cyclophosphamide was reported to be superior to placebo in slowing the rate of progression of SSc lung disease at 12 months after start of treatment, but later follow-up showed that the overall effect was modest and not sustained at 24 months [43, 44]. However, cyclophosphamide might be considered a standard of care for individuals with SSc since no other immunosuppressive treatment has been shown in a controlled setting to be of any benefit whatsoever. Important supportive care measures for SSc patients include angiotensin-converting enzyme inhibitors for management of renal crisis, and bosentan or other agents for management of pulmonary hypertension.
A still limited number of clinical trials of HDIT and autologous HCT for SSc have been conducted. Patients included in these clinical trials had a poor prognosis based on the presence of diffuse cutaneous disease and internal organ involvement. In a single center study of high-dose cyclophosphamide as a single agent (n=10) or melphalan (n=1) and autologous HCT, major or partial responses were observed in 8 of 11 patients, but at a median of 18 months, 8 patients had relapsed or not achieved a response (Table 2) [15].
Table 2. Clinical trials of HDIT and autologous HCT for systemic sclerosis
*There was one additional death at 5 years after HDIT from lung cancer.
BL=baseline; Cy=cyclophosphamide (mobilization: 2 or 4 g/m2; treatment: 120 mg/kg in combination with TBI or 200 mg/kg if single cytotoxic agent); DLCO=diffusion capacity of the lung for carbon monoxide; EFS=event-free survival; Mel=melphalan; mRSS=modified Rodnan skin score (ranges from 0–51; increasing score indicates worsening scleroderma); PFS=progression-free survival.
Author | Patient | BL Median DLCO% (range) | BL Median mRSS (range) | Mobilization | High-dose therapy | T-cell depletion | Follow-up Median months (range) | Treatment-related/ Disease-related Mortality, | Clinical results |
|---|---|---|---|---|---|---|---|---|---|
(McSweeney et al, 2002 [45]; Nash et al, 2007 [7]) | 34 | 61 | 30 | G-CSF | TBI / Cy + ATG | CD34 selection | 48 | 8/4 | PFS – 64% |
(Farge et al, 2002 [15]) | 11 | 67 | 29 | G-CSF + Cy | G-CSF + Cy | CD34 selection (n=9) | 18 | 1/3 | 3 patients alive in remission (27%) |
(Tsukamoto et al, 2006 [46]) | 6 | 47 | 26 | G-CSF + Cy | Cy | CD34 selection | 20 | 0/0 | Improvement in skin score (P=0.05) and lung function |
(Loh et al, 2007 [48]; Milanetti et al, 2009 [47]) | 37 | ? | 25 | G-CSF + Cy | Cy + ATG | None | 24 | 4/2 | EFS 68% |
(Vonk et al, 2008) [10] | 28 | 55 | 32 | G-CSF + Cy | Cy | CD34 selection | 63 (12–90) | 2/2* | EFS (evaluable, n=26) |
Four patients (36%) had died by 18 months after HDIT. In a later study of patients who had survived at least 6 months after high-dose cyclophosphamide only and HCT (n=26), survival was 96% and event-free survival was 64% at 5 years [10]. However, about half of the patients included in this study had diffuse cutaneous disease albeit without internal organ involvement. In the North American multicenter pilot study of a more intensive HDIT regimen consisting of TBI and cyclophosphamide in patients with diffuse cutaneous disease and internal organ involvement, 17 of 27 evaluable patients (63%) who survived at least 1 year after HDIT had sustained responses (without progression or disease activation) at a median follow-up of 4 years [7]. Patients with sustained responses had required no immune-based treatment after HDIT. There was a major improvement in the degree of scleroderma as measured by mRSS and in overall function as measured by the mHAQ at final evaluation (Figure 1A and B).
Figure 1. Change in modified Rodnan skin score (mRSS), modified Health Assessment Questionnaire (mHAQ) score, and lung function after high-dose immunosuppressive therapy (HDIT) and autologous hematopoietic cell transplantation
A determination was made whether a parameter value was statistically significantly increasing or decreasing over time using a generalized estimating equation (GEE) model. The bold black solid line represents the mean value over time for the parameter of interest. The bold black dotted line represents an estimate of the modeled linear relationship between the parameter value and time and summarizes the results of the GEE models. The gray solid lines are parameter values for individual patients. The mean mRSS and mHAQ values statistically significantly decreased with time after HDIT (both P<0.0001; panels A and B, respectively). The mean values for diffusion capacity of the lung for carbon monoxide (DLCO) adjusted for hemoglobin levels did not significantly change (P=0.50, panel C), and forced vital capacity statistically significantly increased with time (P=0.01, panel D). (This figure based on a figure originally published in Blood. Nash RA, McSweeney PA, Crofford LJ, Abidi M, et al. High-dose immunosuppressive therapy and autologous hematopoietic cell transplantation for severe systemic sclerosis: long-term follow-up of the U.S. multicenter pilot study. Blood. 2007;110:1388-1396. © the American Society of Hematology.)

Skin biopsies confirmed that the improvement in skin score was associated with a significant decrease of dermal fibrosis (Figure 2) [7, 49].
Figure 2. Resolution of dermal fibrosis after HDIT and autologous HCT
Shown are full thickness skin biopsies from a patient in the North American pilot study for the SCOT clinical trial. Skin biopsies were collected at baseline (A and B) and then at 1 (C and D) and 5 years (E and F) after HDIT from the same location. Dermal fibrosis was evaluated after staining the skin with H&E and examined under low and high power magnification. At baseline, pan-dermal sclerosis from the dermal-epidermal border to the hypodermis (subcutaneous fat) was observed.
The reticular dermis is replaced by a dense compact collagen without normal collagen bundles or dermal appendages. (Original optic 5x. B)
As in 1A but at higher power, the straightened dermal-subcutaneous border demonstrates the abnormal, densely packed, homogenized collagen. (Original optic 20x. C)
A low power view of the skin biopsy at 1 year after HDIT shows crowded collagen bundles with focal areas of residual sclerosis but less than at baseline. (Original optic 5x. D)
A higher power view of the 1-year skin biopsy from C shows collagen bundles some of which are hypereosinophilic and straightened but overall there is no longer the appearance of homogenization. (Original optic 20x. E)
The skin biopsy at 5 years shows that the thickness of the dermis has decreased from baseline. There has been resolution of the dermal fibrosis. There is now some thinning of the collagen bundles with a relative increase in the space between the collagen bands. The dermal-epidermal border remains straightened with loss of rete ridges. (Original optic 5x. F)
A higher power view of collagen in lower reticular dermis demonstrates a change to thin wavy collagen bundles separated by increased ground substance. (Original optic 20x)
(This figure is based upon a figure originally published in Blood. Nash RA, McSweeney PA, Crofford LJ, Abidi M, et al. High-dose immunosuppressive therapy and autologous hematopoietic cell transplantation for severe systemic sclerosis: long-term follow-up of the U.S. multicenter pilot study. Blood. 2007;110:1388-1396. © the American Society of Hematology.)

Lung, heart and kidney function, in general, remained clinically stable (Figure 1C and D). Histological studies of the microvasculature of the skin also showed improvement after HDIT [50]. There was an increased capillary count in post-transplant SSc skin and interferon alpha, vascular endothelial cadherin and RGS5 had returned to normal levels. The treatment-related mortality was 23%, and progression-free survival was 64% at 5 years. Other studies have also suggested a major clinical effect of HDIT on skin and function [46, 47]. The cumulative probability of disease progression at 5 years was 48% and the cumulative probability of survival at 5 years was 72% in registry data from EBMT [21]. Two randomized clinical trials of HDIT followed by autologous HCT for SSc are currently being conducted, one in Europe (ASTIS) and the other in North America (SCOT; website: www.sclerodermatrial.org).
Systemic lupus erythematosus
Systemic lupus erythematosus (SLE) is characterized by the presence of anti-nuclear antibodies and immune complexes [51]. Disease severity may vary from mild to life threatening, and numerous organ systems may be involved. Antinuclear antibodies, anti-double stranded DNA antibodies, and anti-Smith antibodies are present in 98%, 70% and 25% of SLE patients, respectively. Overall, the 10-year survival of patients with SLE has been reported as 75–85%, with more than 90% surviving at 5 years [52]. Standard treatment options are not curative and complete sustained remissions are rare. Antimalarials such as hydroxychloroquine reduce the frequency of disease flares, and low-dose corticosteroids are used for patients in whom disease symptoms have not been controlled by more conservative measures. Agents such as cyclophosphamide, azathioprine, rituximab and mycophenolate mofetil have also been found effective in controlling disease activity [53]. The SLE Disease Activity Index (SLEDAI) is a validated tool for following disease activity [54].
Clinical trials of HDIT with and without HCT were conducted on patients with SLE who were refractory to standard therapies. In a single center study (n=50) of HDIT and HCT, patients underwent stem cell mobilization with G-CSF and cyclophosphamide, and the autologous graft was T cell-depleted by CD34-selection [8]. The HDIT regimen consisted of high-dose cyclophosphamide (200 mg/kg) and ATG. There was a significant improvement in the SLEDAI score, renal function stabilized and titers of the anti-nuclear and anti-double stranded DNA antibodies improved after HDIT. Overall and disease-free survival at 5 years was 84% and 50%, respectively. Treatment-related mortality was 4% (two patients) and both deaths occurred before HDIT. The EBMT registry reported the experience with HDIT and autologous HCT for SLE and observed significant disease responses in 31 of 50 patients, although many remained on some maintenance therapy after transplantation [55]. In comparison, a study of high-dose cyclophosphamide (200 mg/kg) without HCT (n=14) showed that only 5 patients (36%) had durable complete remissions at a median follow-up of 27 months [20]. Although this approach avoids the re-infusion of cells, the relapse rates were comparable with or without the transplant of autologous hematopoietic cells. If there is no difference in relapse rates, then transplantation of hematopoietic cells would be expected to be beneficial due to a reduction in the time to recovery of blood cell counts. Although experience is still limited, HDIT can induce a high percentage of disease responses in patients with SLE who had otherwise been refractory to standard therapy, and remissions have been durable in a significant proportion of patients.
Rheumatoid arthritis
The pathological hallmark of Rheumatoid arthritis (RA) is synovial inflammation with proliferation of macrophages and fibroblasts. If severe, the inflamed synovium develops into an invasive pannus which destroys cartilage and bone [56]. Other complications are a vasculitis, cervical spine disease, lung nodules or interstitial fibrosis, and cardiac complications including pericarditis. Risk of progression can be predicted by prognostic factors such as increased number of affected joints, a high level of C-reactive protein, presence of rheumatoid factor, and extra-articular features of the disease [56]. The risk of mortality is increased with more severe disease activity or ≥ 1 extra-articular disease manifestation [57, 58, 59]. There is a mortality of approximately 30% at 5 years for patients with the highest disease activity. Many anti-cytokine or immunomodulatory agents have been approved for the treatment of RA including methotrexate, hydroxychloroquine, sulfsalazine, leflunamide, infliximab, adalimumab, etanercept, abatacept, and anakinra. B-cell targeted therapy with rituximab has recently been shown to be effective as well. The goal of standard therapy is to relieve the signs and symptoms of the disease since none of these treatments are curative. The criteria for determining response to treatment have been defined by the American College of Rheumatology [60].
Four small clinical trials of high-dose cyclophosphamide with or without ATG for patients with RA who had failed standard treatment have been reported [14, 61, 62, 63, 64, 65]. There were early major responses in the majority of the patients, but on long-term follow-up, all 32 patients accrued to these clinical trials relapsed and required additional treatment. Although disease activity recurred, one study showed that after HDIT, there was a decrease in progression of joint damage compared to baseline [66]. No mortality was observed in any of the clinical trials. Seventy-six patients with RA who underwent HDIT and autologous HCT were available for analysis in the EBMT registry, and the outcomes were comparable to the experience reported from the clinical trials [67]. Major responses were observed in 67% of patients, with a significant reduction in the measures of disability. Most patients had restarted immunomodulatory treatment by 6 months after HDIT for persistent or recurrent disease activity. No treatment-related mortality was observed. The apparent difference in response of RA to HDIT compared to other autoimmune diseases might be related to immune or non-immune biological factors. More durable responses might be obtained with more intense HDIT regimens, but this may increase the risk for treatment-related mortality. Another strategy to decrease relapses or progression may be the addition of immunomodulatory therapy after HDIT.
Juvenile idiopathic arthritis
Juvenile idiopathic arthritis (JIA) is a heterogeneous group of chronic inflammatory diseases involving the joints and extra-articular tissues that begins before 16 years of age [68]. Severe disease has an effect on bone and joint development resulting in overgrowth or undergrowth of juxta-articular bone resulting in limb deformities. The macrophage activation syndrome is a potentially life-threatening complication in which there is uncontrolled activation and proliferation of macrophages and T cells. This complication may occur in 5–8% of patients with systemic JIA. The mortality is <1% and occurs mostly in the systemic JIA subtype [69]. One clinical trial of HDIT and autologous HCT in patients with treatment-refractory JIA (n=22) was reported with a median follow-up of 80 months [6]. The HDIT regimen consisted of TBI (400 cGy), cyclophosphamide, and ATG. Early in the clinical trial, two patients developed macrophage activation syndrome less than 1 month after HDIT and both died. Precautionary measures added to the treatment may have reduced this risk in later patients. Two other patients died after relapsing and restarting immunosuppressive treatment more than 1 year after HDIT. Overall and disease-free survival was 82% and 36%, respectively. There were significant sustained improvements in disease activity in the group based on disability and active joint scores. In a more recent report of 7 patients, 4 patients had sustained responses, 2 patients relapsed within 1–12 months of transplant, and 1 patient died at 4 months post-transplant [70]. In a report from the EBMT registry on 34 JIA patients, 18 (53%) were in complete remission without additional therapy at 12 to 60 months after HDIT [71]. In a small subset of poor prognosis JIA patients who fail to respond to standard treatment, HDIT and autologous HCT may be of benefit, although this may be associated with a substantial risk in a disease that is not per se life threatening.
Crohn’s disease
In a clinical trial of patients with treatment-refractory Crohn’s disease, 11 of 12 patients achieved sustained remissions at a median of 18 (7–37) months after HDIT without significant treatment-related toxicity or mortality [72]. In another study, 3 of 4 patients achieved clinical and endoscopic remissions at a median of 16.5 months after HDIT [73]. Longer follow-up is required to assess the durability of response.
Diabetes mellitus
An interesting clinical trial was performed in patients with recent-onset diabetes mellitus. Fourteen of 15 patients had prolonged periods of insulin independence after high-dose cyclophosphamide and autologous HCT [16]. In a follow-up to that report and with inclusion of 8 additional patients, 20 of 23 patients became insulin-independent after HDIT and 12 patients maintained that status for a mean of 31 months; 8 patients relapsed and required insulin again [74]. C-peptide levels were significantly increased after transplant compared to baseline. About 50% of patients may achieve a prolonged insulin-free period after HDIT but longer follow-up is required.
Immune reconstitution after high-dose immunosuppressive therapy
Natural killer (NK) cell counts recovered by 1 month and B and CD8+ T-cell counts recovered by 6–12 months after HDIT. There was a slower recovery of CD4+ T cell counts, which reach low–normal levels by 2 years [12]. Immune recovery at 2 years after HDIT was associated with increasing thymic-derived naïve CD4+ T cells (Figure 3) [11].
Figure 3. Central memory CD4+ T cells decreased and naïve CD4+ T cells increased at 2 years after HDIT and autologous HCT for MS
At the 2-year follow-up, the frequency of naïve CD4+ T cells in the blood had increased 118% as compared with pretherapy (P=0.032). Correspondingly, CM CD4+ T cells had decreased 38% at 2 years after therapy (P=0.008). The frequencies of the EM CD4+ T cells did not change significantly at the 2-year follow-up compared with the baseline. These data support the concept that there is significant immunomodulation at 2 years after HDIT and autologous HCT, and this may explain the observed durable clinical remissions in a significant proportion of patients with autoimmune disease. Reproduced with permission. © Muraro et al., 2005. J. Exp. Med. doi:10.1084/jem.20041679

It was also observed that there was an increase in T cell receptor excision circles (TRECs; a marker for recent thymic emigrants) in CD4+ T cells at 1 and 2 years after HDIT and a steady decrease over time in CD4+ central memory T cells. CD4+ effector memory cells were relatively increased at 6 months after HDIT, likely from homeostatic proliferation, but had recovered to normal levels by 2 years. There were no significant changes in the CD8+ T cell subsets. Several investigators have reported an increase in regulatory CD4+ FoxP3+ and CD8+FoxP3+ T cells, and broader clonal diversity than present before [11, 13, 75, 76, 77]. In association with the increased levels of naïve CD4+ T cells, there was hypertrophy of the thymus at 1 and 2 years compared to baseline especially in the younger patients (less than 43 years of age) [12]. This evidence suggested a thymic origin for the recovery of the CD4+ T-cell repertoire after HDIT and autologous HCT. Even though B-cell counts were very low in the first 3 months after HDIT, median serum levels of immunoglobulin G specific for tetanus toxoid, Hemophilus influenzae and Streptococcus pneumoniae, were normal [12]. There was recovery of the naïve B cell compartment in SLE patients by 1 year after HDIT [76]. The clinical responses to HDIT, which have persisted for 2 or more years in several autoimmune diseases, may be a result of these late immunomodulatory effects.
Allogeneic HCT for autoimmune diseases
Outcomes in patients with autoimmune diseases transplanted for another primary disease
Our first understanding of the effect of allogeneic HCT on human autoimmune diseases came from experience in transplanting patients with hematologic disorders who also suffered from autoimmune diseases (Table 3) [78, 79, 80, 81, 82, 83, 84, 85, 86, 87, 88, 89, 90, 91, 92, 93, 94,95].
Table 3. Outcomes in patients with autoimmune diseases transplanted with an allogeneic hematopoietic cell graft for another primary disease
Abbreviations: AML=acute myeloid leukemia; ALL=acute lymphoblastic leukemia; ANA=anti-nuclear antibody; CML=chronic myelogenous leukemia; LGL=large granular lymphocytes; MM=multiple myeloma; NHL=Non-Hodgkin lymphoma; SAA=severe aplastic anemia.
*Clinical remission but ANA remained positive.
†Relapse occurred in patient with mixed chimerism.
Autoimmune Disease | Hematologic Disease | Evaluable Patients (total) n | Remission of Autoimmune Disease after HCT, n | Outcome (alive at last follow-up), n | Follow-up |
|---|---|---|---|---|---|
Rheumatoid arthritis (Baldwin et al, 1977 [78]; Jacobs et al, 1986 [79]; McKendry et al, 1996 [80]; Lowenthal et al, 1993 [81]; Snowden et al, 1998 [82]; Lowenthal et al, 2006 [83]; Tapprich et al, 2003 [84]) | SAA (n=8), 1 MM | 9 | 7 (2 relapses +1 transient relapse) | 6 | 2 mos–21 yrs |
Systemic lupus erythematosus (Gur-Lavi, 1999 [85]) | SAA | 1 | 1* (ANA titer +) | 1 | 15 yrs |
Psoriatic arthritis (Yin & Jowitt, 1992 [86]; Slavin et al, 2000 [87]; Snowden et al, 1998 [82]; Eedy et al, 1990 [88]) | AML, CML (n=3) | 4 | 3 (1 relapse) | 3 | 1, 3, 5, 5 yrs |
Ulcerative colitis (Yin & Jowitt, 1992 [86]) | AML | 1 | 1 | 1 | 4 yrs |
Crohn’s disease [Lopez-Cubero et al, 1998 [89] | CML | 5 | 4† | 5 | 4.5–15.3 yrs |
Multiple sclerosis (Mandalfino et al, 2000 [90]; McAllister et al, 1997 [91]; La Nasa et al, 2004 [92]; Jeffery, 2007 [93]) | CML (n=2), LGL Leukemia, AML | 4 | 3 | 3 | 1, 2, 3, 4 yrs |
Autoimmune hepatitis (Vento et al, 1996 [94]) | ALL | 1 | 1 | 1 | 4 yrs |
Lupus anticoagulant (Olalla et al, 1999 [95]) | CML | 1 | 1 | 1 | 5 yrs |
In RA patients, sustained remissions have been observed for as long as 20 years after allogeneic HCT [83]. However, relapses were observed in 3 of the 9 reported RA patients. One of the relapses was transient with a subsequent treatment-free remission of 11 years. In one of the two sustained relapses, the HLA-identical donor was serologically positive for rheumatoid factor but without clinical disease [79]. Sustained remissions and some relapses have also been observed in patients with other concomitant autoimmune diseases after allogeneic HCT (Table 3). One patient who relapsed with Crohn’s disease had mixed hematopoietic chimerism detected at 3 months after HCT. Hinterberger et al did a literature search and identified reports of patients with an autoimmune disease who were transplanted for severe aplastic anemia or a hematologic malignancy between 1977 and 2001 [96]. Attempts were then made to update these reports. Disease-free survival after allogeneic HCT of patients with aplastic anemia (n=23) was 78% at 16 years and survival in unmaintained remission of the concomitant autoimmune disease was 64% at 13 years. The results were similar for patients with autoimmune diseases who underwent allogeneic HCT for hematologic malignancies. An association was noted between the development of GVHD and the risk for relapse of the autoimmune disease. The risk for relapse of the autoimmune disease was lower after allogeneic than after autologous HCT. There were insufficient data from the case reports/series to develop an understanding of why relapses occurred after allogeneic HCT. After allogeneic HCT from an HLA-identical sibling, one possible explanation for recurrence of the autoimmune disease may be genetic factors that are shared between the donor and recipient. Another possible explanation is the persistence of host immune cells resulting in the recurrence of disease activity.
Allogeneic hematopoietic cell transplantation for autoimmune diseases as the primary indication
The primary risks of allogeneic HCT are the morbidity and mortality associated with a delayed immune reconstitution and graft-versus-host disease (GVHD). Therefore, there has been a reluctance to consider this approach except for extreme cases of refractory autoimmune diseases. Although the risk of complications and treatment-related mortality is greater than after autologous HCT, there may be a greater potential for sustained remissions of severe autoimmune diseases after allogeneic HCT and, therefore, the possibility of an improved overall outcome. Survival after allogeneic HCT for nonmalignant hematological disorders or good-risk hematological malignancies such as chronic myelogenous leukemia in chronic phase has ranged from 85–95%. The best outcomes were observed in young patients transplanted from HLA-matched donors. No clinical trials have yet been conducted of allogeneic HCT for which an autoimmune disease was the primary indication, but a small number of cases have been reported. The largest experience has been in patients with autoimmune cytopenias [97, 98, 99, 100]. Of the seven evaluable patients reported from the EBMT registry, five were alive and in remission at a median follow-up of 41 months [97]. One patient with Evans syndrome in the report from the EBMT registry had disease progression and died. The second patient died from treatment-related complications after HCT from an HLA-haploidentical donor. Of the three case reports of Evans syndrome in the literature, one patient relapsed and died and the other two died of transplant-related complications in complete remission [98, 99, 100]. There are six cases reported of allogeneic HCT for connective tissue diseases like SSc, overlap syndrome, and RA [48, 101, 102, 103, 104]. Two patients with SSc had high-dose conditioning, one of whom was alive at 5 years in disease remission with resolution of the dermal fibrosis and severe scleroderma. The four other patients received reduced intensity conditioning regimens. All patients were alive at last follow-up and in remission. Three of these patients had stable mixed hematopoietic chimerism and no history of GVHD. Regulatory immune mechanisms associated with the establishment of mixed hematopoietic chimerism may be responsible for inducing remission of the autoimmune disease [105]. Daikeler et al. reported a case series of 35 patients who had allogeneic HCT between 1984 and 2007 for a primary indication of an autoimmune disease and were reported to the EBMT registry [106]. Responses occurred in 78% of patients, but in this heavily pre-treated population, the treatment-related mortality was 22%. Relapses were again observed in a small number of cases. These registry data had significant limitations since the patient population was very heterogeneous for both treatment and disease type, as well as the fact that the data were often incomplete. Conclusions regarding the therapeutic role of allogeneic HCT for severe autoimmune diseases await the results from prospective clinical trials conducted in carefully selected patients.
Conclusions
A high rate of remission in autoimmune diseases is observed after HDIT and autologous HCT, and a significant proportion are sustained after 4–5 years. The rate and durability of response may depend on the intensity of the HDIT regimen and the type of autoimmune disease being treated. Randomized clinical trials are now being conducted in specific autoimmune diseases. The experience with allogeneic HCT as a treatment for autoimmune diseases is still limited, but promises to be highly effective. Carefully selected patients with active autoimmune disease that is life-threatening or threatening critical organ function and refractory to standard treatment should be considered as candidates for clinical trials of allogeneic HCT or HDIT followed by autologous HCT.
Acknowledgements
Grants to acknowledge are: National MS Society- RG4183
References
1. Good RA, Ikehara S. Preclinical investigations that subserve efforts to employ bone marrow transplantation for rheumatoid or autoimmune diseases. Journal of Rheumatology. 1997;24(48);5-12.
2. Shizuru JA. The experimental basis for hematopoietic cell transplantation for autoimmune diseases. Thomas' Hematopoietic Cell Transplantation (ed. by F.R.Appelbaum, S.J.Forman, R.S.Negrin and K.G.Blume), Oxford, UK, Wiley-Blackwell. 2009. 264 p.
4. Cooley HM, Snowden JA, Grigg AP, Wicks IP. Outcome of rheumatoid arthritis and psoriasis following autologous stem cell transplantation for hematologic malignancy. Arthritis and Rheumatism. 1997;40:1712-1715.
9. Saccardi R, Kozak T, Bocelli-Tyndall C, Fassas A, et al, Autoimmune Diseases Working Party of EBMT. Autologous stem cell transplantation for progressive multiple sclerosis: update of the European Group for Blood and Marrow Transplantation autoimmune diseases working party database. Multiple Sclerosis. 2006;12:814-823.
10. Vonk MC, Marjanovic Z, van den Hoogen FH, Zohar R, et al. Long-term follow-up results after autologous haematopoietic stem cell transplantation for severe systemic sclerosis [Erratum appears in Ann Rheum Dis. 2008 Feb;67(2):280]. Annals of the Rheumatic Diseases. 2008;67:98-104.
12. Storek J, Zhao Z, Lin E, Berger T, et al. Recovery from and consequences of severe iatrogenic lymphopenia (induced to treat autoimmune diseases). Clinical Immunology. 2004;113:285-298.
15. Farge D, Marolleau JP, Zohar R, Marjanovic Z, et al, Intensification et Autogreffe dans les Maladies Auto Immunes Resistantes (ISAMAIR) Study Group. Autologous bone marrow transplantation in the treatment of refractory systemic sclerosis: early results from a French multicentre phase I-II study. British Journal of Haematology. 2002;119:726-739.
18. Burt RK, Loh Y, Cohen B, Stefoski D, et al. Autologous non-myeloablative haemopoietic stem cell transplantation in relapsing-remitting multiple sclerosis: a phase I/II study [Erratum appears in Lancet Neurol. 2009 Apr;8(4):309]. Lancet Neurology. 2009;8:244-253.
19. Brodsky RA, Chen AR, Brodsky I, Jones RJ. High-dose cyclophosphamide as salvage therapy for severe aplastic anemia. Experimental Hematology. 2004;32:435-440.
22. Mayes M, Crofford L, Csuka ME, Furst D, et al. Autologous transplantation for systemic sclerosis in North America. Report of the scleroderma: cyclophosphamide or transplantation trial. Haematopoietic Stem Cell Transplantation for Severe Autoimmune Diseases, Abstract Book. 2009;4(Abstract):12.
25. Openshaw H, Lund BT, Kashyap A, Atkinson R, et al. Peripheral blood stem cell transplantation in multiple sclerosis with busulfan and cyclophosphamide conditioning: report of toxicity and immunological monitoring. Biology of Blood and Marrow Transplantation. 2000;6:563-575.
26. Shevchenko YL, Novik AA, Kuznetsov AN, Afanasiev BV, et al. High-dose immunosuppressive therapy with autologous hematopoietic stem cell transplantation as a treatment option in multiple sclerosis. Experimental Hematology. 2008;36:922-928.
27. Fagius J, Lundgren J, Oberg G. Early highly aggressive MS successfully treated by hematopoietic stem cell transplantation. Multiple Sclerosis. 2009;15:229-237.
30. Samijn JP, te Boekhorst PA, Mondria T, van Doorn PA, et al. Intense T cell depletion followed by autologous bone marrow transplantation for severe multiple sclerosis. Journal of Neurology. Neurosurgery and Psychiatry. 2006;77:46-50.
32. Fassas A, Nash R. Stem cell transplantation for autoimmune disorders. Multiple
sclerosis. Best Pract Res Clin Haematol. 2004 Jun;17(2):247-62.
33. Saiz A, Blanco Y, Carreras E, Berenguer J, et al. Clinical and MRI outcome after autologous hematopoietic stem cell transplantation in MS. Neurology. 2004;62:282-284.
34. Kozak T, Havrdova E, Pit'ha J, Gregora E, et al. Immunoablative therapy with autologous stem cell transplantation in the treatment of poor risk multiple sclerosis. Transplantation Proceedings. 2001;33:2179-2181.
35. Chen JT, Collins DL, Atkins HL, Freedman MS, et al, Canadian MS BMT Study Group. Brain atrophy after immunoablation and stem cell transplantation in multiple sclerosis. Neurology. 2006;66:1935-1937.
36. Roccatagliata L, Rocca M, Valsasina P, Bonzano L, et al, Italian GITMO-NEURO Intergroup on Autologous Stem Cell Transplantation. The long-term effect of AHSCT on MRI measures of MS evolution: a five-year follow-up study. Multiple Sclerosis. 2007;13:1068-1070.
38. Cassiani-Ingoni R, Muraro PA, Magnus T, Reichert-Scrivner R, et al. Disease progression after bone marrow transplantation in a model of multiple sclerosis is associated with chronic microglial and glial progenitor response. Journal of Neuropathology and Experimental Neurology. 2007;66:637-649.
41. Valentini G, Black C. Systemic sclerosis (Review). Best Practice and Research in Clinical Rheumatology. 2002;16:807-816.
42. Clements PJ, Lachenbruch PA, Ng SC, Simmons M, et al. Skin score. A semiquantitative measure of cutaneous involvement that improves prediction of prognosis in systemic sclerosis. Arthritis and Rheumatism. 1990;33:1256-1263.
44. Tashkin DP, Elashoff R, Clements PJ, Roth MD, et al. Effects of 1-year treatment with cyclophosphamide on outcomes at 2 years in scleroderma lung disease. American Journal of Respiratory and Critical Care Medicine. 2007;176:1026-1034.
46. Tsukamoto H, Nagafuji K, Horiuchi T, Miyamoto T, et al. A phase I-II trial of autologous peripheral blood stem cell transplantation in the treatment of refractory autoimmune disease. Annals of the Rheumatic Diseases. 2006;65:508-514.
47. Milanetti F, Bucha J, Kwasny M, Boyce K, et al. Autologous non-myeloablative hematopoietic stem cell transplantation in patients with systemic sclerosis. Haematopoietic Stem Cell Transplantation for Severe Autoimmune Diseases, Abstract Book. 2009;9(Abstract):44-45.
51. D'Cruz DP, Khamashta MA, Hughes GR. Systemic lupus erythematosus (Review). Lancet. 2007;369:587-596.
53. Smith KG, Jones RB, Burns SM, Jayne DR. Long-term comparison of rituximab treatment for refractory systemic lupus erythematosus and vasculitis: Remission, relapse, and re-treatment. Arthritis and Rheumatism. 2006;54:2970-2982.
54. Bombardier C, Gladman DD, Urowitz MB, et al. Derivation of the SLEDAI. A disease activity index for lupus patients. The Committee on Prognosis Studies in SLE. Arthritis and Rheumatism. 1992;35:630-640.
55. Jayne D, Passweg J, Marmont A, Farge D, et al. Autologous stem cell transplantation for systemic lupus erythematosus. Lupus. 2004;13:168-176.
56. Lee DM, Weinblatt ME, Lee DM, Weinblatt ME. Rheumatoid arthritis (Review). Lancet. 2001;358:903-911.
60. Pinals RS, Masi AT, Larsen RA. Preliminary criteria for clinical remission in rheumatoid arthritis. Arthritis and Rheumatism. 1981;24:1308-1315.
61. Bingham SJ, Snowden J, McGonagle D, Richards R, et al. Autologous stem cell transplantation for rheumatoid arthritis – interim report of 6 patients. Journal of Rheumatology. 2001;64(Suppl.):21-24.
65. Pavletic SZ, Klassen LW, Pope R, O'Dell JR, et al. Treatment of relapse after autologous blood stem cell transplantation for severe rheumatoid arthritis. Journal of Rheumatology. 2001;64(Suppl.):28-31.
67. Snowden JA, Passweg J, Moore JJ, Milliken R, et al. Autologous hemopoietic stem cell transplantation in severe rheumatoid arthritis: a report from the EBMT and ABMTR. Journal of Rheumatology. 2004;31:482-488.
68. Ravelli A, Martini A. Juvenile idiopathic arthritis (Review). Lancet. 2007;369:767-778.
70. Abinun M, Flood TJ, Cant AJ, Veys P, et al. Autologous T cell depleted haematopoietic stem cell transplantation in children with severe juvenile idiopathic arthritis in the UK (2000-2007). Molecular Immunology. 2009;47:46-51.
72. Oyama Y, Craig RM, Traynor AE, Quigley K, Statkute L, Halverson A, Brush M, Verda L, Kowalska B, Krosnjar N, Kletzel M, Whitington PF, Burt RK. Autologous hematopoietic stem cell transplantation in patients with refractory Crohn's disease. Gastroenterology. 2005;128:552-563.
73. Cassinotti A, Annaloro C, Ardizzone R, Onida F, et al. Autologous haematopoietic stem cell transplantation without CD34+ cell selection in refractory Crohn's disease. Gut. 2008;57:211-217.
74. Couri CE, Oliveira MC, Stracieri AB, Moraes DA, et al. C-peptide levels and insulin independence following autologous nonmyeloablative hematopoietic stem cell transplantation in newly diagnosed type 1 diabetes mellitus. Journal of the American Medical Association. 2009;301:1573-1579.
75. Zhang L, Bertucci AM, Ramsey-Goldman R, et al. Regulatory T cell (Treg) subsets return in patients with refractory lupus following stem cell transplantation, and TGF-beta-producing CD8+ Treg cells are associated with immunological remission of lupus. Journal of Immunology. 2009;183:6346-6358.
78. Baldwin JL, Storb R, Thomas ED, Mannik M. Bone marrow transplantation in patients with gold-induced marrow aplasia. Arthritis and Rheumatism. 1977;20:1043-1048.
79. McKendry RJ, Huebsch L, Leclair B. Progression of rheumatoid arthritis following bone marrow transplantation. A case report with a 13-year followup. Arthritis and Rheumatism. 1996;39:1246-1253.
80. Jacobs P, Vincent MD, Martell RW. Prolonged remission of severe refractory rheumatoid arthritis following allogeneic bone marrow transplantation for drug-induced aplastic anemia. Bone Marrow Transplantation. 1986:1:237-239.
81. Lowenthal RM, Cohen ML, Atkinson K, Biggs JC. Apparent cure of rheumatoid arthritis by bone marrow transplantation. Journal of Rheumatology. 1993;20:137-140.
83. Lowenthal RM, Francis H, Gill DS. Twenty-year remission of rheumatoid arthritis in 2 patients after allogeneic bone marrow transplant. Journal of Rheumatology. 2006;33:812-813.
86. Yin JA, Jowitt SN. Resolution of immune-mediated diseases following allogeneic bone marrow transplantation for leukaemia. Bone Marrow Transplantation. 1992;9:31-33.
87. Slavin R, Nagler A, Varadi G, Or R. Graft vs autoimmunity following allogeneic non-myeloablative blood stem cell transplantation in a patient with chronic myelogenous leukemia and severe systemic psoriasis and psoriatic polyarthritis. Experimental Hematology. 2000;28:853-857.
89. Lopez-Cubero SO, Sullivan KM, McDonald GB. Course of Crohn's disease after allogeneic marrow transplantation. Gastroenterology. 1998;114:433-440.
90. Mandalfino P, Rice G, Smith A, Klein JL, et al. Bone marrow transplantation in multiple sclerosis. Journal of Neurology. 2000;247:691-695.
92. La Nasa G, Littera R, Cocco E, Battistini L, et al. Allogeneic hematopoietic stem cell transplantation in a patient affected by large granular lymphocyte leukemia and multiple sclerosis. Annals of Hematology. 2004;83:403-405.
93. Jeffery DR. Failure of allogeneic bone marrow transplantation to arrest disease activity in multiple sclerosis. Multiple Sclerosis. 2007;13:1071-1075.
94. Vento R, Cainelli F, Renzini C, et al. Resolution of autoimmune hepatitis after bone-marrow transplantation. Lancet. 1996;348:544-545.
102. Khorshid O, Hosing C, Bibawi R, Ueno N, et al. Nonmyeloablative stem cell transplant in a patient with advanced systemic sclerosis and systemic lupus erythematosus. Journal of Rheumatology. 2004;31:2513-2516.
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "500" ["~SORT"]=> string(3) "500" ["CODE"]=> string(70) "transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh" ["~CODE"]=> string(70) "transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh" ["EXTERNAL_ID"]=> string(4) "1441" ["~EXTERNAL_ID"]=> string(4) "1441" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["ELEMENT_META_KEYWORDS"]=> string(0) "" ["ELEMENT_META_DESCRIPTION"]=> string(180) "Трансплантация гемопоэтических клеток при аутоиммунных болезняхHematopoietic cell transplantation for autoimmune diseases" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(1911) "<p class="bodytext">Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут. </p> <h3>Ключевые слова</h3> <p>аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток</p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_META_TITLE"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_META_KEYWORDS"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_META_DESCRIPTION"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_PICTURE_FILE_ALT"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_PICTURE_FILE_TITLE"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_PICTURE_FILE_NAME"]=> string(74) "transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh-img" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(122) "Трансплантация гемопоэтических клеток при аутоиммунных болезнях" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(74) "transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh-img" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(74) "transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh-img" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(74) "transplantatsiya-gemopoeticheskikh-kletok-pri-autoimmunnykh-boleznyakh-img" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(2) "80" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> bool(false) ["VALUE"]=> bool(false) ["DESCRIPTION"]=> bool(false) ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> bool(false) ["~DESCRIPTION"]=> bool(false) ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19132" ["VALUE"]=> string(22) "06/14/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "06/14/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19133" ["VALUE"]=> string(22) "06/30/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "06/30/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19134" ["VALUE"]=> string(22) "12/08/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "12/08/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19135" ["VALUE"]=> string(4) "1440" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1440" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19149" } ["VALUE"]=> array(1) { [0]=> string(4) "1440" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1440" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19140" ["VALUE"]=> array(2) { ["TEXT"]=> string(42) "<p>Ричард А. Нэш</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(30) "Ричард А. Нэш
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19141" ["VALUE"]=> array(2) { ["TEXT"]=> string(1911) "<p class="bodytext">Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут. </p> <h3>Ключевые слова</h3> <p>аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1865) "Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут.
Ключевые слова
аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19137" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000082.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000082.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19144" ["VALUE"]=> array(2) { ["TEXT"]=> string(38) "<p>Richard A. Nash, MD</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(26) "Richard A. Nash, MD
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19145" ["VALUE"]=> array(2) { ["TEXT"]=> string(127) "<p>Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(115) "Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19146" ["VALUE"]=> array(2) { ["TEXT"]=> string(957) "<p class="bodytext">Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2]. </p> <h3>Keywords </h3><p>autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(911) "Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2].
Keywords
autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19138" ["VALUE"]=> string(58) "Hematopoietic cell transplantation for autoimmune diseases" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(58) "Hematopoietic cell transplantation for autoimmune diseases" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19142" ["VALUE"]=> string(3) "934" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "934" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19147" ["VALUE"]=> string(3) "935" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "935" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(12) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19144" ["VALUE"]=> array(2) { ["TEXT"]=> string(38) "<p>Richard A. Nash, MD</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(26) "Richard A. Nash, MD
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(26) "Richard A. Nash, MD
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19146" ["VALUE"]=> array(2) { ["TEXT"]=> string(957) "<p class="bodytext">Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2]. </p> <h3>Keywords </h3><p>autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(911) "Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2].
Keywords
autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(911) "Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2].
Keywords
autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19137" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000082.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000082.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2010-en-000082.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19138" ["VALUE"]=> string(58) "Hematopoietic cell transplantation for autoimmune diseases" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(58) "Hematopoietic cell transplantation for autoimmune diseases" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(58) "Hematopoietic cell transplantation for autoimmune diseases" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19145" ["VALUE"]=> array(2) { ["TEXT"]=> string(127) "<p>Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(115) "Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(115) "Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19149" } ["VALUE"]=> array(1) { [0]=> string(4) "1440" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1440" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(59) "Richard A. Nash" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19140" ["VALUE"]=> array(2) { ["TEXT"]=> string(42) "<p>Ричард А. Нэш</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(30) "Ричард А. Нэш
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(30) "Ричард А. Нэш
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19132" ["VALUE"]=> string(22) "06/14/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "06/14/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "06/14/2010 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19133" ["VALUE"]=> string(22) "06/30/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "06/30/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "06/30/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19134" ["VALUE"]=> string(22) "12/08/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "12/08/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "12/08/2010 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19135" ["VALUE"]=> string(4) "1440" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1440" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(59) "Richard A. Nash" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19141" ["VALUE"]=> array(2) { ["TEXT"]=> string(1911) "<p class="bodytext">Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут. </p> <h3>Ключевые слова</h3> <p>аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1865) "Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут.
Ключевые слова
аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1865) "Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут.
Ключевые слова
аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток
" } } } [6]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "80" ["~IBLOCK_SECTION_ID"]=> string(2) "80" ["ID"]=> string(4) "1439" ["~ID"]=> string(4) "1439" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["~NAME"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "10/18/2017 05:18:18 pm" ["~TIMESTAMP_X"]=> string(22) "10/18/2017 05:18:18 pm" ["DETAIL_PAGE_URL"]=> string(124) "/en/archive/tom-2-nomer-3-7/obzornye-stati/bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu/" ["~DETAIL_PAGE_URL"]=> string(124) "/en/archive/tom-2-nomer-3-7/obzornye-stati/bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(123322) "Introduction
Allogeneic hematopoietic stem cell transplantation has become one of the most frequent forms of transplantation, with currently more than 6000 transplants being performed annually. Its use is still increasing in the treatment of hematological and other malignancies. In addition there are a large number of patients with debilitating and life threatening hematological dis-eases, thalassemia, sickle cell anemia, and other non-malignant diseases that may benefit from transplantation. However, the major obstacle to the wider use of transplantation is graft-versus-host disease (GVHD); still a serious threat to these patients. However, at the same time graft-versus-host reactions directed at leukemia, lymphoma, myeloma, and other tumors of the host may be beneficial. Therefore it is necessary to understand GVHD in order to ex-ploit the potential advantages without incurring the risks. Allogeneic stem cell transplantation conveys tolerance toward organs of the donor. As a rule, immunosuppressive therapy can be discontinued after several months without the risk of rejection and GVHD. This tolerance with chimerism allows the transplantation of cells and organs of the same donor without life-long immune suppression. The success of immunotherapy with donor cells and of transplantation of solid organs from the stem cell donor depends on whether or not GVHD can be controlled.
Early observations
Mice protected from hematopoietic failure following total body irradiation by bone marrow transplantation succumbed to a “secondary disease” if the bone marrow was taken from a different strain [1]. This disease was related to an immune reaction of donor cells against the host rather than a delayed radiation syndrome: cells of diseased mice induced hepato-splenomegaly when transferred to non-irradiated newborn mice [2]. Further proof was the oc-currence of this secondary disease in F1-hybrid mice transplanted with parental marrow, but not in parental mice transplanted with F1-hybrid marrow [3]. Finally, organs containing more immunologically competent cells such as those from the spleen produced more secondary disease than bone marrow [4]. Eventually, the principle requirements for GVHD were defined by Billingham [5]: 1. the graft must contain immune reactive cells, 2. the recipient must be im-munogenetically different, and 3. the recipient cannot reject the graft. The first patients with acute GVHD were described by Mathé and colleagues [6]. A major step towards successful transplantation was the selection of marrow donors within the family according to major his-tocompatibility antigens (HLA) [7]. HLA had been previously detected in humans with pre-formed antibodies [8, 9]. Most preconditions for allogeneic transplantation in humans have been elaborated in animal experiments, particularly in dogs 10].
Therefore the principles for prevention of GVHD are 1. selection of a histocompatible donor, 2. adequate immune suppression for the patient before and after transplantation, and 3. ma-nipulation of the graft. In more recent years much has been learned about the regulation of the T cell response and mechanisms of tolerance, which may guide the way for immune suppression [11].
Animal models
The manifestation of GVHD in every species investigated so far involves skin, gut, and liver; primarily however hematopoietic tissue (Fig.1). Acute GVHD is a syndrome with similar fea-tures in mice, rats, monkeys, and humans; without prevention or treatment it can be rapidly fatal. Therefore pathophysiology, prevention, and treatment of acute GVHD can be studied in animal models. Chronic GVHD cannot be readily studied in animal models; it is not known why certain organs are involved and others are spared. Obviously hematopoietic cells are the primary targets, and the skin, gut, and liver may contain cells of hematopoietic origin such as dendritic cells and macrophages. These cells produce pro-inflammatory cytokines including interferon-gamma (IFN-g), tumor necrosis factor-alpha (TNF-a), interleukin 6 (IL-6), and others that stimulate donor T cells and induce expression of HLA class II antigens in host tissue (Fig.2). Dendritic cells activated by CD4 cells may stimulate CD8 cells to react against HLA class I presented peptides (Fig.3). Recent studies, however, showed that deficient production of IFN-g can increase GVHD in the skin, and failure of IFN-g induction of B7-H1 enhanced TH2 cells can produce idiopathic pneumonia [12]. TH2 cells and TH17 cells were guided to lungs and skin by the expression of chemokine receptors.
Figure 1. Host target tissues affected in the course of graft-versus-host disease

Figure 2. A proposed role of cytokine network and specific receptors of immune cells at initiation of GvHD (for details see text)

Figure 3. Dendritic cells boost CD8+ cells to react against host target tissues

GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. These antigens can be defined by the major histocompatibility complex, a highly polymorphic genetic region determining class I and class II antigens. Class I antigens are present in all cells of the organism, and class II normally only in hematopoietic cells. They may be expressed in other cells if these are affected by inflammation or injury. CD4-positive T cells exert GVH reactions against cells expressing class II antigens, and CD8-positive T cells act against class I antigens [13]. Differences in both antigen classes can induce severe and rapidly fatal GVHD. Polymorphic proteins not encoded by the major histo-compatibility complex may also cause severe GVH reactions. Peptides of these proteins can be presented by MHC class I and class II antigens. In general, MHC class I presents peptides of endogenous proteins of the cell, whereas class II antigens present peptides of exogenously acquired proteins [14, 15]. Here, minor histocompatibility (mHA) directed CD8 T cells require help from CD4 T cells for expansion and generation of memory T cells [16]. Therefore, reactions against mHA require a longer phase of immune recognition and activation than reactions against MHC antigens. Class II antigens are mainly expressed in hematopoietic progenitor cells, and in the case of injury and inflammation they may be expressed in non-hematopoietic cells as well. Reactions directed against class II antigens may induce severe marrow aplasia [17].
The mechanism of initiation of acute GVHD is not entirely clear; the preconditions are given before transplantation [18]. Much has been explained and published on cytokines and the cyto-kine storm liberated by intensive conditioning treatment, including high dose radiation and chemotherapy [19]. The role of cytokine release is confirmed by the suppression of acute GVHD using TNF-a antibodies [20]. There is some evidence that the systemic release of IFN-g leads to the secretion of chemokines in organs affected by GVHD and attracts activated T cells. In transgenic mice carrying the T cell receptor for ovalbumin the distribution of T cells was dependent on whether the antigen was given alone or together with lipopolysaccharide (LPS). Intravenous injection of antigens alone homes the T cells to secondary lymphoid tissue where they produce IL2, whereas injection of a combination of antigens and LPS homes the T cells to the lung, liver, gut, and skin where they produce IFN-g [21]. Systematically activated T cells produce interferons and induce chemokines in GVHD target organs [22]. However, the “danger signal” brought about by LPS may not be necessary, since in human patients donor lymphocyte transfusion may produce GVHD without conditioning treatment and infection [23].
The host's antigen presenting cells survive the conditioning treatment for various periods of time, with the most efficient cells being dendritic cells, but B cells, macrophages and other cells present antigens as well. Whereas dendritic cells in the blood of the host are rapidly re-placed by those of the donor, data on chimerism of dendritic cells in tissues are controversial [24]. Cytokine release by the host's activated dendritic cells and the graft's T cells is part of the initiation of GVH reactions (Fig. 2), and may be powerful enough to induce fatal GVHD even in the absence of histoincompatibility [25]. In general however, histocompatibility differences are necessary to induce and maintain GVH reactions. These histocompatibility differences may be of the major histocompatibility complex (MHC) class I or class II involving CD4- or CD8-positive T cells of the graft, and minor histocompatibility differences requiring profes-sional antigen presentation by dendritic cells of the host. GVHD occurring in the skin, liver, and gut requires dendritic cells expressing class I [26]. There is a possibility of cross presenta-tion of host antigens by donor dendritic cells, but their effects are inferior to direct presentation [27].
In contrast to cases involving the transplantation of solid organs, immunosuppressive therapy can be discontinued 3–6 months after transplantation in most patients receiving hematopoietic stem cell transplants, although patients who develop chronic GVHD may require therapy for several years. The host’s immune system is continuously suppressed by the graft, and the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion [28-30]. In DLA-identical canine chimeras tolerance could not be abrogated by the transfusion of donor lymphocytes unless the donors were immunized against the recipient [31]. Refractoriness to donor lymphocytes inducing GVHD develops at about two months after T cell depleted transplantation [32]. It may occur earlier in dogs transplanted with marrow depleted of T cells by CD6-antibody sparing NK cells [33]. NK cells can inactivate host dendritic cells and thereby prevent GVHD in mice [34]. Besides depletion of T cells and dendritic cells in the graft and the host, responder cells to antigen stimulation may respectively be eliminated by subsequent chemotherapy with methotrexate or cyclophosphamide. Cyclophosphamide can be given in rather high doses after transplantation without jeopardizing engraftment [35]. Modulation and suppression of GVH reactions has been shown for fractions of marrow cells such as mesenchymal stromal cells [36], NK-T cells (NKT1.1) [37], and regulatory T cells [11].
The results of animal models are highly informative with respect to the principles and me-chanisms of GVHD, but they also have their limitations. Apart from species-specific regulato-ry mechanisms of hematopoiesis and the immune system, animals are mostly young, have grown up in a protected environment, and are free of disease for which clinical transplantation is undertaken. In contrast, human patients are commonly older, have a history of infections and most likely a number of latent viral infections, and are possibly allo-immunized by previous transfusions and pregnancies, as are their donors. Moreover the primary disease and its treatment have a major impact on the transplant course.
The role of the immune repertoire of donor and host is still poorly defined. Female donors produce more GVHD and GVL in male recipients; most likely due to immunization during pregnancies by antigens derived from the fetuses' father [38]. Conversely, central memory T cells produce less GVHD than naïve T cells, indicating that the GVH reaction in most cases is a primary reaction [39]. Presumably central memory T cells cannot be involved in new primary reactions; there is also a risk that central memory T cells may produce vigorous GVHD when they recognize the antigen against which they developed. Alternatively they could be regulated by regulatory T cells.
Genetics
Selecting an HLA-identical sibling as donor was the major step towards successful stem cell transplantation. Selecting the donor within a family by typing for HLA-A, -B and DR-antigens is sufficient for successful transplantation, since antigen typing defines the haplotypes inhe-rited from the parents. Unlike identity by inheritance, selection of an unrelated donor relies on the most accurate typing of as many loci as possible. In general genetic definition of alleles of 10 HLA-loci is required to select a matched donor [40]. Severe GVHD can occur with any form of mismatch, but graft failure is less serious with mismatches for HLA-alleles than for the broader HLA-antigens [41]. In multiple mismatches the impact of various HLA-loci (A, B, C, DR) was similar, with the possible exception of HLA-DQ, which was less important. Notewor-thy is a possible racial difference in the role of HLA-C; in Japanese populations HLA-C has a lesser effect on GVHD than other HLA-loci [42]. In Caucasian populations HLA-C is as impor-tant for GVHD as other HLA-antigens [43]. The linkage disequilibrium, i.e. the occurrence of two antigens together, is more frequent than expected by the antigen frequency, is high for HLA-B and -C as well as for HLA-DRB1 and DQB1; therefore isolated mismatches are infre-quent. The linkage disequilibrium of HLA-DP with HLA-DRB1 is rather low, and differences of HLA-DP do not carry an additional risk for GVHD. They may, however, have an effect on the graft-versus-leukemia activity [44].
Presently little is known about permissible HLA-mismatches that allow for the development of tolerance. There may be racial differences as shown for HLA-C in Japanese as compared to Caucasian populations. In general HLA-mismatches are more permissible in patients with advanced disease than in patients with early disease. An allele mismatch may produce se-vere GVHD in a patient in chronic phase CML, but it may not have an effect in a patient with relapse of leukemia [43]. Cytokine levels and cytokine receptors are coded for by genes of the major histocompatibility complex. Sequence polymorphisms of genes for tumor necrosis fac-tor alpha (TNF-a), IL-6 and interferon-gamma (IFN-g) are different in persons with different racial backgrounds, i.e. Caucasians, Africans, and Cubans [45]. There have been several al-leles defined for both the TNF-a locus and the TNF-a receptor II locus that are associated with an increased risk of GVHD. Contrary to the pro-inflammatory cytokine TNF-a, IL-10 has anti-inflammatory effects. Polymorphisms of the promoter of IL-10 had an impact on GVHD. High levels of IL-10 correlated with a lower risk of GVHD.
Genetic factors outside of the HLA-complex may also be involved in the pathogenesis of GVHD. In the analysis of the gene expression profiles of donor cells, a particular role of transforming growth factor beta for chronic GVHD has been found [45]. In patients transplanted for chronic myelogenous leukemia [46] polymorphic alleles of TNF-receptor in the patient and certain alleles in IL10 and IL1 receptor in donor lymphocytes were associated with an in-creased risk of GVHD and decreased survival. A genetic factor associated with inflammatory bowel disease had an impact on GVHD (NOD/Card1) [47]. However, the effect could be dimi-nished if the gut was microbiologically well decontaminated. Antimicrobial prophylaxis de-creases the risk of GVHD without the GVL effect deteriorating.
There is good evidence that minor histocompatibility antigens play a role in GVHD and GVL reactivity [48, 49]. However, a recent analysis of the role of minor antigens in HLA-matched unrelated transplants by the NMDP did not find an impact of minor HA differences on the out-come of allogeneic stem cell transplantation [50].
Clinical features
Acute GVHD
GVHD was described and classified in the '70s [51, 52], when most patients were conditioned with total body irradiation. Skin is the organ most frequently affected; a maculopapular rash is common. This rash starts frequently in the upper thorax, arms, and face, but it can occur elsewhere and spread over the whole body. Features range from a maculopapular rash to general dermatitis with blisters and epidermal necrolysis. Histological findings are degenera-tion and apoptosis of the basal cells, dyskeratosis and lymphocytic infiltration. Involvement of the gastrointestinal tract is clinically characterized by diarrhea, malaise and vomitus; diarrhea may be severe with several liters of liquid and bloody stools. Histological findings are flatten-ing of the mucosa with debris in crypts (crypt abscesses); the most frequently affected part is the ileum. GVHD of the liver is characterized by jaundice and increases of liver enzymes. Histologically the Glisson triads are infiltrated, and the bile ducts are destroyed by infiltrating lymphocytes. Unfortunately none of the histological signs are diagnostic — viral infections and drug reactions may present similar features. Nevertheless biopsies may be indicated in order to exclude other diagnoses with characteristic signs and to obtain material for microbio-logical studies.
Despite prophylactic treatment with immunosuppressive drugs the prevalence of acute GVHD of all grades of severity is high, with a rate of 40–60% in patients with an HLA-identical sibling donor and 60–90% with a matched unrelated donor. Only at a severity of grade 2 and higher is additional immunosuppressive treatment required: this equates to 40–70% of patients. Another grading system was designed by the International Bone Marrow Transplant Registry IBMTR and validated in two studies [53, 54]. This grading system does not take into account the clinical performance as does the system of H. Glucksberg [51]. No advantage of one system over the other has been shown [54]. In both grading systems microangiopathy has not been scored as a form of acute GVHD; microangiopathy is characterized by red cell fragmentation, high levels of serum lactate dehydrogenase and thrombocytopenia. It is more frequent in patients treated with calcineurin inhibitors [18] or sirolimus, and resembles thrombotic thrombocytopenic purpura, but polymers of von Willebrand factor have not been found [55].
Table I. Acute GVHD. Diagnostic criteria according to H. Glucksberg
|
Stage |
Skin maculopapular rash |
Liver bilirubin |
Gut diarrhea |
|---|---|---|---|
|
+ |
< 25% body surface area |
2 - 3 mg/dl |
> 500 ml |
|
++ |
25 - 505 BSA |
3,1 - 6 mg/dl |
> 1000 ml |
|
+++ |
Generalized erythroderma |
6,1 - 15 mg/dl |
> 1500 ml |
|
++++ |
General erythroderma with bulla formation and desquamation |
> 15 mg/dl |
Severe abdominal pain w/wo ileus |
|
Cell Ther Transplant. 2012;2:e.000089.01. doi:10.3205/ctt-2012-en-000089.01-table1 |
|||
Table II. Acute GVHD. Diagnostic criteria according to H. Glucksberg
|
Grade of aGVHD |
Skin |
Liver: |
Gut: |
Clinical performance |
|---|---|---|---|---|
|
I |
+ - ++ |
bilirubin < 2,0 mg/dl |
No diarrhea |
Ok |
|
II |
+ - +++ |
3,1 - 6 mg/dl |
Diarrhea > 500 ml |
Mild decrease |
|
III |
++ - +++ |
6,1 - 15 mg/dl |
> 1000 ml |
Marked decrease |
|
IV |
++ - ++++ |
> 6,1 mg/dl |
> 1000 ml |
Severe decrease |
|
Cell Ther Transplant. 2012;2:e.000089.01. doi:10.3205/ctt-2012-en-000089.01-table2 |
||||
Chronic GVHD
Acute GVHD may resolve completely with immunosuppressive treatment or it may lead to chronic GVHD. Chronic GVHD may also develop de novo without prior acute GVHD within a year from transplantation. Chronic GVHD involves most frequently the skin with lichenoid and sclerotic changes, the nails with dystrophy, the eyes with keratoconjunctivitis, the mouth with dryness and paradontosis, the vagina with dryness and sclerosis, liver and lungs. The clinical features of chronic GVHD resemble autoimmune diseases like lupus erythematodes, Sjögren syndrome, and biliary cirrhosis in many aspects. Characteristically there is hypogammaglo-bulinemia with loss of IgA, and lymphopenia, but there may also be hypergammaglobulinemia and eosinophilia. Thrombocytopenia is a sign of poor prognosis; another factor of poor prognosis is involvement of the lungs, which may be in the form of late interstitial pneumonitis and fibrosis or obliterating bronchiolitis. As a rule lung involvement is progressive and carries the risk of severe infections. The skeletal system may be involved in form of fasciitis, muscle dystrophy, tendinitis, and contractures. Transplant vasculopathy is a problem of solid organ transplants: in stem cell transplanted patients vasculitic changes in the CNS have been observed and vascular events can be seen in young patients [56] without other risk factors.
Overlapping GVHD
Besides the clinical features, acute and chronic GVHD have been defined by the time of oc-currence: acute GVHD in the first weeks and months, and chronic GVHD after day 100. This definition has been challenged by the introduction of cyclosporine A for immune suppression and conditioning with reduced intensity. Following discontinuation of cyclosporine A, a flare of acute GVHD may occur, and following reduced intensity conditioning, acute GVHD may occur late. Similarly, late onset of acute GVHD has been observed after prophylactic treat-ment with TNF-antibody during conditioning [20]. Obviously the activation of T cells is delayed by reduced intensity conditioning and prophylactic treatment, with TNF-antibodies leading to late acute GVHD.
Prophylaxis of GVHD
Some form of prophylaxis of GVHD is absolutely necessary even in HLA-identical sibling transplants, as hyperacute GVHD was seen in every patient with engraftment [57]. T cells are responsible for GVHD and depletion of T cells from the transplant was very successful in an-imal models [58, 59]. In the clinical setting GVHD could be prevented or suppressed [60, 61] effec-tively. Antithymocyte globulin (ATG) has a broad specificity, recognizing not only T cells, but other mononuclear cells as well. The monoclonal antibody alemtuzumab recognizes CD52, an antigen that is present in many leukocytes including lymphocytes, monocytes, and den-dritic cells; alemtuzumab has broad activities despite its specificity. In humans [62] as in dogs [63] the number of clonable T cells should be below 105/ kg body weight for effective prevention of GVHD. So far more selective depletion of T cells has not improved the overall results of transplantation [64], and depletion of CD8 has been insufficient in preventing GVHD [65]. CD6 has the advantage of sparing most of the NK cells in the transplant [64]. In dogs CD6-depleted marrow suppresses alloresponses [66] and recipients of CD6-depleted marrow tolerate donor lymphocyte transfusions earlier than recipients of marrow treated with absorbed ATG [33].
However, the advantage of ex vivo T cell depletion was offset by a high rate of graft rejection, relapse, infections, and EBV-associated post transplant lymphoproliferative disease (PTLD) [67, 68]. Treatment of the patient prior to transplantation with ATG prevents rejection; T cell anti-bodies persist in the patient for 4–5 weeks and deplete T cells of the graft in vivo. A rando-mized study comparing standard post-grafting immune suppressive treatment with and with-out ATG prior to transplantation showed lower rates of acute and chronic GVHD in the group treated with ATG [69]. A beneficial effect of ATG in the conditioning treatment for chronic GVHD has also been observed in Italian studies [70] and in retrospective analyses of non-randomized studies (own unpublished observations).
Alemtuzumab also persists in the patient for a prolonged period of time, and reconstitution of T cells is delayed for 6–9 months [71]. Severity of GVHD is low in patients treated with alemtu-zumab, but graft failures have been observed [72]. There is also an increased risk of viral infec-tions, particularly cytomegalovirus, and insufficient response of the malignant disease. These deficiencies can be compensated at least partially by the transfusion of donor lymphocytes [73].
In the last decade G-CSF mobilized peripheral blood stem cells (PBSC) have replaced mar-row in most instances. PBSC contain enormous amounts of T cells and depletion of T cells has been largely unsuccessful. Surprisingly, transplantation of PBSC is not associated with an increased risk of acute GVHD, but is instead associated with a more rapid engraftment and an increased risk of chronic GVHD [74]. PBSC may be preferable for patients with advanced disease and elderly patients. Conversely, T cell depletion and marrow transplantation may be the preferred treatment for patients with early disease, non-malignant disease, and patients who are younger.
Other approaches to prevent GVHD use specific conditioning regimens [37] or specific cells to induce transplantation tolerance. Low dose total lymphoid irradiation in combination with ATG may spare natural killer T cells in the marrow and regulatory T cells suppressing GVHD, but allow graft-versus-leukemia/lymphoma effects. The addition of regulatory T cells to the graft has suppressed GVHD without inhibiting GVL effects in mice [75] and recently in humans (Martelli F, Plenary session ASH 2009). Another immunosuppressive cell product are me-senchymal stromal cells, which have been successful in the treatment of severe GVHD [76]. Co-transplantation of mesenchymal stromal cells prevented rejection in HLA-haploidentical transplants [77] and GVHD was less severe, but the difference did not reach significance be-cause of low numbers. We have used CD6-depleted PBSC transfused 6 days after trans-plantation of unmodified marrow from HLA-haploidentical donors with a low rate of acute GVHD [78].
Post-graft immunosuppressive treatment with either methotrexate or cyclophosphamide has been used since the early days of stem cell transplantation. Both agents preferably kill proli-ferating cells and should be started early after grafting. These drugs suppress donor cells proliferating in response to host antigens as well as residual host cells responding to the graft. They sustain engraftment and suppress GVHD at the same time. They induce transplantation tolerance by killing the responsive cells, and therefore patients with incomplete responses usually take a disastrous course. A recent application of this principle is the use of large doses of cyclophosphamide 3 and 4 days after HLA-haploidentical transplantation [35, 79].
The introduction of the calcineurin inhibitors cyclosporine A and tacrolimus has also changed the outlook for these patients. Both drugs inhibit the activation and proliferation of T cells by inhibiting dephosphorylation and translocation of the nuclear factor of activated T cells (NFAT). The continuous inhibition is effective in suppressing GVHD and rejection, but the effect is not necessarily maintained after discontinuation of treatment; calcineurin inhibitors are less potent in the induction of transplantation tolerance [80]. Treatment should be started prior to transplantation in order to avoid antigen recognition and T cell activation. Tacrolimus is a somewhat stronger immunosuppressive than cyclosporine A and possibly less neurotoxic. However, in controlled studies comparing tacrolimus and cyclosporine A less severe GVHD was not associated with improved survival [81].
The combination of cyclosporine A and methotrexate is better than either drug alone [82]. It has become the gold standard of GVHD prophylaxis. In recent years mycophenolate mofetil (MMF) has been introduced to replace methotrexate [83]. MMF inhibits the purine synthesis and the de novo pathway of guanosine nucleotide synthesis; it kills not only proliferating T cells, but also T cells in the interphase. MMF produces less mucositis and less marrow toxicity than methotrexate. However the best regimen and timing (2–3 times per day) remains unknown.
Sirolimus binds to the tacrolimus binding protein FKBP12 and forms a complex with mTOR (target of rapamycin) that inhibits several signal transduction pathways including PTEN, PI3kinase and AKT as well as the JANUS kinase pathway. Thereby it produces several ef-fects including immunosuppression of T cells, anti-angiogenesis and inhibition of tumor growth [84]. Its immunosuppressive activity is presumably linked to the suppression of the second signal of T cell activation. This way T cell apoptosis and specific peripheral non-responsiveness may be induced [85]. Th1 cells and their cytokines are more affected by siroli-mus than Th2 cells and regulatory T cells [86, 87]. The sirolimus/mTOR complex inhibits the ac-tivation signals of CD28 and CD40L stimulation and thereby the second signal essential for T cell activation [88], a situation that may lead to transplantation tolerance. The combination of sirolimus and tacrolimus is synergistic and has shown little toxicity [89], but veno-occlusive dis-ease of the liver and thrombotic microangiopathy have been observed [90]. The combination of sirolimus and MMF was promising in a smaller group of patients, where VOD and TMA were not observed [91].
The goal of preventing GVHD is the induction of tolerance in both directions, the host-versus-graft and graft-versus-host direction. Contrary to transplantation of solid organs, stem cell transplantation induces self-sustained tolerance without life-long immunosuppressive therapy. As a rule, a period of 4–6 months of immunosuppressive therapy is sufficient for tolerance to become established. In clinical terms tolerance is evident by persistent chimerism without GVHD and without severe infections more than 30 days after discontinuation of immunosuppression.
Treatment
Glucocorticoids
Despite prophylactic treatment with immunosuppressive agents, acute GVHD requiring addi-tional treatment occurs in 40–80% of patients within 3–4 weeks of transplantation [92]. Corti-costeroid therapy is the standard of treatment for acute GVHD, but the regimen and the do-sage is still under discussion. Originally, treatment with large doses was favored [93], but there are no controlled studies to support this treatment. Similarly, in organ transplantation, rejection crises are treated with bolus methylprednisolone without prospective randomized trials supporting this. Despite this general use there are only a few studies on the schedule and the dosage rates. A randomized Italian trial comparing 2mg/kg per day with 10mg/kg per day showed no advantage for the higher dose [94], however 50% of patients were switched to a high dose because of insufficient response. Recently, a retrospective study from Seattle indi-cated that even lower doses of corticosteroids (1mg/kg instead of the standard 2 mg/kg) can be given without disadvantage [95]. However the patients of the low dose group had more fa-vorable risk factors and less severe GVHD; in addition oral non-absorbable corticosteroids were given more frequently.
The mechanisms of the actions of glucocorticoids are still not fully understood, lymphopenia is mainly due to sequestration of lymphocytes, and less to lympholysis. However, glucocorti-coids exhibit strong anti-inflammatory effects in several ways including genomic and non-genomic pathways [96]. Glucocorticoids are bound to a receptor from which heat shock protein 70 is released. The glucocorticoid complex activates anti-inflammatory proteins directly and their production genomically. Inhibition of nuclear factor kB is highly sensitive to glucocortico-ids preventing the production of inflammatory proteins. Sensitivity to the treatment with glu-cocorticoids may be determined by the relative levels of glucocorticoid receptor α and ß. This may explain interpatient variation of sensitivity [97]; memory T cells [98] as well as mature den-dritic cells are less sensitive to glucocorticoids. In macrophages low doses of glucocorticoids stimulate the production of proinflammatory cytokines, whereas high doses suppress it [99]. High dose glucocorticoid therapy given for few days has shown little immune suppression in vivo [100].
Commonly treatment is started in patients with clinical grade II–IV severity of GVHD. About 40–50% of patients respond with resolution or improvement of clinical symptoms [92]. The re-mainder are classified as “steroid-refractory”. The time until refractoriness to glucocorticoids is stated may vary from 5 to 14 days [101]. Many centers increase the dose of steroids in re-fractory patients prior to the addition of other agents. We prefer to start with rather high doses of glucocorticoids (1–2mg/kg every 8 hours) and score the response after three days of treatment for refractoriness. This way we initiate secondary treatment early in refractory pa-tients. The decision to start the treatment is made by two physicians. In the case of a pro-gressive and characteristic skin rash the diagnosis is not difficult, but in cases of isolated ga-strointestinal GVHD with diarrhea and nausea or isolated hepatic GVHD the diagnosis may be more difficult. Persistent toxicity of the conditioning treatment, veno-occlusive disease of the liver, drug-induced changes and viral infections are considered as differential diagnosis. In our centre skin biopsies are regularly performed, biopsies of gut and liver are only made in patients that do not respond to the treatment. This way we obtain not only histological con-firmation of the clinical suspicion, but also information about viral infection. Concomitant vi-rostatic treatment is given to patients with biopsies positive for viral infection as well as those that are seropositive for cytomegalovirus. Another option is the use of high doses of iv immu-noglobulins that may inhibit the deleterious effects of FAS by their blockade of FAS-L [102]. Al-though their immune modulating effects are far from understood [103], 20–30% of patients with skin GVHD do respond to the treatment with iv immunoglobulins. In any case early treatment is important as delay of the start of treatment until the results of laboratory investigations are available may jeopardize the response to glucocorticoids.
The effect of systemic glucocorticoids on gastrointestinal GVHD can be improved by local treatment with beclomethasone [104] and budesonide [105].
Antibodies
In many instances the first choice in patients with steroid refractory GVHD has been immu-nosuppressive antibodies. Antithymocyte globulin (ATG) has been used in several uncon-trolled studies with some success [106], but in controlled studies a beneficial effect could not be demonstrated [107]. Similarly, OKT3 is a monoclonal antibody against CD3 on T cells: it dep-letes T cells and stimulates proliferation by its mitogenic activity. Even though many patients have responded to the treatment with OKT3 with complete remission of GVHD, better surviv-al could not be demonstrated in controlled clinical trials [108]. Alemtuzumab has been used mainly for prophylaxis of acute GVHD by treating the patient in vivo or the graft prior to transplantation ex vivo: recently beneficial outcomes of treatment of established GVHD have been reported in two uncontrolled studies [109, 110]. Viral infections may complicate treatment with alemtuzumab; therefore regular control and pre-emptive treatment is necessary. ATG and OKT3 both stimulate proliferation of lymphocytes that are not killed by cytolysis; there-fore the combination of antibody treatment with chemotherapy (methotrexate, Cyclophos-phamide, mycophenolate mofetil, etc.) may be beneficial. A humanized CD3-antibody (visili-zumab) produced good first results [111] which unfortunately were not confirmed in multicenter trials [112]. In those patients the reactivation of EBV and the incidence of post transplant lym-phoproliferative disease (PTLD) increased.
Encouraging results were also reported with ABXCBL, an antibody against CD147 that is ex-pressed in activated T cells [113]. However in a comparative study ABXCBL was not better than ATG, where survival was even inferior [114].
Antibodies against tumor necrosis factor α (TNF-a) and soluble receptors of TNF-a (etaner-cept) have been studied in the prophylaxis of GVHD [20] and the treatment of steroid refractory GVHD [115]. There has been a high rate of complete response to infliximab even in gastrointes-tinal GVHD, but this is complicated by an increased risk of fungal infections [116, 117]. Contrary to infliximab etanercept neutralizes soluble TNF-a without affecting TNF-a in phagocytic cells. Etanercept is associated with a lower risk of fungal infections. The combination of etanercept with an anti-IL2-receptor antibody showed high response rates to acute GVHD, but the long-term survival was rather poor [118]. In comparison, a pilot trial of etanercept in combination with tacrolimus and steroids gave a 75% complete response and a 50% survival rate [119]. When comparing etanercept combined with steroids to steroids alone a significantly better response to the combination was observed [120]. The combination of etanercept with ATG and tacrolimus was compared to ATG and tacrolimus alone [121]; considering the limited number of patients the response and the survival of patients given etanercept was better. Neutralization of TNF-a released by the ATG treatment by etanercept may have been contributing to the better outcome.
Antibodies against IL-2 receptor have been studied early [122] with some transient success. The importance of an early treatment start was stressed. Several studies with humanized anti-IL2-receptor antibodies were encouraging [123, 124], but a randomized study was stopped prematurely because of inferior survival of the antibody (daclizumab) group [125]. There is little doubt that the IL2- receptor antibody is effective in suppressing GVHD of the skin and the gut when started early, but it may have an adverse effect on the generation of regulatory T cells expressing high levels of the IL-2 receptor.
Alefacept is a fusion protein of the CD2-binding domain of LFA-3 and the Fc portion of IgG with specific activities against memory T cells [126]. Promising results in steroid refractory acute GVHD and in chronic GVHD have been reported, but there may be an increased risk of viral and fungal infections [127].
Recently, the role of B cells has been discussed more frequently, although the role of T cells in GVHD is not disputed. However, cytotoxic antibodies may be produced in HLA-mismatched chimeras, and depletion of B cells may prevent EBV-induced B cell lymphoma. Single patients have been reported to show a response to steroid refractory GVHD to the treatment with rituximab [128].
Drugs
As a rule the treatment given for prophylaxis is continued during the treatment of established GVHD, and includes glucocorticoids at a low level. Depending on the prophylactic regimen, cyclosporine A may be substituted by tacrolimus and new drugs may be added. In most Eu-ropean centers a calcineurin inhibitor is combined with methotrexate or mycophenolate mofe-til. In patients not treated prophylactically a trial with mycophenolate mofetil may be justified; a response rate of 47–48% has been reported in steroid refractory GVHD, but the survival at 6 and 12 months was not improved [129]. Methotrexate on a weekly basis in low doses has been helpful in single cases. Mucositis and myelosuppression are limiting factors.
Similarly, sirolimus can be used for patients not treated prophylactically, as response rates of 77% overall and 44–72% complete response have been reported [130, 131]. Again microangiopa-thy has been a problem, but could be controlled by discontinuation of the calcineurin inhibitor (CNH) or both sirolimus and CNH. A small study suggests a good response of acute GVHD to sirolimus without prior treatment with glucocorticoids [132]. Due to its anti-tumor activity siro-limus is preferred to calcineurin inhibitors and glucocorticoids by many investigators [133], par-ticularly in patients with lymphoma [134].
Pentostatin is an inhibitor of the salvage pathway of thymidine kinase that is specific for T cells. Phase I studies have shown efficacy in the treatment of steroid-refractory GVHD [135]. A retrospective analysis has shown activity comparable to other immunosuppressive regimens [136]. However, pentostatin has shown activity in the treatment of chronic GVHD [137, 138]. Pentostatin may have better effects in patients with chronic GVHD.
Thalidomide [139, 140] and more recently lenalidomide [141] have been studied in the treatment of GVHD. The initially positive results of treatment with thalidomide in chronic GVHD [139] were not confirmed in a randomized study [140]. The treatment of recurrent myeloma with lenalido-mide suggested an immune modulatory effect of lenalidomide in producing regulatory T cells [141].
Bortezomib has been tested in mice [142] and patients with HLA-mismatched unrelated donors [143]. The immunomodulatory effect has been related to the suppression of monocyte-derived dendritic cells and modified antigen presentation and release of TNF-a from CD4-positive T cells [142]. It has shown promising activity in the prophylaxis of GVHD [143].
After the description of activating antibodies against the receptor of platelet derived growth factor (PDGF) [144] in patients with systemic sclerosis similar antibodies were found in patients with sclerodermatous chronic GVHD [145] and several groups have treated sclerodermatous chronic GVHD [146, 147], as well as obliterating bronchiolitis with imatinib [148, 145]. In one study more than 70% of patients with sclerotic chronic GVHD responded with partial and complete remissions [147].
Cells
Many treatment regimens of GVHD favor the development of regulatory T cells characterized by the expression of CD 4 and CD25 in high density [149]. The suppressive activity is limited to cells of the CD4/CD25 immune phenotype that are positive for FoxP3 mRNA. Typically regulatory T cells should be negative for the IL7 receptor (CD127). Immunomagnetically selected regulatory T cells have been tested in vitro for immunosuppressive effects [149, 150], and preliminary applications for the treatment of refractory GVHD have been promising (M. Edinger, pers. comm.). The first results of preventive application have been reported (Di Ianni et al. ASH 2009); 17 of 20 evaluable patients did not produce GVHD after HLA-haploidentical stem cell transplantation despite admixture of a limited amount of conventional T cells to the CD34-selected graft.
More information is available on the treatment of refractory GVHD with mesenchymal stromal cells [76]. The results were confirmed in a multicenter study of the EBMT involving [151] 55 patients with steroid-refractory GVHD. Twenty-seven patients received one dose, 22 two doses and 6 three doses and more from HLA-mismatched or HLA-matched donors for treatment; 30 patients had a complete response, and an improvement was seen in 9 patients. Responders had a better chance of survival than non-responders. Mesenchymal stem cells have multiple properties including differentiation into bone, cartilage, tendon and muscle cells, repair of damaged tissue and modulation of immune responses [36].
UV light
Ultraviolet light has immunosuppressive properties [152]. UV-A in combination with 8-methoxypsoralen (PUVA) has been used to treat chronic GVHD [153]. UVA may be applied to the skin in combination with oral psoralen or with a bath in psoralen containing water. PUVA treatment was studied in 103 patients with steroid-resistant acute GVHD [154] with good res-ponses in GVHD of the skin and sparing of glucocorticoid doses. The treatment was well to-lerated, but it may induce a flare before lichenoid skin changes respond to the treatment. In chronic GVHD 31 of 40 patients had an improvement following PUVA treatment, but partial and complete responses were limited to the skin [155]. Best responses were seen in the liche-noid phases of chronic GVHD, and less in the sclerodermatous phases. However, the com-bination of PUVA bath with oral isotretinoin has been effective in a small study of scleroder-matous chronic GVHD: 11 of 14 patients responded, four of these with complete remission [156].
Alternatively PUVA may be applied directly to the blood resp. leukocytes separated by a dis-continuous blood cell separator (extracorporeal photopheresis, ECP). Responses to ECP have been reported for steroid-refractory, acute GVHD [157-159] and chronic GVHD [160]. Complete resolution of acute GVHD of the skin in 82%, liver in 61% and gut in 61% of pa-tients has been reported [158]. Response was associated with better survival. In our own study of 30 patients with acute GVHD, 20 patients responded with CR and PR defined as steroid discontinuation and reduction to 10 mg or less per day respectively (unpublished). Eleven of 20 responders survived as compared to only one non-responder. Steroid treatment was a major risk factor in the treatment of acute GVHD of pediatric patients [161]. In a single centre study on steroid refractory chronic GVHD 22% of patients could discontinue steroid therapy after one year, with response to ECP and absence of thrombocytopenia being the favorable factors for survival [160]. A randomized prospective multicentre study [162] comparing standard treatment with standard treatment plus ECP showed improvement of the skin score and sig-nificant steroid sparing. ECP is a good treatment option in patients with steroid-refractory acute and chronic GVHD with little side effects. The mechanism of the immunosuppression by ECP is not completely understood as only 5–10% of all T cells may be reached by extra-corporeal irradiation. However, a shift of dendritic cells from activating DC1 to down-regulating DC2 and from Th1 to Th2 has been described in the course of ECP [163]. Ex vivo a decrease of T cells producing pro-inflammatory cytokines was described [164]. In a murine model ECP-treated T cells induced regulatory T cells in recipients with established GVHD [165]. An increase in the proportion of regulatory T cells was observed in patients that responded to ECP [166]. Therefore ECP may be one method to induce GVH-tolerance without too many side effects.
Induction of graft-versus-host tolerance
Unlike transplantation of solid organs, transplantation of hematopoietic stem cells induces transplantation tolerance, enabling immunosuppressive therapy to be discontinued. In the form of central tolerance, lymphoid progenitor cells derived from transplanted stem cells tra-vel to the thymus where T cells tolerant to the host’s tissue are produced [167-169]. However, the thymus shows progressive involution in adulthood; central tolerance may be the major form of tolerance in children and young adults. The majority of patients subjected to stem cell transplantation are older, and the thymus has shrunk to a small remnant. Therefore in the majority of our patients a peripheral form of tolerance prevails, but function of the thymus can be recovered even in elderly individuals [170]. Several studies have been performed to speed up recovery of the thymus, mostly without convincing success [171], but new agents may give better results [172, 173, 169]. However, GVHD may affect the thymus [174] and thereby may inhibit the induction of central tolerance in both young and adult patients. Peripheral tolerance is a first step and may be replaced by central tolerance with time. The mechanisms of tolerance may be similar, clonal deletion, clonal anergy, and suppression.
Clonal deletion is a mechanism of self tolerance occurring in the thymus [175]; in the case of allogeneic stem cell transplantation T cells of donor origin derived from lymphoid progenitors may be eliminated by the same mechanism and primed towards host MHC antigens in se-miallogeneic hosts [176]. Deletion in the periphery may be accomplished by the treatment with antimetabolite drugs such as methotrexate, or cycle active drugs like cyclophosphamide; both of which have been shown to induce tolerance in stem cell transplanted patients [177, 178]. The principle of selective depletion of responsive lymphocytes has been applied more recently in HLA-haploidentical transplantation [179]. Unlike these cytotoxic agents calcineurin inhibitors do not kill the responsive cells, but inhibit cytokine production and thereby the progress of the immune response. However they may not favor the induction of tolerance; flares of GVHD have been observed after discontinuation of cyclosporin A, and late rejection of marrow grafts have been reported in single patients with aplastic anemia. Activation induced cell death (AICD) is a natural decrease of the clone size by IFN-g secretion of mature Th1 T cells and death of immature T cells, which may be achieved by the external pathway.
Clonal anergy may be the result of competitive inhibition by anergic T cells or active sup-pression by a variety of suppressor cells. Formerly, CD8-positive T cells were considered “cytotoxic/suppressor” cells, but the evidence for specific suppression was weak. Instead, several mechanisms of suppression have been described including “veto” cells suppressing the immune reaction against themselves [180]. The veto mechanism, described as the effector cells inhibiting or killing themselves has been primarily ascribed to CD8-positive T cells, but later also to other cells including stem cells. CD8-positive suppressor cells may not only func-tion as veto cells, but they may also suppress third party reactions by the secretion of FAS [181>]. Other cells with suppressor function are myeloid derived suppressor cells [182], NKT cells in the marrow [183], NK cells [184], dendritic cells type 2 [185] and mesenchymal stromal cells [76]; all of them suppress activated T cells more or less specifically. Some of these have already shown clinical effectiveness [183, 76], others are still in a developmental state. In recent years the detection of FoxP3 (forkhead transcription factors) showed suppressive function of CD4, CD25 positive T cells and even CD8 T cells [186]. Naïve CD4, CD25-positive regulatory T cells are able to down regulate allogeneic immune responses without inhibiting graft-versus-leukemia responses [75]. These may be naïve and non-specifically down regulating dendritic cells or adaptive and directed against specific antigen. Recently the Perugia group has reported the use of naïve regulatory T cells suppressing GVHD in patients given HLA-haploidentical transplants including small amounts of conventional T cells (ASH 2009, New Orleans).
Rapamycin exerts differential effects on T cells, inhibiting CD8 positive cells more than CD4 positive cells [86]; CD4 T cells spared by Rapamycin may become regulatory T cells without compromising GVL reactions [133]. Long-term observations of patients treated with Rapamycin and tacrolimus are encouraging with regard to control of acute GVHD and GVL [89]. Chronic GVHD still remains a problem despite tolerogenic effects of Rapamycin. Recently, the Milan group [187] (EBMT 2010) has reported generation of regulatory T cells in patients with HLA-haploidentical transplants. After conditioning with treosulfan, fludarabine, ATG and rituximab, and GVH prophylaxis with Rapamycin and mycophenolate mofetil, immune reconstitution was better than after transplantation of CD34-selected transplants, and regulatory T cells were detected early after transplantation.
Tolerogenic effects have also been described for the treatment with extracorporeal photo-pheresis (ECP) [188]. In acute GVHD ECP was applied with good results [158]. In most patients the effects of ECP are not immediate, but occur after some weeks. ECP has also beneficial effects against chronic GVHD [162] and may be preferable to other treatments for GVHD.
The main goal of prophylactic and therapeutic treatment of GVHD should be the induction of transplantation tolerance. Therefore treatment protocols interfering with tolerance should be avoided in protracted periods in favor of regimens allowing the development of tolerance. Glucocorticoids and calcineurin inhibitors are effective in controlling the acute disease, but they do not support the development of tolerance. Similarly, IL2-R antibodies may be effec-tive in the acute control of GVHD, but may not support the development of tolerance. Toler-ance may be achieved by depletion of mature T cells from the graft, killing of antigen respon-sive T cells with cell cycle active chemotherapy as Cyclophosphamide, methotrexate, or my-cophenolate mofetil, activating CTLA4 receptors by CTLA4-Ig or using drugs like Rapamycin that block the co-stimulatory pathway or ECP producing apoptotic cells that induce tolerance.
Future prospects
The time point to initiate treatment of acute and chronic GVHD is of paramount importance. Therefore, early diagnosis tests, before clinical diagnosis is possible, may improve the out-come significantly. Several proteins have been found in the urine of patients that developed GVHD [189]; a prospective study will help to demonstrate the value of early treatment. Similarly, elafin has been identified as a prognostic marker in the plasma of patients developing skin GVHD [190]. Early diagnosis will allow early treatment and thereby avoid the development of memory T cells or T stem cells with memory that are extremely difficult to suppress.
References
1. Barnes DHW, Loutit JF. Spleen protection: the cellular hypothesis. In: Bacq ZM and Alexander P: Radiobiology Symposium : Proceedings of the Symposium held at Liege, August-September, 1954. London: Butterworths, 1955:134-135.
2. Simonsen M, Jensen E. The graft-versus-host assay in transplantation chimeras. In: Albert F, Lejeune-Ledant G, eds. Biological problems of grafting. Oxford: Blackwell; 1959:214-236.
3. Uphoff, D. E. and Law, P. Genetic factors influencing irradiation protection by bone marrow. II. The histocompatibility 2 (H-2) locus. J Natl Cancer Inst 20, 617-624. 1958. pmid: 13539612.
4. van Bekkum, D. W. The selective elimination of immunologically competent cells from bone marrow and lymphatic cell mixtures. I.Effect of storage at 4°C. Transplantation 2, 393-404. 1964.
5. Billingham, RE. The biology of graft-versus-host reactions. Harvey Lect 1966-1967 62, 21-78. 1967. pmid: 4875305.
6. Mathé G, Amiel JL, Schwartzenberg L, et al. Successful allogeneic bone marrow transplantation in man: Chimerism, induced specific tolerance and possible antileukemic effects. Blood 1965;25:179-96. pmid: 14267694.
7. Epstein RB, Storb R, Ragde H, Thomas ED. Cytotoxic typing antisera for marrow grafting in littermate dogs. Transplantation 1968;6:45-58. pmid: 4866738.
8. Dausset J, Rapaport FT, Colombani J, Feingold N. A leucocyte group and its relationship to tissue histocompatibility in man. Transplantation 1965;3:701-705. pmid: 5324831.
9. van Rood JJ, van Leeuwen A, Eernisse JG, Frederiks E and Bosch LJ. Relationship of Leukocyte groups to tissue transplantation compatibility. Ann.N.Y.Acad.Sci. 1964;120:285-298.
10. Thomas ED, Storb R, Epstein RB, Rudolph RH. Symposium on bone marrow transplantation: experimental aspects in canines. Transplant.Proc. 1969;1:31-33. pmid: 5002661.
13. Korngold R, Sprent J. Surface markers of T cells causing lethal graft-vs-host disease to class I vs class II H-2 differences. J Immunol. 1985;135:3004-3010. pmid: 3876371.
14. Klein J, Sato A. The HLA system. First of two parts. N Engl J Med. 2000 Sep 7;343(10):702-9 .doi: 10.1056/NEJM200009073431006.
15. Klein J, Sato A. The HLA system. Second of two parts. N Engl J Med. 2000 Sep 14;343(11):782-6. Review. Erratum in: N Engl J Med 2000 Nov 16;343(20):1504. doi: 10.1056/NEJM200009143431106.
19. Ferrara JLM, Deeg HJ. Graft-versus-host disease. N Engl J Med 1991;324:667-674. doi: 10.1056/NEJM199103073241005.
21. Reinhardt, RL, Khoruts A, Merica R, Zell T, and Jenkins MK. Visualizing the generation of memory CD4 T cells in the whole body. Nature 410, 101-105. 2001. doi: 10.1038/35065111.
23. Kolb HJ, Mittermueller J, Holler E, et al. Treatment of recurrent chronic myelogenous leukemia posttransplant with interferone alpha (INFa) and donor leukocyte transfusions [abstract]. Blut. 1990;61:122.
24. Hessel H, Mittermuller J, Zitzelsberger H, Weier HU, Bauchinger M. Combined immunophenotyping and FISH with sex chromosome-specific DNA probes for the detection of Langerhans cells after sex-mismatched bone marrow transplantation. Histochem Cell Biol. 1996;106:481-485. pmid: 8950606.
25. Teshima T, Ordemann R, Reddy P, et al. Acute graft-versus-host disease does not require alloantigen expression on host epithelium. Nat Med. 2002;8:575-581. doi: 10.1038/nm0602-575.
26. Shlomchik WD, Couzens MS, Tang CB, et al. Prevention of graft versus host disease by inactivation of host antigen-presenting cells. Science 1999;285:412-415. pmid: 10411505. PDF: Free with Registration at http://www.sciencemag.org/content/285/5426/412.long
27. Matte CC, Liu J, Cormier J, et al. Donor APCs are required for maximal GVHD but not for GVL. Nat.Med. 2004;10:987-992. doi: 10.1038/nm1089.
28. Tutschka PJ, Hess AD, Beschorner WE, Santos GW. Suppressor cells in transplantation tolerance. I. Suppressor cells in the mechanism of tolerance in radiation chimeras. Transplantation 1981;32:203-209. pmid: 6456580.
29. Tutschka PJ, Ki PF, Beschorner WE, Hess AD, Santos GW. Suppressor cells in transplantation tolerance. II. maturation of suppressor cells in the bone marrow chimera. Transplantation 1981;32:321-325. pmid: 6460354.
30. Tutschka PJ, Hess AD, Beschorner WE, Santos GW. Suppressor cells in transplantation tolerance. III. The role of antigen in the maintenance of transplantation tolerance. Transplantation 1982;33:510-514. pmid: 6211807.
31. Weiden PL, Storb R, Tsoi M-S, et al. Infusion of donor lymphocytes into stable canine radiation chimeras: Implications for mechanism of transplantation tolerance. J.Immunol. 1976;116:1212-1219. pmid: 774975.
32. Kolb HJ, Günther W, Schumm M, et al. Adoptive immunotherapy in canine chimeras. Transplantation 1997;63:430-436. pmid: 9039935.
33. Zorn J, Herber M, Schwamberger S, et al. Tolerance in DLA-haploidentical canine littermates following CD6-depleted marrow transplantation and donor lymphocyte transfusion. Exp Hematol. 2009;37:998-1006. doi: 10.1016/j.exphem.2009.05.001.
34. Ruggeri L, Capanni M, Urbani E, et al. Effectiveness of donor natural killer cell alloreactivity in mismatched hematopoietic transplants. Science. 2002;295:2097-2100. doi: 10.1126/science.1068440.
36. Le BK, Ringden O. Mesenchymal stem cells: properties and role in clinical bone marrow transplantation. Curr.Opin.Immunol. 2006;18:586-591. doi: 10.1016/j.coi.2006.07.004 .
38. Gratwohl A, Brand R, Apperley J, et al. Graft-versus-host disease and outcome in HLA-identical sibling transplantations for chronic myeloid leukemia. Blood.doi: 10.1182/blood.V100.12.3877 2002;100:3877-3886.
39. Shlomchik WD. Graft-versus-host disease. Nat.Rev.Immunol. 2007;7:340-352. doi: 10.1038/nri2000.
40. Petersdorf EW, Malkki M. Genetics of risk factors for graft-versus-host disease. Semin.Hematol. 2006;43:11-23. doi: 10.1053/j.seminhematol.2005.09.002.
43. Petersdorf EW. Risk assessment in haematopoietic stem cell transplantation: histocompatibility. Best.Pract.Res.Clin.Haematol. 2007;20:155-170. doi: 10.1016/j.beha.2006.09.001.
47. Holler E, Rogler G, Herfarth H, et al. Both donor and recipient NOD2/CARD15 mutations associate with transplant-related mortality and GvHD following allogeneic stem cell transplantation. Blood. 2004;104:889-894. doi: 10.1182/blood-2003-10-3543.
48. Goulmy E. Human minor histocompatibility antigens: New concepts for marrow transplantation and adoptive immunotherapy. Immunol.Rev. 1997;157:125-140.
51. Glucksberg H, Storb R, Fefer A, et al. Clinical manifestations of graft-versus-host disease in human recipients of HL-A-matched sibling donors. Transplantation 1974;18:295-304. pmid: 4153799.
52. Kolb H, Sale GE, Lerner KG, Storb R, Thomas ED. Pathology of acute
graft-versus-host disease in the dog. An autopsy study of ninety-five dogs. Am J Pathol. 1979 Aug;96(2):581-94.
57. Sullivan KM, Deeg HJ, Sanders J, et al. Hyperacute graft-v-host disease in patients not given immunosuppression after allogeneic marrow transplantation. Blood. 1986;67:1172-1175. pmid: 3513869.
58. Rodt H, Netzel B, Brehm G, Thierfelder S. Production of antibodies specific for human thymus derived lymphocytes purified from antibodies crossreacting with colony-forming cells. Blut. 1974;29:416-422. pmid: 4548852.
59. Kolb HJ, Rieder I, Rodt H, et al. Antilymphocytic antibodies and marrow transplantation. VI. Graft- versus-host tolerance in DLA-incompatible dogs after in vitro treatment of bone marrow with absorbed antithymocyte globulin. Transplantation. 1979;27:242-245. pmid: 35870.
60. Rodt H, Thierfelder S, Bender-Gotze C, et al. Serological inhibition of graft versus host disease: recent results in 28 patients with leukemia. Haematol.Blood Transfus. 1983;28:92-96. pmid: 6345300.
61. Goldman JM, Apperley J, Jones L, et al. Bone marrow transplantation for patients with chronic myeloid leukemia. N Engl J Med 1986;314:202-207. pmid: 6345300.
63. Schumm M, Günther W, Kolb HJ, et al. Prevention of graft-versus-host disease in DLA-haplotype mismatched dogs and hemopoietic engraftment of CD6-depleted marrow with and without cG-CSF treatment after transplantation. Tissue Antigens 1994;43:170-178. pmid: 7522357.
64. Soiffer RJ, Ritz J. Selective T cell depletion of donor allogeneic marrow with anti-CD6 monoclonal antibody: rationale and results. Bone Marrow Transplant 1993;12 Suppl 3:S7-10. pmid: 8124262.
66. Guenther W, Kolb HJ, Schumm M, Thierfelder S, Wilmanns W. Suppressive- and veto-effect of canine bone marrow cells [abstract]. 3rd Int Vet Immun Symp Abstractbook 1992.
67. Goldman JM, Gale RP, Horowitz MM, et al. Bone marrow transplantation for chronic myelogenous leukemia in chronic phase: Increased risk of relapse associated with T-cell depletion. Ann.Intern.Med. 1988;108:806-814. pmid: 3285744.
68. Kolb HJ, Rodt H, Netzel B, et al. In vitro treatment of marrow with ATCG or Campath 1 for prophylaxis of GVHD - Results of the AG-KMT München. Exp Hematol 1985;13:147.
69. Finke J, Bethge WA, Schmoor C, et al. Standard graft-versus-host disease prophylaxis with or without anti-T-cell globulin in haematopoietic cell transplantation from matched unrelated donors: a randomised, open-label, multicentre phase 3 trial. Lancet Oncol. 2009;10:855-864.
75. Edinger M, Hoffmann P, Ermann J, et al. CD4+CD25+ regulatory T cells preserve graft-versus-tumor activity while inhibiting graft-versus-host disease after bone marrow transplantation. Nat.Med. 2003;9:1144-1150. pmid: 12925844.
76. Le BK, Rasmusson I, Sundberg B, et al. Treatment of severe acute graft-versus-host disease with third party haploidentical mesenchymal stem cells. Lancet. 2004;363:1439-1441. pmid: 15121408.
78. Kolb HJ, Simoes B, Hoetzl F, et al. CD6-negative mobilized blood cells facilitating HLA-haploidentical marrow transplantation for the treatment of high-risk hematopoietic neoplasia. [abstract]. Blood. 2002;100:637a.
80. White DJ, Lim SM. The induction of tolerance by cyclosporine. Transplantation 1988;46:118S-121S. pmid: 3043793.
82. Storb R, Deeg HJ, Whitehead J, et al. Methotrexate and cyclosporine compared with cyclosporine alone for prophylaxis of acute graft-versus-host disease after marrow transplantation for leukemia. N Engl J Med 1986;314:729-735. pmid: 3513012.
84. Seghal SN. Sirolimus: its discovery, biological properties, and mechanism of action. Transplant Proc 2003;35:7S-14S. pmid: 12742462.
85. Wells AD, Li XC, Li Y, et al. Requirement for T-cell apoptosis in the induction of peripheral transplantation tolerance. Nat Med 1999;5:1303-1307. pmid: 10545998.
88. Yu X, Carpenter P, Anasetti C. Advances in transplantation tolerance. Lancet 2001;357:1959-1963. pmid: 11425437.
92. Deeg HJ. How I treat refractory acute GVHD. Blood. 2007;109:4119-4126.
93. Bacigalupo A, van Lint MT, Frassoni F, et al. High dose bolus methylprednisolone for the treatment of acute graft versus host disease. Blut. 1983;46:125-132. pmid: 6337655.
96. Rhen T, Cidlowski JA. Antiinflammatory action of glucocorticoids--new mechanisms for old drugs. N.Engl.J.Med. 2005;353:1711-1723. pmid: 16236742.
98. Nijhuis EW, Hinloopen B, van Lier RA, Nagelkerken L. Differential sensitivity of human naive and memory CD4+ T cells for dexamethasone. Int.Immunol. 1995;7:591-595. pmid: 7547686.
100. Fan PT, Yu DT, Clements PJ, et al. Effect of corticosteroids on the human immune response: comparison of one and three daily 1 gm intravenous pulses of methylprednisolone. J.Lab Clin.Med. 1978;91:625-634. pmid: 76667.
102. Viard I, Wehrli P, Bullani R, et al. Inhibition of toxic epidermal necrolysis by blockade of CD95 with human intravenous immunoglobulin. Science. 1998;282:490-493. pmid: 9774279.
104. McDonald GB, Bouvier M, Hockenbery DM, et al. Oral beclomethasone dipropionate for treatment of intestinal graft-versus-host disease: a randomized, controlled trial. Gastroenterology. 1998;115:28-35. pmid: 9649455.
108. Knop S, Hebart H, Gratwohl A, et al. Treatment of steroid-resistant acute GVHD with OKT3 and high-dose steroids results in better disease control and lower incidence of infectious complications when compared to high-dose steroids alone: a randomized multicenter trial by the EBMT Chronic Leukemia Working Party. Leukemia. 2007;21:1830-1833. pmid: 17495972.
130. Hoda D, Pidala J, Salgado-Vila N, et al. Sirolimus for treatment of steroid-refractory acute graft-versus-host disease. Bone Marrow Transplant. 2009;45:1347-1351.
131. Ghez D, Rubio MT, Maillard N, et al. Rapamycin for refractory acute graft-versus-host disease. Transplantation 2009;88:1081-1087. pmid: 19898203.
133. Durakovic N, Radojcic V, Powell J, Luznik L. Rapamycin promotes emergence of IL-10-secreting donor lymphocyte infusion-derived T cells without compromising their graft-versus-leukemia reactivity. Transplantation 2007;83:631-640. pmid: 17353785.
134. Armand P, Gannamaneni S, Kim HT et al. Improved survival in lymphoma patients receiving sirolimus for graft-versus-host disease prophylaxis after allogeneic hematopoietic stem-cell transplantation with reduced-intensity conditioning. J Clin.Oncol. 2008;26:5767-5774. pmid: 19001324.
136. Schmitt T, Luft T, Hegenbart U, et al. Pentostatin for treatment of steroid-refractory acute GVHD: a retrospective single-center analysis. Bone Marrow Transplant. 2010 Jun 21. doi:10.1038/bmt.2010.146.
141. Lioznov M, El-Cheikh J Jr, Hoffmann F, et al. Lenalidomide as salvage therapy after allo-SCT for multiple myeloma is effective and leads to an increase of activated NK (NKp44(+)) and T (HLA-DR(+)) cells. Bone Marrow Transplant. 2010;45:349-353. pmid: 19584825.
151. Le BK, Frassoni F, Ball L, et al. Mesenchymal stem cells for treatment of steroid-resistant, severe, acute graft-versus-host disease: a phase II study. Lancet. 2008;371:1579-1586. pmid: 18468541.
152. Deeg HJ. Ultraviolet irradiation in transplantation biology. Manipulation of immunity and immunogenicity. Transplantation 1988;45:845-851. pmid: 3285528.
153. Hymes SR, Morison WL, Farmer ER, et al. Methoxsalen and ultraviolet A radiation in treatment of chronic cutaneous graft-versus-host reaction. J Am.Acad.Dermatol. 1985;12:30-37. pmid: 3980801.
155. Vogelsang GB, Wolff D, Altomonte V, et al. Treatment of chronic graft-versus-host disease with ultraviolet irradiation and psoralen (PUVA). Bone Marrow Transplant. 1996;17:1061-1067. pmid: 8807115.
161. Perotti C, Del Fante C, Tinelli C, et al. Extracorporeal photochemotherapy in graft-versus-host disease: a longitudinal study on factors influencing the response and survival in pediatric patients. Transfusion. 2010;50:1359-1369.
164. Bladon J, Taylor PC. Early reduction in number of T cells producing proinflammatory cytokines, observed after extracorporeal photopheresis, is not linked to apoptosis induction. Transplant Proc. 2003;35:1328-1332. pmid: 12826151.
166. Di Biaso I, Di Maio L, Bugarin C, et al. Regulatory T cells and extracorporeal photochemotherapy: correlation with clinical response and decreased frequency of proinflammatory T cells. Transplantation. 2009;87:1422-1425.
167. Ford CE, Micklem HS. The thymus and lymph-nodes in radiation chimaeras. Lancet 1963;1:359-362. pmid: 13958695.
168. Zinkernagel RM. Thymus and lymphohemopoietic cells: their role in T cell maturation in selection of T cells' H-2-restriction-specificity and in H-2 linked Ir gene control. Immunol Rev. 1978;42:224-270. pmid: 83701.
170. Steffens CM, Al Harthi L, Shott S, Yogev R, Landay A. Evaluation of Thymopoiesis Using T Cell Receptor Excision Circles (TRECs): Differential Correlation between Adult and Pediatric TRECs and Naive Phenotypes. Clin Immunol. 2000;97:95-101. pmid: 11027449.
171. Witherspoon RP, Sullivan KM, Lum LG, et al. Use of thymic grafts or thymic factors to augment immunologic recovery after bone marrow transplantation: brief report with 2 to 12 years' follow-up. Bone Marrow Transplant. 1988;3:425-435. pmid: 3056551.
172. Wils EJ, Cornelissen JJ. Thymopoiesis following allogeneic stem cell transplantation: new possibilities for improvement. Blood Rev. 2005;19:89-98. pmid: 15603912.
175. Pullen AM, Kappler JW, Marrack P. Tolerance to self antigens shapes the T-cell repertoire. Immunol Rev. 1989;107:125-139. pmid: 2522084.
176. Zinkernagel RM, Doherty PC. Restriction of in vitro T cell-mediated cytotoxicity in lymphocytic choriomeningitis within a syngeneic or semiallogeneic system. Nature. 1974;248:701-702. pmid: 4133807.
177. Thomas ED, Kasakura S, Cavins JA, Ferrebee JW. Marrow transplants in lethally irradiated dogs: The effect of Methotrexate on survival of the host and the homograft. Transplantation. 1963;1:571-574. pmid: 14071268.
178. Santos GW. Immunosuppression for clinical marrow transplantation. Semin.Hematol. 1974;11:341-351. pmid: 4151847.
180. Miller RG, Muraoka S, Claesson MH, Reimann J, Benveniste P. The veto phenomenon in T-cell regulation. Ann N Y Acad Sci. 1988;532:170-6. pmid: 2972242.
182. Gabrilovich DI, Nagaraj S. Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev.Immunol 2009;9:162-174. pmid: 19197294.
186. Kapp JA, Bucy RP. CD8+ suppressor T cells resurrected. Hum.Immunol 2008;69:715-720. pmid: 18817830.
187. Peccatori J, Clerici D, Forcina A, et al. In vivo T-regs generation by rapamycin-mycophenolate-ATG as a new platform for GVHD prophylaxis in T-cell repleted unmanipulated haploidentical peripheral stem cell transplantation: results in 59 patients [abstract]. EBMT Meeting Vienna. 2010. 2010;S3-S4.
190. Paczesny S, Braun TM, Levine JE et al. Elafin is a biomarker of graft-versus-host disease of the skin. Sci.Transl.Med 2010;2:13ra2. pmid: 20371463.
" ["~DETAIL_TEXT"]=> string(123322) "Introduction
Allogeneic hematopoietic stem cell transplantation has become one of the most frequent forms of transplantation, with currently more than 6000 transplants being performed annually. Its use is still increasing in the treatment of hematological and other malignancies. In addition there are a large number of patients with debilitating and life threatening hematological dis-eases, thalassemia, sickle cell anemia, and other non-malignant diseases that may benefit from transplantation. However, the major obstacle to the wider use of transplantation is graft-versus-host disease (GVHD); still a serious threat to these patients. However, at the same time graft-versus-host reactions directed at leukemia, lymphoma, myeloma, and other tumors of the host may be beneficial. Therefore it is necessary to understand GVHD in order to ex-ploit the potential advantages without incurring the risks. Allogeneic stem cell transplantation conveys tolerance toward organs of the donor. As a rule, immunosuppressive therapy can be discontinued after several months without the risk of rejection and GVHD. This tolerance with chimerism allows the transplantation of cells and organs of the same donor without life-long immune suppression. The success of immunotherapy with donor cells and of transplantation of solid organs from the stem cell donor depends on whether or not GVHD can be controlled.
Early observations
Mice protected from hematopoietic failure following total body irradiation by bone marrow transplantation succumbed to a “secondary disease” if the bone marrow was taken from a different strain [1]. This disease was related to an immune reaction of donor cells against the host rather than a delayed radiation syndrome: cells of diseased mice induced hepato-splenomegaly when transferred to non-irradiated newborn mice [2]. Further proof was the oc-currence of this secondary disease in F1-hybrid mice transplanted with parental marrow, but not in parental mice transplanted with F1-hybrid marrow [3]. Finally, organs containing more immunologically competent cells such as those from the spleen produced more secondary disease than bone marrow [4]. Eventually, the principle requirements for GVHD were defined by Billingham [5]: 1. the graft must contain immune reactive cells, 2. the recipient must be im-munogenetically different, and 3. the recipient cannot reject the graft. The first patients with acute GVHD were described by Mathé and colleagues [6]. A major step towards successful transplantation was the selection of marrow donors within the family according to major his-tocompatibility antigens (HLA) [7]. HLA had been previously detected in humans with pre-formed antibodies [8, 9]. Most preconditions for allogeneic transplantation in humans have been elaborated in animal experiments, particularly in dogs 10].
Therefore the principles for prevention of GVHD are 1. selection of a histocompatible donor, 2. adequate immune suppression for the patient before and after transplantation, and 3. ma-nipulation of the graft. In more recent years much has been learned about the regulation of the T cell response and mechanisms of tolerance, which may guide the way for immune suppression [11].
Animal models
The manifestation of GVHD in every species investigated so far involves skin, gut, and liver; primarily however hematopoietic tissue (Fig.1). Acute GVHD is a syndrome with similar fea-tures in mice, rats, monkeys, and humans; without prevention or treatment it can be rapidly fatal. Therefore pathophysiology, prevention, and treatment of acute GVHD can be studied in animal models. Chronic GVHD cannot be readily studied in animal models; it is not known why certain organs are involved and others are spared. Obviously hematopoietic cells are the primary targets, and the skin, gut, and liver may contain cells of hematopoietic origin such as dendritic cells and macrophages. These cells produce pro-inflammatory cytokines including interferon-gamma (IFN-g), tumor necrosis factor-alpha (TNF-a), interleukin 6 (IL-6), and others that stimulate donor T cells and induce expression of HLA class II antigens in host tissue (Fig.2). Dendritic cells activated by CD4 cells may stimulate CD8 cells to react against HLA class I presented peptides (Fig.3). Recent studies, however, showed that deficient production of IFN-g can increase GVHD in the skin, and failure of IFN-g induction of B7-H1 enhanced TH2 cells can produce idiopathic pneumonia [12]. TH2 cells and TH17 cells were guided to lungs and skin by the expression of chemokine receptors.
Figure 1. Host target tissues affected in the course of graft-versus-host disease

Figure 2. A proposed role of cytokine network and specific receptors of immune cells at initiation of GvHD (for details see text)

Figure 3. Dendritic cells boost CD8+ cells to react against host target tissues

GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. These antigens can be defined by the major histocompatibility complex, a highly polymorphic genetic region determining class I and class II antigens. Class I antigens are present in all cells of the organism, and class II normally only in hematopoietic cells. They may be expressed in other cells if these are affected by inflammation or injury. CD4-positive T cells exert GVH reactions against cells expressing class II antigens, and CD8-positive T cells act against class I antigens [13]. Differences in both antigen classes can induce severe and rapidly fatal GVHD. Polymorphic proteins not encoded by the major histo-compatibility complex may also cause severe GVH reactions. Peptides of these proteins can be presented by MHC class I and class II antigens. In general, MHC class I presents peptides of endogenous proteins of the cell, whereas class II antigens present peptides of exogenously acquired proteins [14, 15]. Here, minor histocompatibility (mHA) directed CD8 T cells require help from CD4 T cells for expansion and generation of memory T cells [16]. Therefore, reactions against mHA require a longer phase of immune recognition and activation than reactions against MHC antigens. Class II antigens are mainly expressed in hematopoietic progenitor cells, and in the case of injury and inflammation they may be expressed in non-hematopoietic cells as well. Reactions directed against class II antigens may induce severe marrow aplasia [17].
The mechanism of initiation of acute GVHD is not entirely clear; the preconditions are given before transplantation [18]. Much has been explained and published on cytokines and the cyto-kine storm liberated by intensive conditioning treatment, including high dose radiation and chemotherapy [19]. The role of cytokine release is confirmed by the suppression of acute GVHD using TNF-a antibodies [20]. There is some evidence that the systemic release of IFN-g leads to the secretion of chemokines in organs affected by GVHD and attracts activated T cells. In transgenic mice carrying the T cell receptor for ovalbumin the distribution of T cells was dependent on whether the antigen was given alone or together with lipopolysaccharide (LPS). Intravenous injection of antigens alone homes the T cells to secondary lymphoid tissue where they produce IL2, whereas injection of a combination of antigens and LPS homes the T cells to the lung, liver, gut, and skin where they produce IFN-g [21]. Systematically activated T cells produce interferons and induce chemokines in GVHD target organs [22]. However, the “danger signal” brought about by LPS may not be necessary, since in human patients donor lymphocyte transfusion may produce GVHD without conditioning treatment and infection [23].
The host's antigen presenting cells survive the conditioning treatment for various periods of time, with the most efficient cells being dendritic cells, but B cells, macrophages and other cells present antigens as well. Whereas dendritic cells in the blood of the host are rapidly re-placed by those of the donor, data on chimerism of dendritic cells in tissues are controversial [24]. Cytokine release by the host's activated dendritic cells and the graft's T cells is part of the initiation of GVH reactions (Fig. 2), and may be powerful enough to induce fatal GVHD even in the absence of histoincompatibility [25]. In general however, histocompatibility differences are necessary to induce and maintain GVH reactions. These histocompatibility differences may be of the major histocompatibility complex (MHC) class I or class II involving CD4- or CD8-positive T cells of the graft, and minor histocompatibility differences requiring profes-sional antigen presentation by dendritic cells of the host. GVHD occurring in the skin, liver, and gut requires dendritic cells expressing class I [26]. There is a possibility of cross presenta-tion of host antigens by donor dendritic cells, but their effects are inferior to direct presentation [27].
In contrast to cases involving the transplantation of solid organs, immunosuppressive therapy can be discontinued 3–6 months after transplantation in most patients receiving hematopoietic stem cell transplants, although patients who develop chronic GVHD may require therapy for several years. The host’s immune system is continuously suppressed by the graft, and the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion [28-30]. In DLA-identical canine chimeras tolerance could not be abrogated by the transfusion of donor lymphocytes unless the donors were immunized against the recipient [31]. Refractoriness to donor lymphocytes inducing GVHD develops at about two months after T cell depleted transplantation [32]. It may occur earlier in dogs transplanted with marrow depleted of T cells by CD6-antibody sparing NK cells [33]. NK cells can inactivate host dendritic cells and thereby prevent GVHD in mice [34]. Besides depletion of T cells and dendritic cells in the graft and the host, responder cells to antigen stimulation may respectively be eliminated by subsequent chemotherapy with methotrexate or cyclophosphamide. Cyclophosphamide can be given in rather high doses after transplantation without jeopardizing engraftment [35]. Modulation and suppression of GVH reactions has been shown for fractions of marrow cells such as mesenchymal stromal cells [36], NK-T cells (NKT1.1) [37], and regulatory T cells [11].
The results of animal models are highly informative with respect to the principles and me-chanisms of GVHD, but they also have their limitations. Apart from species-specific regulato-ry mechanisms of hematopoiesis and the immune system, animals are mostly young, have grown up in a protected environment, and are free of disease for which clinical transplantation is undertaken. In contrast, human patients are commonly older, have a history of infections and most likely a number of latent viral infections, and are possibly allo-immunized by previous transfusions and pregnancies, as are their donors. Moreover the primary disease and its treatment have a major impact on the transplant course.
The role of the immune repertoire of donor and host is still poorly defined. Female donors produce more GVHD and GVL in male recipients; most likely due to immunization during pregnancies by antigens derived from the fetuses' father [38]. Conversely, central memory T cells produce less GVHD than naïve T cells, indicating that the GVH reaction in most cases is a primary reaction [39]. Presumably central memory T cells cannot be involved in new primary reactions; there is also a risk that central memory T cells may produce vigorous GVHD when they recognize the antigen against which they developed. Alternatively they could be regulated by regulatory T cells.
Genetics
Selecting an HLA-identical sibling as donor was the major step towards successful stem cell transplantation. Selecting the donor within a family by typing for HLA-A, -B and DR-antigens is sufficient for successful transplantation, since antigen typing defines the haplotypes inhe-rited from the parents. Unlike identity by inheritance, selection of an unrelated donor relies on the most accurate typing of as many loci as possible. In general genetic definition of alleles of 10 HLA-loci is required to select a matched donor [40]. Severe GVHD can occur with any form of mismatch, but graft failure is less serious with mismatches for HLA-alleles than for the broader HLA-antigens [41]. In multiple mismatches the impact of various HLA-loci (A, B, C, DR) was similar, with the possible exception of HLA-DQ, which was less important. Notewor-thy is a possible racial difference in the role of HLA-C; in Japanese populations HLA-C has a lesser effect on GVHD than other HLA-loci [42]. In Caucasian populations HLA-C is as impor-tant for GVHD as other HLA-antigens [43]. The linkage disequilibrium, i.e. the occurrence of two antigens together, is more frequent than expected by the antigen frequency, is high for HLA-B and -C as well as for HLA-DRB1 and DQB1; therefore isolated mismatches are infre-quent. The linkage disequilibrium of HLA-DP with HLA-DRB1 is rather low, and differences of HLA-DP do not carry an additional risk for GVHD. They may, however, have an effect on the graft-versus-leukemia activity [44].
Presently little is known about permissible HLA-mismatches that allow for the development of tolerance. There may be racial differences as shown for HLA-C in Japanese as compared to Caucasian populations. In general HLA-mismatches are more permissible in patients with advanced disease than in patients with early disease. An allele mismatch may produce se-vere GVHD in a patient in chronic phase CML, but it may not have an effect in a patient with relapse of leukemia [43]. Cytokine levels and cytokine receptors are coded for by genes of the major histocompatibility complex. Sequence polymorphisms of genes for tumor necrosis fac-tor alpha (TNF-a), IL-6 and interferon-gamma (IFN-g) are different in persons with different racial backgrounds, i.e. Caucasians, Africans, and Cubans [45]. There have been several al-leles defined for both the TNF-a locus and the TNF-a receptor II locus that are associated with an increased risk of GVHD. Contrary to the pro-inflammatory cytokine TNF-a, IL-10 has anti-inflammatory effects. Polymorphisms of the promoter of IL-10 had an impact on GVHD. High levels of IL-10 correlated with a lower risk of GVHD.
Genetic factors outside of the HLA-complex may also be involved in the pathogenesis of GVHD. In the analysis of the gene expression profiles of donor cells, a particular role of transforming growth factor beta for chronic GVHD has been found [45]. In patients transplanted for chronic myelogenous leukemia [46] polymorphic alleles of TNF-receptor in the patient and certain alleles in IL10 and IL1 receptor in donor lymphocytes were associated with an in-creased risk of GVHD and decreased survival. A genetic factor associated with inflammatory bowel disease had an impact on GVHD (NOD/Card1) [47]. However, the effect could be dimi-nished if the gut was microbiologically well decontaminated. Antimicrobial prophylaxis de-creases the risk of GVHD without the GVL effect deteriorating.
There is good evidence that minor histocompatibility antigens play a role in GVHD and GVL reactivity [48, 49]. However, a recent analysis of the role of minor antigens in HLA-matched unrelated transplants by the NMDP did not find an impact of minor HA differences on the out-come of allogeneic stem cell transplantation [50].
Clinical features
Acute GVHD
GVHD was described and classified in the '70s [51, 52], when most patients were conditioned with total body irradiation. Skin is the organ most frequently affected; a maculopapular rash is common. This rash starts frequently in the upper thorax, arms, and face, but it can occur elsewhere and spread over the whole body. Features range from a maculopapular rash to general dermatitis with blisters and epidermal necrolysis. Histological findings are degenera-tion and apoptosis of the basal cells, dyskeratosis and lymphocytic infiltration. Involvement of the gastrointestinal tract is clinically characterized by diarrhea, malaise and vomitus; diarrhea may be severe with several liters of liquid and bloody stools. Histological findings are flatten-ing of the mucosa with debris in crypts (crypt abscesses); the most frequently affected part is the ileum. GVHD of the liver is characterized by jaundice and increases of liver enzymes. Histologically the Glisson triads are infiltrated, and the bile ducts are destroyed by infiltrating lymphocytes. Unfortunately none of the histological signs are diagnostic — viral infections and drug reactions may present similar features. Nevertheless biopsies may be indicated in order to exclude other diagnoses with characteristic signs and to obtain material for microbio-logical studies.
Despite prophylactic treatment with immunosuppressive drugs the prevalence of acute GVHD of all grades of severity is high, with a rate of 40–60% in patients with an HLA-identical sibling donor and 60–90% with a matched unrelated donor. Only at a severity of grade 2 and higher is additional immunosuppressive treatment required: this equates to 40–70% of patients. Another grading system was designed by the International Bone Marrow Transplant Registry IBMTR and validated in two studies [53, 54]. This grading system does not take into account the clinical performance as does the system of H. Glucksberg [51]. No advantage of one system over the other has been shown [54]. In both grading systems microangiopathy has not been scored as a form of acute GVHD; microangiopathy is characterized by red cell fragmentation, high levels of serum lactate dehydrogenase and thrombocytopenia. It is more frequent in patients treated with calcineurin inhibitors [18] or sirolimus, and resembles thrombotic thrombocytopenic purpura, but polymers of von Willebrand factor have not been found [55].
Table I. Acute GVHD. Diagnostic criteria according to H. Glucksberg
|
Stage |
Skin maculopapular rash |
Liver bilirubin |
Gut diarrhea |
|---|---|---|---|
|
+ |
< 25% body surface area |
2 - 3 mg/dl |
> 500 ml |
|
++ |
25 - 505 BSA |
3,1 - 6 mg/dl |
> 1000 ml |
|
+++ |
Generalized erythroderma |
6,1 - 15 mg/dl |
> 1500 ml |
|
++++ |
General erythroderma with bulla formation and desquamation |
> 15 mg/dl |
Severe abdominal pain w/wo ileus |
|
Cell Ther Transplant. 2012;2:e.000089.01. doi:10.3205/ctt-2012-en-000089.01-table1 |
|||
Table II. Acute GVHD. Diagnostic criteria according to H. Glucksberg
|
Grade of aGVHD |
Skin |
Liver: |
Gut: |
Clinical performance |
|---|---|---|---|---|
|
I |
+ - ++ |
bilirubin < 2,0 mg/dl |
No diarrhea |
Ok |
|
II |
+ - +++ |
3,1 - 6 mg/dl |
Diarrhea > 500 ml |
Mild decrease |
|
III |
++ - +++ |
6,1 - 15 mg/dl |
> 1000 ml |
Marked decrease |
|
IV |
++ - ++++ |
> 6,1 mg/dl |
> 1000 ml |
Severe decrease |
|
Cell Ther Transplant. 2012;2:e.000089.01. doi:10.3205/ctt-2012-en-000089.01-table2 |
||||
Chronic GVHD
Acute GVHD may resolve completely with immunosuppressive treatment or it may lead to chronic GVHD. Chronic GVHD may also develop de novo without prior acute GVHD within a year from transplantation. Chronic GVHD involves most frequently the skin with lichenoid and sclerotic changes, the nails with dystrophy, the eyes with keratoconjunctivitis, the mouth with dryness and paradontosis, the vagina with dryness and sclerosis, liver and lungs. The clinical features of chronic GVHD resemble autoimmune diseases like lupus erythematodes, Sjögren syndrome, and biliary cirrhosis in many aspects. Characteristically there is hypogammaglo-bulinemia with loss of IgA, and lymphopenia, but there may also be hypergammaglobulinemia and eosinophilia. Thrombocytopenia is a sign of poor prognosis; another factor of poor prognosis is involvement of the lungs, which may be in the form of late interstitial pneumonitis and fibrosis or obliterating bronchiolitis. As a rule lung involvement is progressive and carries the risk of severe infections. The skeletal system may be involved in form of fasciitis, muscle dystrophy, tendinitis, and contractures. Transplant vasculopathy is a problem of solid organ transplants: in stem cell transplanted patients vasculitic changes in the CNS have been observed and vascular events can be seen in young patients [56] without other risk factors.
Overlapping GVHD
Besides the clinical features, acute and chronic GVHD have been defined by the time of oc-currence: acute GVHD in the first weeks and months, and chronic GVHD after day 100. This definition has been challenged by the introduction of cyclosporine A for immune suppression and conditioning with reduced intensity. Following discontinuation of cyclosporine A, a flare of acute GVHD may occur, and following reduced intensity conditioning, acute GVHD may occur late. Similarly, late onset of acute GVHD has been observed after prophylactic treat-ment with TNF-antibody during conditioning [20]. Obviously the activation of T cells is delayed by reduced intensity conditioning and prophylactic treatment, with TNF-antibodies leading to late acute GVHD.
Prophylaxis of GVHD
Some form of prophylaxis of GVHD is absolutely necessary even in HLA-identical sibling transplants, as hyperacute GVHD was seen in every patient with engraftment [57]. T cells are responsible for GVHD and depletion of T cells from the transplant was very successful in an-imal models [58, 59]. In the clinical setting GVHD could be prevented or suppressed [60, 61] effec-tively. Antithymocyte globulin (ATG) has a broad specificity, recognizing not only T cells, but other mononuclear cells as well. The monoclonal antibody alemtuzumab recognizes CD52, an antigen that is present in many leukocytes including lymphocytes, monocytes, and den-dritic cells; alemtuzumab has broad activities despite its specificity. In humans [62] as in dogs [63] the number of clonable T cells should be below 105/ kg body weight for effective prevention of GVHD. So far more selective depletion of T cells has not improved the overall results of transplantation [64], and depletion of CD8 has been insufficient in preventing GVHD [65]. CD6 has the advantage of sparing most of the NK cells in the transplant [64]. In dogs CD6-depleted marrow suppresses alloresponses [66] and recipients of CD6-depleted marrow tolerate donor lymphocyte transfusions earlier than recipients of marrow treated with absorbed ATG [33].
However, the advantage of ex vivo T cell depletion was offset by a high rate of graft rejection, relapse, infections, and EBV-associated post transplant lymphoproliferative disease (PTLD) [67, 68]. Treatment of the patient prior to transplantation with ATG prevents rejection; T cell anti-bodies persist in the patient for 4–5 weeks and deplete T cells of the graft in vivo. A rando-mized study comparing standard post-grafting immune suppressive treatment with and with-out ATG prior to transplantation showed lower rates of acute and chronic GVHD in the group treated with ATG [69]. A beneficial effect of ATG in the conditioning treatment for chronic GVHD has also been observed in Italian studies [70] and in retrospective analyses of non-randomized studies (own unpublished observations).
Alemtuzumab also persists in the patient for a prolonged period of time, and reconstitution of T cells is delayed for 6–9 months [71]. Severity of GVHD is low in patients treated with alemtu-zumab, but graft failures have been observed [72]. There is also an increased risk of viral infec-tions, particularly cytomegalovirus, and insufficient response of the malignant disease. These deficiencies can be compensated at least partially by the transfusion of donor lymphocytes [73].
In the last decade G-CSF mobilized peripheral blood stem cells (PBSC) have replaced mar-row in most instances. PBSC contain enormous amounts of T cells and depletion of T cells has been largely unsuccessful. Surprisingly, transplantation of PBSC is not associated with an increased risk of acute GVHD, but is instead associated with a more rapid engraftment and an increased risk of chronic GVHD [74]. PBSC may be preferable for patients with advanced disease and elderly patients. Conversely, T cell depletion and marrow transplantation may be the preferred treatment for patients with early disease, non-malignant disease, and patients who are younger.
Other approaches to prevent GVHD use specific conditioning regimens [37] or specific cells to induce transplantation tolerance. Low dose total lymphoid irradiation in combination with ATG may spare natural killer T cells in the marrow and regulatory T cells suppressing GVHD, but allow graft-versus-leukemia/lymphoma effects. The addition of regulatory T cells to the graft has suppressed GVHD without inhibiting GVL effects in mice [75] and recently in humans (Martelli F, Plenary session ASH 2009). Another immunosuppressive cell product are me-senchymal stromal cells, which have been successful in the treatment of severe GVHD [76]. Co-transplantation of mesenchymal stromal cells prevented rejection in HLA-haploidentical transplants [77] and GVHD was less severe, but the difference did not reach significance be-cause of low numbers. We have used CD6-depleted PBSC transfused 6 days after trans-plantation of unmodified marrow from HLA-haploidentical donors with a low rate of acute GVHD [78].
Post-graft immunosuppressive treatment with either methotrexate or cyclophosphamide has been used since the early days of stem cell transplantation. Both agents preferably kill proli-ferating cells and should be started early after grafting. These drugs suppress donor cells proliferating in response to host antigens as well as residual host cells responding to the graft. They sustain engraftment and suppress GVHD at the same time. They induce transplantation tolerance by killing the responsive cells, and therefore patients with incomplete responses usually take a disastrous course. A recent application of this principle is the use of large doses of cyclophosphamide 3 and 4 days after HLA-haploidentical transplantation [35, 79].
The introduction of the calcineurin inhibitors cyclosporine A and tacrolimus has also changed the outlook for these patients. Both drugs inhibit the activation and proliferation of T cells by inhibiting dephosphorylation and translocation of the nuclear factor of activated T cells (NFAT). The continuous inhibition is effective in suppressing GVHD and rejection, but the effect is not necessarily maintained after discontinuation of treatment; calcineurin inhibitors are less potent in the induction of transplantation tolerance [80]. Treatment should be started prior to transplantation in order to avoid antigen recognition and T cell activation. Tacrolimus is a somewhat stronger immunosuppressive than cyclosporine A and possibly less neurotoxic. However, in controlled studies comparing tacrolimus and cyclosporine A less severe GVHD was not associated with improved survival [81].
The combination of cyclosporine A and methotrexate is better than either drug alone [82]. It has become the gold standard of GVHD prophylaxis. In recent years mycophenolate mofetil (MMF) has been introduced to replace methotrexate [83]. MMF inhibits the purine synthesis and the de novo pathway of guanosine nucleotide synthesis; it kills not only proliferating T cells, but also T cells in the interphase. MMF produces less mucositis and less marrow toxicity than methotrexate. However the best regimen and timing (2–3 times per day) remains unknown.
Sirolimus binds to the tacrolimus binding protein FKBP12 and forms a complex with mTOR (target of rapamycin) that inhibits several signal transduction pathways including PTEN, PI3kinase and AKT as well as the JANUS kinase pathway. Thereby it produces several ef-fects including immunosuppression of T cells, anti-angiogenesis and inhibition of tumor growth [84]. Its immunosuppressive activity is presumably linked to the suppression of the second signal of T cell activation. This way T cell apoptosis and specific peripheral non-responsiveness may be induced [85]. Th1 cells and their cytokines are more affected by siroli-mus than Th2 cells and regulatory T cells [86, 87]. The sirolimus/mTOR complex inhibits the ac-tivation signals of CD28 and CD40L stimulation and thereby the second signal essential for T cell activation [88], a situation that may lead to transplantation tolerance. The combination of sirolimus and tacrolimus is synergistic and has shown little toxicity [89], but veno-occlusive dis-ease of the liver and thrombotic microangiopathy have been observed [90]. The combination of sirolimus and MMF was promising in a smaller group of patients, where VOD and TMA were not observed [91].
The goal of preventing GVHD is the induction of tolerance in both directions, the host-versus-graft and graft-versus-host direction. Contrary to transplantation of solid organs, stem cell transplantation induces self-sustained tolerance without life-long immunosuppressive therapy. As a rule, a period of 4–6 months of immunosuppressive therapy is sufficient for tolerance to become established. In clinical terms tolerance is evident by persistent chimerism without GVHD and without severe infections more than 30 days after discontinuation of immunosuppression.
Treatment
Glucocorticoids
Despite prophylactic treatment with immunosuppressive agents, acute GVHD requiring addi-tional treatment occurs in 40–80% of patients within 3–4 weeks of transplantation [92]. Corti-costeroid therapy is the standard of treatment for acute GVHD, but the regimen and the do-sage is still under discussion. Originally, treatment with large doses was favored [93], but there are no controlled studies to support this treatment. Similarly, in organ transplantation, rejection crises are treated with bolus methylprednisolone without prospective randomized trials supporting this. Despite this general use there are only a few studies on the schedule and the dosage rates. A randomized Italian trial comparing 2mg/kg per day with 10mg/kg per day showed no advantage for the higher dose [94], however 50% of patients were switched to a high dose because of insufficient response. Recently, a retrospective study from Seattle indi-cated that even lower doses of corticosteroids (1mg/kg instead of the standard 2 mg/kg) can be given without disadvantage [95]. However the patients of the low dose group had more fa-vorable risk factors and less severe GVHD; in addition oral non-absorbable corticosteroids were given more frequently.
The mechanisms of the actions of glucocorticoids are still not fully understood, lymphopenia is mainly due to sequestration of lymphocytes, and less to lympholysis. However, glucocorti-coids exhibit strong anti-inflammatory effects in several ways including genomic and non-genomic pathways [96]. Glucocorticoids are bound to a receptor from which heat shock protein 70 is released. The glucocorticoid complex activates anti-inflammatory proteins directly and their production genomically. Inhibition of nuclear factor kB is highly sensitive to glucocortico-ids preventing the production of inflammatory proteins. Sensitivity to the treatment with glu-cocorticoids may be determined by the relative levels of glucocorticoid receptor α and ß. This may explain interpatient variation of sensitivity [97]; memory T cells [98] as well as mature den-dritic cells are less sensitive to glucocorticoids. In macrophages low doses of glucocorticoids stimulate the production of proinflammatory cytokines, whereas high doses suppress it [99]. High dose glucocorticoid therapy given for few days has shown little immune suppression in vivo [100].
Commonly treatment is started in patients with clinical grade II–IV severity of GVHD. About 40–50% of patients respond with resolution or improvement of clinical symptoms [92]. The re-mainder are classified as “steroid-refractory”. The time until refractoriness to glucocorticoids is stated may vary from 5 to 14 days [101]. Many centers increase the dose of steroids in re-fractory patients prior to the addition of other agents. We prefer to start with rather high doses of glucocorticoids (1–2mg/kg every 8 hours) and score the response after three days of treatment for refractoriness. This way we initiate secondary treatment early in refractory pa-tients. The decision to start the treatment is made by two physicians. In the case of a pro-gressive and characteristic skin rash the diagnosis is not difficult, but in cases of isolated ga-strointestinal GVHD with diarrhea and nausea or isolated hepatic GVHD the diagnosis may be more difficult. Persistent toxicity of the conditioning treatment, veno-occlusive disease of the liver, drug-induced changes and viral infections are considered as differential diagnosis. In our centre skin biopsies are regularly performed, biopsies of gut and liver are only made in patients that do not respond to the treatment. This way we obtain not only histological con-firmation of the clinical suspicion, but also information about viral infection. Concomitant vi-rostatic treatment is given to patients with biopsies positive for viral infection as well as those that are seropositive for cytomegalovirus. Another option is the use of high doses of iv immu-noglobulins that may inhibit the deleterious effects of FAS by their blockade of FAS-L [102]. Al-though their immune modulating effects are far from understood [103], 20–30% of patients with skin GVHD do respond to the treatment with iv immunoglobulins. In any case early treatment is important as delay of the start of treatment until the results of laboratory investigations are available may jeopardize the response to glucocorticoids.
The effect of systemic glucocorticoids on gastrointestinal GVHD can be improved by local treatment with beclomethasone [104] and budesonide [105].
Antibodies
In many instances the first choice in patients with steroid refractory GVHD has been immu-nosuppressive antibodies. Antithymocyte globulin (ATG) has been used in several uncon-trolled studies with some success [106], but in controlled studies a beneficial effect could not be demonstrated [107]. Similarly, OKT3 is a monoclonal antibody against CD3 on T cells: it dep-letes T cells and stimulates proliferation by its mitogenic activity. Even though many patients have responded to the treatment with OKT3 with complete remission of GVHD, better surviv-al could not be demonstrated in controlled clinical trials [108]. Alemtuzumab has been used mainly for prophylaxis of acute GVHD by treating the patient in vivo or the graft prior to transplantation ex vivo: recently beneficial outcomes of treatment of established GVHD have been reported in two uncontrolled studies [109, 110]. Viral infections may complicate treatment with alemtuzumab; therefore regular control and pre-emptive treatment is necessary. ATG and OKT3 both stimulate proliferation of lymphocytes that are not killed by cytolysis; there-fore the combination of antibody treatment with chemotherapy (methotrexate, Cyclophos-phamide, mycophenolate mofetil, etc.) may be beneficial. A humanized CD3-antibody (visili-zumab) produced good first results [111] which unfortunately were not confirmed in multicenter trials [112]. In those patients the reactivation of EBV and the incidence of post transplant lym-phoproliferative disease (PTLD) increased.
Encouraging results were also reported with ABXCBL, an antibody against CD147 that is ex-pressed in activated T cells [113]. However in a comparative study ABXCBL was not better than ATG, where survival was even inferior [114].
Antibodies against tumor necrosis factor α (TNF-a) and soluble receptors of TNF-a (etaner-cept) have been studied in the prophylaxis of GVHD [20] and the treatment of steroid refractory GVHD [115]. There has been a high rate of complete response to infliximab even in gastrointes-tinal GVHD, but this is complicated by an increased risk of fungal infections [116, 117]. Contrary to infliximab etanercept neutralizes soluble TNF-a without affecting TNF-a in phagocytic cells. Etanercept is associated with a lower risk of fungal infections. The combination of etanercept with an anti-IL2-receptor antibody showed high response rates to acute GVHD, but the long-term survival was rather poor [118]. In comparison, a pilot trial of etanercept in combination with tacrolimus and steroids gave a 75% complete response and a 50% survival rate [119]. When comparing etanercept combined with steroids to steroids alone a significantly better response to the combination was observed [120]. The combination of etanercept with ATG and tacrolimus was compared to ATG and tacrolimus alone [121]; considering the limited number of patients the response and the survival of patients given etanercept was better. Neutralization of TNF-a released by the ATG treatment by etanercept may have been contributing to the better outcome.
Antibodies against IL-2 receptor have been studied early [122] with some transient success. The importance of an early treatment start was stressed. Several studies with humanized anti-IL2-receptor antibodies were encouraging [123, 124], but a randomized study was stopped prematurely because of inferior survival of the antibody (daclizumab) group [125]. There is little doubt that the IL2- receptor antibody is effective in suppressing GVHD of the skin and the gut when started early, but it may have an adverse effect on the generation of regulatory T cells expressing high levels of the IL-2 receptor.
Alefacept is a fusion protein of the CD2-binding domain of LFA-3 and the Fc portion of IgG with specific activities against memory T cells [126]. Promising results in steroid refractory acute GVHD and in chronic GVHD have been reported, but there may be an increased risk of viral and fungal infections [127].
Recently, the role of B cells has been discussed more frequently, although the role of T cells in GVHD is not disputed. However, cytotoxic antibodies may be produced in HLA-mismatched chimeras, and depletion of B cells may prevent EBV-induced B cell lymphoma. Single patients have been reported to show a response to steroid refractory GVHD to the treatment with rituximab [128].
Drugs
As a rule the treatment given for prophylaxis is continued during the treatment of established GVHD, and includes glucocorticoids at a low level. Depending on the prophylactic regimen, cyclosporine A may be substituted by tacrolimus and new drugs may be added. In most Eu-ropean centers a calcineurin inhibitor is combined with methotrexate or mycophenolate mofe-til. In patients not treated prophylactically a trial with mycophenolate mofetil may be justified; a response rate of 47–48% has been reported in steroid refractory GVHD, but the survival at 6 and 12 months was not improved [129]. Methotrexate on a weekly basis in low doses has been helpful in single cases. Mucositis and myelosuppression are limiting factors.
Similarly, sirolimus can be used for patients not treated prophylactically, as response rates of 77% overall and 44–72% complete response have been reported [130, 131]. Again microangiopa-thy has been a problem, but could be controlled by discontinuation of the calcineurin inhibitor (CNH) or both sirolimus and CNH. A small study suggests a good response of acute GVHD to sirolimus without prior treatment with glucocorticoids [132]. Due to its anti-tumor activity siro-limus is preferred to calcineurin inhibitors and glucocorticoids by many investigators [133], par-ticularly in patients with lymphoma [134].
Pentostatin is an inhibitor of the salvage pathway of thymidine kinase that is specific for T cells. Phase I studies have shown efficacy in the treatment of steroid-refractory GVHD [135]. A retrospective analysis has shown activity comparable to other immunosuppressive regimens [136]. However, pentostatin has shown activity in the treatment of chronic GVHD [137, 138]. Pentostatin may have better effects in patients with chronic GVHD.
Thalidomide [139, 140] and more recently lenalidomide [141] have been studied in the treatment of GVHD. The initially positive results of treatment with thalidomide in chronic GVHD [139] were not confirmed in a randomized study [140]. The treatment of recurrent myeloma with lenalido-mide suggested an immune modulatory effect of lenalidomide in producing regulatory T cells [141].
Bortezomib has been tested in mice [142] and patients with HLA-mismatched unrelated donors [143]. The immunomodulatory effect has been related to the suppression of monocyte-derived dendritic cells and modified antigen presentation and release of TNF-a from CD4-positive T cells [142]. It has shown promising activity in the prophylaxis of GVHD [143].
After the description of activating antibodies against the receptor of platelet derived growth factor (PDGF) [144] in patients with systemic sclerosis similar antibodies were found in patients with sclerodermatous chronic GVHD [145] and several groups have treated sclerodermatous chronic GVHD [146, 147], as well as obliterating bronchiolitis with imatinib [148, 145]. In one study more than 70% of patients with sclerotic chronic GVHD responded with partial and complete remissions [147].
Cells
Many treatment regimens of GVHD favor the development of regulatory T cells characterized by the expression of CD 4 and CD25 in high density [149]. The suppressive activity is limited to cells of the CD4/CD25 immune phenotype that are positive for FoxP3 mRNA. Typically regulatory T cells should be negative for the IL7 receptor (CD127). Immunomagnetically selected regulatory T cells have been tested in vitro for immunosuppressive effects [149, 150], and preliminary applications for the treatment of refractory GVHD have been promising (M. Edinger, pers. comm.). The first results of preventive application have been reported (Di Ianni et al. ASH 2009); 17 of 20 evaluable patients did not produce GVHD after HLA-haploidentical stem cell transplantation despite admixture of a limited amount of conventional T cells to the CD34-selected graft.
More information is available on the treatment of refractory GVHD with mesenchymal stromal cells [76]. The results were confirmed in a multicenter study of the EBMT involving [151] 55 patients with steroid-refractory GVHD. Twenty-seven patients received one dose, 22 two doses and 6 three doses and more from HLA-mismatched or HLA-matched donors for treatment; 30 patients had a complete response, and an improvement was seen in 9 patients. Responders had a better chance of survival than non-responders. Mesenchymal stem cells have multiple properties including differentiation into bone, cartilage, tendon and muscle cells, repair of damaged tissue and modulation of immune responses [36].
UV light
Ultraviolet light has immunosuppressive properties [152]. UV-A in combination with 8-methoxypsoralen (PUVA) has been used to treat chronic GVHD [153]. UVA may be applied to the skin in combination with oral psoralen or with a bath in psoralen containing water. PUVA treatment was studied in 103 patients with steroid-resistant acute GVHD [154] with good res-ponses in GVHD of the skin and sparing of glucocorticoid doses. The treatment was well to-lerated, but it may induce a flare before lichenoid skin changes respond to the treatment. In chronic GVHD 31 of 40 patients had an improvement following PUVA treatment, but partial and complete responses were limited to the skin [155]. Best responses were seen in the liche-noid phases of chronic GVHD, and less in the sclerodermatous phases. However, the com-bination of PUVA bath with oral isotretinoin has been effective in a small study of scleroder-matous chronic GVHD: 11 of 14 patients responded, four of these with complete remission [156].
Alternatively PUVA may be applied directly to the blood resp. leukocytes separated by a dis-continuous blood cell separator (extracorporeal photopheresis, ECP). Responses to ECP have been reported for steroid-refractory, acute GVHD [157-159] and chronic GVHD [160]. Complete resolution of acute GVHD of the skin in 82%, liver in 61% and gut in 61% of pa-tients has been reported [158]. Response was associated with better survival. In our own study of 30 patients with acute GVHD, 20 patients responded with CR and PR defined as steroid discontinuation and reduction to 10 mg or less per day respectively (unpublished). Eleven of 20 responders survived as compared to only one non-responder. Steroid treatment was a major risk factor in the treatment of acute GVHD of pediatric patients [161]. In a single centre study on steroid refractory chronic GVHD 22% of patients could discontinue steroid therapy after one year, with response to ECP and absence of thrombocytopenia being the favorable factors for survival [160]. A randomized prospective multicentre study [162] comparing standard treatment with standard treatment plus ECP showed improvement of the skin score and sig-nificant steroid sparing. ECP is a good treatment option in patients with steroid-refractory acute and chronic GVHD with little side effects. The mechanism of the immunosuppression by ECP is not completely understood as only 5–10% of all T cells may be reached by extra-corporeal irradiation. However, a shift of dendritic cells from activating DC1 to down-regulating DC2 and from Th1 to Th2 has been described in the course of ECP [163]. Ex vivo a decrease of T cells producing pro-inflammatory cytokines was described [164]. In a murine model ECP-treated T cells induced regulatory T cells in recipients with established GVHD [165]. An increase in the proportion of regulatory T cells was observed in patients that responded to ECP [166]. Therefore ECP may be one method to induce GVH-tolerance without too many side effects.
Induction of graft-versus-host tolerance
Unlike transplantation of solid organs, transplantation of hematopoietic stem cells induces transplantation tolerance, enabling immunosuppressive therapy to be discontinued. In the form of central tolerance, lymphoid progenitor cells derived from transplanted stem cells tra-vel to the thymus where T cells tolerant to the host’s tissue are produced [167-169]. However, the thymus shows progressive involution in adulthood; central tolerance may be the major form of tolerance in children and young adults. The majority of patients subjected to stem cell transplantation are older, and the thymus has shrunk to a small remnant. Therefore in the majority of our patients a peripheral form of tolerance prevails, but function of the thymus can be recovered even in elderly individuals [170]. Several studies have been performed to speed up recovery of the thymus, mostly without convincing success [171], but new agents may give better results [172, 173, 169]. However, GVHD may affect the thymus [174] and thereby may inhibit the induction of central tolerance in both young and adult patients. Peripheral tolerance is a first step and may be replaced by central tolerance with time. The mechanisms of tolerance may be similar, clonal deletion, clonal anergy, and suppression.
Clonal deletion is a mechanism of self tolerance occurring in the thymus [175]; in the case of allogeneic stem cell transplantation T cells of donor origin derived from lymphoid progenitors may be eliminated by the same mechanism and primed towards host MHC antigens in se-miallogeneic hosts [176]. Deletion in the periphery may be accomplished by the treatment with antimetabolite drugs such as methotrexate, or cycle active drugs like cyclophosphamide; both of which have been shown to induce tolerance in stem cell transplanted patients [177, 178]. The principle of selective depletion of responsive lymphocytes has been applied more recently in HLA-haploidentical transplantation [179]. Unlike these cytotoxic agents calcineurin inhibitors do not kill the responsive cells, but inhibit cytokine production and thereby the progress of the immune response. However they may not favor the induction of tolerance; flares of GVHD have been observed after discontinuation of cyclosporin A, and late rejection of marrow grafts have been reported in single patients with aplastic anemia. Activation induced cell death (AICD) is a natural decrease of the clone size by IFN-g secretion of mature Th1 T cells and death of immature T cells, which may be achieved by the external pathway.
Clonal anergy may be the result of competitive inhibition by anergic T cells or active sup-pression by a variety of suppressor cells. Formerly, CD8-positive T cells were considered “cytotoxic/suppressor” cells, but the evidence for specific suppression was weak. Instead, several mechanisms of suppression have been described including “veto” cells suppressing the immune reaction against themselves [180]. The veto mechanism, described as the effector cells inhibiting or killing themselves has been primarily ascribed to CD8-positive T cells, but later also to other cells including stem cells. CD8-positive suppressor cells may not only func-tion as veto cells, but they may also suppress third party reactions by the secretion of FAS [181>]. Other cells with suppressor function are myeloid derived suppressor cells [182], NKT cells in the marrow [183], NK cells [184], dendritic cells type 2 [185] and mesenchymal stromal cells [76]; all of them suppress activated T cells more or less specifically. Some of these have already shown clinical effectiveness [183, 76], others are still in a developmental state. In recent years the detection of FoxP3 (forkhead transcription factors) showed suppressive function of CD4, CD25 positive T cells and even CD8 T cells [186]. Naïve CD4, CD25-positive regulatory T cells are able to down regulate allogeneic immune responses without inhibiting graft-versus-leukemia responses [75]. These may be naïve and non-specifically down regulating dendritic cells or adaptive and directed against specific antigen. Recently the Perugia group has reported the use of naïve regulatory T cells suppressing GVHD in patients given HLA-haploidentical transplants including small amounts of conventional T cells (ASH 2009, New Orleans).
Rapamycin exerts differential effects on T cells, inhibiting CD8 positive cells more than CD4 positive cells [86]; CD4 T cells spared by Rapamycin may become regulatory T cells without compromising GVL reactions [133]. Long-term observations of patients treated with Rapamycin and tacrolimus are encouraging with regard to control of acute GVHD and GVL [89]. Chronic GVHD still remains a problem despite tolerogenic effects of Rapamycin. Recently, the Milan group [187] (EBMT 2010) has reported generation of regulatory T cells in patients with HLA-haploidentical transplants. After conditioning with treosulfan, fludarabine, ATG and rituximab, and GVH prophylaxis with Rapamycin and mycophenolate mofetil, immune reconstitution was better than after transplantation of CD34-selected transplants, and regulatory T cells were detected early after transplantation.
Tolerogenic effects have also been described for the treatment with extracorporeal photo-pheresis (ECP) [188]. In acute GVHD ECP was applied with good results [158]. In most patients the effects of ECP are not immediate, but occur after some weeks. ECP has also beneficial effects against chronic GVHD [162] and may be preferable to other treatments for GVHD.
The main goal of prophylactic and therapeutic treatment of GVHD should be the induction of transplantation tolerance. Therefore treatment protocols interfering with tolerance should be avoided in protracted periods in favor of regimens allowing the development of tolerance. Glucocorticoids and calcineurin inhibitors are effective in controlling the acute disease, but they do not support the development of tolerance. Similarly, IL2-R antibodies may be effec-tive in the acute control of GVHD, but may not support the development of tolerance. Toler-ance may be achieved by depletion of mature T cells from the graft, killing of antigen respon-sive T cells with cell cycle active chemotherapy as Cyclophosphamide, methotrexate, or my-cophenolate mofetil, activating CTLA4 receptors by CTLA4-Ig or using drugs like Rapamycin that block the co-stimulatory pathway or ECP producing apoptotic cells that induce tolerance.
Future prospects
The time point to initiate treatment of acute and chronic GVHD is of paramount importance. Therefore, early diagnosis tests, before clinical diagnosis is possible, may improve the out-come significantly. Several proteins have been found in the urine of patients that developed GVHD [189]; a prospective study will help to demonstrate the value of early treatment. Similarly, elafin has been identified as a prognostic marker in the plasma of patients developing skin GVHD [190]. Early diagnosis will allow early treatment and thereby avoid the development of memory T cells or T stem cells with memory that are extremely difficult to suppress.
References
1. Barnes DHW, Loutit JF. Spleen protection: the cellular hypothesis. In: Bacq ZM and Alexander P: Radiobiology Symposium : Proceedings of the Symposium held at Liege, August-September, 1954. London: Butterworths, 1955:134-135.
2. Simonsen M, Jensen E. The graft-versus-host assay in transplantation chimeras. In: Albert F, Lejeune-Ledant G, eds. Biological problems of grafting. Oxford: Blackwell; 1959:214-236.
3. Uphoff, D. E. and Law, P. Genetic factors influencing irradiation protection by bone marrow. II. The histocompatibility 2 (H-2) locus. J Natl Cancer Inst 20, 617-624. 1958. pmid: 13539612.
4. van Bekkum, D. W. The selective elimination of immunologically competent cells from bone marrow and lymphatic cell mixtures. I.Effect of storage at 4°C. Transplantation 2, 393-404. 1964.
5. Billingham, RE. The biology of graft-versus-host reactions. Harvey Lect 1966-1967 62, 21-78. 1967. pmid: 4875305.
6. Mathé G, Amiel JL, Schwartzenberg L, et al. Successful allogeneic bone marrow transplantation in man: Chimerism, induced specific tolerance and possible antileukemic effects. Blood 1965;25:179-96. pmid: 14267694.
7. Epstein RB, Storb R, Ragde H, Thomas ED. Cytotoxic typing antisera for marrow grafting in littermate dogs. Transplantation 1968;6:45-58. pmid: 4866738.
8. Dausset J, Rapaport FT, Colombani J, Feingold N. A leucocyte group and its relationship to tissue histocompatibility in man. Transplantation 1965;3:701-705. pmid: 5324831.
9. van Rood JJ, van Leeuwen A, Eernisse JG, Frederiks E and Bosch LJ. Relationship of Leukocyte groups to tissue transplantation compatibility. Ann.N.Y.Acad.Sci. 1964;120:285-298.
10. Thomas ED, Storb R, Epstein RB, Rudolph RH. Symposium on bone marrow transplantation: experimental aspects in canines. Transplant.Proc. 1969;1:31-33. pmid: 5002661.
13. Korngold R, Sprent J. Surface markers of T cells causing lethal graft-vs-host disease to class I vs class II H-2 differences. J Immunol. 1985;135:3004-3010. pmid: 3876371.
14. Klein J, Sato A. The HLA system. First of two parts. N Engl J Med. 2000 Sep 7;343(10):702-9 .doi: 10.1056/NEJM200009073431006.
15. Klein J, Sato A. The HLA system. Second of two parts. N Engl J Med. 2000 Sep 14;343(11):782-6. Review. Erratum in: N Engl J Med 2000 Nov 16;343(20):1504. doi: 10.1056/NEJM200009143431106.
19. Ferrara JLM, Deeg HJ. Graft-versus-host disease. N Engl J Med 1991;324:667-674. doi: 10.1056/NEJM199103073241005.
21. Reinhardt, RL, Khoruts A, Merica R, Zell T, and Jenkins MK. Visualizing the generation of memory CD4 T cells in the whole body. Nature 410, 101-105. 2001. doi: 10.1038/35065111.
23. Kolb HJ, Mittermueller J, Holler E, et al. Treatment of recurrent chronic myelogenous leukemia posttransplant with interferone alpha (INFa) and donor leukocyte transfusions [abstract]. Blut. 1990;61:122.
24. Hessel H, Mittermuller J, Zitzelsberger H, Weier HU, Bauchinger M. Combined immunophenotyping and FISH with sex chromosome-specific DNA probes for the detection of Langerhans cells after sex-mismatched bone marrow transplantation. Histochem Cell Biol. 1996;106:481-485. pmid: 8950606.
25. Teshima T, Ordemann R, Reddy P, et al. Acute graft-versus-host disease does not require alloantigen expression on host epithelium. Nat Med. 2002;8:575-581. doi: 10.1038/nm0602-575.
26. Shlomchik WD, Couzens MS, Tang CB, et al. Prevention of graft versus host disease by inactivation of host antigen-presenting cells. Science 1999;285:412-415. pmid: 10411505. PDF: Free with Registration at http://www.sciencemag.org/content/285/5426/412.long
27. Matte CC, Liu J, Cormier J, et al. Donor APCs are required for maximal GVHD but not for GVL. Nat.Med. 2004;10:987-992. doi: 10.1038/nm1089.
28. Tutschka PJ, Hess AD, Beschorner WE, Santos GW. Suppressor cells in transplantation tolerance. I. Suppressor cells in the mechanism of tolerance in radiation chimeras. Transplantation 1981;32:203-209. pmid: 6456580.
29. Tutschka PJ, Ki PF, Beschorner WE, Hess AD, Santos GW. Suppressor cells in transplantation tolerance. II. maturation of suppressor cells in the bone marrow chimera. Transplantation 1981;32:321-325. pmid: 6460354.
30. Tutschka PJ, Hess AD, Beschorner WE, Santos GW. Suppressor cells in transplantation tolerance. III. The role of antigen in the maintenance of transplantation tolerance. Transplantation 1982;33:510-514. pmid: 6211807.
31. Weiden PL, Storb R, Tsoi M-S, et al. Infusion of donor lymphocytes into stable canine radiation chimeras: Implications for mechanism of transplantation tolerance. J.Immunol. 1976;116:1212-1219. pmid: 774975.
32. Kolb HJ, Günther W, Schumm M, et al. Adoptive immunotherapy in canine chimeras. Transplantation 1997;63:430-436. pmid: 9039935.
33. Zorn J, Herber M, Schwamberger S, et al. Tolerance in DLA-haploidentical canine littermates following CD6-depleted marrow transplantation and donor lymphocyte transfusion. Exp Hematol. 2009;37:998-1006. doi: 10.1016/j.exphem.2009.05.001.
34. Ruggeri L, Capanni M, Urbani E, et al. Effectiveness of donor natural killer cell alloreactivity in mismatched hematopoietic transplants. Science. 2002;295:2097-2100. doi: 10.1126/science.1068440.
36. Le BK, Ringden O. Mesenchymal stem cells: properties and role in clinical bone marrow transplantation. Curr.Opin.Immunol. 2006;18:586-591. doi: 10.1016/j.coi.2006.07.004 .
38. Gratwohl A, Brand R, Apperley J, et al. Graft-versus-host disease and outcome in HLA-identical sibling transplantations for chronic myeloid leukemia. Blood.doi: 10.1182/blood.V100.12.3877 2002;100:3877-3886.
39. Shlomchik WD. Graft-versus-host disease. Nat.Rev.Immunol. 2007;7:340-352. doi: 10.1038/nri2000.
40. Petersdorf EW, Malkki M. Genetics of risk factors for graft-versus-host disease. Semin.Hematol. 2006;43:11-23. doi: 10.1053/j.seminhematol.2005.09.002.
43. Petersdorf EW. Risk assessment in haematopoietic stem cell transplantation: histocompatibility. Best.Pract.Res.Clin.Haematol. 2007;20:155-170. doi: 10.1016/j.beha.2006.09.001.
47. Holler E, Rogler G, Herfarth H, et al. Both donor and recipient NOD2/CARD15 mutations associate with transplant-related mortality and GvHD following allogeneic stem cell transplantation. Blood. 2004;104:889-894. doi: 10.1182/blood-2003-10-3543.
48. Goulmy E. Human minor histocompatibility antigens: New concepts for marrow transplantation and adoptive immunotherapy. Immunol.Rev. 1997;157:125-140.
51. Glucksberg H, Storb R, Fefer A, et al. Clinical manifestations of graft-versus-host disease in human recipients of HL-A-matched sibling donors. Transplantation 1974;18:295-304. pmid: 4153799.
52. Kolb H, Sale GE, Lerner KG, Storb R, Thomas ED. Pathology of acute
graft-versus-host disease in the dog. An autopsy study of ninety-five dogs. Am J Pathol. 1979 Aug;96(2):581-94.
57. Sullivan KM, Deeg HJ, Sanders J, et al. Hyperacute graft-v-host disease in patients not given immunosuppression after allogeneic marrow transplantation. Blood. 1986;67:1172-1175. pmid: 3513869.
58. Rodt H, Netzel B, Brehm G, Thierfelder S. Production of antibodies specific for human thymus derived lymphocytes purified from antibodies crossreacting with colony-forming cells. Blut. 1974;29:416-422. pmid: 4548852.
59. Kolb HJ, Rieder I, Rodt H, et al. Antilymphocytic antibodies and marrow transplantation. VI. Graft- versus-host tolerance in DLA-incompatible dogs after in vitro treatment of bone marrow with absorbed antithymocyte globulin. Transplantation. 1979;27:242-245. pmid: 35870.
60. Rodt H, Thierfelder S, Bender-Gotze C, et al. Serological inhibition of graft versus host disease: recent results in 28 patients with leukemia. Haematol.Blood Transfus. 1983;28:92-96. pmid: 6345300.
61. Goldman JM, Apperley J, Jones L, et al. Bone marrow transplantation for patients with chronic myeloid leukemia. N Engl J Med 1986;314:202-207. pmid: 6345300.
63. Schumm M, Günther W, Kolb HJ, et al. Prevention of graft-versus-host disease in DLA-haplotype mismatched dogs and hemopoietic engraftment of CD6-depleted marrow with and without cG-CSF treatment after transplantation. Tissue Antigens 1994;43:170-178. pmid: 7522357.
64. Soiffer RJ, Ritz J. Selective T cell depletion of donor allogeneic marrow with anti-CD6 monoclonal antibody: rationale and results. Bone Marrow Transplant 1993;12 Suppl 3:S7-10. pmid: 8124262.
66. Guenther W, Kolb HJ, Schumm M, Thierfelder S, Wilmanns W. Suppressive- and veto-effect of canine bone marrow cells [abstract]. 3rd Int Vet Immun Symp Abstractbook 1992.
67. Goldman JM, Gale RP, Horowitz MM, et al. Bone marrow transplantation for chronic myelogenous leukemia in chronic phase: Increased risk of relapse associated with T-cell depletion. Ann.Intern.Med. 1988;108:806-814. pmid: 3285744.
68. Kolb HJ, Rodt H, Netzel B, et al. In vitro treatment of marrow with ATCG or Campath 1 for prophylaxis of GVHD - Results of the AG-KMT München. Exp Hematol 1985;13:147.
69. Finke J, Bethge WA, Schmoor C, et al. Standard graft-versus-host disease prophylaxis with or without anti-T-cell globulin in haematopoietic cell transplantation from matched unrelated donors: a randomised, open-label, multicentre phase 3 trial. Lancet Oncol. 2009;10:855-864.
75. Edinger M, Hoffmann P, Ermann J, et al. CD4+CD25+ regulatory T cells preserve graft-versus-tumor activity while inhibiting graft-versus-host disease after bone marrow transplantation. Nat.Med. 2003;9:1144-1150. pmid: 12925844.
76. Le BK, Rasmusson I, Sundberg B, et al. Treatment of severe acute graft-versus-host disease with third party haploidentical mesenchymal stem cells. Lancet. 2004;363:1439-1441. pmid: 15121408.
78. Kolb HJ, Simoes B, Hoetzl F, et al. CD6-negative mobilized blood cells facilitating HLA-haploidentical marrow transplantation for the treatment of high-risk hematopoietic neoplasia. [abstract]. Blood. 2002;100:637a.
80. White DJ, Lim SM. The induction of tolerance by cyclosporine. Transplantation 1988;46:118S-121S. pmid: 3043793.
82. Storb R, Deeg HJ, Whitehead J, et al. Methotrexate and cyclosporine compared with cyclosporine alone for prophylaxis of acute graft-versus-host disease after marrow transplantation for leukemia. N Engl J Med 1986;314:729-735. pmid: 3513012.
84. Seghal SN. Sirolimus: its discovery, biological properties, and mechanism of action. Transplant Proc 2003;35:7S-14S. pmid: 12742462.
85. Wells AD, Li XC, Li Y, et al. Requirement for T-cell apoptosis in the induction of peripheral transplantation tolerance. Nat Med 1999;5:1303-1307. pmid: 10545998.
88. Yu X, Carpenter P, Anasetti C. Advances in transplantation tolerance. Lancet 2001;357:1959-1963. pmid: 11425437.
92. Deeg HJ. How I treat refractory acute GVHD. Blood. 2007;109:4119-4126.
93. Bacigalupo A, van Lint MT, Frassoni F, et al. High dose bolus methylprednisolone for the treatment of acute graft versus host disease. Blut. 1983;46:125-132. pmid: 6337655.
96. Rhen T, Cidlowski JA. Antiinflammatory action of glucocorticoids--new mechanisms for old drugs. N.Engl.J.Med. 2005;353:1711-1723. pmid: 16236742.
98. Nijhuis EW, Hinloopen B, van Lier RA, Nagelkerken L. Differential sensitivity of human naive and memory CD4+ T cells for dexamethasone. Int.Immunol. 1995;7:591-595. pmid: 7547686.
100. Fan PT, Yu DT, Clements PJ, et al. Effect of corticosteroids on the human immune response: comparison of one and three daily 1 gm intravenous pulses of methylprednisolone. J.Lab Clin.Med. 1978;91:625-634. pmid: 76667.
102. Viard I, Wehrli P, Bullani R, et al. Inhibition of toxic epidermal necrolysis by blockade of CD95 with human intravenous immunoglobulin. Science. 1998;282:490-493. pmid: 9774279.
104. McDonald GB, Bouvier M, Hockenbery DM, et al. Oral beclomethasone dipropionate for treatment of intestinal graft-versus-host disease: a randomized, controlled trial. Gastroenterology. 1998;115:28-35. pmid: 9649455.
108. Knop S, Hebart H, Gratwohl A, et al. Treatment of steroid-resistant acute GVHD with OKT3 and high-dose steroids results in better disease control and lower incidence of infectious complications when compared to high-dose steroids alone: a randomized multicenter trial by the EBMT Chronic Leukemia Working Party. Leukemia. 2007;21:1830-1833. pmid: 17495972.
130. Hoda D, Pidala J, Salgado-Vila N, et al. Sirolimus for treatment of steroid-refractory acute graft-versus-host disease. Bone Marrow Transplant. 2009;45:1347-1351.
131. Ghez D, Rubio MT, Maillard N, et al. Rapamycin for refractory acute graft-versus-host disease. Transplantation 2009;88:1081-1087. pmid: 19898203.
133. Durakovic N, Radojcic V, Powell J, Luznik L. Rapamycin promotes emergence of IL-10-secreting donor lymphocyte infusion-derived T cells without compromising their graft-versus-leukemia reactivity. Transplantation 2007;83:631-640. pmid: 17353785.
134. Armand P, Gannamaneni S, Kim HT et al. Improved survival in lymphoma patients receiving sirolimus for graft-versus-host disease prophylaxis after allogeneic hematopoietic stem-cell transplantation with reduced-intensity conditioning. J Clin.Oncol. 2008;26:5767-5774. pmid: 19001324.
136. Schmitt T, Luft T, Hegenbart U, et al. Pentostatin for treatment of steroid-refractory acute GVHD: a retrospective single-center analysis. Bone Marrow Transplant. 2010 Jun 21. doi:10.1038/bmt.2010.146.
141. Lioznov M, El-Cheikh J Jr, Hoffmann F, et al. Lenalidomide as salvage therapy after allo-SCT for multiple myeloma is effective and leads to an increase of activated NK (NKp44(+)) and T (HLA-DR(+)) cells. Bone Marrow Transplant. 2010;45:349-353. pmid: 19584825.
151. Le BK, Frassoni F, Ball L, et al. Mesenchymal stem cells for treatment of steroid-resistant, severe, acute graft-versus-host disease: a phase II study. Lancet. 2008;371:1579-1586. pmid: 18468541.
152. Deeg HJ. Ultraviolet irradiation in transplantation biology. Manipulation of immunity and immunogenicity. Transplantation 1988;45:845-851. pmid: 3285528.
153. Hymes SR, Morison WL, Farmer ER, et al. Methoxsalen and ultraviolet A radiation in treatment of chronic cutaneous graft-versus-host reaction. J Am.Acad.Dermatol. 1985;12:30-37. pmid: 3980801.
155. Vogelsang GB, Wolff D, Altomonte V, et al. Treatment of chronic graft-versus-host disease with ultraviolet irradiation and psoralen (PUVA). Bone Marrow Transplant. 1996;17:1061-1067. pmid: 8807115.
161. Perotti C, Del Fante C, Tinelli C, et al. Extracorporeal photochemotherapy in graft-versus-host disease: a longitudinal study on factors influencing the response and survival in pediatric patients. Transfusion. 2010;50:1359-1369.
164. Bladon J, Taylor PC. Early reduction in number of T cells producing proinflammatory cytokines, observed after extracorporeal photopheresis, is not linked to apoptosis induction. Transplant Proc. 2003;35:1328-1332. pmid: 12826151.
166. Di Biaso I, Di Maio L, Bugarin C, et al. Regulatory T cells and extracorporeal photochemotherapy: correlation with clinical response and decreased frequency of proinflammatory T cells. Transplantation. 2009;87:1422-1425.
167. Ford CE, Micklem HS. The thymus and lymph-nodes in radiation chimaeras. Lancet 1963;1:359-362. pmid: 13958695.
168. Zinkernagel RM. Thymus and lymphohemopoietic cells: their role in T cell maturation in selection of T cells' H-2-restriction-specificity and in H-2 linked Ir gene control. Immunol Rev. 1978;42:224-270. pmid: 83701.
170. Steffens CM, Al Harthi L, Shott S, Yogev R, Landay A. Evaluation of Thymopoiesis Using T Cell Receptor Excision Circles (TRECs): Differential Correlation between Adult and Pediatric TRECs and Naive Phenotypes. Clin Immunol. 2000;97:95-101. pmid: 11027449.
171. Witherspoon RP, Sullivan KM, Lum LG, et al. Use of thymic grafts or thymic factors to augment immunologic recovery after bone marrow transplantation: brief report with 2 to 12 years' follow-up. Bone Marrow Transplant. 1988;3:425-435. pmid: 3056551.
172. Wils EJ, Cornelissen JJ. Thymopoiesis following allogeneic stem cell transplantation: new possibilities for improvement. Blood Rev. 2005;19:89-98. pmid: 15603912.
175. Pullen AM, Kappler JW, Marrack P. Tolerance to self antigens shapes the T-cell repertoire. Immunol Rev. 1989;107:125-139. pmid: 2522084.
176. Zinkernagel RM, Doherty PC. Restriction of in vitro T cell-mediated cytotoxicity in lymphocytic choriomeningitis within a syngeneic or semiallogeneic system. Nature. 1974;248:701-702. pmid: 4133807.
177. Thomas ED, Kasakura S, Cavins JA, Ferrebee JW. Marrow transplants in lethally irradiated dogs: The effect of Methotrexate on survival of the host and the homograft. Transplantation. 1963;1:571-574. pmid: 14071268.
178. Santos GW. Immunosuppression for clinical marrow transplantation. Semin.Hematol. 1974;11:341-351. pmid: 4151847.
180. Miller RG, Muraoka S, Claesson MH, Reimann J, Benveniste P. The veto phenomenon in T-cell regulation. Ann N Y Acad Sci. 1988;532:170-6. pmid: 2972242.
182. Gabrilovich DI, Nagaraj S. Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev.Immunol 2009;9:162-174. pmid: 19197294.
186. Kapp JA, Bucy RP. CD8+ suppressor T cells resurrected. Hum.Immunol 2008;69:715-720. pmid: 18817830.
187. Peccatori J, Clerici D, Forcina A, et al. In vivo T-regs generation by rapamycin-mycophenolate-ATG as a new platform for GVHD prophylaxis in T-cell repleted unmanipulated haploidentical peripheral stem cell transplantation: results in 59 patients [abstract]. EBMT Meeting Vienna. 2010. 2010;S3-S4.
190. Paczesny S, Braun TM, Levine JE et al. Elafin is a biomarker of graft-versus-host disease of the skin. Sci.Transl.Med 2010;2:13ra2. pmid: 20371463.
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "500" ["~SORT"]=> string(3) "500" ["CODE"]=> string(80) "bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu" ["~CODE"]=> string(80) "bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu" ["EXTERNAL_ID"]=> string(4) "1439" ["~EXTERNAL_ID"]=> string(4) "1439" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["ELEMENT_META_KEYWORDS"]=> string(0) "" ["ELEMENT_META_DESCRIPTION"]=> string(214) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманиюGraft-versus-host disease: from experiments to clinical insight" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(5938) "<p class="bodytext">Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов. <br /><br />Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний. <br /><br />Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ. </p> <p class="bodytext">Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки. </p> <h3>Ключевые слова</h3> <p>болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия </p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_META_TITLE"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_META_KEYWORDS"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_META_DESCRIPTION"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_PICTURE_FILE_ALT"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_PICTURE_FILE_TITLE"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_PICTURE_FILE_NAME"]=> string(84) "bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu-img" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(151) "Болезнь «трансплантат против хозяина»: от экспериментов к клиническому пониманию" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(84) "bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu-img" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(84) "bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu-img" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(84) "bolezn-transplantat-protiv-khozyaina-ot-eksperimentov-k-klinicheskomu-ponimaniyu-img" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(2) "80" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> bool(false) ["VALUE"]=> bool(false) ["DESCRIPTION"]=> bool(false) ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> bool(false) ["~DESCRIPTION"]=> bool(false) ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19106" ["VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19107" ["VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19108" ["VALUE"]=> string(22) "05/15/2012 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "05/15/2012 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19119" } ["VALUE"]=> array(1) { [0]=> string(4) "1383" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1383" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19113" ["VALUE"]=> array(2) { ["TEXT"]=> string(47) "<p>Хaнc-Иохем Кольб</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(35) "Хaнc-Иохем Кольб
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19114" ["VALUE"]=> array(2) { ["TEXT"]=> string(5938) "<p class="bodytext">Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов. <br /><br />Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний. <br /><br />Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ. </p> <p class="bodytext">Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки. </p> <h3>Ключевые слова</h3> <p>болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(5846) "Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов.
Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний.
Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ.
Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки.
Ключевые слова
болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19110" ["VALUE"]=> string(29) "10.3205/ctt-2012-en-000089.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2012-en-000089.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19116" ["VALUE"]=> array(2) { ["TEXT"]=> string(35) "<p>Hans-Jochem Kolb</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(23) "Hans-Jochem Kolb
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19117" ["VALUE"]=> array(2) { ["TEXT"]=> string(577) "<p>Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany</p> <p class="bodytext"><b>Correspondence</b><br> Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany <br> E-mail: <a href="javascript:linkTo_UnCryptMailto('qempxs.l1n1ospfDaif2hi');">h-j-kolb@<span style="display:none;">spam is bad</span>web.de</a> </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(475) "Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
Correspondence
Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
E-mail: h-j-kolb@web.de
The pathophysiology, prevention, and treatment of acute graft-versus-host disease (GVHD) occurring, mainly, after allogeneic hematopoietic stem cell transplantation (allo-HSCT), should be understood, in order to exploit its potential benefits while avoiding certain clinical risks. Many studies have shown haematopoietic cells to be primary targets, as well as skin, gut, and liver containing macrophage-derived cells. The latters produce pro-inflammatory cytokines that stimulate donor T cells and induce HLA class II antigens in host tissue. Dendritic cells (DCs) boost CD 8 cells to react against HLA class I peptides. Hence, GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. Polymorphic non-HLA proteins may also cause severe GVH reactions. The reactions against minor histocompatibility antigens require a longer phase of activation than reactions against MHC antigens.
The preconditions of acute GVHD (aGVHD) are given before transplantation (the s.c. “cytokine storm” liberated by intensive conditioning treatment and probable infections). However, in human patients, donor lymphocyte transfusion may produce GVHD without conditioning treatment. In general, the host’s immune system is continuously suppressed by the graft and; the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion, being also mediated by mesenchymal stromal cells, NK-T cells, and regulatory T cells. Selecting an HLA-identical sibling as donor was the major step towards successful HSCT (generally, definition of 10 HLA-loci is required to prevent severe GVHD). Several TNF-a and TNF-a receptor alleles are associated with an increased risk of GVHD. The well-known clinical features of aGVHD are also described, including skin, liver, and gut lesions. The issues of chronic GVHD are also described. Its clinical and pathological signs resemble autoimmune diseases in many aspects.
GVHD prophylaxis is well established, and should be used in any clinical setting. Special attention is given to T cell depletion and modern immunosuppressive therapies post-transplant. Current schedules of GVHD treatment are described including calcineurin inhibitors, and some novel suppressive drugs. The role of various treatment regimens is considered in view of regulatory T cell (Treg), mesenchymal stem cells and UV-A irradiation as possible means of GVHD management.
Special attention is drawn to induction of a graft-versus-host tolerance in clinical HSCT. In the majority of patients, the peripheral (thymus-independent) form of tolerance prevails. Specific selective effects of Rapamycin upon T cells are discussed.
Keywords
graft-versus-host disease, prophylaxis, treatment, conditioning therapy, dendritic cells, Т-lymphocytes, immune suppression, immune therapy
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19111" ["VALUE"]=> string(63) "Graft-versus-host disease: from experiments to clinical insight" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(63) "Graft-versus-host disease: from experiments to clinical insight" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(11) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19116" ["VALUE"]=> array(2) { ["TEXT"]=> string(35) "<p>Hans-Jochem Kolb</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(23) "Hans-Jochem Kolb
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(23) "Hans-Jochem Kolb
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19118" ["VALUE"]=> array(2) { ["TEXT"]=> string(3117) "<p class="bodytext">The pathophysiology, prevention, and treatment of acute graft-versus-host disease (GVHD) occurring, mainly, after allogeneic hematopoietic stem cell transplantation (allo-HSCT), should be understood, in order to exploit its potential benefits while avoiding certain clinical risks. Many studies have shown haematopoietic cells to be primary targets, as well as skin, gut, and liver containing macrophage-derived cells. The latters produce pro-inflammatory cytokines that stimulate donor T cells and induce HLA class II antigens in host tissue. Dendritic cells (DCs) boost CD 8 cells to react against HLA class I peptides. Hence, GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. Polymorphic non-HLA proteins may also cause severe GVH reactions. The reactions against minor histocompatibility antigens require a longer phase of activation than reactions against MHC antigens. <br /><br />The preconditions of acute GVHD (aGVHD) are given before transplantation (the s.c. “cytokine storm” liberated by intensive conditioning treatment and probable infections). However, in human patients, donor lymphocyte transfusion may produce GVHD without conditioning treatment. In general, the host’s immune system is continuously suppressed by the graft and; the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion, being also mediated by mesenchymal stromal cells, NK-T cells, and regulatory T cells. Selecting an HLA-identical sibling as donor was the major step towards successful HSCT (generally, definition of 10 HLA-loci is required to prevent severe GVHD). Several TNF-a and TNF-a receptor alleles are associated with an increased risk of GVHD. The well-known clinical features of aGVHD are also described, including skin, liver, and gut lesions. The issues of chronic GVHD are also described. Its clinical and pathological signs resemble autoimmune diseases in many aspects. <br /><br />GVHD prophylaxis is well established, and should be used in any clinical setting. Special attention is given to T cell depletion and modern immunosuppressive therapies post-transplant. Current schedules of GVHD treatment are described including calcineurin inhibitors, and some novel suppressive drugs. The role of various treatment regimens is considered in view of regulatory T cell (Treg), mesenchymal stem cells and UV-A irradiation as possible means of GVHD management. <br /><br />Special attention is drawn to induction of a graft-versus-host tolerance in clinical HSCT. In the majority of patients, the peripheral (thymus-independent) form of tolerance prevails. Specific selective effects of Rapamycin upon T cells are discussed.</p> <h3>Keywords</h3> <p>graft-versus-host disease, prophylaxis, treatment, conditioning therapy, dendritic cells, Т-lymphocytes, immune suppression, immune therapy </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(3035) "The pathophysiology, prevention, and treatment of acute graft-versus-host disease (GVHD) occurring, mainly, after allogeneic hematopoietic stem cell transplantation (allo-HSCT), should be understood, in order to exploit its potential benefits while avoiding certain clinical risks. Many studies have shown haematopoietic cells to be primary targets, as well as skin, gut, and liver containing macrophage-derived cells. The latters produce pro-inflammatory cytokines that stimulate donor T cells and induce HLA class II antigens in host tissue. Dendritic cells (DCs) boost CD 8 cells to react against HLA class I peptides. Hence, GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. Polymorphic non-HLA proteins may also cause severe GVH reactions. The reactions against minor histocompatibility antigens require a longer phase of activation than reactions against MHC antigens.
The preconditions of acute GVHD (aGVHD) are given before transplantation (the s.c. “cytokine storm” liberated by intensive conditioning treatment and probable infections). However, in human patients, donor lymphocyte transfusion may produce GVHD without conditioning treatment. In general, the host’s immune system is continuously suppressed by the graft and; the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion, being also mediated by mesenchymal stromal cells, NK-T cells, and regulatory T cells. Selecting an HLA-identical sibling as donor was the major step towards successful HSCT (generally, definition of 10 HLA-loci is required to prevent severe GVHD). Several TNF-a and TNF-a receptor alleles are associated with an increased risk of GVHD. The well-known clinical features of aGVHD are also described, including skin, liver, and gut lesions. The issues of chronic GVHD are also described. Its clinical and pathological signs resemble autoimmune diseases in many aspects.
GVHD prophylaxis is well established, and should be used in any clinical setting. Special attention is given to T cell depletion and modern immunosuppressive therapies post-transplant. Current schedules of GVHD treatment are described including calcineurin inhibitors, and some novel suppressive drugs. The role of various treatment regimens is considered in view of regulatory T cell (Treg), mesenchymal stem cells and UV-A irradiation as possible means of GVHD management.
Special attention is drawn to induction of a graft-versus-host tolerance in clinical HSCT. In the majority of patients, the peripheral (thymus-independent) form of tolerance prevails. Specific selective effects of Rapamycin upon T cells are discussed.
Keywords
graft-versus-host disease, prophylaxis, treatment, conditioning therapy, dendritic cells, Т-lymphocytes, immune suppression, immune therapy
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(3035) "The pathophysiology, prevention, and treatment of acute graft-versus-host disease (GVHD) occurring, mainly, after allogeneic hematopoietic stem cell transplantation (allo-HSCT), should be understood, in order to exploit its potential benefits while avoiding certain clinical risks. Many studies have shown haematopoietic cells to be primary targets, as well as skin, gut, and liver containing macrophage-derived cells. The latters produce pro-inflammatory cytokines that stimulate donor T cells and induce HLA class II antigens in host tissue. Dendritic cells (DCs) boost CD 8 cells to react against HLA class I peptides. Hence, GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. Polymorphic non-HLA proteins may also cause severe GVH reactions. The reactions against minor histocompatibility antigens require a longer phase of activation than reactions against MHC antigens.
The preconditions of acute GVHD (aGVHD) are given before transplantation (the s.c. “cytokine storm” liberated by intensive conditioning treatment and probable infections). However, in human patients, donor lymphocyte transfusion may produce GVHD without conditioning treatment. In general, the host’s immune system is continuously suppressed by the graft and; the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion, being also mediated by mesenchymal stromal cells, NK-T cells, and regulatory T cells. Selecting an HLA-identical sibling as donor was the major step towards successful HSCT (generally, definition of 10 HLA-loci is required to prevent severe GVHD). Several TNF-a and TNF-a receptor alleles are associated with an increased risk of GVHD. The well-known clinical features of aGVHD are also described, including skin, liver, and gut lesions. The issues of chronic GVHD are also described. Its clinical and pathological signs resemble autoimmune diseases in many aspects.
GVHD prophylaxis is well established, and should be used in any clinical setting. Special attention is given to T cell depletion and modern immunosuppressive therapies post-transplant. Current schedules of GVHD treatment are described including calcineurin inhibitors, and some novel suppressive drugs. The role of various treatment regimens is considered in view of regulatory T cell (Treg), mesenchymal stem cells and UV-A irradiation as possible means of GVHD management.
Special attention is drawn to induction of a graft-versus-host tolerance in clinical HSCT. In the majority of patients, the peripheral (thymus-independent) form of tolerance prevails. Specific selective effects of Rapamycin upon T cells are discussed.
Keywords
graft-versus-host disease, prophylaxis, treatment, conditioning therapy, dendritic cells, Т-lymphocytes, immune suppression, immune therapy
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19110" ["VALUE"]=> string(29) "10.3205/ctt-2012-en-000089.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2012-en-000089.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2012-en-000089.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19111" ["VALUE"]=> string(63) "Graft-versus-host disease: from experiments to clinical insight" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(63) "Graft-versus-host disease: from experiments to clinical insight" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(63) "Graft-versus-host disease: from experiments to clinical insight" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19117" ["VALUE"]=> array(2) { ["TEXT"]=> string(577) "<p>Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany</p> <p class="bodytext"><b>Correspondence</b><br> Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany <br> E-mail: <a href="javascript:linkTo_UnCryptMailto('qempxs.l1n1ospfDaif2hi');">h-j-kolb@<span style="display:none;">spam is bad</span>web.de</a> </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(475) "Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
Correspondence
Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
E-mail: h-j-kolb@web.de
Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
Correspondence
Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
E-mail: h-j-kolb@web.de
Хaнc-Иохем Кольб
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(35) "Хaнc-Иохем Кольб
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19106" ["VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "11/10/2010 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19107" ["VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "11/10/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "11/10/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19108" ["VALUE"]=> string(22) "05/15/2012 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "05/15/2012 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "05/15/2012 12:00:00 am" } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19114" ["VALUE"]=> array(2) { ["TEXT"]=> string(5938) "<p class="bodytext">Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов. <br /><br />Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний. <br /><br />Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ. </p> <p class="bodytext">Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки. </p> <h3>Ключевые слова</h3> <p>болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(5846) "Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов.
Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний.
Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ.
Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки.
Ключевые слова
болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(5846) "Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов.
Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний.
Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ.
Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки.
Ключевые слова
болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия
" } } } [7]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "80" ["~IBLOCK_SECTION_ID"]=> string(2) "80" ["ID"]=> string(4) "1425" ["~ID"]=> string(4) "1425" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(143) "Трансплантация клеток пуповинной крови для лечения неопухолевых заболеваний" ["~NAME"]=> string(143) "Трансплантация клеток пуповинной крови для лечения неопухолевых заболеваний" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "09/27/2017 11:37:50 am" ["~TIMESTAMP_X"]=> string(22) "09/27/2017 11:37:50 am" ["DETAIL_PAGE_URL"]=> string(126) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-kletok-pupovinnoy-krovi-dlya-lecheniya-neopukholevykh-zabolevaniy/" ["~DETAIL_PAGE_URL"]=> string(126) "/en/archive/tom-2-nomer-3-7/obzornye-stati/transplantatsiya-kletok-pupovinnoy-krovi-dlya-lecheniya-neopukholevykh-zabolevaniy/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(51948) "Since the first related donor umbilical cord blood (UCB) transplant in 1988 for a patient with Fanconi anemia, and the first successful unrelated donor UCB transplant in 1993, an estimated 15,000 UCB transplantations have been performed [23]. Today, this approach is being applied to patients of all ages with a variety of diseases, including nonmalignant hematologic disorders and congenital metabolic disorders, as well as hematologic malignancies [2, 15, 16]. Between 2004 and 2007, the Center for International Blood and Marrow Transplant Research (CIBMTR) reported that for patients under age 20 years, 40% of unrelated donor stem cell grafts were collected from the bone marrow, 40% from umbilical cord blood, and 20% from peripheral blood. In contrast, for patients over age 20 years, only 7% of unrelated stem cell grafts were derived from UCB during the same time period. There are a number of factors contributing to increased usage of UCB stem cells. The most important factor is that results with UCB have improved progressively.
Furthermore, the cord blood banking infrastructure has improved, allowing for increased availability of high quality unrelated UCB. Compared to stem cell grafts obtained from unrelated adult donors, UCB stem cells can be procured more quickly, without risk or inconvenience to the donor. Finally, there is the possibility that contained within the UCB are totipotential stem cells with regenerative potential for non-hematopoietic tissues [23, 38]. This is particularly relevant when treating inborn errors of metabolism, which can result in damage to neuronal tissue.
This review will focus on the use of UCB transplantation to treat inherited or acquired hematopoietic disorders. Included are inborn errors of metabolism, in which promising outcomes have been demonstrated with allogeneic stem cell transplantation. As a group, bone marrow failure and congenital immunodeficiency disorders, as well as inborn errors of metabolism are rare. As a result, the worldwide experience with UCB transplantation is limited. Despite this, it is clear that UCB has proven to be a viable and effective stem cell source that will continue to play a major role in allogeneic stem cell therapy.
Use of UCB stem cell grafts for allogeneic transplantation; historical perspective
The 1988 report of successful engraftment and outcome of a patient with Fanconi anemia who was transplanted with cord blood from a new-born HLA-identical sibling, generated considerable interest in further development of this novel transplant approach [15]. From 1988 until 1993, UCB transplants were limited to grafts collected from HLA-identical related donors. This early experience was important in that it confirmed the pre-clinical observation that contained within the UCB graft were true pluripotent long-term repopulating cells. What also became apparent from the early experience was that the graft vs host disease (GvHD)-inducing potential of HLA-matched related cord blood T-cells was less than been observed with similarly matched bone marrow grafts [37,47]. The encouraging results in matched related donor cord blood transplantation prompted Kurtzberg and colleagues to perform the first mismatched cord blood transplantation [24]. This series of three patients and the larger series later reported by Wagner and colleagues were notable for the engraftment potential and low GvHD potential of these unrelated, cryopreserved cells [24, 48]. Due to the limited number of stem cells contained within the cord blood graft, early experience was restricted primarily to children where the UCB cell dose relative to body weight was more favorable. However, as promising outcome data began to emerge from large UCB bank and international registry studies, the experience in adult patients began to grow.
In recent years, great strides have been made in identifying factors predictive of successful outcome. The two most important characteristics of an UCB graft are the cellular content and donor-recipient HLA-matching. It is generally accepted that a total nucleated cell dose under 2 x 107/kg recipient body weight results in an unacceptably high rate of graft failure. CD34+ cell content and colony forming unit potential of the donor graft have also proven to be predictive of donor cell engraftment [25]. However, practical issues surrounding accurate characterization of prospective units for their progenitor cell content remain to be worked out. For example, while CD34+ cell content is often enumerated by individual cord blood banks prior to cryopreservation, there remains considerable concern that inter-bank comparison of these values is not valid due to subtle differences in CD34+ quantification techniques. Therefore, choosing cord blood units based on CD34+ cell content as measured by different banks is not yet realistic.
As the outcome data are presented in this review, it is important to remember that earlier results were significantly compromised by lack of a clear understanding of the many factors that contribute to successful UCB transplantation. While advances in supportive care, patient selection, and transplantation techniques have improved outcomes of allogeneic stem cell transplantation as a whole, the advances are more pronounced with UCB transplantation.
Umbilical cord blood transplantation for inherited immunodeficiency disorders
Lymphoid immunodeficiency disorders
Severe Combined Immunodeficiency Disorders (SCID)
Included in this discussion of UCB transplantation for SCID will be the classical form of SCID characterized by an X-linked mutation of the common gamma-chain, adenosine deaminase deficient SCID, autosomal recessive SCID, and Omenn syndrome. Data on cord blood transplantation for treatment of these disorders remain scant. The largest single center series comes from Diaz de Heredia and colleagues who report the outcomes of 12 SCID patients (median age 11.6 months) transplanted with UCB at three Spanish hospitals between 1996 and 2002 [10]. All but 2 patients received a high dose busulfan/cyclophosphamide preparative regimen. Two patients received a reduced intensity melphalan/fludarabine preparative regimen. All patients achieved donor stem cell engraftment. The 5-year overall survival (which includes 3 additional patients with non-SCID immunodeficiency disorders) was 73%, with 3 patients dying from graft versus host disease, and one from progressive interstitial lung disease. Importantly, all surviving children had normal age-adjusted levels of T-cells, B-cells and NK cells by 24 months following transplantation. In contrast to what has been observed following stem cell transplantation without conditioning, quantitative and qualitative T-cell and B-cell functions are durable following UCB transplantation using high intensity transplant conditioning.
The outcomes of 16 children transplanted with UCB for treatment of SCID are reported in three separate retrospective reports [5, 22, 45]. One of 16 failed to engraft, and 13 of 16 are long-term survivors with normalization of immune function.
Wiscott-Aldrich Syndrome
Wiscott-Aldrich Syndrome (WAS) is due to an X-linked mutation in the WASP gene, with an incidence of 4 per million live male births. The role of stem cell transplantation for treatment of this disorder has been firmly established. The initial reports demonstrated cure rates as high as 89% when matched unrelated donor transplantation is performed before the age of 5 years [13]. The published experience of UCB transplantation for WAS has grown significantly in the past few years. In 2003, Knutsen and colleagues were among the first to demonstrate feasibility of UCB transplantation for WAS with successful treatment of 3 children age 2–8 yrs [21]. More recently, the Duke University group reported the outcome of 15 patients transplanted with UCB between 1998 and 2007 [42]. All patients achieved donor cell engraftment following a conditioning regimen consisting of busulfan, cyclophosphamide, +/- ATG. Six of 15 patients died from transplant-related complications, resulting in an overall survival of 60%. Chronic GvHD was observed in 11 of 12 surviving patients (limited in 10, extensive in 1). The authors found this incidence of chronic GvHD to be in excess of what has been observed in other patients with congenital immunodeficiency disorders transplanted with UCB. They postulate a potential link to pre-existing eczema, which is commonly seen in patients with WAS.
A recent review of registry data collected by the CIBMTR (unpublished) compared 113 WAS recipients of unrelated bone marrow with 65 WAS recipients of unrelated cord blood transplants carried out between 1995 and 2005. This analysis showed equivalent 3-year survival for recipients age <5 years at the time of transplantation (73% vs 75%). Taken together, these data support the use of UCB for stem cell transplantation of WAS.
The CIBMTR has received registration reports of UCB transplantation for other rare lymphoid immunodeficiency disorders. These include Cartilage Hair Hypoplasia, X-linked Lymphoproliferative syndrome, Common Variable Immunodeficiency, Reticular dysgenesis and Bare Lymphocyte syndrome. Unfortunately, the outcomes of these transplants are not available for review.
Myeloid immunodeficiency disorders
Chronic Granulomatous Disease (CGD)
CGD is a congenital neutrophil disorder that is a consequence of an X-linked or autosomal recessive mutation in the NADPH-oxidase complex. The curative potential of stem cell transplantation has been clearly demonstrated [17, 40]. There are 8 reported cases of UCB transplantation for CGD [4, 31, 32, 35, 43]. Reduced intensity conditioning was successfully used in the oldest patient of this compilation of reports (age 20 yrs). The others were conditioned with high intensity regimen; 2 experienced primary graft failure. Six of 8 patients are long-term survivors.
Leukocyte adhesion deficiency is another life-threatening myeloid immune disorder. To date, there are no published reports of UCB transplantation for treatment of this disorder.
Immune/Inflammatory disorders
Hemophagocytic Lymphohistiocytosis (HLH)
The familial or inherited form of HLH as well as the EBV-associated HLH will be considered together in this review. In general, the outcomes of allogeneic stem cell transplantation following high dose conditioning, regardless of the stem cell source, are not as favorable as that observed for other inherited immunodeficiencies. This has prompted a movement toward the use of reduced intensity preparative regimens for this disorder [8]. Ohga and colleagues recently reviewed data from the Japanese Society of Pediatric Hematology [34]. Outcomes of 57 patients (familial HLA-43, EBV-associated HLH-14), 21 of whom received UCB grafts, are reported. The overall survival by log-rank analysis of the UCB transplant recipients was 66%, which did not differ from recipients of related or unrelated bone marrow or peripheral blood stem cell transplantation.
Chediak-Higashi
The team from the University of California at Los Angeles has reported in abstract form successful UCB transplantation of 3 patients with Chediak-Higashi. Limited information is available on long-term outcome [50].
Umbilical cord blood transplantation for inborn errors of metabolism
Current data supports the use of allogeneic stem cell transplantation for the treatment of lysosomal and peroxisomal storage disorders. Enzyme replacement therapies are currently available, but questions remain as to the long-term efficacy of these therapies and their ability to positively impact the natural history of the disorder. Stem cell transplantation provides the opportunity for enzyme replacement via “cross correction” of enzyme-deficient cells by neighboring donor derived, enzyme-replete cells [9, 20]. Furthermore, stem cell transplantation (and UCB transplantation in particular) provides the potential for repair of damaged non-hematopoietic tissue such as microglial cells in the brain and Kupffer cells in the liver via differentiation of tissue-specific progenitor cells or transdifferentiation.
Lysosomal and peroxisomal storage diseases affect multiple organ systems, with the central and peripheral nervous system particularly impacted. Depending on the extent of damage at the time of stem cell transplantation, the impact of allogeneic SCT may require extensive and sophisticated neurocognitive testing to objectively measure response. It is clear that many of the neurocognitive deficits incurred by the patients will not be corrected by stem cell transplantation. However, a plateau in survival appears to be evident from a large, single center series of UCB transplants for inherited metabolic disorders [36, Fig. 3]. Longer follow-up and more experience will be required to optimize the timing and impact of this treatment modality.
Krabbe’s disease
The potential for UCB transplantation to favorably impact on the natural history of inborn errors of metabolism was elegantly demonstrated by Escolar and colleagues in patients with Krabbe’s disease [11]. Children born with Krabbe’s disease are deficient of the lysosomal enzyme galactocerebrosidase. As a result, the children experience rapidly progressive neurologic deterioration and death at an early age. Escolar et al found that when children undergo UCB transplantation prior to the onset of symptoms, most will go on to have age-appropriate cognitive and motor function, along with 100% overall survival. Those who underwent UCB transplantation after the onset of symptoms showed little improvement in neurologic function and had an overall survival of only 43%. The study demonstrates the importance of early recognition of inborn errors along with early intervention with stem cell transplantation before irreversible damage occurs.
Hurler’s syndrome
Hurler’s syndrome is an autosomal recessive mucopolysaccharidosis caused by deficiency of alpha-L-iduronidase. Multiple organs, including the central nervous system, heart, bone, eyes, and liver are affected. Although enzyme replacement therapy has been available since 2003, due to poor CNS penetration, it does not completely prevent neurologic deterioration. Therefore, allogeneic stem cell transplantation remains the treatment of choice. Both European and North American registry data suggest that over 500 patients with Hurler’s syndrome have been treated with allogeneic stem cell transplantation. Staba and colleagues reported the Duke University experience with UCB transplantation for 20 children with Hurler’s syndrome [41]. The patients were prepared with high dose conditioning and received UCB units from mismatched unrelated donors. The median cell dose was 8.8x107 nucleated cells/kg. Only one patient failed to engraft with donor cells. Long-term survival was achieved in 17 of 20 patients with all surviving patients having normal alpha-L-iduronidase activity. Many of the surviving children continue to have neurocognitive impairment. Despite this, 81% of the surviving school-age children attend school in age-appropriate classrooms [36]. However, many Hurler’s patients continue to have problems with skeletal deformities that require corrective surgery.
Boelens and colleagues reviewed data from the European Blood and Marrow Transplant Registry regarding outcome of patients with Hurler’s syndrome undergoing allogeneic transplantation [6]. While overall survival was not affected by cell source selection, the data suggested that UCB grafts significantly improved the chance for achieving full donor chimerism and, as a result, normal circulating enzyme levels compared to patients receiving peripheral blood or bone marrow grafts.
X-linked Adrenoleukodystrophy (X-ALD)
X-ALD is a peroxisomal disorder stemming from a defective ABCD1 gene. This results in accumulation of long chain fatty acids, which has devastating neurologic consequences. The therapeutic potential of UCB transplantation was best described by Beam and colleagues who report the outcomes of 12 boys, 3 of whom were transplanted early in life, before symptoms of the disease developed [3]. All patients received high dose conditioning with busulfan, cyclophosphamide, and anti-thymocyte globulin followed by partially matched unrelated UCB transplantation. Extensive baseline neurophysiologic, neuroimaging and neurodevelopmental testing was performed prior to transplantation and followed serially after the transplantation. One patient died early from toxicity and another experienced primary graft failure, but was rescued with a second transplant. Overall survival at 6 months was 67%. The authors found that the degree of pre-transplant ALD-associated brain involvement (Loes score) was a strong predictor of post-transplantation cognitive and motor outcome. Many of the patients with severe neurocognitive impairment at the time of transplantation experienced disease progression despite transplantation. In contrast, the 3 boys who were asymptomatic at the time of transplant had excellent outcomes.
Composite reports of UCB transplantation for rare inborn errors
Disease-specific reports of allogeneic transplantation for rare inborn errors of metabolism lack the detail or sample size to draw definitive conclusions about outcomes [30, 36, 44]. Table 1 lists the disorders that have been treated with UCB transplantation. Questions remain as to the appropriate timing for the transplant as well as the therapeutic benefit. It is for this reason that use of allogeneic SCT for treatment of many of these disorders remains investigational.
Table 1. Inborn metabolism errors treated with umbilical cord blood transplantation
|
Hurler syndrome |
|
Krabbe's disease |
|
Sanfilippo syndrome |
|
Metachromatic leukodystrophy |
|
Adrenoleukodystrophy |
|
Tay Sachs disease |
|
Hunter syndrome |
|
Lesch-Nyhan disease |
|
Sandhoff disease |
|
Hurler Scheie |
|
Neimann-Pick |
|
Alpha mannosidosis |
|
GM1 gangliosidosis |
|
I-cell disease |
|
Maroteaux-Lamy syndrome |
|
Pelizaeus-Merzbacher disease |
|
Fucosidosis |
|
Wolman disease (Acid Lipase Deficiency) |
The common theme among all the reports is that the earlier the transplant is done, the better the outcome. In the largest of these composite reports from the Duke University group, 159 children representing 16 different inborn errors of metabolism were transplanted following high dose conditioning (busulfan, cyclophosphamide, and equine anti-thymocyte globulin) over a 12-year period, ending in 2007. The probability of engraftment, acute and chronic GvHD, overall survival and factors influencing survival has been shown [36, Fig. 1]. Of note, the 1 and 5 year overall survivals for the most common disorders treated on the study (Hurler, Hunter, and Sanfilippo syndrome, metachromatic leukodystrophy, and adrenoleukodystrophy) were all similar. This suggests that timing of the transplant, not the underlying disease, is most important in predicting outcome.
Umbilical cord blood transplantation for hemoglobinopathies
Related UCB transplantation for β-thalassemia and sickle cell disease
Unlike the situation with inborn errors of metabolism, there is an established role for allogeneic stem cell transplantation for the treatment of β-thalassemia and sickle cell disease [27, 28, 49]. The published experience of UCB transplantation for β-thalassemia remains quite limited [12, 26]. The largest report comes from the Eurocord registry data describing the outcome of 33 β-thalassemia patients transplanted with matched related UCB grafts [26]. All patients had a low disease severity (Pesaro 1 in 20 pts, Pesaro 2 in 13 pts). All patients received high dose e conditioning and GvHD prophylaxis with cyclosporine alone or combined with methotrexate. Seven of 33 patients experienced graft failure, but were rescued with either autologous stem cells or bone marrow from the original matched sibling cord blood donor at a later date. With a median follow-up of 24 months, all 33 patients were alive and well, but 4 retained the β-thalassemia phenotype.
The Locatelli report also included outcomes of 11 patients with sickle cell disease transplanted with UCB from related donors matched 6/6 (9 pts) or 5/6 (2 pts) [26]. The conditioning and GvHD prophylaxis regimens were similar to those used for the β-thalassemia patients. Primary engraftment was achieved in 10 of 11 patients, and all 11 patients are alive and well (1 with sickle cell disease) with a median follow-up of 24 months.
Unrelated UCB transplantation for β-thalassemia and sickle cell disease
There has yet to be enough published experience with unrelated UCB transplantation for β-thalassemia or sickle cell disease to fully assess the risk versus benefit considerations. The relative dearth of reports in the literature likely portrays unresolved challenges that remain with this mode of therapy. The few available reports suggest feasibility of unrelated UCB transplantation for hemoglobinopathies [1, 18, 19, 46]. However, it appears that establishment of stable donor engraftment is more challenging in this population of patients [1]. This may be related to the chemotherapy naïve status of the patients combined with a highly proliferative, cellular bone marrow milieu.
Umbilical cord blood transplantation for bone marrow failure disorders
The published experience with UCB for treatment of acquired bone marrow failure disorders is outlined in Table 2. Most investigators have relegated UCB transplantation to a treatment of last resort. Thus, those transplanted with UCB represent an extremely high-risk subset of patients who have failed prior therapy. Interpretation of the data is further compromised by the heterogeneous transplantation techniques. The data suggests that UCB transplantation for severe aplastic anemia is feasible. Larger studies will be needed to garner a better understanding of the relative risk of graft failure compared to patients with other non-malignant or malignant disorders.
Table 2. Umbilical cord blood transplantation for treatment of severe aplastic anemia and paroxysmal nocturnal hemoglobinurea
|
Reference |
Disorder- |
Median |
Preparative |
Median |
Percent |
Outcome |
|---|---|---|---|---|---|---|
|
(Mao, |
AA-9 |
25 |
Cy/ATG |
2.19 (1.6-10.7)* |
78 |
EFS-78 OS-78 |
|
(Ohga, |
AA-1 |
11 |
TBI-5Gy |
3.9 |
100 |
EFS-100 OS-100 |
|
(Chan, |
AA-9 |
9 |
Cy/ATG-2 |
5.4 (3.5-20) |
67 |
EFS-67 OS-78
|
|
(Yoshimi, |
AA-31 |
28 |
TBI (4-5Gy)/Flu/Mel-12 |
NA |
55 |
OS (2yrs)-41 |
|
(Ruggeri, |
SAA-4 PNH-1 |
19 |
Bu/Cy/Flu-3 |
4.7 (2.9-9.7) (Dual Cord Blood Graft) |
80 |
EFS-60 OS-80 |
*Post-thaw cell dose (cryopreserved cell dose not reported)
References
12. Fang, J., Huang, S., Chen, C., Zhou, D., Li, C.K., Li, Y. & Huang, K. (2004) Umbilical cord blood transplantation in Chinese children with beta-thalassemia. J Pediatr Hematol Oncol, 26, 185-189.
15. Gluckman, E., Broxmeyer, H.A., Auerbach, A.D., Friedman, H.S., Douglas, G.W., Devergie, A., Esperou, H., Thierry, D., Socie, G., Lehn, P. & et al. (1989, now open access in this issue of CTT) Hematopoietic reconstitution in a patient with Fanconi's anemia by means of umbilical-cord blood from an HLA-identical sibling. N Engl J Med, 321, 1174-1178.
21. Knutsen, A.P., Steffen, M., Wassmer, K. & Wall, D.A. (2003) Umbilical cord blood transplantation in Wiskott Aldrich syndrome. J Pediatr, 142, 519-523.
22. Knutsen, A.P. & Wall, D.A. (2000) Umbilical cord blood transplantation in severe T-cell immunodeficiency disorders: two-year experience. J Clin Immunol, 20, 466-476.
23. Kurtzberg, J. (2009) Update on umbilical cord blood transplantation. Curr Opin Pediatr, 21, 22-29.
24. Kurtzberg, J., Graham, M., Casey, J., Olson, J., Stevens, C.E. & Rubinstein, P. (1994) The use of umbilical cord blood in mismatched related and unrelated hemopoietic stem cell transplantation. Blood Cells, 20, 275-283; discussion 284.
28. Lucarelli, G., Galimberti, M., Polchi, P., Angelucci, E., Baronciani, D., Giardini, C., Politi, P., Durazzi, S.M., Muretto, P. & Albertini, F. (1990) Bone marrow transplantation in patients with thalassemia. N Engl J Med, 322, 417-421.
29. Mao, P., Zhu, Z., Wang, H., Wang, S., Mo, W., Ying, Y., Li, Q. & Xu, Y. (2005) Sustained and stable hematopoietic donor-recipient mixed chimerism after unrelated cord blood transplantation for adult patients with severe aplastic anemia. Eur J Haematol, 75, 430-435.
31. Mochizuki, K., Kikuta, A., Ito, M., Akaihata, M., Sano, H., Ohto, H. & Hosoya, M. (2009) Successful unrelated cord blood transplantation for chronic granulomatous disease: a case report and review of the literature. Pediatr Transplant, 13, 384-389.
32. Nakano, T., Boku, E., Yoshioka, A. & Fujimura, Y. (1999) A Case of McLeod Phenotype Chronic Granulomatous Disease who Received Unrelated Cord Blood Transplantation. Journal of Pediatric Hematology, 12, 264.
33. Ohga, S., Ichino, K., Goto, K., Hattori, S., Nomura, A., Takada, H., Nakamura, K. & Hara, T. (2006) Unrelated donor cord blood transplantation for childhood severe aplastic anemia after a modified conditioning. Pediatr Transplant, 10, 497-500.
34. Ohga, S., Kudo, K., Ishii, E., Honjo, S., Morimoto, A., Osugi, Y., Sawada, A., Inoue, M., Tabuchi, K., Suzuki, N., Ishida, Y., Imashuku, S., Kato, S. & Hara, T. (2009) Hematopoietic stem cell transplantation for familial hemophagocytic lymphohistiocytosis and Epstein-Barr virus-associated hemophagocytic lymphohistiocytosis in Japan. Pediatr Blood Cancer, 54, 299-306.
35. Parikh, S.H., Szabolcs, P., Prasad, V.K., Lakshminarayanan, S., Martin, P.L., Driscoll, T.A. & Kurtzberg, J. (2007) Correction of chronic granulomatous disease after second unrelated-donor umbilical cord blood transplantation. Pediatr Blood Cancer, 49, 982-984.
36. Prasad, V.K., Mendizabal, A., Parikh, S.H., Szabolcs, P., Driscoll, T.A., Page, K., Lakshminarayanan, S., Allison, J., Wood, S., Semmel, D., Escolar, M.L., Martin, P.L., Carter, S. & Kurtzberg, J. (2008) Unrelated donor umbilical cord blood transplantation for inherited metabolic disorders in 159 pediatric patients from a single center: influence of cellular composition of the graft on transplantation outcomes. Blood, 112, 2979-2989. Figure 3. Figure 1.
38. Rogers, I., Yamanaka, N., Bielecki, R., Wong, C.J., Chua, S., Yuen, S. & Casper, R.F. (2007) Identification and analysis of in vitro cultured CD45-positive cells capable of multi-lineage differentiation. Exp Cell Res, 313, 1839-1852.
42. Sun, J.M., Driscoll, T., Prasad, V.K., Parikh, S.H., Szabolcs, P., Kurtzberg, J. & Martin, P. (2009) Unrelated Umbilical Cord Blood Transplantation is an Effective Therapy for Wiskott-Aldrich Syndrome. Biol Blood Marrow Transplant, 15, 76.
43. Suzuki, N., Hatakeyama, N., Yamamoto, M., Mizue, N., Kuroiwa, Y., Yoda, M., Takahashi, J., Tani, Y. & Tsutsumi, H. (2007) Treatment of McLeod phenotype chronic granulomatous disease with reduced-intensity conditioning and unrelated-donor umbilical cord blood transplantation. Int J Hematol, 85, 70-72.
44. Tokimasa, S., Ohta, H., Takizawa, S., Kusuki, S., Hashii, Y., Sakai, N., Taniike, M., Ozono, K. & Hara, J. (2008) Umbilical cord-blood transplantations from unrelated donors in patients with inherited metabolic diseases: Single-institute experience. Pediatr Transplant, 12, 672-676.
46. Vanichsetakul, P., Wacharaprechanont, T., R, O.C., Seksarn, P. & Kupatawintu, P. (2004) Umbilical cord blood transplantation in children with beta-thalassemia diseases. J Med Assoc Thai, 87 Suppl 2, S62-67.
47. Wagner, J.E., Kernan, N.A., Steinbuch, M., Broxmeyer, H.E. & Gluckman, E. (1995) Allogeneic sibling umbilical-cord-blood transplantation in children with malignant and non-malignant disease.[see comment]. Lancet, 346, 214-219.
50. Wang, K., Lin, E., Moore, T. & Roberts, R. (2009) Cord Blood Transplantation for Treatment of Chediak-Higashi Syndrome. Clinical Immunology, 131, S77-S78.
Since the first related donor umbilical cord blood (UCB) transplant in 1988 for a patient with Fanconi anemia, and the first successful unrelated donor UCB transplant in 1993, an estimated 15,000 UCB transplantations have been performed [23]. Today, this approach is being applied to patients of all ages with a variety of diseases, including nonmalignant hematologic disorders and congenital metabolic disorders, as well as hematologic malignancies [2, 15, 16]. Between 2004 and 2007, the Center for International Blood and Marrow Transplant Research (CIBMTR) reported that for patients under age 20 years, 40% of unrelated donor stem cell grafts were collected from the bone marrow, 40% from umbilical cord blood, and 20% from peripheral blood. In contrast, for patients over age 20 years, only 7% of unrelated stem cell grafts were derived from UCB during the same time period. There are a number of factors contributing to increased usage of UCB stem cells. The most important factor is that results with UCB have improved progressively.
Furthermore, the cord blood banking infrastructure has improved, allowing for increased availability of high quality unrelated UCB. Compared to stem cell grafts obtained from unrelated adult donors, UCB stem cells can be procured more quickly, without risk or inconvenience to the donor. Finally, there is the possibility that contained within the UCB are totipotential stem cells with regenerative potential for non-hematopoietic tissues [23, 38]. This is particularly relevant when treating inborn errors of metabolism, which can result in damage to neuronal tissue.
This review will focus on the use of UCB transplantation to treat inherited or acquired hematopoietic disorders. Included are inborn errors of metabolism, in which promising outcomes have been demonstrated with allogeneic stem cell transplantation. As a group, bone marrow failure and congenital immunodeficiency disorders, as well as inborn errors of metabolism are rare. As a result, the worldwide experience with UCB transplantation is limited. Despite this, it is clear that UCB has proven to be a viable and effective stem cell source that will continue to play a major role in allogeneic stem cell therapy.
Use of UCB stem cell grafts for allogeneic transplantation; historical perspective
The 1988 report of successful engraftment and outcome of a patient with Fanconi anemia who was transplanted with cord blood from a new-born HLA-identical sibling, generated considerable interest in further development of this novel transplant approach [15]. From 1988 until 1993, UCB transplants were limited to grafts collected from HLA-identical related donors. This early experience was important in that it confirmed the pre-clinical observation that contained within the UCB graft were true pluripotent long-term repopulating cells. What also became apparent from the early experience was that the graft vs host disease (GvHD)-inducing potential of HLA-matched related cord blood T-cells was less than been observed with similarly matched bone marrow grafts [37,47]. The encouraging results in matched related donor cord blood transplantation prompted Kurtzberg and colleagues to perform the first mismatched cord blood transplantation [24]. This series of three patients and the larger series later reported by Wagner and colleagues were notable for the engraftment potential and low GvHD potential of these unrelated, cryopreserved cells [24, 48]. Due to the limited number of stem cells contained within the cord blood graft, early experience was restricted primarily to children where the UCB cell dose relative to body weight was more favorable. However, as promising outcome data began to emerge from large UCB bank and international registry studies, the experience in adult patients began to grow.
In recent years, great strides have been made in identifying factors predictive of successful outcome. The two most important characteristics of an UCB graft are the cellular content and donor-recipient HLA-matching. It is generally accepted that a total nucleated cell dose under 2 x 107/kg recipient body weight results in an unacceptably high rate of graft failure. CD34+ cell content and colony forming unit potential of the donor graft have also proven to be predictive of donor cell engraftment [25]. However, practical issues surrounding accurate characterization of prospective units for their progenitor cell content remain to be worked out. For example, while CD34+ cell content is often enumerated by individual cord blood banks prior to cryopreservation, there remains considerable concern that inter-bank comparison of these values is not valid due to subtle differences in CD34+ quantification techniques. Therefore, choosing cord blood units based on CD34+ cell content as measured by different banks is not yet realistic.
As the outcome data are presented in this review, it is important to remember that earlier results were significantly compromised by lack of a clear understanding of the many factors that contribute to successful UCB transplantation. While advances in supportive care, patient selection, and transplantation techniques have improved outcomes of allogeneic stem cell transplantation as a whole, the advances are more pronounced with UCB transplantation.
Umbilical cord blood transplantation for inherited immunodeficiency disorders
Lymphoid immunodeficiency disorders
Severe Combined Immunodeficiency Disorders (SCID)
Included in this discussion of UCB transplantation for SCID will be the classical form of SCID characterized by an X-linked mutation of the common gamma-chain, adenosine deaminase deficient SCID, autosomal recessive SCID, and Omenn syndrome. Data on cord blood transplantation for treatment of these disorders remain scant. The largest single center series comes from Diaz de Heredia and colleagues who report the outcomes of 12 SCID patients (median age 11.6 months) transplanted with UCB at three Spanish hospitals between 1996 and 2002 [10]. All but 2 patients received a high dose busulfan/cyclophosphamide preparative regimen. Two patients received a reduced intensity melphalan/fludarabine preparative regimen. All patients achieved donor stem cell engraftment. The 5-year overall survival (which includes 3 additional patients with non-SCID immunodeficiency disorders) was 73%, with 3 patients dying from graft versus host disease, and one from progressive interstitial lung disease. Importantly, all surviving children had normal age-adjusted levels of T-cells, B-cells and NK cells by 24 months following transplantation. In contrast to what has been observed following stem cell transplantation without conditioning, quantitative and qualitative T-cell and B-cell functions are durable following UCB transplantation using high intensity transplant conditioning.
The outcomes of 16 children transplanted with UCB for treatment of SCID are reported in three separate retrospective reports [5, 22, 45]. One of 16 failed to engraft, and 13 of 16 are long-term survivors with normalization of immune function.
Wiscott-Aldrich Syndrome
Wiscott-Aldrich Syndrome (WAS) is due to an X-linked mutation in the WASP gene, with an incidence of 4 per million live male births. The role of stem cell transplantation for treatment of this disorder has been firmly established. The initial reports demonstrated cure rates as high as 89% when matched unrelated donor transplantation is performed before the age of 5 years [13]. The published experience of UCB transplantation for WAS has grown significantly in the past few years. In 2003, Knutsen and colleagues were among the first to demonstrate feasibility of UCB transplantation for WAS with successful treatment of 3 children age 2–8 yrs [21]. More recently, the Duke University group reported the outcome of 15 patients transplanted with UCB between 1998 and 2007 [42]. All patients achieved donor cell engraftment following a conditioning regimen consisting of busulfan, cyclophosphamide, +/- ATG. Six of 15 patients died from transplant-related complications, resulting in an overall survival of 60%. Chronic GvHD was observed in 11 of 12 surviving patients (limited in 10, extensive in 1). The authors found this incidence of chronic GvHD to be in excess of what has been observed in other patients with congenital immunodeficiency disorders transplanted with UCB. They postulate a potential link to pre-existing eczema, which is commonly seen in patients with WAS.
A recent review of registry data collected by the CIBMTR (unpublished) compared 113 WAS recipients of unrelated bone marrow with 65 WAS recipients of unrelated cord blood transplants carried out between 1995 and 2005. This analysis showed equivalent 3-year survival for recipients age <5 years at the time of transplantation (73% vs 75%). Taken together, these data support the use of UCB for stem cell transplantation of WAS.
The CIBMTR has received registration reports of UCB transplantation for other rare lymphoid immunodeficiency disorders. These include Cartilage Hair Hypoplasia, X-linked Lymphoproliferative syndrome, Common Variable Immunodeficiency, Reticular dysgenesis and Bare Lymphocyte syndrome. Unfortunately, the outcomes of these transplants are not available for review.
Myeloid immunodeficiency disorders
Chronic Granulomatous Disease (CGD)
CGD is a congenital neutrophil disorder that is a consequence of an X-linked or autosomal recessive mutation in the NADPH-oxidase complex. The curative potential of stem cell transplantation has been clearly demonstrated [17, 40]. There are 8 reported cases of UCB transplantation for CGD [4, 31, 32, 35, 43]. Reduced intensity conditioning was successfully used in the oldest patient of this compilation of reports (age 20 yrs). The others were conditioned with high intensity regimen; 2 experienced primary graft failure. Six of 8 patients are long-term survivors.
Leukocyte adhesion deficiency is another life-threatening myeloid immune disorder. To date, there are no published reports of UCB transplantation for treatment of this disorder.
Immune/Inflammatory disorders
Hemophagocytic Lymphohistiocytosis (HLH)
The familial or inherited form of HLH as well as the EBV-associated HLH will be considered together in this review. In general, the outcomes of allogeneic stem cell transplantation following high dose conditioning, regardless of the stem cell source, are not as favorable as that observed for other inherited immunodeficiencies. This has prompted a movement toward the use of reduced intensity preparative regimens for this disorder [8]. Ohga and colleagues recently reviewed data from the Japanese Society of Pediatric Hematology [34]. Outcomes of 57 patients (familial HLA-43, EBV-associated HLH-14), 21 of whom received UCB grafts, are reported. The overall survival by log-rank analysis of the UCB transplant recipients was 66%, which did not differ from recipients of related or unrelated bone marrow or peripheral blood stem cell transplantation.
Chediak-Higashi
The team from the University of California at Los Angeles has reported in abstract form successful UCB transplantation of 3 patients with Chediak-Higashi. Limited information is available on long-term outcome [50].
Umbilical cord blood transplantation for inborn errors of metabolism
Current data supports the use of allogeneic stem cell transplantation for the treatment of lysosomal and peroxisomal storage disorders. Enzyme replacement therapies are currently available, but questions remain as to the long-term efficacy of these therapies and their ability to positively impact the natural history of the disorder. Stem cell transplantation provides the opportunity for enzyme replacement via “cross correction” of enzyme-deficient cells by neighboring donor derived, enzyme-replete cells [9, 20]. Furthermore, stem cell transplantation (and UCB transplantation in particular) provides the potential for repair of damaged non-hematopoietic tissue such as microglial cells in the brain and Kupffer cells in the liver via differentiation of tissue-specific progenitor cells or transdifferentiation.
Lysosomal and peroxisomal storage diseases affect multiple organ systems, with the central and peripheral nervous system particularly impacted. Depending on the extent of damage at the time of stem cell transplantation, the impact of allogeneic SCT may require extensive and sophisticated neurocognitive testing to objectively measure response. It is clear that many of the neurocognitive deficits incurred by the patients will not be corrected by stem cell transplantation. However, a plateau in survival appears to be evident from a large, single center series of UCB transplants for inherited metabolic disorders [36, Fig. 3]. Longer follow-up and more experience will be required to optimize the timing and impact of this treatment modality.
Krabbe’s disease
The potential for UCB transplantation to favorably impact on the natural history of inborn errors of metabolism was elegantly demonstrated by Escolar and colleagues in patients with Krabbe’s disease [11]. Children born with Krabbe’s disease are deficient of the lysosomal enzyme galactocerebrosidase. As a result, the children experience rapidly progressive neurologic deterioration and death at an early age. Escolar et al found that when children undergo UCB transplantation prior to the onset of symptoms, most will go on to have age-appropriate cognitive and motor function, along with 100% overall survival. Those who underwent UCB transplantation after the onset of symptoms showed little improvement in neurologic function and had an overall survival of only 43%. The study demonstrates the importance of early recognition of inborn errors along with early intervention with stem cell transplantation before irreversible damage occurs.
Hurler’s syndrome
Hurler’s syndrome is an autosomal recessive mucopolysaccharidosis caused by deficiency of alpha-L-iduronidase. Multiple organs, including the central nervous system, heart, bone, eyes, and liver are affected. Although enzyme replacement therapy has been available since 2003, due to poor CNS penetration, it does not completely prevent neurologic deterioration. Therefore, allogeneic stem cell transplantation remains the treatment of choice. Both European and North American registry data suggest that over 500 patients with Hurler’s syndrome have been treated with allogeneic stem cell transplantation. Staba and colleagues reported the Duke University experience with UCB transplantation for 20 children with Hurler’s syndrome [41]. The patients were prepared with high dose conditioning and received UCB units from mismatched unrelated donors. The median cell dose was 8.8x107 nucleated cells/kg. Only one patient failed to engraft with donor cells. Long-term survival was achieved in 17 of 20 patients with all surviving patients having normal alpha-L-iduronidase activity. Many of the surviving children continue to have neurocognitive impairment. Despite this, 81% of the surviving school-age children attend school in age-appropriate classrooms [36]. However, many Hurler’s patients continue to have problems with skeletal deformities that require corrective surgery.
Boelens and colleagues reviewed data from the European Blood and Marrow Transplant Registry regarding outcome of patients with Hurler’s syndrome undergoing allogeneic transplantation [6]. While overall survival was not affected by cell source selection, the data suggested that UCB grafts significantly improved the chance for achieving full donor chimerism and, as a result, normal circulating enzyme levels compared to patients receiving peripheral blood or bone marrow grafts.
X-linked Adrenoleukodystrophy (X-ALD)
X-ALD is a peroxisomal disorder stemming from a defective ABCD1 gene. This results in accumulation of long chain fatty acids, which has devastating neurologic consequences. The therapeutic potential of UCB transplantation was best described by Beam and colleagues who report the outcomes of 12 boys, 3 of whom were transplanted early in life, before symptoms of the disease developed [3]. All patients received high dose conditioning with busulfan, cyclophosphamide, and anti-thymocyte globulin followed by partially matched unrelated UCB transplantation. Extensive baseline neurophysiologic, neuroimaging and neurodevelopmental testing was performed prior to transplantation and followed serially after the transplantation. One patient died early from toxicity and another experienced primary graft failure, but was rescued with a second transplant. Overall survival at 6 months was 67%. The authors found that the degree of pre-transplant ALD-associated brain involvement (Loes score) was a strong predictor of post-transplantation cognitive and motor outcome. Many of the patients with severe neurocognitive impairment at the time of transplantation experienced disease progression despite transplantation. In contrast, the 3 boys who were asymptomatic at the time of transplant had excellent outcomes.
Composite reports of UCB transplantation for rare inborn errors
Disease-specific reports of allogeneic transplantation for rare inborn errors of metabolism lack the detail or sample size to draw definitive conclusions about outcomes [30, 36, 44]. Table 1 lists the disorders that have been treated with UCB transplantation. Questions remain as to the appropriate timing for the transplant as well as the therapeutic benefit. It is for this reason that use of allogeneic SCT for treatment of many of these disorders remains investigational.
Table 1. Inborn metabolism errors treated with umbilical cord blood transplantation
|
Hurler syndrome |
|
Krabbe's disease |
|
Sanfilippo syndrome |
|
Metachromatic leukodystrophy |
|
Adrenoleukodystrophy |
|
Tay Sachs disease |
|
Hunter syndrome |
|
Lesch-Nyhan disease |
|
Sandhoff disease |
|
Hurler Scheie |
|
Neimann-Pick |
|
Alpha mannosidosis |
|
GM1 gangliosidosis |
|
I-cell disease |
|
Maroteaux-Lamy syndrome |
|
Pelizaeus-Merzbacher disease |
|
Fucosidosis |
|
Wolman disease (Acid Lipase Deficiency) |
The common theme among all the reports is that the earlier the transplant is done, the better the outcome. In the largest of these composite reports from the Duke University group, 159 children representing 16 different inborn errors of metabolism were transplanted following high dose conditioning (busulfan, cyclophosphamide, and equine anti-thymocyte globulin) over a 12-year period, ending in 2007. The probability of engraftment, acute and chronic GvHD, overall survival and factors influencing survival has been shown [36, Fig. 1]. Of note, the 1 and 5 year overall survivals for the most common disorders treated on the study (Hurler, Hunter, and Sanfilippo syndrome, metachromatic leukodystrophy, and adrenoleukodystrophy) were all similar. This suggests that timing of the transplant, not the underlying disease, is most important in predicting outcome.
Umbilical cord blood transplantation for hemoglobinopathies
Related UCB transplantation for β-thalassemia and sickle cell disease
Unlike the situation with inborn errors of metabolism, there is an established role for allogeneic stem cell transplantation for the treatment of β-thalassemia and sickle cell disease [27, 28, 49]. The published experience of UCB transplantation for β-thalassemia remains quite limited [12, 26]. The largest report comes from the Eurocord registry data describing the outcome of 33 β-thalassemia patients transplanted with matched related UCB grafts [26]. All patients had a low disease severity (Pesaro 1 in 20 pts, Pesaro 2 in 13 pts). All patients received high dose e conditioning and GvHD prophylaxis with cyclosporine alone or combined with methotrexate. Seven of 33 patients experienced graft failure, but were rescued with either autologous stem cells or bone marrow from the original matched sibling cord blood donor at a later date. With a median follow-up of 24 months, all 33 patients were alive and well, but 4 retained the β-thalassemia phenotype.
The Locatelli report also included outcomes of 11 patients with sickle cell disease transplanted with UCB from related donors matched 6/6 (9 pts) or 5/6 (2 pts) [26]. The conditioning and GvHD prophylaxis regimens were similar to those used for the β-thalassemia patients. Primary engraftment was achieved in 10 of 11 patients, and all 11 patients are alive and well (1 with sickle cell disease) with a median follow-up of 24 months.
Unrelated UCB transplantation for β-thalassemia and sickle cell disease
There has yet to be enough published experience with unrelated UCB transplantation for β-thalassemia or sickle cell disease to fully assess the risk versus benefit considerations. The relative dearth of reports in the literature likely portrays unresolved challenges that remain with this mode of therapy. The few available reports suggest feasibility of unrelated UCB transplantation for hemoglobinopathies [1, 18, 19, 46]. However, it appears that establishment of stable donor engraftment is more challenging in this population of patients [1]. This may be related to the chemotherapy naïve status of the patients combined with a highly proliferative, cellular bone marrow milieu.
Umbilical cord blood transplantation for bone marrow failure disorders
The published experience with UCB for treatment of acquired bone marrow failure disorders is outlined in Table 2. Most investigators have relegated UCB transplantation to a treatment of last resort. Thus, those transplanted with UCB represent an extremely high-risk subset of patients who have failed prior therapy. Interpretation of the data is further compromised by the heterogeneous transplantation techniques. The data suggests that UCB transplantation for severe aplastic anemia is feasible. Larger studies will be needed to garner a better understanding of the relative risk of graft failure compared to patients with other non-malignant or malignant disorders.
Table 2. Umbilical cord blood transplantation for treatment of severe aplastic anemia and paroxysmal nocturnal hemoglobinurea
|
Reference |
Disorder- |
Median |
Preparative |
Median |
Percent |
Outcome |
|---|---|---|---|---|---|---|
|
(Mao, |
AA-9 |
25 |
Cy/ATG |
2.19 (1.6-10.7)* |
78 |
EFS-78 OS-78 |
|
(Ohga, |
AA-1 |
11 |
TBI-5Gy |
3.9 |
100 |
EFS-100 OS-100 |
|
(Chan, |
AA-9 |
9 |
Cy/ATG-2 |
5.4 (3.5-20) |
67 |
EFS-67 OS-78
|
|
(Yoshimi, |
AA-31 |
28 |
TBI (4-5Gy)/Flu/Mel-12 |
NA |
55 |
OS (2yrs)-41 |
|
(Ruggeri, |
SAA-4 PNH-1 |
19 |
Bu/Cy/Flu-3 |
4.7 (2.9-9.7) (Dual Cord Blood Graft) |
80 |
EFS-60 OS-80 |
*Post-thaw cell dose (cryopreserved cell dose not reported)
References
12. Fang, J., Huang, S., Chen, C., Zhou, D., Li, C.K., Li, Y. & Huang, K. (2004) Umbilical cord blood transplantation in Chinese children with beta-thalassemia. J Pediatr Hematol Oncol, 26, 185-189.
15. Gluckman, E., Broxmeyer, H.A., Auerbach, A.D., Friedman, H.S., Douglas, G.W., Devergie, A., Esperou, H., Thierry, D., Socie, G., Lehn, P. & et al. (1989, now open access in this issue of CTT) Hematopoietic reconstitution in a patient with Fanconi's anemia by means of umbilical-cord blood from an HLA-identical sibling. N Engl J Med, 321, 1174-1178.
21. Knutsen, A.P., Steffen, M., Wassmer, K. & Wall, D.A. (2003) Umbilical cord blood transplantation in Wiskott Aldrich syndrome. J Pediatr, 142, 519-523.
22. Knutsen, A.P. & Wall, D.A. (2000) Umbilical cord blood transplantation in severe T-cell immunodeficiency disorders: two-year experience. J Clin Immunol, 20, 466-476.
23. Kurtzberg, J. (2009) Update on umbilical cord blood transplantation. Curr Opin Pediatr, 21, 22-29.
24. Kurtzberg, J., Graham, M., Casey, J., Olson, J., Stevens, C.E. & Rubinstein, P. (1994) The use of umbilical cord blood in mismatched related and unrelated hemopoietic stem cell transplantation. Blood Cells, 20, 275-283; discussion 284.
28. Lucarelli, G., Galimberti, M., Polchi, P., Angelucci, E., Baronciani, D., Giardini, C., Politi, P., Durazzi, S.M., Muretto, P. & Albertini, F. (1990) Bone marrow transplantation in patients with thalassemia. N Engl J Med, 322, 417-421.
29. Mao, P., Zhu, Z., Wang, H., Wang, S., Mo, W., Ying, Y., Li, Q. & Xu, Y. (2005) Sustained and stable hematopoietic donor-recipient mixed chimerism after unrelated cord blood transplantation for adult patients with severe aplastic anemia. Eur J Haematol, 75, 430-435.
31. Mochizuki, K., Kikuta, A., Ito, M., Akaihata, M., Sano, H., Ohto, H. & Hosoya, M. (2009) Successful unrelated cord blood transplantation for chronic granulomatous disease: a case report and review of the literature. Pediatr Transplant, 13, 384-389.
32. Nakano, T., Boku, E., Yoshioka, A. & Fujimura, Y. (1999) A Case of McLeod Phenotype Chronic Granulomatous Disease who Received Unrelated Cord Blood Transplantation. Journal of Pediatric Hematology, 12, 264.
33. Ohga, S., Ichino, K., Goto, K., Hattori, S., Nomura, A., Takada, H., Nakamura, K. & Hara, T. (2006) Unrelated donor cord blood transplantation for childhood severe aplastic anemia after a modified conditioning. Pediatr Transplant, 10, 497-500.
34. Ohga, S., Kudo, K., Ishii, E., Honjo, S., Morimoto, A., Osugi, Y., Sawada, A., Inoue, M., Tabuchi, K., Suzuki, N., Ishida, Y., Imashuku, S., Kato, S. & Hara, T. (2009) Hematopoietic stem cell transplantation for familial hemophagocytic lymphohistiocytosis and Epstein-Barr virus-associated hemophagocytic lymphohistiocytosis in Japan. Pediatr Blood Cancer, 54, 299-306.
35. Parikh, S.H., Szabolcs, P., Prasad, V.K., Lakshminarayanan, S., Martin, P.L., Driscoll, T.A. & Kurtzberg, J. (2007) Correction of chronic granulomatous disease after second unrelated-donor umbilical cord blood transplantation. Pediatr Blood Cancer, 49, 982-984.
36. Prasad, V.K., Mendizabal, A., Parikh, S.H., Szabolcs, P., Driscoll, T.A., Page, K., Lakshminarayanan, S., Allison, J., Wood, S., Semmel, D., Escolar, M.L., Martin, P.L., Carter, S. & Kurtzberg, J. (2008) Unrelated donor umbilical cord blood transplantation for inherited metabolic disorders in 159 pediatric patients from a single center: influence of cellular composition of the graft on transplantation outcomes. Blood, 112, 2979-2989. Figure 3. Figure 1.
38. Rogers, I., Yamanaka, N., Bielecki, R., Wong, C.J., Chua, S., Yuen, S. & Casper, R.F. (2007) Identification and analysis of in vitro cultured CD45-positive cells capable of multi-lineage differentiation. Exp Cell Res, 313, 1839-1852.
42. Sun, J.M., Driscoll, T., Prasad, V.K., Parikh, S.H., Szabolcs, P., Kurtzberg, J. & Martin, P. (2009) Unrelated Umbilical Cord Blood Transplantation is an Effective Therapy for Wiskott-Aldrich Syndrome. Biol Blood Marrow Transplant, 15, 76.
43. Suzuki, N., Hatakeyama, N., Yamamoto, M., Mizue, N., Kuroiwa, Y., Yoda, M., Takahashi, J., Tani, Y. & Tsutsumi, H. (2007) Treatment of McLeod phenotype chronic granulomatous disease with reduced-intensity conditioning and unrelated-donor umbilical cord blood transplantation. Int J Hematol, 85, 70-72.
44. Tokimasa, S., Ohta, H., Takizawa, S., Kusuki, S., Hashii, Y., Sakai, N., Taniike, M., Ozono, K. & Hara, J. (2008) Umbilical cord-blood transplantations from unrelated donors in patients with inherited metabolic diseases: Single-institute experience. Pediatr Transplant, 12, 672-676.
46. Vanichsetakul, P., Wacharaprechanont, T., R, O.C., Seksarn, P. & Kupatawintu, P. (2004) Umbilical cord blood transplantation in children with beta-thalassemia diseases. J Med Assoc Thai, 87 Suppl 2, S62-67.
47. Wagner, J.E., Kernan, N.A., Steinbuch, M., Broxmeyer, H.E. & Gluckman, E. (1995) Allogeneic sibling umbilical-cord-blood transplantation in children with malignant and non-malignant disease.[see comment]. Lancet, 346, 214-219.
50. Wang, K., Lin, E., Moore, T. & Roberts, R. (2009) Cord Blood Transplantation for Treatment of Chediak-Higashi Syndrome. Clinical Immunology, 131, S77-S78.
Митчелл Э. Хорвитц, Нельсон Чао
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18928" ["VALUE"]=> array(2) { ["TEXT"]=> string(1930) "<p class="bodytext">По мере улучшения результатов трансплантации клеток пуповинной крови (ТКПК), подлежат пересмотру также и расчеты соотношений риска и выгоды при лечении неопухолевых заболеваний. Недавно полученные результаты дают основания считать, что исход ТКПК сравним с таковым при пересадке от совместимого неродственного донора. Следовательно, в отношении больных, не подлежащих такой потенциально излечивающей терапии из-за отсутствия подходящего совместимого донора, могут рассматриваться возможности совместимой или несовместимой трансплантации неродственных клеток пуповинной крови. В данном обзорe будут обсуждаться наиболее современные данные, касающиеся ТКПК в целях лечения врожденных иммунодефицитных заболеваний, врожденных болезней обмена веществ, синдромов дефицита функций костного мозга и гемоглобинопатий. </p> <h3>Ключевые слова</h3> <p> трансплантация стволовых клеток, пуповинная кровь, исходы, клинические результаты, иммунодефицит, неопухолевые заболевания, дефицит функций костного мозга, обзор</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1884) "По мере улучшения результатов трансплантации клеток пуповинной крови (ТКПК), подлежат пересмотру также и расчеты соотношений риска и выгоды при лечении неопухолевых заболеваний. Недавно полученные результаты дают основания считать, что исход ТКПК сравним с таковым при пересадке от совместимого неродственного донора. Следовательно, в отношении больных, не подлежащих такой потенциально излечивающей терапии из-за отсутствия подходящего совместимого донора, могут рассматриваться возможности совместимой или несовместимой трансплантации неродственных клеток пуповинной крови. В данном обзорe будут обсуждаться наиболее современные данные, касающиеся ТКПК в целях лечения врожденных иммунодефицитных заболеваний, врожденных болезней обмена веществ, синдромов дефицита функций костного мозга и гемоглобинопатий.
Ключевые слова
трансплантация стволовых клеток, пуповинная кровь, исходы, клинические результаты, иммунодефицит, неопухолевые заболевания, дефицит функций костного мозга, обзор
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18929" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000069.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000069.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18930" ["VALUE"]=> array(2) { ["TEXT"]=> string(66) "<p>Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(54) "Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18931" ["VALUE"]=> array(2) { ["TEXT"]=> string(108) "<p>Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(96) "Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18932" ["VALUE"]=> array(2) { ["TEXT"]=> string(1059) "<p class="bodytext">As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies. </p> <h3>Keywords</h3> <p> stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1013) "As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies.
Keywords
stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18933" ["VALUE"]=> string(77) "Umbilical cord blood transplantation for treatment of non-malignant disorders" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(77) "Umbilical cord blood transplantation for treatment of non-malignant disorders" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18934" ["VALUE"]=> string(3) "910" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "910" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(12) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18930" ["VALUE"]=> array(2) { ["TEXT"]=> string(66) "<p>Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(54) "Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(54) "Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18932" ["VALUE"]=> array(2) { ["TEXT"]=> string(1059) "<p class="bodytext">As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies. </p> <h3>Keywords</h3> <p> stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review </p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1013) "As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies.
Keywords
stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1013) "As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies.
Keywords
stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18929" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000069.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000069.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2010-en-000069.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18933" ["VALUE"]=> string(77) "Umbilical cord blood transplantation for treatment of non-malignant disorders" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(77) "Umbilical cord blood transplantation for treatment of non-malignant disorders" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(77) "Umbilical cord blood transplantation for treatment of non-malignant disorders" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18931" ["VALUE"]=> array(2) { ["TEXT"]=> string(108) "<p>Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(96) "Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(96) "Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(2) { [0]=> string(5) "18935" [1]=> string(5) "18936" } ["VALUE"]=> array(2) { [0]=> string(4) "1423" [1]=> string(4) "1424" } ["DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { [0]=> string(4) "1423" [1]=> string(4) "1424" } ["~DESCRIPTION"]=> array(2) { [0]=> string(0) "" [1]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> array(2) { [0]=> string(63) "Mitchell E. Horwitz" [1]=> string(55) "Nelson Chao" } ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18927" ["VALUE"]=> array(2) { ["TEXT"]=> string(75) "<p>Митчелл Э. Хорвитц, Нельсон Чао</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(63) "Митчелл Э. Хорвитц, Нельсон Чао
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(63) "Митчелл Э. Хорвитц, Нельсон Чао
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18921" ["VALUE"]=> string(22) "01/15/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/15/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/15/2010 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18922" ["VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/25/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/25/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18923" ["VALUE"]=> string(22) "06/09/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "06/09/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "06/09/2010 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18924" ["VALUE"]=> string(4) "1423" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1423" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(63) "Mitchell E. Horwitz" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "18928" ["VALUE"]=> array(2) { ["TEXT"]=> string(1930) "<p class="bodytext">По мере улучшения результатов трансплантации клеток пуповинной крови (ТКПК), подлежат пересмотру также и расчеты соотношений риска и выгоды при лечении неопухолевых заболеваний. Недавно полученные результаты дают основания считать, что исход ТКПК сравним с таковым при пересадке от совместимого неродственного донора. Следовательно, в отношении больных, не подлежащих такой потенциально излечивающей терапии из-за отсутствия подходящего совместимого донора, могут рассматриваться возможности совместимой или несовместимой трансплантации неродственных клеток пуповинной крови. В данном обзорe будут обсуждаться наиболее современные данные, касающиеся ТКПК в целях лечения врожденных иммунодефицитных заболеваний, врожденных болезней обмена веществ, синдромов дефицита функций костного мозга и гемоглобинопатий. </p> <h3>Ключевые слова</h3> <p> трансплантация стволовых клеток, пуповинная кровь, исходы, клинические результаты, иммунодефицит, неопухолевые заболевания, дефицит функций костного мозга, обзор</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1884) "По мере улучшения результатов трансплантации клеток пуповинной крови (ТКПК), подлежат пересмотру также и расчеты соотношений риска и выгоды при лечении неопухолевых заболеваний. Недавно полученные результаты дают основания считать, что исход ТКПК сравним с таковым при пересадке от совместимого неродственного донора. Следовательно, в отношении больных, не подлежащих такой потенциально излечивающей терапии из-за отсутствия подходящего совместимого донора, могут рассматриваться возможности совместимой или несовместимой трансплантации неродственных клеток пуповинной крови. В данном обзорe будут обсуждаться наиболее современные данные, касающиеся ТКПК в целях лечения врожденных иммунодефицитных заболеваний, врожденных болезней обмена веществ, синдромов дефицита функций костного мозга и гемоглобинопатий.
Ключевые слова
трансплантация стволовых клеток, пуповинная кровь, исходы, клинические результаты, иммунодефицит, неопухолевые заболевания, дефицит функций костного мозга, обзор
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1884) "По мере улучшения результатов трансплантации клеток пуповинной крови (ТКПК), подлежат пересмотру также и расчеты соотношений риска и выгоды при лечении неопухолевых заболеваний. Недавно полученные результаты дают основания считать, что исход ТКПК сравним с таковым при пересадке от совместимого неродственного донора. Следовательно, в отношении больных, не подлежащих такой потенциально излечивающей терапии из-за отсутствия подходящего совместимого донора, могут рассматриваться возможности совместимой или несовместимой трансплантации неродственных клеток пуповинной крови. В данном обзорe будут обсуждаться наиболее современные данные, касающиеся ТКПК в целях лечения врожденных иммунодефицитных заболеваний, врожденных болезней обмена веществ, синдромов дефицита функций костного мозга и гемоглобинопатий.
Ключевые слова
трансплантация стволовых клеток, пуповинная кровь, исходы, клинические результаты, иммунодефицит, неопухолевые заболевания, дефицит функций костного мозга, обзор
" } } } [8]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "81" ["~IBLOCK_SECTION_ID"]=> string(2) "81" ["ID"]=> string(4) "1435" ["~ID"]=> string(4) "1435" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["~NAME"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "09/29/2017 04:45:02 pm" ["~TIMESTAMP_X"]=> string(22) "09/29/2017 04:45:02 pm" ["DETAIL_PAGE_URL"]=> string(116) "/en/archive/tom-2-nomer-3-7/forum/nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn/" ["~DETAIL_PAGE_URL"]=> string(116) "/en/archive/tom-2-nomer-3-7/forum/nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(27253) "Introduction
Scientific blogging is a Web 2.0 tool [1], which combines all blogs about different aspects of science, which are usually run by scientists or people familiar with science. As examples of this growing online community you can look at some platforms and aggregators: ScienceBlogs.com, ResearchBlogging.org, and Nature Network.
There are many reasons why scientists blog. To get a sense you can read “The science blog meme”, an online interview with 34 scientists on the subject “Why do we blog” [2]. The most common reasons mentioned are the following [3]: passion to share new exciting research (done by you or others) in your field and discussions with colleagues around the world, to talk about science in informal settings, to learn online tools for scientists, to improve writing skills, etc.
I have been blogging for 7 years and stayed tightly in my area of expertise (niche). When I started blogging in English (my first language is Russian), I set up a few goals:
• Practice tight and productive networking with scientists and medical professionals in the same niche of interest from around the world.
• Transform professional connections online into real connections and collaborations.
• Get a sense of what is science online, and what web tools I can use to increase my scientific productivity.
• Summarize all of my notes, bookmarks and thoughts in the area of my interest and put them in one place online (database), where I can easily find them at any time.
• Improve my language (English) and writing skills.
• Monetize and possibly earn some money from blogging.
• Acquire professional value, peer recognition and my “authority” for advancement in career.
It turns out that the networking part has worked especially wonderfully for me. I’ll share my experience in this essay.
Information overload and its management
During my PhD work I started to look for literature online and useful tools that would allow me to manage information, and there was nothing at the time that was specifically suitable for scientists. Now we have a lot of scientific information available online, frequently called “information overload”, but also enough tools to manage it. The problem is that not many scientists know about these tools and sometimes don’t want to pick them up if they do know. I started intensively using RSS technology and reference managers, which allowed me to deal with this information overload.
I use a RSS Reader to set up my personal informational filters online. I subscribe by RSS to PubMed via the query “stem cell” (about 50 new articles daily), about 20 “stem cell blogs”, about 10 scientific blogs, some scientific journals (which get indexed in PubMed slowly after publication release), and a few news services.
For managing web pages that I like, including articles, I use online bookmarking tools (reference managers [4, 5]), such as: Connotea and Mendeley. These two and some others (Zotero, EndNote, Papers, etc.) were designed specifically for scientists. They allow you to create your personal searchable online library by keywords (tags) and find like-minded people who are using the same tags. So, your scientific library could be completely in the web (cloud) or in your pocket (though smartphone mobile applications) and you don’t need to pack your computer.
At some point, I wanted to make notes from my tagged references online in order to summarize current knowledge and trends. I decided to blog, because the number of reasons that I mentioned above motivated me and I wanted to share information with other professionals in my field. I set up the first blog – Hematopoiesis.info, dedicated to professional networking in 2007.
Blogging analytical content
Because now there are a lot of tools available for information management, I decide to fill my blog with analytical content. I pick and summarize the most exciting and controversial work in my field – adult stem cell research. I’m writing about current trends in the field with a translational focus. My content is based not only on publications, but also on information from conferences that I attend and personal communication. It makes the content quite distinctive in my niche. Each of my posts contains links to a few papers, all connected by a particular topic. I put some of my thoughts into it and try to provoke reader discussion. I also try to incorporate some online tools in the blog that could be very useful for scientists.
I think with the variety of tools available right now, there is no need to have a blog just for quick sharing of some links or news or videos or fresh papers with your peers. We can do it on so-called microblogging platforms, such as Twitter or on Google Buzz or Facebook. Another great online communication aggregator, FriendFeed (FF), allows you to easily share links from any web-services that you use and become social by commenting. I was so excited by the possibilities of FriendFeed for science online that I wrote a post entitled “FriendFeed as a blogging killer” [6].
Finally, I came up with the idea that nothing can replace a blog post if it's made in the format of a unique analytical thoughtful mini-article. You can even consider scientific blog posts as a small online publication judged by your peers from networking. I think blogging will be widely accepted in the scientific mainstream only if it can bring some professional value, i.e., unique trusted information with the possibility of real time discussion in informal settings.
The blog as a professional networking tool
So I’m using a blog as a hub for gathering information picked from my bookmarks, and its analysis. In this case, high quality analytical information is an input, but what is the output? I consider a blog as a part of an online project, which connects the shared information with professionals working in the same field. In order to get the output I share links to my blog posts in professional networking web-services, such as LinkedIn. I’m networking in 20 LinkedIn professional groups, where I can submit discussion (as a forum) or share a link and switch to personal communication. Unexpectedly, I started to get more productive discussions about my blog posts on LinkedIn than on the blog itself. If people like my thoughts in the post, they contact me personally and make a connection. I was lucky enough to meet some people from my online connection on LinkedIn and Twitter in person through conferences. So professional networking online in your niche can be easily transformed to real connections.
Besides LinkedIn, I’m also submitting links to my posts to Twitter, sharing them in FriendFeed, Google Buzz, and Google Reader. I’m doing that because different people prefer different platforms for discussions online. I’m getting the maximum feedback only from all tools combined, where I share my blog posts. Recently, I’ve gotten more than 35 comments in LinkedIn and 10 comments on Google Buzz on one of my recent posts (Do we really need hematopoietic stem cell expansion for clinical use?), but nothing on the blog itself. Sometimes, I have discussion only via emails, because some scientists do not trust blogs and hesitate to post information online for public exposure.
So, discussion about my blog posts can occur anywhere: comments under the post itself, comments in LinkedIn groups, replies on Twitter, comments on FriendFeed, and personal communication via email. I think that using a few tools together makes your networking online more productive and valuable.
From personal filter to collaborative filter
Scientists like to collaborate. I started to collaborate online simply by sharing drafts of my blog posts with my friends via Google Documents. I asked their opinions about the draft, and even for them to check my grammar. It was my first experience with sharing documents online. Later, I was trying to move from my personal information filters to collaborative filters.
Collaborative filters aim to sort the information stream from the popular (mass-media) and search engines (Google, PubMed) to professional user-trusted content with the possibility of discussion and collaboration [7]. The blog could be a good start for setting up a collaborative filter in your professional niche. You can use FF-like a tool to filter “trusted content” recommended to you by friends and experts, but not search engines [8]. Today we can use a number of tools for collaborative filters with or without blogging.
I was always thinking about how to move the blog with my professional networking to collaboration. Via my connections online I simply sent a message and found a person who was interested in an online collaboration with me in setting up a new project – Stem Cell Assays. This project is dedicated to promoting rigorous reproducible results in stem cell research by sharing methods.
Another example of collaboration online is to make a community project. I created a Google Wave “Cell processing devices in cell therapy”, made it public (everyone can read it) and embedded it into a Stem Cell Assays blog post. The link to this blog post went to LinkedIn groups and Twitter. The next day I got very good traffic from LinkedIn, but again people didn’t comment on the blog post. Instead, I got some nice feedback in comments on LinkedIn and some people came directly to the Google Wave and started to update information in real time.
Links

Connotea
EndNote
Facebook
FriendFeed
Google Buzz
Google Documents
Google Reader
Google Wave
Hematopoiesis
LinkedIn
Mendeley
Nature Network
Papers
PubMed
Research Blogging
ScienceBlogs
Twitter
Zotero
Figure 1. The model of scientific blogging as a platform for professional networking online
Concluding remarks and future perspectives
There is a lot of discussion going on on the Web about the future of scientific blogging [9]. Will academic blogging advance your career [10] or is it a waste of time? Scientific blogging is evolving [11]. I think blogs and scientific blogging in particular will survive and take a very precise niche among the variety of other web tools, only if it can provide trusted, valid, and useful content. Some analytical blog posts with ideas could be cited [12] in scientific papers. Blogs will play more of a role in “article-level metrics” [13] if the paper was mentioned by a blogger. Real time and updatable comments more likely will not be anonymous [14] and more valuable for scientific community. This could be the biggest advantage compared to traditionally published papers.
Taking into account all of the good things about scientific blogging, I wouldn’t say that everyone should do it. You should try to blog if you’re curious and motivated enough to do it. Not every scientist is very social and curious about web tools. Not every scientist feels like sharing information online [15] and being publically exposed [16]. Importantly, scientific blogging is your continuous contribution in science after hours. So, you have to feel a strong commitment to a particular scientific field (your niche) and also realize that it’s time consuming. You should be responsible for high quality valid content, which could be citable and trusted by your peers. Scientific bloggers also have to realize that unpublished information (that you have heard from yesterday’s talk, for example) should be very carefully chosen, and that its release is not going to hurt your colleagues. Only in this case you can build your “scientific equity” or authority successfully.
I think that the proposed model (Figure 1) of scientific blogging as an online networking tool will work the best for junior investigators, e.g., PhD students, postdoctoral fellows and young PIs. In part, because these categories of people don’t have enough scientific authority yet to be heard by established academic professors, clinicians and business executives. When a young generation of scientists is coming to LinkedIn to discuss recent advances and controversies they have much less chance to be heard by established and respected scientists. In this case, building a meaningful foundation online, such a blog, could work nicely in order to network professionally at a high level.
Acknowledgements
I declare no conflict of interest.
I’d like to thank Joanna Balcerek (Robert Wood Johnson Medical School, New Brunswick, NJ, USA) for her contribution to the Hematopoiesis.info project and for reviewing this manuscript.
References
1. Crotty David. Web 2.0 for Biologists–Are any of the current tools worth using? Bench Marks blog. April 3, 2008. http://www.cshblogs.org/cshprotocols/2008/04/03/web-20-for-biologists-are-any-of-the-current-tools-worth-using/
2. Fenner Martin. Why do we blog and other important questions, answered by 34 science bloggers. Gobbledygook blog. November 30, 2008. http://blogs.nature.com/mfenner/2008/11/30/why-do-we-blog-and-other-important-questions-answered-by-34-science-bloggers
3. Brown Daniel. Science blogging: The future of science communication & why you should be a part of it. Biochemical Soul blog. March 17, 2009.
http://biochemicalsoul.com/2009/03/science-blogging-the-future-of-science-communication-why-you-should-be-a-part-of-it/
4. Fenner Martin. What is a reference manager? Gobbledygook blog. May 19, 2010;
http://blogs.nature.com/mfenner/2010/05/19/post
5. Fenner Martin. What is the right reference manager for you? SlideShare presentation.
http://www.slideshare.net/mfenner/which-reference-manager
6. Bersenev Alexey. How FriendFeed is killing blogging. Hematopoiesis blog. Septermber 3, 2009.
http://hematopoiesis.info/2008/09/03/how-friendfeed-is-killing-blogging/
7. Bersenev Alexey. Collaborative filters online. Hematopoiesis blog. January 26, 2009.
http://hematopoiesis.info/2009/01/26/collaborative-filters-online/
8. Rubel Steve. Friendfeed can disrupt search and reshape advertising. Micro Persuasion blog. June 11, 2008. http://www.micropersuasion.com/2008/06/friendfeed-can.html
9. Neylon Cameron. The nature of science blog networks. Science in the Open blog. July 25, 2010.
http://cameronneylon.net/blog/the-nature-of-science-blog-networks/
10. Lemire Daniel. The negative myths about academic blogging. Daniel Lemire's blog. April 4, 2008.
http://www.daniel-lemire.com/blog/archives/2008/04/04/the-negative-myths-about-academic-blogging/
11. Zivkovic Bora. A farewell to Scienceblogs: the changing science blogging ecosystem. Blog Around the Clock. July 19, 2010. http://coturnix.wordpress.com/2010/07/19/a-farewell-to-scienceblogs-the-changing-science-blogging-ecosystem/
12. Zivkovic Bora. Why or why not cite blog posts in scientific papers? Blog Around the Clock. June 11, 2009. http://scienceblogs.com/clock/2009/06/why_or_why_not_cite_blog_posts.php
13. Article-level metrics information. PLoS ONE.
http://www.plosone.org/static/almInfo.action
14. Gunn William. Online Engagement of Scientists with the literature: anonymity vs. ResearcherID. Synthesis blog. May 24, 2009. http://synthesis.williamgunn.org/2009/05/24/online-engagement-of-scientists-with-the-literature-anonymity-vs-researcherid/
15. Bersenev Alexey. What makes scientists not comment online? Hematopoiesis blog. April 6, 2009. http://hematopoiesis.info/2008/04/06/what-makes-scientists-not-comment-online/
16. When blogs make sense. Editorial. Nature 2010;466:8. doi:10.1038/466008a
" ["~DETAIL_TEXT"]=> string(27253) "Introduction
Scientific blogging is a Web 2.0 tool [1], which combines all blogs about different aspects of science, which are usually run by scientists or people familiar with science. As examples of this growing online community you can look at some platforms and aggregators: ScienceBlogs.com, ResearchBlogging.org, and Nature Network.
There are many reasons why scientists blog. To get a sense you can read “The science blog meme”, an online interview with 34 scientists on the subject “Why do we blog” [2]. The most common reasons mentioned are the following [3]: passion to share new exciting research (done by you or others) in your field and discussions with colleagues around the world, to talk about science in informal settings, to learn online tools for scientists, to improve writing skills, etc.
I have been blogging for 7 years and stayed tightly in my area of expertise (niche). When I started blogging in English (my first language is Russian), I set up a few goals:
• Practice tight and productive networking with scientists and medical professionals in the same niche of interest from around the world.
• Transform professional connections online into real connections and collaborations.
• Get a sense of what is science online, and what web tools I can use to increase my scientific productivity.
• Summarize all of my notes, bookmarks and thoughts in the area of my interest and put them in one place online (database), where I can easily find them at any time.
• Improve my language (English) and writing skills.
• Monetize and possibly earn some money from blogging.
• Acquire professional value, peer recognition and my “authority” for advancement in career.
It turns out that the networking part has worked especially wonderfully for me. I’ll share my experience in this essay.
Information overload and its management
During my PhD work I started to look for literature online and useful tools that would allow me to manage information, and there was nothing at the time that was specifically suitable for scientists. Now we have a lot of scientific information available online, frequently called “information overload”, but also enough tools to manage it. The problem is that not many scientists know about these tools and sometimes don’t want to pick them up if they do know. I started intensively using RSS technology and reference managers, which allowed me to deal with this information overload.
I use a RSS Reader to set up my personal informational filters online. I subscribe by RSS to PubMed via the query “stem cell” (about 50 new articles daily), about 20 “stem cell blogs”, about 10 scientific blogs, some scientific journals (which get indexed in PubMed slowly after publication release), and a few news services.
For managing web pages that I like, including articles, I use online bookmarking tools (reference managers [4, 5]), such as: Connotea and Mendeley. These two and some others (Zotero, EndNote, Papers, etc.) were designed specifically for scientists. They allow you to create your personal searchable online library by keywords (tags) and find like-minded people who are using the same tags. So, your scientific library could be completely in the web (cloud) or in your pocket (though smartphone mobile applications) and you don’t need to pack your computer.
At some point, I wanted to make notes from my tagged references online in order to summarize current knowledge and trends. I decided to blog, because the number of reasons that I mentioned above motivated me and I wanted to share information with other professionals in my field. I set up the first blog – Hematopoiesis.info, dedicated to professional networking in 2007.
Blogging analytical content
Because now there are a lot of tools available for information management, I decide to fill my blog with analytical content. I pick and summarize the most exciting and controversial work in my field – adult stem cell research. I’m writing about current trends in the field with a translational focus. My content is based not only on publications, but also on information from conferences that I attend and personal communication. It makes the content quite distinctive in my niche. Each of my posts contains links to a few papers, all connected by a particular topic. I put some of my thoughts into it and try to provoke reader discussion. I also try to incorporate some online tools in the blog that could be very useful for scientists.
I think with the variety of tools available right now, there is no need to have a blog just for quick sharing of some links or news or videos or fresh papers with your peers. We can do it on so-called microblogging platforms, such as Twitter or on Google Buzz or Facebook. Another great online communication aggregator, FriendFeed (FF), allows you to easily share links from any web-services that you use and become social by commenting. I was so excited by the possibilities of FriendFeed for science online that I wrote a post entitled “FriendFeed as a blogging killer” [6].
Finally, I came up with the idea that nothing can replace a blog post if it's made in the format of a unique analytical thoughtful mini-article. You can even consider scientific blog posts as a small online publication judged by your peers from networking. I think blogging will be widely accepted in the scientific mainstream only if it can bring some professional value, i.e., unique trusted information with the possibility of real time discussion in informal settings.
The blog as a professional networking tool
So I’m using a blog as a hub for gathering information picked from my bookmarks, and its analysis. In this case, high quality analytical information is an input, but what is the output? I consider a blog as a part of an online project, which connects the shared information with professionals working in the same field. In order to get the output I share links to my blog posts in professional networking web-services, such as LinkedIn. I’m networking in 20 LinkedIn professional groups, where I can submit discussion (as a forum) or share a link and switch to personal communication. Unexpectedly, I started to get more productive discussions about my blog posts on LinkedIn than on the blog itself. If people like my thoughts in the post, they contact me personally and make a connection. I was lucky enough to meet some people from my online connection on LinkedIn and Twitter in person through conferences. So professional networking online in your niche can be easily transformed to real connections.
Besides LinkedIn, I’m also submitting links to my posts to Twitter, sharing them in FriendFeed, Google Buzz, and Google Reader. I’m doing that because different people prefer different platforms for discussions online. I’m getting the maximum feedback only from all tools combined, where I share my blog posts. Recently, I’ve gotten more than 35 comments in LinkedIn and 10 comments on Google Buzz on one of my recent posts (Do we really need hematopoietic stem cell expansion for clinical use?), but nothing on the blog itself. Sometimes, I have discussion only via emails, because some scientists do not trust blogs and hesitate to post information online for public exposure.
So, discussion about my blog posts can occur anywhere: comments under the post itself, comments in LinkedIn groups, replies on Twitter, comments on FriendFeed, and personal communication via email. I think that using a few tools together makes your networking online more productive and valuable.
From personal filter to collaborative filter
Scientists like to collaborate. I started to collaborate online simply by sharing drafts of my blog posts with my friends via Google Documents. I asked their opinions about the draft, and even for them to check my grammar. It was my first experience with sharing documents online. Later, I was trying to move from my personal information filters to collaborative filters.
Collaborative filters aim to sort the information stream from the popular (mass-media) and search engines (Google, PubMed) to professional user-trusted content with the possibility of discussion and collaboration [7]. The blog could be a good start for setting up a collaborative filter in your professional niche. You can use FF-like a tool to filter “trusted content” recommended to you by friends and experts, but not search engines [8]. Today we can use a number of tools for collaborative filters with or without blogging.
I was always thinking about how to move the blog with my professional networking to collaboration. Via my connections online I simply sent a message and found a person who was interested in an online collaboration with me in setting up a new project – Stem Cell Assays. This project is dedicated to promoting rigorous reproducible results in stem cell research by sharing methods.
Another example of collaboration online is to make a community project. I created a Google Wave “Cell processing devices in cell therapy”, made it public (everyone can read it) and embedded it into a Stem Cell Assays blog post. The link to this blog post went to LinkedIn groups and Twitter. The next day I got very good traffic from LinkedIn, but again people didn’t comment on the blog post. Instead, I got some nice feedback in comments on LinkedIn and some people came directly to the Google Wave and started to update information in real time.
Links

Connotea
EndNote
Facebook
FriendFeed
Google Buzz
Google Documents
Google Reader
Google Wave
Hematopoiesis
LinkedIn
Mendeley
Nature Network
Papers
PubMed
Research Blogging
ScienceBlogs
Twitter
Zotero
Figure 1. The model of scientific blogging as a platform for professional networking online
Concluding remarks and future perspectives
There is a lot of discussion going on on the Web about the future of scientific blogging [9]. Will academic blogging advance your career [10] or is it a waste of time? Scientific blogging is evolving [11]. I think blogs and scientific blogging in particular will survive and take a very precise niche among the variety of other web tools, only if it can provide trusted, valid, and useful content. Some analytical blog posts with ideas could be cited [12] in scientific papers. Blogs will play more of a role in “article-level metrics” [13] if the paper was mentioned by a blogger. Real time and updatable comments more likely will not be anonymous [14] and more valuable for scientific community. This could be the biggest advantage compared to traditionally published papers.
Taking into account all of the good things about scientific blogging, I wouldn’t say that everyone should do it. You should try to blog if you’re curious and motivated enough to do it. Not every scientist is very social and curious about web tools. Not every scientist feels like sharing information online [15] and being publically exposed [16]. Importantly, scientific blogging is your continuous contribution in science after hours. So, you have to feel a strong commitment to a particular scientific field (your niche) and also realize that it’s time consuming. You should be responsible for high quality valid content, which could be citable and trusted by your peers. Scientific bloggers also have to realize that unpublished information (that you have heard from yesterday’s talk, for example) should be very carefully chosen, and that its release is not going to hurt your colleagues. Only in this case you can build your “scientific equity” or authority successfully.
I think that the proposed model (Figure 1) of scientific blogging as an online networking tool will work the best for junior investigators, e.g., PhD students, postdoctoral fellows and young PIs. In part, because these categories of people don’t have enough scientific authority yet to be heard by established academic professors, clinicians and business executives. When a young generation of scientists is coming to LinkedIn to discuss recent advances and controversies they have much less chance to be heard by established and respected scientists. In this case, building a meaningful foundation online, such a blog, could work nicely in order to network professionally at a high level.
Acknowledgements
I declare no conflict of interest.
I’d like to thank Joanna Balcerek (Robert Wood Johnson Medical School, New Brunswick, NJ, USA) for her contribution to the Hematopoiesis.info project and for reviewing this manuscript.
References
1. Crotty David. Web 2.0 for Biologists–Are any of the current tools worth using? Bench Marks blog. April 3, 2008. http://www.cshblogs.org/cshprotocols/2008/04/03/web-20-for-biologists-are-any-of-the-current-tools-worth-using/
2. Fenner Martin. Why do we blog and other important questions, answered by 34 science bloggers. Gobbledygook blog. November 30, 2008. http://blogs.nature.com/mfenner/2008/11/30/why-do-we-blog-and-other-important-questions-answered-by-34-science-bloggers
3. Brown Daniel. Science blogging: The future of science communication & why you should be a part of it. Biochemical Soul blog. March 17, 2009.
http://biochemicalsoul.com/2009/03/science-blogging-the-future-of-science-communication-why-you-should-be-a-part-of-it/
4. Fenner Martin. What is a reference manager? Gobbledygook blog. May 19, 2010;
http://blogs.nature.com/mfenner/2010/05/19/post
5. Fenner Martin. What is the right reference manager for you? SlideShare presentation.
http://www.slideshare.net/mfenner/which-reference-manager
6. Bersenev Alexey. How FriendFeed is killing blogging. Hematopoiesis blog. Septermber 3, 2009.
http://hematopoiesis.info/2008/09/03/how-friendfeed-is-killing-blogging/
7. Bersenev Alexey. Collaborative filters online. Hematopoiesis blog. January 26, 2009.
http://hematopoiesis.info/2009/01/26/collaborative-filters-online/
8. Rubel Steve. Friendfeed can disrupt search and reshape advertising. Micro Persuasion blog. June 11, 2008. http://www.micropersuasion.com/2008/06/friendfeed-can.html
9. Neylon Cameron. The nature of science blog networks. Science in the Open blog. July 25, 2010.
http://cameronneylon.net/blog/the-nature-of-science-blog-networks/
10. Lemire Daniel. The negative myths about academic blogging. Daniel Lemire's blog. April 4, 2008.
http://www.daniel-lemire.com/blog/archives/2008/04/04/the-negative-myths-about-academic-blogging/
11. Zivkovic Bora. A farewell to Scienceblogs: the changing science blogging ecosystem. Blog Around the Clock. July 19, 2010. http://coturnix.wordpress.com/2010/07/19/a-farewell-to-scienceblogs-the-changing-science-blogging-ecosystem/
12. Zivkovic Bora. Why or why not cite blog posts in scientific papers? Blog Around the Clock. June 11, 2009. http://scienceblogs.com/clock/2009/06/why_or_why_not_cite_blog_posts.php
13. Article-level metrics information. PLoS ONE.
http://www.plosone.org/static/almInfo.action
14. Gunn William. Online Engagement of Scientists with the literature: anonymity vs. ResearcherID. Synthesis blog. May 24, 2009. http://synthesis.williamgunn.org/2009/05/24/online-engagement-of-scientists-with-the-literature-anonymity-vs-researcherid/
15. Bersenev Alexey. What makes scientists not comment online? Hematopoiesis blog. April 6, 2009. http://hematopoiesis.info/2008/04/06/what-makes-scientists-not-comment-online/
16. When blogs make sense. Editorial. Nature 2010;466:8. doi:10.1038/466008a
" ["DETAIL_TEXT_TYPE"]=> string(4) "html" ["~DETAIL_TEXT_TYPE"]=> string(4) "html" ["PREVIEW_TEXT"]=> string(0) "" ["~PREVIEW_TEXT"]=> string(0) "" ["PREVIEW_TEXT_TYPE"]=> string(4) "text" ["~PREVIEW_TEXT_TYPE"]=> string(4) "text" ["PREVIEW_PICTURE"]=> NULL ["~PREVIEW_PICTURE"]=> NULL ["LANG_DIR"]=> string(4) "/ru/" ["~LANG_DIR"]=> string(4) "/ru/" ["SORT"]=> string(3) "500" ["~SORT"]=> string(3) "500" ["CODE"]=> string(81) "nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn" ["~CODE"]=> string(81) "nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn" ["EXTERNAL_ID"]=> string(4) "1435" ["~EXTERNAL_ID"]=> string(4) "1435" ["IBLOCK_TYPE_ID"]=> string(7) "journal" ["~IBLOCK_TYPE_ID"]=> string(7) "journal" ["IBLOCK_CODE"]=> string(7) "volumes" ["~IBLOCK_CODE"]=> string(7) "volumes" ["IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["~IBLOCK_EXTERNAL_ID"]=> string(1) "2" ["LID"]=> string(2) "s2" ["~LID"]=> string(2) "s2" ["EDIT_LINK"]=> NULL ["DELETE_LINK"]=> NULL ["DISPLAY_ACTIVE_FROM"]=> string(0) "" ["IPROPERTY_VALUES"]=> array(18) { ["ELEMENT_META_TITLE"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["ELEMENT_META_KEYWORDS"]=> string(0) "" ["ELEMENT_META_DESCRIPTION"]=> string(213) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайнScientific blogging as a model for professional networking online" ["ELEMENT_PREVIEW_PICTURE_FILE_ALT"]=> string(1767) "<p class="bodytext">Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.</p><h3>Ключевые слова</h3> <p> наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн</p>" ["ELEMENT_PREVIEW_PICTURE_FILE_TITLE"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["ELEMENT_DETAIL_PICTURE_FILE_ALT"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["ELEMENT_DETAIL_PICTURE_FILE_TITLE"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_META_TITLE"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_META_KEYWORDS"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_META_DESCRIPTION"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_PICTURE_FILE_ALT"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_PICTURE_FILE_TITLE"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_PICTURE_FILE_NAME"]=> string(85) "nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn-img" ["SECTION_DETAIL_PICTURE_FILE_ALT"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_DETAIL_PICTURE_FILE_TITLE"]=> string(148) "Научное ведение блога как модель профессиональной работы с помощью сетей онлайн" ["SECTION_DETAIL_PICTURE_FILE_NAME"]=> string(85) "nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn-img" ["ELEMENT_PREVIEW_PICTURE_FILE_NAME"]=> string(85) "nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn-img" ["ELEMENT_DETAIL_PICTURE_FILE_NAME"]=> string(85) "nauchnoe-vedenie-bloga-kak-model-professionalnoy-raboty-s-pomoshchyu-setey-onlayn-img" } ["FIELDS"]=> array(1) { ["IBLOCK_SECTION_ID"]=> string(2) "81" } ["PROPERTIES"]=> array(18) { ["KEYWORDS"]=> array(36) { ["ID"]=> string(2) "19" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:46:01" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(27) "Ключевые слова" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "KEYWORDS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "19" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "4" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "Y" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "Y" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> bool(false) ["VALUE"]=> bool(false) ["DESCRIPTION"]=> bool(false) ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> bool(false) ["~DESCRIPTION"]=> bool(false) ["~NAME"]=> string(27) "Ключевые слова" ["~DEFAULT_VALUE"]=> string(0) "" } ["SUBMITTED"]=> array(36) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19051" ["VALUE"]=> string(22) "07/23/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "07/23/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL } ["ACCEPTED"]=> array(36) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19052" ["VALUE"]=> string(22) "07/29/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "07/29/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL } ["PUBLISHED"]=> array(36) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19053" ["VALUE"]=> string(22) "08/02/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "08/02/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL } ["CONTACT"]=> array(36) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19054" ["VALUE"]=> string(4) "1434" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1434" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHORS"]=> array(36) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19069" } ["VALUE"]=> array(1) { [0]=> string(4) "1434" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1434" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_RU"]=> array(36) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19059" ["VALUE"]=> array(2) { ["TEXT"]=> string(50) "<p>Алексей Берсенев</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(38) "Алексей Берсенев
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_RU"]=> array(36) { ["ID"]=> string(2) "26" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(22) "Организации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "26" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(22) "Организации" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_RU"]=> array(36) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19060" ["VALUE"]=> array(2) { ["TEXT"]=> string(1767) "<p class="bodytext">Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.</p><h3>Ключевые слова</h3> <p> наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1721) "Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.
Ключевые слова
наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["DOI"]=> array(36) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19056" ["VALUE"]=> string(29) "10.3205/ctt-2010-en-000084.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2010-en-000084.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" } ["AUTHOR_EN"]=> array(36) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19062" ["VALUE"]=> array(2) { ["TEXT"]=> string(43) "<p>Alexey Bersenev, MD, PhD</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(31) "Alexey Bersenev, MD, PhD
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19063" ["VALUE"]=> array(2) { ["TEXT"]=> string(110) "<p>314G Abramson Research Center, Children’s Hospital of Philadelphia, Philadelphia, PA, USA</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(98) "314G Abramson Research Center, Children’s Hospital of Philadelphia, Philadelphia, PA, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19064" ["VALUE"]=> array(2) { ["TEXT"]=> string(1179) "<p> Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online. </p> <h3>Keywords</h3> <img width="160" alt="RTEmagicC_Bersenev_Keywords_01.gif" src="/upload/medialibrary/a6f/rtemagicc_bersenev_keywords_01.gif" height="160" title="RTEmagicC_Bersenev_Keywords_01.gif" align="left"> <div style="margin-left:190px;"> <p> science online, Web 2.0, blog, scientific blogging, networking </p> </div> " ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1055) "Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online.
Keywords

science online, Web 2.0, blog, scientific blogging, networking
Alexey Bersenev, MD, PhD
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(31) "Alexey Bersenev, MD, PhD
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19064" ["VALUE"]=> array(2) { ["TEXT"]=> string(1179) "<p> Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online. </p> <h3>Keywords</h3> <img width="160" alt="RTEmagicC_Bersenev_Keywords_01.gif" src="/upload/medialibrary/a6f/rtemagicc_bersenev_keywords_01.gif" height="160" title="RTEmagicC_Bersenev_Keywords_01.gif" align="left"> <div style="margin-left:190px;"> <p> science online, Web 2.0, blog, scientific blogging, networking </p> </div> " ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1055) "Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online.
Keywords

science online, Web 2.0, blog, scientific blogging, networking
Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online.
Keywords

science online, Web 2.0, blog, scientific blogging, networking
314G Abramson Research Center, Children’s Hospital of Philadelphia, Philadelphia, PA, USA
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(98) "314G Abramson Research Center, Children’s Hospital of Philadelphia, Philadelphia, PA, USA
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19069" } ["VALUE"]=> array(1) { [0]=> string(4) "1434" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1434" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(59) "Alexey Bersenev" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["AUTHOR_RU"]=> array(37) { ["ID"]=> string(2) "25" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "25" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19059" ["VALUE"]=> array(2) { ["TEXT"]=> string(50) "<p>Алексей Берсенев</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(38) "Алексей Берсенев
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(38) "Алексей Берсенев
" } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19051" ["VALUE"]=> string(22) "07/23/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "07/23/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "07/23/2010 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19052" ["VALUE"]=> string(22) "07/29/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "07/29/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "07/29/2010 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19053" ["VALUE"]=> string(22) "08/02/2010 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "08/02/2010 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "08/02/2010 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19054" ["VALUE"]=> string(4) "1434" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1434" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(59) "Alexey Bersenev" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUMMARY_RU"]=> array(37) { ["ID"]=> string(2) "27" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:01:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Описание/Резюме" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "27" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19060" ["VALUE"]=> array(2) { ["TEXT"]=> string(1767) "<p class="bodytext">Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.</p><h3>Ключевые слова</h3> <p> наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(1721) "Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.
Ключевые слова
наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Описание/Резюме" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(1721) "Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.
Ключевые слова
наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн
" } } } [9]=> array(49) { ["IBLOCK_SECTION_ID"]=> string(2) "81" ["~IBLOCK_SECTION_ID"]=> string(2) "81" ["ID"]=> string(4) "1443" ["~ID"]=> string(4) "1443" ["IBLOCK_ID"]=> string(1) "2" ["~IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(90) "Online medical content curation and personal time management with Web 2.0: an exciting era" ["~NAME"]=> string(90) "Online medical content curation and personal time management with Web 2.0: an exciting era" ["ACTIVE_FROM"]=> NULL ["~ACTIVE_FROM"]=> NULL ["TIMESTAMP_X"]=> string(22) "11/28/2017 02:08:34 pm" ["~TIMESTAMP_X"]=> string(22) "11/28/2017 02:08:34 pm" ["DETAIL_PAGE_URL"]=> string(124) "/en/archive/tom-2-nomer-3-7/forum/online-medical-content-curation-and-personal-time-management-with-web-2-0-an-exciting-era/" ["~DETAIL_PAGE_URL"]=> string(124) "/en/archive/tom-2-nomer-3-7/forum/online-medical-content-curation-and-personal-time-management-with-web-2-0-an-exciting-era/" ["LIST_PAGE_URL"]=> string(12) "/en/archive/" ["~LIST_PAGE_URL"]=> string(12) "/en/archive/" ["DETAIL_TEXT"]=> string(26120) "Introduction
The number of users seeking medical websites and health information online has been growing rapidly in the last few years [1]. Over 60% of Americans alone have searched for diseases, symptoms, or treatments [2]. Alongside this, the web usage of medical professionals is also growing [3]. With new web tools and applications, it is not only communication between patients that has gone through significant changes (e.g. Patientslikeme.com), but communication between medical professionals has become faster and more efficient, too, providing different opportunities depending on the particular medical specialty [4].
This article discusses the importance and the forms of online medical content curation as well as some time management tools and the advantages of crowdsourcing, which can save time and effort.
Although these opportunities seem to be obvious [5], judging the quality of medical online resources is still a crucial issue. Basically, it has two options: 1) learning the process of assessment, which takes years and a lot of effort; or 2) using online aggregators that feature resources selected by professionals and highlight the reason for inclusion. Currently, there is one free service worldwide curating social media by covering over 80 medical topics in over 17 languages, Webicina.com (Figure 1).
Figure 1. A new era in the relationship between medicine and the Internet

Other solutions that aggregate medical content online but not social media include Faculty of 1000, a post publication peer-review platform where Faculty Members can evaluate and rank particular papers published in the biomedical field; Medpedia, the medical alternative to Wikipedia; Health on the Net Foundation, a non-profit organization, and Medworm.com, among others (Table 1).
Table 1. List of online medical services focusing on content or resource curation
|
Name |
URL |
When was it founded? |
Who curates it? |
What is curated? |
|---|---|---|---|---|
|
Faculty of 1000 |
2002 |
Faculty Members |
Papers in medical journals |
|
|
Health on the Net Foundation |
1995 |
Group of medical professionals |
Medical websites and Blogs |
|
|
Healthcare Bloggers Code of Ethics |
Unknown |
Group of medical bloggers |
Medical blogs |
|
|
Medpedia |
2009 |
Group of medical professionals |
Medical content |
|
|
Medworm |
Frankie Dolan |
Websites and journals |
||
|
Webicina |
2008 |
Group of medical professionals |
Medical resources including Social media |
|
|
Cell Ther Transplant. 2011;3:e.000093.01. doi:10.3205/ctt-2011-en-000093-table1 |
||||
Online medical content curation
Before 2008, whenever I tried to find a good diabetes blog or quality cardiology resources, it took a lot of time to find them — not because I did not know how to search properly, but because it really takes time to learn how to assess the quality of medical websites. In this respect, the fields of politics and sports are totally different from medicine and healthcare. So I thought there should be a service that curates medical resources for patients and doctors — for free — and by using professionals and not algorithms or search engines. Webicina was launched in 2008 and now has over 3000 curated resources, from blogs and podcasts to wikis and mobile apps, focusing on 80 medical specialties or conditions in 17 languages; and all these numbers are constantly growing.
Webicina has thousands of collaborators from around the world, and these are medical professionals as well as empowered patients. Anyone can join this project. Usually, we come up with a selection of social media resources focusing on a medical specialty or condition, and as there are several simple ways to contribute to these databases, users send us hundreds of suggestions weekly, which we try to process as quickly as possible. Each resource that is included in Webicina goes through a rigorous evaluation and review process that is based on the quality of health information in the resource, whether the authors are identifiable, whether a description, privacy policy, disclaimer and contact information are available, and several other factors. That is how we can make sure all resources are curated and relevant.
Although not all patients and not all doctors are going to be web-savvy, today’s trend seems to point in the direction of more and more patients becoming so-called e-patients who strategically use the Internet in their health management. But in my experience, the number of web-savvy doctors is not growing so quickly, so there is a huge gap that should be filled somehow. I try to help this process in 2 ways: 1) Webicina offers free services to professionals about using the Internet more effectively and efficiently, and 2) I teach medical, dentistry, pharmacy, and public health students at my university about using social media in medicine. This is the first accredited course of its kind in the world.
Efficient time management with Web 2.0
I first became active in Web 2.0/social media back in 2005 when I realized whenever I did a search for any terms, I ended up on Wikipedia, where I could edit the entries, especially the genetics-related ones. So I became a Wikipedia editor, and later in 2006, an administrator. A few months later, I came across Wordpress.com and launched my medical blog, Scienceroll.com, which received a special mention in Medgadget’s Weblog Awards a few months later; giving me the idea that I should keep on blogging and take it very seriously. At the time, I was a 3rd year medical student.
These tools and resources now play a huge role in my life: they connect me to people, colleagues from around the world, they let me see what’s happening in the world in my fields of interest; they help me collaborate and discover new aspects of my work. Obviously, Wikipedia is still close to my heart, and I also liked Google Mail from the first moments. At the time, there was no YouTube, Twitter, Facebook, or Friendfeed, so generally I visited the websites of medical journals such as NEJM, BMJ, and Nature quite regularly. Years ago, open access journals were not as widespread in my field as they are now. It is enough to mention PLoS and BMC.
As it strikes me, we have moved from websites to resources or services such as Twitter or Facebook. While all of these can be individualized, I believe these are now centered around cloud computing. The reason I manage accounts on many services is that after building medical communities on Twitter, Friendfeed or Facebook for years, I can now get quite a clear picture of what’s happening in genomics and in medicine 2.0 day by day without actively searching for information. My communities, my clouds, filter the huge amount of incoming medical information for me without even knowing it. That is why it is really worth keeping all of these active. Although it is true that I might miss newcomers in this way, in my opinion it is the crowd that is crucial, not the individual.
I use web 2.0 very actively both because of my PhD studies in genomics, and also my online activities related to blogging and Webicina.com.
Table 2. Differences in my online activities between 2000 and today
|
What would I do if |
In 2000 |
Now |
|---|---|---|
|
I need clinical answer |
Try to find a colleague who knows it |
Post a question on Twitter |
|
I want to hear a patient's story about a specific condition |
Try to find a patient in my town |
Read blogs, watch YouTube |
|
I want to be up-to-date |
Go to the library once a week |
Use RSS and follow hundreds of journals |
|
I want to work on a manuscript with my team |
We gather around the table |
Use Google Docs without geographical limits |
|
Cell Ther Transplant. 2011;3:e.000093.01. doi:10.3205/ctt-2011-en-000093-table2 |
||
I have several blogs on Wordpress.com, I use Twitter.com every day as a filter that collects the most interesting news for me, Friendfeed.com for science-related discussions, and Google Reader for keeping myself up-to-date by following the RSS feeds of over 300 medical journals and blogs. I consider Gmail the center of my online activities. It is here that I store to-do lists and notes to myself. I created medical/genetic Facebook groups so I can see what kind of articles they share day by day and I do all collaborative projects in Google Docs.
Staying up-to-date in one of the most emerging scientific fields
Crowdsourcing is crucial today. I check the best-of-the-day feature on Friendfeed, because I have hundreds of scientific contacts there who select the most important scientific news and discussions every day. On Twitter I do the same but for medicine, and Facebook for me is more about keeping up with what is happening with my colleagues from around the world and what kind of projects they are launching. Google Reader is for news sites and blogs, and I use Webicina’s PeRSSonalized Medicine to see the latest improvements in genomics.
I graduated from medical school in 2009 and immediately started a PhD in the field of personal genomics. It was an important change because 1) I had wanted to become a geneticist since my childhood, and 2) I had more time now than in medical school. It means these days I can focus on genomics research from morning until the afternoon, while at night I have time to update my blog, check the updates of my online accounts and work on my projects related to medicine in social media. The biggest issue in my career was to find the best resources/tools for different purposes.
If you want to communicate with people, start browsing Twitter, if you want to collaborate online, take a look at Google Docs, Dropbox, etc. Obviously, not all doctors and patients can and should use all the services I use, but this may be a way to find the resources and services they really need — and only those that can facilitate their online activities.
Of course, despite that fact that web 2.0 can provide numerous opportunities for collaboration, reputation management, and communication, it has plenty of dangers. More and more patients want to friend their doctors on Facebook, which is inappropriate in my view. Medical students share party photos online while they are not really aware of their privacy settings. Medical bloggers are sued because of their blogs, and there are many other examples. I believe the only solution here is to educate the medical community about these dangers and also publish guides for patients about how to use the Internet in their health management safely and efficiently. That is what we try to do on Webicina.com.
Web 2.0 activities and also the open access approach are seriously changing medical research. If the scientific community is open to these new tools and resources, it will significantly change communication, ways of collaboration, and possibly publication too. Scientists can now find each other easily through, e.g., ResearchGATE, share scientific news on, e.g., Friendfeed, and assess the importance of publications by categories on, e.g., BioWizard. During my PhD training, I do a lot of things online: keep myself up-to-date, collaborate, write papers, find papers, find colleagues, publish reports, get feedback through my blog for my research projects, ask specific questions on Twitter, and more. A paper on using Wikipedia as a global public health promotion tool was just published by our team of medical Wikipedia editors in an open access journal and this was really an international online collaboration. Web 2.0 totally formed the way I do my research.
There are strict guidelines for citing blogs in medical journals, and I myself come across cited medical blog entries in peer-reviewed journals more and more often. As a Wikipedia admin and long-time editor, I’m totally sure that what matters online is the quality of information instead of credentials and platforms. If you think that everything you read in medical papers is perfect, take a look at the blog called Retraction Watch. I think both patients and professionals should learn how to assess the quality of online medical information, or at least they should use free services that help them do so.
Conclusions
Content curation is a key element in the future of Internet technologies from the medical perspective. As the number of online medical resources and people seeking medical information is constantly growing, there is a clear need for a free service providing selected resources both for medical professionals and patients.
In order to be able to handle this huge amount of online medical information, time management tools combined with crowdsourcing are becoming crucial parts of the lives of medical professionals. Becoming active in the web 2.0 world takes only a few minutes if we find the resources that can help us the most.
Acknowledgements
The author is the managing director of Webicina.com.
References
1. Mesko B, and Dubecz A. New possibilities provided by the internet in medicine. Orv Hetil 148. 2007:2095-2099.
2. Susannah Fox SJ. The Social Life of Health Information. Pew Internet Project. 2009.
Recommended further reading
1. Sara Kjellberg. I am a blogging researcher: Motivations for blogging in a scholarly context. First Monday, Volume 15, Number 8, 2 August 2010.
2. Catherine Gray. If you build it, will they come? How researchers perceive and use web 2.0, 06 July 2010.
3. Bertalan Mesko. Internet in Medicine: 2000 vs 2010.
4. Richard Gordon and Bryan J. Poulin. There is but one journal: the scientific literature. Comment on: Young NS, Ioannidis JPA, Al-Ubaydli O, 2008. Why Current Publication Practices May Distort Science. PLoS Med 5(10):e201. doi:10.1371/journal.pmed.0050201.
5. Abigail De Kosnik. Teaching with Google Docs, or, How to Teach in a Digital Media Lab without Losing Students’ Attention. In: Learning through Digital Media, Essays on Technology and Pedagogy (in open peer review phase).
Introduction
The number of users seeking medical websites and health information online has been growing rapidly in the last few years [1]. Over 60% of Americans alone have searched for diseases, symptoms, or treatments [2]. Alongside this, the web usage of medical professionals is also growing [3]. With new web tools and applications, it is not only communication between patients that has gone through significant changes (e.g. Patientslikeme.com), but communication between medical professionals has become faster and more efficient, too, providing different opportunities depending on the particular medical specialty [4].
This article discusses the importance and the forms of online medical content curation as well as some time management tools and the advantages of crowdsourcing, which can save time and effort.
Although these opportunities seem to be obvious [5], judging the quality of medical online resources is still a crucial issue. Basically, it has two options: 1) learning the process of assessment, which takes years and a lot of effort; or 2) using online aggregators that feature resources selected by professionals and highlight the reason for inclusion. Currently, there is one free service worldwide curating social media by covering over 80 medical topics in over 17 languages, Webicina.com (Figure 1).
Figure 1. A new era in the relationship between medicine and the Internet

Other solutions that aggregate medical content online but not social media include Faculty of 1000, a post publication peer-review platform where Faculty Members can evaluate and rank particular papers published in the biomedical field; Medpedia, the medical alternative to Wikipedia; Health on the Net Foundation, a non-profit organization, and Medworm.com, among others (Table 1).
Table 1. List of online medical services focusing on content or resource curation
|
Name |
URL |
When was it founded? |
Who curates it? |
What is curated? |
|---|---|---|---|---|
|
Faculty of 1000 |
2002 |
Faculty Members |
Papers in medical journals |
|
|
Health on the Net Foundation |
1995 |
Group of medical professionals |
Medical websites and Blogs |
|
|
Healthcare Bloggers Code of Ethics |
Unknown |
Group of medical bloggers |
Medical blogs |
|
|
Medpedia |
2009 |
Group of medical professionals |
Medical content |
|
|
Medworm |
Frankie Dolan |
Websites and journals |
||
|
Webicina |
2008 |
Group of medical professionals |
Medical resources including Social media |
|
|
Cell Ther Transplant. 2011;3:e.000093.01. doi:10.3205/ctt-2011-en-000093-table1 |
||||
Online medical content curation
Before 2008, whenever I tried to find a good diabetes blog or quality cardiology resources, it took a lot of time to find them — not because I did not know how to search properly, but because it really takes time to learn how to assess the quality of medical websites. In this respect, the fields of politics and sports are totally different from medicine and healthcare. So I thought there should be a service that curates medical resources for patients and doctors — for free — and by using professionals and not algorithms or search engines. Webicina was launched in 2008 and now has over 3000 curated resources, from blogs and podcasts to wikis and mobile apps, focusing on 80 medical specialties or conditions in 17 languages; and all these numbers are constantly growing.
Webicina has thousands of collaborators from around the world, and these are medical professionals as well as empowered patients. Anyone can join this project. Usually, we come up with a selection of social media resources focusing on a medical specialty or condition, and as there are several simple ways to contribute to these databases, users send us hundreds of suggestions weekly, which we try to process as quickly as possible. Each resource that is included in Webicina goes through a rigorous evaluation and review process that is based on the quality of health information in the resource, whether the authors are identifiable, whether a description, privacy policy, disclaimer and contact information are available, and several other factors. That is how we can make sure all resources are curated and relevant.
Although not all patients and not all doctors are going to be web-savvy, today’s trend seems to point in the direction of more and more patients becoming so-called e-patients who strategically use the Internet in their health management. But in my experience, the number of web-savvy doctors is not growing so quickly, so there is a huge gap that should be filled somehow. I try to help this process in 2 ways: 1) Webicina offers free services to professionals about using the Internet more effectively and efficiently, and 2) I teach medical, dentistry, pharmacy, and public health students at my university about using social media in medicine. This is the first accredited course of its kind in the world.
Efficient time management with Web 2.0
I first became active in Web 2.0/social media back in 2005 when I realized whenever I did a search for any terms, I ended up on Wikipedia, where I could edit the entries, especially the genetics-related ones. So I became a Wikipedia editor, and later in 2006, an administrator. A few months later, I came across Wordpress.com and launched my medical blog, Scienceroll.com, which received a special mention in Medgadget’s Weblog Awards a few months later; giving me the idea that I should keep on blogging and take it very seriously. At the time, I was a 3rd year medical student.
These tools and resources now play a huge role in my life: they connect me to people, colleagues from around the world, they let me see what’s happening in the world in my fields of interest; they help me collaborate and discover new aspects of my work. Obviously, Wikipedia is still close to my heart, and I also liked Google Mail from the first moments. At the time, there was no YouTube, Twitter, Facebook, or Friendfeed, so generally I visited the websites of medical journals such as NEJM, BMJ, and Nature quite regularly. Years ago, open access journals were not as widespread in my field as they are now. It is enough to mention PLoS and BMC.
As it strikes me, we have moved from websites to resources or services such as Twitter or Facebook. While all of these can be individualized, I believe these are now centered around cloud computing. The reason I manage accounts on many services is that after building medical communities on Twitter, Friendfeed or Facebook for years, I can now get quite a clear picture of what’s happening in genomics and in medicine 2.0 day by day without actively searching for information. My communities, my clouds, filter the huge amount of incoming medical information for me without even knowing it. That is why it is really worth keeping all of these active. Although it is true that I might miss newcomers in this way, in my opinion it is the crowd that is crucial, not the individual.
I use web 2.0 very actively both because of my PhD studies in genomics, and also my online activities related to blogging and Webicina.com.
Table 2. Differences in my online activities between 2000 and today
|
What would I do if |
In 2000 |
Now |
|---|---|---|
|
I need clinical answer |
Try to find a colleague who knows it |
Post a question on Twitter |
|
I want to hear a patient's story about a specific condition |
Try to find a patient in my town |
Read blogs, watch YouTube |
|
I want to be up-to-date |
Go to the library once a week |
Use RSS and follow hundreds of journals |
|
I want to work on a manuscript with my team |
We gather around the table |
Use Google Docs without geographical limits |
|
Cell Ther Transplant. 2011;3:e.000093.01. doi:10.3205/ctt-2011-en-000093-table2 |
||
I have several blogs on Wordpress.com, I use Twitter.com every day as a filter that collects the most interesting news for me, Friendfeed.com for science-related discussions, and Google Reader for keeping myself up-to-date by following the RSS feeds of over 300 medical journals and blogs. I consider Gmail the center of my online activities. It is here that I store to-do lists and notes to myself. I created medical/genetic Facebook groups so I can see what kind of articles they share day by day and I do all collaborative projects in Google Docs.
Staying up-to-date in one of the most emerging scientific fields
Crowdsourcing is crucial today. I check the best-of-the-day feature on Friendfeed, because I have hundreds of scientific contacts there who select the most important scientific news and discussions every day. On Twitter I do the same but for medicine, and Facebook for me is more about keeping up with what is happening with my colleagues from around the world and what kind of projects they are launching. Google Reader is for news sites and blogs, and I use Webicina’s PeRSSonalized Medicine to see the latest improvements in genomics.
I graduated from medical school in 2009 and immediately started a PhD in the field of personal genomics. It was an important change because 1) I had wanted to become a geneticist since my childhood, and 2) I had more time now than in medical school. It means these days I can focus on genomics research from morning until the afternoon, while at night I have time to update my blog, check the updates of my online accounts and work on my projects related to medicine in social media. The biggest issue in my career was to find the best resources/tools for different purposes.
If you want to communicate with people, start browsing Twitter, if you want to collaborate online, take a look at Google Docs, Dropbox, etc. Obviously, not all doctors and patients can and should use all the services I use, but this may be a way to find the resources and services they really need — and only those that can facilitate their online activities.
Of course, despite that fact that web 2.0 can provide numerous opportunities for collaboration, reputation management, and communication, it has plenty of dangers. More and more patients want to friend their doctors on Facebook, which is inappropriate in my view. Medical students share party photos online while they are not really aware of their privacy settings. Medical bloggers are sued because of their blogs, and there are many other examples. I believe the only solution here is to educate the medical community about these dangers and also publish guides for patients about how to use the Internet in their health management safely and efficiently. That is what we try to do on Webicina.com.
Web 2.0 activities and also the open access approach are seriously changing medical research. If the scientific community is open to these new tools and resources, it will significantly change communication, ways of collaboration, and possibly publication too. Scientists can now find each other easily through, e.g., ResearchGATE, share scientific news on, e.g., Friendfeed, and assess the importance of publications by categories on, e.g., BioWizard. During my PhD training, I do a lot of things online: keep myself up-to-date, collaborate, write papers, find papers, find colleagues, publish reports, get feedback through my blog for my research projects, ask specific questions on Twitter, and more. A paper on using Wikipedia as a global public health promotion tool was just published by our team of medical Wikipedia editors in an open access journal and this was really an international online collaboration. Web 2.0 totally formed the way I do my research.
There are strict guidelines for citing blogs in medical journals, and I myself come across cited medical blog entries in peer-reviewed journals more and more often. As a Wikipedia admin and long-time editor, I’m totally sure that what matters online is the quality of information instead of credentials and platforms. If you think that everything you read in medical papers is perfect, take a look at the blog called Retraction Watch. I think both patients and professionals should learn how to assess the quality of online medical information, or at least they should use free services that help them do so.
Conclusions
Content curation is a key element in the future of Internet technologies from the medical perspective. As the number of online medical resources and people seeking medical information is constantly growing, there is a clear need for a free service providing selected resources both for medical professionals and patients.
In order to be able to handle this huge amount of online medical information, time management tools combined with crowdsourcing are becoming crucial parts of the lives of medical professionals. Becoming active in the web 2.0 world takes only a few minutes if we find the resources that can help us the most.
Acknowledgements
The author is the managing director of Webicina.com.
References
1. Mesko B, and Dubecz A. New possibilities provided by the internet in medicine. Orv Hetil 148. 2007:2095-2099.
2. Susannah Fox SJ. The Social Life of Health Information. Pew Internet Project. 2009.
Recommended further reading
1. Sara Kjellberg. I am a blogging researcher: Motivations for blogging in a scholarly context. First Monday, Volume 15, Number 8, 2 August 2010.
2. Catherine Gray. If you build it, will they come? How researchers perceive and use web 2.0, 06 July 2010.
3. Bertalan Mesko. Internet in Medicine: 2000 vs 2010.
4. Richard Gordon and Bryan J. Poulin. There is but one journal: the scientific literature. Comment on: Young NS, Ioannidis JPA, Al-Ubaydli O, 2008. Why Current Publication Practices May Distort Science. PLoS Med 5(10):e201. doi:10.1371/journal.pmed.0050201.
5. Abigail De Kosnik. Teaching with Google Docs, or, How to Teach in a Digital Media Lab without Losing Students’ Attention. In: Learning through Digital Media, Essays on Technology and Pedagogy (in open peer review phase).
Bertalan Mesko, MD
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["ORGANIZATION_EN"]=> array(36) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19167" ["VALUE"]=> array(2) { ["TEXT"]=> string(52) "<p>Managing director of Webicina.com</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(40) "Managing director of Webicina.com
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["SUMMARY_EN"]=> array(36) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19168" ["VALUE"]=> array(2) { ["TEXT"]=> string(642) "<p>The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.</p> <h3>Keywords</h3> <p>Internet, content curation, time management, Web 2.0</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(606) "The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.
Keywords
Internet, content curation, time management, Web 2.0
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["NAME_EN"]=> array(36) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19164" ["VALUE"]=> string(90) "Online medical content curation and personal time management with Web 2.0: an exciting era" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(90) "Online medical content curation and personal time management with Web 2.0: an exciting era" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" } ["FULL_TEXT_RU"]=> array(36) { ["ID"]=> string(2) "42" ["TIMESTAMP_X"]=> string(19) "2015-09-07 20:29:18" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(23) "Полный текст" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(12) "FULL_TEXT_RU" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "42" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(23) "Полный текст" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } } ["PDF_RU"]=> array(36) { ["ID"]=> string(2) "43" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF RUS" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_RU" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "43" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(7) "PDF RUS" ["~DEFAULT_VALUE"]=> string(0) "" } ["PDF_EN"]=> array(36) { ["ID"]=> string(2) "44" ["TIMESTAMP_X"]=> string(19) "2015-09-09 16:05:20" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(7) "PDF ENG" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(6) "PDF_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "F" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "44" ["FILE_TYPE"]=> string(18) "doc, txt, rtf, pdf" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19169" ["VALUE"]=> string(3) "939" ["DESCRIPTION"]=> NULL ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(3) "939" ["~DESCRIPTION"]=> NULL ["~NAME"]=> string(7) "PDF ENG" ["~DEFAULT_VALUE"]=> string(0) "" } ["NAME_LONG"]=> array(36) { ["ID"]=> string(2) "45" ["TIMESTAMP_X"]=> string(19) "2023-04-13 00:55:00" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(72) "Название (для очень длинных заголовков)" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "NAME_LONG" ["DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "45" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(80) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> NULL ["VALUE"]=> string(0) "" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(0) "" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(72) "Название (для очень длинных заголовков)" ["~DEFAULT_VALUE"]=> array(2) { ["TYPE"]=> string(4) "HTML" ["TEXT"]=> string(0) "" } } } ["DISPLAY_PROPERTIES"]=> array(10) { ["AUTHOR_EN"]=> array(37) { ["ID"]=> string(2) "37" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(6) "Author" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "AUTHOR_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "37" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19166" ["VALUE"]=> array(2) { ["TEXT"]=> string(37) "<p>Bertalan Mesko, MD</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(25) "Bertalan Mesko, MD
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(6) "Author" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(25) "Bertalan Mesko, MD
" } ["SUMMARY_EN"]=> array(37) { ["ID"]=> string(2) "39" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Description / Summary" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(10) "SUMMARY_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "39" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19168" ["VALUE"]=> array(2) { ["TEXT"]=> string(642) "<p>The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.</p> <h3>Keywords</h3> <p>Internet, content curation, time management, Web 2.0</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(606) "The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.
Keywords
Internet, content curation, time management, Web 2.0
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Description / Summary" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(606) "The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.
Keywords
Internet, content curation, time management, Web 2.0
" } ["DOI"]=> array(37) { ["ID"]=> string(2) "28" ["TIMESTAMP_X"]=> string(19) "2016-04-06 14:11:12" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(3) "DOI" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(3) "DOI" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "28" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19163" ["VALUE"]=> string(29) "10.3205/ctt-2011-en-000093.01" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(29) "10.3205/ctt-2011-en-000093.01" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(3) "DOI" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(29) "10.3205/ctt-2011-en-000093.01" } ["NAME_EN"]=> array(37) { ["ID"]=> string(2) "40" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:49:47" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(4) "Name" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "NAME_EN" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "80" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "40" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> NULL ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19164" ["VALUE"]=> string(90) "Online medical content curation and personal time management with Web 2.0: an exciting era" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(90) "Online medical content curation and personal time management with Web 2.0: an exciting era" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(4) "Name" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(90) "Online medical content curation and personal time management with Web 2.0: an exciting era" } ["ORGANIZATION_EN"]=> array(37) { ["ID"]=> string(2) "38" ["TIMESTAMP_X"]=> string(19) "2015-09-02 18:02:59" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Organization" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(15) "ORGANIZATION_EN" ["DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "38" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(4) "HTML" ["USER_TYPE_SETTINGS"]=> array(1) { ["height"]=> int(200) } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19167" ["VALUE"]=> array(2) { ["TEXT"]=> string(52) "<p>Managing director of Webicina.com</p>" ["TYPE"]=> string(4) "HTML" } ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(2) { ["TEXT"]=> string(40) "Managing director of Webicina.com
" ["TYPE"]=> string(4) "HTML" } ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(12) "Organization" ["~DEFAULT_VALUE"]=> array(2) { ["TEXT"]=> string(0) "" ["TYPE"]=> string(4) "HTML" } ["DISPLAY_VALUE"]=> string(40) "Managing director of Webicina.com
" } ["AUTHORS"]=> array(38) { ["ID"]=> string(2) "24" ["TIMESTAMP_X"]=> string(19) "2015-09-03 10:45:07" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(12) "Авторы" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "AUTHORS" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "Y" ["XML_ID"]=> string(2) "24" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> array(1) { [0]=> string(5) "19172" } ["VALUE"]=> array(1) { [0]=> string(4) "1442" } ["DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> array(1) { [0]=> string(4) "1442" } ["~DESCRIPTION"]=> array(1) { [0]=> string(0) "" } ["~NAME"]=> string(12) "Авторы" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(58) "Bertalan Mesko" ["LINK_ELEMENT_VALUE"]=> bool(false) } ["SUBMITTED"]=> array(37) { ["ID"]=> string(2) "20" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(21) "Дата подачи" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "SUBMITTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "20" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19158" ["VALUE"]=> string(22) "01/02/2011 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "01/02/2011 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(21) "Дата подачи" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "01/02/2011 12:00:00 am" } ["ACCEPTED"]=> array(37) { ["ID"]=> string(2) "21" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(25) "Дата принятия" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(8) "ACCEPTED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "21" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19159" ["VALUE"]=> string(22) "09/09/2011 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "09/09/2011 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(25) "Дата принятия" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "09/09/2011 12:00:00 am" } ["PUBLISHED"]=> array(37) { ["ID"]=> string(2) "22" ["TIMESTAMP_X"]=> string(19) "2015-09-02 17:21:42" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(29) "Дата публикации" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(9) "PUBLISHED" ["DEFAULT_VALUE"]=> NULL ["PROPERTY_TYPE"]=> string(1) "S" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "22" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "0" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "N" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(8) "DateTime" ["USER_TYPE_SETTINGS"]=> NULL ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19160" ["VALUE"]=> string(22) "12/10/2011 12:00:00 am" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(22) "12/10/2011 12:00:00 am" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(29) "Дата публикации" ["~DEFAULT_VALUE"]=> NULL ["DISPLAY_VALUE"]=> string(32) "12/10/2011 12:00:00 am" } ["CONTACT"]=> array(38) { ["ID"]=> string(2) "23" ["TIMESTAMP_X"]=> string(19) "2015-09-03 14:43:05" ["IBLOCK_ID"]=> string(1) "2" ["NAME"]=> string(14) "Контакт" ["ACTIVE"]=> string(1) "Y" ["SORT"]=> string(3) "500" ["CODE"]=> string(7) "CONTACT" ["DEFAULT_VALUE"]=> string(0) "" ["PROPERTY_TYPE"]=> string(1) "E" ["ROW_COUNT"]=> string(1) "1" ["COL_COUNT"]=> string(2) "30" ["LIST_TYPE"]=> string(1) "L" ["MULTIPLE"]=> string(1) "N" ["XML_ID"]=> string(2) "23" ["FILE_TYPE"]=> string(0) "" ["MULTIPLE_CNT"]=> string(1) "5" ["TMP_ID"]=> NULL ["LINK_IBLOCK_ID"]=> string(1) "3" ["WITH_DESCRIPTION"]=> string(1) "N" ["SEARCHABLE"]=> string(1) "N" ["FILTRABLE"]=> string(1) "N" ["IS_REQUIRED"]=> string(1) "Y" ["VERSION"]=> string(1) "1" ["USER_TYPE"]=> string(13) "EAutocomplete" ["USER_TYPE_SETTINGS"]=> array(9) { ["VIEW"]=> string(1) "E" ["SHOW_ADD"]=> string(1) "Y" ["MAX_WIDTH"]=> int(0) ["MIN_HEIGHT"]=> int(24) ["MAX_HEIGHT"]=> int(1000) ["BAN_SYM"]=> string(2) ",;" ["REP_SYM"]=> string(1) " " ["OTHER_REP_SYM"]=> string(0) "" ["IBLOCK_MESS"]=> string(1) "N" } ["HINT"]=> string(0) "" ["PROPERTY_VALUE_ID"]=> string(5) "19161" ["VALUE"]=> string(4) "1442" ["DESCRIPTION"]=> string(0) "" ["VALUE_ENUM"]=> NULL ["VALUE_XML_ID"]=> NULL ["VALUE_SORT"]=> NULL ["~VALUE"]=> string(4) "1442" ["~DESCRIPTION"]=> string(0) "" ["~NAME"]=> string(14) "Контакт" ["~DEFAULT_VALUE"]=> string(0) "" ["DISPLAY_VALUE"]=> string(58) "Bertalan Mesko" ["LINK_ELEMENT_VALUE"]=> bool(false) } } } }11/01/2011

Afanasyev B. V. (St. Petersburg, Russia)
Wagemaker G. (Rotterdam, Netherlands)
Zander A. R. (Hamburg, Germany)
Chukhlovin A. B. (St. Petersburg, Russia)
Fehse B. (Hamburg, Germany)
Novik A. А. (Moscow, Russia)
Claudia Koltzenburg (Hamburg, Germany)
Aleynikova O. (Minsk, Belarus)
Alyansky A. (St. Petersburg, Russia)
Anagnostou A. (Boston, USA)
Andreeff M. (Houston, USA)
Bacher U. (Hamburg, Germany)
Baуkov V. (St. Petersburg, Russia)
Baranov V. S. (St. Petersburg, Russia)
Barkhatov I. (St. Petersburg, Russia)
Baum C. (Hannover, Germany)
Bilko N. (Kiev, Ukraine)
Borset M. (Trondheim, Norway)
Buechner Th. (Muenster, Germany)
Bykov V. (St. Petersburg, Russia)
Dini G. (Genoa, Italy)
Drize N. (Moscow, Russia)
Egeland T. (Oslo, Norway)
Elstner E. (Berlin, Germany)
Emanuel V. (St. Petersburg, Russia)
Everaus H. (Tartu, Estonia)
Ferrara J. (Ann Arbor, USA)
Fibbe W. (Leiden, Netherlands)
Galibin O. (St. Petersburg, Russia)
Ganser A. (Hannover, Germany)
Granov D. (St. Petersburg, Russia)
Ivanov R. (Moscow, Russia)
Klimko N. (St. Petersburg, Russia)
Kolb H.-J. (Muenchen, Germany)
Konopleva M. (Houston, USA)
Koza V. (Pilsen, Czech Republic)
Kroeger N. (Hamburg, Germany)
Malikov A. (St. Petersburg, Russia)
Mikhailova N. (St. Petersburg, Russia)
Mentkevich G. (Moscow, Russia)
Nagler A. (Tel Hashomer, Israel)
Nemkov A. (St. Petersburg, Russia)
Neth R. (Hamburg, Germany)
Nevorotin A.J. (St. Petersburg, Russia)
Ostertag W. (Hamburg, Germany)
Palutke M. (Detroit, USA)
Roumiantsev A. G. (Moscow, Russia)
Savchenko V. G. (Moscow, Russia)
Smirnov A. V. (St. Petersburg, Russia)
Stamm C. (Berlin, Germany)
Tetz V. (St. Petersburg, Russia)
To B. (Adelaide, Australia)
Totolian A. A. (St. Petersburg, Russia)
Uss A.L. (Minsk, Belarus)
Vilesov A. (St. Petersburg, Russia)
Westenfelder Ch. (Salt Lake City, USA)
Wisloff F. (Oslo, Norway)
Zubarovskaya L. (St. Petersburg, Russia)
Zvartau E. (St. Petersburg, Russia)
Milestone article
Eliane Gluckman1, Hal E. Broxmeyer2, Arleen D. Auerbach3, Henry S. Friedman4, Gordon W. Douglas5, Agnes Devergie1, Helene Esperou1, Dominique Thierry6, Gerard Socie1, Pierre Lehn1, Scott Cooper2, Denis English2, Joanne Kurtzberg4, Judith Bard7, and Edward A. Boyse7
Reviews
Surapol Issaragrisil
Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)
Jakub Tolar, M.D., Ph.D.1, K. Scott Baker, M.D.2, Paul J. Orchard, M.D.1
Lauri Burroughs (MD), Ann Woolfrey (MD)
Richard A. Nash, MD
Hans-Jochem Kolb
Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)
Forum
Alexey Bersenev, MD, PhD
Milestone article
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 18890
[1] => 18891
[2] => 18892
[3] => 18893
[4] => 18894
[5] => 18895
[6] => 18896
[7] => 18897
[8] => 18898
[9] => 18899
[10] => 18900
[11] => 18901
[12] => 18902
[13] => 18903
[14] => 18904
)
[VALUE] => Array
(
[0] => 1407
[1] => 1408
[2] => 1409
[3] => 1410
[4] => 1411
[5] => 1412
[6] => 1413
[7] => 1414
[8] => 1415
[9] => 1416
[10] => 1417
[11] => 1418
[12] => 1419
[13] => 1420
[14] => 1421
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
[7] =>
[8] =>
[9] =>
[10] =>
[11] =>
[12] =>
[13] =>
[14] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1407
[1] => 1408
[2] => 1409
[3] => 1410
[4] => 1411
[5] => 1412
[6] => 1413
[7] => 1414
[8] => 1415
[9] => 1416
[10] => 1417
[11] => 1418
[12] => 1419
[13] => 1420
[14] => 1421
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
[3] =>
[4] =>
[5] =>
[6] =>
[7] =>
[8] =>
[9] =>
[10] =>
[11] =>
[12] =>
[13] =>
[14] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18837
[VALUE] => Array
(
[TEXT] => <p>Элиана Глюкман, Хэл Е. Броксмайер, Арлин Д. Ауэрбах, Генри С. Фридман, Гордон У. Дуглас, Агнес Девержи, Элен Эсперо, Доминик Тьерри, Жерар Соси, Пьер Лен, Скотт Купер, Денис Инглиш, Джоан Кюртцберг, Юдифь Бард, Эдвард А. Бойз</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Элиана Глюкман, Хэл Е. Броксмайер, Арлин Д. Ауэрбах, Генри С. Фридман, Гордон У. Дуглас, Агнес Девержи, Элен Эсперо, Доминик Тьерри, Жерар Соси, Пьер Лен, Скотт Купер, Денис Инглиш, Джоан Кюртцберг, Юдифь Бард, Эдвард А. Бойз
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18838
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Клинические проявления анемии Фанкони, аутосомной рецессивной болезни, включают прогрессирующую панцитопению, предрасположенность к злокачественным опухолям и развитию аномалий, не связанных с гемопоэзом. Гиперчувствительность к кластогенным эффектам – разрывам хромосом под действием препаратов, способствующих сшивке цепей ДНК, таких как диэпоксибутан, используется как диагностический признак генотипа анемии Фанкони, как пре- так и постнатально. Пренатальное <br>HLA-типирование даёт возможность установить, является ли плод HLA-идентичным больному сиблингу. <br /><br />Мы описываем здесь восстановление гемопоэза у мальчика с тяжёлой формой анемии Фанкони, которому была введена криоконсервированная пуповинная кровь сестры, не поражённой, по данным пренатального тестирования, данным заболеванием, имевшей нормальный кариотип и HLA-идентичный фенотип. <br /><br />Мы использовали претрансплантационный режим кондиционирования, разработанный специально для таких больных; метод основан на гиперчувствительности аномальных клеток к алкилирующим агентам, вызывающих сшивки цепей ДНК, и воздействию радиации. Метод позволяет использовать пуповинную кровь и избежать забора клеток костного мозга у новорожденного сиблинга. Такое применение пуповинной крови вытекало из предположения одного из нас о том, что кровь, взятая из пуповинной вены при рождении и обычно не используемая, может восстанавливать гемопоэз – предположении, основанном на наших предварительных исследованиях, согласующихся с сообщениями о наличии гемопоэтических стволовых и мультипотентных (CFU-GEMM), эритроидных (BFU-E) и гранулоцитарно-макрофагальных (CFU-GM) клеток-предшественников в пуповинной крови человека (см. ссылки в работе Broxmeyer et al.).<br /><br />
<h3>Ключевые слова</h3>
<p> анемия, апластическая терапия, консервация крови, анемия Фанкони, женская особь, плодная кровь, HLA антигены, трансплантация гемопоэтических стволовых клеток, тестирование гистосовместимости, человек, мужская особь, беременность, пренатальный диагноз, дети дошкольного возраста
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Клинические проявления анемии Фанкони, аутосомной рецессивной болезни, включают прогрессирующую панцитопению, предрасположенность к злокачественным опухолям и развитию аномалий, не связанных с гемопоэзом. Гиперчувствительность к кластогенным эффектам – разрывам хромосом под действием препаратов, способствующих сшивке цепей ДНК, таких как диэпоксибутан, используется как диагностический признак генотипа анемии Фанкони, как пре- так и постнатально. Пренатальное
HLA-типирование даёт возможность установить, является ли плод HLA-идентичным больному сиблингу.
Мы описываем здесь восстановление гемопоэза у мальчика с тяжёлой формой анемии Фанкони, которому была введена криоконсервированная пуповинная кровь сестры, не поражённой, по данным пренатального тестирования, данным заболеванием, имевшей нормальный кариотип и HLA-идентичный фенотип.
Мы использовали претрансплантационный режим кондиционирования, разработанный специально для таких больных; метод основан на гиперчувствительности аномальных клеток к алкилирующим агентам, вызывающих сшивки цепей ДНК, и воздействию радиации. Метод позволяет использовать пуповинную кровь и избежать забора клеток костного мозга у новорожденного сиблинга. Такое применение пуповинной крови вытекало из предположения одного из нас о том, что кровь, взятая из пуповинной вены при рождении и обычно не используемая, может восстанавливать гемопоэз – предположении, основанном на наших предварительных исследованиях, согласующихся с сообщениями о наличии гемопоэтических стволовых и мультипотентных (CFU-GEMM), эритроидных (BFU-E) и гранулоцитарно-макрофагальных (CFU-GM) клеток-предшественников в пуповинной крови человека (см. ссылки в работе Broxmeyer et al.).
Ключевые слова
анемия, апластическая терапия, консервация крови, анемия Фанкони, женская особь, плодная кровь, HLA антигены, трансплантация гемопоэтических стволовых клеток, тестирование гистосовместимости, человек, мужская особь, беременность, пренатальный диагноз, дети дошкольного возраста
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18839
[VALUE] => 10.3205/ctt-2010-en-000079.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000079.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18871
[VALUE] => Array
(
[TEXT] => <p><strong>Eliane Gluckman</strong><sup>1</sup><strong>, Hal E. Broxmeyer</strong><sup>2</sup><strong>, Arleen D. Auerbach</strong><sup>3</sup><strong>, Henry S. Friedman</strong><sup>4</sup><strong>, Gordon W. Douglas</strong><sup>5</sup><strong>, Agnes Devergie</strong><sup>1</sup><strong>, Helene Esperou</strong><sup>1</sup><strong>, Dominique Thierry</strong><sup>6</sup><strong>, Gerard Socie<sup>1</sup>, Pierre Lehn</strong><sup>1</sup><strong>, Scott Cooper</strong><sup>2</sup><strong>, Denis English</strong><sup>2</sup><strong>, Joanne Kurtzberg</strong><sup>4</sup><strong>, Judith Bard</strong><sup>7</sup><strong>, and Edward A. Boyse</strong><sup>7</sup></p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Eliane Gluckman1, Hal E. Broxmeyer2, Arleen D. Auerbach3, Henry S. Friedman4, Gordon W. Douglas5, Agnes Devergie1, Helene Esperou1, Dominique Thierry6, Gerard Socie1, Pierre Lehn1, Scott Cooper2, Denis English2, Joanne Kurtzberg4, Judith Bard7, and Edward A. Boyse7
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18872
[VALUE] => Array
(
[TEXT] => <p class="bodytext"><sup>1</sup>Bone Marrow Transplant Unit, Hôpital Saint-Louis, Paris, France; <sup>2</sup>Departments of Medicine (Hematology/Oncology), Microbiology and Immunology, Pathology, and the Walther Oncology Center, Indiana University School of Medicine, Indianapolis, USA; <sup>3</sup>Laboratory for Investigative Dermatology, Rockefeller University, New York, USA; <sup>4</sup>Department of Pediatrics (Hematology/Oncology), Duke University Medical Center, Durham, N.C., USA; <sup>5</sup>Department of Obstetrics and Gynecology, New York University Medical Center, New York, USA; <sup>6</sup>Central Nuclear Agency, Paris, France; <sup>7</sup>Memorial Sloan-Kettering Cancer Center, New York, USA.
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 1Bone Marrow Transplant Unit, Hôpital Saint-Louis, Paris, France; 2Departments of Medicine (Hematology/Oncology), Microbiology and Immunology, Pathology, and the Walther Oncology Center, Indiana University School of Medicine, Indianapolis, USA; 3Laboratory for Investigative Dermatology, Rockefeller University, New York, USA; 4Department of Pediatrics (Hematology/Oncology), Duke University Medical Center, Durham, N.C., USA; 5Department of Obstetrics and Gynecology, New York University Medical Center, New York, USA; 6Central Nuclear Agency, Paris, France; 7Memorial Sloan-Kettering Cancer Center, New York, USA.
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18873
[VALUE] => Array
(
[TEXT] => <p class="bodytext">The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].<br />We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.<br />This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).<br /><br />
<h3>Keywords </h3>
<p>anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child
</p>
<p class="bodytext">© 1989 Massachusetts Medical Society. All rights reserved.<br />Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].
We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.
This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).
Keywords
anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child
© 1989 Massachusetts Medical Society. All rights reserved.
Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18840
[VALUE] => Hematopoietic reconstitution in a patient with Fanconi's anemia by means of umbilical-cord blood from an HLA-identical sibling (1989)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Hematopoietic reconstitution in a patient with Fanconi's anemia by means of umbilical-cord blood from an HLA-identical sibling (1989)
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18874
[VALUE] => 908
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 908
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Eliane Gluckman1, Hal E. Broxmeyer2, Arleen D. Auerbach3, Henry S. Friedman4, Gordon W. Douglas5, Agnes Devergie1, Helene Esperou1, Dominique Thierry6, Gerard Socie1, Pierre Lehn1, Scott Cooper2, Denis English2, Joanne Kurtzberg4, Judith Bard7, and Edward A. Boyse7
1Bone Marrow Transplant Unit, Hôpital Saint-Louis, Paris, France; 2Departments of Medicine (Hematology/Oncology), Microbiology and Immunology, Pathology, and the Walther Oncology Center, Indiana University School of Medicine, Indianapolis, USA; 3Laboratory for Investigative Dermatology, Rockefeller University, New York, USA; 4Department of Pediatrics (Hematology/Oncology), Duke University Medical Center, Durham, N.C., USA; 5Department of Obstetrics and Gynecology, New York University Medical Center, New York, USA; 6Central Nuclear Agency, Paris, France; 7Memorial Sloan-Kettering Cancer Center, New York, USA.
The clinical manifestations of Fanconi's anemia, an autosomal recessive disorder, include progressive pancytopenia, a predisposition to neoplasia, and nonhematopoietic developmental anomalies [1-3]. Hypersensitivity to the clastogenic effect of DNA-cross-linking agents such as diepoxybutane acts as a diagnostic indicator of the genotype of Fanconi's anemia, both prenatally and postnatally [3-6]. Prenatal HLA typing has made it possible to ascertain whether a fetus is HLA-identical to an affected sibling [7].
We report here on hematopoietic reconstitution in a boy with severe Fanconi's anemia who received cryo-preserved umbilical-cord blood from a sister shown by prenatal testing to be unaffected by the disorder, to have a normal karyotype, and to be HLA-identical to the patient. We used a pretransplantation conditioning procedure developed specifically for the treatment of such patients [8]; this technique makes use of the hypersensitivity of the abnormal cells to alkylating agents that cross-link DNA [9, 10] and to irradiation [11] In this case, the availability of cord blood obviated the need for obtaining bone marrow from the infant sibling.
This use of cord blood followed the suggestion of one of us that blood retrieved from umbilical cord at delivery, usually discarded, might restore hematopoiesis – a proposal supported by preparatory studies by some of us [12] and consistent with reports on the presence of hematopoietic stem and multipotential (CFU-GEMM), erythroid (BFU-E), and granulocyte-macrophage (CFU-GM) progenitor cells in human umbilical-cord blood (see the references cited by Broxmeyer et al. [12]).
Keywords
anemia, aplastic therapy, blood preservation, Fanconi anemia, female, fetal blood, HLA antigens, hematopoietic stem cell transplantation, histocompatibility testing, humans, male, pregnancy, prenatal diagnosis, preschool child
© 1989 Massachusetts Medical Society. All rights reserved.
Originally published: N Engl J Med. 1989 Oct 26;321(17):1174-8. pmid: 2571931
Reviews
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19023
[VALUE] => 01/04/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/04/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19024
[VALUE] => 01/15/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/15/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19025
[VALUE] => 11/17/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 11/17/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19026
[VALUE] => 1432
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1432
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 19040
)
[VALUE] => Array
(
[0] => 1432
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1432
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19028
[VALUE] => Array
(
[TEXT] => <p>Сурапол Иссарагризил</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Сурапол Иссарагризил
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19039
[VALUE] => Array
(
[TEXT] => <p class="bodytext">
Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов. <br>
<br>
Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов.
</p>
<h3>Ключевые слова</h3>
<p> талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] =>
Трансплантация гемопоэтических стволовых клеток является единственной возможностью потенциального излечения при тяжелой талассемии, в том числе при гомозиготной β-талассемии и тяжелой талассемии с гемоглобином E/β. При заболевании 1-го или 2-го классов риска всем детям должна проводиться трансплантация, если они имеют HLA-идентичных братьев или сестер, и такую трансплантацию следует осуществлять как можно раньше. Пересадка клеток пуповинной крови от братьев или сестер рекомендуется детям с заболеванием 1-го или 2-го классов риска, если имеются в наличии адекватные количества клеток пуповинной крови от младших сиблингов.
Трансплантация костного мозга детям 3-го класса риска и взрослым больным с применением соответствующих режимов кондиционирования дает лучшие результаты по сравнению с теми, которые получаются при использовании пуповинной крови. Мы рекомендуем, однако, чтобы больные и их семьи могли обсудить в подробностях возможные факторы риска и преимущества лечения, и трансплантация должна проводиться только мотивированным пациентам, которые имеют четкое понятие обо всем процессе. Новые надежды связаны с возможным успехом гаплоидентичной трансплантации, но требуются дальнейшие исследования для подтверждения предыдущих результатов.
Ключевые слова
талассемия, клинические факторы риска, трансплантация гемопоэтических стволовых клеток, показания, преимущества
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19030
[VALUE] => 10.3205/ctt-2010-en-000070.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000070.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19034
[VALUE] => Array
(
[TEXT] => <p>Surapol Issaragrisil</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Surapol Issaragrisil
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19035
[VALUE] => Array
(
[TEXT] => <p>Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19036
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.<br /><br />Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.</p><h3>Keywords</h3>
<p> thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.
Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.
Keywords
thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19031
[VALUE] => Hematopoietic stem cell transplantation for thalassemia
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Hematopoietic stem cell transplantation for thalassemia
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19032
[VALUE] => 918
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 918
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19037
[VALUE] => 919
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 919
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Surapol Issaragrisil
Bone Marrow Transplant Center, Division of Hematology, Department of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand
Hematopoietic stem cell transplantation is the only modality that offers the potential of cure for severe thalassemia, including homozygous β-thalassemia and severe Hb E/β-thalassemia. All children with class 1 or 2 disease should be transplanted if they have HLA-identical siblings, and transplantation should be performed as early as possible. Sibling cord blood transplantation is recommended in children with class 1 or 2 of the disease if adequate numbers of cord blood cells from younger siblings are available.
Bone marrow transplantation in class 3 children and adult patients with appropriate conditioning regimen gives results that are superior to those obtained with cord blood. However, we recommend that patients and their families should discuss in detail the risks and benefits, and transplantation should be performed in only motivated patients who have a clear understanding of the entire process. There is new hope that haploidentical transplantation will be successful, but further studies are required to confirm early results.
Keywords
thalassemia, clinical risk factors, hematopoietic stem cell transplantation, indications, benefits
Reviews
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18953
[VALUE] => 12/08/2009 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 12/08/2009 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18954
[VALUE] => 01/25/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/25/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18955
[VALUE] => 04/29/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 04/29/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18956
[VALUE] => 1426
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1426
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 18970
[1] => 18971
)
[VALUE] => Array
(
[0] => 1426
[1] => 1427
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1426
[1] => 1427
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18959
[VALUE] => Array
(
[TEXT] => <p>Аравинд Рамакришнан, Биверли Дж.Торок-Шторб</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Аравинд Рамакришнан, Биверли Дж.Торок-Шторб
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18960
[VALUE] => Array
(
[TEXT] => <p class="bodytext"><span lang="RU">Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.</p>
<h3>Ключевые слова</h3>
<p> гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Успешность трансплантации гемопоэтических стволовых клеток зависит от приживления плюрипотентных гемопоэтических стволовых клеток (ГСК) и регулируемой пролиферации и созревания коммитированных родоначальных клеток. В целом, существует согласие в том, что эти процессы не могут возникать без соответствующей среды, которую обеспечивает компетентное микроокружение костного мозга. Оно состоит как из негемопоэтических клеток, так и клеток гемопоэтического происхождения, и впоследствии, после аллогенной трансплантации ГСК, становится химерным, содержащим стромальные клетки реципиента и макрофаги донора.
Ключевые слова
гемопоэтическое микроокружение, стромальные клетки, трансплантация, ниша стволовых клеток, единицы микроокружения, моноцит/макрофаг
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18961
[VALUE] => 10.3205/ctt-2010-en-000072.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000072.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18965
[VALUE] => Array
(
[TEXT] => <p>Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18966
[VALUE] => Array
(
[TEXT] => <p>Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18967
[VALUE] => Array
(
[TEXT] => <p class="bodytext">The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages. </p>
<h3>Keywords</h3>
<p> hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages.
Keywords
hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18962
[VALUE] => The role of the marrow microenvironment in hematopoietic stem cell transplantation
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => The role of the marrow microenvironment in hematopoietic stem cell transplantation
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18968
[VALUE] => 914
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 914
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18969
[VALUE] => 915
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 915
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Aravind Ramakrishnan (MD), Beverly J. Torok-Storb (Ph.D.)
Fred Hutchinson Cancer Research Center and the University of Washington, Seattle, USA
The success of hematopoietic stem cell transplantation depends on the engraftment of pluripotent hematopoietic stem cells and the regulated proliferation and maturation of committed progenitor cells. It is generally agreed that these processes cannot occur without an appropriate milieu provided by a competent marrow microenvironment (ME). The ME is composed of both non-hematopoietic and hematopoietic stem cell derived cells and consequently is chimeric following allogeneic stem cell transplantation, containing recipient stromal cells and donor macrophages.
Keywords
hematopoietic microenvironment, stromal cell, transplantation, stem cell niche, ME units, monocyte/macrophage
Reviews
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18990
[VALUE] => 01/11/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/11/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18991
[VALUE] => 01/25/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/25/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18992
[VALUE] => 03/22/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 03/22/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18993
[VALUE] => 1429
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1429
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 19012
[1] => 19013
[2] => 19014
)
[VALUE] => Array
(
[0] => 1429
[1] => 1291
[2] => 1430
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1429
[1] => 1291
[2] => 1430
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
[2] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18997
[VALUE] => Array
(
[TEXT] => <p>Якуб Толар, К.Скотт Бэйкер, Пол Дж. Орчард</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Якуб Толар, К.Скотт Бэйкер, Пол Дж. Орчард
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18998
[VALUE] => Array
(
[TEXT] => <p class="bodytext">В данной обзорной статье представлены сведения о трансплантации гемопоэтических стволовых клеток (ТГСК) у детей с врожденными метаболическими болезнями накопления (ВМБН), и о нерешенных вопросах ТГСК при этих состояниях. Обсуждаются как миелоаблативные, так и менее интенсивные режимы кондиционирования. Показана выгода стандартизированного подхода к ТГСК при болезни Хурлера и ранней адренолейкодистрофии (АЛД) головного мозга. Режимы кондиционирования со сниженной интенсивностью могут оказаться более успешными в плане снижения смертности и развития осложнений, особенно у больных с развивающимся неврологическим дефектом. В ситуациях с ТГСК при наследственных заболеваниях можно ожидать, что потенциальные доноры-сибсы могут быть носителями мутации данного гена. Нерешенная проблема состоит в том, может ли альтернативный донор иметь преимущество в сравнении с сибсом, который может быть носителем заболевания. Обычно применяют стволовые неродственные донорские клетки из различных источников (костного мозга, периферических клеток, пуповинной крови) с хорошими результатами. Рассматривается эффективность энзим-заместительной терапии по сравнению с ТГСК в качестве подходящего лечения при менее тяжелых формах мукополисахаридозов (МПС), и ТГСК признано стандартом терапии для больных с тяжелыми клиническими формами МПС типа I. В противоположность синдрому Хурлера, ТГСК не выявила существенного влияния у больных с тяжелым МПС типа II (синдром Хантера), т.е. дети с тяжелой формой МПС типа II, по-видимому, не имеют преимуществ в нейрокогнитивном развитии при ТГСК. Что касается метахроматической или глобоидноклеточной лейкодистрофии, то данные об эффективности ТГСК здесь более скудные. Получение четких данных об исходах ТГСК у больных с ВМБН оказалось сложной задачей из-за редкости этих заболеваний, вариабельности их генотипов и фенотипов, различий в источниках стволовых клеток, кондиционирующих режимах и оценке «успешных» результатов. Дальнейшие исследования установят полезность комбинированной терапии с/без трансплантации, включая субстратное ингибирование, терапию шаперонами, энзимотерапию и т.д. Кроме того, интерес к неонатальному скринингу обеспечит раннее вмешательство в течение этих болезней, т.к. это очень важно для получения оптимальных результатов. Наконец, модификация процедуры ТГСК или применение селективно размножающихся клеточных популяций, или обработка цитокинами могут усилить приживление микроглии, что может существенно облегчить достаку энзимов в центральную нервную систему. В это отношении будут важны многоцентровые исследования с общим подходом и оценкой клинических исходов.
</p>
<h3>Ключевые слова</h3>
<p>наследственные болезни накопления, мукополисахаридозы, трансплантация гемопоэтических клеток, режимы кондиционирования, клинический эффект
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => В данной обзорной статье представлены сведения о трансплантации гемопоэтических стволовых клеток (ТГСК) у детей с врожденными метаболическими болезнями накопления (ВМБН), и о нерешенных вопросах ТГСК при этих состояниях. Обсуждаются как миелоаблативные, так и менее интенсивные режимы кондиционирования. Показана выгода стандартизированного подхода к ТГСК при болезни Хурлера и ранней адренолейкодистрофии (АЛД) головного мозга. Режимы кондиционирования со сниженной интенсивностью могут оказаться более успешными в плане снижения смертности и развития осложнений, особенно у больных с развивающимся неврологическим дефектом. В ситуациях с ТГСК при наследственных заболеваниях можно ожидать, что потенциальные доноры-сибсы могут быть носителями мутации данного гена. Нерешенная проблема состоит в том, может ли альтернативный донор иметь преимущество в сравнении с сибсом, который может быть носителем заболевания. Обычно применяют стволовые неродственные донорские клетки из различных источников (костного мозга, периферических клеток, пуповинной крови) с хорошими результатами. Рассматривается эффективность энзим-заместительной терапии по сравнению с ТГСК в качестве подходящего лечения при менее тяжелых формах мукополисахаридозов (МПС), и ТГСК признано стандартом терапии для больных с тяжелыми клиническими формами МПС типа I. В противоположность синдрому Хурлера, ТГСК не выявила существенного влияния у больных с тяжелым МПС типа II (синдром Хантера), т.е. дети с тяжелой формой МПС типа II, по-видимому, не имеют преимуществ в нейрокогнитивном развитии при ТГСК. Что касается метахроматической или глобоидноклеточной лейкодистрофии, то данные об эффективности ТГСК здесь более скудные. Получение четких данных об исходах ТГСК у больных с ВМБН оказалось сложной задачей из-за редкости этих заболеваний, вариабельности их генотипов и фенотипов, различий в источниках стволовых клеток, кондиционирующих режимах и оценке «успешных» результатов. Дальнейшие исследования установят полезность комбинированной терапии с/без трансплантации, включая субстратное ингибирование, терапию шаперонами, энзимотерапию и т.д. Кроме того, интерес к неонатальному скринингу обеспечит раннее вмешательство в течение этих болезней, т.к. это очень важно для получения оптимальных результатов. Наконец, модификация процедуры ТГСК или применение селективно размножающихся клеточных популяций, или обработка цитокинами могут усилить приживление микроглии, что может существенно облегчить достаку энзимов в центральную нервную систему. В это отношении будут важны многоцентровые исследования с общим подходом и оценкой клинических исходов.
Ключевые слова
наследственные болезни накопления, мукополисахаридозы, трансплантация гемопоэтических клеток, режимы кондиционирования, клинический эффект
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18999
[VALUE] => 10.3205/ctt-2010-en-000075.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000075.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19005
[VALUE] => Array
(
[TEXT] => <p>Jakub Tolar, M.D., Ph.D.<sup>1</sup>, K. Scott Baker, M.D.<sup>2</sup>, Paul J. Orchard, M.D.<sup>1</sup></p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Jakub Tolar, M.D., Ph.D.1, K. Scott Baker, M.D.2, Paul J. Orchard, M.D.1
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19006
[VALUE] => Array
(
[TEXT] => <p class="bodytext"><sup>1</sup>Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; <sup>2</sup>Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 1Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; 2Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19007
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.</p>
<h3>Keywords</h3>
<p> hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.
Keywords
hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19000
[VALUE] => Hematopoietic stem cell transplantation for metabolic storage diseases
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Hematopoietic stem cell transplantation for metabolic storage diseases
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19001
[VALUE] => 916
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 916
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19011
[VALUE] => 917
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 917
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Jakub Tolar, M.D., Ph.D.1, K. Scott Baker, M.D.2, Paul J. Orchard, M.D.1
1Division of Hematology/Oncology and Blood and Marrow Transplantation, Department of Pediatrics, University of Minnesota, Minneapolis, USA; 2Clinical Research Division, Fred Hutchinson Cancer Research Center, Seattle, WA, USA
Almost thirty years of hematopoietic cell transplantation for congenital enzymopathies have revealed that the transfer of relatively few hematopoietic stem cells is able to fully reconstitute the lymphohematopoietic system in conditioned recipients and to maintain long term complementation of the enzyme defect in the recipient. Despite decades of effort to illuminate the mechanisms whereby the cross correction occurs, it remains unclear why hematopoietic cell transplantation is adequate only in some enzyme deficiencies. Here we review both biochemical and clinical data on the metabolic storage diseases in which the natural history and quality of life have been changed after hematopoietic cell transplantation. The challenge ahead is to understand the pathophysiology of congenital enzymopathies resistant to correction with hematopoietic cell transplantation, and to test whether the advances in stem cell therapy and gene correction can be translated into less toxic and even more effective therapy of metabolic storage diseases for which hematopoietic cell transplantation is a standard of care today.
Keywords
hematopoietic cell transplantation, conditioning regimen for hematopoietic cell transplantation, mucopolysaccharidosis, Hurler syndrome, metachromatic leukodystrophy, globoid cell leukodystrophy, Krabbe disease, adrenoleukodystrophy, mannosidosis, late effects after hematopoietic cell transplantation
Reviews
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19084
[VALUE] => 02/04/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 02/04/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19085
[VALUE] => 05/02/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 05/02/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19086
[VALUE] => 08/31/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08/31/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19087
[VALUE] => 1437
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1437
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 19104
[1] => 19105
)
[VALUE] => Array
(
[0] => 1436
[1] => 1437
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1436
[1] => 1437
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19094
[VALUE] => Array
(
[TEXT] => <p>Л. Барроуз, Э. Вулфри</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Л. Барроуз, Э. Вулфри
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19095
[VALUE] => Array
(
[TEXT] => <p>Центр раковых исследований Фреда Хатчинсона и Университет Вашингтона, Сиэтл, США</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Центр раковых исследований Фреда Хатчинсона и Университет Вашингтона, Сиэтл, США
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19096
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима.
</p>
<p class="bodytext">ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов.
</p>
<p class="bodytext">Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК.
</p>
<p class="bodytext">Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте.
</p>
<p class="bodytext">Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК.
</p>
<p class="bodytext">ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций.
</p>
<h3>Ключевые слова</h3>
<p> первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы </p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Трансплантация гемопоэтических клеток (ТГСК) является средством лечения первичных синдромов иммунодефицита (ПСИД), представляющих собой группу заболеваний, первично нарушающих один из ростков, например, лимфоидный или миелоидный. В целом, применение различных кондиционирующих режимов ТГСК зависит от типа ПСИД. Некоторые синдромы, вызывающие глубокий иммунодефицит, могут и не требовать кондиционирования. Возможно, однако, что существует иммунный барьер даже в случаях тяжелого комбинированного иммунодефицита (ТКИД), особенно в ситуации с расхождением по HLA или при гаплоидентичной ТГСК. Например, донорский В-клеточный химеризм менее вероятен при дефиците γ-цепей (X-сцепленный ТКИД), поскольку клетки больного занимают нишу В-клеток, нежели при синдромах без В-клеток (например при дефиците аденозиндезаминазы. Иммунный дефект может быть исправлен путем частичного восстановления нормальных иммунных клеток, другими словами – может и не требоваться полный донорский химеризм поврежденной клеточной субпопуляции. Эта концепция может служить дальнейшим доводом в пользу ограничения интенсивности кондиционирующего режима.
ТКИД включает в себя широкий круг врожденных дефктов, которые в каждом случае приводят к глубокому иммунодефициту как Т-, так и В-клеточной функции. Индивидуальные генетические дефекты ведут к развитию разнообразных фенотипов, и, поскольку цель ТГСК состоит в восстановлении как Т-, так и В-клеточных функций, то фенотип ТКИД должен приниматься в расчет, наряду со степенью различий донора и реципиента. Другие биологические факторы, ассоциированные с фенотипом ТКИД могут влиять на барьер приживления, такие, как НК-клетки больного, которые могут выжмивать после интенсивных кондиционирующих режимов.
Одной из проблем в анализе исходов ТГСК у больных ТКИД является относительная редкость этого заболевания, что требует больших многоцентровых программ. Недавние исследования показали, что наиболее важным фактором лучшего приживления после HLA-идентичной пересадки от сибса является более юный возраст в момент ТГСК. Факторами, существенно связанными с лучшим выживанием, после гаплоидентичных трансплантаций были: B+ фенотип больных ТКИД, защищенная (асептическая) среда обитания, и отсутствие легочных инфекций до ТГСК.
Внедрение неонатального скрининга и диагностика in utero позволили рано выявлять ТКИД и, тем самым, способствуют лечению в раннем возрасте.
Синдромы с первичным Т-клеточным иммунодефицитомс (ПТКИД) могут быть дифференцированы от ТКИД по снижению, но не полному отсутствию Т-клеточной функции, или же по отсутствию Т-клеточной активности при наличии функций В-лимфоцитов или НК-клеток. Аллогенная пересадка костного мозга остается единственным исцеляющим методом лечения, доступным для таких заболеваний. Независимо от донорских факторов, у больных с ПТКИД наблюдаются худшие клинические исходы, по сравнению с другими типами ИДС. Хотя опасные для жизни инфекции могут быть в раннем возрасте менее частыми, у детей с ПТКИД часто развивается органная патология из-за хронических инфекций, в особенности болезни легких до проведения ТГСК.
ТГСК при синдроме Вискотт-Олдрича дает больным значительные шансы на выживание. Показано, что достижение полного донорского химеризма является здесь благоприятным фактором. В целом, однако, многочисленные исследования при ИДС показывают, что кондиционирование низкой интенсивности создает условия для приживления донорских клеток при меньшей заболеваемости по сравнению со стандартными режимами, что является важным фактором для больных, у которых может быть неприемлемо высоким риск от проведения обычных трансплантаций.
Ключевые слова
первичные иммунодефициты, тяжелый комбинированный иммунодефицит (ТКИД), первичные Т-клеточные дефициты, трансплантация гемопоэтических стволовых клеток (ТГСК), кондиционирующие режимы, клинические исходы
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19090
[VALUE] => 10.3205/ctt-2010-en-000077.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000077.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19100
[VALUE] => Array
(
[TEXT] => <p>Lauri Burroughs (MD), Ann Woolfrey (MD)</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Lauri Burroughs (MD), Ann Woolfrey (MD)
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19101
[VALUE] => Array
(
[TEXT] => <p>Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19102
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen.
</p>
<p class="bodytext">SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age.
</p>
<p class="bodytext">Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT.
</p>
<p class="bodytext">In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
</p>
<h3>Keywords</h3>
<p>Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen.
SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age.
Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT.
In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
Keywords
Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19091
[VALUE] => Hematopoietic cell transplantation for treatment of primary immune deficiencies
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Hematopoietic cell transplantation for treatment of primary immune deficiencies
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19097
[VALUE] => 927
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 927
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19103
[VALUE] => 930
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 930
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Lauri Burroughs (MD), Ann Woolfrey (MD)
Fred Hutchinson Cancer Research Center and University of Washington, Seattle, WA
Hematopoietic cell transplantation (HCT) has the potential to cure primary immune deficiency syndromes (PIDS) that are a group of disorders primarily affecting a single lineage, e.g., lymphoid or myeloid lineage. Generally, implementation of various conditioning regimens depends the type of IDS. Some syndromes that cause profound immune deficiency may not require a conditioning regimen. There appears to be a barrier even in cases of severe combined immune deficiency (SCID), particularly in the situation of HLA mismatched or haploidentical grafts. For example, donor B cell chimerism is less likely in γ-chain deficiency (X-SCID), as host cells persistently occupy the B lymphocyte niche, than in syndromes without B cells such as adenosine deaminase (ADA) deficiency. The immune defect may be corrected by partial reconstitution of normal immune cells, in other words full donor chimerism of the affected cell subset may not be required. This concept may add further rationale to limiting the intensity of the conditioning regimen.
SCID encompasses a broad range of inherited defects that individually cause a profound immune deficiency of both T and B cell function. The individual genetic defects give rise to various phenotypes, and, since the goal of HCT is to restore both T and B cell function, the SCID phenotype must be taken into consideration in addition to the degree of recipient-donor mismatch. Other biologic factors associated with the SCID phenotype may influence the barrier to engraftment, such as host NK cells, which may survive intensive conditioning regimens. One of the difficulties in analyzing outcome of HCT in SCID patients is the relative rarity of the condition, thus needing large multicentric studies. Recent studies show that the most important factor for improved survival after an HLA-identical sibling graft was younger age at time of HCT. Factors significantly associated with improved survival after haploidentical transplants were B+ SCID phenotype, protected environment, and lack of pulmonary infections before HCT. The advent of neonatal screening and in utero diagnosis has allowed early detection of SCID and therefore prompt intervention at an early age.
Primary T cell immunodeficiency (PTCD) syndromes may be differentiated from SCID by virtue of reduced but not completely absent T cell function, or absent T cell function with the presence of B lymphocyte or NK cell function. Allogeneic marrow transplantation remains the only curative therapy available for these disorders. Worse outcomes were seen in patients with PTCD compared to other types of immune deficiencies, regardless of donor. Although life-threatening infections may be less common early in life, children with PTCD often develop organ damage from chronic infections, particularly lung disease, prior to HCT.
In Wiskott-Aldrich syndrome, HCT offers significantly improved survival chances for patients. Achieving full donor chimerism was shown to be a favorable factor. In general, however, the studies suggest that low intensity regimens offer the potential for achieving donor cell engraftment with less morbidity than standard regimens, an important consideration for patients who currently may consider the risks of conventional transplants unacceptably high.
Keywords
Primary immune deficiencies, SCID, primary T cell deficiencies, hematopoietic stem cell transplantation, conditioning regimens, outcomes
Reviews
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19132
[VALUE] => 06/14/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 06/14/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19133
[VALUE] => 06/30/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 06/30/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19134
[VALUE] => 12/08/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 12/08/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19135
[VALUE] => 1440
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1440
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 19149
)
[VALUE] => Array
(
[0] => 1440
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1440
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19140
[VALUE] => Array
(
[TEXT] => <p>Ричард А. Нэш</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Ричард А. Нэш
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19141
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут.
</p>
<h3>Ключевые слова</h3> <p>аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Аутоиммунные болезни характеризуются наличием или отсутствием определённых антигенных мишеней и могут вовлекать один или несколько органов. Большинство аутоиммунных болезней можно успешно контролировать, хотя и не излечивать полностью, но некоторые из них могут быть рефрактерными к традиционной терапии, представлять угрозу для жизни, или приводить к нарушениям деятельности основных органов. В таких случаях следует думать о более агрессивных лечебных подходах с применением трансплантации аутологичных или аллогенных гемопоэтических клеток (ТГК). Клинические испытания ТГК при аутоиммунных болезнях были начаты более десяти лет назад и основывались на положительных результатах доклинических испытаний. Доклинические испытания аутологичных и аллогенных ТГК при аутоиммунных болезнях рассматривались в специальных работах и здесь обсуждаться не будут.
Ключевые слова
аутоиммунные болезни, системная склеродермия, рассеянный склероз, трансплантация гемопоэтических клеток
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19137
[VALUE] => 10.3205/ctt-2010-en-000082.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000082.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19144
[VALUE] => Array
(
[TEXT] => <p>Richard A. Nash, MD</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Richard A. Nash, MD
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19145
[VALUE] => Array
(
[TEXT] => <p>Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19146
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2].
</p>
<h3>Keywords </h3><p>autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2].
Keywords
autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19138
[VALUE] => Hematopoietic cell transplantation for autoimmune diseases
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Hematopoietic cell transplantation for autoimmune diseases
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19142
[VALUE] => 934
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 934
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19147
[VALUE] => 935
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 935
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Richard A. Nash, MD
Fred Hutchinson Cancer Research Center and the University of Washington School of Medicine, Seattle, WA, USA
Autoimmune diseases may or may not have defined antigenic targets and may involve single or multiple organs. Although most autoimmune diseases can be effectively managed even if not cured, some autoimmune diseases may be refractory to conventional treatments and become life-threatening or cause critical organs to fail. This then would be the candidate population for consideration of a more aggressive approach requiring autologous or allogeneic hematopoietic cell transplantation (HCT). The clinical trials of HCT for autoimmune disease were started more than a decade ago and were based on successful preclinical studies. Preclinical studies of autologous and allogeneic HCT for autoimmune diseases have been reviewed and will not be discussed further [1, 2].
Keywords
autoimmune diseases, systemic sclerosis, multiple sclerosis, hematopoietic cell transplantation
Reviews
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19106
[VALUE] => 11/10/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 11/10/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19107
[VALUE] => 11/10/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 11/10/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19108
[VALUE] => 05/15/2012 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 05/15/2012 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 19119
)
[VALUE] => Array
(
[0] => 1383
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1383
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19113
[VALUE] => Array
(
[TEXT] => <p>Хaнc-Иохем Кольб</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Хaнc-Иохем Кольб
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19114
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов. <br /><br />Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний. <br /><br />Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ.
</p>
<p class="bodytext">Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки. </p>
<h3>Ключевые слова</h3>
<p>болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Проблемы патофизиологии, профилактики и лечения острой РТПХ (оРТПХ), возникающей чаще всего после аллогенной трансплантации гемопоэтических стволовых клеток (алло-ТГСК), необходимо изучить, чтобы использовать ее потенциальную выгоду без увеличения рисков. Многие исследований показали, что первичными мишенями являются гемопоэтические клетки, а также кожа, кишечник и печень, содержащие клетки макрофагального происхождения. Последние продуцируют провоспалительные цитокины, которые стимулируют донорские Т-клетки и индуцируют HLA-антигены II класса в тканях реципиента. Дендритные клетки (ДК) стимулируют CD 8 лимфоциты к реакции на пептиды HLA класса I. Таким образом, РТПХ направлена против антигенов гистосовместимости реципиента, которые чужеродны по отношению к донору. Полиморфные белки (не-HLA) могут также вызвать тяжелые реакции РТПХ. Реакции против минорных антигенов гистосовместимости требуют более длительных сроков для активации, нежели реакции против MHC-антигенов.
Предпосылки к РТПХ возникают до трансплантации (так наз. «цитокиновая буря», которая вызывается интенсивной кондиционирующей терапией и возможными инфекциями). Однако, в клинике показано, что переливание донорских лимфоцитов может вызвать РТПХ и без кондиционирующего лечения. В целом, иммунная система реципиента постоянно подавляется трансплантатом: трансплантат при этом становится толерантным по отношению к реципиенту. Механизм этой толерантности связан с появлением неспецифических и специфических клеток-супрессоров и последующей клональной делецией, а также при посредстве мезенхимных стволовых клеток, NK-Т-клеток и регуляторных Т-клеток. Выбор HLA-идентичного донора является залогом успешной ТГСК (на практике требуется определить до 10 локусов HLA). Несколько аллелей генов TNF-a и его рецептора II ассоциированы с повышенным риском РТПХ. Описываются также хорошо известные клинические особенности оРТПХ, включая поражения кожи, печени и кишечника. Рассматриваются также вопросы диагностики хронической РТПХ. Ее клинические и гистологические признаки во многом напоминают симптоматику аутоиммунных заболеваний.
Профилактика РТПХ хорошо разработана и ее следует применять в любой клинической ситуации. Особое внимание уделяется удалению Т-клеток из трансплантата современным методам иммуносупрессии после трансплантации. Рассматриваются некоторые вопросы, касающиеся удаления Т-клеток при трансплантации периферических ТГСК. Обсуждаются текущие схемы лечения ОТПХ, в том числе ингибиторов кальцинейрина, ряда новых супрессивных препаратов. Роль различных режимов терапии рассматривается в аспекте развития популяции Т-регуляторных клеток, а также мезенхимальных клеток и УФА-облучения для контроля РТПХ.
Особое внимание уделено индукции толерантности к РТПХ у больных после ТГСК. В большинстве случаев преобладает периферическая (тимус-независимая) форма толерантности. Обсуждаются специфические селективные эффекты рапамицина на Т-клетки.
Ключевые слова
болезнь «трансплантат против хозяина», профилактика, лечение, кондиционирующая терапия, дендритные клетки, Т-лимфоциты, иммуносупрессия, иммунотерапия
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19110
[VALUE] => 10.3205/ctt-2012-en-000089.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2012-en-000089.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19116
[VALUE] => Array
(
[TEXT] => <p>Hans-Jochem Kolb</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Hans-Jochem Kolb
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19117
[VALUE] => Array
(
[TEXT] => <p>Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany</p>
<p class="bodytext"><b>Correspondence</b><br> Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
<br> E-mail: <a href="javascript:linkTo_UnCryptMailto('qempxs.l1n1ospfDaif2hi');">h-j-kolb@<span style="display:none;">spam is bad</span>web.de</a>
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
Correspondence
Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
E-mail: h-j-kolb@web.de
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19118
[VALUE] => Array
(
[TEXT] => <p class="bodytext">The pathophysiology, prevention, and treatment of acute graft-versus-host disease (GVHD) occurring, mainly, after allogeneic hematopoietic stem cell transplantation (allo-HSCT), should be understood, in order to exploit its potential benefits while avoiding certain clinical risks. Many studies have shown haematopoietic cells to be primary targets, as well as skin, gut, and liver containing macrophage-derived cells. The latters produce pro-inflammatory cytokines that stimulate donor T cells and induce HLA class II antigens in host tissue. Dendritic cells (DCs) boost CD 8 cells to react against HLA class I peptides. Hence, GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. Polymorphic non-HLA proteins may also cause severe GVH reactions. The reactions against minor histocompatibility antigens require a longer phase of activation than reactions against MHC antigens. <br /><br />The preconditions of acute GVHD (aGVHD) are given before transplantation (the s.c. “cytokine storm” liberated by intensive conditioning treatment and probable infections). However, in human patients, donor lymphocyte transfusion may produce GVHD without conditioning treatment. In general, the host’s immune system is continuously suppressed by the graft and; the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion, being also mediated by mesenchymal stromal cells, NK-T cells, and regulatory T cells. Selecting an HLA-identical sibling as donor was the major step towards successful HSCT (generally, definition of 10 HLA-loci is required to prevent severe GVHD). Several TNF-a and TNF-a receptor alleles are associated with an increased risk of GVHD. The well-known clinical features of aGVHD are also described, including skin, liver, and gut lesions. The issues of chronic GVHD are also described. Its clinical and pathological signs resemble autoimmune diseases in many aspects. <br /><br />GVHD prophylaxis is well established, and should be used in any clinical setting. Special attention is given to T cell depletion and modern immunosuppressive therapies post-transplant. Current schedules of GVHD treatment are described including calcineurin inhibitors, and some novel suppressive drugs. The role of various treatment regimens is considered in view of regulatory T cell (Treg), mesenchymal stem cells and UV-A irradiation as possible means of GVHD management. <br /><br />Special attention is drawn to induction of a graft-versus-host tolerance in clinical HSCT. In the majority of patients, the peripheral (thymus-independent) form of tolerance prevails. Specific selective effects of Rapamycin upon T cells are discussed.</p>
<h3>Keywords</h3>
<p>graft-versus-host disease, prophylaxis, treatment, conditioning therapy, dendritic cells, Т-lymphocytes, immune suppression, immune therapy
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => The pathophysiology, prevention, and treatment of acute graft-versus-host disease (GVHD) occurring, mainly, after allogeneic hematopoietic stem cell transplantation (allo-HSCT), should be understood, in order to exploit its potential benefits while avoiding certain clinical risks. Many studies have shown haematopoietic cells to be primary targets, as well as skin, gut, and liver containing macrophage-derived cells. The latters produce pro-inflammatory cytokines that stimulate donor T cells and induce HLA class II antigens in host tissue. Dendritic cells (DCs) boost CD 8 cells to react against HLA class I peptides. Hence, GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. Polymorphic non-HLA proteins may also cause severe GVH reactions. The reactions against minor histocompatibility antigens require a longer phase of activation than reactions against MHC antigens.
The preconditions of acute GVHD (aGVHD) are given before transplantation (the s.c. “cytokine storm” liberated by intensive conditioning treatment and probable infections). However, in human patients, donor lymphocyte transfusion may produce GVHD without conditioning treatment. In general, the host’s immune system is continuously suppressed by the graft and; the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion, being also mediated by mesenchymal stromal cells, NK-T cells, and regulatory T cells. Selecting an HLA-identical sibling as donor was the major step towards successful HSCT (generally, definition of 10 HLA-loci is required to prevent severe GVHD). Several TNF-a and TNF-a receptor alleles are associated with an increased risk of GVHD. The well-known clinical features of aGVHD are also described, including skin, liver, and gut lesions. The issues of chronic GVHD are also described. Its clinical and pathological signs resemble autoimmune diseases in many aspects.
GVHD prophylaxis is well established, and should be used in any clinical setting. Special attention is given to T cell depletion and modern immunosuppressive therapies post-transplant. Current schedules of GVHD treatment are described including calcineurin inhibitors, and some novel suppressive drugs. The role of various treatment regimens is considered in view of regulatory T cell (Treg), mesenchymal stem cells and UV-A irradiation as possible means of GVHD management.
Special attention is drawn to induction of a graft-versus-host tolerance in clinical HSCT. In the majority of patients, the peripheral (thymus-independent) form of tolerance prevails. Specific selective effects of Rapamycin upon T cells are discussed.
Keywords
graft-versus-host disease, prophylaxis, treatment, conditioning therapy, dendritic cells, Т-lymphocytes, immune suppression, immune therapy
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19111
[VALUE] => Graft-versus-host disease: from experiments to clinical insight
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Graft-versus-host disease: from experiments to clinical insight
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Hans-Jochem Kolb
Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
Correspondence
Kolb Consulting UG, Senior Consultant, 3. Medizinische Klinik, Klinikum rechts der Isar, Technische Universität München, Germany
E-mail: h-j-kolb@web.de
The pathophysiology, prevention, and treatment of acute graft-versus-host disease (GVHD) occurring, mainly, after allogeneic hematopoietic stem cell transplantation (allo-HSCT), should be understood, in order to exploit its potential benefits while avoiding certain clinical risks. Many studies have shown haematopoietic cells to be primary targets, as well as skin, gut, and liver containing macrophage-derived cells. The latters produce pro-inflammatory cytokines that stimulate donor T cells and induce HLA class II antigens in host tissue. Dendritic cells (DCs) boost CD 8 cells to react against HLA class I peptides. Hence, GVH reactions of the graft are directed against histocompatibility antigens of the recipient that are foreign to the donor. Polymorphic non-HLA proteins may also cause severe GVH reactions. The reactions against minor histocompatibility antigens require a longer phase of activation than reactions against MHC antigens.
The preconditions of acute GVHD (aGVHD) are given before transplantation (the s.c. “cytokine storm” liberated by intensive conditioning treatment and probable infections). However, in human patients, donor lymphocyte transfusion may produce GVHD without conditioning treatment. In general, the host’s immune system is continuously suppressed by the graft and; the graft becomes tolerant towards the host. The mechanism of tolerance has been related to the occurrence of non-specific and specific suppressor cells followed by clonal deletion, being also mediated by mesenchymal stromal cells, NK-T cells, and regulatory T cells. Selecting an HLA-identical sibling as donor was the major step towards successful HSCT (generally, definition of 10 HLA-loci is required to prevent severe GVHD). Several TNF-a and TNF-a receptor alleles are associated with an increased risk of GVHD. The well-known clinical features of aGVHD are also described, including skin, liver, and gut lesions. The issues of chronic GVHD are also described. Its clinical and pathological signs resemble autoimmune diseases in many aspects.
GVHD prophylaxis is well established, and should be used in any clinical setting. Special attention is given to T cell depletion and modern immunosuppressive therapies post-transplant. Current schedules of GVHD treatment are described including calcineurin inhibitors, and some novel suppressive drugs. The role of various treatment regimens is considered in view of regulatory T cell (Treg), mesenchymal stem cells and UV-A irradiation as possible means of GVHD management.
Special attention is drawn to induction of a graft-versus-host tolerance in clinical HSCT. In the majority of patients, the peripheral (thymus-independent) form of tolerance prevails. Specific selective effects of Rapamycin upon T cells are discussed.
Keywords
graft-versus-host disease, prophylaxis, treatment, conditioning therapy, dendritic cells, Т-lymphocytes, immune suppression, immune therapy
Reviews
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18921
[VALUE] => 01/15/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/15/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18922
[VALUE] => 01/25/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/25/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18923
[VALUE] => 06/09/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 06/09/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18924
[VALUE] => 1423
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1423
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 18935
[1] => 18936
)
[VALUE] => Array
(
[0] => 1423
[1] => 1424
)
[DESCRIPTION] => Array
(
[0] =>
[1] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1423
[1] => 1424
)
[~DESCRIPTION] => Array
(
[0] =>
[1] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18927
[VALUE] => Array
(
[TEXT] => <p>Митчелл Э. Хорвитц, Нельсон Чао</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Митчелл Э. Хорвитц, Нельсон Чао
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18928
[VALUE] => Array
(
[TEXT] => <p class="bodytext">По мере улучшения результатов трансплантации клеток пуповинной крови (ТКПК), подлежат пересмотру также и расчеты соотношений риска и выгоды при лечении неопухолевых заболеваний. Недавно полученные результаты дают основания считать, что исход ТКПК сравним с таковым при пересадке от совместимого неродственного донора. Следовательно, в отношении больных, не подлежащих такой потенциально излечивающей терапии из-за отсутствия подходящего совместимого донора, могут рассматриваться возможности совместимой или несовместимой трансплантации неродственных клеток пуповинной крови. В данном обзорe будут обсуждаться наиболее современные данные, касающиеся ТКПК в целях лечения врожденных иммунодефицитных заболеваний, врожденных болезней обмена веществ, синдромов дефицита функций костного мозга и гемоглобинопатий.
</p>
<h3>Ключевые слова</h3>
<p> трансплантация стволовых клеток, пуповинная кровь, исходы, клинические результаты, иммунодефицит, неопухолевые заболевания, дефицит функций костного мозга, обзор</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => По мере улучшения результатов трансплантации клеток пуповинной крови (ТКПК), подлежат пересмотру также и расчеты соотношений риска и выгоды при лечении неопухолевых заболеваний. Недавно полученные результаты дают основания считать, что исход ТКПК сравним с таковым при пересадке от совместимого неродственного донора. Следовательно, в отношении больных, не подлежащих такой потенциально излечивающей терапии из-за отсутствия подходящего совместимого донора, могут рассматриваться возможности совместимой или несовместимой трансплантации неродственных клеток пуповинной крови. В данном обзорe будут обсуждаться наиболее современные данные, касающиеся ТКПК в целях лечения врожденных иммунодефицитных заболеваний, врожденных болезней обмена веществ, синдромов дефицита функций костного мозга и гемоглобинопатий.
Ключевые слова
трансплантация стволовых клеток, пуповинная кровь, исходы, клинические результаты, иммунодефицит, неопухолевые заболевания, дефицит функций костного мозга, обзор
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18929
[VALUE] => 10.3205/ctt-2010-en-000069.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000069.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18930
[VALUE] => Array
(
[TEXT] => <p>Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18931
[VALUE] => Array
(
[TEXT] => <p>Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 18932
[VALUE] => Array
(
[TEXT] => <p class="bodytext">As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies.
</p>
<h3>Keywords</h3>
<p> stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review
</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies.
Keywords
stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18933
[VALUE] => Umbilical cord blood transplantation for treatment of non-malignant disorders
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Umbilical cord blood transplantation for treatment of non-malignant disorders
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 18934
[VALUE] => 910
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 910
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Mitchell E. Horwitz (MD), Nelson Chao (MD, MBA)
Division of Cellular Therapy, Duke University Medical Center, Durham, North Carolina, USA
As the outcomes of umbilical cord blood transplantation improve, the risk versus benefit considerations with respect to treatment of non-malignant disorders must be reassessed. Recent data would suggest that the outcome of umbilical cord blood transplantation is comparable to that of matched unrelated donor transplantation. Thus, patients felt not to be candidates for this potentially curative treatment modality due to lack of an available matched donor should be considered for matched or mismatched unrelated umbilical cord blood transplantation. This review will cover the most recent data pertaining to umbilical cord blood transplantation for the treatment of congenital immunodeficiency disorders, inborn errors of metabolism, bone marrow failure disorders, and hemoglobinopathies.
Keywords
stem cell transplantation, umbilical cord blood, outcomes, clinical results, immunodeficiency, non-malignant disorders, bone marrow failure, review
Forum
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19051
[VALUE] => 07/23/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 07/23/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19052
[VALUE] => 07/29/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 07/29/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19053
[VALUE] => 08/02/2010 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 08/02/2010 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19054
[VALUE] => 1434
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1434
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 19069
)
[VALUE] => Array
(
[0] => 1434
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1434
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19059
[VALUE] => Array
(
[TEXT] => <p>Алексей Берсенев</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Алексей Берсенев
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19060
[VALUE] => Array
(
[TEXT] => <p class="bodytext">Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.</p><h3>Ключевые слова</h3>
<p> наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Научное ведение блога - это относительно новый вид деятельности, который ученые и люди, связанные с наукой, практикуют онлайн. В этом эссе я делюсь своим опытом о том, как научное ведение блога может быть использовано для становления и продвижения Вашей профессиональной работы с помощью сетей онлайн. Используемая мною модель сочетает ведение блога аналитического характера из определённой научной сферы и участие в обсуждениях и обменах мнениями среди экспертов с помощью веб-инструментов. Я использую блог в качетсве центрального узла для анализа информации, поступающей из моих личных фильтров, и для настройки совместных фильтров онлайн, основанных на профессиональном надёжном содержании. В целом, я думаю, что блог может быть одним из лучших веб-инструментов для ученых для создания профессиональной сети онлайн.
Ключевые слова
наука онлайн, Веб 2.0, блог, научное ведение блога, работа с помощью сетей онлайн
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19056
[VALUE] => 10.3205/ctt-2010-en-000084.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2010-en-000084.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19062
[VALUE] => Array
(
[TEXT] => <p>Alexey Bersenev, MD, PhD</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Alexey Bersenev, MD, PhD
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19063
[VALUE] => Array
(
[TEXT] => <p>314G Abramson Research Center, Children’s Hospital of Philadelphia, Philadelphia, PA, USA</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => 314G Abramson Research Center, Children’s Hospital of Philadelphia, Philadelphia, PA, USA
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19064
[VALUE] => Array
(
[TEXT] => <p>
Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online.
</p>
<h3>Keywords</h3>
<img width="160" alt="RTEmagicC_Bersenev_Keywords_01.gif" src="/upload/medialibrary/a6f/rtemagicc_bersenev_keywords_01.gif" height="160" title="RTEmagicC_Bersenev_Keywords_01.gif" align="left">
<div style="margin-left:190px;">
<p>
science online, Web 2.0, blog, scientific blogging, networking
</p>
</div>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] =>
Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online.
Keywords

science online, Web 2.0, blog, scientific blogging, networking
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19057
[VALUE] => Scientific blogging as a model for professional networking online
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Scientific blogging as a model for professional networking online
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19065
[VALUE] => 921
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 921
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Alexey Bersenev, MD, PhD
314G Abramson Research Center, Children’s Hospital of Philadelphia, Philadelphia, PA, USA
Scientific blogging is a relatively new kind of activity that scientists and people related to science do online. In this essay I’m sharing my own experience about how scientific blogging could be used to establish and advance your professional networking online. The model I use proposes blogging analytical content in a precise scientific niche and sharing discussion and expert opinions through web tools. I use a blog as a central hub for analysis of information flowing from my personal filters and for setting up collaborative filters online, based on professional trusted content. Overall, I think a blog could be one of the best web tools for scientists to build a professional network online.
Keywords

science online, Web 2.0, blog, scientific blogging, networking
Forum
Array
(
[KEYWORDS] => Array
(
[ID] => 19
[TIMESTAMP_X] => 2015-09-03 10:46:01
[IBLOCK_ID] => 2
[NAME] => Ключевые слова
[ACTIVE] => Y
[SORT] => 500
[CODE] => KEYWORDS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 19
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 4
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => Y
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => Y
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Ключевые слова
[~DEFAULT_VALUE] =>
)
[SUBMITTED] => Array
(
[ID] => 20
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата подачи
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUBMITTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 20
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19158
[VALUE] => 01/02/2011 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 01/02/2011 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата подачи
[~DEFAULT_VALUE] =>
)
[ACCEPTED] => Array
(
[ID] => 21
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата принятия
[ACTIVE] => Y
[SORT] => 500
[CODE] => ACCEPTED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 21
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19159
[VALUE] => 09/09/2011 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 09/09/2011 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата принятия
[~DEFAULT_VALUE] =>
)
[PUBLISHED] => Array
(
[ID] => 22
[TIMESTAMP_X] => 2015-09-02 17:21:42
[IBLOCK_ID] => 2
[NAME] => Дата публикации
[ACTIVE] => Y
[SORT] => 500
[CODE] => PUBLISHED
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 22
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => DateTime
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19160
[VALUE] => 12/10/2011 12:00:00 am
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 12/10/2011 12:00:00 am
[~DESCRIPTION] =>
[~NAME] => Дата публикации
[~DEFAULT_VALUE] =>
)
[CONTACT] => Array
(
[ID] => 23
[TIMESTAMP_X] => 2015-09-03 14:43:05
[IBLOCK_ID] => 2
[NAME] => Контакт
[ACTIVE] => Y
[SORT] => 500
[CODE] => CONTACT
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 23
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19161
[VALUE] => 1442
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 1442
[~DESCRIPTION] =>
[~NAME] => Контакт
[~DEFAULT_VALUE] =>
)
[AUTHORS] => Array
(
[ID] => 24
[TIMESTAMP_X] => 2015-09-03 10:45:07
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHORS
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => E
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => Y
[XML_ID] => 24
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 3
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] => EAutocomplete
[USER_TYPE_SETTINGS] => Array
(
[VIEW] => E
[SHOW_ADD] => Y
[MAX_WIDTH] => 0
[MIN_HEIGHT] => 24
[MAX_HEIGHT] => 1000
[BAN_SYM] => ,;
[REP_SYM] =>
[OTHER_REP_SYM] =>
[IBLOCK_MESS] => N
)
[HINT] =>
[PROPERTY_VALUE_ID] => Array
(
[0] => 19172
)
[VALUE] => Array
(
[0] => 1442
)
[DESCRIPTION] => Array
(
[0] =>
)
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[0] => 1442
)
[~DESCRIPTION] => Array
(
[0] =>
)
[~NAME] => Авторы
[~DEFAULT_VALUE] =>
)
[AUTHOR_RU] => Array
(
[ID] => 25
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Авторы
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 25
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Авторы
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_RU] => Array
(
[ID] => 26
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Организации
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 26
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Организации
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_RU] => Array
(
[ID] => 27
[TIMESTAMP_X] => 2015-09-02 18:01:20
[IBLOCK_ID] => 2
[NAME] => Описание/Резюме
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 27
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Описание/Резюме
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[DOI] => Array
(
[ID] => 28
[TIMESTAMP_X] => 2016-04-06 14:11:12
[IBLOCK_ID] => 2
[NAME] => DOI
[ACTIVE] => Y
[SORT] => 500
[CODE] => DOI
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 28
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19163
[VALUE] => 10.3205/ctt-2011-en-000093.01
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 10.3205/ctt-2011-en-000093.01
[~DESCRIPTION] =>
[~NAME] => DOI
[~DEFAULT_VALUE] =>
)
[AUTHOR_EN] => Array
(
[ID] => 37
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Author
[ACTIVE] => Y
[SORT] => 500
[CODE] => AUTHOR_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 37
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19166
[VALUE] => Array
(
[TEXT] => <p>Bertalan Mesko, MD</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Bertalan Mesko, MD
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Author
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[ORGANIZATION_EN] => Array
(
[ID] => 38
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Organization
[ACTIVE] => Y
[SORT] => 500
[CODE] => ORGANIZATION_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 38
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19167
[VALUE] => Array
(
[TEXT] => <p>Managing director of Webicina.com</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => Managing director of Webicina.com
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Organization
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[SUMMARY_EN] => Array
(
[ID] => 39
[TIMESTAMP_X] => 2015-09-02 18:02:59
[IBLOCK_ID] => 2
[NAME] => Description / Summary
[ACTIVE] => Y
[SORT] => 500
[CODE] => SUMMARY_EN
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 39
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] => 19168
[VALUE] => Array
(
[TEXT] => <p>The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.</p>
<h3>Keywords</h3>
<p>Internet, content curation, time management, Web 2.0</p>
[TYPE] => HTML
)
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Array
(
[TEXT] => The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.
Keywords
Internet, content curation, time management, Web 2.0
[TYPE] => HTML
)
[~DESCRIPTION] =>
[~NAME] => Description / Summary
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[NAME_EN] => Array
(
[ID] => 40
[TIMESTAMP_X] => 2015-09-03 10:49:47
[IBLOCK_ID] => 2
[NAME] => Name
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 80
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 40
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => Y
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19164
[VALUE] => Online medical content curation and personal time management with Web 2.0: an exciting era
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => Online medical content curation and personal time management with Web 2.0: an exciting era
[~DESCRIPTION] =>
[~NAME] => Name
[~DEFAULT_VALUE] =>
)
[FULL_TEXT_RU] => Array
(
[ID] => 42
[TIMESTAMP_X] => 2015-09-07 20:29:18
[IBLOCK_ID] => 2
[NAME] => Полный текст
[ACTIVE] => Y
[SORT] => 500
[CODE] => FULL_TEXT_RU
[DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 42
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 200
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Полный текст
[~DEFAULT_VALUE] => Array
(
[TEXT] =>
[TYPE] => HTML
)
)
[PDF_RU] => Array
(
[ID] => 43
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF RUS
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_RU
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 43
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => PDF RUS
[~DEFAULT_VALUE] =>
)
[PDF_EN] => Array
(
[ID] => 44
[TIMESTAMP_X] => 2015-09-09 16:05:20
[IBLOCK_ID] => 2
[NAME] => PDF ENG
[ACTIVE] => Y
[SORT] => 500
[CODE] => PDF_EN
[DEFAULT_VALUE] =>
[PROPERTY_TYPE] => F
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 44
[FILE_TYPE] => doc, txt, rtf, pdf
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] =>
[USER_TYPE_SETTINGS] =>
[HINT] =>
[PROPERTY_VALUE_ID] => 19169
[VALUE] => 939
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] => 939
[~DESCRIPTION] =>
[~NAME] => PDF ENG
[~DEFAULT_VALUE] =>
)
[NAME_LONG] => Array
(
[ID] => 45
[TIMESTAMP_X] => 2023-04-13 00:55:00
[IBLOCK_ID] => 2
[NAME] => Название (для очень длинных заголовков)
[ACTIVE] => Y
[SORT] => 500
[CODE] => NAME_LONG
[DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
[PROPERTY_TYPE] => S
[ROW_COUNT] => 1
[COL_COUNT] => 30
[LIST_TYPE] => L
[MULTIPLE] => N
[XML_ID] => 45
[FILE_TYPE] =>
[MULTIPLE_CNT] => 5
[TMP_ID] =>
[LINK_IBLOCK_ID] => 0
[WITH_DESCRIPTION] => N
[SEARCHABLE] => N
[FILTRABLE] => N
[IS_REQUIRED] => N
[VERSION] => 1
[USER_TYPE] => HTML
[USER_TYPE_SETTINGS] => Array
(
[height] => 80
)
[HINT] =>
[PROPERTY_VALUE_ID] =>
[VALUE] =>
[DESCRIPTION] =>
[VALUE_ENUM] =>
[VALUE_XML_ID] =>
[VALUE_SORT] =>
[~VALUE] =>
[~DESCRIPTION] =>
[~NAME] => Название (для очень длинных заголовков)
[~DEFAULT_VALUE] => Array
(
[TYPE] => HTML
[TEXT] =>
)
)
)
Bertalan Mesko, MD
Managing director of Webicina.com
The recent increase in the number of online medical resources has raised important questions about content curation on the World Wide Web and the importance of time management tools and applications used in medicine and healthcare. Content curation is crucial at a time when patients and their doctors are searching more online but the majority of health resources are considered medically unreliable. The value of crowdsourcing and time management tools that can save time and effort for professionals is demonstrated.
Keywords
Internet, content curation, time management, Web 2.0

