Hemorrhagic cystitis as a complication after allogeneic hematopoietic stem cell transplantation
Vera A. Vasilyeva, Elena N. Parovichnikova, Mikhail Y. Drokov, Larisa A. Kuzmina, Olga M. Koroleva, Daria S. Dubnyak, Ekaterina D. Mikhaltsova, Natalia N. Popova, Zoya V. Konova, Valery G. Savchenko and CIC 930
National Research Center for Hematology, Moscow, Russian Federation
Summary
Introduction
Hemorrhagic cystitis (HC) is one of the most serious complication after allogeneic hematopoietic stem cell transplantation (alloHSCT) and generally associated with using cyclophosphamide (CY) in conditioning regimen or as a tolerance inductor after allo-HSCT. Also HC can be connected with persistence of Polyomaviridae viruses family.Patients and methods
267 patients with different hematological malignancies underwent alloHSCT between November 2011 and February 2017 at the BMT Department of National Research Center for Hematology. Hemorrhagic cystitis (HC) occurred in 39 cases (14.6%). There were 29 patients with acute leukemia (AML, 17; ALL, 12), five patients had MDS and MPD, three subjects had lymphoproliferative neoplasms; 1, aplastic anemia, and 1 patient with CML. Median of age was 34 years (19 to 61 years). 27 patients (69.2%) were in remission before conditioning regimen, and 12 (30.8%) were transplanted in progression. Related donors were used in 11 (28.2%) cases, unrelated donor, in 28 (71.8%). 23 (59%) patients were transplanted from fully matched donor (10 of 10), whereas 16 patients (41%) were transplanted from a partially matched donor, including haploidentical HSCT. Myeloablative conditioning regimen (MAC) was administered in 17 patients (43.6%), reduced-intensity conditioning (RIC) was applied in 22 (56.4%) of the patients. Cyclophosphamide (CY) had been used as a part of conditioning regimen and/or after transplantation on +3, +4 day in 32 patients (82.1%). Sixteen patients of 39 (41%) developed acute GVHD, being of severe grade (3-4) in 50% of this subgroup.Results
The onset of HC ranged from 1 to 139 days after alloHSCT (a median of 39 days), and lasted for 6 to 133 days (median of 25 days). As to clinical grading, the cystitis was classified by hematuria grade (Droller et al. 1982). We observed grade I HC in 7 (17.9%) patients; grade II, in 18 (46.2%); grade III, in 10 (25.6%); grade IV. in 4 cases (10.3%) . HC occured more frequently during the early post-transplant period Cystitis associated with chemotherapy (within first week after ending the conditioning), especially after CY-containing regimens, was revealed after allo-HCT in four patients (10.25%). Late occurrence of HC was detected in 35 cases (89,75%). Late HC was associated with the following etiological factors: viral infections (BK virus, JC virus, CMV, human herpesvirus type 6, herpes simplex virus type 1/2, or a combination of this viruses) observed in 19 cases (54.4%); bacterial infection in 4 cases (11.4%); mixed infection,in 8 (22.8%). In 4 cases (11.4%), we didn’t detect any etiological factor, but polyomaviruses were not checked due to technical problems (Fig. 1). Gram-positive bacteria from Enterococcaceae family were detected in bacterial and mixed infection in most cases of late HC.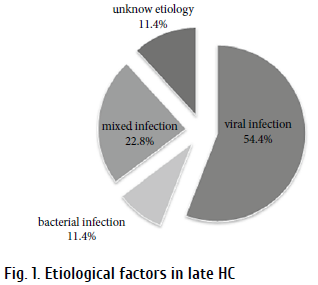
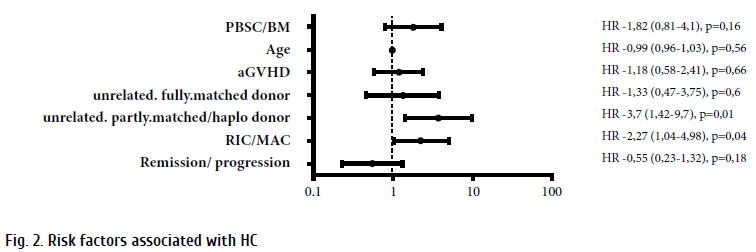
The factors associated with a significantly elevated risk of HC from multi-factor analysis were: alloHSCT from unrelated partly matched donor or haploidentical (i.e. using more immunosuppressive therapy) (p=0.01) and MAC (p=0.04) (Fig. 2). It should be noted that CY was used as a part of conditioning regimen and/or after transplantation in 82.1% patients with HC.
Conclusion
HC is a frequent complication (14.6%) in BMT practice. Early HC is a rare complication in our days due to common prophylaxis such as intravenous hyperhydration (3l/m2/d) and Mesna. The majority of patients with HC needed to administer antibiotics, antiviral drugs and i/v immunoglobulin infusions.Thus HC is still a serious complication which can significant prolong hospitalization and decrease life quality.


