Restoration of bone marrow niches is the basis of optimization of HSC engraftment
Ilya Ya. Bozo
Moscow Dental University, OJSC "Human Stem Cells Institute", Moscow, Russia
Correspondence
Ilya Ya. Bozo, Moscow Dental University, OJSC "Human Stem Cells Institute", 3/2 Gubkina str., 119991, Moscow, Russia; Phone: +7965147-12-77, Fax: +7495646-80-76
E-mail: bozo.ilya@gmail.com
Accepted 10 December 2011
Published 14 December 2011
Summary
The essay presents the problematic aspects of hematopoietic stem cell transplantation, from the position of fundamental notions about cell niches and contemporary data on the bone marrow stroma of recipient and donor, taking into account the results of one’s own research.
Keywords
hematopoietic stem cells (HSCs) transplantation, cell niches, bone marrow stroma
Introduction
Hematopoietic stem cell (HSC) transplantation is the best example of cell technology usage in clinical practice. However, the complexity associated with low HSC engraftment, the development of the "graft-versus-host disease" reaction, and infectious complications have not been eliminated so far [24]. The causes and manifestations of immunological disorders are clear in general, but low engraftment etiology remains the subject of lively debates. The subject of the development is progenitor cells, conditioning protocols, and the "destiny" of elements of bone marrow (BM) stroma transplanted along with HSCs, which specifications are necessary for the development of HSC engraftment. Our research group efforts are also focused on solving the problem. Thus this essay is directed toward systemizing the fundamental and current data of HSC engraftment and the causes of its low level in allogeneic transplantation, as well as to discuss world trends in optimization of HSC engraftment using one’s own data.
Current approaches to improve HSC engraftment
Modern solutions aimed at increasing HSC engraftment can be divided into two directions:
a) techniques directed to the donor’s body and the graft in order to improve the quality and graft "acceptance";
b) methods of influence on the recipient’s body to optimize the "acceptance" of the transplanted HSCs.
The first direction is based on current data of possible HSC expansion in vitro [23], cell activation, and on studies of alternative HSC sources (cord blood, in particular) [5]. The fundamentals of the second approach are associated with studies of BM stroma, HSCs niches, and the processes occurring to stroma cellular elements forming a part of the graft into the recipient’s body. There are no comprehensive data of the processes occurring to BM stroma or bone tissue as an element of cell niches under the influence of conditioning protocols, and there is no generalized concept of the "destiny" of transplanted cellular elements of BM stroma. At the same time the necessity for such data is enormous, as it, on the one hand, helps to develop the most effective methods of HSC engraftment, and on the other hand helps to develop the technology of pathology correction of connective tissues (myelofibrosis, osteogenesis imperfecta, etc).
The concept of HSC niches is the best implementation of theoretical data on BM stroma and its role in providing hematopoiesis, and it serves for better understanding and practical application as well.
HSC niches: fundamental provisions and new vision
Generally, a cell niche is an elementary functional unit of the microenvironment. However, there is no unified, generally accepted definition of the "cell niche". The first part of the hypothetical definition, reflecting niche structure (the set of spatially organized cell elements and components of intercellular matrix) is not contested, although the functional aspect is debatable. Some authors believe that a cell niche maintains a stem cell in undifferentiated quiescent state [3]. The majority take a different view, giving a cell niche a greater role: not only the maintenance of "cellular homeostasis", but also the regulation and provision of morpho-functional activity [16].
Nowadays, scientists distinguish two types of HSCs niches: vascular (endothelial) and endosteal (osteoblastic) [22]. To my mind, this differentiation is rather conditional, since the osteoblastic line cells, forming the niches of the same name and requiring active oxygenation, are situated close to the microvasculature (the critical distance is 200–250 mkm [11]). Consequently, sinusoidal endothelial cells (EC) must be an integral component of the so-called osteoblastic niches. The main cellular elements of BM niches are osteoblasts, EC and multipotent mesenchymal stromal cells (MMSCs) [16]. Implementation of the activity of cells which form cell niches is carried out in two principal directions.
A. Direct impact due to intercellular contacts and products of specific biologically active substances (SDF-1, SCF, TPO, interleukins, etc) [17]. Thus, spindle-shaped osteoblasts by means of tight adhesive contacts with N-cadherin/β-catenin system interact with HSCs, maintaining them in a "quiescent" state [3, 10];
B. Indirect impact: paracrine incentives transfer (erythropoietin, SDF-1, parathyroid hormone, etc.) from other components of the uniform functional system of hematopoiesis: kidneys, liver, spleen, endocrine glands, autonomic nervous system [25, 26].
However, the results of studies in recent years significantly extend the notion of HSC niches, particularly, HSCs that are found in adipose tissue [13], spleen [15], and placenta [12], given the description of HSC migration to extramedullary tissues, for instance, in polytrauma [1]. Taken together, the results of HSCs' persistence in extramedullary tissues indicate the presence of their niches outside the BM. In this respect, the fundamental classic works of the Russian histology school become critical again. According to the theory of "mesenchymal reserve" by A. Maximow, there are progenitor cells for the connective tissues in definitive tissues, marked by him as "stem mesenchymal cells" [19]. Later, the theory was supported by A. Zavarzin [2] and N. Khlopin [4] and has now been proven with contemporary data [6]. The presence of poorly differentiated cells (perivasculоcytes) going along with blood vessels conforming by their differentiating MMSC potency is now proven and indisputable.
Thus, there is at least a vascular HSC niche in extramedullary tissues. In light of fundamental notions and current data, the adjustment of concepts of HSC niches seems to be logical. To my mind, it is correct to speak about a uniform cell niche consisting of two components (Table 1).
Table 1. Components of HSC niches
|
Signs of comparison |
Nonspecific component |
Specific component |
|---|---|---|
|
Cells |
EC and MMSCs |
Resident cells of the definitive tissues (osteoblasts of bone marrow, fibroblasts of fibrous connective tissue, etc.) |
|
Function |
Provision of migration, transduction of regulatory incentives and regulation of non-specific functions |
Provision of a specific function* |
|
*Osteoblasts play the defining role in the regulation of hematopoietic HSC function. It is proved that osteoblasts induce proliferation and differentiation of HSCs in a greater degree than MMSCs [20]. In extramedullary tissues the specific component of cell niches incentivizes HSC homing and the implementation of other specific effects, such as participation in reparative regeneration [1]. |
||
|
Cell Ther Transplant. 2011;3:e.000095.01. doi:10.3205/ctt-2011-en-000095-table1 |
||
Such a systematic generalized concept of HSCs niche is easier and more practical.
The possibilities to restore cell niches
The practical significance of the concept of HSCs niche is in clearer comprehension of the functioning of BM stroma and the possibility of a selective approach to its restoration after conditioning. However, it is necessary to solve two problem issues to perform it in practice.
1. What components of cell niches are damaged with different conditioning protocols, and to what degree?
2. What way can a damaged component of a cell niche be restored?
Currently there are not enough data to give an exhaustive answer to the questions. It is established that in total irradiation the specific component of BM niches is not really damaged, thus providing a moderate level of HSC engraftment [10]. Irradiation causes marked damage to a nonspecific component: sinusoidal ES are damaged [14], and MMSCs obtain functional defects [21]. Apparently, a similar situation is typical of extramedullary HSCs niches. The influence of chemotherapy on BM niches is less studied due to the great variety of protocols. In general chemotherapy does less damage to the nonspecific component of niches [14].
However, taking into consideration the paucity of data on the damaging effect of conditioning regimens, therapeutic conditions which are aimed at restoring the two components of the niches are clear.
Our research group managed to figure out the processes to a certain extent, concerning the transplanted cellular elements of BM stroma. It has been shown with an experimental model of osteogenesis that the restoration of wholeness of mice shin bones irradiated at a dose of 7–7.5 Gy is mainly carried out due to the transplanted transgenic (GFP+) cells of allogeneic BM (Fig. 1). Moreover, even under physiological conditions the inserted components of allogeneic BM stroma planted the patches of typical location of the dispersed cambium of skeletal tissues (periosteum, endosteum, BM stroma, perivascular niches). Up to 30% of osteocytes of bone tissue were of donor origin (Fig. 2) [7]. These data are consistent with the results of other research groups and prove the possibility of the planting of recipient tissues transplanted with HSC elements of allogeneic BM stroma, as well as confirm their involvement in the implementation of reparative processes in skeletal tissues [9]. Consequently, the use of components of BM stroma (MMSCs, endothelial progenitor cells) is potentially practiced for regeneration of BM HSC niches, as well as for treatment of patients with the pathology of skeletal tissue stroma. However, the number of necessary stroma components in the whole BM is not enough (2–5×103 MMSCs/kg), and consequently only 7% of transplanted MMSCs remain for long in the stroma of a recipient’s BM [21]. At the same time the expansion of MMSCs in vitro up to the concentration in the graft (20–30×106 MMSCs per 1 kg of a recipient’s weight) significantly increases the level of stroma planting of the recipient’s BM, which are maintained over time [8]. Moreover, there are published data on the improvement of HSCs' engraftment during their co-transplantation with so-called "stromal cells of umbilical cord blood" [18].
Figure 1. Shin bone tissues of the recipient mouse: A: spongy bone tissue (1: GFP-positive cells of bone marrow and stroma, 2: endosteum with GFP-positive osteoblast, 3: bony trabeculae), magnification ×100. B: trabecula of bone and cartilage regenerate, consisting of GFP-positive cells; magnification ×400. C: isogenous group of GFP-positive chondrocytes in the bone and cartilage regenerate; magnification ×800. Confocal microscopy. Color: propidium iodide
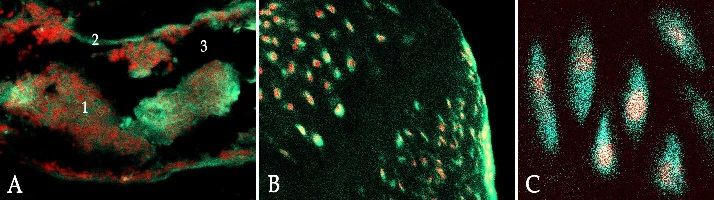
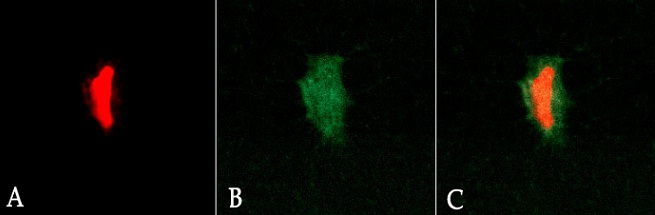
Figure 2. Osteocyte in the reticular fibrous bone tissue of the regenerate, having donor origin: А: a cell nucleus, propidium iodide stained, B: cytoplasm autofluorescence; C: combined image. Magnification ×800. Confocal microscopy
Thus, the fortification of the whole BM graft or a purified HSCs fraction with stromal cellular components in concentrations exceeding physiologic congestion is potentially effective. Furthermore, considering the important role of EC as the components of HSCs niches, transplantation of their progenitor cells in high concentrations seems to be promising, especially in combination with factors stimulating angiogenesis (for instance, medicines on the basis of VEGF). In any case, the actual clinical application of the methods requires further clinical trials.
Acknowledgements
The author wishes to thank Roman V. Deev (OJSC "Human Stem Cells Institute", Moscow, Russia), and Natalia V. Tsupkina (Institute of Cytology RAS, St. Petersburg, Russia), for qualified direction and assistance in scientific research.
References
1. Александров ВН, Сергеев ВС. Влияние тяжелой политравмы на миграцию стволовых кроветворных клеток у мышей. Клеточная трансплантология и тканевая инженерия. 2006;2(4):59-62.
2. Заварзин АА. Курс гистологической и микроскопической анатомии. Л.: Гос. из-во мед. лит-ры. 1938. 634 c.
3. Пинаев ГП. Ниши стволовых клеток (понятие «тканевой ниши» и значение белков внеклеточного матрикса для регулирования функций стволовых клеток). Материалы школы-конференции для молодых ученых «Клеточные технологии для регенеративной медицины». СПб. 17-21 окт. 2011.
4. Хлопин НГ. Общебиологические и экспериментальные основы гистологию Л.: Из-во АН СССР. 492 с.
7. Deev RV, Tsupkina NV, Serikov VB, Gololobov VG, Pinaev GP. Participation of transfused bone marrow cells in reparative osteohistogenesis. Tsitologiia. 2005;47(9):755-759. In Russian.
8. Devine SM, Bartholomew AM, et al. Mesenchymal stem cells are capable of homing to the bone marrow of non-human primates following systemic infusion. Exp Hematol. 2001 Feb;29(2):244-55.
15. Iseki A, Morita Y, Nakauchi H, et al. Hematopoietic Stem Cells in the Mouse Spleen. Blood (ASH Annual Meeting Abstracts). 2008:112.
16. Isern J, Méndez-Ferrer S. Stem cell interactions in a bone marrow niche. Curr Osteoporos Rep. 2011 Dec;9(4):210-8.
18. Liu Y, Yi L, Zhang X, Gao L, Zhang C, Feng YM, Chen XH. Cotransplantation of human umbilical cord blood-derived stromal cells enhances hematopoietic reconstitution and engraftment in irradiated BABL/c mice. Cancer Biol Ther. 2011 Jan 1;11(1):84-94.
19. Brodersen J, Maximow A, Schaffer J. Handbuch der mikroskopischen Anatomie des Menschen. Bd. 2., Die Gewebe; T. 1., Epithel- u. Drüsengewebe, Bindegewebe und blutbildende Gewebe, Blut. Berlin: Springer, 1927.
20. Mishima S, Nagai A, Abdullah S, Matsuda C, Taketani T, Kumakura S, Shibata H, Ishikura H, Kim SU, Masuda J. Effective ex vivo expansion of hematopoietic stem cells using osteoblast-differentiated mesenchymal stem cells is CXCL12 dependent. Eur J Haematol. 2010 Jun;84(6):538-46. doi: 10.1111/j.1600-0609.2010.01419.x.
24. Rafeah NT, Fadilah SA. The A-B-C of haematopoietic stem cell transplantation. Med J Malaysia. 2009 Mar;64(1):94-100.
25. Rashidi N, Adams GB. The influence of parathyroid hormone on the adult hematopoietic stem cell niche. Curr Osteoporos Rep. 2009 Jul;7(2):53-7.
26. Visigalli I, Biffi A. Maintenance of a functional hematopoietic stem cell niche through galactocerebrosidase and other enzymes. Curr Opin Hematol. 2011 Jul;18(4):214-9.
Accepted 10 December 2011
Published 14 December 2011


