Impact of leucocytes recovery on longterm outcomes after allo-HSCT in acute leukemia patients in complete remission
Ekaterina D. Mikhaltsova, Mikhail Y. Drokov, Julia O. Davydova, Larisa A. Kuzmina, Vera A. Vasilyeva, Natalia N. Popova, Darya S. Dubnyak, Olga M. Koroleva, Nikolay M. Kapranov, Zoya V. Konova, Irina V. Galtseva, Elena N. Parovichnikova, Valery G. Savchenko
National Research Center for Hematology, Moscow, Russian Federation
Summary
Introduction
Reconstitution of leucocyte subpopulations is an important factor that determines success of hematopoietic stem cell transplantation (HSCT). We hypothesized that the leucocyte recovery should be strongly associated with clinical outcomes. Our aim was to evaluate possible impact of leucocyte recovery upon long-term outcomes after allo-HSCT in acute leukemia patients transplanted in complete remission (CR).Patients and methods
This study included 28 patients (7 males and 21 females) with a median age of 36 years (range 21 to 61), who underwent allo-HSCT from 2015 to 2017 at the National Research Center for Hematology. All patients had an acute leukemia: 11, ALL and 17, AML; all of them were transplanted in complete remission (CR). 12 patients underwent myeloablative conditioning regimen and 16 patients, reduced-intensity treatment. 23 patients received bone marrow transplant as a stem cell source, and 5 patients received PBSC. Reconstitution of leucocyte subpopulations was tested by means of flow cytometric analysis of peripheral blood on days +14, +30, +60, and +90 after allo-HSCT. Anti-CD3 FITC, anti-CD16PE, anti-CD56 PE, anti-CD45 Per-CP-CYTM5.5, anti-CD4 PE-CyTM7, anti-CD19 APC, anti-CD8 APC-Cy7 (BD Biosciences, USA) as well as anti-CD14PE, anti-CD16PE, anti-HLA-DR APC (eBiosciences, USA) were used to identify the white blood cell subsets. Predictive significance of leucocyte reconstitution after allo-HSCT was evaluated by receiver-operating characteristic (ROC) curve analysis. Fisher’s exact test was used for 2×2 tables. Kaplan-Meier analysis with log-rank test was used for survival analysis and group comparison. A p value <0.05 was considered significant.Results
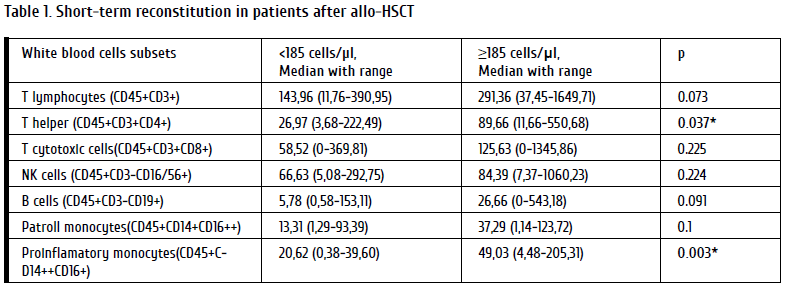
According to the data of ROC-curve analysis, classical monocytes proved to be of highest predictive significance for poor (lethal) outcome (AUC= 0.78; p=0.05) after allo-HSCT in acute leukemia patients transplanted in CR, with a cut-off level of 185 cells/μL. The two corresponding groups of HSCT patients (≥185 cells/μl, and <185 cells/μl) were matched by age (p=0.64), gender (p=0.38), diagnosis (p=0.7), conditioning regimens (p=0.7) and stem cell source (p=0.35). Their detailed cell characteristics are presented in Table 1. When analyzing survival rates, the absolute counts of classical monocytes <185 cells/μl by day 90 were associated with decreased overall survival (58.9%), compared to 93.7% survival at higher monocyte levels, thus showing significant difference (p=0,02) (Figure 1). The mortality analysis revealed that five patients have died in the “<185 cells/μl” group. Lethal outcome was due to the disease progression in 2 cases, and 3 patients died from infectious complications.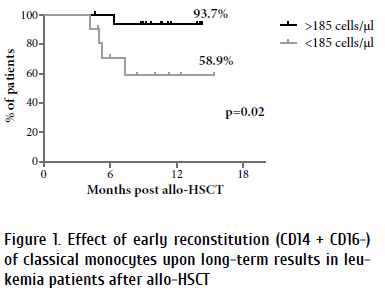
Conclusion
Poor recovery of classical monocytes is combined with low numbers of CD4+ cells (p=0.037), and pro-inflammatory monocytes (p=0.003). A significantly poor and slow reconstitution after allo-HSCT is strongly associated with poor outcomes due to infectious complications and relapses during first 12 months after allo-HSCT in patients with acute leukemia.Keywords
Leucocyte recovery, stem cell transplantation, clinical outcome after allo-HSCT, classical monocytes, CD4+ cells, proinlammatory monocytes.