First experience of high-dose chemotherapy with autologous hematopoietic stem cell transplantation in patients with lymphoma and HIV
Yulia A. Rogacheva, Marina O. Popova, Anastasia V. Nekrasova, Ivan V. Tsygankov, Kirill V. Lepik, Olga V. Pirogova, Elena I. Darskaya, Lilia V. Stelmah, Maria D. Vladovskaya, Ivan S. Moiseev, Sergey N. Bondarenko, Natalia B. Mikhaylova, Boris V. Afanasyev
Raisa Gorbacheva Institute of Children Oncology, Hematology and Transplantation, First Pavlov State Medical University of Saint-Petersburg, Saint-Petersburg, Russia
Summary
Introduction
HIV infection is often associated with a significantly increased risk of cancer including Hodgkin lymphoma (HL) and non-Hodgkin lymphoma (NHL), even when the patients are treated successfully with modern combined anti-retroviral therapy (cART). Broad implementation of cART caused immune system protection, thus changing therapeutic approaches to HIV-related lymphoma, allowing usage of aggressive treatment strategies including high-dose chemotherapy (HDC) followed by autologous hematopoietic stem cell transplantation (ASCT). The aim of our study was to estimate safety and efficiency of ASCT procedure in patients with HIV-related lymphoma who met standard transplant criteria.Patients and methods
Since January 2016, five patients with HIV-related lymphoma who underwent ASCT were included in prospective single- centre study (study group – HIV group, n=5). The data on the non-HIV-infected patients with lymphoma undergoing ASCT at the same period of time (control group, n=25) were also collected, in order to compare efficacy and safety of the procedure (1:5). Median follow-up time was 14 (1-20) months for the both groups. The primary endpoint of the study was to estimate overall survival (OS) at 12 months after ASCT. Secondary endpoints included time of hematopoietic recovery and toxicity effects. ASCTs were performed at the Raisa Gorbacheva Institute of Children Oncology, Haematology and Transplantation, First Pavlov State Medical University of St. Petersburg. Common Terminology Criteria for Adverse Events (CTCAE 4.0) have been used for the toxicity analysis. The underlying diseases in control group were: HL (n=18; 72%), and NHL (n=7; 28%), HIV-group with HL (n=3; 60%), NHL (n=2; 40%). The median day from diagnosis to ASCT was 362 days in control group, and 525 days in HIV-group. HIV status in study group at the moment of transplantation showed undetectable HIV viral in 100% of the cases; the median CD4+ cell number was 255 cells/mcL, and all the patients received cART.Results
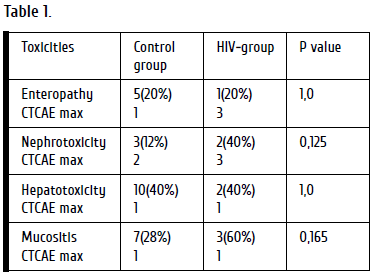
Overall survival (OS) for the entire patient group (n=30) was 93% at 12 months after ASCT, with OS at 12 months of 100% in the HIV-group vs 92% in control group (p=0.475). The median recovery terms for leukocytes, neutrophils, and platelets were D+13, D+18, D+13, respectively, in control group, and D+13, D+14, D+16 in HIV-group. The rates of toxicity according to CTCAE are outlined in Table 1. Relapse of the underlying disease at 12 months after ASCT was diagnosed in 3 (12%) patients of control group, and in one case (20%) from the HIV-infected group (p=0.63).